Updated Mild Traumatic Brain Injury Guideline for Adults
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Diagnoses to Include in the Problem List Whenever Applicable
Diagnoses to include in the problem list whenever applicable Tips: 1. Always say acute or open when applicable 2. Always relate to the original trauma 3. Always include acid-base abnormalities, AKI due to ATN, sodium/osmolality abnormalities 4. Address in the plan of your note 5. Do NOT say possible, potential, likely… Coders can only use a real diagnosis. Make a real diagnosis. Neurological/Psych: Head: 1. Skull fracture of vault – open vs closed 2. Basilar skull fracture 3. Facial fractures 4. Nerve injury____________ 5. LOC – include duration (max duration needed is >24 hrs) and whether they returned to neurological baseline 6. Concussion with or without return to baseline consciousness 7. DAI/severe concussion with or without return to baseline consciousness 8. Type of traumatic brain injury (hemorrhages and contusions) – include size a. Tiny = <0.6 cm b. Small/moderate = 0.6-1 cm c. Large/extensive = >1 cm 9. Cerebral contusion/hemorrhage 10. Cerebral edema 11. Brainstem compression 12. Anoxic brain injury 13. Seizures 14. Brain death Spine: 1. Cervical spine fracture with (complete or incomplete) or without cord injury 2. Thoracic spine fracture with (complete or incomplete) or without cord injury 3. Lumbar spine fracture with (complete or incomplete) or without cord injury 4. Cord syndromes: central, anterior, or Brown-Sequard 5. Paraplegia or quadriplegia (any deficit in the upper extremity is consistent with quadriplegia) Cardiovascular: 1. Acute systolic heart failure 40 2. Acute diastolic heart failure 3. Chronic systolic heart failure 4. Chronic diastolic heart failure 5. Combined heart failure 6. Cardiac injury or vascular injuries 7. -

A Rare Case of Penetrating Trauma of Frontal Sinus with Anterior Table Fracture Himanshu Raval1*, Mona Bhatt2 and Nihar Gaur3
ISSN: 2643-4474 Raval et al. Neurosurg Cases Rev 2020, 3:046 DOI: 10.23937/2643-4474/1710046 Volume 3 | Issue 2 Neurosurgery - Cases and Reviews Open Access CASE REPORT Case Report: A Rare Case of Penetrating Trauma of Frontal Sinus with Anterior Table Fracture Himanshu Raval1*, Mona Bhatt2 and Nihar Gaur3 1 Department of Neurosurgery, NHL Municipal Medical College, SVP Hospital Campus, Gujarat, India Check for updates 2Medical Officer, CHC Dolasa, Gujarat, India 3GAIMS-GK General Hospital, Gujarat, India *Corresponding author: Dr. Himanshu Raval, Resident, Department of Neurosurgery, NHL Municipal Medical College, SVP Hospital Campus, Elisbridge, Ahmedabad, Gujarat, 380006, India, Tel: 942-955-3329 Abstract Introduction Background: Head injury is common component of any Road traffic accident (RTA) is the most common road traffic accident injury. Injury involving only frontal sinus cause of cranio-facial injury and involvement of frontal is uncommon and unique as its management algorithm is bone fractures are rare and constitute 5-9% of only fa- changing over time with development of radiological modal- ities as well as endoscopic intervention. Frontal sinus inju- cial trauma. The degree of association has been report- ries may range from isolated anterior table fractures causing ed to be 95% with fractures of the anterior table or wall a simple aesthetic deformity to complex fractures involving of the frontal sinuses, 60% with the orbital rims, and the frontal recess, orbits, skull base, and intracranial con- 60% with complex injuries of the naso-orbital-ethmoid tents. Only anterior table injury of frontal sinus is rare in pen- region, 33% with other orbital wall fractures and 27% etrating head injury without underlying brain injury with his- tory of unconsciousness and questionable convulsion which with Le Fort level fractures. -

Cervical Spine Injury Risk Factors in Children with Blunt Trauma Julie C
Cervical Spine Injury Risk Factors in Children With Blunt Trauma Julie C. Leonard, MD, MPH,a Lorin R. Browne, DO,b Fahd A. Ahmad, MD, MSCI,c Hamilton Schwartz, MD, MEd,d Michael Wallendorf, PhD,e Jeffrey R. Leonard, MD,f E. Brooke Lerner, PhD,b Nathan Kuppermann, MD, MPHg BACKGROUND: Adult prediction rules for cervical spine injury (CSI) exist; however, pediatric rules abstract do not. Our objectives were to determine test accuracies of retrospectively identified CSI risk factors in a prospective pediatric cohort and compare them to a de novo risk model. METHODS: We conducted a 4-center, prospective observational study of children 0 to 17 years old who experienced blunt trauma and underwent emergency medical services scene response, trauma evaluation, and/or cervical imaging. Emergency department providers recorded CSI risk factors. CSIs were classified by reviewing imaging, consultations, and/or telephone follow-up. We calculated bivariable relative risks, multivariable odds ratios, and test characteristics for the retrospective risk model and a de novo model. RESULTS: Of 4091 enrolled children, 74 (1.8%) had CSIs. Fourteen factors had bivariable associations with CSIs: diving, axial load, clotheslining, loss of consciousness, neck pain, inability to move neck, altered mental status, signs of basilar skull fracture, torso injury, thoracic injury, intubation, respiratory distress, decreased oxygen saturation, and neurologic deficits. The retrospective model (high-risk motor vehicle crash, diving, predisposing condition, neck pain, decreased neck mobility (report or exam), altered mental status, neurologic deficits, or torso injury) was 90.5% (95% confidence interval: 83.9%–97.2%) sensitive and 45.6% (44.0%–47.1%) specific for CSIs. -

Anesthesia for Trauma
Anesthesia for Trauma Maribeth Massie, CRNA, MS Staff Nurse Anesthetist, The Johns Hopkins Hospital Assistant Professor/Assistant Program Director Columbia University School of Nursing Program in Nurse Anesthesia OVERVIEW • “It’s not the speed which kills, it’s the sudden stop” Epidemiology of Trauma • ~8% worldwide death rate • Leading cause of death in Americans from 1- 45 years of age • MVC’s leading cause of death • Blunt > penetrating • Often drug abusers, acutely intoxicated, HIV and Hepatitis carriers Epidemiology of Trauma • “Golden Hour” – First hour after injury – 50% of patients die within the first seconds to minutesÆ extent of injuries – 30% of patients die in next few hoursÆ major hemorrhage – Rest may die in weeks Æ sepsis, MOSF Pre-hospital Care • ABC’S – Initial assessment and BLS in trauma – GO TEAM: role of CRNA’s at Maryland Shock Trauma Center • Resuscitation • Reduction of fractures • Extrication of trapped victims • Amputation • Uncooperative patients Initial Management Plan • Airway maintenance with cervical spine protection • Breathing: ventilation and oxygenation • Circulation with hemorrhage control • Disability • Exposure Initial Assessment • Primary Survey: – AIRWAY • ALWAYS ASSUME A CERVICAL SPINE INJURY EXISTS UNTIL PROVEN OTHERWISE • Provide MANUAL IN-LINE NECK STABILIZATION • Jaw-thrust maneuver Initial Assessment • Airway cont’d: – Cervical spine evaluation • Cross table lateral and swimmer’s view Xray • Need to see all seven cervical vertebrae • Only negative CT scan R/O injury Initial Assessment • Cervical -

CASE REPORT Injuries Following Segway Personal
UC Irvine Western Journal of Emergency Medicine: Integrating Emergency Care with Population Health Title Injuries Following Segway Personal Transporter Accidents: Case Report and Review of the Literature Permalink https://escholarship.org/uc/item/37r4387d Journal Western Journal of Emergency Medicine: Integrating Emergency Care with Population Health, 16(5) ISSN 1936-900X Authors Ashurst, John Wagner, Benjamin Publication Date 2015 DOI 10.5811/westjem.2015.7.26549 License https://creativecommons.org/licenses/by/4.0/ 4.0 Peer reviewed eScholarship.org Powered by the California Digital Library University of California CASE REPORT Injuries Following Segway Personal Transporter Accidents: Case Report and Review of the Literature John Ashurst DO, MSc Conemaugh Memorial Medical Center, Department of Emergency Medicine, Benjamin Wagner, DO Johnstown, Pennsylvania Section Editor: Rick A. McPheeters, DO Submission history: Submitted April 20, 2015; Accepted July 9, 2015 Electronically published October 20, 2015 Full text available through open access at http://escholarship.org/uc/uciem_westjem DOI: 10.5811/westjem.2015.7.26549 The Segway® self-balancing personal transporter has been used as a means of transport for sightseeing tourists, military, police and emergency medical personnel. Only recently have reports been published about serious injuries that have been sustained while operating this device. This case describes a 67-year-old male who sustained an oblique fracture of the shaft of the femur while using the Segway® for transportation around his community. We also present a review of the literature. [West J Emerg Med. 2015;16(5):693-695.] INTRODUCTION no parasthesia was noted. In 2001, Dean Kamen developed a self-balancing, zero Radiograph of the right femur demonstrated an oblique emissions personal transportation vehicle, known as the fracture of the proximal shaft of the femur with severe Segway® Personal Transporter (PT).1 The Segway’s® top displacement and angulation (Figure). -
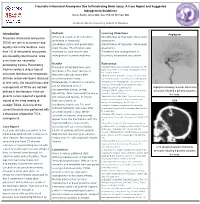
Traumatic Intracranial Aneurysms Due to Penetrating Brain Injury. a Case Report and Suggested Management Guidelines Breck Aaron Jones MD; Alex Patrick Michael MD
Traumatic Intracranial Aneurysms Due to Penetrating Brain Injury. A Case Report and Suggested Management Guidelines Breck Aaron Jones MD; Alex Patrick Michael MD Southern Illinois University School of Medicine Methods Learning Objectives Introduction Angiogram Traumatic intracranial aneurysms A Pubmed search of the literature Identification of traumatic intracranial pertaining to traumatic aneurysms. (TICA) are rare in occurrence and pseudoaneurysms and penetrating Classification of traumatic intracranial equally rare in the literature. Less brain trauma. The literature was aneurysms. than 1% of intracranial aneurysms reviewed for case reports and Treatment and management of are caused by blunt trauma, while management recommendations. traumatic intracranial aneurysms. even fewer are caused by penetrating trauma. Penetrating Results References Traumatic intracranial aneurysm 1.Aarabi B. Management of traumatic aneurysms caused by trauma creates a unique type of high-velocity missile head wounds. Neurosurg Clin N Am. formation is the most commonly aneurysm that does not incorporate Oct 1995;6(4):775-797. described vascular injury after 2.Rao GP, Rao NS, Reddy PK. Technique of removal of an all three vessel wall layers. Because penetrating brain injury. impacted sharp object in a penetrating head injury using the of their rarity, the natural history and Histologically, traumatic aneurysms lever principle. Br J Neurosurg. Dec 1998;12(6):569-571. 3.Vascular complications of penetrating brain injury. J can be described as true management of TICAs are not well Trauma. Aug 2001;51(2 Suppl):S26-28. Angiogram showing traumatic intracranial (incorporating intima, media, defined in the literature. Here we 4.Crompton MR. The pathogenesis of cerebral aneurysms. aneurysm following a gunshot wound to adventitia), false (incorporating one or Brain. -

In Drivers of Open-Wheel Open Cockpit Race Cars
SPORTS MEDICINE SPINE FRACTURES IN DRIVERS OF OPEN-WHEEL OPEN COCKPIT RACE CARS – Written by Terry Trammell and Kathy Flint, USA This paper is intended to explain the mechanisms responsible for production of spinal fracture in the driver of an open cockpit single seat, open-wheel racing car (Indy Car) and what can be done to lessen the risk of fracture. In a report of fractures in multiple racing • Seated angle (approximately 45°) • Lumbar spine flexed series drivers (Championship Auto Racing • Hips and knees flexed • Seated semi-reclining Cars [CART]/Champ cars, Toyota Atlantics, Indy Racing League [IRL], Indy Lights and Figure 1: Body alignment in the Indy Car. Formula 1 [F1]), full details of the crash and mechanism of injury were captured and analysed. This author was the treating physician in all cases from 1996 to 2011. All images, medical records, data available BASILAR SKULL FRACTURE Use of this specific safety feature from the Accident Data Recorder-2 (ADR), Following a fatal distractive basilar is compulsory in most professional crash video, specific on track information, skull fracture in 1999, the Head and Neck motorsport sanctions and has resulted in a post-accident investigation of damage and Support (HANS) device was introduced into dramatic reduction to near elimination of direction of major impact correlated with Indy Cars. Basilar skull fracture occurs when fatal basilar skull fractures. No basilar skull ADR-2 data were analysed. Results provided neck tension exceeds 3113.75 N forces. fractures have occurred in the IRL since the groundwork for understanding spine No data demonstrates that HANS introduction of the HANS and since 2006 fracture and forces applied to the driver in predisposes the wearer to other cervical there has been only one cervical fracture. -

Diagnosis and Treatment of Cerebrospinal Fluid Rhinorrhea Following Accidental Traumatic Anterior Skull Base Fractures
Neurosurg Focus 32 (6):E3, 2012 Diagnosis and treatment of cerebrospinal fluid rhinorrhea following accidental traumatic anterior skull base fractures MATEO ZIU, M.D., JENNIFER GENTRY SAVAGE, M.D., AND DAVID F. JIMENEZ, M.D. Department of Neurosurgery, University of Texas Health Science Center at San Antonio, Texas Cerebrospinal fluid rhinorrhea is a serious and potentially fatal condition because of an increased risk of menin- gitis and brain abscess. Approximately 80% of all cases occur in patients with head injuries and craniofacial fractures. Despite technical advances in the diagnosis and management of CSF rhinorrhea caused by craniofacial injury through the introduction of MRI and endoscopic extracranial surgical approaches, difficulties remain. The authors review here the pathophysiology, diagnosis, and management of CSF rhinorrhea relevant exclusively to traumatic anterior skull base injuries and attempt to identify areas in which further work is needed. (http://thejns.org/doi/abs/10.3171/2012.4.FOCUS1244) KEY WORDS • craniomaxillofacial trauma • head trauma • cerebrospinal fluid rhinorrhea • meningitis • dural repair • endoscopic surgery • skull base fracture EREBROSPINAL fluid rhinorrhea is a serious and po- Furthermore, the issues related to CSF leak caused tentially fatal condition that still presents a major by traumatic injury are complex and multiple. Having challenge in terms of its diagnosis and manage- conducted a thorough review of existing literature, we Cment. It is estimated that meningitis develops in approxi- discuss here the pathophysiology, diagnosis, and man- mately 10%–25% of patients with this disorder, and 10% agement of CSF rhinorrhea relevant to traumatic anterior of them die as a result. Approximately 80% of all cases of skull base injuries and attempt to identify areas in which CSF rhinorrhea are caused by head injuries that are asso- further research is needed. -

Prehospital Spine Immobilization for Penetrating Trauma—Review and Recommendations from the Prehospital Trauma Life Support Executive Committee
REVIEW ARTICLE Prehospital Spine Immobilization for Penetrating Trauma—Review and Recommendations From the Prehospital Trauma Life Support Executive Committee Lance E. Stuke, MD, MPH, Peter T. Pons, MD, Jeffrey S. Guy, MD, MSc, MMHC, Will P. Chapleau, RN, EMT-P, Frank K. Butler, MD, Capt MC USN (Ret), and Norman E. McSwain, MD pine immobilization in trauma patients suspected of hav- In the case of penetrating injuries, delays in transport Sing a spinal injury has been a cornerstone of prehospital prolong the time before patients receive the prompt surgical treatment for decades. Current practices are based on the care needed to arrest hemorrhage. Even with experienced belief that a patient with an injured spinal column can prehospital providers, spine immobilization is time consum- deteriorate neurologically without immobilization. Most ing. The time required for experienced emergency medical treatment protocols do not differentiate between blunt and technicians to properly immobilize a cervical spine has been penetrating mechanisms of injury. Current Emergency Med- reported to be 5.64 minutes (Ϯ1.49 minutes).6 This scene ical Service (EMS) protocols for spinal immobilization of delay can be catastrophic for a patient with penetrating penetrating trauma are based on historic practices rather than trauma requiring urgent surgical intervention for airway com- scientific merits. Although blunt spinal column injuries will promise or hemorrhage. Studies have demonstrated that cervical collars increase occasionally produce unstable vertebral -

Deaths from Abdominal Trauma: Analysis of 1888 Forensic Autopsies
DOI: 10.1590/0100-69912017006006 Original Article Deaths from abdominal trauma: analysis of 1888 forensic autopsies Óbitos por trauma abdominal: análise de 1888 autopsias médico-legais POLYANNA HELENA COELHO BORDONI1; DANIELA MAGALHÃES MOREIRA DOS SANTOS2; JAÍSA SANTANA TEIXEIRA2; LEONARDO SANTOS BORDONI2-4. ABSTRACT Objective: to evaluate the epidemiological profile of deaths due to abdominal trauma at the Forensic Medicine Institute of Belo Horizonte, MG - Brazil. Methods: we conducted a retrospective study of the reports of deaths due to abdominal trauma autopsied from 2006 to 2011. Results: we analyzed 1.888 necropsy reports related to abdominal trauma. Penetrating trauma was more common than blunt one and gun- shot wounds were more prevalent than stab wounds. Most of the individuals were male, brown-skinned, single and occupationally active. The median age was 34 years. The abdominal organs most injured in the penetrating trauma were the liver and the intestines, and in blunt trauma, the liver and the spleen. Homicide was the most prevalent circumstance of death, followed by traffic accidents, and almost half of the cases were referred to the Forensic Medicine Institute by a health unit. The blood alcohol test was positive in a third of the necropsies where it was performed. Cocaine and marijuana were the most commonly found substances in toxicology studies. Conclusion: in this sam- ple. there was a predominance of penetrating abdominal trauma in young, brown and single men, the liver being the most injured organ. Keywords: Autopsy. Forensic Medicine. Homicide. Abdominal Injuries. INTRODUCTION In addition, the accuracy of abdominal phy- sical examination is low and the level of consciousness eaths from external causes represent the second produced by hemorrhages or by the association of ab- Dleading cause of mortality in Brazil and the main dominal trauma (AT) with traumatic brain injury and/or cause when considering individuals under the age of effects of central nervous system of previously consu- 351. -

Western Trauma Association Critical Decisions in Trauma: Penetrating Chest Trauma
WTA 2014 ALGORITHM Western Trauma Association Critical Decisions in Trauma: Penetrating chest trauma Riyad Karmy-Jones, MD, Nicholas Namias, MD, Raul Coimbra, MD, Ernest E. Moore, MD, 09/30/2020 on BhDMf5ePHKav1zEoum1tQfN4a+kJLhEZgbsIHo4XMi0hCywCX1AWnYQp/IlQrHD3Ypodx1mzGi19a2VIGqBjfv9YfiJtaGCC1/kUAcqLCxGtGta0WPrKjA== by http://journals.lww.com/jtrauma from Downloaded Martin Schreiber, MD, Robert McIntyre, Jr., MD, Martin Croce, MD, David H. Livingston, MD, Jason L. Sperry, MD, Ajai K. Malhotra, MD, and Walter L. Biffl, MD, Portland, Oregon Downloaded from http://journals.lww.com/jtrauma his is a recommended algorithm of the Western Trauma Historical Perspective TAssociation for the acute management of penetrating chest The precise incidence of penetrating chest injury, varies injury. Because of the paucity of recent prospective randomized depending on the urban environment and the nature of the trials on the evaluation and management of penetrating chest review. Overall, penetrating chest injuries account for 1% to injury, the current algorithms and recommendations are based 13% of trauma admissions, and acute exploration is required in by on available published cohort, observational and retrospective BhDMf5ePHKav1zEoum1tQfN4a+kJLhEZgbsIHo4XMi0hCywCX1AWnYQp/IlQrHD3Ypodx1mzGi19a2VIGqBjfv9YfiJtaGCC1/kUAcqLCxGtGta0WPrKjA== 5% to 15% of cases; exploration is required in 15% to 30% of studies, and the expert opinion of the Western Trauma Asso- patients who are unstable or in whom active hemorrhage is ciation members. The two algorithms should be reviewed in the suspected. Among patients managed by tube thoracostomy following sequence: Figure 1 for the management and damage- alone, complications including retained hemothorax, empy- control strategies in the unstable patient and Figure 2 for the ema, persistent air leak, and/or occult diaphragmatic injuries management and definitive repair strategies in the stable patient. -

ABC Ofmajor' Trauma ABDOMINAL TRAUMA BMJ: First Published As 10.1136/Bmj.301.6744.172 on 21 July 1990
ABC ofMajor' Trauma ABDOMINAL TRAUMA BMJ: first published as 10.1136/bmj.301.6744.172 on 21 July 1990. Downloaded from Andrew Cope, William Stebbings The aim ofthis article is to enable all those concerned with the management of patients with abdominal trauma to perform a thorough examination and assessment with the help of diagnostic tests and to institute safe and correct treatment. Intra-abdominal injuries carry a high morbidity and mortality because they are often not detected or their severity is underestimated. This is particularly common in cases of blunt trauma, in which there may be few or no external signs. Always have a high index ofsuspicion ofabdominal injury when the history suggests severe trauma. Traditionally, abdominal trauma is classified as either blunt or penetrating, but the initial assessment and, if required, resuscitation are essentially the same. Blunt trauma Road traffic accidents are one of the commonest causes of blunt injuries. Since wearing seat belts was made compulsory the number of fatal head injuries has declined, but a pattern of blunt abdominal trauma that is specific to seat belts has emerged. This often includes avulsion injuries of the mesentery of the small bowel. The symptoms and signs of blunt abdominal trauma can be subtle, and consequently diagnosis is difficult. A high degree of suspicion of underlying intra-abdominal injury must be adopted when dealing with blunt trauma. Blunt abdominal trauma is -usually associated with trauma to other areas, especially the head, chest, http://www.bmj.com/ .. , :and pelvis. Penetrating trauma Penetrating wounds are either due to low velocity projectiles such as on 1 October 2021 by guest.