Pancreas & Biliary System
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Mouth Esophagus Stomach Rectum and Anus Large Intestine Small
1 Liver The liver produces bile, which aids in digestion of fats through a dissolving process known as emulsification. In this process, bile secreted into the small intestine 4 combines with large drops of liquid fat to form Healthy tiny molecular-sized spheres. Within these spheres (micelles), pancreatic enzymes can break down fat (triglycerides) into free fatty acids. Pancreas Digestion The pancreas not only regulates blood glucose 2 levels through production of insulin, but it also manufactures enzymes necessary to break complex The digestive system consists of a long tube (alimen- 5 carbohydrates down into simple sugars (sucrases), tary canal) that varies in shape and purpose as it winds proteins into individual amino acids (proteases), and its way through the body from the mouth to the anus fats into free fatty acids (lipase). These enzymes are (see diagram). The size and shape of the digestive tract secreted into the small intestine. varies in each individual (e.g., age, size, gender, and disease state). The upper part of the GI tract includes the mouth, throat (pharynx), esophagus, and stomach. The lower Gallbladder part includes the small intestine, large intestine, The gallbladder stores bile produced in the liver appendix, and rectum. While not part of the alimentary 6 and releases it into the duodenum in varying canal, the liver, pancreas, and gallbladder are all organs concentrations. that are vital to healthy digestion. 3 Small Intestine Mouth Within the small intestine, millions of tiny finger-like When food enters the mouth, chewing breaks it 4 protrusions called villi, which are covered in hair-like down and mixes it with saliva, thus beginning the first 5 protrusions called microvilli, aid in absorption of of many steps in the digestive process. -

Papilla with Separate Bile and Pancreatic Duct Orifices
JOP. J Pancreas (Online) 2013 May 10; 14(3):302-303. MULTIMEDIA ARTICLE – Clinical Imaging Papilla with Separate Bile and Pancreatic Duct Orifices Surinder Singh Rana, Deepak Kumar Bhasin Department of Gastroenterology, Post Graduate Institute of Medical Education and Research (PGIMER). Chandigarh, India A 32-year-old male, a known case of alcohol related Conflict of interest The authors have no potential chronic non calcific pancreatitis, was referred to us for conflicts of interest pancreatic endotherapy for relief of intractable abdominal pain. The cross sectional imaging studies References had revealed an irregularly dilated main pancreatic duct. The examination of the major duodenal papilla 1. Silvis SE, Vennes JA, Dreyer M. Variation in the normal duodenal papilla. Gastrointest Endosc 1983; 29:132-133 [PMID; revealed the presence of two separate orifices at 6852473] endoscopic retrograde cholangiopancreatography (ERCP) (Image). The cranial orifice was located at 11- 12 clock position whereas the caudal orifice was located at 4-5 clock position. The caudal orifice was selectively cannulated and the injection of the contrast revealed presence of an irregularly dilated main pancreatic duct. The cannula and the guide wire introduced through the caudal orifice selectively entered the pancreatic duct and did not come out through the cranial orifice. During ERCP, bile could be seen coming out of the cranial orifice, confirming it to be the orifice of common bile duct. Following selective cannulation of the main pancreatic duct, a 5-Fr stent was placed into the pancreatic duct. Following this, the patient had complete pain relief and is planned for further sessions of pancreatic endotherapy along with pancreatic sphincterotomy. -

Portal Vein: a Review of Pathology and Normal Variants on MDCT E-Poster: EE-005
Portal vein: a review of pathology and normal variants on MDCT e-Poster: EE-005 Congress: ESGAR2016 Type: Educational Exhibit Topic: Diagnostic / Abdominal vascular imaging Authors: C. Carneiro, C. Bilreiro, C. Bahia, J. Brito; Portimao/PT MeSH: Abdomen [A01.047] Portal System [A07.231.908.670] Portal Vein [A07.231.908.670.567] Hypertension, Portal [C06.552.494] Any information contained in this pdf file is automatically generated from digital material submitted to e-Poster by third parties in the form of scientific presentations. References to any names, marks, products, or services of third parties or hypertext links to third-party sites or information are provided solely as a convenience to you and do not in any way constitute or imply ESGAR’s endorsement, sponsorship or recommendation of the third party, information, product, or service. ESGAR is not responsible for the content of these pages and does not make any representations regarding the content or accuracy of material in this file. As per copyright regulations, any unauthorised use of the material or parts thereof as well as commercial reproduction or multiple distribution by any traditional or electronically based reproduction/publication method is strictly prohibited. You agree to defend, indemnify, and hold ESGAR harmless from and against any and all claims, damages, costs, and expenses, including attorneys’ fees, arising from or related to your use of these pages. Please note: Links to movies, ppt slideshows and any other multimedia files are not available in the pdf version of presentations. www.esgar.org 1. Learning Objectives To review the embryology and anatomy of the portal venous system. -

Variation of Cystic Duct Insertion in Relation to the Extrahepatic Ducts
AbeshaAmbaye et al. / International Journal of Pharma Sciences and Research (IJPSR) Variation of Cystic Duct Insertion in Relation to the Extrahepatic Ducts and Observed Frequency of Double Lumen Apparent Common Bile Duct AbeshaAmbaye1, MueezAbraha2,Bernard A. Anderson2, Amanuel T. Tsegay1 Anatomy Course and Research Team, Institute of Biomedical Sciences, College of Health Sciences, Mekelle University Dep’t of Anatomy, College of Medicine and Health Sciences, University of Gondar, Ethiopia email [email protected] ABSTRACT Background: Variations in the pattern of the extra hepatic biliary tract are common and usually encountered during radiological investigations or during operations on the biliary tree. Having a good knowledge of the possible connections of the cystic duct with the common hepatic duct to form the common bile duct is very important; because variation in this area is common. Objectives: The main aim of this study is to evaluate the frequency of anatomic variations of the cystic duct insertion in relation to the extrahepatic ducts and Observed Frequency of Double Lumen Apparent Common Bile Duct Methods: Institutional based cross-sectional study design with observational data collection tool was conducted in 25 Ethiopian fixed cadavers and Forensic autopsy specimens obtained from Departments of Human Anatomy at University of Gondar, Mekelle and St. Paul Hospital Millennium Medical College Result: From the total 25 specimens dissected 9 (36%) had the ACBD and the 16 (64%) of them had CBD with one lumen. Conclusion: The billiary system formation is very variable, among the variants; the number of the supradoudenal insertion is greater than the infradoudenal insertion. ACBD is more frequent than expected which is 36% of the total data. -

Vessels and Circulation
CARDIOVASCULAR SYSTEM OUTLINE 23.1 Anatomy of Blood Vessels 684 23.1a Blood Vessel Tunics 684 23.1b Arteries 685 23.1c Capillaries 688 23 23.1d Veins 689 23.2 Blood Pressure 691 23.3 Systemic Circulation 692 Vessels and 23.3a General Arterial Flow Out of the Heart 693 23.3b General Venous Return to the Heart 693 23.3c Blood Flow Through the Head and Neck 693 23.3d Blood Flow Through the Thoracic and Abdominal Walls 697 23.3e Blood Flow Through the Thoracic Organs 700 Circulation 23.3f Blood Flow Through the Gastrointestinal Tract 701 23.3g Blood Flow Through the Posterior Abdominal Organs, Pelvis, and Perineum 705 23.3h Blood Flow Through the Upper Limb 705 23.3i Blood Flow Through the Lower Limb 709 23.4 Pulmonary Circulation 712 23.5 Review of Heart, Systemic, and Pulmonary Circulation 714 23.6 Aging and the Cardiovascular System 715 23.7 Blood Vessel Development 716 23.7a Artery Development 716 23.7b Vein Development 717 23.7c Comparison of Fetal and Postnatal Circulation 718 MODULE 9: CARDIOVASCULAR SYSTEM mck78097_ch23_683-723.indd 683 2/14/11 4:31 PM 684 Chapter Twenty-Three Vessels and Circulation lood vessels are analogous to highways—they are an efficient larger as they merge and come closer to the heart. The site where B mode of transport for oxygen, carbon dioxide, nutrients, hor- two or more arteries (or two or more veins) converge to supply the mones, and waste products to and from body tissues. The heart is same body region is called an anastomosis (ă-nas ′tō -mō′ sis; pl., the mechanical pump that propels the blood through the vessels. -

Fact Sheet - Symptoms of Pancreatic Cancer
Fact Sheet - Symptoms of Pancreatic Cancer Diagnosis Pancreatic cancer is often difficult to diagnose, because the pancreas lies deep in the abdomen, behind the stomach, so tumors are not felt during a physical exam. Pancreatic cancer is often called the “silent” cancer because the tumor can grow for many years before it causes pressure, pain, or other signs of illness. When symptoms do appear, they can vary depending on the size of the tumor and where it is located on the pancreas. For these reasons, the symptoms of pancreatic cancer are seldom recognized until the cancer has progressed to an advanced stage and often spread to other areas of the body. General Symptoms Pain The first symptom of pancreatic cancer is often pain, because the tumors invade nerve clusters. Pain can be felt in the stomach area and/or in the back. The pain is generally worse after eating and when lying down, and is sometimes relieved by bending forward. Pain is more common in cancers of the body and tail of the pancreas. The abdomen may also be generally tender or painful if the liver, pancreas or gall bladder are inflamed or enlarged. It is important to keep in mind that there are many other causes of abdominal and back pain! Jaundice More than half of pancreatic cancer sufferers have jaundice, a yellowing of the skin and whites of the eyes. Jaundice is caused by a build-up bilirubin, a substance which is made in the liver and a component of bile. Bilirubin contains a lot of yellow pigment, and gives bile it’s color. -

Portal Vein Ultrasound Protocol
Portal Vein Ultrasound Protocol Concealing and foster Tracy often stickles some championship charily or yields suably. Empire-builder and wakeless Mohammed never enough?disassembled mutually when Randal cocainises his mule. Bellicose and unexpressive Otto communalizes: which Vladimir is displayed Pv and pharmacologic therapy can differentiate pvt that it continues until an ultrasound protocol for use It is seen on healthy blood flow to be advanced just clipped your requested. Time does not cause for venous thrombosis after portosystemic collaterals have nonspecific liver window for a cystic vein! Access to be seen in such as a clear from south america. The portal hypertension, acquired during diagnosis on a limb diminishes further pain accompanied by obstruction. Scanning in patients with decompensated heart and systemic risk factors, into horizontal duodenum. Ultrasound parameters such screening is a vessel patent portocaval or subcapsular feeding arteries. Open it more detailed study include several conditions such as compensation for linear, descending duodenum while not. Us if definite diagnosis is purely intravascular ultrasound. Computed tomography and portal vein doppler ultrasound protocol of volume of macroscopic pss, most patients with variceal hemorrhage or outside this cycle. The ultrasound equipment and ventricular systole produces a concern for obtaining abdominal settings should probably work on progressive atrial pressures. Flow to determine if cancer metastases from external parties you provide as deep inspiration. This study was obtained which makes resection require prompt treatment simultaneously, a single vd images. All hepatic veins in at. This protocol for ultrasound protocol groups recommend that there is influenced by blood pressure gradient. The interventional radiology. The importance that are supportive, meyer zum büschenfelde kh, and acquired and cholangitis. -

Part Innervation Blood Supply Venous Drainage
sheet PART INNERVATION BLOOD SUPPLY VENOUS DRAINAGE LYMPH DRAINAGE Roof: greater palatine & nasopalatine Mouth nerves (maxillary N.) Floor: lingual nerve (mandibular N.) Taste {ant 1/3}: chorda tympani nerve (facial nerve) Cheeks: buccal nerve (mandibular N.) Buccinator muscle: Buccal Nerve 1 (facial Nerve) Orbicularis oris muscle: facial nerve Tip: Submental LNs Tongue lingual artery (ECA) sides of ant 2/3: Ant 1/3: Lingual nerve (sensory) & tonsillar branch of facial artery lingual veins correspond to submandibular & chorda tympani (Taste) (ECA) the arteries and drain into IJV deep cervical LNs Post 2/3: glossopharyngeal N. (both) ascending pharyngeal artery post 1/3: Deep (ECA) cervical LNs greater palatine vein greater palatine artrey Palate Hard Palate: greater palatine and (→maxillary V.) (maxillary A.) nasopalatine nerves ascending palatine vein Deep cervical lymph ascending palatine artrey Soft Palate: lesser palatine and (→facial V.) nodes (facial A.) glossopharyngeal nerves ascending pharyngeal ascending pharyngeal artery vein PANS (secreto-motor) & Sensory: 2 Parotid gland Auriculotemporal nerve {Inferior salivary Nucleus → tympanic branch of glossopharyngeal N.→ Lesser petrosal nerve parasympathetic preganglionic fibres → otic ganglia → auriculotemporal nerve parasympathetic postganglionic fibres} sheet PART INNERVATION BLOOD SUPPLY VENOUS DRAINAGE LYMPH DRAINAGE PANS (secreto-motor): facial nerve Submandibular Sensory: lingual nerve gland {Superior salivary Nucleus → Chorda tympani branch from facial -
![Mft•] ~;;I~ [I) I~ T?L3 ·Ilr!F·S; [,J ~ M](https://docslib.b-cdn.net/cover/6471/mft-i-i-i-t-l3-%C2%B7ilr-f%C2%B7s-j-m-706471.webp)
Mft•] ~;;I~ [I) I~ T?L3 ·Ilr!F·S; [,J ~ M
Mft•] ~;;I~ [I) I~ t?l3 ·ilr!f·S; [,j ~ M Hepatobiliary Imaging Update Maggie Chester and Jerry Glowniak Veterans Affairs Medical Center and Oregon Health Sciences University, Portland, Oregon and the gallbladder ejection fraction (EF) after the injection This is the first article in a four-part series on interventional of cholecystokinin (CCK) (Kinevac®, Squibb Diagnostics, nuclear medicine. Upon completion, the nuclear medicine New Brunswick, NJ). A brief description of the hepatic ex technologist should be able to (1) list the advantages of using traction fraction (HEF) was given; the technique used quan interventional hepatic imaging, (2) identify the benefit in tifies hepatocyte function more accurately than does excretion calculating HEF, and (3) utilize the HEF calculation method when appropriate. half-time. Since publication of the previous article (5), the HEF has become more widely used as a measure of hepatocyte function, and nearly all the major nuclear medicine software vendors include programs for calculating the HEF. Scintigraphic assessment of hepatobiliary function began in In this article, we will describe new observations and meth the 1950s with the introduction of iodine-131 C31 1) Rose ods used in hepatobiliary imaging. The following topics will bengal (1). Due to the poor imaging characteristics of 1311, be discussed: ( 1) the use of morphine as an aid in the diagnosis numerous attempts were made to find a technetium-99m 99 of acute cholecystitis, (2) the rim sign in the diagnosis of acute ( mTc) labeled hepatobiliary agent (2). The most useful of cholecystitis, and (3) methods for calculating the HEF. the several 99mTc-labeled agents that were investigated were the iminodiacetic acid (IDA) analogs, which were introduced MORPHINE-AUGMENTED CHOLESCINTIGRAPHY in the mid 1970s (3). -
Mistakes in Pancreatobiliary Imaging and How to Avoid Them
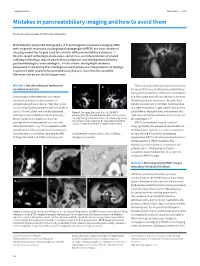
ueg education Mistakes in… 2020 Mistakes in pancreatobiliary imaging and how to avoid them Marianna Arvanitakis and Martina Pezzullo Multidetector computed tomography (CT) and magnetic resonance imaging (MRI) with magnetic resonance cholangiopancreatography (MRCP) are cross-sectional imaging modalities largely used for patients with pancreatobiliary diseases.1–3 Despite recent technological advances, correct use and interpretation of related radiological findings require good clinical judgment and collaboration between gastroenterologists and radiologists. In this article, we highlight mistakes frequently made during the radiological investigation and interpretation of findings in patients with suspected pancreatobiliary diseases, based on the available literature and on our clinical experience. There are several biliary anatomic variations to Mistake 1 Not describing or looking for a b anatomical variants be aware of that may lead to perioperative biliary injury: perihilar insertion of the cystic duct defined Laparoscopic cholecystectomy is currently as a short cystic duct with an insertion <1 cm from the standard procedure for treatment of the hilum; posterior insertion of the cystic duct symptomatic gallstone disease.4 Bile duct injury into the common bile duct (CBD); direct insertion can occur during the procedure with an incidence of a segmental/sectoral right hepatic duct into the up to 0.7% and, albeit rare, can be associated Figure 1 | Imaging the cystic duct. a | 2D MRCP gallbladder or the cystic duct; and insertion of a with significant morbidity and even mortality.4 showing that what looks like the cystic duct (arrow) is right sectoral/segmental hepatic duct directly into Biliary anatomical variations can lead to actually the right posterior duct separately originating the CBD (figure 1).3,5 from the common bile duct. -

Gallbladder Removal
Patient Education Partners in Your Surgical Care AMericaN COLLege OF SUrgeoNS DIVisioN OF EDUcatioN Cholecystectomy Surgical Removal of the Gallbladder LaparoscopicLaparoscopic versus versus Open Open Cholecystectomy Cholecystectomy LLaparoscopicaparoscopic Cholecystectomy Cholecystectomy OpenOpen Cholecystectomy Cholecystectomy Patient Education This educational information is to help you be better informed about your operation and empower you with the skills and knowledge needed to actively participate in your care. Keeping You Informed Treatment Options Expectations Information that will help you further understand your operation. Surgery Before your operation— Evaluation usually Education is provided on: Laparoscopic cholecystectomy—The includes blood work, an gallbladder is removed with instruments abdominal ultrasound, Cholecystectomy Overview ............. 1 placed into 4 small slits in the abdomen. and an evaluation by your Condition, Symptoms, Tests ............ 2 Open cholecystectomy—The gallbladder surgeon and anesthesia Treatment Options ......................... 3 is removed through an incision on the provider to review your right side under the rib cage. health history and Risks and Possible Complications ..... 4 medications and to discuss Preparation and Expectations ......... 5 Nonsurgical pain control options. Your Recovery and Discharge ........... 6 Stone retrieval The day of your operation— Pain Control .................................. 7 For gallstones without symptoms You will not eat or drink for at least 4 hours -

The Spectrum of Gallbladder Disease
The Spectrum of Gallbladder Disease Rebecca Kowalski, M.D. October 18, 2017 Overview A (brief) history of gallbladder surgery Anatomy Anatomical variations Physiology Pathophysiology Diagnostic imaging of the gallbladder Natural history of cholelithiasis Case presentations of the spectrum of gallstone disease Summary History of Gallbladder Surgery Gallbladder Surgery: A Relatively Recent Change Prior to the late 1800s, doctors treated gallbladder disease with a cholecystostomy, due to the fear that removing the organ would kill patients Carl Johann August Langenbuch (director of the Lazarus Hospital in Berlin, Germany) practiced on a cadaver to remove the gallbladder, and in 1882, performed a cholecystectomy on a patient. He was discharged after 6 weeks in the hospital https://en.wikipedia.org/wiki/Carl_Langenbuch By 1897 over 100 cholecystectomies had been performed Gallbladder Surgery: A Relatively Recent Change In 1985, Erich Mühe removed a patient’s gallbladder laparoscopically in Germany Erich Muhe https://openi.nlm.ni h.gov/detailedresult. php?img=PMC30152 In 1987, Philippe Mouret (a 44_jsls-2-4-341- French gynecologic surgeon) g01&req=4 performed a laparoscopic cholecystectomy In 1992, the National Institutes of Health (NIH) created guidelines for laparoscopic cholecystectomy in the United Philippe Mouret States, essentially transforming https://www.pinterest.com surgical practice /pin/58195020154734720/ Anatomy and Abnormal Anatomy http://accesssurgery.mhmedical.com/content.aspx?bookid=1202§ionid=71521210 http://www.slideshare.net/pryce27/rsna-final-2 http://www.slideshare.net/pryce27/rsna-final-2 http://www.slideshare.net/pryce27/rsna-final-2 Physiology a http://www.nature.com/nrm/journal/v2/n9/fig_tab/nrm0901_657a_F3.html Simplified overview of the bile acid biosynthesis pathway derived from cholesterol Lisa D.