A Balance Point Approach to Modeling Hemodynamics In
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Determination of Cardiac Output by Equating Venous Return Curves with Cardiac Response Curves
Determination of Cardiac Output By Equating Ve- nous Return Curves With Cardiac Response Curves1 ARTHUR C. GUYTQN From the Department of Physiology and Biophysics, School of Medicine, University of Mississippi, University, Mississippi HE CONCEPT that the heart responds with increasing cardiac output when there occurs increasing venous return was popularized by Starling and, in- deed, has come to be known as Starling’s law. There are many different forms in which Starling’s law can be expressed,including the relationship of cardiac output to right atria1 pressure, the relationship of cardiac output to the degree of distention of the right ventricle at the end of diastole, the relationship of cardiac work to right atria1 pressure or right ventricular distention, the relationship of left ventricular work to right atria1 pressure or right ventricular distention, etc. For the determina- tion of cardiac output, the form of Starling’s law which will be used in the present discussion is the relationship of cardiac output to mean right atria1 pressure, and this type of cruve will be called the “cardiac responsecurve” to right atria1 pressure. It is well known that many factors in the peripheral circulatory system combine together to determine the rate of venous return to the heart. These include the quantity of blood available, the degree of vascular resistance in various parts of the peripheral circulatory system, and the back pressure from the right atrium. It is with these factors that this paper is especially concerned, and it is hoped that this presentation will demonstrate how cardiac output is determined by equating the peripheral circulatory factors with the cardiac responsecurves. -
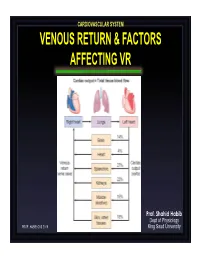
Venous Return & Factors Affecting Vr
CARDIOVASCULAR SYSTEM VENOUS RETURN & FACTORS AFFECTING VR Prof. Shahid Habib Dept of Physiology PROF. HABIB CVS 2019 King Saud University OBJECTIVES At the end of the lecture you should be able to ….. Discuss functions of the veins as blood reservoirs. Describe measurement of central venous pressure (CVP) and state its physiological and clinical significance. State determinants of venous return and explain how they influence venous return. Define mean systemic filling pressure, give its normal value and describe the factors which affect it. Explain the effect of gravity on venous pressure and explain pathophysiology of varicose veins. Describe vascular and cardiac function curves under physiological and pathophysiological conditions. DISTRIBUTION OF BLOOD Capacitance Vessels Veins are blood reservoirs When the body is at rest and many of the capillaries are closed, the capacity of the venous reservoir is increased as extra blood bypasses the capillaries and enters the veins. When this extra volume of blood stretches the veins, the blood moves forward through the veins more slowly because the total cross sectional area of the veins has increased as a result of the stretching. Therefore, blood spends more time in the veins. When the stored blood is needed, such as during exercise, extrinsic factors reduce the capacity of the venous reservoir and drive the extra blood from the veins to the heart so that it can be pumped to the tissues. Rt. Lt. At At Right Left ven ven Large veins Large arteries CAPACITANCE VESSELS EXCHANGE VESSELS RESISTANCE VESSELS Venules Capillaries Arterioles Vascular circuit • all 3 layers are present, but thinner than in •In varicose veins, arteries of corresponding size (external blood pools because diameter). -

Cardiac Output Venous Return
Circulatory Physiology As a Country Doc Episode 3 Cardiac Output and Venous Return Patrick Eggena, M.D. Novateur Medmedia, LLC. Circulatory Physiology As a Country Doc Episode 3 Cardiac Output and Venous Return Patrick Eggena, M.D. Novateur Medmedia, LLC. i Copyright This Episode is derived from: Course in Cardiovascular Physiology by Patrick Eggena, M.D. © Copyright Novateur Medmedia, LLC. April 13, 2012 The United States Copyright Registration Number: PAu3-662-048 Ordering Information via iBooks: ISBN 978-0-9663441-2-7 Circulatory Physiology as a Country Doc, Episode 3: Cardiac Output and Venous Return Contact Information: Novateur Medmedia, LLC 39 Terry Hill Road, Carmel, NY 10512 email: [email protected] Credits: Oil Paintings by Bonnie Eggena, PsD. Music by Alan Goodman from his CD Under the Bed, Cancoll Music, copyright 2005 (with permission). Illustrations, movies, text, and lectures by Patrick Eggena, M.D. Note: Knowledge in the basic and clinical sciences is constantly changing. The reader is advised to carefully consult the instruc- tions and informational material included in the package inserts of each drug or therapeutic agent before administration. The Country Doctor Series illustrates Physiological Principles and is not intended as a guide to Medical Therapeutics. Care has been taken to present correct information in this book, however, the author and publisher are not responsible for errors or omissions or for any consequence from application of the information in this work and make no warranty, expressed or implied, with re- spect to the contents of this publication or that its operation will be uninterrupted and error free on any particular recording de- vice. -

Guyton's Venous Return Curves Should Be Taught at Medical Schools
J Physiol Sci (2017) 67:447–458 DOI 10.1007/s12576-017-0533-0 REVIEW Guyton’s venous return curves should be taught at medical schools (complete English translation of Japanese version) Kenji Sunagawa1 Received: 9 February 2017 / Accepted: 6 March 2017 / Published online: 27 March 2017 Ó The Physiological Society of Japan and Springer Japan 2017 Abstract Guyton’s most significant contributions are the around 2000, sparking a flurry of debates in scientific exploration into the development of venous return and journals. This article introduces the most important points circulatory equilibrium. Recently, several physiologists of argument among the various controversies, and explains challenged the validity of venous return as a function of the views of the authors. Based on this background, the venous pressure. Guyton’s experiment in effect controlled latest development of Guyton’s physiology will be com- venous pressure by changing cardiac output. Thus, critics mented. Some terms that appear frequently in this article claimed that cardiac output is the determinant of venous may be unfamiliar to some readers. For the benefit of those return. This claim is true, but in the presence of constant readers, Memos are added to explain these terms in simple stressed volume, venous return and venous pressure have a language. For those readers who already know the defini- fixed reciprocal relationship. Thus, it is meaningless to tions of these terms, they may skip these Memos and argue which one is the independent variable. We fully continue to read on. Moreover, many equations are used to support Guyton’s venous return and in particular circula- explain how the basic concept proposed in Guyton’s tory equilibrium. -

The Use of Central Venous Pressure in Critically Ill Patients
The Use of Central Venous Pressure in Critically Ill Patients S. Magder Introduction The assessment of the central venous pressure (CVP) is one of the basic elements of a standard physical exam. This is done at the bedside by measuring the vertical height of the distension of the jugular veins above the sternal angle, which is where the second rib meets the sternum. The sternal angle is used because it is fortui- tously approximately 5 cm above the mid-point of the right atrium whether the patient is lying down or whether the patient is sitting upright at a 60° angle. This works because the right atrium is a relatively anterior structure and sits just below the sternal angle. Differences in heart size only add a small difference to the measurement, and this standard reference point allows comparisons over time and by different operators. The midpoint of the right atrium is used as the stand- ard reference point because it represents the lowest pressure for the blood return- ing to the heart, and the starting point from which the heart raises the pressure. The value is in cmH2O, which can be converted to mmHg by dividing the value in centimeters by 1.36, which accounts for the density of mercury and the conversion from cmH2O to mmHg. A major reason given for assessing the CVP is that it gives an indication of a person’s volume status, but before the usefulness of this meas- ure can be assessed, it is important to appreciate the factors that determine CVP and right atrial pressure [1]. -

NROSCI/BIOSC 1070 and MSNBIO 2070 September 18 & 20, 2017
NROSCI/BIOSC 1070 and MSNBIO 2070 September 18 & 20, 2017 Cardiovascular 3 & 4: Mechanical Actions of the Heart and Determinants of Cardiac Output An essential component for the operation of the heart is the action of the valves. The valves insure that blood moves in only one direction. The opening and closing of the heart valves is controlled simply by the pressure gradients on the two sides of the valves. The two arteriovenous (AV) valves, the tricuspid and mitral valves, are comprised of flaps of connective tissue. On the ventricular side, the valves are attached to collagen cords called the cordae tendinae. The opposite ends of the cords are attached to the moundlike extensions of ventricular muscle called papillary muscles. The cordae tendinae prevent the flaps of the valve from getting stuck against the ventricular wall during ventricular filling and from being forced into the atria during ventricular systole. In contrast, the aortic and pulmonary semilunar valves have three cuplike leaflets that fill with blood, and which snap closed when backward pressure is placed on them. Special tethering such as the chordae tendinae are not required to insure that the semilunar valves close properly. The closing of the heart valves generates vibrations, which result in the heart sounds that physicians often monitor during examinations. The major heart sounds are commonly referred to as “lub-dub”. The softer “lub” is associated with closing of the tricuspid and mitral valves, and the “dub” comes from the closing of the semilunar valves. Careful assessment of the heart sounds can be done using a stethoscope; the procedure is referred to a auscultation. -

Lecture 7-8 Cardiac Output & Venous Return
Lecture 7-8 Cardiac output & Venous Return •Red: important •Black: in male / female slides •Pink: in female slides only •Blue: in male slides only Physiology •Gray: extra information MED438 Editing file Objectives: ● Define Cardiac Output and its normal values. ● Define stroke volume, End- systolic volume, and end- diastolic volume. ● Identify factors affecting and determining Cardiac Output. ● Role of stroke volume and heart rate regulation on Cardiac Output regulation. ● Understand the role of venous return on Cardiac Output. ● Understand factors affecting the EDV (venous return) and the end- systolic volume (ESV). Definitions 01 End-Diastolic Volume (EDV): 02 Stroke Volume (SV): Volume of blood in the ventricles at the end Amount of blood pumped/ejected from of diastole (before ejection). ventricles (out of ventricles) per beat. ● Volume = 110-130 ml ● Volume = 70 - 80 ml/beat ● EDV - ESV = SV 03 End-Systolic Volume (ESV): Ejection fraction (EF):1 04 Amount of blood left/remained in ventricles The percentage (Fraction) of ventricular at the end of systole (after ejection). EDV which is ejected with each stroke ● Volume = 40-60 ml (beat), it’s around 60-65%. ● Increase in SV → decrease ESV ● It’s a good index of ventricular function. ● EF = SV (EDV-ESV) / EDV X 100 1. Ejection fraction is important in emergencies, for example, when a patient is having an operation, the value must be checked before starting the operation, if the value is (60-65%) then he’s fit for the operation, if not (e.g. 50%) then the doctor will make sure the operation is done under general anesthesia ONLY, because anesthesia decrease contractility therefore decrease the ejection fraction. -

Overview of the Circulation; Biophysics of Pressure, Flow, and Resistance
CHAPTER 14 UNIT Overview of the Circulation; Biophysics I V of Pressure, Flow, and Resistance The function of the circula- is released into the capillaries. Arterioles have strong tion is to service the needs of muscular walls that can close the arterioles completely or the body tissues—to trans- can, by relaxing, dilate the vessels severalfold, thus having port nutrients to the body the capability of vastly altering blood flow in each tissue tissues, to transport waste in response to its needs. products away, to transport The function of the capillaries is to exchange fluid, hormones from one part of nutrients, electrolytes, hormones, and other substances the body to another, and, in general, to maintain an appro- between the blood and the interstitial fluid. To serve this priate environment in all the tissue fluids of the body for role, the capillary walls are very thin and have numer- optimal survival and function of the cells. ous minute capillary pores permeable to water and other The rate of blood flow through many tissues is con- small molecular substances. trolled mainly in response to tissue need for nutrients. In The venules collect blood from the capillaries and some organs, such as the kidneys, the circulation serves gradually coalesce into progressively larger veins. additional functions. Blood flow to the kidney, for exam- The veins function as conduits for transport of blood ple, is far in excess of its metabolic requirements and is from the venules back to the heart; equally important, related to its excretory function, which demands that a they serve as a major reservoir of extra blood. -

Physiology of Venous Return?
Concise Definitive Review Series Editor, Jonathan E. Sevransky, MD, MHS Deepa & Naresh CCM The Role of Venous Return in Critical Illness and CCM Shock—Part I: Physiology Critical Care Medicine Duane J. Funk, MD1,2; Eric Jacobsohn, MD1,2; Anand Kumar, MD1,3 Crit Care Med Objective: To provide a conceptual and clinical review of the phys- stressed conditions. The first part describes the basic physiology of Lippincott Williams & Wilkins iology of the venous system as it is relates to cardiac function in the venous system, and part two focuses on the role of the venous health and disease. system in different pathophysiologic states, particularly shock. Hagerstown, MD Data: An integration of venous and cardiac physiology under nor- Conclusion: An improved understanding of the role of the venous mal conditions, critical illness, and resuscitation. system in health and disease will allow intensivists to better ap- Summary: The usual teaching of cardiac physiology focuses on left preciate the complex circulatory physiology of shock and may al- 10.1097/CCM.0b013e3182772ab6 ventricular function. As a result of the wide array of shock states low for better hemodynamic management of this disorder. (Crit with which intensivists contend, an approach that takes into account Care Med 2013; 41:255–262) 204217 the function of the venous system and its interaction with the right Key Words: cardiogenic shock; cardiovascular physiology; and left heart may be more useful. This two-part review focuses on hemodynamics; hemorrhagic shock; obstructive shock; septic the function of the venous system and right heart under normal and shock n the modern era, the typical hemodynamic analysis of This two-part review discusses the role of the heart and cardiovascular function focuses on left ventricular (LV) venous system in regulating venous return (VR) and cardiac Iphysiology. -

Problem Solving Exercises in Cardiovascular Physiology and Pathophysiology
Prakash ES. Problem Solving Exercises in Cardiovascular Physiology & Pathophysiology. Revised July 2014 Problem Solving Exercises in Cardiovascular Physiology and Pathophysiology Elapulli S. Prakash, MBBS, MD Division of Basic Medical Sciences, Mercer University School of Medicine Macon, GA, USA E-mail: [email protected] 1 Prakash ES. Problem Solving Exercises in Cardiovascular Physiology & Pathophysiology. Revised July 2014 Some notes on terminology: Unless otherwise specified, the term BP refers to systemic arterial blood pressure obtained in the brachial artery held at the level of the heart, and mean arterial pressure refers to mean systemic arterial pressure. stroke volume, end-diastolic volume, end-diastolic pressure, and ejection fraction, refer to parameters of the left ventricle. systolic pressure, diastolic pressure, pulse pressure, mean arterial pressure all refer to pressures in the systemic arteries. Any other usage of these terms should be with appropriate qualifications; example, pulse pressure in pulmonary artery. 2 Prakash ES. Problem Solving Exercises in Cardiovascular Physiology & Pathophysiology. Revised July 2014 Questions and Answers: 1. Does constriction of arterioles in finger flexors increase mean arterial pressure (MAP)? It may or it may not. Vasoconstriction in a tissue (i.e., an increase in Local Vascular Resistance, LVR) does not necessarily increase total peripheral resistance (TPR; aka. systemic vascular resistance (SVR). MAP is the product of SVR and cardiac output, and one cannot predict with certainty if a change in LVR in one tissue will TPR and or cardiac output. Vasoconstriction in certain tissues (example, coronary circulation), may elicits a reflex increase in sympathetic discharge. This may result in an increase in TPR. Myocardial ischemia, CNS ischemia, ischemia of metabolically active skeletal muscle, renal ischemia, are all known to elicit reflex increases in sympathetic discharge to resistance vessels that may result in a rise in MAP. -

Guyton Physiology : Guyton and Hall Textbook of Medical Physiology
CHAPTER 16 UNIT The Microcirculation and Lymphatic System: Capillary Fluid Exchange, Interstitial I V Fluid, and Lymph Flow The most purposeful func- the capillary. This is called the precapillary sphincter. This tion of the circulation occurs sphincter can open and close the entrance to the capillary. in the microcirculation: This The venules are larger than the arterioles and have a is transport of nutrients to much weaker muscular coat. Yet the pressure in the venules the tissues and removal of is much less than that in the arterioles, so the venules can cell excreta. The small arte- still contract considerably despite the weak muscle. rioles control blood flow to This typical arrangement of the capillary bed is not each tissue, and local conditions in the tissues in turn con- found in all parts of the body, although a similar arrange- trol the diameters of the arterioles. Thus, each tissue, in ment may serve the same purposes. Most important, the most instances, controls its own blood flow in relation to its metarterioles and the precapillary sphincters are in close individual needs, a subject that is discussed in Chapter 17. contact with the tissues they serve. Therefore, the local The walls of the capillaries are extremely thin, con- conditions of the tissues—the concentrations of nutri- structed of single-layer, highly permeable endothelial ents, end products of metabolism, hydrogen ions, and so cells. Therefore, water, cell nutrients, and cell excreta can forth—can cause direct effects on the vessels to control all interchange quickly and easily between the tissues and local blood flow in each small tissue area. -

Volume and Its Relationship to Cardiac Output and Venous Return S
Magder Critical Care (2016) 20:271 DOI 10.1186/s13054-016-1438-7 REVIEW Open Access Volume and its relationship to cardiac output and venous return S. Magder Abstract Volume infusions are one of the commonest clinical interventions in critically ill patients yet the relationship of volume to cardiac output is not well understood. Blood volume has a stressed and unstressed component but only the stressed component determines flow. It is usually about 30 % of total volume. Stressed volume is relatively constant under steady state conditions. It creates an elastic recoil pressure that is an important factor in the generation of blood flow. The heart creates circulatory flow by lowering the right atrial pressure and allowing the recoil pressure in veins and venules to drain blood back to the heart. The heart then puts the volume back into the systemic circulation so that stroke return equals stroke volume. The heart cannot pump out more volume than comes back. Changes in cardiac output without changes in stressed volume occur because of changes in arterial and venous resistances which redistribute blood volume and change pressure gradients throughout the vasculature. Stressed volume also can be increased by decreasing vascular capacitance, which means recruiting unstressed volume into stressed volume. This is the equivalent of an auto-transfusion. It is worth noting that during exercise in normal young males, cardiac output can increase five-fold with only small changes in stressed blood volume. The mechanical characteristics of the cardiac chambers and the circulation thus ultimately determine the relationship between volume and cardiac output and are the subject of this review.