Trauma Triage Criteria
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Blunt and Blast Head Trauma: Different Entities
International Tinnitus Journal, Vol. 15, No. 2, 115–118 (2009) Blunt and Blast Head Trauma: Different Entities Michael E. Hoffer,1 Chadwick Donaldson,1 Kim R. Gottshall1, Carey Balaban,2 and Ben J. Balough1 1 Spatial Orientation Center, Department of Otolaryngology, Naval Medical Center San Diego, San Diego, California, and 2 Department of Otolaryngology, University of Pittsburgh, Pittsburgh, Pennsylvania, USA Abstract: Mild traumatic brain injury (mTBI) caused by blast-related and blunt head trauma is frequently encountered in clinical practice. Understanding the nuances between these two distinct types of injury leads to a more focused approach by clinicians to develop better treat- ment strategies for patients. In this study, we evaluated two separate cohorts of mTBI patients to ascertain whether any difference exists in vestibular-ocular reflex (VOR) testing (n ϭ 55 en- rolled patients: 34 blunt, 21 blast) and vestibular-spinal reflex (VSR) testing (n ϭ 72 enrolled patients: 33 blunt, 39 blast). The VOR group displayed a preponderance of patients with blunt mTBI, demonstrating normal to high-frequency phase lag on rotational chair testing, whereas patients experiencing mTBI from blast-related causes revealed a trend toward low-frequency phase lag on evaluation. The VSR cohort showed that patients with posttraumatic migraine- associated dizziness tended to test higher on posturography. However, an indepth look at the total patient population in this second cohort reveals that a higher percentage of blast-exposed patients exhibited a significantly increased latency on motor control testing as compared to pa- tients with blunt head injury ( p Ͻ .02). These experiments identify a distinct difference be- tween blunt-injury and blast-injury mTBI patients and provide evidence that treatment strategies should be individualized on the basis of each mechanism of injury. -

Mass/Multiple Casualty Triage
9.1 MASS/MULTIPLE CASUALTY TRIAGE PURPOSE · The goal of the mass/multiple Casualty Triage protocol is to prepare for a unified, coordinated, and immediate EMS mutual aid response by prehospital and hospital agencies to effectively expedite the emergency management of the victims of any type of Mass Casualty Incident (MCI). · Successful management of any MCI depends upon the effective cooperation, organization, and planning among health care professionals, hospital administrators and out-of-hospital EMS agencies, state and local government representatives, and individuals and/or organizations associated with disaster-related support agencies. · Adoption of Model Uniform Core Criteria (MUCC). DEFINITIONS Multiple Casualty Situations · The number of patients and the severity of the injuries do not exceed the ability of the provider to render care. Patients with life-threatening injuries are treated first. Mass Casualty Incidents · The number of patients and the severity of the injuries exceed the capability of the provider, and patients sustaining major injuries who have the greatest chance of survival with the least expenditure of time, equipment, supplies, and personnel are managed first. H a z GENERAL CONSIDERATIONS m Initial assessment to include the following: a t · Location of incident. & · Type of incident. M · Any hazards. C · Approximate number of victims. I · Type of assistance required. 9 . 1 COMMUNICATION · Within the scope of a Mass Casualty Incident, the EMS provider may, within the limits of their scope of practice, perform necessary ALS procedures, that under normal circumstances would require a direct physician’s order. · These procedures shall be the minimum necessary to prevent the loss of life or the critical deterioration of a patient’s condition. -
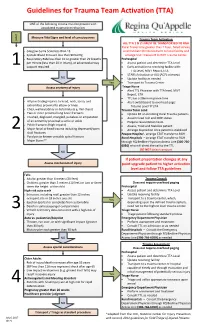
Guidelines for Trauma Team Activation (TTA)
Guidelines for Trauma Team Activation (TTA) ONE of the following criteria must be present with associated traumatic mechanism L e v e Measure Vital Signs and level of consciousness l Trauma Team Activation ALL TTA 1 & 2's MUST BE TRANSPORTED TO RGH Rural Travel time greater than 1 hour, failed airway · Glasgow Coma Scale less than 13 or immediate life threat divert to local facility and · Systolic Blood Pressure less than 90mmHg arrange STAT transport to RGH Trauma Center · Respiratory Rate less than 10 or greater then 29 breaths Prehospital per minute (less than 20 in infant), or advanced airway · Assess patient and determine TTA Level 1 support required · Early activation to receiving facility with: TTA Level, MIVT Report, ETA · STARS Activation or ALS (ACP) intercept NO · Update facility as needed Yes · Transport to Trauma Center Assess anatomy of injury Triage Nurse · Alert TTL Physician with TTA level, MIVT Report, ETA · TTL has a 20min response time · All penetrating injuries to head, neck, torso, and · Alert switchboard to overhead page: extremities proximal to elbow or knee Trauma Level ‘#’ ETA · Chest wall instability or deformity (e.g. flail chest) Trauma Team Lead · Two or more proximal long-bone fractures · Update ER on incoming Rural Trauma patients · Crushed, degloved, mangled, pulseless or amputation · Assume lead role and MRP status of an extremity proximal to wrist or ankle · Prepare resuscitation team · Pelvic fractures (high impact) · Assess, Treat and Stabilize patient 2 · Major facial or head trauma including depressed/open -

MASS CASUALTY TRAUMA TRIAGE PARADIGMS and PITFALLS July 2019
1 Mass Casualty Trauma Triage - Paradigms and Pitfalls EXECUTIVE SUMMARY Emergency medical services (EMS) providers arrive on the scene of a mass casualty incident (MCI) and implement triage, moving green patients to a single area and grouping red and yellow patients using triage tape or tags. Patients are then transported to local hospitals according to their priority group. Tagged patients arrive at the hospital and are assessed and treated according to their priority. Though this triage process may not exactly describe your agency’s system, this traditional approach to MCIs is the model that has been used to train American EMS As a nation, we’ve got a lot providers for decades. Unfortunately—especially in of trailers with backboards mass violence incidents involving patients with time- and colored tape out there critical injuries and ongoing threats to responders and patients—this model may not be feasible and may result and that’s not what the focus in mis-triage and avoidable, outcome-altering delays of mass casualty response is in care. Further, many hospitals have not trained or about anymore. exercised triage or re-triage of exceedingly large numbers of patients, nor practiced a formalized secondary triage Dr. Edward Racht process that prioritizes patients for operative intervention American Medical Response or transfer to other facilities. The focus of this paper is to alert EMS medical directors and EMS systems planners and hospital emergency planners to key differences between “conventional” MCIs and mass violence events when: • the scene is dynamic, • the number of patients far exceeds usual resources; and • usual triage and treatment paradigms may fail. -

Isolated Severe Blunt Traumatic Brain Injury: Effect of Obesity on Outcomes
CLINICAL ARTICLE J Neurosurg 134:1667–1674, 2021 Isolated severe blunt traumatic brain injury: effect of obesity on outcomes Jennifer T. Cone, MD, MHS,1 Elizabeth R. Benjamin, MD, PhD,2 Daniel B. Alfson, MD,2 and Demetrios Demetriades, MD, PhD2 1Department of Surgery, Section of Trauma and Acute Care Surgery, University of Chicago, Illinois; and 2Department of Surgery, Division of Trauma, Emergency Surgery, and Surgical Critical Care, LAC+USC Medical Center, University of Southern California, Los Angeles, California OBJECTIVE Obesity has been widely reported to confer significant morbidity and mortality in both medical and surgical patients. However, contemporary data indicate that obesity may confer protection after both critical illness and certain types of major surgery. The authors hypothesized that this “obesity paradox” may apply to patients with isolated severe blunt traumatic brain injuries (TBIs). METHODS The Trauma Quality Improvement Program (TQIP) database was queried for patients with isolated severe blunt TBI (head Abbreviated Injury Scale [AIS] score 3–5, all other body areas AIS < 3). Patient data were divided based on WHO classification levels for BMI: underweight (< 18.5 kg/m2), normal weight (18.5–24.9 kg/m2), overweight (25.0–29.9 kg/m2), obesity class 1 (30.0–34.9 kg/m2), obesity class 2 (35.0–39.9 kg/m2), and obesity class 3 (≥ 40.0 kg/ m2). The role of BMI in patient outcomes was assessed using regression models. RESULTS In total, 103,280 patients were identified with isolated severe blunt TBI. Data were excluded for patients aged < 20 or > 89 years or with BMI < 10 or > 55 kg/m2 and for patients who were transferred from another treatment center or who showed no signs of life upon presentation, leaving data from 38,446 patients for analysis. -

Traumatic Brain Injury (TBI)
Traumatic Brain Injury (TBI) Carol A. Waldmann, MD raumatic brain injury (TBI), caused either by blunt force or acceleration/ deceleration forces, is common in the general population. Homeless persons Tare at particularly high risk of head trauma and adverse outcomes to TBI. Even mild traumatic brain injury can lead to persistent symptoms including cognitive, physical, and behavioral problems. It is important to understand brain injury in the homeless population so that appropriate referrals to specialists and supportive services can be made. Understanding the symptoms and syndromes caused by brain injury sheds light on some of the difficult behavior observed in some homeless persons. This understanding can help clinicians facilitate and guide the care of these individuals. Prevalence and Distribution recover fully, but up to 15% of patients diagnosed TBI and Mood Every year in the USA, approximately 1.5 with MTBI by a physician experience persistent Swings. million people sustain traumatic brain injury disabling problems. Up to 75% of brain injuries This man suffered (TBI), 230,000 people are hospitalized due to TBI are classified as MTBI. These injuries cost the US a gunshot wound and survive, over 50,000 people die from TBI, and almost $17 billion per year. The groups most at risk to the head and many subsequent more than 1 million people are treated in emergency for TBI are those aged 15-24 years and those aged traumatic brain rooms for TBI. In persons under the age of 45 years, 65 years and older. Men are twice as likely to sustain injuries while TBI is the leading cause of death. -

A Uniform Triage Scale in Emergency Medicine Information Paper
A Uniform Triage Scale in Emergency Medicine Information Paper Triage: sorting, sifting (Webster’s New Collegiate Dictionary) from the French verb trier- “to sort.” Triage has long been considered a simple frontline sorting mechanism in hospital-based emergency departments (EDs). However, evolution in the practice of emergency medicine during the past two decades necessitates a change in how this entry point process is performed and utilized. Many triage systems are in use in the US, but there is no uniform triage scale that would facilitate the development of operational standards in EDs. A nationally standardized triage scale would provide an analytic basis for determining whether the health care system provides safe access to emergency care based on design, resources, and utilization. The performance of EDs could be compared based on case mix and acuity, and expected standards for facilities could be defined. Planners and policy makers would have the tools and the data needed to make rational improvements in the health care delivery system. This paper on triage will acquaint the reader with the history of triage, and provide an overview of the Australian and Canadian systems which are already in use on a national level. The reliability of triage is addressed, and the Canadian and Australian scales are compared. Future implications for a national triage scale are described, along with the goals and benefits of triage development. While there is some controversy about potential liability issues, the many advantages of a national triage scale appear to outweigh any potential disadvantages. History of triage The first medical application of triage occurred on the French battlefield where sorting the victims determined who would be left behind. -

Severe Localized Scapular Pain After a Strenuous Weight-Lifting Session
CASE REPORT Severe localized scapular Editor’s key points With the rising popularity of ultra- pain after a strenuous distance endurance events, strength and conditioning programs, and obstacle course races, exertional weight-lifting session rhabdomyolysis (ER) has become increasingly common in sporting Rosamond E. Lougheed Simpson MD MSc CCFP(SEM) DipSportMed communities. Steven R. Joseph MD MA CCFP(SEM) DipSportMed Lisa Fischer MD CCFP(SEM) FCFP DipSportMed Exertional rhabdomyolysis is often characterized by the classic triad habdomyolysis is a medical condition whereby the intracellular con- of generalized weakness, myalgia, tents from damaged skeletal muscle tissues are released into the blood, and myoglobinuria; however, it is critical to recognize that many cases causing myriad clinical symptoms and outcomes. These can range will not present with all 3 of these Rfrom muscle pain to compartment syndrome, end-organ failure, and death.1-3 criteria. For the male patient in this While the triggers of rhabdomyolysis are numerous, physical exertion as a report, severe myalgia was his only presenting symptom from the triad. causal factor has been receiving increasing media attention recently.4-7 The incidence of exertional rhabdomyolysis (ER) has been challenging The ability to recognize ER, stratify 8 patients into low- and high-risk to estimate, as many cases are likely underrecognized. Current incidence categories, and understand how estimates range from 22.2 to 29.9 per 100 000 patients a year.9,10 As ultra- risk affects patients’ return to play distance endurance events, strength and conditioning programs (eg, CrossFit), can help family physicians make treatment, referral, and return- and obstacle course races have become wildly popular with the superfit to-play decisions with increased and weekend warriors alike, ER is being increasingly recognized as common confidence. -

Redefining the Trauma Triage Matrix
journalofsurgicalresearch july 2020 (251) 195e201 Available online at www.sciencedirect.com ScienceDirect journal homepage: www.JournalofSurgicalResearch.com Redefining the Trauma Triage Matrix: The Role of Emergent Interventions Rachel S. Morris, MD,a,* Nicholas J. Davis, MD,b Amy Koestner, MSN,c Lena M. Napolitano, MD,d Mark R. Hemmila, MD,d and Christopher J. Tignanelli, MDa,b,e a Department of Surgery, University of Minnesota, Minneapolis, Minnesota b Department of Surgery, North Memorial Medical Center, Robbinsdale, Minnesota c Department of Surgery, Spectrum Health - Butterworth Hospital, Grand Rapids, Michigan d Department of Surgery, University of Michigan, Ann Arbor, Michigan e Institute for Health Informatics, University of Minnesota, Minneapolis, Minnesota article info abstract Article history: Background: A tiered trauma team activation (TTA) system aims to allocate resources pro- Received 10 July 2019 portional to the patient’s need based upon injury burden. The current metrics used to Received in revised form evaluate appropriateness of TTA are the trauma triage matrix (TTM), need for trauma 22 October 2019 intervention (NFTI), and secondary triage assessment tool (STAT). Accepted 2 November 2019 Materials and methods: In this retrospective study, we compared the effectiveness of the Available online xxx need for an emergent intervention within 6 h (NEI-6) with existing definitions. Data from the Michigan Trauma Quality Improvement Program was utilized. The dataset contains Keywords: information from 31 level 1 and 2 trauma centers from 2011 to 2017. Inclusion criteria were: Activation adult patients (16 y) and ISS 5. Trauma Results: 73,818 patients were included in the study. Thirty percentage of trauma patients Triage met criteria for STAT, 21% for NFTI, 20% for TTM, and 13% for NEI-6. -

Mass Casualty Incident (MCI) Response Module 1
Mass Casualty Incident (MCI) Response Module 1 (Hamilton County Fire Chief's Association, 2013) 1 Objectives Purpose: This module will educate staff on mass casualty triage incident response, including how to: • Define mass casualty triage • Determine considerations for adults and pediatrics • Understand the importance of a patient tracking system • Recognize and implement the patient admission/ discharge MCI triage process • Determine how to appropriately handle the deceased in a large-scale MCI • Recognize the range of incidents that may cause MCIs 2 MCI Basics 3 What is an MCI? • A mass casualty incident (MCI) is an incident where the number of patients exceeds the amount of healthcare resources available. • This number varies widely across the country, but is typically greater than 10 patients. 4 Types of MCI Notifications • During a large scale incident such as a mass casualty, it is important to have a mass notification system. Successful mass notification systems will: . Internally: alert staff to activate MCI protocols and prepare for a potential surge of patients . Externally: increase community awareness 5 Assisting in MCI Response Considerations for hospital staff in an MCI: • Some patients may arrive to the hospital without having been assessed/ triaged at the scene • MCI response requires efficiency and coordination • Non-clinical personnel (including hospital volunteers) can assist in moving patients to designated areas based on level of care • Help gather patient information in the emergency treatment area • Staff should review patients in clinical assignment for any potential discharges/ transfers to make room for potential MCI admissions, a process known as “surge discharge” (Chung S, 2019) 6 Triage Basics Definition of MCI Triage Triage means “to sort.” Triage in an MCI is the assignment of resources based on the initial patient assessment and consideration of available resources. -

Chronic Traumatic Encephalopathy: the Dangers of Getting “Dinged” Shaheen E Lakhan1* and Annette Kirchgessner1,2
Lakhan and Kirchgessner SpringerPlus 2012, 1:2 http://www.springerplus.com/content/1/1/2 a SpringerOpen Journal REVIEW Open Access Chronic traumatic encephalopathy: the dangers of getting “dinged” Shaheen E Lakhan1* and Annette Kirchgessner1,2 Abstract Chronic traumatic encephalopathy (CTE) is a form of neurodegeneration that results from repetitive brain trauma. Not surprisingly, CTE has been linked to participation in contact sports such as boxing, hockey and American football. In American football getting “dinged” equates to moments of dizziness, confusion, or grogginess that can follow a blow to the head. There are approximately 100,000 to 300,000 concussive episodes occurring in the game of American football alone each year. It is believed that repetitive brain trauma, with or possibly without symptomatic concussion, sets off a cascade of events that result in neurodegenerative changes highlighted by accumulations of hyperphosphorylated tau and neuronal TAR DNA-binding protein-43 (TDP-43). Symptoms of CTE may begin years or decades later and include a progressive decline of memory, as well as depression, poor impulse control, suicidal behavior, and, eventually, dementia similar to Alzheimer’s disease. In some individuals, CTE is also associated with motor neuron disease similar to amyotrophic lateral sclerosis. Given the millions of athletes participating in contact sports that involve repetitive brain trauma, CTE represents an important public health issue. In this review, we discuss recent advances in understanding the etiology of CTE. It is now known that those instances of mild concussion or “dings” that we may have previously not noticed could very well be causing progressive neurodegenerative damage to a player’s brain. -

Heart Rate and Posttraumatic Stress in Injured Children
ORIGINAL ARTICLE Heart Rate and Posttraumatic Stress in Injured Children Nancy Kassam-Adams, PhD; J. Felipe Garcia-España, PhD; Joel A. Fein, MD; Flaura Koplin Winston, MD, PhD Background: Elevated, acute heart rate has been re- Main Outcome Measure: Clinician-Administered PTSD lated to later posttraumatic stress disorder (PTSD) de- Scale for Children and Adolescents. velopment in injured adults, but this has not been ex- amined in children and adolescents. Better understanding Results: The group of children who developed partial of the relationship between acute physiological arousal or full PTSD had a higher mean±SD heart rate at ED tri- and later child PTSD could help elucidate the etiology age than those who did not go on to have PTSD of posttrauma responses in children and might identify (109.6±22.3 vs 99.7±18.0 beats per minute). Children useful markers for PTSD risk. with an elevated heart rate (defined as Ն2 SDs higher than the normal resting heart rate for their age and sex) at ED Objective: To evaluate the relationship between heart triage were more likely to meet criteria for partial or full rate assessed in the emergency department (ED) during PTSD at follow-up, even after adjusting for age, sex, and normal clinical care and later PTSD outcome in trau- injury (adjusted odds ratio, 2.4 [95% confidence inter- matically injured children. val, 1.1-5.4]). Design: Prospective cohort study assessed heart rate at Conclusion: These results suggest an association be- ED triage and PTSD an average of 6 months’ postinjury. tween early physiological arousal and the development Setting: Large, urban pediatric academic medical cen- or persistence of PTSD symptoms in injured children and ter in the northeastern United States.