Deaths from Abdominal Trauma: Analysis of 1888 Forensic Autopsies
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

A Rare Case of Penetrating Trauma of Frontal Sinus with Anterior Table Fracture Himanshu Raval1*, Mona Bhatt2 and Nihar Gaur3
ISSN: 2643-4474 Raval et al. Neurosurg Cases Rev 2020, 3:046 DOI: 10.23937/2643-4474/1710046 Volume 3 | Issue 2 Neurosurgery - Cases and Reviews Open Access CASE REPORT Case Report: A Rare Case of Penetrating Trauma of Frontal Sinus with Anterior Table Fracture Himanshu Raval1*, Mona Bhatt2 and Nihar Gaur3 1 Department of Neurosurgery, NHL Municipal Medical College, SVP Hospital Campus, Gujarat, India Check for updates 2Medical Officer, CHC Dolasa, Gujarat, India 3GAIMS-GK General Hospital, Gujarat, India *Corresponding author: Dr. Himanshu Raval, Resident, Department of Neurosurgery, NHL Municipal Medical College, SVP Hospital Campus, Elisbridge, Ahmedabad, Gujarat, 380006, India, Tel: 942-955-3329 Abstract Introduction Background: Head injury is common component of any Road traffic accident (RTA) is the most common road traffic accident injury. Injury involving only frontal sinus cause of cranio-facial injury and involvement of frontal is uncommon and unique as its management algorithm is bone fractures are rare and constitute 5-9% of only fa- changing over time with development of radiological modal- ities as well as endoscopic intervention. Frontal sinus inju- cial trauma. The degree of association has been report- ries may range from isolated anterior table fractures causing ed to be 95% with fractures of the anterior table or wall a simple aesthetic deformity to complex fractures involving of the frontal sinuses, 60% with the orbital rims, and the frontal recess, orbits, skull base, and intracranial con- 60% with complex injuries of the naso-orbital-ethmoid tents. Only anterior table injury of frontal sinus is rare in pen- region, 33% with other orbital wall fractures and 27% etrating head injury without underlying brain injury with his- tory of unconsciousness and questionable convulsion which with Le Fort level fractures. -

Thoracic and Abdominal Trauma
INJURIESINJURIES TOTO THETHE TRUNKTRUNK THROACIC AND ABDOMINAL INJURIES INITIALINITIAL ASSESSMENTASSESSMENT 1. PRIMARY SURVEY (1. MIN) 2. VITAL FUNCTIONS TREAT LIFE THREATENING FIRST 3. SECONDARY SURVEY 4. DEFINITIVE CARE A.B.C.D.E. LIFELIFE THREATENINGTHREATENING INJURIESINJURIES A. INJURIES TO THE AIRWAYS B. TENSION PTX SUCKING CHEST WOUND MASSIVE HEMOTHORAX FLAIL CHEST C. CARDIAC TAMPONADE MASSIVE HEMOTHORAX LIFELIFE THREATENINGTHREATENING CHESTCHEST INJURIESINJURIES •PNEUMOTHORAX •HEMOTHORAX •PULMONARY CONTUSION •TRACHEBRONCHIAL TREE INJURY •BLUNT CARDIAC INJURY •TRAUMATIC AORTIC INJURY •TRAMATIC DIAPHRAGMATIG INJURY •MEDIASTINAL TRANSVERSING WOUNDS PNEUMOTHORAXPNEUMOTHORAX AIR BETWEEN THE PARIETAL AND VISCERAL PLEURA RIB FRACTURES INJURIES TO THE LUNG INJURIES TO THE AIRWAYS BULLAS IATROGENIG FROM THE RETROPERITONEUM PNEUMOTHORAXPNEUMOTHORAX 1. 2. TENSIONTENSION PNEUMOTHORAXPNEUMOTHORAX ONE WAY VALVE – AIR FROM THE LUNG OR THROUGH THE CHEST WALL INTO THE THORACIC CAVITY CONSEQUENCE: HYPOXIA, BLOCKING OF THE VENOUS INFLOW CHEST PAIN, AIR HUNGER, HYPOTENSION, NECK VEIN DISTENSION, TACHYCARDIA CARDIAC TAMPONADE – NO BREATH SOUNDS IMMEDIATE TREATMENT TENSIONTENSION PNEUMOTHORAXPNEUMOTHORAX TENSION PTX NEEDLE THORACOCENTESIS HEMOTHORAXHEMOTHORAX BLOOD IN THE THORACIC CAVITY LUNG LACERATION RIB FRACTURE INTERCOSTAL VESSEL INJURY ART. MAMMARY INJURY PENETRATING OR BLUNT INJURY HEMOTHORAXHEMOTHORAX 1. ? 2. ! HTXHTX HEMOTHORAXHEMOTHORAX TREATMENT : CHEST TUBE – THORACOTOMY IS RARELY INDICATED THORACOTOMY: 1500 ML / DRAINAGE OR 200 ML/ HOUR -

Anesthesia for Trauma
Anesthesia for Trauma Maribeth Massie, CRNA, MS Staff Nurse Anesthetist, The Johns Hopkins Hospital Assistant Professor/Assistant Program Director Columbia University School of Nursing Program in Nurse Anesthesia OVERVIEW • “It’s not the speed which kills, it’s the sudden stop” Epidemiology of Trauma • ~8% worldwide death rate • Leading cause of death in Americans from 1- 45 years of age • MVC’s leading cause of death • Blunt > penetrating • Often drug abusers, acutely intoxicated, HIV and Hepatitis carriers Epidemiology of Trauma • “Golden Hour” – First hour after injury – 50% of patients die within the first seconds to minutesÆ extent of injuries – 30% of patients die in next few hoursÆ major hemorrhage – Rest may die in weeks Æ sepsis, MOSF Pre-hospital Care • ABC’S – Initial assessment and BLS in trauma – GO TEAM: role of CRNA’s at Maryland Shock Trauma Center • Resuscitation • Reduction of fractures • Extrication of trapped victims • Amputation • Uncooperative patients Initial Management Plan • Airway maintenance with cervical spine protection • Breathing: ventilation and oxygenation • Circulation with hemorrhage control • Disability • Exposure Initial Assessment • Primary Survey: – AIRWAY • ALWAYS ASSUME A CERVICAL SPINE INJURY EXISTS UNTIL PROVEN OTHERWISE • Provide MANUAL IN-LINE NECK STABILIZATION • Jaw-thrust maneuver Initial Assessment • Airway cont’d: – Cervical spine evaluation • Cross table lateral and swimmer’s view Xray • Need to see all seven cervical vertebrae • Only negative CT scan R/O injury Initial Assessment • Cervical -
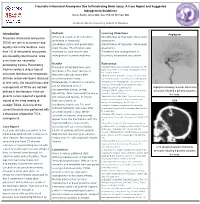
Traumatic Intracranial Aneurysms Due to Penetrating Brain Injury. a Case Report and Suggested Management Guidelines Breck Aaron Jones MD; Alex Patrick Michael MD
Traumatic Intracranial Aneurysms Due to Penetrating Brain Injury. A Case Report and Suggested Management Guidelines Breck Aaron Jones MD; Alex Patrick Michael MD Southern Illinois University School of Medicine Methods Learning Objectives Introduction Angiogram Traumatic intracranial aneurysms A Pubmed search of the literature Identification of traumatic intracranial pertaining to traumatic aneurysms. (TICA) are rare in occurrence and pseudoaneurysms and penetrating Classification of traumatic intracranial equally rare in the literature. Less brain trauma. The literature was aneurysms. than 1% of intracranial aneurysms reviewed for case reports and Treatment and management of are caused by blunt trauma, while management recommendations. traumatic intracranial aneurysms. even fewer are caused by penetrating trauma. Penetrating Results References Traumatic intracranial aneurysm 1.Aarabi B. Management of traumatic aneurysms caused by trauma creates a unique type of high-velocity missile head wounds. Neurosurg Clin N Am. formation is the most commonly aneurysm that does not incorporate Oct 1995;6(4):775-797. described vascular injury after 2.Rao GP, Rao NS, Reddy PK. Technique of removal of an all three vessel wall layers. Because penetrating brain injury. impacted sharp object in a penetrating head injury using the of their rarity, the natural history and Histologically, traumatic aneurysms lever principle. Br J Neurosurg. Dec 1998;12(6):569-571. 3.Vascular complications of penetrating brain injury. J can be described as true management of TICAs are not well Trauma. Aug 2001;51(2 Suppl):S26-28. Angiogram showing traumatic intracranial (incorporating intima, media, defined in the literature. Here we 4.Crompton MR. The pathogenesis of cerebral aneurysms. aneurysm following a gunshot wound to adventitia), false (incorporating one or Brain. -

Characteristics and Management of Penetrating Abdominal Injuries in a German Level I Trauma Center
European Journal of Trauma and Emergency Surgery (2019) 45:315–321 https://doi.org/10.1007/s00068-018-0911-1 ORIGINAL ARTICLE Characteristics and management of penetrating abdominal injuries in a German level I trauma center Patrizia Malkomes1 · Philipp Störmann2 · Hanan El Youzouri1 · Sebastian Wutzler2 · Ingo Marzi2 · Thomas Vogl3 · Wolf Otto Bechstein1 · Nils Habbe4 Received: 19 October 2017 / Accepted: 13 January 2018 / Published online: 22 January 2018 © Springer-Verlag GmbH Germany, part of Springer Nature 2018 Abstract Purpose Penetrating abdominal injuries caused by stabbing or firearms are rare in Germany, thus there is lack of descriptive studies. The management of hemodynamically stable patients is still under dispute. The aim of this study is to review and improve our management of penetrating abdominal injuries. Methods We retrospectively reviewed a 10-year period from the Trauma Registry of our level I trauma center. The data of all patients regarding demographics, clinical and outcome parameters were examined. Further, charts were reviewed for FAST and CT results and correlated with intraoperative findings. Results A total of 115 patients with penetrating abdominal trauma (87.8% men) were analyzed. In 69 patients, the injuries were caused by interpersonal violence and included 88 stab and 4 firearm wounds. 8 patients (6.9%) were in a state of shock at presentation. 52 patients (44.8%) suffered additional extraabdominal injuries. 38 patients were managed non-operatively, while almost two-thirds of all patients underwent surgical treatment. Hereof, 20 laparoscopies and 3 laparotomies were non- therapeutic. There were two missed injuries, but no patient experienced morbidity or mortality related to delay in treatment. -

Prehospital Spine Immobilization for Penetrating Trauma—Review and Recommendations from the Prehospital Trauma Life Support Executive Committee
REVIEW ARTICLE Prehospital Spine Immobilization for Penetrating Trauma—Review and Recommendations From the Prehospital Trauma Life Support Executive Committee Lance E. Stuke, MD, MPH, Peter T. Pons, MD, Jeffrey S. Guy, MD, MSc, MMHC, Will P. Chapleau, RN, EMT-P, Frank K. Butler, MD, Capt MC USN (Ret), and Norman E. McSwain, MD pine immobilization in trauma patients suspected of hav- In the case of penetrating injuries, delays in transport Sing a spinal injury has been a cornerstone of prehospital prolong the time before patients receive the prompt surgical treatment for decades. Current practices are based on the care needed to arrest hemorrhage. Even with experienced belief that a patient with an injured spinal column can prehospital providers, spine immobilization is time consum- deteriorate neurologically without immobilization. Most ing. The time required for experienced emergency medical treatment protocols do not differentiate between blunt and technicians to properly immobilize a cervical spine has been penetrating mechanisms of injury. Current Emergency Med- reported to be 5.64 minutes (Ϯ1.49 minutes).6 This scene ical Service (EMS) protocols for spinal immobilization of delay can be catastrophic for a patient with penetrating penetrating trauma are based on historic practices rather than trauma requiring urgent surgical intervention for airway com- scientific merits. Although blunt spinal column injuries will promise or hemorrhage. Studies have demonstrated that cervical collars increase occasionally produce unstable vertebral -

Updated Mild Traumatic Brain Injury Guideline for Adults
Heads Up to Clinicians: Updated Mild Traumatic Brain Injury Guideline for Adults This Guideline is based on the 2008 Mild TBI Clinical Policy for adults, which revises the previous 2002 Clinical Policy. To help improve diagnosis, treatment, and outcomes for patients with mild TBI, it is critical that you become familiar with this guideline. The guideline is especially important for clinicians working in hospital-based emergency care. Inclusion Criteria: This guideline is intended for patients with non-penetrating trauma to the head who present to the ED within 24 hours of injury, who have a Glascow Coma Scale (GCS) score of 14 or 15 on initial evaluation in the ED, and are ≥ 16 years old. Exclusion Criteria: This guideline is not intended for patients with penetrating trauma or multisystem trauma who have a GCS score of < 14 on initial evaluation in the ED and are < 16 years old. Please turn over. What You Need to Know: This guideline provides recommendations for determining which patients with a known or suspected mild TBI require a head CT and which may be safely discharged. Here are a few important points to note: There is no evidence to recommend the use of a head Discuss discharge instructions with patients and give MRI over a CT in acute evaluation. them a discharge instruction sheet to take home and share with their family and/or caregiver. Be sure to: A noncontrast head CT is indicated in head trauma patients with loss of consciousness or posttraumatic • Alert patients to look for postconcussive symptoms amnesia in presence of specific symptoms. -

Western Trauma Association Critical Decisions in Trauma: Penetrating Chest Trauma
WTA 2014 ALGORITHM Western Trauma Association Critical Decisions in Trauma: Penetrating chest trauma Riyad Karmy-Jones, MD, Nicholas Namias, MD, Raul Coimbra, MD, Ernest E. Moore, MD, 09/30/2020 on BhDMf5ePHKav1zEoum1tQfN4a+kJLhEZgbsIHo4XMi0hCywCX1AWnYQp/IlQrHD3Ypodx1mzGi19a2VIGqBjfv9YfiJtaGCC1/kUAcqLCxGtGta0WPrKjA== by http://journals.lww.com/jtrauma from Downloaded Martin Schreiber, MD, Robert McIntyre, Jr., MD, Martin Croce, MD, David H. Livingston, MD, Jason L. Sperry, MD, Ajai K. Malhotra, MD, and Walter L. Biffl, MD, Portland, Oregon Downloaded from http://journals.lww.com/jtrauma his is a recommended algorithm of the Western Trauma Historical Perspective TAssociation for the acute management of penetrating chest The precise incidence of penetrating chest injury, varies injury. Because of the paucity of recent prospective randomized depending on the urban environment and the nature of the trials on the evaluation and management of penetrating chest review. Overall, penetrating chest injuries account for 1% to injury, the current algorithms and recommendations are based 13% of trauma admissions, and acute exploration is required in by on available published cohort, observational and retrospective BhDMf5ePHKav1zEoum1tQfN4a+kJLhEZgbsIHo4XMi0hCywCX1AWnYQp/IlQrHD3Ypodx1mzGi19a2VIGqBjfv9YfiJtaGCC1/kUAcqLCxGtGta0WPrKjA== 5% to 15% of cases; exploration is required in 15% to 30% of studies, and the expert opinion of the Western Trauma Asso- patients who are unstable or in whom active hemorrhage is ciation members. The two algorithms should be reviewed in the suspected. Among patients managed by tube thoracostomy following sequence: Figure 1 for the management and damage- alone, complications including retained hemothorax, empy- control strategies in the unstable patient and Figure 2 for the ema, persistent air leak, and/or occult diaphragmatic injuries management and definitive repair strategies in the stable patient. -

ABC Ofmajor' Trauma ABDOMINAL TRAUMA BMJ: First Published As 10.1136/Bmj.301.6744.172 on 21 July 1990
ABC ofMajor' Trauma ABDOMINAL TRAUMA BMJ: first published as 10.1136/bmj.301.6744.172 on 21 July 1990. Downloaded from Andrew Cope, William Stebbings The aim ofthis article is to enable all those concerned with the management of patients with abdominal trauma to perform a thorough examination and assessment with the help of diagnostic tests and to institute safe and correct treatment. Intra-abdominal injuries carry a high morbidity and mortality because they are often not detected or their severity is underestimated. This is particularly common in cases of blunt trauma, in which there may be few or no external signs. Always have a high index ofsuspicion ofabdominal injury when the history suggests severe trauma. Traditionally, abdominal trauma is classified as either blunt or penetrating, but the initial assessment and, if required, resuscitation are essentially the same. Blunt trauma Road traffic accidents are one of the commonest causes of blunt injuries. Since wearing seat belts was made compulsory the number of fatal head injuries has declined, but a pattern of blunt abdominal trauma that is specific to seat belts has emerged. This often includes avulsion injuries of the mesentery of the small bowel. The symptoms and signs of blunt abdominal trauma can be subtle, and consequently diagnosis is difficult. A high degree of suspicion of underlying intra-abdominal injury must be adopted when dealing with blunt trauma. Blunt abdominal trauma is -usually associated with trauma to other areas, especially the head, chest, http://www.bmj.com/ .. , :and pelvis. Penetrating trauma Penetrating wounds are either due to low velocity projectiles such as on 1 October 2021 by guest. -

Secondary Abdominal Compartment Syndrome Following Severe Extremity Injury: Unavoidable Or Unnecessary?
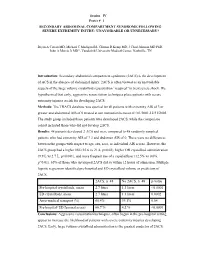
Session IV Poster # 1 SECONDARY ABDOMINAL COMPARTMENT SYNDROME FOLLOWING SEVERE EXTREMITY INJURY: UNAVOIDABLE OR UNNECESSARY? Bryan A Cotton MD, Michael C Madigan BS, Clinton D Kemp MD, J Chad Johnson MD PhD, John A Morris Jr MD*, Vanderbilt University Medical Center, Nashville, TN Introduction: Secondary abdominal compartment syndrome (2ACS) is the development of ACS in the absence of abdominal injury. 2ACS is often viewed as an unavoidable sequela of the large volume crystalloid resuscitation “required” to treat severe shock. We hypothesized that early, aggressive resuscitation techniques place patients with severe extremity injuries at risk for developing 2ACS. Methods: The TRACS database was queried for all patients with extremity AIS of 3 or greater and abdominal AIS of 0 treated at our institution between 01/01/2001-12/31/2005. The study group included those patients who developed 2ACS, while the comparison cohort included those who did not develop 2ACS. Results: 48 patients developed 2 ACS and were compared to 48 randomly sampled patients who had extremity AIS of ? 3 and abdomen AIS of 0. There were no differences between the groups with respect to age, sex, race, or individual AIS scores. However, the 2ACS group had a higher ISS (25.6 vs 21.4, p=0.02), higher OR crystalloid administration (9.9 L vs 2.7 L, p<0.001), and more frequent use of a rapid infuser (12.5% vs 0.0%, p=0.01). 65% of those who developed 2ACS did so within 12 hours of admission. Multiple logistic regression identified pre-hospital and ED crystalloid volume as predictors of 2ACS. -

Blunt Abdominal Trauma
TRM 05.03 BLUNT ABDOMINAL TRAUMA Trauma Service Guidelines Title: Blunt Abdominal Trauma Developed by: Y. Cho, R. Judson, K. Gumm, R. Santos, M. Walsh, D. Pascoe & ACT Created: Version 1.0 July 2012 Revised by: C. Kozul, R. Judson, K. Gumm, R. Santos, M. Walsh, D. Pascoe & ACT Revised: Version 2.0 August 2017 Table of Content Introduction ...................................................................................................................................................................1 Diagnosis of an abdominal injury:.............................................................................................................................1 Decision making in BAT:..............................................................................................................................................2 Management of haemodynamically unstable patients SBP <90mmHg .......................................................2 Management of haemodynamically stable patients.......................................................................................3 Serial Abdominal Examinations .......................................................................................................................3 Patients with no findings on CT.........................................................................................................................4 Operative management:............................................................................................................................................4 Laparotomy -

Penetrating Vascular Injuries of the Face and Neck: Clinical and Angiographic Correlation
855 Penetrating Vascular Injuries of the Face and Neck: Clinical and Angiographic Correlation Charles M. North 1. 2 A retrospective review was made of 139 clinically stable patients who had sustained Jamshid Ahmadi penetrating trauma to the face and neck. The study was done to learn more about the Hervey D. Segall indications for angiography and the impact of angiography upon patient management. Chi-Shing Zee Some relationship between the physical examination and the angiographic findings was found. In the presence of anyone of four physical signs or symptoms (absent pulse, bruit, hematoma, or alteration of neurologic status) there was a 30% incidence of vascular injury. However, it is unlikely that a clinically significant traumatic vascular lesion will be missed if angiography is not obtained when these clinical signs and symptoms are not present. In the group of 78 patients who presented with only a wound penetrating the ' platysma and no other findings or symptoms, just two had vascular injuries on angiograms; one of these lesions was minor and the other did not affect the patient's management. There was a substantially higher rate (50%) of vascular injury in patients with trauma cephalad to the angle of the mandible compared with 11 % of patients who had neck trauma. Gunshot wounds were associated with vascular damage more frequently than were stab wounds. Angiography is often performed in penetrating trauma to the head and neck to evaluate the possibility of vascular injury and to aid in planning appropriate management [1]. Nonetheless, the role of angiography in penetrating head and neck trauma has remained controversial.