Cystic Duct Lithiasis Post-Cholecystectomy: a Singular
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Variation of Cystic Duct Insertion in Relation to the Extrahepatic Ducts
AbeshaAmbaye et al. / International Journal of Pharma Sciences and Research (IJPSR) Variation of Cystic Duct Insertion in Relation to the Extrahepatic Ducts and Observed Frequency of Double Lumen Apparent Common Bile Duct AbeshaAmbaye1, MueezAbraha2,Bernard A. Anderson2, Amanuel T. Tsegay1 Anatomy Course and Research Team, Institute of Biomedical Sciences, College of Health Sciences, Mekelle University Dep’t of Anatomy, College of Medicine and Health Sciences, University of Gondar, Ethiopia email [email protected] ABSTRACT Background: Variations in the pattern of the extra hepatic biliary tract are common and usually encountered during radiological investigations or during operations on the biliary tree. Having a good knowledge of the possible connections of the cystic duct with the common hepatic duct to form the common bile duct is very important; because variation in this area is common. Objectives: The main aim of this study is to evaluate the frequency of anatomic variations of the cystic duct insertion in relation to the extrahepatic ducts and Observed Frequency of Double Lumen Apparent Common Bile Duct Methods: Institutional based cross-sectional study design with observational data collection tool was conducted in 25 Ethiopian fixed cadavers and Forensic autopsy specimens obtained from Departments of Human Anatomy at University of Gondar, Mekelle and St. Paul Hospital Millennium Medical College Result: From the total 25 specimens dissected 9 (36%) had the ACBD and the 16 (64%) of them had CBD with one lumen. Conclusion: The billiary system formation is very variable, among the variants; the number of the supradoudenal insertion is greater than the infradoudenal insertion. ACBD is more frequent than expected which is 36% of the total data. -
![Mft•] ~;;I~ [I) I~ T?L3 ·Ilr!F·S; [,J ~ M](https://docslib.b-cdn.net/cover/6471/mft-i-i-i-t-l3-%C2%B7ilr-f%C2%B7s-j-m-706471.webp)
Mft•] ~;;I~ [I) I~ T?L3 ·Ilr!F·S; [,J ~ M
Mft•] ~;;I~ [I) I~ t?l3 ·ilr!f·S; [,j ~ M Hepatobiliary Imaging Update Maggie Chester and Jerry Glowniak Veterans Affairs Medical Center and Oregon Health Sciences University, Portland, Oregon and the gallbladder ejection fraction (EF) after the injection This is the first article in a four-part series on interventional of cholecystokinin (CCK) (Kinevac®, Squibb Diagnostics, nuclear medicine. Upon completion, the nuclear medicine New Brunswick, NJ). A brief description of the hepatic ex technologist should be able to (1) list the advantages of using traction fraction (HEF) was given; the technique used quan interventional hepatic imaging, (2) identify the benefit in tifies hepatocyte function more accurately than does excretion calculating HEF, and (3) utilize the HEF calculation method when appropriate. half-time. Since publication of the previous article (5), the HEF has become more widely used as a measure of hepatocyte function, and nearly all the major nuclear medicine software vendors include programs for calculating the HEF. Scintigraphic assessment of hepatobiliary function began in In this article, we will describe new observations and meth the 1950s with the introduction of iodine-131 C31 1) Rose ods used in hepatobiliary imaging. The following topics will bengal (1). Due to the poor imaging characteristics of 1311, be discussed: ( 1) the use of morphine as an aid in the diagnosis numerous attempts were made to find a technetium-99m 99 of acute cholecystitis, (2) the rim sign in the diagnosis of acute ( mTc) labeled hepatobiliary agent (2). The most useful of cholecystitis, and (3) methods for calculating the HEF. the several 99mTc-labeled agents that were investigated were the iminodiacetic acid (IDA) analogs, which were introduced MORPHINE-AUGMENTED CHOLESCINTIGRAPHY in the mid 1970s (3). -
Mistakes in Pancreatobiliary Imaging and How to Avoid Them
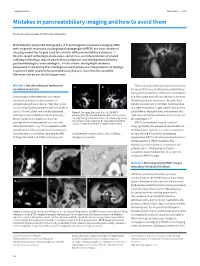
ueg education Mistakes in… 2020 Mistakes in pancreatobiliary imaging and how to avoid them Marianna Arvanitakis and Martina Pezzullo Multidetector computed tomography (CT) and magnetic resonance imaging (MRI) with magnetic resonance cholangiopancreatography (MRCP) are cross-sectional imaging modalities largely used for patients with pancreatobiliary diseases.1–3 Despite recent technological advances, correct use and interpretation of related radiological findings require good clinical judgment and collaboration between gastroenterologists and radiologists. In this article, we highlight mistakes frequently made during the radiological investigation and interpretation of findings in patients with suspected pancreatobiliary diseases, based on the available literature and on our clinical experience. There are several biliary anatomic variations to Mistake 1 Not describing or looking for a b anatomical variants be aware of that may lead to perioperative biliary injury: perihilar insertion of the cystic duct defined Laparoscopic cholecystectomy is currently as a short cystic duct with an insertion <1 cm from the standard procedure for treatment of the hilum; posterior insertion of the cystic duct symptomatic gallstone disease.4 Bile duct injury into the common bile duct (CBD); direct insertion can occur during the procedure with an incidence of a segmental/sectoral right hepatic duct into the up to 0.7% and, albeit rare, can be associated Figure 1 | Imaging the cystic duct. a | 2D MRCP gallbladder or the cystic duct; and insertion of a with significant morbidity and even mortality.4 showing that what looks like the cystic duct (arrow) is right sectoral/segmental hepatic duct directly into Biliary anatomical variations can lead to actually the right posterior duct separately originating the CBD (figure 1).3,5 from the common bile duct. -

Nomina Histologica Veterinaria, First Edition
NOMINA HISTOLOGICA VETERINARIA Submitted by the International Committee on Veterinary Histological Nomenclature (ICVHN) to the World Association of Veterinary Anatomists Published on the website of the World Association of Veterinary Anatomists www.wava-amav.org 2017 CONTENTS Introduction i Principles of term construction in N.H.V. iii Cytologia – Cytology 1 Textus epithelialis – Epithelial tissue 10 Textus connectivus – Connective tissue 13 Sanguis et Lympha – Blood and Lymph 17 Textus muscularis – Muscle tissue 19 Textus nervosus – Nerve tissue 20 Splanchnologia – Viscera 23 Systema digestorium – Digestive system 24 Systema respiratorium – Respiratory system 32 Systema urinarium – Urinary system 35 Organa genitalia masculina – Male genital system 38 Organa genitalia feminina – Female genital system 42 Systema endocrinum – Endocrine system 45 Systema cardiovasculare et lymphaticum [Angiologia] – Cardiovascular and lymphatic system 47 Systema nervosum – Nervous system 52 Receptores sensorii et Organa sensuum – Sensory receptors and Sense organs 58 Integumentum – Integument 64 INTRODUCTION The preparations leading to the publication of the present first edition of the Nomina Histologica Veterinaria has a long history spanning more than 50 years. Under the auspices of the World Association of Veterinary Anatomists (W.A.V.A.), the International Committee on Veterinary Anatomical Nomenclature (I.C.V.A.N.) appointed in Giessen, 1965, a Subcommittee on Histology and Embryology which started a working relation with the Subcommittee on Histology of the former International Anatomical Nomenclature Committee. In Mexico City, 1971, this Subcommittee presented a document entitled Nomina Histologica Veterinaria: A Working Draft as a basis for the continued work of the newly-appointed Subcommittee on Histological Nomenclature. This resulted in the editing of the Nomina Histologica Veterinaria: A Working Draft II (Toulouse, 1974), followed by preparations for publication of a Nomina Histologica Veterinaria. -

Anatomy of the Digestive System
The Digestive System Anatomy of the Digestive System We need food for cellular utilization: organs of digestive system form essentially a long !nutrients as building blocks for synthesis continuous tube open at both ends !sugars, etc to break down for energy ! alimentary canal (gastrointestinal tract) most food that we eat cannot be directly used by the mouth!pharynx!esophagus!stomach! body small intestine!large intestine !too large and complex to be absorbed attached to this tube are assorted accessory organs and structures that aid in the digestive processes !chemical composition must be modified to be useable by cells salivary glands teeth digestive system functions to altered the chemical and liver physical composition of food so that it can be gall bladder absorbed and used by the body; ie pancreas mesenteries Functions of Digestive System: The GI tract (digestive system) is located mainly in 1. physical and chemical digestion abdominopelvic cavity 2. absorption surrounded by serous membrane = visceral peritoneum 3. collect & eliminate nonuseable components of food this serous membrane is continuous with parietal peritoneum and extends between digestive organs as mesenteries ! hold organs in place, prevent tangling Human Anatomy & Physiology: Digestive System; Ziser Lecture Notes, 2014.4 1 Human Anatomy & Physiology: Digestive System; Ziser Lecture Notes, 2014.4 2 is suspended from rear of soft palate The wall of the alimentary canal consists of 4 layers: blocks nasal passages when swallowing outer serosa: tongue visceral peritoneum, -

Surgical Significance of Variations in Anatomy in the Biliary Region
International Journal of Research in Medical Sciences Hassan AU et al. Int J Res Med Sci. 2013 Aug;1(3):xx-xx www.msjonline.org pISSN 2320-6071 | eISSN 2320-6012 DOI: 10.5455/2320-6012.ijrms20130812 Review Article Surgical significance of variations in anatomy in the biliary region Ashfaq Ul Hassan1*, Showqat A. Zargar2, Aijaz Malik3, Pervez Shah4 1Department of Anatomy, SKIMS Medical College, Srinagar, Kashmir, India 2Department of Gastroenterology, SKIMS, Srinagar, Kashmir, India 3Department of Surgery, SKIMS, Srinagar, Kashmir, India 4Department of Medicine, SMHS Hospital, Srinagar, Kashmir, India Received: 8 May 2013 Accepted: 21 May 2013 *Correspondence: Dr. Ashfaq Ul Hassan, E-mail: [email protected] © 2013 Hassan AU et al. This is an open-access article distributed under the terms of the Creative Commons Attribution Non-Commercial License, which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. ABSTRACT Variations in the anatomy of the gallbladder, the bile ducts, and the arteries that supply them and the liver are important to the surgeon, because failure to recognize them can cause iatrogenic injury to the biliary tract. A surgeon should be always be careful while operating in this area. In addition these anomalies are associated with a range of other congenital anomalies, including biliary atresia and cardiovascular or other gastrointestinal malformations, biliary lithiasis, choledochal cyst, anomalous pancreaticobiliary junction etc, so a look out for other anomalies should be carried out simultaneously. Keywords: Gall bladder, Cystic fossa, Calots triangle, Monyhans hump, Extrahepatic, Atresia, Double Gall bladder, Triple Gall bladder, Agenesis, Cystic duct, Carolis disease NORMAL ANATOMY the left from the neck of the gallbladder, and joins the common hepatic duct to form the common bile duct. -

Cystic Duct Cholangiography Leo Chaikof
Henry Ford Hospital Medical Journal Volume 22 Number 3 Laurence S. Fallis, M.D. Commemorative Article 7 Issue 9-1974 Cystic Duct Cholangiography Leo Chaikof T. L. Friedlich R. A. Affifi H. Weizel Follow this and additional works at: https://scholarlycommons.henryford.com/hfhmedjournal Part of the Life Sciences Commons, Medical Specialties Commons, and the Public Health Commons Recommended Citation Chaikof, Leo; Friedlich, T. L.; Affifi, R. A.; and Weizel, H. (1974) "Cystic Duct Cholangiography," Henry Ford Hospital Medical Journal : Vol. 22 : No. 3 , 129-136. Available at: https://scholarlycommons.henryford.com/hfhmedjournal/vol22/iss3/7 This Article is brought to you for free and open access by Henry Ford Health System Scholarly Commons. It has been accepted for inclusion in Henry Ford Hospital Medical Journal by an authorized editor of Henry Ford Health System Scholarly Commons. Henry Ford Hosp. Med. Journal Vol. 22, No. 3, 1974 Cystic Duct Cholangiography Leo Chaikof, MD,* T.L. Friedlich, MD, R.A. Affifi, MD and H. Weizel, MD ALTHOUGH operative cholangiog raphy was first used in 1932 by Mirizzi,^'^ it is still not done routinely as part of the surgical procedure in biliary tract opera tions. According to Jolly, Baker et al,^ only 18% of members of the American Surgical Association use it routinely. De spite a great deal of discussion pro and con in the literature,^'" it appears that, if A series of 837 cystic duct cholangiograms the frequency of common duct explora has been reviewed. The technique is simple and safe to carry out. It is not time consuming tion can be reduced, certainly its as and does not require any unusual equipment. -
Primary Sclerosing Cholangitis: Introduction
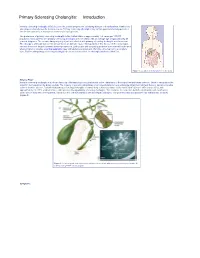
Primary Sclerosing Cholangitis: Introduction Primary sclerosing cholangitis (PSC) is a chronic , usually progressive, stricturing disease of the biliary tree. Remissions and relapses characterize the disease course. Primary sclerosing cholangitis may remain quiescent for long periods of time in some patients; in most cases, however, it is progressive. The prevalence of primary sclerosing cholangitis in the United States is approximately 1–6 cases per 100,000 population. Most patients with primary sclerosing cholangitis are men (75%) with an average age of approximately 40 years at diagnosis. The overwhelming majority of patients affected with primary sclerosing cholangitis are Caucasian. The etiology is unknown but current opinion favors an immune cause. Management of this disease in the early stages involves the use of drugs to prevent disease progression. Endoscopic and surgical approaches are reserved for the time when symptoms develop. Liver transplantation may ultimately be required and offers the only chance for a complete cure. Patients with primary sclerosing cholangitis are at an increased risk for cholangiocarcinoma (10–15%). Figure 1. Location of the biliary tree in the body. What is PSC? Primary sclerosing cholangitis is a chronic fibrosing inflammatory process that results in the obliteration of the biliary tree and biliary cirrhosis. There is variability in the extent of involvement of the biliary system. The majority of patients with primary sclerosing cholangitis have underlying inflammatory bowel disease, namely ulcerative colitis or Crohn’s disease. Patients with primary sclerosing cholangitis are more likely to have ulcerative colitis than Crohn’s disease (85% versus 15%), with approximately 2.5–7.5% of all ulcerative colitis patients having primary sclerosing cholangitis. -

Adult Bile Duct Strictures: Role of MR Imaging and MR Cholangiopan Creatography in Characterization1
Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. GASTROINTESTINAL IMAGING 565 Adult Bile Duct Strictures: Role of MR Imaging and MR Cholangiopan- creatography in Characterization1 Venkata S. Katabathina, MD Anil K. Dasyam, MD Bile duct strictures in adults are secondary to a wide spectrum Navya Dasyam, MBBS of benign and malignant pathologic conditions. Benign causes Keyanoosh Hosseinzadeh, MD2 of bile duct strictures include iatrogenic causes, acute or chronic pancreatitis, choledocholithiasis, primary sclerosing cholangitis, Abbreviations: AIDS = acquired immunodefi- IgG4-related sclerosing cholangitis, liver transplantation, recurrent ciency syndrome, AIP = autoimmune pancreati- pyogenic cholangitis, Mirizzi syndrome, acquired immunodeficien- tis, CBD = common bile duct, CHD = common hepatic duct, ERCP = endoscopic retrograde cy syndrome cholangiopathy, and sphincter of Oddi dysfunction. cholangiopancreatography, MIP = maximum in- Malignant causes include cholangiocarcinoma, pancreatic adeno- tensity projection, MPD = main pancreatic duct, carcinoma, and periampullary carcinomas. Rare causes include PSC = primary sclerosing cholangitis, RARE = rapid acquisition with relaxation enhancement, biliary inflammatory pseudotumor, gallbladder carcinoma, hepato- RHD = right hepatic duct, RPC = recurrent cellular carcinoma, metastases to bile ducts, and extrinsic bile duct pyogenic cholangitis, SOD = sphincter of Oddi dysfunction, 3D = three-dimensional, 2D = compression secondary to periportal or peripancreatic lymphade- two-dimensional nopathy. Contrast material–enhanced magnetic resonance (MR) RadioGraphics 2014; 34:565–586 imaging with MR cholangiopancreatography is extremely helpful in the noninvasive evaluation of patients with obstructive jaundice, an Published online 10.1148/rg.343125211 obstructive pattern of liver function, or incidentally detected biliary Content Codes: duct dilatation. -

Pancreas & Biliary System
Pancreas & Biliary System Gastrointestinal block-Anatomy-Lecture 4 Editing file Objectives Color guide : Only in boys slides in Green Only in girls slides in Purple important in Red At the end of the lecture, students should be able to: Notes in Grey ● Describe the location, surface anatomy, parts, relations & peritoneal reflection of the pancreas and gallbladder. ● Describe blood supply, nerve supply andlymphatic drainage of pancreas and gallbladder. ● Describe Course of each of common hepatic, cystic and common bile duct and pancreatic ducts Pancreas Location ● Located in Epigastrium & Left upper quadrant (left hypochondriac) of abdomen behind the stomach. in front of spleen (from concavity of the duodenum to the hilum of spleen opposite the level of T12– L3 vertebrae). ● 12–15 cm ,6-10 inch in length and 60-100 gram in weight. ● soft, lobulated elongated gland ● The greater part is Retroperitoneal behind the lesser sac. ● “J”-shaped or RETORT shaped ● Lies across the posterior abdominal wall in a transverse/oblique directions at the transpyloric plane (L1 vertebra) (except the tail it lies at the level of T12) has exocrine and endocrine functions. Endocrine component Exocrine component ● makes and secretes hormones (insulin, ● makes and secretes digestive glucagon, somatostatin) enzymes into the intestine ● control energy metabolism and storage (Exocrine pancreas) throughout the body (Endocrine ● comprise more than 95% of the pancreas Islet's of Langerhans). pancreatic mass ● comprise 1-2% of pancreatic mass 3 Pancreas Parts 1 Head 2 Neck 3 Body 4 Tail Head ● enlarged, disc-shaped right end of the pancreas ● lies in the concavity of the C-shaped duodenal loop in front of the L2 vertebra. -

Ta2, Part Iii
TERMINOLOGIA ANATOMICA Second Edition (2.06) International Anatomical Terminology FIPAT The Federative International Programme for Anatomical Terminology A programme of the International Federation of Associations of Anatomists (IFAA) TA2, PART III Contents: Systemata visceralia Visceral systems Caput V: Systema digestorium Chapter 5: Digestive system Caput VI: Systema respiratorium Chapter 6: Respiratory system Caput VII: Cavitas thoracis Chapter 7: Thoracic cavity Caput VIII: Systema urinarium Chapter 8: Urinary system Caput IX: Systemata genitalia Chapter 9: Genital systems Caput X: Cavitas abdominopelvica Chapter 10: Abdominopelvic cavity Bibliographic Reference Citation: FIPAT. Terminologia Anatomica. 2nd ed. FIPAT.library.dal.ca. Federative International Programme for Anatomical Terminology, 2019 Published pending approval by the General Assembly at the next Congress of IFAA (2019) Creative Commons License: The publication of Terminologia Anatomica is under a Creative Commons Attribution-NoDerivatives 4.0 International (CC BY-ND 4.0) license The individual terms in this terminology are within the public domain. Statements about terms being part of this international standard terminology should use the above bibliographic reference to cite this terminology. The unaltered PDF files of this terminology may be freely copied and distributed by users. IFAA member societies are authorized to publish translations of this terminology. Authors of other works that might be considered derivative should write to the Chair of FIPAT for permission to publish a derivative work. Caput V: SYSTEMA DIGESTORIUM Chapter 5: DIGESTIVE SYSTEM Latin term Latin synonym UK English US English English synonym Other 2772 Systemata visceralia Visceral systems Visceral systems Splanchnologia 2773 Systema digestorium Systema alimentarium Digestive system Digestive system Alimentary system Apparatus digestorius; Gastrointestinal system 2774 Stoma Ostium orale; Os Mouth Mouth 2775 Labia oris Lips Lips See Anatomia generalis (Ch. -

The Digestive System
THE DIGESTIVE SYSTEM COMPILED BY HOWIE BAUM DIGESTIVE SYSTEM People are probably more aware of their digestive system than of any other system, not least because of its frequent messages. Hunger, thirst, appetite, gas ☺, and the frequency and nature of bowel movements, are all issues affecting daily life. The Digestive Tract • Six Functions of the Digestive System 1. Ingestion 2. Mechanical processing 3. Digestion 4. Secretion 5. Absorption 6. Excretion The Digestive Tract • Ingestion – Occurs when materials enter digestive tract via the mouth • Mechanical Processing – Crushing and shearing – Makes materials easier to propel along digestive tract • Digestion – The chemical breakdown of food into small organic fragments for absorption by digestive epithelium The Digestive Tract • Secretion – Is the release of water, acids, enzymes, buffers, and salts – By epithelium of digestive tract – By glandular organs • Absorption – Movement of organic substrates, electrolytes, vitamins, and water – Across digestive epithelium tissue – Into the interstitial fluid of digestive tract • Excretion – Removal of waste products from body fluids – Process called defecation removes feces AN INTRODUCTION TO THE DIGESTIVE SYSTEM • The Digestive Tract • Also called the gastrointestinal (GI) tract or alimentary canal • Is a muscular tube • Extends from our mouth to the anus • Passes through the pharynx, esophagus, stomach, and small and large intestines The digestive system is one of the most clearly defined in the body. It consists of a long passageway, the digestive