Withholding and Termination of Resuscitation of Adult Cardiopulmonary Arrest Secondary to Trauma: Resource Document to the Joint NAEMSP-ACSCOT Position Statements
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

A Rare Case of Penetrating Trauma of Frontal Sinus with Anterior Table Fracture Himanshu Raval1*, Mona Bhatt2 and Nihar Gaur3
ISSN: 2643-4474 Raval et al. Neurosurg Cases Rev 2020, 3:046 DOI: 10.23937/2643-4474/1710046 Volume 3 | Issue 2 Neurosurgery - Cases and Reviews Open Access CASE REPORT Case Report: A Rare Case of Penetrating Trauma of Frontal Sinus with Anterior Table Fracture Himanshu Raval1*, Mona Bhatt2 and Nihar Gaur3 1 Department of Neurosurgery, NHL Municipal Medical College, SVP Hospital Campus, Gujarat, India Check for updates 2Medical Officer, CHC Dolasa, Gujarat, India 3GAIMS-GK General Hospital, Gujarat, India *Corresponding author: Dr. Himanshu Raval, Resident, Department of Neurosurgery, NHL Municipal Medical College, SVP Hospital Campus, Elisbridge, Ahmedabad, Gujarat, 380006, India, Tel: 942-955-3329 Abstract Introduction Background: Head injury is common component of any Road traffic accident (RTA) is the most common road traffic accident injury. Injury involving only frontal sinus cause of cranio-facial injury and involvement of frontal is uncommon and unique as its management algorithm is bone fractures are rare and constitute 5-9% of only fa- changing over time with development of radiological modal- ities as well as endoscopic intervention. Frontal sinus inju- cial trauma. The degree of association has been report- ries may range from isolated anterior table fractures causing ed to be 95% with fractures of the anterior table or wall a simple aesthetic deformity to complex fractures involving of the frontal sinuses, 60% with the orbital rims, and the frontal recess, orbits, skull base, and intracranial con- 60% with complex injuries of the naso-orbital-ethmoid tents. Only anterior table injury of frontal sinus is rare in pen- region, 33% with other orbital wall fractures and 27% etrating head injury without underlying brain injury with his- tory of unconsciousness and questionable convulsion which with Le Fort level fractures. -
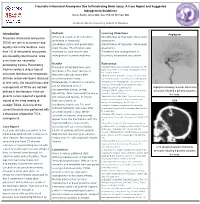
Traumatic Intracranial Aneurysms Due to Penetrating Brain Injury. a Case Report and Suggested Management Guidelines Breck Aaron Jones MD; Alex Patrick Michael MD
Traumatic Intracranial Aneurysms Due to Penetrating Brain Injury. A Case Report and Suggested Management Guidelines Breck Aaron Jones MD; Alex Patrick Michael MD Southern Illinois University School of Medicine Methods Learning Objectives Introduction Angiogram Traumatic intracranial aneurysms A Pubmed search of the literature Identification of traumatic intracranial pertaining to traumatic aneurysms. (TICA) are rare in occurrence and pseudoaneurysms and penetrating Classification of traumatic intracranial equally rare in the literature. Less brain trauma. The literature was aneurysms. than 1% of intracranial aneurysms reviewed for case reports and Treatment and management of are caused by blunt trauma, while management recommendations. traumatic intracranial aneurysms. even fewer are caused by penetrating trauma. Penetrating Results References Traumatic intracranial aneurysm 1.Aarabi B. Management of traumatic aneurysms caused by trauma creates a unique type of high-velocity missile head wounds. Neurosurg Clin N Am. formation is the most commonly aneurysm that does not incorporate Oct 1995;6(4):775-797. described vascular injury after 2.Rao GP, Rao NS, Reddy PK. Technique of removal of an all three vessel wall layers. Because penetrating brain injury. impacted sharp object in a penetrating head injury using the of their rarity, the natural history and Histologically, traumatic aneurysms lever principle. Br J Neurosurg. Dec 1998;12(6):569-571. 3.Vascular complications of penetrating brain injury. J can be described as true management of TICAs are not well Trauma. Aug 2001;51(2 Suppl):S26-28. Angiogram showing traumatic intracranial (incorporating intima, media, defined in the literature. Here we 4.Crompton MR. The pathogenesis of cerebral aneurysms. aneurysm following a gunshot wound to adventitia), false (incorporating one or Brain. -

Blunt and Blast Head Trauma: Different Entities
International Tinnitus Journal, Vol. 15, No. 2, 115–118 (2009) Blunt and Blast Head Trauma: Different Entities Michael E. Hoffer,1 Chadwick Donaldson,1 Kim R. Gottshall1, Carey Balaban,2 and Ben J. Balough1 1 Spatial Orientation Center, Department of Otolaryngology, Naval Medical Center San Diego, San Diego, California, and 2 Department of Otolaryngology, University of Pittsburgh, Pittsburgh, Pennsylvania, USA Abstract: Mild traumatic brain injury (mTBI) caused by blast-related and blunt head trauma is frequently encountered in clinical practice. Understanding the nuances between these two distinct types of injury leads to a more focused approach by clinicians to develop better treat- ment strategies for patients. In this study, we evaluated two separate cohorts of mTBI patients to ascertain whether any difference exists in vestibular-ocular reflex (VOR) testing (n ϭ 55 en- rolled patients: 34 blunt, 21 blast) and vestibular-spinal reflex (VSR) testing (n ϭ 72 enrolled patients: 33 blunt, 39 blast). The VOR group displayed a preponderance of patients with blunt mTBI, demonstrating normal to high-frequency phase lag on rotational chair testing, whereas patients experiencing mTBI from blast-related causes revealed a trend toward low-frequency phase lag on evaluation. The VSR cohort showed that patients with posttraumatic migraine- associated dizziness tended to test higher on posturography. However, an indepth look at the total patient population in this second cohort reveals that a higher percentage of blast-exposed patients exhibited a significantly increased latency on motor control testing as compared to pa- tients with blunt head injury ( p Ͻ .02). These experiments identify a distinct difference be- tween blunt-injury and blast-injury mTBI patients and provide evidence that treatment strategies should be individualized on the basis of each mechanism of injury. -

Management of Acute Liver Failure In
Management of Acute Liver Failure in ICU Philip Berry MRCP, Clinical Research Fellow, Institute of Liver Studies, Kings College Hospital, London, UK Email: [email protected] Self assessment questions Scenario: A twenty-year-old female is brought into the Emergency Department having been found unconscious in her bedsit. There is no other recent history. She did not respond to a bolus of 50% dextrose in the ambulance, despite having an unrecordable blood glucose when tested by the paramedics. While she is being intubated on account of reduced level of consciousness, an arterial blood gas sample reveals profound lactic acidosis (pH 7.05, pCO2 2.5 kPa, base deficit – 10, lactate 13 mg/L). Blood pressure is 95/50 mmHg. 1. What are the possible explanations for her presentation? Laboratory tests demonstrate hepatocellular necrosis (AST 21,000 U/L) and coagulopathy (INR 9.1) with thrombocytopenia (platelet count 26 x 109/L). Acute liver failure appears the most likely diagnosis. 2. What are the most likely causes of acute liver failure (ALF) in this previously well patient? Her mean arterial blood pressure remains low (50mmHg) after 3 litres of colloid and crystalloid. The casualty nurse, who is doing half-hourly neurological observations, reports reduced pupillary response to light. 3. What severe complications of ALF may result in death within hours, and what are the immediate management priorities for this patient? Introduction Successful management of this rare but potentially devastating disorder relies on early recognition. The hallmark of acute liver failure (ALF) is encephalopathy (ranging from a subtle alterations in consciousness level to coma) in the context of an acute, severe liver injury. -

Isolated Severe Blunt Traumatic Brain Injury: Effect of Obesity on Outcomes
CLINICAL ARTICLE J Neurosurg 134:1667–1674, 2021 Isolated severe blunt traumatic brain injury: effect of obesity on outcomes Jennifer T. Cone, MD, MHS,1 Elizabeth R. Benjamin, MD, PhD,2 Daniel B. Alfson, MD,2 and Demetrios Demetriades, MD, PhD2 1Department of Surgery, Section of Trauma and Acute Care Surgery, University of Chicago, Illinois; and 2Department of Surgery, Division of Trauma, Emergency Surgery, and Surgical Critical Care, LAC+USC Medical Center, University of Southern California, Los Angeles, California OBJECTIVE Obesity has been widely reported to confer significant morbidity and mortality in both medical and surgical patients. However, contemporary data indicate that obesity may confer protection after both critical illness and certain types of major surgery. The authors hypothesized that this “obesity paradox” may apply to patients with isolated severe blunt traumatic brain injuries (TBIs). METHODS The Trauma Quality Improvement Program (TQIP) database was queried for patients with isolated severe blunt TBI (head Abbreviated Injury Scale [AIS] score 3–5, all other body areas AIS < 3). Patient data were divided based on WHO classification levels for BMI: underweight (< 18.5 kg/m2), normal weight (18.5–24.9 kg/m2), overweight (25.0–29.9 kg/m2), obesity class 1 (30.0–34.9 kg/m2), obesity class 2 (35.0–39.9 kg/m2), and obesity class 3 (≥ 40.0 kg/ m2). The role of BMI in patient outcomes was assessed using regression models. RESULTS In total, 103,280 patients were identified with isolated severe blunt TBI. Data were excluded for patients aged < 20 or > 89 years or with BMI < 10 or > 55 kg/m2 and for patients who were transferred from another treatment center or who showed no signs of life upon presentation, leaving data from 38,446 patients for analysis. -

Prehospital Spine Immobilization for Penetrating Trauma—Review and Recommendations from the Prehospital Trauma Life Support Executive Committee
REVIEW ARTICLE Prehospital Spine Immobilization for Penetrating Trauma—Review and Recommendations From the Prehospital Trauma Life Support Executive Committee Lance E. Stuke, MD, MPH, Peter T. Pons, MD, Jeffrey S. Guy, MD, MSc, MMHC, Will P. Chapleau, RN, EMT-P, Frank K. Butler, MD, Capt MC USN (Ret), and Norman E. McSwain, MD pine immobilization in trauma patients suspected of hav- In the case of penetrating injuries, delays in transport Sing a spinal injury has been a cornerstone of prehospital prolong the time before patients receive the prompt surgical treatment for decades. Current practices are based on the care needed to arrest hemorrhage. Even with experienced belief that a patient with an injured spinal column can prehospital providers, spine immobilization is time consum- deteriorate neurologically without immobilization. Most ing. The time required for experienced emergency medical treatment protocols do not differentiate between blunt and technicians to properly immobilize a cervical spine has been penetrating mechanisms of injury. Current Emergency Med- reported to be 5.64 minutes (Ϯ1.49 minutes).6 This scene ical Service (EMS) protocols for spinal immobilization of delay can be catastrophic for a patient with penetrating penetrating trauma are based on historic practices rather than trauma requiring urgent surgical intervention for airway com- scientific merits. Although blunt spinal column injuries will promise or hemorrhage. Studies have demonstrated that cervical collars increase occasionally produce unstable vertebral -

Validation of Lactate Clearance at 6 H for Mortality Prediction in Critically Ill Children
570 Research Article Validation of lactate clearance at 6 h for mortality prediction in critically ill children Rajeev Kumar, Nirmal Kumar Background and Aims: To validate the lactate clearance (LC) at 6 h for mortality Access this article online prediction in Pediatric Intensive Care Unit (PICU)-admitted patients and its comparison Website: www.ijccm.org with a pediatric index of mortality 2 (PIM 2) score. Design: A prospective, observational DOI: 10.4103/0972-5229.192040 study in a tertiary care center. Materials and Methods: Children <13 years of age, Quick Response Code: Abstract admitted to PICU were included in the study. Lactate levels were measured at 0 and 6 h of admission for clearance. LC and delayed or nonclearance group compared for in-hospital mortality and compared with PIM 2 score for mortality prediction. Results: Of the 140 children (mean age 33.42 months) who were admitted to PICU, 23 (16.42%) patients died. For LC cut-off (16.435%) at 6 h, 92 patients qualified for clearance and 48 for delayed or non-LC group. High mortality was observed (39.6%) in delayed or non-LC group as compared to clearance group (4.3%) (P = 0.000). LC cut-off of 16.435% at 6 h (sensitivity 82.6%, specificity 75.2%, positive predictive value 39.6%, and negative predictive value 95.7%) correlates with mortality. Area under receiver operating characteristic (ROC) for LC at 6 h for mortality prediction was 0.823 (P = 0.000). The area under ROC curve for expected mortality prediction by PIM 2 score at admission was 0.906 and at 12.3% cut-off of PIM 2 Score was related with mortality. -

Deaths from Abdominal Trauma: Analysis of 1888 Forensic Autopsies
DOI: 10.1590/0100-69912017006006 Original Article Deaths from abdominal trauma: analysis of 1888 forensic autopsies Óbitos por trauma abdominal: análise de 1888 autopsias médico-legais POLYANNA HELENA COELHO BORDONI1; DANIELA MAGALHÃES MOREIRA DOS SANTOS2; JAÍSA SANTANA TEIXEIRA2; LEONARDO SANTOS BORDONI2-4. ABSTRACT Objective: to evaluate the epidemiological profile of deaths due to abdominal trauma at the Forensic Medicine Institute of Belo Horizonte, MG - Brazil. Methods: we conducted a retrospective study of the reports of deaths due to abdominal trauma autopsied from 2006 to 2011. Results: we analyzed 1.888 necropsy reports related to abdominal trauma. Penetrating trauma was more common than blunt one and gun- shot wounds were more prevalent than stab wounds. Most of the individuals were male, brown-skinned, single and occupationally active. The median age was 34 years. The abdominal organs most injured in the penetrating trauma were the liver and the intestines, and in blunt trauma, the liver and the spleen. Homicide was the most prevalent circumstance of death, followed by traffic accidents, and almost half of the cases were referred to the Forensic Medicine Institute by a health unit. The blood alcohol test was positive in a third of the necropsies where it was performed. Cocaine and marijuana were the most commonly found substances in toxicology studies. Conclusion: in this sam- ple. there was a predominance of penetrating abdominal trauma in young, brown and single men, the liver being the most injured organ. Keywords: Autopsy. Forensic Medicine. Homicide. Abdominal Injuries. INTRODUCTION In addition, the accuracy of abdominal phy- sical examination is low and the level of consciousness eaths from external causes represent the second produced by hemorrhages or by the association of ab- Dleading cause of mortality in Brazil and the main dominal trauma (AT) with traumatic brain injury and/or cause when considering individuals under the age of effects of central nervous system of previously consu- 351. -

Package for Emergency Resuscitation and Intensive Care Unit
Package for Emergency Resuscitation and Intensive Care Unit Extracted from WHO manual Surgical Care at the District Hospital and WHO Integrated Management for Emergency & Essential Surgical Care toolkit For further details and anaesthetic resources please refer to full text at: http://www.who.int/surgery/publications/imeesc/en/index.html 1 1. Anaesthesia and Oxygen XYGEN KEY POINTS: • A reliable oxygen supply is essential for anaesthesia and for any seriously ill patients • In many places, oxygen concentrators are the most suitable and economical way of providing oxygen, with a few backup cylinders in case of electricity failure • Whatever your source of oxygen, you need an effective system for maintenance and spares • Clinical staff need to be trained how to use oxygen safely, effectively and economically. • A high concentration of oxygen is needed during and after anaesthesia: • If the patient is very young, old, sick, or anaemic • If agents that cause cardio-respiratory depression, such as halothane, are used. Air already contains 20.9% oxygen, so oxygen enrichment with a draw-over system is a very economical method of providing oxygen. Adding only 1 litre per minute may increase the oxygen concentration in the inspired gas to 35–40%. With oxygen enrichment at 5 litres per minute, a concentration of 80% may be achieved. Industrial-grade oxygen, such as that used for welding, is perfectly acceptable for the enrichment of a draw-over system and has been widely used for this purpose. Oxygen Sources In practice, there are two possible sources of oxygen for medical purposes: • Cylinders: derived from liquid oxygen • Concentrators: which separate oxygen from air. -

Traumatic Cardiac Arrest
TRAUMATIC CARDIAC ARREST There are a number of studies that show that attempts at resuscitation of traumatic arrests are futile in certain situations. In these futile situations a patient should be considered dead and there should be no further resuscitation efforts. All traumatic pulseless non-breathers will undergo full resuscitation efforts unless: x All trauma with a significant mechanism of injury – If on the first arrival of EMS the patient is pulseless, apneic, and without other signs of life (pupil reactivity, spontaneous movement) or is asystolic, then the patient is not resuscitatable. x If the injuries are incompatible with life (e.g. Decapitation), the patient is not resuscitatable. Any patient not meeting one of the above criteria should have attempted resuscitation – Begin CPR. Follow appropriate Cardiac Arrest, PEA/Asystole protocol in addition to protocol below. If resuscitation has started but it is determined that patient has criteria where additional care is futile, terminate resuscitation if protocol criteria are met (line 10) or contact medical control to determine if resuscitation should be terminated. a. Once determination has been made that the patient is not resuscitatable, law enforcement and the local coroner/medical examiner should be contacted b. The EMS team is not required to stay until the coroner/medical examiner arrives, but should provide law enforcement with: i. Time of arrival and time resuscitation stopped, if applicable. ii. Names of medical crew (and Medical Control Physician if applicable). iii. Name of your EMS agency/department and business phone number. EMERGENCY MEDICAL RESPONDER (EMR) / EMERGENCY MEDICAL TECHNICIAN (EMT)/ ADVANCED EMT (AEMT)/ INTERMEDIATE / PARAMEDIC 1. -

Updated Mild Traumatic Brain Injury Guideline for Adults
Heads Up to Clinicians: Updated Mild Traumatic Brain Injury Guideline for Adults This Guideline is based on the 2008 Mild TBI Clinical Policy for adults, which revises the previous 2002 Clinical Policy. To help improve diagnosis, treatment, and outcomes for patients with mild TBI, it is critical that you become familiar with this guideline. The guideline is especially important for clinicians working in hospital-based emergency care. Inclusion Criteria: This guideline is intended for patients with non-penetrating trauma to the head who present to the ED within 24 hours of injury, who have a Glascow Coma Scale (GCS) score of 14 or 15 on initial evaluation in the ED, and are ≥ 16 years old. Exclusion Criteria: This guideline is not intended for patients with penetrating trauma or multisystem trauma who have a GCS score of < 14 on initial evaluation in the ED and are < 16 years old. Please turn over. What You Need to Know: This guideline provides recommendations for determining which patients with a known or suspected mild TBI require a head CT and which may be safely discharged. Here are a few important points to note: There is no evidence to recommend the use of a head Discuss discharge instructions with patients and give MRI over a CT in acute evaluation. them a discharge instruction sheet to take home and share with their family and/or caregiver. Be sure to: A noncontrast head CT is indicated in head trauma patients with loss of consciousness or posttraumatic • Alert patients to look for postconcussive symptoms amnesia in presence of specific symptoms. -

Traumatic Brain Injury (TBI)
Traumatic Brain Injury (TBI) Carol A. Waldmann, MD raumatic brain injury (TBI), caused either by blunt force or acceleration/ deceleration forces, is common in the general population. Homeless persons Tare at particularly high risk of head trauma and adverse outcomes to TBI. Even mild traumatic brain injury can lead to persistent symptoms including cognitive, physical, and behavioral problems. It is important to understand brain injury in the homeless population so that appropriate referrals to specialists and supportive services can be made. Understanding the symptoms and syndromes caused by brain injury sheds light on some of the difficult behavior observed in some homeless persons. This understanding can help clinicians facilitate and guide the care of these individuals. Prevalence and Distribution recover fully, but up to 15% of patients diagnosed TBI and Mood Every year in the USA, approximately 1.5 with MTBI by a physician experience persistent Swings. million people sustain traumatic brain injury disabling problems. Up to 75% of brain injuries This man suffered (TBI), 230,000 people are hospitalized due to TBI are classified as MTBI. These injuries cost the US a gunshot wound and survive, over 50,000 people die from TBI, and almost $17 billion per year. The groups most at risk to the head and many subsequent more than 1 million people are treated in emergency for TBI are those aged 15-24 years and those aged traumatic brain rooms for TBI. In persons under the age of 45 years, 65 years and older. Men are twice as likely to sustain injuries while TBI is the leading cause of death.