Psychiatric Symptoms in Parkinson's Disease
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
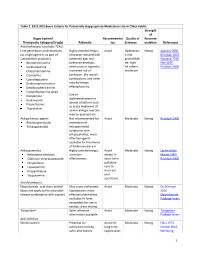
Table 2. 2012 AGS Beers Criteria for Potentially
Table 2. 2012 AGS Beers Criteria for Potentially Inappropriate Medication Use in Older Adults Strength of Organ System/ Recommendat Quality of Recomm Therapeutic Category/Drug(s) Rationale ion Evidence endation References Anticholinergics (excludes TCAs) First-generation antihistamines Highly anticholinergic; Avoid Hydroxyzin Strong Agostini 2001 (as single agent or as part of clearance reduced with e and Boustani 2007 combination products) advanced age, and promethazi Guaiana 2010 Brompheniramine tolerance develops ne: high; Han 2001 Carbinoxamine when used as hypnotic; All others: Rudolph 2008 Chlorpheniramine increased risk of moderate Clemastine confusion, dry mouth, Cyproheptadine constipation, and other Dexbrompheniramine anticholinergic Dexchlorpheniramine effects/toxicity. Diphenhydramine (oral) Doxylamine Use of diphenhydramine in Hydroxyzine special situations such Promethazine as acute treatment of Triprolidine severe allergic reaction may be appropriate. Antiparkinson agents Not recommended for Avoid Moderate Strong Rudolph 2008 Benztropine (oral) prevention of Trihexyphenidyl extrapyramidal symptoms with antipsychotics; more effective agents available for treatment of Parkinson disease. Antispasmodics Highly anticholinergic, Avoid Moderate Strong Lechevallier- Belladonna alkaloids uncertain except in Michel 2005 Clidinium-chlordiazepoxide effectiveness. short-term Rudolph 2008 Dicyclomine palliative Hyoscyamine care to Propantheline decrease Scopolamine oral secretions. Antithrombotics Dipyridamole, oral short-acting* May -

Drugs to Avoid in Patients with Dementia
Detail-Document #240510 -This Detail-Document accompanies the related article published in- PHARMACIST’S LETTER / PRESCRIBER’S LETTER May 2008 ~ Volume 24 ~ Number 240510 Drugs To Avoid in Patients with Dementia Elderly people with dementia often tolerate drugs less favorably than healthy older adults. Reasons include increased sensitivity to certain side effects, difficulty with adhering to drug regimens, and decreased ability to recognize and report adverse events. Elderly adults with dementia are also more prone than healthy older persons to develop drug-induced cognitive impairment.1 Medications with strong anticholinergic (AC) side effects, such as sedating antihistamines, are well- known for causing acute cognitive impairment in people with dementia.1-3 Anticholinergic-like effects, such as urinary retention and dry mouth, have also been identified in drugs not typically associated with major AC side effects (e.g., narcotics, benzodiazepines).3 These drugs are also important causes of acute confusional states. Factors that may determine whether a patient will develop cognitive impairment when exposed to ACs include: 1) total AC load (determined by number of AC drugs and dose of agents utilized), 2) baseline cognitive function, and 3) individual patient pharmacodynamic and pharmacokinetic features (e.g., renal/hepatic function).1 Evidence suggests that impairment of cholinergic transmission plays a key role in the development of Alzheimer’s dementia. Thus, the development of the cholinesterase inhibitors (CIs). When used appropriately, the CIs (donepezil [Aricept], rivastigmine [Exelon], and galantamine [Razadyne, Reminyl in Canada]) may slow the decline of cognitive and functional impairment in people with dementia. In order to achieve maximum therapeutic effect, they ideally should not be used in combination with ACs, agents known to have an opposing mechanism of action.1,2 Roe et al studied AC use in 836 elderly patients.1 Use of ACs was found to be greater in patients with probable dementia than healthy older adults (33% vs. -

Nomination Background: Ketamine Hydrochloride (CASRN: 1867-66-9)
KETAMINE Nomination TABLE OF CONTENTS Page 1.0 BASIS OF NOMINATION 1 2.0 BACKGROUND INFORMATION 1 3.0 CHEMICAL PROPERTIES 2 3.1 Chemical Identification 2 3.2 Physico-Chemical Properties 3 3.3 Purity and Commercial Availability 4 4.0 PRODUCTION PROCESSES AND ANALYSIS 6 5.0 PRODUCTION AND IMPORT VOLUMES 7 6.0 USES 7 7.0 ENVIRONMENTAL OCCURRENCE 7 8.0 HUMAN EXPOSURE 7 9.0 REGULATORY STATUS 7 10.0 CLINICAL PHARMACOLOGY 7 11.0 TOXICOLOGICAL DATA 13 11.1 General Toxicology 13 11.2 Neurotoxicology 14 12.0 CONCLUSIONS 15 APPENDIX A 17 APPENDIX B 23 APPENDIX C 27 1 KETAMINE 1.0 BASIS OF NOMINATION Ketamine, a noncompetitive NMDA receptor blocker, has been used extensively off - label as a pediatric anesthetic for surgical procedures in infants and toddlers. Recently, Olney and coworkers have demonstrated severe widespread apoptotic degeneration throughout the rapidly developing brain of the 7-day-old rat after ketamine administration. Recent research at FDA has confirmed and extended Olney’s observations. These findings are cause for concern with respect to ketamine use in children. The issue of whether the neurotoxicity found in this animal model (rat) has scientific and regulatory relevance for the pediatric use of ketamine relies heavily upon confirmation of these findings that may be obtained from the conduct of an appropriate study in non-human primates. 2.0 BACKGROUND INFORMATION The issue of potential ketamine neurotoxicity in children surfaced as a result of FDA’s reluctance to approve an NIH pediatric clinical trial using this compound because of its documented neurotoxic effects in young rats (published in several papers over the last ten years by Olney and co-workers). -

The Anticholinergic Toxidrome
Poison HOTLINE Partnership between Iowa Health System and University of Iowa Hospitals and Clinics July 2011 The Anticholinergic Toxidrome A toxidrome is a group of symptoms associated with poisoning by a particular class of agents. One example is the opiate toxidrome, the triad of CNS depression, respiratory depression, and pinpoint pupils, and which usually responds to naloxone. The anticholinergic toxidrome is most frequently associated with overdoses of diphenhydramine, a very common OTC medication. However, many drugs and plants can produce the anticholinergic toxidrome. A partial list includes: tricyclic antidepressants (amitriptyline), older antihistamines (chlorpheniramine), Did you know …… phenothiazines (promethazine) and plants containing the anticholinergic alkaloids atropine, hyoscyamine and scopolamine (Jimson Weed). Each summer, the ISPCC receives approximately 10-20 The mnemonic used to help remember the symptoms and signs of this snake bite calls, some being toxidrome are derived from the Alice in Wonderland story: from poisonous snakes (both Blind as a Bat (mydriasis and inability to focus on near objects) local and exotic). Red as a Beet (flushed skin color) Four poisonous snakes can be Hot as Hades (elevated temperature) found in Iowa: the prairie These patients can sometimes die of agitation-induced hyperthermia. rattlesnake, the massasauga, Dry as a Bone (dry mouth and dry skin) the copperhead, and the Mad as a Hatter (hallucinations and delirium) timber rattlesnake. Each Bowel and bladder lose their tone (urinary retention and constipation) snake has specific territories Heart races on alone (tachycardia) within the state. ISPCC A patient who has ingested only an anticholinergic substance and is not specialists have access to tachycardic argues against a serious anticholinergic overdose. -

3 Drugs That May Cause Delirium Or Problem Behaviors CARD 03 19 12 JUSTIFIED.Pub
Drugs that May Cause Delirium or Problem Behaviors Drugs that May Cause Delirium or Problem Behaviors This reference card lists common and especially problemac drugs that may Ancholinergics—all drugs on this side of the card. May impair cognion cause delirium or contribute to problem behaviors in people with demena. and cause psychosis. Drugs available over‐the‐counter marked with * This does not always mean the drugs should not be used, and not all such drugs are listed. If a paent develops delirium or has new problem Tricyclic Andepressants Bladder Anspasmodics behaviors, a careful review of all medicaons is recommended. Amitriptyline – Elavil Darifenacin – Enablex Be especially mindful of new medicaons. Clomipramine – Anafranil Flavoxate – Urispas Desipramine – Norpramin Anconvulsants Psychiatric Oxybutynin – Ditropan Doxepin – Sinequan Solifenacin – VESIcare All can cause delirium, e.g. All psychiatric medicaons should be Imipramine – Tofranil Tolterodine – Detrol Carbamazepine – Tegretol reviewed as possible causes, as Nortriptyline – Aventyl, Pamelor Gabapenn – Neuronn effects are unpredictable. Trospium – Sanctura Anhistamines / Allergy / Leveracetam – Keppra Notable offenders include: Insomnia / Sleep Valproic acid – Depakote Benzodiazepines e.g. Cough & Cold Medicines *Diphenhydramine – Sominex, ‐Alprazolam – Xanax *Azelasne – Astepro Pain Tylenol‐PM, others ‐Clonazepam – Klonopin *Brompheniramine – Bromax, All opiates can cause delirium if dose *Doxylamine – Unisom, Medi‐Sleep ‐Lorazepam – Avan Bromfed, Lodrane is too high or -

Medicare Part D Excluded Drug List
MEDICARE PART D EXCLUDED DRUGS LIST 2016_updated July 2016 Reason: LIST = multiple reasons it's excluded; "not covered under Part D law" Reason: Not properly listed with FDA = CMS considers it best practice for Part D sponsors to consider the proper listing of a drug product with the FDA as a prerequisite for making a Part D drug coverage determination. The FDA is unable to provide regulatory status determinations through their regular processes if a drug product is not properly listed. Therefore, Part D sponsors should begin the drug coverage determination process by confirming that a prescription drug product national drug code (NDC) is properly listed with the FDA. Reason: DESI = Less Than Effective (LTE) drug for ALL indications Label Name Reason 1ST BASE CRE Bulk Ingredient 2-FUCCOSYLLA PAK LACTO-N Medical Food ABANEU-SL SUB Vitamin/Mineral ABLAVAR INJ 244MG/ML Diagnostic Agent ACACIA EXTRA SOL 1:20 Non-standardized allergenic ACCUCAINE INJ 1% LIST ACD FORMULA SOL A Blood Component ACD-A SOL Blood Component ACLARO PD EMU 4% Cosmetic ACREMONIUM SOL 20000PNU Non-standardized allergenic ACTCT FLEX 3 PAD 4"X4" Not properly listed with FDA ACTHREL INJ 100MCG Diagnostic Agent ACTI ANTIMIC PAD 2"X2" Not properly listed with FDA ACTI ANTIMIC PAD 4"X4" Not properly listed with FDA ACTICOAT 7 PAD 2"X2" Not properly listed with FDA ACTICOAT 7 PAD 4"X5" Not properly listed with FDA ACTICOAT ABS PAD 4"X5" Not properly listed with FDA ACTICOAT MOI PAD 2"X2" Surgical Supply/Medical ACTICOAT MOI PAD 4"X4" Surgical Supply/Medical ACTICOAT MOI PAD -

Hyoscyamine, Atropine, Scopolamine, and Phenobarbital
PATIENT & CAREGIVER EDUCATION Hyoscyamine, Atropine, Scopolamine, and Phenobarbital This information from Lexicomp® explains what you need to know about this medication, including what it’s used for, how to take it, its side effects, and when to call your healthcare provider. Brand Names: US Donnatal; Phenohytro What is this drug used for? It is used to treat irritable bowel syndrome. It is used to treat ulcer disease. It may be given to your child for other reasons. Talk with the doctor. What do I need to tell the doctor BEFORE my child takes this drug? If your child is allergic to this drug; any part of this drug; or any other drugs, foods, or substances. Tell the doctor about the allergy and what signs your child had. If your child has any of these health problems: Heart problems due to bleeding, bowel block, enlarged colon, glaucoma, a hernia Hyoscyamine, Atropine, Scopolamine, and Phenobarbital 1/9 that involves your stomach (hiatal hernia), myasthenia gravis, slow-moving GI (gastrointestinal) tract, trouble passing urine, or ulcerative colitis. If your child has ever had porphyria. If your child has been restless or overexcited in the past after taking phenobarbital. If your child is addicted to drugs or alcohol, or has been in the past. This is not a list of all drugs or health problems that interact with this drug. Tell the doctor and pharmacist about all of your child’s drugs (prescription or OTC, natural products, vitamins) and health problems. You must check to make sure that it is safe to give this drug with all of your child’s other drugs and health problems. -

Hb 185 an Act Listing Synthetic
62nd Legislature HB0185 AN ACT LISTING SYNTHETIC MARIJUANA AND SALVIA AS DANGEROUS DRUGS; REQUIRING RULEMAKING BY THE DEPARTMENT OF PUBLIC HEALTH AND HUMAN SERVICES; PROVIDING PENALTIES; AMENDING SECTIONS 44-12-102, 45-9-101, 45-9-102, 45-9-110, 50-31-306, 50-31-310, AND 50-32-222, MCA; AND PROVIDING AN IMMEDIATE EFFECTIVE DATE. BE IT ENACTED BY THE LEGISLATURE OF THE STATE OF MONTANA: Section 1. Section 44-12-102, MCA, is amended to read: "44-12-102. Things subject to forfeiture. (1) The following are subject to forfeiture: (a) all controlled substances that have been manufactured, distributed, prepared, cultivated, compounded, processed, or possessed in violation of Title 45, chapter 9; (b) all money, raw materials, products, and equipment of any kind that are used or intended for use in manufacturing, preparing, cultivating, compounding, processing, delivering, importing, or exporting any controlled substance in violation of Title 45, chapter 9, except items used or intended for use in connection with quantities of marijuana in amounts less than 60 grams; (c) except as provided in subsection (2)(d), all property that is used or intended for use as a container for anything enumerated in subsection (1)(a) or (1)(b); (d) except as provided in subsection (2), all conveyances, including aircraft, vehicles, and vessels, that are used or intended for use in any manner to facilitate the commission of a violation of Title 45, chapter 9; (e) all books, records, and research products and materials, including formulas, microfilm, tapes, and data, -

Symptomatic Approach to Gas, Belching and Bloating 21
20 Osteopathic Family Physician (2019) 20 - 25 Osteopathic Family Physician | Volume 11, No. 2 | March/April, 2019 Gennaro, Larsen Symptomatic Approach to Gas, Belching and Bloating 21 Review ARTICLE to escape. This mechanism prevents the stomach from becoming IRRITABLE BOWEL SYNDROME (IBS) Symptomatic Approach to Gas, Belching and Bloating damaged by excessive dilation.2 IBS is abdominal pain or discomfort associated with altered with OMT Treatment Options Many patients with GERD report increased belching. Transient bowel habits. It is the most commonly diagnosed GI disorder lower esophageal sphincter (LES) relaxation is the major and accounts for about 30% of all GI referrals.7 Criteria for IBS is recurrent abdominal pain at least one day per week in the Carly Gennaro, DO1; Helaine Larsen, DO1 mechanism for both belching and GERD. Recent studies have shown that the number of belches is related to the number of last three months associated with at least two of the following: times someone swallows air. These studies have concluded that 1) association with defecation, 2) change in stool frequency, 1 Good Samaritan Hospital Medical Center, West Islip, NY patients with GERD swallow more air in response to heartburn and 3) change in stool form. Diagnosis should be made using these therefore belch more frequently.3 There is no specific treatment clinical criteria and limited testing. Common symptoms are for belching in GERD patients, so for now, physicians continue to abdominal pain, bloating, alternating diarrhea and constipation, treat GERD with proton pump inhibitors (PPIs) and histamine-2 and pain relief after defecation. Pain can be present anywhere receptor antagonists with the goal of suppressing heartburn and in the abdomen, but the lower abdomen is the most common KEYWORDS: ABSTRACT: Intestinal gas production is a normal physiologic progress. -

(+)-Hyoscyamine and (–)-Scopolamine
CALL FOR DATA ON (–)-HYOSCYAMINE, (+)-HYOSCYAMINE AND (–)-SCOPOLAMINE Deadline: 31 January 2020 Background Atropine and scopolamine belong to the class of tropane alkaloids (TA), a group of compounds that are secondary metabolites occurring in several plant families, such as Brassicaceae, Solanaceae and Erythroxylaceae. While there are more than 200 different TA identified in various plants, this call for data focuses on (–)-hyoscyamine, (+)-hyoscyamine and (–)-scopolamine. The racemic mixture of (–)-hyoscyamine and (+)-hyoscyamine is called atropine. Tropane Alkaloid related incident Assisting 86.7 million people in around 83 countries each year, the World Food Programme (WFP) is the leading humanitarian organization saving lives and changing lives, delivering food assistance in emergencies and working with communities to improve nutrition and build resilience. Super Cereal is a flour-type product made of pre-cooked corn, soybean and micronutrients. It is used mainly for pregnant and lactating mothers (PLW), nutritionally vulnerable groups including people living with HIV and tuberculosis (TB), and children above five years old. Annually, WFP distributes approximately 130,000 MT Super Cereal to 4.9 million people with the objective of improving food security and preventing malnutrition. In March 2019, four people died and 296 were admitted to health facilities after eating Super Cereal in Uganda. A joint investigation performed by Uganda Government, US CDC/FDA, WHO and WFP pointed towards tropane alkaloids, contaminants issued from toxic seeds (i.e. Datura stramonium), as the cause of intoxication. WFP took immediate measures on the stock and the implicated supplier, and continue to actively consult with experts, including FAO’s Office of Food Safety to manage this risk. -
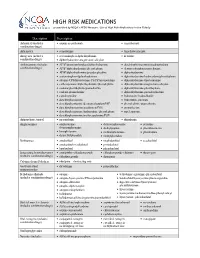
HIGH RISK MEDICATIONS As Specified by NCQA’S HEDIS Measure: Use of High Risk Medications in the Elderly
HIGH RISK MEDICATIONS as specified by NCQA’s HEDIS Measure: Use of High Risk Medications in the Elderly Description Prescription Antianxiety (includes • aspirin-meprobamate • meprobamate combination drugs) Antiemetics • scopolamine • trimethobenzamide Analgesics (includes • acetaminophen-diphenhydramine • ketorolac combination drugs) • diphenhydramine-magnesium salicylate Antihistamines (includes • APAP/dextromethorphan/diphenhydramine • dexchlorpheniramine-pseudoephedrine combination drugs) • APAP/diphenhydramine/phenylephrine • dextromethorphan-promethazine • APAP/diphenhydramine/pseudoephedrine • diphenhydramine • acetaminophen-diphenhydramine • diphenhydramine/hydrocodone/phenylephrine • atropine/CPM/hyoscyamine/PE/PPA/scopolamine • diphenhydramine-tripelennamine • carbetapentane/diphenhydramine/phenylephrine • diphenhydramine-magnesium salicylate • codeine/phenylephrine/promethazine • diphenhydramine-phenylephrine • codeine-promethazine • diphenhydramine-pseudoephedrine • cyproheptadine • hydroxyzine hydrochloride • dexchlorpheniramine • hydroxyzine pamoate • dexchlorpheniramine/dextromethorphan/PSE • phenylephrine-promethazine • dexchlorpheniramine/guaifenesin/PSE • promethazine • dexchlorpheniramine/hydrocodone/phenylephrine • tripelennamine • dexchlorpheniramine/methscopolamine/PSE Antipsychotic, typical • mesoridazine • thioridazine Amphetamines • amphetamine- • dextroamphetamine • pemoline dextroamphetamine • diethylpropion • phendimetrazine • benzphetamine • methamphetamine • phentermine • dexmethylphenidate • methylphenidate -

Hyoscyamine Fact Sheet
Hyoscyamine: MedlinePlus Drug Information Page 1 of 3 Skip navigation Other drug names: A B C D E F G H I J K L M N O P Q R S T U V W X Y Z 0-9 Hyoscyamine (hye oh sye' a meen) Contents of this page: z Why is this medication prescribed? z What storage conditions are needed for this z How should this medicine be used? medicine? z What special precautions should I follow? z In case of emergency/overdose z What special dietary instructions should I follow? z What other information should I know? z What should I do if I forget a dose? z Brand names z What side effects can this medication cause? Why is this medication prescribed? Return to top Hyoscyamine is used to control symptoms associated with disorders of the gastrointestinal (GI) tract. It works by decreasing the motion of the stomach and intestines and the secretion of stomach fluids, including acid. Hyoscyamine is also used in the treatment of bladder spasms, peptic ulcer disease, diverticulitis, colic, irritable bowel syndrome, cystitis, and pancreatitis. Hyoscyamine may also be used to treat certain heart conditions, to control the symptoms of Parkinson's disease and rhinitis (runny nose), and to reduce excess saliva production. This medication is sometimes prescribed for other uses; ask your doctor or pharmacist for more information. How should this medicine be used? Return to top Hyoscyamine comes as a tablet, an extended-release (long-acting) capsule, a liquid to take by mouth, and in an injectable form. The tablets and liquid are usually taken three or four times a day.