Surgical Significance of Variations in Anatomy in the Biliary Region
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Variation of Cystic Duct Insertion in Relation to the Extrahepatic Ducts
AbeshaAmbaye et al. / International Journal of Pharma Sciences and Research (IJPSR) Variation of Cystic Duct Insertion in Relation to the Extrahepatic Ducts and Observed Frequency of Double Lumen Apparent Common Bile Duct AbeshaAmbaye1, MueezAbraha2,Bernard A. Anderson2, Amanuel T. Tsegay1 Anatomy Course and Research Team, Institute of Biomedical Sciences, College of Health Sciences, Mekelle University Dep’t of Anatomy, College of Medicine and Health Sciences, University of Gondar, Ethiopia email [email protected] ABSTRACT Background: Variations in the pattern of the extra hepatic biliary tract are common and usually encountered during radiological investigations or during operations on the biliary tree. Having a good knowledge of the possible connections of the cystic duct with the common hepatic duct to form the common bile duct is very important; because variation in this area is common. Objectives: The main aim of this study is to evaluate the frequency of anatomic variations of the cystic duct insertion in relation to the extrahepatic ducts and Observed Frequency of Double Lumen Apparent Common Bile Duct Methods: Institutional based cross-sectional study design with observational data collection tool was conducted in 25 Ethiopian fixed cadavers and Forensic autopsy specimens obtained from Departments of Human Anatomy at University of Gondar, Mekelle and St. Paul Hospital Millennium Medical College Result: From the total 25 specimens dissected 9 (36%) had the ACBD and the 16 (64%) of them had CBD with one lumen. Conclusion: The billiary system formation is very variable, among the variants; the number of the supradoudenal insertion is greater than the infradoudenal insertion. ACBD is more frequent than expected which is 36% of the total data. -

Annual Meeting in Tulsa (Hosted by Elmus Beale) on June 11-15, 2019, We Were All Energized
37th ANNUAL Virtual Meeting 2020 June 15-19 President’s Report June 15-19, 2020 Virtual Meeting #AACA Strong Due to the unprecedented COVID-19 pandemic, our 2020 annual AACA meeting in June 15-19 at Weill Cornell in New York City has been canceled. While this is disappointing on many levels, it was an obvious decision (a no brainer for this neurosurgeon) given the current situation and the need to be safe. These past few weeks have been stressful and uncertain for our society, but for all of us personally, professionally and collectively. Through adversity comes opportunity: how we choose to react to this challenge will determine our future. Coming away from the 36th Annual meeting in Tulsa (hosted by Elmus Beale) on June 11-15, 2019, we were all energized. An informative inaugural newsletter edited by Mohammed Khalil was launched in the summer. In the fall, Christina Lewis hosted a successful regional meeting (Augmented Approaches for Incorporating Clinical Anatomy into Education, Research, and Informed Therapeutic Management) with an excellent faculty and nearly 50 attendees at Samuel Merritt University in Oakland, CA. The midyear council meeting was coordinated to overlap with that regional meeting to show solidarity. During the following months, plans for the 2020 New York meeting were well in motion. COVID-19 then surfaced: first with its ripple effect and then its storm. Other societies’ meetings - including AAA and EB – were canceled and outreach to them was extended for them to attend our meeting later in the year. Unfortunately, we subsequently had to cancel the plans for NY. -
![Mft•] ~;;I~ [I) I~ T?L3 ·Ilr!F·S; [,J ~ M](https://docslib.b-cdn.net/cover/6471/mft-i-i-i-t-l3-%C2%B7ilr-f%C2%B7s-j-m-706471.webp)
Mft•] ~;;I~ [I) I~ T?L3 ·Ilr!F·S; [,J ~ M
Mft•] ~;;I~ [I) I~ t?l3 ·ilr!f·S; [,j ~ M Hepatobiliary Imaging Update Maggie Chester and Jerry Glowniak Veterans Affairs Medical Center and Oregon Health Sciences University, Portland, Oregon and the gallbladder ejection fraction (EF) after the injection This is the first article in a four-part series on interventional of cholecystokinin (CCK) (Kinevac®, Squibb Diagnostics, nuclear medicine. Upon completion, the nuclear medicine New Brunswick, NJ). A brief description of the hepatic ex technologist should be able to (1) list the advantages of using traction fraction (HEF) was given; the technique used quan interventional hepatic imaging, (2) identify the benefit in tifies hepatocyte function more accurately than does excretion calculating HEF, and (3) utilize the HEF calculation method when appropriate. half-time. Since publication of the previous article (5), the HEF has become more widely used as a measure of hepatocyte function, and nearly all the major nuclear medicine software vendors include programs for calculating the HEF. Scintigraphic assessment of hepatobiliary function began in In this article, we will describe new observations and meth the 1950s with the introduction of iodine-131 C31 1) Rose ods used in hepatobiliary imaging. The following topics will bengal (1). Due to the poor imaging characteristics of 1311, be discussed: ( 1) the use of morphine as an aid in the diagnosis numerous attempts were made to find a technetium-99m 99 of acute cholecystitis, (2) the rim sign in the diagnosis of acute ( mTc) labeled hepatobiliary agent (2). The most useful of cholecystitis, and (3) methods for calculating the HEF. the several 99mTc-labeled agents that were investigated were the iminodiacetic acid (IDA) analogs, which were introduced MORPHINE-AUGMENTED CHOLESCINTIGRAPHY in the mid 1970s (3). -

Intrahepatic Pancreatic Pseudocyst: Case Series
JOP. J Pancreas (Online) 2016 Jul 08; 17(4):410-413. CASE SERIES Intrahepatic Pancreatic Pseudocyst: Case Series Dhaval Gupta, Nirav Pipaliya, Nilesh Pandav, Kaivan Shah, Meghraj Ingle, Prabha Sawant Department of Gastroenterology, Lokmanya Tilak Municipal Medical College &Hospital, Sion, Mumbai, India ABSTRACT Intrahepatic pseudocyst is a very rare complication of pancreatitis. Lack of experience and literature makes diagnosis and management of intrahepatic pseudocyst very difficult. Majority of published cases were managed by either percutaneous or surgical drainage. Less than 30 cases of intrahepatic pseudocysts have been reported in the literature and there is not a single report of endoscopic ultrasound guided management of intrahepatic pseudocysts. Here we report a case series of 2 patients who presented with intrahepatic pseudocysts and out of which first case was successfully managed by EUS guided drainage. Our second case is also the youngest patient presented with intrahepatic pseudocyst till now. INTRODUCTION abdominal distention since last 1 month. However he did located in or around t not have significant weight loss, gastrointestinal bleeding, A pancreatic pseudocyst is a collection of pancreatic fluid pedal edema, jaundice, fever. His past medical history and he pancreas. Pancreatic pseudocysts family history was not significant. He was chronic alcoholic are encased by a non-epithelial lining of fibrous, necrotic since last 15 years with intake of approximately 90 gram and granulation tissue secondary to pancreatic injury. -

Normal Anatomy of Porta Hepatis—A Cadaveric Study
THIEME 22 Original Article Normal Anatomy of Porta Hepatis—A Cadaveric Study Dhanalaxmi D. Neginhal1 Umesh K. Kulkarni1 1Department of Anatomy, Belagavi Institute of Medical Sciences, Address for correspondence Umesh K. Kulkarni, MS (Anat), Belagavi, Karnataka, India Department of Anatomy, Belagavi Institute of Medical Sciences, Belagavi, Karnataka, India (e-mail: [email protected]). Natl J Clin Anat 2019;8:22–26 Abstract Background and Aim Porta hepatis (PH) of the liver acts as a gateway for exit and entry of important structures like portal vein, hepatic artery, and hepatic duct. Having knowledge of variations about the dimensions and structures at PH becomes important to avoid complications during surgical and radiological interventions. Our study aims to observe the dimensions of PH and also the number, arrangement, and variations of structures passing through PH. Materials and Methods Fifty adult cadaveric human livers which were preserved in formalin were studied. Transverse diameter, anteroposterior diameter, and circumference of PH were measured using vernier calipers, measuring scale, and thread. PH was carefully dissected to study the number, arrangement, and combination of arteries, veins, and ducts at PH. Results The mean transverse diameter, anteroposterior diameter, and total circumference of PH was 3.17 ± 0.50, 1.68 ± 0.36, and 10.46 ± 1.415 cm, respectively. Eighteen specimens showed presence of two arteries, two veins, and one duct at PH. Keywords Maximum number of arteries, veins, and ducts passing through PH were 5, 4, and 1, ► porta hepatis respectively. The ducts were anterior, arteries in the middle, and veins were posterior ► portal vein in PH of all the livers. -
Mistakes in Pancreatobiliary Imaging and How to Avoid Them
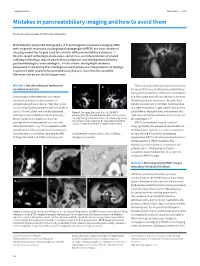
ueg education Mistakes in… 2020 Mistakes in pancreatobiliary imaging and how to avoid them Marianna Arvanitakis and Martina Pezzullo Multidetector computed tomography (CT) and magnetic resonance imaging (MRI) with magnetic resonance cholangiopancreatography (MRCP) are cross-sectional imaging modalities largely used for patients with pancreatobiliary diseases.1–3 Despite recent technological advances, correct use and interpretation of related radiological findings require good clinical judgment and collaboration between gastroenterologists and radiologists. In this article, we highlight mistakes frequently made during the radiological investigation and interpretation of findings in patients with suspected pancreatobiliary diseases, based on the available literature and on our clinical experience. There are several biliary anatomic variations to Mistake 1 Not describing or looking for a b anatomical variants be aware of that may lead to perioperative biliary injury: perihilar insertion of the cystic duct defined Laparoscopic cholecystectomy is currently as a short cystic duct with an insertion <1 cm from the standard procedure for treatment of the hilum; posterior insertion of the cystic duct symptomatic gallstone disease.4 Bile duct injury into the common bile duct (CBD); direct insertion can occur during the procedure with an incidence of a segmental/sectoral right hepatic duct into the up to 0.7% and, albeit rare, can be associated Figure 1 | Imaging the cystic duct. a | 2D MRCP gallbladder or the cystic duct; and insertion of a with significant morbidity and even mortality.4 showing that what looks like the cystic duct (arrow) is right sectoral/segmental hepatic duct directly into Biliary anatomical variations can lead to actually the right posterior duct separately originating the CBD (figure 1).3,5 from the common bile duct. -

A Novel Approach of Gross Structure of Human Liver
wjpmr, 2019,5(2), 181-186 SJIF Impact Factor: 4.639 WORLD JOURNAL OF PHARMACEUTICAL Research Article Manoj et al. AND MEDICAL RESEARCH World Journal of Pharmaceutical and Medical ResearchISSN 2455 -3301 www.wjpmr.com WJPMR A NOVEL APPROACH OF GROSS STRUCTURE OF HUMAN LIVER A. Manoj and Annamma Paul Department of Anatomy, School of Medical Education, M.G University (Accredited by NAAC with A-Grade), Kottayam, Kerala, India. *Corresponding Author: A. Manoj Department of Anatomy, Government Medical College, Thrissur- 680596, under Directorate of Medical Education Health and Family Welfare– Government of Kerala, India. Article Received on 05/12/2018 Article Revised on 26/12/2018 Article Accepted on 16/01/2019 ABSTRACT This current exploratory research conducted to design for comprehensive study of human liver inorder to get best knowledge of learning objectives of its Gross structure. Topography of the liver was taken to know the exact position of liver. The weight, length of surfaces and borders were measured. It had two principal anatomical lobes based on attachment of ligaments and two functional lobes due to the distribution of blood and bile. It had five surfaces with one distinct border. Owing to the dichotomous divisions of the hepatic artery, portal vein and bile ducts it has to have eight vascular segments which can be resected without damaging those remaining. Apart from peritoneal covering it had been connected with falciform ligaments, Coronary ligaments, Triangular ligaments, Ligamentum teres, Ligamentum venosum. The nonperitoneal areas were fissures of ligamentum venosum, teres hepatis, Groove of inferior venacava, Fossa for gall bladder and bare area. -

Nomina Histologica Veterinaria, First Edition
NOMINA HISTOLOGICA VETERINARIA Submitted by the International Committee on Veterinary Histological Nomenclature (ICVHN) to the World Association of Veterinary Anatomists Published on the website of the World Association of Veterinary Anatomists www.wava-amav.org 2017 CONTENTS Introduction i Principles of term construction in N.H.V. iii Cytologia – Cytology 1 Textus epithelialis – Epithelial tissue 10 Textus connectivus – Connective tissue 13 Sanguis et Lympha – Blood and Lymph 17 Textus muscularis – Muscle tissue 19 Textus nervosus – Nerve tissue 20 Splanchnologia – Viscera 23 Systema digestorium – Digestive system 24 Systema respiratorium – Respiratory system 32 Systema urinarium – Urinary system 35 Organa genitalia masculina – Male genital system 38 Organa genitalia feminina – Female genital system 42 Systema endocrinum – Endocrine system 45 Systema cardiovasculare et lymphaticum [Angiologia] – Cardiovascular and lymphatic system 47 Systema nervosum – Nervous system 52 Receptores sensorii et Organa sensuum – Sensory receptors and Sense organs 58 Integumentum – Integument 64 INTRODUCTION The preparations leading to the publication of the present first edition of the Nomina Histologica Veterinaria has a long history spanning more than 50 years. Under the auspices of the World Association of Veterinary Anatomists (W.A.V.A.), the International Committee on Veterinary Anatomical Nomenclature (I.C.V.A.N.) appointed in Giessen, 1965, a Subcommittee on Histology and Embryology which started a working relation with the Subcommittee on Histology of the former International Anatomical Nomenclature Committee. In Mexico City, 1971, this Subcommittee presented a document entitled Nomina Histologica Veterinaria: A Working Draft as a basis for the continued work of the newly-appointed Subcommittee on Histological Nomenclature. This resulted in the editing of the Nomina Histologica Veterinaria: A Working Draft II (Toulouse, 1974), followed by preparations for publication of a Nomina Histologica Veterinaria. -

Anatomy of the Digestive System
The Digestive System Anatomy of the Digestive System We need food for cellular utilization: organs of digestive system form essentially a long !nutrients as building blocks for synthesis continuous tube open at both ends !sugars, etc to break down for energy ! alimentary canal (gastrointestinal tract) most food that we eat cannot be directly used by the mouth!pharynx!esophagus!stomach! body small intestine!large intestine !too large and complex to be absorbed attached to this tube are assorted accessory organs and structures that aid in the digestive processes !chemical composition must be modified to be useable by cells salivary glands teeth digestive system functions to altered the chemical and liver physical composition of food so that it can be gall bladder absorbed and used by the body; ie pancreas mesenteries Functions of Digestive System: The GI tract (digestive system) is located mainly in 1. physical and chemical digestion abdominopelvic cavity 2. absorption surrounded by serous membrane = visceral peritoneum 3. collect & eliminate nonuseable components of food this serous membrane is continuous with parietal peritoneum and extends between digestive organs as mesenteries ! hold organs in place, prevent tangling Human Anatomy & Physiology: Digestive System; Ziser Lecture Notes, 2014.4 1 Human Anatomy & Physiology: Digestive System; Ziser Lecture Notes, 2014.4 2 is suspended from rear of soft palate The wall of the alimentary canal consists of 4 layers: blocks nasal passages when swallowing outer serosa: tongue visceral peritoneum, -

BILIARY OBSTRUCTION in the REGION of the PORTA HEPATIS Hunterian Lecture Delivered at the Royal College of Surgeons of England on 13Th February 1958* by Anthony J
BILIARY OBSTRUCTION IN THE REGION OF THE PORTA HEPATIS Hunterian Lecture delivered at the Royal College of Surgeons of England on 13th February 1958* by Anthony J. H. Rains, M.S., F.R.C.S. Senior Lecturer in Surgery, University of Birmingham, Surgeon, United Birmingham Hospitals IN CLINICAL PRACTICE, cases of obstruction of the bile ducts in this particular region of anatomy are comparatively rare, though they are of acclaimed notoriety. In a series of 2,033 cases of disease of the gall- bladder and bile ducts treated in the United Birmingham Hospitals, there were ninety-three cases of primary obstruction in the region of the porta hepatis (4.5 per cent.). When first encountering a case, one is assailed by personal lack of experience of such lesions and the knowledge which can be applied to provide a remedy or relief for the patients who are often afflicted at the dawn or in the prime of their lives, by lesions which are not always intrinsically fatal but which have fatal consequences in so far as they lead to the impairment of the drainage of bile with increasing liver damage. Unlike obstruction to blood vessels, no help is to be expected from the natural development of collaterals, and the surgeon is faced with relieving the obstruction or the eventual death of the patient. His task is made difficult, not only by the anatomical inaccessibility and the complexity and variations of bile ducts, hepatic artery and portal vein, but also by a characteristic inflammatory response to local extravasations of bile, varieties of cholangitis, and what is often misguidedly called " previous operative interference." Types of lesion Table I shows the different types of lesion that may be encountered and the incidence in this series. -

Cystic Duct Cholangiography Leo Chaikof
Henry Ford Hospital Medical Journal Volume 22 Number 3 Laurence S. Fallis, M.D. Commemorative Article 7 Issue 9-1974 Cystic Duct Cholangiography Leo Chaikof T. L. Friedlich R. A. Affifi H. Weizel Follow this and additional works at: https://scholarlycommons.henryford.com/hfhmedjournal Part of the Life Sciences Commons, Medical Specialties Commons, and the Public Health Commons Recommended Citation Chaikof, Leo; Friedlich, T. L.; Affifi, R. A.; and Weizel, H. (1974) "Cystic Duct Cholangiography," Henry Ford Hospital Medical Journal : Vol. 22 : No. 3 , 129-136. Available at: https://scholarlycommons.henryford.com/hfhmedjournal/vol22/iss3/7 This Article is brought to you for free and open access by Henry Ford Health System Scholarly Commons. It has been accepted for inclusion in Henry Ford Hospital Medical Journal by an authorized editor of Henry Ford Health System Scholarly Commons. Henry Ford Hosp. Med. Journal Vol. 22, No. 3, 1974 Cystic Duct Cholangiography Leo Chaikof, MD,* T.L. Friedlich, MD, R.A. Affifi, MD and H. Weizel, MD ALTHOUGH operative cholangiog raphy was first used in 1932 by Mirizzi,^'^ it is still not done routinely as part of the surgical procedure in biliary tract opera tions. According to Jolly, Baker et al,^ only 18% of members of the American Surgical Association use it routinely. De spite a great deal of discussion pro and con in the literature,^'" it appears that, if A series of 837 cystic duct cholangiograms the frequency of common duct explora has been reviewed. The technique is simple and safe to carry out. It is not time consuming tion can be reduced, certainly its as and does not require any unusual equipment. -
Primary Sclerosing Cholangitis: Introduction
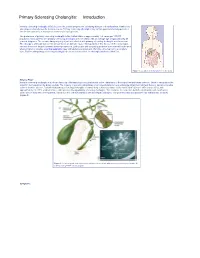
Primary Sclerosing Cholangitis: Introduction Primary sclerosing cholangitis (PSC) is a chronic , usually progressive, stricturing disease of the biliary tree. Remissions and relapses characterize the disease course. Primary sclerosing cholangitis may remain quiescent for long periods of time in some patients; in most cases, however, it is progressive. The prevalence of primary sclerosing cholangitis in the United States is approximately 1–6 cases per 100,000 population. Most patients with primary sclerosing cholangitis are men (75%) with an average age of approximately 40 years at diagnosis. The overwhelming majority of patients affected with primary sclerosing cholangitis are Caucasian. The etiology is unknown but current opinion favors an immune cause. Management of this disease in the early stages involves the use of drugs to prevent disease progression. Endoscopic and surgical approaches are reserved for the time when symptoms develop. Liver transplantation may ultimately be required and offers the only chance for a complete cure. Patients with primary sclerosing cholangitis are at an increased risk for cholangiocarcinoma (10–15%). Figure 1. Location of the biliary tree in the body. What is PSC? Primary sclerosing cholangitis is a chronic fibrosing inflammatory process that results in the obliteration of the biliary tree and biliary cirrhosis. There is variability in the extent of involvement of the biliary system. The majority of patients with primary sclerosing cholangitis have underlying inflammatory bowel disease, namely ulcerative colitis or Crohn’s disease. Patients with primary sclerosing cholangitis are more likely to have ulcerative colitis than Crohn’s disease (85% versus 15%), with approximately 2.5–7.5% of all ulcerative colitis patients having primary sclerosing cholangitis.