Patient Information Leaflet
Total Page:16
File Type:pdf, Size:1020Kb

Load more
Recommended publications
-

The Protean Neurologic Manifestations of Varicella-Zoster Virus Infection
REVIEW MARIA A. NAGEL, MD DONALD H. GILDEN, MD Department of Neurology, University of Departments of Neurology and Microbiology, Colorado Health Sciences Center, Denver University of Colorado Health Sciences Center, Denver The protean neurologic manifestations of varicella-zoster virus infection ■ ABSTRACT ARICELLA-ZOSTER VIRUS (VZV) is an V exclusively human, highly neurotropic Multiple neurologic complications may follow the alphaherpesvirus. Primary infection causes reactivation of varicella-zoster virus (VZV), including chickenpox, after which the virus becomes herpes zoster (also known as zoster or shingles), latent in cranial nerve ganglia, dorsal root postherpetic neuralgia, vasculopathy, myelitis, necrotizing ganglia, and autonomic ganglia along the retinitis, and zoster sine herpete (pain without rash). entire neuraxis. Decades later, VZV can reac- These conditions can be difficult to recognize, especially tivate to cause a number of neurologic condi- as several can occur without rash. tions. This article discusses the protean manifes- ■ KEY POINTS tations of VZV reactivation and their diagno- sis and treatment. The most common sequela of herpes zoster is postherpetic neuralgia, which can persist for months and ■ VZV REACTIVATION sometimes years after the rash resolves. HAS MANY MANIFESTATIONS VZV vasculopathy can present as transient ischemic VZV reactivation can produce a number of neurologic complications: attacks, ischemic or hemorrhagic stroke, or aneurysm. •Herpes zoster (shingles), manifesting as pain and rash in up to three dermatomes Vasculopathy and neurologic complications of VZV are • Postherpetic neuralgia, the most common best diagnosed by detecting VZV DNA in bodily fluids or sequela of zoster, is pain that persists for tissues or anti-VZV immunoglobulin G in the months and sometimes years after the rash cerebrospinal fluid. -
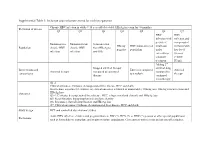
Inclusion and Exclusion Criteria for Each Key Question
Supplemental Table 1: Inclusion and exclusion criteria for each key question Chronic HBV infection in adults ≥ 18 year old (detectable HBsAg in serum for >6 months) Definition of disease Q1 Q2 Q3 Q4 Q5 Q6 Q7 HBV HBV infection with infection and persistent compensated Immunoactive Immunotolerant Seroconverted HBeAg HBV mono-infected viral load cirrhosis with Population chronic HBV chronic HBV from HBeAg to negative population under low level infection infection anti-HBe entecavir or viremia tenofovir (<2000 treatment IU/ml) Adding 2nd Stopped antiviral therapy antiviral drug Interventions and Entecavir compared Antiviral Antiviral therapy compared to continued compared to comparisons to tenofovir therapy therapy continued monotherapy Q1-2: Clinical outcomes: Cirrhosis, decompensated liver disease, HCC and death Intermediate outcomes (if evidence on clinical outcomes is limited or unavailable): HBsAg loss, HBeAg seroconversion and Outcomes HBeAg loss Q3-4: Cirrhosis, decompensated liver disease, HCC, relapse (viral and clinical) and HBsAg loss Q5: Renal function, hypophosphatemia and bone density Q6: Resistance, flare/decompensation and HBeAg loss Q7: Clinical outcomes: Cirrhosis, decompensated liver disease, HCC and death Study design RCT and controlled observational studies Acute HBV infection, children and pregnant women, HIV (+), HCV (+) or HDV (+) persons or other special populations Exclusions such as hemodialysis, transplant, and treatment failure populations. Co treatment with steroids and uncontrolled studies. Supplemental Table 2: Detailed Search Strategy: Ovid Database(s): Embase 1988 to 2014 Week 37, Ovid MEDLINE(R) In-Process & Other Non- Indexed Citations and Ovid MEDLINE(R) 1946 to Present, EBM Reviews - Cochrane Central Register of Controlled Trials August 2014, EBM Reviews - Cochrane Database of Systematic Reviews 2005 to July 2014 Search Strategy: # Searches Results 1 exp Hepatitis B/dt 26410 ("hepatitis B" or "serum hepatitis" or "hippie hepatitis" or "injection hepatitis" or 2 178548 "hepatitis type B").mp. -

CDK4/6 Inhibitors in Breast Cancer Treatment: Potential Interactions with Drug, Gene and Pathophysiological Conditions
Review CDK4/6 Inhibitors in Breast Cancer Treatment: Potential Interactions with Drug, Gene and Pathophysiological Conditions Rossana Roncato 1,*,†, Jacopo Angelini 2,†, Arianna Pani 2,3,†, Erika Cecchin 1, Andrea Sartore-Bianchi 2,4, Salvatore Siena 2,4, Elena De Mattia 1, Francesco Scaglione 2,3,‡ and Giuseppe Toffoli 1,‡ 1 1 Experimental and Clinical Pharmacology Unit, Centro di Riferimento Oncologico (CRO), IRCCS, 33081 Aviano, Italy; [email protected] (E.C.); [email protected] (E.D.M.); [email protected] (G.T.) 2 Department of Oncology and Hemato-Oncology, Università degli Studi di Milano, 20122 Milan, Italy; [email protected] (J.A.); [email protected] (A.P.); [email protected] (A.S-B.); [email protected] (S.S.); [email protected] (F.S.) 3 Clinical Pharmacology Unit, ASST Grande Ospedale Metropolitano Niguarda, Piazza dell'Ospedale Maggiore 3, 20162 Milan, Italy 4 Department of Hematology and Oncology, Niguarda Cancer Center, Grande Ospedale Metropolitano Niguarda, 20162 Milan, Italy * Correspondence: [email protected]; Tel.:+390434659130 † These authors contributed equally. ‡ These authors share senior authorship. Int. J. Mol. Sci. 2020, 21, x; doi: www.mdpi.com/journal/ijms Int. J. Mol. Sci. 2020, 21, x 2 of 8 Table S1. Co-administered agents categorized according to their potential risk for Drug-Drug interaction (DDI) in combination with CDK4/6 inhibitors (CDKis). Colors suggest the risk of DDI with CDKis: green, low risk DDI; orange, moderate risk DDI; red, high risk DDI. ADME, absorption, distribution, metabolism, and excretion; GI, Gastrointestinal; TdP, Torsades de Pointes; NTI, narrow therapeutic index. * Cardiological toxicity should be considered especially for ribociclib due to the QT prolongation. -

Prediction of Premature Termination Codon Suppressing Compounds for Treatment of Duchenne Muscular Dystrophy Using Machine Learning
Prediction of Premature Termination Codon Suppressing Compounds for Treatment of Duchenne Muscular Dystrophy using Machine Learning Kate Wang et al. Supplemental Table S1. Drugs selected by Pharmacophore-based, ML-based and DL- based search in the FDA-approved drugs database Pharmacophore WEKA TF 1-Palmitoyl-2-oleoyl-sn-glycero-3- 5-O-phosphono-alpha-D- (phospho-rac-(1-glycerol)) ribofuranosyl diphosphate Acarbose Amikacin Acetylcarnitine Acetarsol Arbutamine Acetylcholine Adenosine Aldehydo-N-Acetyl-D- Benserazide Acyclovir Glucosamine Bisoprolol Adefovir dipivoxil Alendronic acid Brivudine Alfentanil Alginic acid Cefamandole Alitretinoin alpha-Arbutin Cefdinir Azithromycin Amikacin Cefixime Balsalazide Amiloride Cefonicid Bethanechol Arbutin Ceforanide Bicalutamide Ascorbic acid calcium salt Cefotetan Calcium glubionate Auranofin Ceftibuten Cangrelor Azacitidine Ceftolozane Capecitabine Benserazide Cerivastatin Carbamoylcholine Besifloxacin Chlortetracycline Carisoprodol beta-L-fructofuranose Cilastatin Chlorobutanol Bictegravir Citicoline Cidofovir Bismuth subgallate Cladribine Clodronic acid Bleomycin Clarithromycin Colistimethate Bortezomib Clindamycin Cyclandelate Bromotheophylline Clofarabine Dexpanthenol Calcium threonate Cromoglicic acid Edoxudine Capecitabine Demeclocycline Elbasvir Capreomycin Diaminopropanol tetraacetic acid Erdosteine Carbidopa Diazolidinylurea Ethchlorvynol Carbocisteine Dibekacin Ethinamate Carboplatin Dinoprostone Famotidine Cefotetan Dipyridamole Fidaxomicin Chlormerodrin Doripenem Flavin adenine dinucleotide -

New Zealand Data Sheet – Tradename (Active Ingredient)
NEW ZEALAND DATA SHEET NEW ZEALAND DATA SHEET FLUOROURACIL EBEWE (FLUOROURACIL) 1. PRODUCT NAME Fluorouracil Ebewe 50 mg/mL solution for injection 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Fluorouracil Ebewe 250 mg/5 mL contains 250 mg fluorouracil*. Fluorouracil Ebewe 500 mg/10 mL contains 100 mg fluorouracil*. Fluorouracil Ebewe 1000 mg/20 mL contains 1000 mg fluorouracil. Fluorouracil Ebewe 2500 mg/50 mL contains 2500 mg fluorouracil. Fluorouracil Ebewe 5000 mg/100 mL contains 5000 mg fluorouracil. For the full list of excipients, see Section 6.1 List of excipients. *Not supplied in New Zealand 3. PHARMACEUTICAL FORM Fluorouracil Ebewe is a sterile solution of fluorouracil for use as an intravenous infusion or injection. The pH of the fluorouracil injection solution is approximately 8.9. 4. CLINICAL PARTICULARS 4.1. THERAPEUTIC INDICATIONS Alone or in combination, for the palliative treatment of malignant tumours, particularly of the breast, colon or rectum; and in the treatment of gastric, primary hepatic, pancreatic, uterine (cervical particularly), ovarian and bladder carcinomas. Fluorouracil should only be used when other proven measures have failed or are considered impractical. 4.2. DOSE AND METHOD OF ADMINISTRATION General Directions Fluorouracil Ebewe contains no antimicrobial agent. The product is for single use in one patient only. Discard any residue. To reduce microbiological hazard, use as soon as practicable after reconstitution/preparation. If storage is necessary, hold at 2°C to 8°C for not more than 24 hours after preparation. Administration should be completed within 24 hours of preparation of the infusion and any residue discarded according to the guidelines for the disposal of cytotoxic drugs (see Section 6.6 Special precautions for disposal). -

PRODUCT INFORMATION Brivudine Item No
PRODUCT INFORMATION Brivudine Item No. 29448 CAS Registry No.: 69304-47-8 Formal Name: 5-[(1E)-2-bromoethenyl]-2′-deoxy-uridine OH Synonym: BVDU OH MF: C11H13BrN2O5 H Br FW: 333.1 N O Purity: ≥98% UV/Vis.: λ: 251, 294 nm max OO Supplied as: A crystalline solid N Storage: -20°C H Stability: ≥2 years Information represents the product specifications. Batch specific analytical results are provided on each certificate of analysis. Laboratory Procedures Brivudine is supplied as a crystalline solid. A stock solution may be made by dissolving the brivudine in the solvent of choice, which should be purged with an inert gas. Brivudine is soluble in organic solvents such as ethanol, DMSO, and dimethyl formamide (DMF). The solubility of brivudine in ethanol is approximately 10 mg/ml and approximately 30 mg/ml in DMSO and DMF. Further dilutions of the stock solution into aqueous buffers or isotonic saline should be made prior to performing biological experiments. Ensure that the residual amount of organic solvent is insignificant, since organic solvents may have physiological effects at low concentrations. Organic solvent-free aqueous solutions of brivudine can be prepared by directly dissolving the crystalline solid in aqueous buffers. The solubility of brivudine in PBS, pH 7.2, is approximately 0.5 mg/ml. We do not recommend storing the aqueous solution for more than one day. Description Brivudine is a thymidine analog and inhibitor of herpes simplex virus 1 (HSV-1) and varicella-zoster virus (VZV) viral replication.1,2 Following conversion to a 5’-triphosphate form by viral kinases, brivudine is incorporated into viral DNA, inhibiting viral DNA polymerases and inducing strand breakage.2 Brivudine (0.02-0.04 μg/ml) inhibits VZV replication in primary human fibroblasts and inhibits cytopathogenic 1,3 effects of the KOS HSV-1 strain in a panel of cell lines (MIC50s = 0.007-0.4 μg/ml). -

Silibinin Component for the Treatment of Hepatitis Silbininkomponente Zur Behandlung Von Hepatitis Composant De Silibinine Pour Le Traitement De L’Hépatite
(19) & (11) EP 2 219 642 B1 (12) EUROPEAN PATENT SPECIFICATION (45) Date of publication and mention (51) Int Cl.: of the grant of the patent: A61K 31/357 (2006.01) A61P 1/16 (2006.01) 21.09.2011 Bulletin 2011/38 A61P 31/12 (2006.01) (21) Application number: 08849759.9 (86) International application number: PCT/EP2008/009659 (22) Date of filing: 14.11.2008 (87) International publication number: WO 2009/062737 (22.05.2009 Gazette 2009/21) (54) SILIBININ COMPONENT FOR THE TREATMENT OF HEPATITIS SILBININKOMPONENTE ZUR BEHANDLUNG VON HEPATITIS COMPOSANT DE SILIBININE POUR LE TRAITEMENT DE L’HÉPATITE (84) Designated Contracting States: (56) References cited: AT BE BG CH CY CZ DE DK EE ES FI FR GB GR WO-A-02/067853 GB-A- 2 167 414 HR HU IE IS IT LI LT LU LV MC MT NL NO PL PT RO SE SI SK TR • POLYAK STEPHEN J ET AL: "Inhibition of T- cell inflammatory cytokines, hepatocyte NF-kappa B (30) Priority: 15.11.2007 EP 07022187 signaling, and HCV infection by standardized 15.11.2007 US 988168 P silymarin" GASTROENTEROLOGY, vol. 132, no. 25.03.2008 EP 08005459 5, May 2007 (2007-05), pages 1925-1936, XP002477920 ISSN: 0016-5085 (43) Date of publication of application: • MAYER K E ET AL: "Silymarin treatment of viral 25.08.2010 Bulletin 2010/34 hepatitis: A systematic review" JOURNAL OF VIRAL HEPATITIS 200511 GB, vol. 12, no. 6, (60) Divisional application: November 2005 (2005-11), pages 559-567, 11005445.9 XP002477921 ISSN: 1352-0504 1365-2893 • CHAVEZ M L: "TREATMENT OF HEPATITIS C (73) Proprietor: Madaus GmbH WITH MILK THISTLE?" JOURNAL OF HERBAL 51067 Köln (DE) PHARMACOTHERAPY, HAWORTH HERBAL PRESS, BINGHAMTON, US, vol. -

Tenofovir, Another Inexpensive, Well-Known and Widely Available Old Drug Repurposed for SARS-COV-2 Infection
pharmaceuticals Review Tenofovir, Another Inexpensive, Well-Known and Widely Available Old Drug Repurposed for SARS-COV-2 Infection Isabella Zanella 1,2,* , Daniela Zizioli 1, Francesco Castelli 3 and Eugenia Quiros-Roldan 3 1 Department of Molecular and Translational Medicine, University of Brescia, 25123 Brescia, Italy; [email protected] 2 Clinical Chemistry Laboratory, Cytogenetics and Molecular Genetics Section, Diagnostic Department, ASST Spedali Civili di Brescia, Piazzale Spedali Civili 1, 25123 Brescia, Italy 3 University Department of Infectious and Tropical Diseases, University of Brescia and ASST Spedali Civili di Brescia, Piazzale Spedali Civili 1, 25123 Brescia, Italy; [email protected] (F.C.); [email protected] (E.Q.-R.) * Correspondence: [email protected]; Tel.: +39-030-399-6806 Abstract: Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection is spreading worldwide with different clinical manifestations. Age and comorbidities may explain severity in critical cases and people living with human immunodeficiency virus (HIV) might be at particularly high risk for severe progression. Nonetheless, current data, although sometimes contradictory, do not confirm higher morbidity, risk of more severe COVID-19 or higher mortality in HIV-infected people with complete access to antiretroviral therapy (ART). A possible protective role of ART has been hypothesized to explain these observations. Anti-viral drugs used to treat HIV infection have been repurposed for COVID-19 treatment; this is also based on previous studies on severe acute respiratory syndrome virus (SARS-CoV) and Middle East respiratory syndrome virus (MERS-CoV). Among Citation: Zanella, I.; Zizioli, D.; them, lopinavir/ritonavir, an inhibitor of viral protease, was extensively used early in the pandemic Castelli, F.; Quiros-Roldan, E. -

The Evolution of Antiviral Therapy for External Ocular Viral Infections Over Twenty-Five Years
Cornea 19(5): 673–680, 2000. © 2000 Lippincott Williams & Wilkins, Inc., Philadelphia The Evolution of Antiviral Therapy for External Ocular Viral Infections Over Twenty-five Years Y. Jerold Gordon, M.D. Purpose. To review the past 25 years of the evolution of antiviral levels on the corneal surface. By 1975, IDU was the treatment of therapy for the treatment of common external ocular viral infec- choice for herpetic epithelial keratitis worldwide. However, the tions (herpes simplex virus type 1, varicella-zoster virus, and ad- shortcomings of topical IDU therapy: significant toxicity (super- enovirus). Methods. A broad-based literature review in the fields ficial punctate keratitis, chemical conjunctivitis, and punctal oc- of virology, antiviral research, and ophthalmology will be carried clusion) and frequent hypersensitivity reactions, limited its useful- out. The pathogenesis of the major external ocular viral infections ness. As an insoluble agent, it had no therapeutic effect on herpetic and history of antiviral development will be cited. Important con- ceptual breakthroughs as well as historical landmarks will be em- stromal keratitis or iritis. Today, IDU is used infrequently in de- phasized. Results. The successful development of effective anti- veloped nations because it has been replaced by better drugs. How- virals to treat the most common external ocular viral infections ever, it remains effective and is used in developing nations where have dramatically reduced morbidity and sight loss. The immune cost issues are critical. pathogenesis of herpetic stromal keratitis is better understood. In the mid-1970s, several promising strategies to treat HSV Conclusions. Remarkable progress in the development of antiviral epithelial keratitis failed. -

Interactions with HBV Treatment
www.hep-druginteractions.org Interactions with HBV Treatment Charts revised September 2021. Full information available at www.hep-druginteractions.org Page 1 of 6 Please note that if a drug is not listed it cannot automatically be assumed it is safe to coadminister. ADV, Adefovir; ETV, Entecavir; LAM, Lamivudine; PEG IFN, Peginterferon; RBV, Ribavirin; TBV, Telbivudine; TAF, Tenofovir alafenamide; TDF, Tenofovir-DF. ADV ETV LAM PEG PEG RBV TBV TAF TDF ADV ETV LAM PEG PEG RBV TBV TAF TDF IFN IFN IFN IFN alfa-2a alfa-2b alfa-2a alfa-2b Anaesthetics & Muscle Relaxants Antibacterials (continued) Bupivacaine ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ Cloxacillin ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ Cisatracurium ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ Dapsone ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ Isoflurane ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ Delamanid ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ Ketamine ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ Ertapenem ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ Nitrous oxide ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ Erythromycin ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ Propofol ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ Ethambutol ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ Thiopental ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ Flucloxacillin ◆ ◆ ◆ ◆ ◆ ◆ Tizanidine ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ Gentamicin ◆ ◆ ◆ ◆ ◆ ◆ Analgesics Imipenem ◆ ◆ ◆ ◆ ◆ ◆ ◆ Aceclofenac ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ Isoniazid ◆ ◆ ◆ ◆ ◆ ◆ Alfentanil ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ Levofloxacin ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ Aspirin ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ Linezolid ◆ ◆ ◆ ◆ ◆ ◆ Buprenorphine ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ Lymecycline ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ Celecoxib ◆ ◆ ◆ ◆ ◆ ◆ ◆ Meropenem ◆ ◆ ◆ ◆ ◆ ◆ Codeine ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ for distribution. for Methenamine ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ Dexketoprofen ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ Metronidazole ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ Dextropropoxyphene ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ ◆ Moxifloxacin ◆ ◆ ◆ -

Surveillance of Antimicrobial Consumption in Europe 2013-2014 SURVEILLANCE REPORT
SURVEILLANCE REPORT SURVEILLANCE REPORT Surveillance of antimicrobial consumption in Europe in Europe consumption of antimicrobial Surveillance Surveillance of antimicrobial consumption in Europe 2013-2014 2012 www.ecdc.europa.eu ECDC SURVEILLANCE REPORT Surveillance of antimicrobial consumption in Europe 2013–2014 This report of the European Centre for Disease Prevention and Control (ECDC) was coordinated by Klaus Weist. Contributing authors Klaus Weist, Arno Muller, Ana Hoxha, Vera Vlahović-Palčevski, Christelle Elias, Dominique Monnet and Ole Heuer. Data analysis: Klaus Weist, Arno Muller and Ana Hoxha. Acknowledgements The authors would like to thank the ESAC-Net Disease Network Coordination Committee members (Marcel Bruch, Philippe Cavalié, Herman Goossens, Jenny Hellman, Susan Hopkins, Stephanie Natsch, Anna Olczak-Pienkowska, Ajay Oza, Arjana Tambić Andrasevic, Peter Zarb) and observers (Jane Robertson, Arno Muller, Mike Sharland, Theo Verheij) for providing valuable comments and scientific advice during the production of the report. All ESAC-Net participants and National Coordinators are acknowledged for providing data and valuable comments on this report. The authors also acknowledge Gaetan Guyodo, Catalin Albu and Anna Renau-Rosell for managing the data and providing technical support to the participating countries. Suggested citation: European Centre for Disease Prevention and Control. Surveillance of antimicrobial consumption in Europe, 2013‒2014. Stockholm: ECDC; 2018. Stockholm, May 2018 ISBN 978-92-9498-187-5 ISSN 2315-0955 -

Drug Interaction Studies on New Drug Applications: Current Situations and Regulatory Views in Japan
Drug Metab. Pharmacokinet. 25 (1): 3–15 (2010). Review Drug Interaction Studies on New Drug Applications: Current Situations and Regulatory Views in Japan Naomi NAGAI* Office of New Drug IV, Pharmaceuticals and Medical Devices Agency (PMDA), Tokyo, Japan Full text of this paper is available at http://www.jstage.jst.go.jp/browse/dmpk Summary: Drug interaction studies on new drug applications (NDAs) for new molecular entities (NMEs) ap- proved in Japan between 1997 and 2008 are examined in the Pharmaceuticals and Medical Devices Agency (PMDA). The situations of drug interaction studies in NDAs have changed over the past 12 years, especially in metabolizing enzyme and transporter-based drug interactions. Materials and approaches to study drug- metabolizing enzyme-based drug interactions have improved, and become more rational based on mechanis- tic theory and new technologies. On the basis of incremental evidence of transporter roles in human phar- macokinetics, transporter-based drug interactions have been increasingly studied during drug development and submitted in recent NDAs. Some recently approved NMEs include transporter-based drug interaction in- formation in their package inserts (PIs). The regulatory document ``Methods of Drug Interaction Studies,'' in addition to recent advances in science and technology, has also contributed to plan and evaluation of drug in- teraction studies in recent new drug development. This review summarizes current situations and further dis- cussionpointsondruginteractionstudiesinNDAsinJapan. Keywords: