Bones of Lower Limb
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
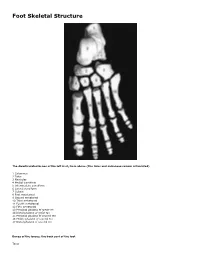
Skeletal Foot Structure
Foot Skeletal Structure The disarticulated bones of the left foot, from above (The talus and calcaneus remain articulated) 1 Calcaneus 2 Talus 3 Navicular 4 Medial cuneiform 5 Intermediate cuneiform 6 Lateral cuneiform 7 Cuboid 8 First metatarsal 9 Second metatarsal 10 Third metatarsal 11 Fourth metatarsal 12 Fifth metatarsal 13 Proximal phalanx of great toe 14 Distal phalanx of great toe 15 Proximal phalanx of second toe 16 Middle phalanx of second toe 17 Distal phalanx of second toe Bones of the tarsus, the back part of the foot Talus Calcaneus Navicular bone Cuboid bone Medial, intermediate and lateral cuneiform bones Bones of the metatarsus, the forepart of the foot First to fifth metatarsal bones (numbered from the medial side) Bones of the toes or digits Phalanges -- a proximal and a distal phalanx for the great toe; proximal, middle and distal phalanges for the second to fifth toes Sesamoid bones Two always present in the tendons of flexor hallucis brevis Origin and meaning of some terms associated with the foot Tibia: Latin for a flute or pipe; the shin bone has a fanciful resemblance to this wind instrument. Fibula: Latin for a pin or skewer; the long thin bone of the leg. Adjective fibular or peroneal, which is from the Greek for pin. Tarsus: Greek for a wicker frame; the basic framework for the back of the foot. Metatarsus: Greek for beyond the tarsus; the forepart of the foot. Talus (astragalus): Latin (Greek) for one of a set of dice; viewed from above the main part of the talus has a rather square appearance. -

June 3, 2016 Karen B. Desalvo, M.D., M.P.H., M.Sc. Acting Assistant
June 3, 2016 Karen B. DeSalvo, M.D., M.P.H., M.Sc. Acting Assistant Secretary Department of Health and Human Services Office of the National Coordinator for Health Information Technology Attention: RFI Regarding Assessing Interoperability for MACRA 330 C Street, SW, Room 7025A Washington, DC 20201 Subject: Office of the National Coordinator for Health Information Technology; Medicare Access and CHIP Reauthorization Act of 2015; Request for Information Regarding Assessing Interoperability for MACRA Dear Acting Assistant Secretary DeSalvo: The American Association of Orthopaedic Surgeons (AAOS) and orthopaedic specialty societies, representing over 18,000 board-certified orthopaedic surgeons, appreciate the opportunity to provide comments on the Request for Information Regarding Assessing Interoperability for MACRA by the Office of the National Coordinator (ONC) for Health Information Technology, and published in the Federal Register on April 8, 2016. The AAOS has been committed to working with ONC in the adoption of electronic health records. As surgical specialists, we have unique Health Information Technology (HIT) needs and respectfully offer some suggestions to improve interoperability to better reflect the needs of our surgical specialists and their patients and accelerate HIT adoption in the future by orthopaedic surgeons. The AAOS thanks ONC in advance for its solicitation and consideration of the following comments and concerns. We have structured our comments in the order that ONC is soliciting public feedback in the RFI document referenced above. Scope of Measurement: Defining Interoperability and Population The focus of measurement should not be limited to “meaningful Electronic Health Records (EHR) users,” as defined (e.g., eligible professionals, eligible hospitals, and CAHs that attest to meaningful use of certified EHR technology under CMS’ Medicare and Medicaid EHR Incentive Programs), and their exchange partners. -

Multiplanar CT Analysis of Fifth Metatarsal Morphology
FAIXXX10.1177/1071100715623041Foot & Ankle InternationalDeSandis et al 623041research-article2015 Article Foot & Ankle International® 2016, Vol. 37(5) 528 –536 Multiplanar CT Analysis of Fifth Metatarsal © The Author(s) 2015 Reprints and permissions: sagepub.com/journalsPermissions.nav Morphology: Implications for Operative DOI: 10.1177/1071100715623041 Management of Zone II Fractures fai.sagepub.com Bridget DeSandis, BA1, Conor Murphy, MD2, Andrew Rosenbaum, MD1, Matthew Levitsky, BA1, Quinn O’Malley1, Gabrielle Konin, MD1, and Mark Drakos, MD1 Abstract Background: Percutaneous internal fixation is currently the method of choice treating proximal zone II fifth metatarsal fractures. Complications have been reported due to poor screw placement and inadequate screw sizing. The purpose of this study was to define the morphology of the fifth metatarsal to help guide surgeons in selecting the appropriate screw size preoperatively. Methods: Multiplanar analysis of fifth metatarsal morphology was completed using computed tomographic (CT) scans from 241 patients. Specific parameters were analyzed and defined in anteroposterior (AP), lateral, and oblique views including metatarsal length, distance from the base to apex of curvature, apex medullary canal width, apex height, and fifth metatarsal angle. Results: The average metatarsal length in the AP view was 71.4 ± 6.1 mm and in the lateral view 70.4 ± 6.0 mm, with 95% of patients having lengths between 59.3 and 83.5 mm and 58.4 and 82.4 mm, respectively. The average canal width at the apex of curvature was 4.1 ± 0.9 mm in the AP view and 5.3 ± 1.1 mm in the lateral view, with 95% of patients having widths between 2.2 and 5.9 mm and 3.2 and 7.5 mm, respectively. -

Rethinking the Evolution of the Human Foot: Insights from Experimental Research Nicholas B
© 2018. Published by The Company of Biologists Ltd | Journal of Experimental Biology (2018) 221, jeb174425. doi:10.1242/jeb.174425 REVIEW Rethinking the evolution of the human foot: insights from experimental research Nicholas B. Holowka* and Daniel E. Lieberman* ABSTRACT presumably owing to their lack of arches and mobile midfoot joints Adaptive explanations for modern human foot anatomy have long for enhanced prehensility in arboreal locomotion (see Glossary; fascinated evolutionary biologists because of the dramatic differences Fig. 1B) (DeSilva, 2010; Elftman and Manter, 1935a). Other studies between our feet and those of our closest living relatives, the great have documented how great apes use their long toes, opposable apes. Morphological features, including hallucal opposability, toe halluces and mobile ankles for grasping arboreal supports (DeSilva, length and the longitudinal arch, have traditionally been used to 2009; Holowka et al., 2017a; Morton, 1924). These observations dichotomize human and great ape feet as being adapted for bipedal underlie what has become a consensus model of human foot walking and arboreal locomotion, respectively. However, recent evolution: that selection for bipedal walking came at the expense of biomechanical models of human foot function and experimental arboreal locomotor capabilities, resulting in a dichotomy between investigations of great ape locomotion have undermined this simple human and great ape foot anatomy and function. According to this dichotomy. Here, we review this research, focusing on the way of thinking, anatomical features of the foot characteristic of biomechanics of foot strike, push-off and elastic energy storage in great apes are assumed to represent adaptations for arboreal the foot, and show that humans and great apes share some behavior, and those unique to humans are assumed to be related underappreciated, surprising similarities in foot function, such as to bipedal walking. -

Common Stress Fractures BRENT W
COVER ARTICLE PRACTICAL THERAPEUTICS Common Stress Fractures BRENT W. SANDERLIN, LCDR, MC, USNR, Naval Branch Medical Clinic, Fort Worth, Texas ROBERT F. RASPA, CAPT, MC, USN, Naval Hospital Jacksonville, Jacksonville, Florida Lower extremity stress fractures are common injuries most often associated with partic- ipation in sports involving running, jumping, or repetitive stress. The initial diagnosis can be made by identifying localized bone pain that increases with weight bearing or repet- itive use. Plain film radiographs are frequently unrevealing. Confirmation of a stress frac- ture is best made using triple phase nuclear medicine bone scan or magnetic resonance imaging. Prevention of stress fractures is most effectively accomplished by increasing the level of exercise slowly, adequately warming up and stretching before exercise, and using cushioned insoles and appropriate footwear. Treatment involves rest of the injured bone, followed by a gradual return to the sport once free of pain. Recent evidence sup- ports the use of air splinting to reduce pain and decrease the time until return to full par- ticipation or intensity of exercise. (Am Fam Physician 2003;68:1527-32. Copyright© 2003 American Academy of Family Physicians) tress fractures are among the involving repetitive use of the arms, such most common sports injuries as baseball or tennis. Stress fractures of and are frequently managed the ribs occur in sports such as rowing. by family physicians. A stress Upper extremity and rib stress fractures fracture should be suspected in are far less common than lower extremity Sany patient presenting with localized stress fractures.1 bone or periosteal pain, especially if he or she recently started an exercise program Etiology and Pathophysiology or increased the intensity of exercise. -

Compiled for Lower Limb
Updated: December, 9th, 2020 MSI ANATOMY LAB: STRUCTURE LIST Lower Extremity Lower Extremity Osteology Hip bone Tibia • Greater sciatic notch • Medial condyle • Lesser sciatic notch • Lateral condyle • Obturator foramen • Tibial plateau • Acetabulum o Medial tibial plateau o Lunate surface o Lateral tibial plateau o Acetabular notch o Intercondylar eminence • Ischiopubic ramus o Anterior intercondylar area o Posterior intercondylar area Pubic bone (pubis) • Pectineal line • Tibial tuberosity • Pubic tubercle • Medial malleolus • Body • Superior pubic ramus Patella • Inferior pubic ramus Fibula Ischium • Head • Body • Neck • Ramus • Lateral malleolus • Ischial tuberosity • Ischial spine Foot • Calcaneus Ilium o Calcaneal tuberosity • Iliac fossa o Sustentaculum tali (talar shelf) • Anterior superior iliac spine • Anterior inferior iliac spine • Talus o Head • Posterior superior iliac spine o Neck • Posterior inferior iliac spine • Arcuate line • Navicular • Iliac crest • Cuboid • Body • Cuneiforms: medial, intermediate, and lateral Femur • Metatarsals 1-5 • Greater trochanter • Phalanges 1-5 • Lesser trochanter o Proximal • Head o Middle • Neck o Distal • Linea aspera • L • Lateral condyle • L • Intercondylar fossa (notch) • L • Medial condyle • L • Lateral epicondyle • L • Medial epicondyle • L • Adductor tubercle • L • L • L • L • 1 Updated: December, 9th, 2020 Lab 3: Anterior and Medial Thigh Anterior Thigh Medial thigh General Structures Muscles • Fascia lata • Adductor longus m. • Anterior compartment • Adductor brevis m. • Medial compartment • Adductor magnus m. • Great saphenous vein o Adductor hiatus • Femoral sheath o Compartments and contents • Pectineus m. o Femoral canal and ring • Gracilis m. Muscles & Associated Tendons Nerves • Tensor fasciae lata • Obturator nerve • Iliotibial tract (band) • Femoral triangle: Boundaries Vessels o Inguinal ligament • Obturator artery o Sartorius m. • Femoral artery o Adductor longus m. -

Injuries to the Lower Extremity II
Injury to lower extremity InjuriesInjuries toto thethe lowerlower extremityextremity IIII Aree Tanavalee MD Associate Professor Department of Orthopaedics Faculty of Medicine Chulalongkorn University Injury to lower extremity TopicsTopics • Fracture of the shaft of the femur • Fractures around the knee • Knee dislocation and fracture dislocation • Fractures of tibia and fibular • Fractures around the ankle • Fracture and fracture dislocation of the foot Injury to lower extremity CommonCommon symptomssymptoms andand signssigns ofof fracturesfractures – Pain – Deformity – Shortening – Swelling – Ecchymosed – Loss of function – Open injury • Gross finding of fractures Injury to lower extremity RadiographicRadiographic evaluationevaluation forfor fracturesfractures • At least, 2 different planes of Fx site – Includes joint above and below – Some types of Fx, special views – Sometimes, 2 different times – Sometimes, calls second opinion Injury to lower extremity ComplicationsComplications ofof fracturesfractures • General – Delayed union – Nonunion – Malunion – Shortening – Infection • Severe – Neurovascular injuries – Compartment syndrome – Fat embolism – Adult respiratory distress syndrome (ARDS) Injury to lower extremity FatFat embolismembolism • Common in Fx of long bone and pelvis • Multiple Fxs >> single Fx • Respiratory insufficiency • Usually manifests within 48 hr • Clinical – Fever – Tachepnea – Tachycardia – Alters consciousness • Treatment – Respiratory support – Early Fx stabilization Injury to lower extremity CompartmentCompartment -

Anatomy: Lower Leg, Knee, & Patella Positioning
Reading assignment: Lower Leg Anatomy: lower leg, knee, & Merrils, Vol. 1: Chapter 6 Film Critique #3 patella Lab demonstration Positioning: lower leg Positioning: knee Reading assignment: Knee Merrils, Vol. 1: Chapter 6 Film Critique #4 & Lab demonstration Positioning: intercondylar fossa Reading assignment: Intercondylar fossa and patella & patella Merrils, Vol. 1: Chapter 6 Lab demonstration Anatomy: Femur Reading assignment: Femur Positioning: Femur Merrils, Vol. 1: Chapters 6 & 7 Film Critique #5 Lab demonstration Leg…… The leg is composed of two long bones: Tibia – medial bone; second largest bone in the body Fibula – lateral bone The tibia has several anatomical features of note. See whether you can locate each on the diagram. Proximal end: Medial condyle Lateral condyle Tibial plateaus Intercondylar eminence Tibial tuberosity Body – features anterior crest Distal end: Medial malleolus Fibular notch The head of the fibula is located at its proximal end and has a pointed apex laterally. Distally, the fibular features the lateral malleolus. The articulations between the two leg bones are discussed on Screen 1.13. Knee….. The knee joint is the articulation between the femoral condyles and the tibial plateaus. Numerous soft tissues support and reinforce the knee, including the: Menisci Cruciate ligaments Collateral ligaments These supporting soft tissue structures are enclosed in a common joint capsule. The knee joint is of the hinge type, capable of flexion and extension only. The anterior knee joint is protected by the patella and patellofemoral joint. The patella is the largest and most constant sesamoid bone. It develops in the quadriceps femoris tendon between the ages of 3 and 5 years. -

Morphometric Study of Tibial Condylar Area in the North Indian Population. Ankit Srivastava1, Dr
JMSCR Volume||2||Issue||3||Page515-519||March 2014 2014 www.jmscr.igmpublication.org Impact Factcor-1.1147 ISSN (e)-2347-176x Morphometric Study of Tibial Condylar area in the North Indian Population. Ankit Srivastava1, Dr. Anjoo Yadav2, Prof. R.J. Thomas3, Ms. Neha Gupta4 1Tutor in AIIMS Bhopal. 2Lecturer in Govt. medical college, Kannauj. 3Professor in Govt. medical college, Kannauj. 4Tutor in Govt. medical college, Kannauj. Email: [email protected] Abstract: The upper end of tibia is expanded to form a mass that consists of two parts: lateral and medial condyles which articulate with the corresponding condylar surfaces of the femur. Separating these two condyles is the intercondylar area whose central part is raised to form the intercondylar eminence. The present study will give information of the exact dimensions and percentage covered by medial and lateral condyles out of total condylar area. This study was undertaken to collect metrical data about the medial and lateral condyles of tibia. The present study was performed on 150 dry tibia of north Indian subjects, Out of which 70 tibia belonged to right side and 80 were of left side. The age and sex of these bones were not known. The anteroposterior length of medial and lateral tibial condylar area was measured along with their transverse diameter. The data was statistically analyzed to hold comparisons between tibia of right and left side and also between medial and lateral tibial condyles of the same side. The area covered by MTC is 38.56% and by LTC is 35.97% out of total condylar area in right side. -

Anatomy, Bony Pelvis and Lower Limb, Leg Bones
NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health. StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2018 Jan-. Anatomy, Bony Pelvis and Lower Limb, Leg Bones Authors Austin J. Cantrell1; Matthew Varacallo2. Affiliations 1 University of Oklahoma College of Med. 2 Department of Orthopaedic Surgery, University of Kentucky School of Medicine Last Update: January 17, 2019. Introduction The leg is the region of the lower limb between the knee and the foot. It comprises two bones: the tibia and the fibula. The role of these two bones is to provide stability and support to the rest of the body, and through articulations with the femur and foot/ankle and the muscles attached to these bones, provide mobility and the ability to ambulate in an upright position. The tibia articulates with the femur at the knee joint. The knee joint consists of three compartments [1][2] medial tibiofemoral compartment lateral tibiofemoral compartment patellofemoral compartment At the ankle, the tibia and fibula create the articular surface for the talus. The ankle mortise is a specialized articulation providing support and optimizing motion and function through the ankle joint. A normal ankle joint ultimately optimizes and allows for physiologic mobility of the foot and its associated joints and articulations. The bones and fascia also divide the lower leg into four compartments [3][4] anterior compartment lateral compartment posterior compartment, superficial posterior compartment, deep Structure and Function The tibia is the second largest bone in the body and provides support for a significant portion of the weight-bearing forces transmitted from the rest of the body. -

Anatomy of the Knee Bony Structures Quad Muscles
Anatomy of the Knee Bony Structures Quad muscles - Tibia: proximal end forms tibial plateaus, tibial plateaus, articulates with Tendon femoral condyles. o Knee hinge joint flexion/extension Patellar tendon o Tibial plateaus separated by intercodylar tubercles . Medial and lateral tubercle Tibial tuberosity Lateral tibial plateau is smaller compare to medial . Tibial plateaus slope posteriorly o Cruciate ligaments and meniscus attach anterior and posterior to tubercles Fibular head o Distal to plateaus is tibial tuberosity . Common insertion for patellar tendon Lateral condyle o Distal and anterior to plateaus are lateral and medial condyles . Lateral condyle has facet that articulates with head of fibula IT Band Facet = extremely smooth surface of bone o Medial to lateral condyle is Gerdys tubercle o GERDYS tubercle – point of muscular attachment - Femur: medial/lateral condyle o Medial condyle is longer than lateral and slightly more distal o Slight external rotation at terminal (full) extension o Femoral condyles project more posterior than they do anterior o Groove between condyles, anteriorly is trochlear or patello- femoral groove o Posteriorly the condyles are separated by intercodylar notch (fossa) . Notch more narrow in women o Linea aspera: longitudinal ridge on posterior surface of femur (rough line) o Medial and lateral super condylar lines: lines running from each femoral condyle posteriorly to the linea aspera o Femur is longest and strongest bone o Directly superior to condyle is epicondyle (epi – above) o On medial side of medial epicondyle is adductor tubercle . Serves as point of attachment for adductor magnus muscle o Small groove present within medial and lateral condyle to accommodate the medial and lateral meniscus (very shallow) - Patella o Largest Sesamoid bone in body o Rounded, triangular bond and has only one articulation with femur o Can only dislocated laterally o Posterior surface has 3 facets . -

The Muscles That Act on the Lower Limb Fall Into Three Groups: Those That Move the Thigh, Those That Move the Lower Leg, and Those That Move the Ankle, Foot, and Toes
MUSCLES OF THE APPENDICULAR SKELETON LOWER LIMB The muscles that act on the lower limb fall into three groups: those that move the thigh, those that move the lower leg, and those that move the ankle, foot, and toes. Muscles Moving the Thigh (Marieb / Hoehn – Chapter 10; Pgs. 363 – 369; Figures 1 & 2) MUSCLE: ORIGIN: INSERTION: INNERVATION: ACTION: ANTERIOR: Iliacus* iliac fossa / crest lesser trochanter femoral nerve flexes thigh (part of Iliopsoas) of os coxa; ala of sacrum of femur Psoas major* lesser trochanter --------------- T – L vertebrae flexes thigh (part of Iliopsoas) 12 5 of femur (spinal nerves) iliac crest / anterior iliotibial tract Tensor fasciae latae* superior iliac spine gluteal nerves flexes / abducts thigh (connective tissue) of ox coxa anterior superior iliac spine medial surface flexes / adducts / Sartorius* femoral nerve of ox coxa of proximal tibia laterally rotates thigh lesser trochanter adducts / flexes / medially Pectineus* pubis obturator nerve of femur rotates thigh Adductor brevis* linea aspera adducts / flexes / medially pubis obturator nerve (part of Adductors) of femur rotates thigh Adductor longus* linea aspera adducts / flexes / medially pubis obturator nerve (part of Adductors) of femur rotates thigh MUSCLE: ORIGIN: INSERTION: INNERVATION: ACTION: linea aspera obturator nerve / adducts / flexes / medially Adductor magnus* pubis / ischium (part of Adductors) of femur sciatic nerve rotates thigh medial surface adducts / flexes / medially Gracilis* pubis / ischium obturator nerve of proximal tibia rotates