Pathology of Acral Nevi and Melanomas
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Acral Compound Nevus SJ Yun S Korea
University of Pennsylvania, Founded by Ben Franklin in 1740 Disclosures Consultant for Myriad Genetics and for SciBase (might try to sell you a book, as well) Multidimensional Pathway Classification of Melanocytic Tumors WHO 4th Edition, 2018 Epidemiologic, Clinical, Histologic and Genomic Aspects of Melanoma David E. Elder, MB ChB, FRCPA University of Pennsylvania, Philadelphia, PA, USA Napa, May, 2018 3rd Edition, 2006 Malignant Melanoma • A malignant tumor of melanocytes • Not all melanomas are the same – variation in: – Epidemiology – risk factors, populations – Cell/Site of origin – Precursors – Clinical morphology – Microscopic morphology – Simulants – Genomic abnormalities Incidence of Melanoma D.M. Parkin et al. CSD/Site-Related Classification • Bastian’s CSD/Site-Related Classification (Taxonomy) of Melanoma – “The guiding principles for distinguishing taxa are genetic alterations that arise early during progression; clinical or histologic features of the primary tumor; characteristics of the host, such as age of onset, ethnicity, and skin type; and the role of environmental factors such as UV radiation.” Bastian 2015 Epithelium associated Site High UV Low UV Glabrous Mucosa Benign Acquired Spitz nevus nevus Atypical Dysplastic Spitz Borderline nevus tumor High Desmopl. Low-CSD Spitzoid Acral Mucosal Malignant CSD melanoma melanoma melanoma melanoma melanoma 105 Point mutations 103 Structural Rearrangements 2018 WHO Classification of Melanoma • Integrates Epidemiologic, Genomic, Clinical and Histopathologic Features • Assists -
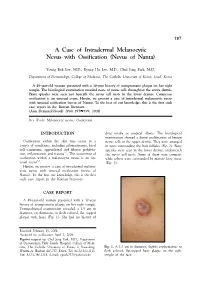
A Case of Intradermal Melanocytic Nevus with Ossification (Nevus of Nanta)
197 A Case of Intradermal Melanocytic Nevus with Ossification (Nevus of Nanta) Young Bok Lee, M.D., Kyung Ho Lee, M.D., Chul Jong Park, M.D. Department of Dermatology, College of Medicine, The Catholic University of Korea, Seoul, Korea A 49-year-old woman presented with a 30-year history of asymptomatic plaque on her right temple. The histological examination revealed nests of nevus cells throughout the entire dermis. Bony spicules were seen just beneath the nevus cell nests in the lower dermis. Cutaneous ossification is an unusual event. Herein, we present a case of intradermal melanocytic nevus with unusual ossification (nevus of Nanta). To the best of our knowledge, this is the first such case report in the Korean literature. (Ann Dermatol (Seoul) 20(4) 197∼199, 2008) Key Words: Melanocytic nevus, Ossification INTRODUCTION drug intake or medical illness. The histological examination showed a dense proliferation of benign Ossification within the skin may occur in a nevus cells in the upper dermis. They were arranged variety of conditions, including pilomatricoma, basal in nests surrounding the hair follicles (Fig. 2). Bony cell carcinoma, appendageal and fibrous prolifera- spicules were seen in the lower dermis, underneath 1,2 tion, inflammation and trauma . The occurrence of the nevus cell nests. Some of them were compact ossification within a melanocytic nevus is an un- while others were surrounded by mature fatty tissue 3-5 usual event . (Fig. 3). Herein, we present a case of intradermal melano- cytic nevus with unusual ossification (nevus of Nanta). To the best our knowledge, this is the first such case report in the Korean literature. -

Short Course 11 Pigmented Lesions of the Skin
Rev Esp Patol 1999; Vol. 32, N~ 3: 447-453 © Prous Science, SA. © Sociedad Espafiola de Anatomfa Patol6gica Short Course 11 © Sociedad Espafiola de Citologia Pigmented lesions of the skin Chairperson F Contreras Spain Ca-chairpersons S McNutt USA and P McKee, USA. Problematic melanocytic nevi melanin pigment is often evident. Frequently, however, the lesion is solely intradermal when it may be confused with a fibrohistiocytic RH. McKee and F.R.C. Path tumor, particularly epithelloid cell fibrous histiocytoma (4). It is typi- cally composed of epitheliold nevus cells with abundant eosinophilic Brigham and Women’s Hospital, Harvard Medical School, Boston, cytoplasm and large, round, to oval vesicular nuclei containing pro- USA. minent eosinophilic nucleoli. Intranuclear cytoplasmic pseudoinclu- sions are common and mitotic figures are occasionally present. The nevus cells which are embedded in a dense, sclerotic connective tis- Whether the diagnosis of any particular nevus is problematic or not sue stroma, usually show maturation with depth. Less frequently the nevus is composed solely of spindle cells which may result in confu- depends upon a variety of factors, including the experience and enthusiasm of the pathologist, the nature of the specimen (shave vs. sion with atrophic fibrous histiocytoma. Desmoplastic nevus can be distinguished from epithelloid fibrous histiocytoma by its paucicellu- punch vs. excisional), the quality of the sections (and their staining), larity, absence of even a focal storiform growth pattern and SiQO pro- the hour of the day or day of the week in addition to the problems relating to the ever-increasing range of histological variants that we tein/HMB 45 expression. -

Oral Pathology
Oral Pathology Palatal blue nevus in a child Catherine M. Flaitz DDS, MS Georgeanne McCandless DDS Dr. Flaitz is professor, Oral and Maxillofacial Pathology and Pediatric Dentistry, Department of Stomatology, University of Texas at Houston Health Science Center Dental Branch; Dr. McCandless has a private practice in The Woodlands, TX. Correspond with Dr. Flaitz at [email protected] Abstract The intraoral blue nevus occurs infrequently in children. This by the labial mucosa (1). Intraoral lesions have a predilection case report describes the clinical features of an acquired blue ne- for females in the third and fourth decades, in contrast to cu- vus in a 7 year-old girl that involved the palatal mucosa. A taneous lesions that normally develop in children. In large differential diagnosis and justification for surgical excision of this biopsy series, only 2% of the oral blue nevi are diagnosed in oral lesion are discussed. (Pediatr Dent 23:354-355, 2001) children and adolescents (1). Similar to their cutaneous coun- terpart, most oral lesions are acquired; however, there are ith the exception of vascular entities, neoplastic isolated reports of congenital examples. lesions with a blue discoloration are an unusual find Clinically, most lesions present as a solitary blue, gray or Wing in children. Although the blue nevus is a blue-black macule or slightly raised nodule that measures less relatively common finding of the skin in the pediatric popula- than 6 mm in size. The margins are often regular but indis- tion, only a few intraoral examples are documented in the tinct and the surface is smooth. -

Optimal Management of Common Acquired Melanocytic Nevi (Moles): Current Perspectives
Clinical, Cosmetic and Investigational Dermatology Dovepress open access to scientific and medical research Open Access Full Text Article REVIEW Optimal management of common acquired melanocytic nevi (moles): current perspectives Kabir Sardana Abstract: Although common acquired melanocytic nevi are largely benign, they are probably Payal Chakravarty one of the most common indications for cosmetic surgery encountered by dermatologists. With Khushbu Goel recent advances, noninvasive tools can largely determine the potential for malignancy, although they cannot supplant histology. Although surgical shave excision with its myriad modifications Department of Dermatology and STD, Maulana Azad Medical College and has been in vogue for decades, the lack of an adequate histological sample, the largely blind Lok Nayak Hospital, New Delhi, Delhi, nature of the procedure, and the possibility of recurrence are persisting issues. Pigment-specific India lasers were initially used in the Q-switched mode, which was based on the thermal relaxation time of the melanocyte (size 7 µm; 1 µsec), which is not the primary target in melanocytic nevus. The cluster of nevus cells (100 µm) probably lends itself to treatment with a millisecond laser rather than a nanosecond laser. Thus, normal mode pigment-specific lasers and pulsed ablative lasers (CO2/erbium [Er]:yttrium aluminum garnet [YAG]) are more suited to treat acquired melanocytic nevi. The complexities of treating this disorder can be overcome by following a structured approach by using lasers that achieve the appropriate depth to treat the three subtypes of nevi: junctional, compound, and dermal. Thus, junctional nevi respond to Q-switched/normal mode pigment lasers, where for the compound and dermal nevi, pulsed ablative laser (CO2/ Er:YAG) may be needed. -

Identification of HRAS Mutations and Absence of GNAQ Or GNA11
Modern Pathology (2013) 26, 1320–1328 1320 & 2013 USCAP, Inc All rights reserved 0893-3952/13 $32.00 Identification of HRAS mutations and absence of GNAQ or GNA11 mutations in deep penetrating nevi Ryan P Bender1, Matthew J McGinniss2, Paula Esmay1, Elsa F Velazquez3,4 and Julie DR Reimann3,4 1Caris Life Sciences, Phoenix, AZ, USA; 2Genoptix Medical Laboratory, Carlsbad, CA, USA; 3Dermatopathology Division, Miraca Life Sciences Research Institute, Newton, MA, USA and 4Department of Dermatology, Tufts Medical Center, Boston, MA, USA HRAS is mutated in B15% of Spitz nevi, and GNAQ or GNA11 is mutated in blue nevi (46–83% and B7% respectively). Epithelioid blue nevi and deep penetrating nevi show features of both blue nevi (intradermal location, pigmentation) and Spitz nevi (epithelioid morphology). Epithelioid blue nevi and deep penetrating nevi can also show overlapping features with melanoma, posing a diagnostic challenge. Although epithelioid blue nevi are considered blue nevic variants, no GNAQ or GNA11 mutations have been reported. Classification of deep penetrating nevi as blue nevic variants has also been proposed, however, no GNAQ or GNA11 mutations have been reported and none have been tested for HRAS mutations. To better characterize these tumors, we performed mutational analysis for GNAQ, GNA11, and HRAS, with blue nevi and Spitz nevi as controls. Within deep penetrating nevi, none demonstrated GNAQ or GNA11 mutations (0/38). However, 6% revealed HRAS mutation (2/32). Twenty percent of epithelioid blue nevi contained a GNAQ mutation (2/10), while none displayed GNA11 or HRAS mutation. Eighty-seven percent of blue nevi contained a GNAQ mutation (26/30), 4% a GNA11 mutation (1/28), and none an HRAS mutation. -

Acral Melanoma
Accepted Date : 07-Jul-2015 Article type : Original Article The BRAAFF checklist: a new dermoscopic algorithm for diagnosing acral melanoma Running head: Dermoscopy of acral melanoma Word count: 3138, Tables: 6, Figures: 6 A. Lallas,1 A. Kyrgidis,1 H. Koga,2 E. Moscarella,1 P. Tschandl,3 Z. Apalla,4 A. Di Stefani,5 D. Ioannides,2 H. Kittler,4 K. Kobayashi,6,7 E. Lazaridou,2 C. Longo,1 A. Phan,8 T. Saida,3 M. Tanaka,6 L. Thomas,8 I. Zalaudek,9 G. Argenziano.10 Article 1. Skin Cancer Unit, Arcispedale Santa Maria Nuova IRCCS, Reggio Emilia, Italy 2. Department of Dermatology, Shinshu University School of Medicine, Matsumoto, Japan 3. Department of Dermatology, Division of General Dermatology, Medical University, Vienna, Austria 4. First Department of Dermatology, Medical School, Aristotle University, Thessaloniki, Greece 5. Division of Dermatology, Complesso Integrato Columbus, Rome, Italy 6. Department of Dermatology, Tokyo Women’s Medical University Medical Center East, Tokyo, Japan 7. Kobayashi Clinic, Tokyo, Japan 8. Department of Dermatology, Claude Bernard - Lyon 1 University, Centre Hospitalier Lyon-Sud, Pierre Bénite, France. 9. Department of Dermatology and Venereology, Medical University, Graz, Austria 10. Dermatology Unit, Second University of Naples, Naples, Italy. This article has been accepted for publication and undergone full peer review but has not been through the copyediting, typesetting, pagination and proofreading process, which may lead to differences between this version and the Version of Record. Please cite this article as Accepted doi: 10.1111/bjd.14045 This article is protected by copyright. All rights reserved. Please address all correspondence to: Aimilios Lallas, MD. -

Nevus of Ota in Children
PEDIATRIC DERMATOLOGY Series Editor: Camila K. Janniger, MD Nevus of Ota in Children Smeeta Sinha, MD; Philip J. Cohen, MD; Robert A. Schwartz, MD, MPH Nevus of Ota, synonymously termed oculodermal seen most commonly in individuals of Japanese melanosis, is an uncommon dermal melanosis descent, and is less likely to present in individuals most commonly seen at birth in children of of Chinese or Korean descent, though individuals Japanese descent, though it can affect individu- descending from the Indian subcontinent, Africa, als of any age or ethnicity. The disease tends to and Europe also may be affected.7 In early sur- persist and extend locally, becoming increasingly veys of Japanese patients at dermatology clinics, prominent with age, puberty, and postmenopausal the incidence of nevus of Ota was determined to state. Treatment should begin early after diagno- be 0.4% (110/27,500).4 Cowan and Balistocky8 sis using multiple sessions of laser photother- calculated the incidence of oculodermal melano- molysis to avoid darkening and extension of the cytosis in black patients to be 0.016%. A study of lesion. Important associated disorders include 2914 Chinese children in Calgary, Alberta, Canada, ipsilateral glaucoma; intracranial melanocyto- reported an incidence of oculodermal melanocytosis sis; and rarely cutaneous, ocular, or intracranial of 0.034% (1/2914).9 melanoma. Recommendations are discussed for managing nevus of Ota in children. Clinical Manifestation Cutis. 2008;82:25-29. The typical nevus of Ota is a unilateral facial dis- coloration that is macular, speckled, and bluish gray or brown, with edges that blend with bordering skin evus of Ota is a rare disorder characterized (Figure).10 The dermatomal distribution of pigment by melanocytic pigmentation of the sclera characterizes this diagnosis in most cases. -

Blue Nevi and Melanomas Natural Blue BLUE NEVUS Blue Nevus (BN)
KJ Busam, M.D. Paris, 2017 Blue Nevi and Melanomas Natural Blue BLUE NEVUS Blue Nevus (BN) • Spectrum of blue nevi – Common, Sclerosing, Epithelioid, Cellular, Plaque type blue nevi • Differential diagnosis – Melanoma ex BN or simulating BN – BN vs other tumors – Biphenotypic/collision lesions Common Blue Nevus Clinical: - Circumscribed small bluish macule/papule - Preferred sites: Scalp, wrist, foot Pathology: - Predominantly reticular dermal lesion - Pigmented fusiform and dendritic cells - Admixed melanophages - Bland cytology Common Blue Nevus Blue Nevus Sclerosing Blue Nevus Pigm BN Cellular Blue Nevus - 49 yo woman - Buttock nodule CBN Cellular Blue Nevus Thrombi and stromal edema Multinucleated giant melanocytes Cellular Blue Nevus Hemorrhagic cystic (“aneurysmal”) change Amelanotic Cellular Blue Nevus 19 yo man with buttock lesion Atypical CBN Plaque-Type Blue Nevus Plaque-type Blue Nevus Plaque Type Blue Nevus Mucosal Blue Nevus Conjunctival Blue Nevus Nodal Blue Nevus Combined epithelioid BN Blue Nevus • M Tieche 1906; Virchow Arch Pathol Anat “Blaue Naevus” • B Upshaw 1947; Surgery “Extensive Blue Nevus” (plaque-type BN) • A Allen 1949; Cancer “ Cellular Blue Nevus” Blue Nevus – Mutation Analysis Type of Lesion GNAQ GNA11 Number Common BN 6.7% 65% 60 Cellular BN 8.3% 72.2% 36 Amelanotic BN 0% 70% 10 Nevus of Ota 5% 10% 20 Nevus of Ito 16.7% 0% 7 TOTAL 6.5% 55% 139 Van Raamsdonk et al NEJM 2010; 2191-9 Blue Nevus – Mutation Analysis Type of Blue Nevus GNAQ Number Common Blue Nevus 40% 4/10 Cellular Blue Nevus 44% 4/9 Hypomelanotic -

Nevus of Ota – an Intraoral Presentation: a Case Report Jennifer Maguire1* and Deborah Holt2
Maguire and Holt Journal of Medical Case Reports (2019) 13:174 https://doi.org/10.1186/s13256-019-2101-0 CASEREPORT Open Access Nevus of Ota – an intraoral presentation: a case report Jennifer Maguire1* and Deborah Holt2 Abstract Background: Nevus of Ota or “oculodermal melanocytosis” is a rare congenital hamartoma of dermal melanocytes causing a blue-gray hyperpigmentation of the eye and surrounding structures. The condition, originally described by Ota and Tanino in 1939, mainly affects the ophthalmic and maxillary divisions of the trigeminal nerve. We describe the first reported case of unilateral oculodermal melanocytosis in a Caucasian woman with oral buccal mucosal involvement. Oral involvement of nevus of Ota is very rare. Case presentation: A 48-year-old Caucasian woman was referred by the dermatology division to the oral medicine department at the University of Liverpool School of Dentistry with new-onset oral pigmentation to the left buccal mucosa. The patient had a previous diagnosis of oculodermal nevus. Conclusion: An incisional biopsy of the left buccal mucosa was completed. The report stated that histological and immunohistochemical features were in keeping with a blue nevus, but within the context of the preexisting occulodermal pigmentation, a diagnosis of oculodermal melanocytosis, also known as “nevus of Ota,” was made. The patient will be kept under review in the oral medicine department because the progression of the lesion on the left buccal mucosa requires active monitoring owing to the potential for malignant change. The patient also requires regular review in the dermatology and ophthalmology divisions. Keywords: Oral, Pigmentation, Nevus, Ota, Oculodermal, Buccal, Mucosa Background the left buccal mucosa. -

Acral Lentiginous Melanoma in Situ: Dermoscopic Features and Management Strategy Byeol Han1,2, Keunyoung Hur1, Jungyoon Ohn1,2, Sophie Soyeon Lim3 & Je‑Ho Mun1,2*
www.nature.com/scientificreports OPEN Acral lentiginous melanoma in situ: dermoscopic features and management strategy Byeol Han1,2, Keunyoung Hur1, Jungyoon Ohn1,2, Sophie Soyeon Lim3 & Je‑Ho Mun1,2* Diagnosis of acral lentiginous melanoma in situ (ALMIS) is challenging. However, data regarding ALMIS are limited in the literature. The aim of this study was to investigate the clinical and dermoscopic features of ALMIS on palmoplantar surfaces. Patients with ALMIS and available dermoscopic images were retrospectively reviewed at our institution between January 2013 and February 2020. Clinical and dermoscopic features were analysed and compared between small (< 15 mm) and large (≥ 15 mm) ALMIS. Twenty‑one patients with ALMIS were included in this study. Mean patient age was 58.5 (range 39–76) years; most lesions were located on the sole (90.5%). The mean maximal diameter was 19.9 ± 13.7 mm (mean ± standard deviation). Statistical analysis of dermoscopic features revealed that parallel ridge patterns (54.5% vs. 100%, P = 0.035), irregular difuse pigmentation (27.3% vs. 100%, P = 0.001) and grey colour (18.2% vs. 90%, P = 0.002) were signifcantly less frequent in small lesions than in large lesions. We have also illustrated two unique cases of small ALMIS; their evolution and follow‑up dermoscopic examination are provided. In conclusion, this study described detailed dermoscopic fndings of ALMIS. Based on the present study and a review of the literature, we proposed a dermoscopic algorithm for the diagnosis of ALMIS. Acral lentiginous melanoma (ALM), frst described by Reed in 1976, is a histological subtype of cutaneous melanoma arising on the acral areas1,2. -

Acquired Blue Nevus of the Nail Bed
Volume 23 Number 2 | February 2017 Dermatology Online Journal || Case Report DOJ 23 (2): 3 Acquired blue nevus of the nail bed Daniel M. Klufas BS, Syril Keena T. Que MD, Adrienne Berke MD, Brett Sloan MD Affiliations: Department of Dermatology, University of Connecticut Health Center, Farmington, Connecticut, USA Corresponding Author: Steven Brett Sloan, MD, Associate Professor of Dermatology, VA Site Director, University of Connecticut Health Center, Department of Dermatology, 21 South Road, Suite 200, Farmington, CT 06030-6231, Tel: 860-679-4600, Email: Steven.Sloan@ va.gov Abstract been reports of malignant degeneration particularly of the cellular variant [1,2,6]. Nonetheless, careful Blue nevi are benign proliferations of melanin- examination and evaluation should be performed producing dendritic melanocytes located in the in order to differentiate between a blue nevus and dermis. These nevi tend to occur mostly on the skin, a subungual malignant melanoma, which carries predominantly on the head and neck, dorsal aspects a poor prognosis. We report here on a 47-year-old of the distal extremities, and the sacral area, but Japanese man with an acquired blue nevus in the can also occasionally appear on mucosal surfaces. nail bed of his right first toe and discuss clinical and Blue nevi of the nail apparatus are uncommon. The pathologic characteristics of this rare finding. majority originate in the nail matrix where there is a higher density of melanocytes. Herein we report on Case Synopsis a 47-year-old man with a rare common blue nevus of A 47-year-old Japanese man with a family history of the nail bed, an area with low melanocyte density.