Emerging Bartonellosis Christoph Dehio & Anna Sander
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Genetic Diversity of Bartonella Species in Small Mammals in the Qaidam
www.nature.com/scientificreports OPEN Genetic diversity of Bartonella species in small mammals in the Qaidam Basin, western China Huaxiang Rao1, Shoujiang Li3, Liang Lu4, Rong Wang3, Xiuping Song4, Kai Sun5, Yan Shi3, Dongmei Li4* & Juan Yu2* Investigation of the prevalence and diversity of Bartonella infections in small mammals in the Qaidam Basin, western China, could provide a scientifc basis for the control and prevention of Bartonella infections in humans. Accordingly, in this study, small mammals were captured using snap traps in Wulan County and Ge’ermu City, Qaidam Basin, China. Spleen and brain tissues were collected and cultured to isolate Bartonella strains. The suspected positive colonies were detected with polymerase chain reaction amplifcation and sequencing of gltA, ftsZ, RNA polymerase beta subunit (rpoB) and ribC genes. Among 101 small mammals, 39 were positive for Bartonella, with the infection rate of 38.61%. The infection rate in diferent tissues (spleens and brains) (χ2 = 0.112, P = 0.738) and gender (χ2 = 1.927, P = 0.165) of small mammals did not have statistical diference, but that in diferent habitats had statistical diference (χ2 = 10.361, P = 0.016). Through genetic evolution analysis, 40 Bartonella strains were identifed (two diferent Bartonella species were detected in one small mammal), including B. grahamii (30), B. jaculi (3), B. krasnovii (3) and Candidatus B. gerbillinarum (4), which showed rodent-specifc characteristics. B. grahamii was the dominant epidemic strain (accounted for 75.0%). Furthermore, phylogenetic analysis showed that B. grahamii in the Qaidam Basin, might be close to the strains isolated from Japan and China. -

Bartonella Henselae Detected in Malignant Melanoma, a Preliminary Study
pathogens Article Bartonella henselae Detected in Malignant Melanoma, a Preliminary Study Marna E. Ericson 1, Edward B. Breitschwerdt 2 , Paul Reicherter 3, Cole Maxwell 4, Ricardo G. Maggi 2, Richard G. Melvin 5 , Azar H. Maluki 4,6 , Julie M. Bradley 2, Jennifer C. Miller 7, Glenn E. Simmons, Jr. 5 , Jamie Dencklau 4, Keaton Joppru 5, Jack Peterson 4, Will Bae 4, Janet Scanlon 4 and Lynne T. Bemis 5,* 1 T Lab Inc., 910 Clopper Road, Suite 220S, Gaithersburg, MD 20878, USA; [email protected] 2 Intracellular Pathogens Research Laboratory, Comparative Medicine Institute, College of Veterinary Medicine, North Carolina State University, Raleigh, NC 27607, USA; [email protected] (E.B.B.); [email protected] (R.G.M.); [email protected] (J.M.B.) 3 Dermatology Clinic, Truman Medical Center, University of Missouri, Kansas City, MO 64108, USA; [email protected] 4 Department of Dermatology, University of Minnesota, Minneapolis, MN 55455, USA; [email protected] (C.M.); [email protected] (A.H.M.); [email protected] (J.D.); [email protected] (J.P.); [email protected] (W.B.); [email protected] (J.S.) 5 Department of Biomedical Sciences, Duluth Campus, Medical School, University of Minnesota, Duluth, MN 55812, USA; [email protected] (R.G.M.); [email protected] (G.E.S.J.); [email protected] (K.J.) 6 Department of Dermatology, College of Medicine, University of Kufa, Kufa 54003, Iraq 7 Galaxy Diagnostics Inc., Research Triangle Park, NC 27709, USA; [email protected] Citation: Ericson, M.E.; * Correspondence: [email protected]; Tel.: +1-720-560-0278; Fax: +1-218-726-7906 Breitschwerdt, E.B.; Reicherter, P.; Maxwell, C.; Maggi, R.G.; Melvin, Abstract: Bartonella bacilliformis (B. -
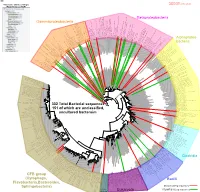
Bacteria Clostridia Bacilli Eukaryota CFB Group
AM935842.1.1361 uncultured Burkholderiales bacterium Class Betaproteobacteria AY283260.1.1552 Alcaligenes sp. PCNB−2 Class Betaproteobacteria AM934953.1.1374 uncultured Burkholderiales bacterium Class Betaproteobacteria AJ581593.1.1460 uncultured betaAM936569.1.1351 proteobacterium uncultured Class Betaproteobacteria Derxia sp. Class Betaproteobacteria AJ581621.1.1418 uncultured beta proteobacterium Class Betaproteobacteria DQ248272.1.1498 uncultured soil bacterium soil uncultured DQ248272.1.1498 DQ248235.1.1498 uncultured soil bacterium RS49 DQ248270.1.1496 uncultured soil bacterium DQ256489.1.1211 Variovorax paradoxus Class Betaproteobacteria Class paradoxus Variovorax DQ256489.1.1211 AF523053.1.1486 uncultured Comamonadaceae bacterium Class Betaproteobacteria AY706442.1.1396 uncultured bacterium uncultured AY706442.1.1396 AJ536763.1.1422 uncultured bacterium CS000359.1.1530 Variovorax paradoxus Class Betaproteobacteria Class paradoxus Variovorax CS000359.1.1530 AY168733.1.1411 uncultured bacterium AJ009470.1.1526 uncultured bacterium SJA−62 Class Betaproteobacteria Class SJA−62 bacterium uncultured AJ009470.1.1526 AY212561.1.1433 uncultured bacterium D16212.1.1457 Rhodoferax fermentans Class Betaproteobacteria Class fermentans Rhodoferax D16212.1.1457 AY957894.1.1546 uncultured bacterium AJ581620.1.1452 uncultured beta proteobacterium Class Betaproteobacteria RS76 AY625146.1.1498 uncultured bacterium RS65 DQ316832.1.1269 uncultured beta proteobacterium Class Betaproteobacteria DQ404909.1.1513 uncultured bacterium uncultured DQ404909.1.1513 AB021341.1.1466 bacterium rM6 AJ487020.1.1500 uncultured bacterium uncultured AJ487020.1.1500 RS7 RS86RC AF364862.1.1425 bacterium BA128 Class Betaproteobacteria AY957931.1.1529 uncultured bacterium uncultured AY957931.1.1529 CP000884.723807.725332 Delftia acidovorans SPH−1 Class Betaproteobacteria AY957923.1.1520 uncultured bacterium uncultured AY957923.1.1520 RS18 AY957918.1.1527 uncultured bacterium uncultured AY957918.1.1527 AY945883.1.1500 uncultured bacterium AF526940.1.1489 uncultured Ralstonia sp. -

Isolation of Francisella Tularensis from Skin Ulcer After a Tick Bite, Austria, 2020
microorganisms Case Report Isolation of Francisella tularensis from Skin Ulcer after a Tick Bite, Austria, 2020 Mateusz Markowicz 1,*, Anna-Margarita Schötta 1 , Freya Penatzer 2, Christoph Matscheko 2, Gerold Stanek 1, Hannes Stockinger 1 and Josef Riedler 2 1 Center for Pathophysiology, Infectiology and Immunology, Institute for Hygiene and Applied Immunology, Medical University of Vienna, Kinderspitalgasse 15, A-1090 Vienna, Austria; [email protected] (A.-M.S.); [email protected] (G.S.); [email protected] (H.S.) 2 Kardinal Schwarzenberg Klinikum, Kardinal Schwarzenbergplatz 1, A-5620 Schwarzach, Austria; [email protected] (F.P.); [email protected] (C.M.); [email protected] (J.R.) * Correspondence: [email protected]; Tel.: +43-1-40160-33023 Abstract: Ulceroglandular tularemia is caused by the transmission of Francisella tularensis by arthro- pods to a human host. We report a case of tick-borne tularemia in Austria which was followed by an abscess formation in a lymph node, making drainage necessary. F. tularensis subsp. holarctica was identified by PCR and multilocus sequence typing. Keywords: tularemia; Francisella tularensis; tick; multi locus sequence typing Depending on the transmission route of Francisella tularensis, tularemia can present Citation: Markowicz, M.; Schötta, as a local infection or a systemic disease [1]. Transmission of the pathogen takes place A.-M.; Penatzer, F.; Matscheko, C.; by contact with infected animals, by bites of arthropods or through contaminated water Stanek, G.; Stockinger, H.; Riedler, J. and soil. Hares and wild rabbits are the main reservoirs of the pathogen in Austria [2]. -

Bartonella Henselae
Maggi et al. Parasites & Vectors 2013, 6:101 http://www.parasitesandvectors.com/content/6/1/101 RESEARCH Open Access Bartonella henselae bacteremia in a mother and son potentially associated with tick exposure Ricardo G Maggi1,3*, Marna Ericson2, Patricia E Mascarelli1, Julie M Bradley1 and Edward B Breitschwerdt1 Abstract Background: Bartonella henselae is a zoonotic, alpha Proteobacterium, historically associated with cat scratch disease (CSD), but more recently associated with persistent bacteremia, fever of unknown origin, arthritic and neurological disorders, and bacillary angiomatosis, and peliosis hepatis in immunocompromised patients. A family from the Netherlands contacted our laboratory requesting to be included in a research study (NCSU-IRB#1960), designed to characterize Bartonella spp. bacteremia in people with extensive arthropod or animal exposure. All four family members had been exposed to tick bites in Zeeland, southwestern Netherlands. The mother and son were exhibiting symptoms including fatigue, headaches, memory loss, disorientation, peripheral neuropathic pain, striae (son only), and loss of coordination, whereas the father and daughter were healthy. Methods: Each family member was tested for serological evidence of Bartonella exposure using B. vinsonii subsp. berkhoffii genotypes I-III, B. henselae and B. koehlerae indirect fluorescent antibody assays and for bacteremia using the BAPGM enrichment blood culture platform. Results: The mother was seroreactive to multiple Bartonella spp. antigens and bacteremia was confirmed by PCR amplification of B. henselae DNA from blood, and from a BAPGM blood agar plate subculture isolate. The son was not seroreactive to any Bartonella sp. antigen, but B. henselae DNA was amplified from several blood and serum samples, from BAPGM enrichment blood culture, and from a cutaneous striae biopsy. -

Bartonella: Feline Diseases and Emerging Zoonosis
BARTONELLA: FELINE DISEASES AND EMERGING ZOONOSIS WILLIAM D. HARDY, JR., V.M.D. Director National Veterinary Laboratory, Inc. P.O Box 239 Franklin Lakes, New Jersey 07417 201-891-2992 www.natvetlab.com or .net Gingivitis Proliferative Gingivitis Conjunctivitis/Blepharitis Uveitis & Conjunctivitis URI Oral Ulcers Stomatitis Lymphadenopathy TABLE OF CONTENTS Page SUMMARY……………………………………………………………………………………... i INTRODUCTION……………………………………………………………………………… 1 MICROBIOLOGY……………………………………………………………………………... 1 METHODS OF DETECTION OF BARTONELLA INFECTION.………………………….. 1 Isolation from Blood…………………………………………………………………….. 2 Serologic Tests…………………………………………………………………………… 2 SEROLOGY……………………………………………………………………………………… 3 CATS: PREVALENCE OF BARTONELLA INFECTIONS…………………………………… 4 Geographic Risk factors for Infection……………………………………………………. 5 Risk Factors for Infection………………………………………………………………… 5 FELINE BARTONELLA DISEASES………………………………………………………….… 6 Bartonella Pathogenesis………………………………………………………………… 7 Therapy of Feline Bartonella Diseases…………………………………………………… 14 Clinical Therapy Results…………………………………………………………………. 15 DOGS: PREVALENCE OF BARTONELLA INFECTIONS…………………………………. 17 CANINE BARTONELLA DISEASES…………………………………………………………... 17 HUMAN BARTONELLA DISEASES…………………………………………………………… 18 Zoonotic Case Study……………………………………………………………………... 21 FELINE BLOOD DONORS……………………………………………………………………. 21 REFERENCES………………………………………………………………………………….. 22 This work was initiated while Dr. Hardy was: Professor of Medicine, Albert Einstein College of Medicine of Yeshiva University, Bronx, New York and Director, -

Transformation of Bartonella Bacilliformis by Electroporation
University of Montana ScholarWorks at University of Montana Graduate Student Theses, Dissertations, & Professional Papers Graduate School 1994 Transformation of Bartonella bacilliformis by electroporation Helen A. Grasseschi The University of Montana Follow this and additional works at: https://scholarworks.umt.edu/etd Let us know how access to this document benefits ou.y Recommended Citation Grasseschi, Helen A., "Transformation of Bartonella bacilliformis by electroporation" (1994). Graduate Student Theses, Dissertations, & Professional Papers. 7287. https://scholarworks.umt.edu/etd/7287 This Thesis is brought to you for free and open access by the Graduate School at ScholarWorks at University of Montana. It has been accepted for inclusion in Graduate Student Theses, Dissertations, & Professional Papers by an authorized administrator of ScholarWorks at University of Montana. For more information, please contact [email protected]. Maureen and Mike MANSFIELD LIBRARY TheMontana University of Permission is granted by the author to reproduce this material in its entirety, provided that this material is used for scholarly purposes and is properly cited in published works and reports. * * P lease check **Yes ” o r **No ” and provide signature*"^ Yes, I grant permission No, I do not grant permission /\ Author’s Signature Date: TG~ f^ Any copying for commercial purposes or financial gain may be undertaken only with the author’s explicit consent. Reproduced with permission of the copyright owner. Further reproduction prohibited without permission. Transformation of Bartonella bacilliformis by Electroporation by Helen A. Grasseschi B. S., The University of Montana— Missoula, 1992 Presented in partial fulfillment of the requirements for the degree of Master of Science in Microbiology The University of Montana 1994 Approved by Chairman, Board of Examiners Daam, Graduate School £2, / 0 9 -/ Date ' Reproduced with permission of the copyright owner. -

Bartonella Is a Stealth Pathogen: It Hides Inside Red Blood Cells and the Cells of Blood-Vessel Walls
The Major Threat You’ve Never Heard Of BY SUE M. COPELAND This “stealth” bacteria is an emerging danger to your dog - and you. It also may be linked to the common canine cancer, hemangiosarcoma. Bartonella is a stealth pathogen: it hides inside red blood cells and the cells of blood-vessel walls. Once there, it eludes the body’s immune system, and often dodges detection by standard diagnostic blood tests. above photo ©North Carolina State University tell my veterinary students that, unless another infectious others, there now are 40 named species, of which 17 have been disease comes along that we don’t yet know about, such associated with an expanding spectrum of disease in dogs and hu- “I as covid-19 did in humans, Bartonella will cause them mans, as well as other mammals. more problems in their careers than anything else.” The bacteria lives inside blood cells and is transmitted by car- That quote is from Edward Breitschwerdt, DVM, DACVIM, riers, known as vectors, which include fleas, lice, and sand flies; Melanie S. Steele Professor of Medicine and Infectious Disease Bartonella DNA has also been found in ticks. These vectors are at North Carolina State University (NCSU) College of Veterinary found on and around such animals as dogs, cats, coyotes, rac- Medicine. He’s been studying the bacteria for 30 years. coons, cows, foxes, horses, rodents, and bats. Bartonellosis is a “Wait, what?” you ask. “What the heck is Bartonella?” zoonotic disease, meaning it can be transmitted from your pets It’s an emerging threat that research is showing can be associ- or other mammals, to humans. -

Rodent-Borne Bartonella Infection Varies According to Host Species Within and Among Cities
EcoHealth 14, 771–782, 2017 DOI: 10.1007/s10393-017-1291-4 Ó 2017 EcoHealth Alliance Original Contribution Rodent-Borne Bartonella Infection Varies According to Host Species Within and Among Cities Anna C. Peterson,1 Bruno M. Ghersi,1 Fernando Alda,2 Cadhla Firth,3 Matthew J. Frye,4 Ying Bai,5 Lynn M. Osikowicz,5 Claudia Riegel,6 W. Ian Lipkin,7 Michael Y. Kosoy,5 and Michael J. Blum1,8 1Department of Ecology and Evolutionary Biology, Tulane University, New Orleans, LA 2Museum of Natural Science, Louisiana State University, Baton Rouge, LA 3School of BioSciences, The University of Melbourne, Parkville, VIC, Australia 4New York State IPM Program, Cornell University, Geneva, NY 5Division of Vector-Borne Diseases, Centers for Disease Control and Prevention, Fort Collins, CO 6City of New Orleans Mosquito, Termite and Rodent Control Board, New Orleans, LA 7Center for Infection and Immunity, Mailman School of Public Health, Columbia University, New York, NY 8Bywater Institute, Tulane University, New Orleans, LA Abstract: It is becoming increasingly likely that rodents will drive future disease epidemics with the continued expansion of cities worldwide. Though transmission risk is a growing concern, relatively little is known about pathogens carried by urban rats. Here, we assess whether the diversity and prevalence of Bartonella bacteria differ according to the (co)occurrence of rat hosts across New Orleans, LA (NO), where both Norway (Rattus norvegicus) and roof rats (Rattus rattus) are found, relative to New York City (NYC) which only harbors Norway rats. We detected human pathogenic Bartonella species in both NYC and New Orleans rodents. We found that Norway rats in New Orleans harbored a more diverse assemblage of Bartonella than Norway rats in NYC and that Norway rats harbored a more diverse and distinct assemblage of Bartonella compared to roof rats in New Orleans. -

Bartonellosis Ed Breitschwerdt, DVM (Ed [email protected]) Tests Available at VBDDL: Serology (IFA) and PCR on Blood Or CSF
Bartonellosis Ed Breitschwerdt, DVM ([email protected]) Tests available at VBDDL: Serology (IFA) and PCR on blood or CSF There are a growing number of Bartonella species associated with disease manifestations in cats, dogs, humans and other less domesticated host species including Bartonella henselae, B. vinsonii subspecies berkhoffii, B.rochalimae, B.clarridgeiae, and B. koehlerae. Genetically unique strains or genotypes are being described within each species. This may affect test interpretation because most laboratories only test for a limited selection of species and serological cross reactivity is not always present. Knowledge of which species are tested for is important for both antibody and DNA testing. Risk factors: o History of flea, tick, biting fly, keds, lice, or sandfly exposure Disease: o Transient lethargy o Fever o Lymphadenopathy o Gingivitis o Stomatitis o Uveitis o Neurologic dysfunction o Endocarditis o Retinal disease Bartonella henselae – B.henselae is a flea-transmitted zoonotic pathogen with the cat identified as a major reservoir for human infection. Fever and bacteremia, endocarditis, lymphadenopathy (cat scratch disease in people), bacillary angiomatosis, neurologic dysfunction and retinal disease can be caused by B. henselae, particularly in immunocompromised individuals. Following flea transmission or blood transfusion to cats, B. henselae causes a relapsing pattern of bacteremia, persisting for months to years. Bartonella koehlerae – B.koehlerae is a zoonotic bacterium that has but rarely been reported as an infectious cause of disease in dogs or human patients. Cats are considered the primary reservoir host for B. koehlerae as with B. henselae. Ctenocephalides felis, the cat flea, is considered a transmission competent vector for both organisms. -

Human Bartonellosis: an Underappreciated Public Health Problem?
Tropical Medicine and Infectious Disease Review Human Bartonellosis: An Underappreciated Public Health Problem? Mercedes A. Cheslock and Monica E. Embers * Division of Immunology, Tulane National Primate Research Center, Tulane University Health Sciences, Covington, LA 70433, USA; [email protected] * Correspondence: [email protected]; Tel.: +(985)-871-6607 Received: 24 March 2019; Accepted: 16 April 2019; Published: 19 April 2019 Abstract: Bartonella spp. bacteria can be found around the globe and are the causative agents of multiple human diseases. The most well-known infection is called cat-scratch disease, which causes mild lymphadenopathy and fever. As our knowledge of these bacteria grows, new presentations of the disease have been recognized, with serious manifestations. Not only has more severe disease been associated with these bacteria but also Bartonella species have been discovered in a wide range of mammals, and the pathogens’ DNA can be found in multiple vectors. This review will focus on some common mammalian reservoirs as well as the suspected vectors in relation to the disease transmission and prevalence. Understanding the complex interactions between these bacteria, their vectors, and their reservoirs, as well as the breadth of infection by Bartonella around the world will help to assess the impact of Bartonellosis on public health. Keywords: Bartonella; vector; bartonellosis; ticks; fleas; domestic animals; human 1. Introduction Several Bartonella spp. have been linked to emerging and reemerging human diseases (Table1)[ 1–5]. These fastidious, gram-negative bacteria cause the clinically complex disease known as Bartonellosis. Historically, the most common causative agents for human disease have been Bartonella bacilliformis, Bartonella quintana, and Bartonella henselae. -

Case Report Long-Lasting Fever and Lymphadenitis: Think About F. Tularensis
Hindawi Publishing Corporation Case Reports in Medicine Volume 2015, Article ID 191406, 4 pages http://dx.doi.org/10.1155/2015/191406 Case Report Long-Lasting Fever and Lymphadenitis: Think about F. tularensis Maria Vittoria Longo,1,2 Katia Jaton,3 Paola Pilo,4 David Chabanel,2 and Véronique Erard5 1 Department of Internal Medecine, Hopitalˆ du Jura, 2800 Delemont,´ Switzerland 2Department of Internal Medecine, Hopitalˆ de la Broye, 1530 Payerne, Switzerland 3Institute of Microbiology, University of Lausanne and University Hospital Center, 1011 Lausanne, Switzerland 4Institute of Veterinary Bacteriology, Vetsuisse Faculty, University of Bern, 3012 Bern, Switzerland 5Unit of Infectious Diseases, Department of Internal Medicine, HFR-Hopitalˆ cantonal, 1708 Fribourg, Switzerland Correspondence should be addressed to Maria Vittoria Longo; [email protected] Received 10 August 2015; Accepted 30 September 2015 Academic Editor: Stephen A. Klotz Copyright © 2015 Maria Vittoria Longo et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. We report the case of glandular tularemia that developed in a man supposedly infected by a tick bite in Western Switzerland. Francisella tularensis (F. tularensis) was identified. In Europe tularemia most commonly manifests itself as ulcero-glandular or glandular disease; the diagnosis of tularemia may be delayed in glandular form where skin or mucous lesion is absent, particularly in areas which are assumed to have a low incidence of the disease. 1. Clinical History disease in serum and CSF, and molecular tests for Herpes simplex virus (HSV), Varicella-zoster virus (VZV), Listeria A 75-year-old man, living in a rural area of Western Switzer- monocytogenes, and Bartonella henselae (B.