VA/Dod CLINICAL PRACTICE GUIDELINE for the MANAGEMENT of CHRONIC MULTISYMPTOM ILLNESS
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Gastrointestinal (GI) Motility, Chronic Therapeutic Class Review
Gastrointestinal (GI) Motility, Chronic Therapeutic Class Review (TCR) March 7, 2019 No part of this publication may be reproduced or transmitted in any form or by any means, electronic or mechanical, including photocopying, recording, digital scanning, or via any information storage or retrieval system without the express written consent of Magellan Rx Management. All requests for permission should be mailed to: Magellan Rx Management Attention: Legal Department 6950 Columbia Gateway Drive Columbia, Maryland 21046 The materials contained herein represent the opinions of the collective authors and editors and should not be construed to be the official representation of any professional organization or group, any state Pharmacy and Therapeutics committee, any state Medicaid Agency, or any other clinical committee. This material is not intended to be relied upon as medical advice for specific medical cases and nothing contained herein should be relied upon by any patient, medical professional or layperson seeking information about a specific course of treatment for a specific medical condition. All readers of this material are responsible for independently obtaining medical advice and guidance from their own physician and/or other medical professional in regard to the best course of treatment for their specific medical condition. This publication, inclusive of all forms contained herein, is intended to be educational in nature and is intended to be used for informational purposes only. Send comments and suggestions to [email protected]. March 2019 Proprietary Information. Restricted Access – Do not disseminate or copy without approval. © 2004–2019 Magellan Rx Management. All Rights Reserved. FDA-APPROVED INDICATIONS Drug Manufacturer Indication(s) alosetron (Lotronex®)1 generic, . -
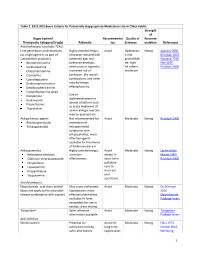
Table 2. 2012 AGS Beers Criteria for Potentially
Table 2. 2012 AGS Beers Criteria for Potentially Inappropriate Medication Use in Older Adults Strength of Organ System/ Recommendat Quality of Recomm Therapeutic Category/Drug(s) Rationale ion Evidence endation References Anticholinergics (excludes TCAs) First-generation antihistamines Highly anticholinergic; Avoid Hydroxyzin Strong Agostini 2001 (as single agent or as part of clearance reduced with e and Boustani 2007 combination products) advanced age, and promethazi Guaiana 2010 Brompheniramine tolerance develops ne: high; Han 2001 Carbinoxamine when used as hypnotic; All others: Rudolph 2008 Chlorpheniramine increased risk of moderate Clemastine confusion, dry mouth, Cyproheptadine constipation, and other Dexbrompheniramine anticholinergic Dexchlorpheniramine effects/toxicity. Diphenhydramine (oral) Doxylamine Use of diphenhydramine in Hydroxyzine special situations such Promethazine as acute treatment of Triprolidine severe allergic reaction may be appropriate. Antiparkinson agents Not recommended for Avoid Moderate Strong Rudolph 2008 Benztropine (oral) prevention of Trihexyphenidyl extrapyramidal symptoms with antipsychotics; more effective agents available for treatment of Parkinson disease. Antispasmodics Highly anticholinergic, Avoid Moderate Strong Lechevallier- Belladonna alkaloids uncertain except in Michel 2005 Clidinium-chlordiazepoxide effectiveness. short-term Rudolph 2008 Dicyclomine palliative Hyoscyamine care to Propantheline decrease Scopolamine oral secretions. Antithrombotics Dipyridamole, oral short-acting* May -

The In¯Uence of Medication on Erectile Function
International Journal of Impotence Research (1997) 9, 17±26 ß 1997 Stockton Press All rights reserved 0955-9930/97 $12.00 The in¯uence of medication on erectile function W Meinhardt1, RF Kropman2, P Vermeij3, AAB Lycklama aÁ Nijeholt4 and J Zwartendijk4 1Department of Urology, Netherlands Cancer Institute/Antoni van Leeuwenhoek Hospital, Plesmanlaan 121, 1066 CX Amsterdam, The Netherlands; 2Department of Urology, Leyenburg Hospital, Leyweg 275, 2545 CH The Hague, The Netherlands; 3Pharmacy; and 4Department of Urology, Leiden University Hospital, P.O. Box 9600, 2300 RC Leiden, The Netherlands Keywords: impotence; side-effect; antipsychotic; antihypertensive; physiology; erectile function Introduction stopped their antihypertensive treatment over a ®ve year period, because of side-effects on sexual function.5 In the drug registration procedures sexual Several physiological mechanisms are involved in function is not a major issue. This means that erectile function. A negative in¯uence of prescrip- knowledge of the problem is mainly dependent on tion-drugs on these mechanisms will not always case reports and the lists from side effect registries.6±8 come to the attention of the clinician, whereas a Another way of looking at the problem is drug causing priapism will rarely escape the atten- combining available data on mechanisms of action tion. of drugs with the knowledge of the physiological When erectile function is in¯uenced in a negative mechanisms involved in erectile function. The way compensation may occur. For example, age- advantage of this approach is that remedies may related penile sensory disorders may be compen- evolve from it. sated for by extra stimulation.1 Diminished in¯ux of In this paper we will discuss the subject in the blood will lead to a slower onset of the erection, but following order: may be accepted. -

Drugs to Avoid in Patients with Dementia
Detail-Document #240510 -This Detail-Document accompanies the related article published in- PHARMACIST’S LETTER / PRESCRIBER’S LETTER May 2008 ~ Volume 24 ~ Number 240510 Drugs To Avoid in Patients with Dementia Elderly people with dementia often tolerate drugs less favorably than healthy older adults. Reasons include increased sensitivity to certain side effects, difficulty with adhering to drug regimens, and decreased ability to recognize and report adverse events. Elderly adults with dementia are also more prone than healthy older persons to develop drug-induced cognitive impairment.1 Medications with strong anticholinergic (AC) side effects, such as sedating antihistamines, are well- known for causing acute cognitive impairment in people with dementia.1-3 Anticholinergic-like effects, such as urinary retention and dry mouth, have also been identified in drugs not typically associated with major AC side effects (e.g., narcotics, benzodiazepines).3 These drugs are also important causes of acute confusional states. Factors that may determine whether a patient will develop cognitive impairment when exposed to ACs include: 1) total AC load (determined by number of AC drugs and dose of agents utilized), 2) baseline cognitive function, and 3) individual patient pharmacodynamic and pharmacokinetic features (e.g., renal/hepatic function).1 Evidence suggests that impairment of cholinergic transmission plays a key role in the development of Alzheimer’s dementia. Thus, the development of the cholinesterase inhibitors (CIs). When used appropriately, the CIs (donepezil [Aricept], rivastigmine [Exelon], and galantamine [Razadyne, Reminyl in Canada]) may slow the decline of cognitive and functional impairment in people with dementia. In order to achieve maximum therapeutic effect, they ideally should not be used in combination with ACs, agents known to have an opposing mechanism of action.1,2 Roe et al studied AC use in 836 elderly patients.1 Use of ACs was found to be greater in patients with probable dementia than healthy older adults (33% vs. -

In Vivo Olanzapine Occupancy of Muscarinic Acetylcholine Receptors in Patients with Schizophrenia Thomas J
In Vivo Olanzapine Occupancy of Muscarinic Acetylcholine Receptors in Patients with Schizophrenia Thomas J. Raedler, M.D., Michael B. Knable, D.O., Douglas W. Jones, Ph.D., Todd Lafargue, M.D., Richard A. Urbina, B.A., Michael F. Egan, M.D., David Pickar, M.D. , and Daniel R. Weinberger, M.D. Olanzapine is an atypical antipsychotic with potent than low-dose in the same regions. Muscarinic occupancy ϭ antimuscarinic properties in vitro (Ki 2–25 nM). We by olanzapine ranged from 13% to 57% at 5 mg/dy and studied in vivo muscarinic receptor occupancy by 26% to 79% at 20 mg/dy with an anatomical pattern olanzapine at both low dose (5 mg/dy) and high dose (20 indicating M2 subtype selectivity. The [I-123]IQNB data mg/dy) in several regions of cortex, striatum, thalamus and indicate that olanzapine is a potent and subtype-selective pons by analyzing [I-123]IQNB SPECT images of seven muscarinic antagonist in vivo, perhaps explaining its low schizophrenia patients. Both low-dose and high-dose extrapyramidal side effect profile and low incidence of olanzapine studies revealed significantly lower anticholinergic side effects. [Neuropsychopharmacology [I-123]IQNB binding than that of drug-free schizophrenia 23:56–68, 2000] Published by Elsevier Science Inc. on patients (N ϭ 12) in all regions except striatum. behalf of the American College of Neuropsychopharmacology [I-123]IQNB binding was significantly lower at high-dose KEY WORDS: Muscarinic receptor; Olanzapine; IQNB; cologically (Watling et al. 1995) and correspond to SPECT; Schizophrenia; Antipsychotic genes (respectively, m1–m5) that have been cloned (Bonner et al. -

Nomination Background: Ketamine Hydrochloride (CASRN: 1867-66-9)
KETAMINE Nomination TABLE OF CONTENTS Page 1.0 BASIS OF NOMINATION 1 2.0 BACKGROUND INFORMATION 1 3.0 CHEMICAL PROPERTIES 2 3.1 Chemical Identification 2 3.2 Physico-Chemical Properties 3 3.3 Purity and Commercial Availability 4 4.0 PRODUCTION PROCESSES AND ANALYSIS 6 5.0 PRODUCTION AND IMPORT VOLUMES 7 6.0 USES 7 7.0 ENVIRONMENTAL OCCURRENCE 7 8.0 HUMAN EXPOSURE 7 9.0 REGULATORY STATUS 7 10.0 CLINICAL PHARMACOLOGY 7 11.0 TOXICOLOGICAL DATA 13 11.1 General Toxicology 13 11.2 Neurotoxicology 14 12.0 CONCLUSIONS 15 APPENDIX A 17 APPENDIX B 23 APPENDIX C 27 1 KETAMINE 1.0 BASIS OF NOMINATION Ketamine, a noncompetitive NMDA receptor blocker, has been used extensively off - label as a pediatric anesthetic for surgical procedures in infants and toddlers. Recently, Olney and coworkers have demonstrated severe widespread apoptotic degeneration throughout the rapidly developing brain of the 7-day-old rat after ketamine administration. Recent research at FDA has confirmed and extended Olney’s observations. These findings are cause for concern with respect to ketamine use in children. The issue of whether the neurotoxicity found in this animal model (rat) has scientific and regulatory relevance for the pediatric use of ketamine relies heavily upon confirmation of these findings that may be obtained from the conduct of an appropriate study in non-human primates. 2.0 BACKGROUND INFORMATION The issue of potential ketamine neurotoxicity in children surfaced as a result of FDA’s reluctance to approve an NIH pediatric clinical trial using this compound because of its documented neurotoxic effects in young rats (published in several papers over the last ten years by Olney and co-workers). -

The Anticholinergic Toxidrome
Poison HOTLINE Partnership between Iowa Health System and University of Iowa Hospitals and Clinics July 2011 The Anticholinergic Toxidrome A toxidrome is a group of symptoms associated with poisoning by a particular class of agents. One example is the opiate toxidrome, the triad of CNS depression, respiratory depression, and pinpoint pupils, and which usually responds to naloxone. The anticholinergic toxidrome is most frequently associated with overdoses of diphenhydramine, a very common OTC medication. However, many drugs and plants can produce the anticholinergic toxidrome. A partial list includes: tricyclic antidepressants (amitriptyline), older antihistamines (chlorpheniramine), Did you know …… phenothiazines (promethazine) and plants containing the anticholinergic alkaloids atropine, hyoscyamine and scopolamine (Jimson Weed). Each summer, the ISPCC receives approximately 10-20 The mnemonic used to help remember the symptoms and signs of this snake bite calls, some being toxidrome are derived from the Alice in Wonderland story: from poisonous snakes (both Blind as a Bat (mydriasis and inability to focus on near objects) local and exotic). Red as a Beet (flushed skin color) Four poisonous snakes can be Hot as Hades (elevated temperature) found in Iowa: the prairie These patients can sometimes die of agitation-induced hyperthermia. rattlesnake, the massasauga, Dry as a Bone (dry mouth and dry skin) the copperhead, and the Mad as a Hatter (hallucinations and delirium) timber rattlesnake. Each Bowel and bladder lose their tone (urinary retention and constipation) snake has specific territories Heart races on alone (tachycardia) within the state. ISPCC A patient who has ingested only an anticholinergic substance and is not specialists have access to tachycardic argues against a serious anticholinergic overdose. -

COMPARISON of the WHO ATC CLASSIFICATION & Ephmra/Intellus Worldwide ANATOMICAL CLASSIFICATION
COMPARISON OF THE WHO ATC CLASSIFICATION & EphMRA/Intellus Worldwide ANATOMICAL CLASSIFICATION: VERSION June 2019 2 Comparison of the WHO ATC Classification and EphMRA / Intellus Worldwide Anatomical Classification The following booklet is designed to improve the understanding of the two classification systems. The development of the two systems had previously taken place separately. EphMRA and WHO are now working together to ensure that there is a convergence of the 2 systems rather than a divergence. In order to better understand the two classification systems, we should pay attention to the way in which substances/products are classified. WHO mainly classifies substances according to the therapeutic or pharmaceutical aspects and in one class only (particular formulations or strengths can be given separate codes, e.g. clonidine in C02A as antihypertensive agent, N02C as anti-migraine product and S01E as ophthalmic product). EphMRA classifies products, mainly according to their indications and use. Therefore, it is possible to find the same compound in several classes, depending on the product, e.g., NAPROXEN tablets can be classified in M1A (antirheumatic), N2B (analgesic) and G2C if indicated for gynaecological conditions only. The purposes of classification are also different: The main purpose of the WHO classification is for international drug utilisation research and for adverse drug reaction monitoring. This classification is recommended by the WHO for use in international drug utilisation research. The EphMRA/Intellus Worldwide classification has a primary objective to satisfy the marketing needs of the pharmaceutical companies. Therefore, a direct comparison is sometimes difficult due to the different nature and purpose of the two systems. -

Guts and Butts: Treatment Options for IBS and Functional Dyspepsia
7/2/2020 Guts and Butts: Treatment Options for IBS and Functional Dyspepsia Amy McCracken, DNP, APRN 1 Learning Objectives: ● Discuss the diagnosis and management of IBS and functional dyspepsia in order to optimize treatment strategies ● Describe pharmacological and alternative treatment approaches of IBS-C, IBS-D, IBS-M, and functional dyspepsia ● Articulate patient-specific treatment options for those with IBS and functional dyspepsia as derived from case studies 2 1 7/2/2020 Irritable Bowel Syndrome (IBS)-Definition and Epidemiology ● Comprises a group of functional bowel disorders in which abdominal discomfort or pain is associated with defecation or a change in bowel habits in the absence of an organic disease. ● The prevalence of IBS in North America is estimated at approximately 10-15%. ● More common in women compared to men. ● Second highest cause of work absenteeism ● IBS accounts for approximately 25 to 50% of all referrals to gastroenterologists. ● Important to remember: This is a diagnosis of exclusion! 3 IBS-Etiology ● Stress ● Visceral hypersensitivity ● Psychosocial factors ● Common-cannot be explained ● Chronic and benign ● High association with stress in the pathophysiology and clinical presentation of IBS 4 2 7/2/2020 IBS-Signs and Symptoms ● Chronic abdominal pain-usually a cramping sensation that varies in intensity with periodic exacerbations ● The character and location of pain can vary widely and often times related to defecation ● Abdominal fullness, bloating or swelling ● Diarrhea, constipation or alternating -

3 Drugs That May Cause Delirium Or Problem Behaviors CARD 03 19 12 JUSTIFIED.Pub
Drugs that May Cause Delirium or Problem Behaviors Drugs that May Cause Delirium or Problem Behaviors This reference card lists common and especially problemac drugs that may Ancholinergics—all drugs on this side of the card. May impair cognion cause delirium or contribute to problem behaviors in people with demena. and cause psychosis. Drugs available over‐the‐counter marked with * This does not always mean the drugs should not be used, and not all such drugs are listed. If a paent develops delirium or has new problem Tricyclic Andepressants Bladder Anspasmodics behaviors, a careful review of all medicaons is recommended. Amitriptyline – Elavil Darifenacin – Enablex Be especially mindful of new medicaons. Clomipramine – Anafranil Flavoxate – Urispas Desipramine – Norpramin Anconvulsants Psychiatric Oxybutynin – Ditropan Doxepin – Sinequan Solifenacin – VESIcare All can cause delirium, e.g. All psychiatric medicaons should be Imipramine – Tofranil Tolterodine – Detrol Carbamazepine – Tegretol reviewed as possible causes, as Nortriptyline – Aventyl, Pamelor Gabapenn – Neuronn effects are unpredictable. Trospium – Sanctura Anhistamines / Allergy / Leveracetam – Keppra Notable offenders include: Insomnia / Sleep Valproic acid – Depakote Benzodiazepines e.g. Cough & Cold Medicines *Diphenhydramine – Sominex, ‐Alprazolam – Xanax *Azelasne – Astepro Pain Tylenol‐PM, others ‐Clonazepam – Klonopin *Brompheniramine – Bromax, All opiates can cause delirium if dose *Doxylamine – Unisom, Medi‐Sleep ‐Lorazepam – Avan Bromfed, Lodrane is too high or -

New Treatment Options for Chronic Constipation: Mechanisms, Efficacy and Safety
View metadata, citation and similar papers at core.ac.uk brought to you by CORE CHRONIC CONSTIPATION – CHALLENGES AND REMEDIES provided by Crossref New treatment options for chronic constipation: Mechanisms, efficacy and safety Michael Camilleri MD M Camilleri. New treatment options for chronic constipation: De nouvelles options thérapeutiques contre la Mechanisms, efficacy and safety. Can J Gastroenterol constipation chronique : leurs mécanismes, leur 2011;(Suppl B):29B-35B. efficacité et leur innocuité The present review has several objectives, the first of which is to review the pharmacology and selectivity of serotonergic agents to La présente analyse comporte plusieurs objectifs, le premier étant de contrast the older serotonergic agents (which were withdrawn because réviser la pharmacologie et la sélectivité des sérotoninergiques pour of cardiac or vascular adverse effects) with the newer generation sero- comparer les anciens sérotoninergiques (retirés du marché en raison de tonin receptor subtype 4 agonists. Second, the chloride ion secret- leurs effets cardiaques ou vasculaires) avec les agonistes de récepteurs agogues that act through the guanylate cyclase C receptor are appraised de la sérotonine de sous-type 4 de nouvelle génération. En deuxième and their pharmacology is compared with the approved medication, lieu, les sécrétagogues des ions chlorures qui agissent par le récepteur lubiprostone. Third, the efficacy and safety of the application of bile du guanylatecyclase C sont évalués, et leur pharmacologie est com- acid modulation to treat constipation are addressed. The long-term parée avec celle du lubiprostone, un médicament approuvé. En studies of surgically induced excess bile acid delivery to the colon are troisième lieu, l’efficacité et l’innocuité de l’application de la modula- reviewed to ascertain the safety of this therapeutic approach. -

Medicare Part D Excluded Drug List
MEDICARE PART D EXCLUDED DRUGS LIST 2016_updated July 2016 Reason: LIST = multiple reasons it's excluded; "not covered under Part D law" Reason: Not properly listed with FDA = CMS considers it best practice for Part D sponsors to consider the proper listing of a drug product with the FDA as a prerequisite for making a Part D drug coverage determination. The FDA is unable to provide regulatory status determinations through their regular processes if a drug product is not properly listed. Therefore, Part D sponsors should begin the drug coverage determination process by confirming that a prescription drug product national drug code (NDC) is properly listed with the FDA. Reason: DESI = Less Than Effective (LTE) drug for ALL indications Label Name Reason 1ST BASE CRE Bulk Ingredient 2-FUCCOSYLLA PAK LACTO-N Medical Food ABANEU-SL SUB Vitamin/Mineral ABLAVAR INJ 244MG/ML Diagnostic Agent ACACIA EXTRA SOL 1:20 Non-standardized allergenic ACCUCAINE INJ 1% LIST ACD FORMULA SOL A Blood Component ACD-A SOL Blood Component ACLARO PD EMU 4% Cosmetic ACREMONIUM SOL 20000PNU Non-standardized allergenic ACTCT FLEX 3 PAD 4"X4" Not properly listed with FDA ACTHREL INJ 100MCG Diagnostic Agent ACTI ANTIMIC PAD 2"X2" Not properly listed with FDA ACTI ANTIMIC PAD 4"X4" Not properly listed with FDA ACTICOAT 7 PAD 2"X2" Not properly listed with FDA ACTICOAT 7 PAD 4"X5" Not properly listed with FDA ACTICOAT ABS PAD 4"X5" Not properly listed with FDA ACTICOAT MOI PAD 2"X2" Surgical Supply/Medical ACTICOAT MOI PAD 4"X4" Surgical Supply/Medical ACTICOAT MOI PAD