Morphometric Study of Tibial Condylar Area in the North Indian Population. Ankit Srivastava1, Dr
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

List: Bones & Bone Markings of Appendicular Skeleton and Knee
List: Bones & Bone markings of Appendicular skeleton and Knee joint Lab: Handout 4 Superior Appendicular Skeleton I. Clavicle (Left or Right?) A. Acromial End B. Conoid Tubercle C. Shaft D. Sternal End II. Scapula (Left or Right?) A. Superior border (superior margin) B. Medial border (vertebral margin) C. Lateral border (axillary margin) D. Scapular notch (suprascapular notch) E. Acromion Process F. Coracoid Process G. Glenoid Fossa (cavity) H. Infraglenoid tubercle I. Subscapular fossa J. Superior & Inferior Angle K. Scapular Spine L. Supraspinous Fossa M. Infraspinous Fossa III. Humerus (Left or Right?) A. Head of Humerus B. Anatomical Neck C. Surgical Neck D. Greater Tubercle E. Lesser Tubercle F. Intertubercular fossa (bicipital groove) G. Deltoid Tuberosity H. Radial Groove (groove for radial nerve) I. Lateral Epicondyle J. Medial Epicondyle K. Radial Fossa L. Coronoid Fossa M. Capitulum N. Trochlea O. Olecranon Fossa IV. Radius (Left or Right?) A. Head of Radius B. Neck C. Radial Tuberosity D. Styloid Process of radius E. Ulnar Notch of radius V. Ulna (Left or Right?) A. Olecranon Process B. Coronoid Process of ulna C. Trochlear Notch of ulna Human Anatomy List: Bones & Bone markings of Appendicular skeleton and Knee joint Lab: Handout 4 D. Radial Notch of ulna E. Head of Ulna F. Styloid Process VI. Carpals (8) A. Proximal row (4): Scaphoid, Lunate, Triquetrum, Pisiform B. Distal row (4): Trapezium, Trapezoid, Capitate, Hamate VII. Metacarpals: Numbered 1-5 A. Base B. Shaft C. Head VIII. Phalanges A. Proximal Phalanx B. Middle Phalanx C. Distal Phalanx ============================================================================= Inferior Appendicular Skeleton IX. Os Coxae (Innominate bone) (Left or Right?) A. -

Compiled for Lower Limb
Updated: December, 9th, 2020 MSI ANATOMY LAB: STRUCTURE LIST Lower Extremity Lower Extremity Osteology Hip bone Tibia • Greater sciatic notch • Medial condyle • Lesser sciatic notch • Lateral condyle • Obturator foramen • Tibial plateau • Acetabulum o Medial tibial plateau o Lunate surface o Lateral tibial plateau o Acetabular notch o Intercondylar eminence • Ischiopubic ramus o Anterior intercondylar area o Posterior intercondylar area Pubic bone (pubis) • Pectineal line • Tibial tuberosity • Pubic tubercle • Medial malleolus • Body • Superior pubic ramus Patella • Inferior pubic ramus Fibula Ischium • Head • Body • Neck • Ramus • Lateral malleolus • Ischial tuberosity • Ischial spine Foot • Calcaneus Ilium o Calcaneal tuberosity • Iliac fossa o Sustentaculum tali (talar shelf) • Anterior superior iliac spine • Anterior inferior iliac spine • Talus o Head • Posterior superior iliac spine o Neck • Posterior inferior iliac spine • Arcuate line • Navicular • Iliac crest • Cuboid • Body • Cuneiforms: medial, intermediate, and lateral Femur • Metatarsals 1-5 • Greater trochanter • Phalanges 1-5 • Lesser trochanter o Proximal • Head o Middle • Neck o Distal • Linea aspera • L • Lateral condyle • L • Intercondylar fossa (notch) • L • Medial condyle • L • Lateral epicondyle • L • Medial epicondyle • L • Adductor tubercle • L • L • L • L • 1 Updated: December, 9th, 2020 Lab 3: Anterior and Medial Thigh Anterior Thigh Medial thigh General Structures Muscles • Fascia lata • Adductor longus m. • Anterior compartment • Adductor brevis m. • Medial compartment • Adductor magnus m. • Great saphenous vein o Adductor hiatus • Femoral sheath o Compartments and contents • Pectineus m. o Femoral canal and ring • Gracilis m. Muscles & Associated Tendons Nerves • Tensor fasciae lata • Obturator nerve • Iliotibial tract (band) • Femoral triangle: Boundaries Vessels o Inguinal ligament • Obturator artery o Sartorius m. • Femoral artery o Adductor longus m. -

Injuries to the Lower Extremity II
Injury to lower extremity InjuriesInjuries toto thethe lowerlower extremityextremity IIII Aree Tanavalee MD Associate Professor Department of Orthopaedics Faculty of Medicine Chulalongkorn University Injury to lower extremity TopicsTopics • Fracture of the shaft of the femur • Fractures around the knee • Knee dislocation and fracture dislocation • Fractures of tibia and fibular • Fractures around the ankle • Fracture and fracture dislocation of the foot Injury to lower extremity CommonCommon symptomssymptoms andand signssigns ofof fracturesfractures – Pain – Deformity – Shortening – Swelling – Ecchymosed – Loss of function – Open injury • Gross finding of fractures Injury to lower extremity RadiographicRadiographic evaluationevaluation forfor fracturesfractures • At least, 2 different planes of Fx site – Includes joint above and below – Some types of Fx, special views – Sometimes, 2 different times – Sometimes, calls second opinion Injury to lower extremity ComplicationsComplications ofof fracturesfractures • General – Delayed union – Nonunion – Malunion – Shortening – Infection • Severe – Neurovascular injuries – Compartment syndrome – Fat embolism – Adult respiratory distress syndrome (ARDS) Injury to lower extremity FatFat embolismembolism • Common in Fx of long bone and pelvis • Multiple Fxs >> single Fx • Respiratory insufficiency • Usually manifests within 48 hr • Clinical – Fever – Tachepnea – Tachycardia – Alters consciousness • Treatment – Respiratory support – Early Fx stabilization Injury to lower extremity CompartmentCompartment -
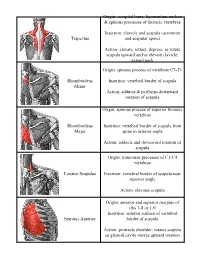
Trapezius Origin: Occipital Bone, Ligamentum Nuchae & Spinous Processes of Thoracic Vertebrae Insertion: Clavicle and Scapul
Origin: occipital bone, ligamentum nuchae & spinous processes of thoracic vertebrae Insertion: clavicle and scapula (acromion Trapezius and scapular spine) Action: elevate, retract, depress, or rotate scapula upward and/or elevate clavicle; extend neck Origin: spinous process of vertebrae C7-T1 Rhomboideus Insertion: vertebral border of scapula Minor Action: adducts & performs downward rotation of scapula Origin: spinous process of superior thoracic vertebrae Rhomboideus Insertion: vertebral border of scapula from Major spine to inferior angle Action: adducts and downward rotation of scapula Origin: transverse precesses of C1-C4 vertebrae Levator Scapulae Insertion: vertebral border of scapula near superior angle Action: elevates scapula Origin: anterior and superior margins of ribs 1-8 or 1-9 Insertion: anterior surface of vertebral Serratus Anterior border of scapula Action: protracts shoulder: rotates scapula so glenoid cavity moves upward rotation Origin: anterior surfaces and superior margins of ribs 3-5 Insertion: coracoid process of scapula Pectoralis Minor Action: depresses & protracts shoulder, rotates scapula (glenoid cavity rotates downward), elevates ribs Origin: supraspinous fossa of scapula Supraspinatus Insertion: greater tuberacle of humerus Action: abduction at the shoulder Origin: infraspinous fossa of scapula Infraspinatus Insertion: greater tubercle of humerus Action: lateral rotation at shoulder Origin: clavicle and scapula (acromion and adjacent scapular spine) Insertion: deltoid tuberosity of humerus Deltoid Action: -

Palpation Techniques
Palpation Techniques Bearbeitet von Wolfgang Stelzenmüller, Michelle Hertrich, Gertrud Graubart Champe, Bernhard Reichert 1. Auflage 2010. Taschenbuch. 500 S. Paperback ISBN 978 3 13 146341 8 Format (B x L): 19,5 x 27 cm Weitere Fachgebiete > Medizin > Komplementäre Medizin, Asiatische Medizin (TCM), Heilpraktiker Zu Inhaltsverzeichnis schnell und portofrei erhältlich bei Die Online-Fachbuchhandlung beck-shop.de ist spezialisiert auf Fachbücher, insbesondere Recht, Steuern und Wirtschaft. Im Sortiment finden Sie alle Medien (Bücher, Zeitschriften, CDs, eBooks, etc.) aller Verlage. Ergänzt wird das Programm durch Services wie Neuerscheinungsdienst oder Zusammenstellungen von Büchern zu Sonderpreisen. Der Shop führt mehr als 8 Millionen Produkte. 140 6 Knee Joint Iliotibial tract Gerdy tubercle Fig. 6.49 Palpation of the iliotibial tract—anterior edge. Fig. 6.51 Palpation of the Gerdy tubercle. With the knee in slight flexion, the patient is instructed to isometrically contract the quadriceps. The hip is also flexed, abducted, and medially rotated. Using a perpendicular palpation technique, the edges of the tract can be identified slightly proximal to the level of the base of the patella (Fig. 6.50). Note • The tract is found directly over the lateral epicondyle when the knee is in 30−40° flexion. Less flexion shifts the tract so that it is then anterior to the epicondyle, while more flexion moves it posteriorly. It now be- comes apparent that the iliotibial tract must slide over the epicondyle during the gait cycle. This can oc- casionally cause symptoms. • A significant number of tract fibers extend down to the lateral edge of the patella and insert slightly distal to the vastus lateralis tendon. -

The Anatomy of the Medial Part of the Knee
LaPrade.fm Page 2000 Thursday, August 16, 2007 12:24 PM COPYRIGHT © 2007 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED The Anatomy of the Medial Part of the Knee By Robert F. LaPrade, MD, PhD, Anders Hauge Engebretsen, Medical Student, Thuan V. Ly, MD, Steinar Johansen, MD, Fred A. Wentorf, MS, and Lars Engebretsen, MD, PhD Investigation performed at the University of Minnesota, Minneapolis, Minnesota Background: While the anatomy of the medial part of the knee has been described qualitatively, quantitative de- scriptions of the attachment sites of the main medial knee structures have not been reported. The purpose of the present study was to verify the qualitative anatomy of medial knee structures and to perform a quantitative evaluation of their anatomic attachment sites as well as their relationships to pertinent osseous landmarks. Methods: Dissections were performed and measurements were made for eight nonpaired fresh-frozen cadaveric knees with use of an electromagnetic three-dimensional tracking sensor system. Results: In addition to the medial epicondyle and the adductor tubercle, a third osseous prominence, the gastrocne- mius tubercle, which corresponded to the attachment site of the medial gastrocnemius tendon, was identified. The average length of the superficial medial (tibial) collateral ligament was 94.8 mm. The superficial medial collateral lig- ament femoral attachment was 3.2 mm proximal and 4.8 mm posterior to the medial epicondyle. The superficial me- dial collateral ligament had two separate attachments on the tibia. The distal attachment of the superficial medial collateral ligament on the tibia was 61.2 mm distal to the knee joint. -

The Patellofemoral Joint
The Patellofemoral Joint Tal Laor, MD Department of Radiology Cincinnati Children’s Hospital Medical Center Patellofemoral Joint Disorders • Overuse pain • Transient patellar dislocation • Arthritis Patellofemoral Joint Disorders • Overuse pain • Transient patellar dislocation • Arthritis Transient Patellar Dislocation • Common in children, adolescents • Lateral dislocation • Spontaneous reduction • Predisposing factors • Associated injuries http://ortho-teaching.feinberg.northwestern.edu/ Transient Patellar Dislocation • Highest incidence 10-17 year olds • Half experience anterior knee pain after episode managed conservatively • High rate of recurrent dislocations • Persistent symptoms, degenerative changes Predisposing Factors • Most factors are congenital/developmental • Osseous –Patellar configuration, location –Femoral (trochlea) –Tibial (tubercle) • Soft tissue Patellar Factors www.boundless.com Patella • Sesamoid bone • Medial, lateral facets • Odd facet (80%): far medial O L M Goodfellow J, et al. JBJS 58-B 1976 Patella • Sesamoid bone • Medial, lateral facets • Odd facet (80%): far medial • Shape medial, lateral facets (Wiberg classification) I II L M III Patella Alta • Associated with instability • Insall-Salvati ratio – Patellar tendon/patellar length – Lateral radiograph in 30° flexion – Standing increases quadriceps contraction and adds to “alta” Modified Insall-Salvati ratio (mIS) Insall-Salvati ratio (IS) Caton-Deschamps Index (CDI) PL TL Normal: IS = 0.8-1.2 Normal: mIS = mean 1.25 (>2 is alta) Normal: CDI = 0.8-1.2 Caton -

OSGOOD-SCHLATTER DISEASE (Osteochondrosis, Apophysitis of the Tibial Tubercle)
Montefiore Pediatric Orthopedic and Scoliosis Center Children’s Hospital at Montefiore Norman Otsuka MD – Eric Fornari MD Jacob Schulz MD – Jaime Gomez MD – Christine Moloney PA th 3400 Bainbridge Avenue, 6 Fl, Bronx, NY 10467 phone 718 920 2060 / fax 718 920 7799 1250 Waters Place, 11th Fl, Bronx, NY 10461 OSGOOD-SCHLATTER DISEASE (Osteochondrosis, Apophysitis of the Tibial Tubercle) Description Osgood-Schlatter disease is characterized by inflammation of the growth plate of the leg just below the knee at the tibial tubercle, a prominence just below the kneecap. The tibial tubercle is the bony attachment on the large bone of the lower leg (tibia) of the big, powerful thigh muscle (quadriceps). The growth plate is an area of relative weakness, and injury to it occurs due to repeated stress or vigorous exercise. It is a temporary condition of the tibial tubercle that is uncommon after age 16. Common Signs and Symptoms • A slightly swollen, warm, and tender bump below the knee • Pain with activity, especially straightening the leg against force (stair climbing, jumping, deep knee bends, or weight-lifting) or following an extended period of vigorous exercise in an adolescent. In more severe cases, pain occurs during less vigorous activity. Causes Osgood-Schlatter disease results from stress or injury to the tibial tubercle growth plate (which is still developing during adolescence), causing a flare-up. Repeated stress or injury interferes with development, causing inflammation. Risk Increases With • Overzealous conditioning routines, such as running, jumping, or jogging • Being overweight • Boys between 11 and 18 • Rapid skeletal growth • Poor physical conditioning (strength and flexibility) Preventive Measures • Lose weight or maintain ideal body weight. -

Anteromedial Tibial Tubercle Osteotomy 1 3 (Fulkerson Osteotomy) 40
2 Anteromedial Tibial Tubercle Osteotomy 1 3 (Fulkerson Osteotomy) 40 4 Jack Farr, Brian J. Cole, James Kercher, Lachlan Batty, [AU1] 5 and Sarvottam Bajaj 6 40.1 Introduction nature of the Fulkerson osteotomy allows for simul- 34 taneous anteriorization and medialization of the tib- 35 ial tubercle. By varying the angle of the osteotomy, the 36 7 The tibial tubercle (interchangeable with tuberosity) tubercle can be biased to a more anterior or more medial 37 8 is the most distal anchor of the extensor mechanism position. Since his initial description, the indications for 38 9 and can serve as a tool in altering patellofemoral (PF) this procedure have evolved significantly and continue 39 10 mechanics. Known collectively as distal realignment to be refined. This has been primarily driven by the evo- 40 11 procedures, osteotomies of the tibial tubercle are a use- lution and outcomes of patellofemoral resurfacing 41 12 ful method to treat a variety of PF conditions by allow- procedures as well as improved objective measures of 42 13 ing coronal, axial, and sagittal plane adjustments of the patellar alignment, contact area, and forces. 43 14 patellofemoral articulation which redistribute patellar The tibial tuberosity to trochlear groove (TT–TG) 44 15 contact pressures (force and contact area) and poten- distance, popularized by Dejour et al.8 as an objective 45 [AU2]16 tially improve tracking. Numerous tibial tubercle osteot- measure of tuberosity position, has helped quantify 46 17 omies have been described in the literature to treat PF abnormal tuberosity position and enhanced appropri- 47 18 pain, chondrosis, and instability. -

The Innominate Tubercle of the Femur: Application to Anterior Surgical Approaches to the Hip
The innominate tubercle of the femur: application to anterior surgical approaches to the hip Kielbasinski Podlaszewska O1, Bekvalac J2, Williams RL3, Adds PJ1 1 Institute of Medical and Biomedical Education (Anatomy), St George’s, University of London, London, UK. 2 The Centre for Human Bioarchaeology, Musuem of London, London, UK 3 Department of Trauma and Orthopaedics, Swansea Hospital, Swansea, UK Abbreviated title: The innominate tubercle: a survey of variability Corresponding author Philip J Adds, Institute of Medical and Biomedical Education (Anatomy), St George’s, University of London, Cranmer Terrace, London SW17 0RE, UK. Email: [email protected], 02087255208 This article has been accepted for publication and undergone full peer review but has not been through the copyediting, typesetting, pagination and proofreading process which may lead to differences between this version and the Version of Record. Please cite this article as an ‘Accepted Article’, doi: 10.1002/ca.22870 This article is protected by copyright. All rights reserved. The innominate tubercle of the femur: application to anterior surgical approaches to the hip Abstract Introduction. There has recently been an increase in popularity of the direct anterior approach (DAA) hip arthroplasty, due to the muscle sparing nature of its interneural intervals, with the innominate tubercle being used as a lateral reference point for the femoral neck osteotomy. However, there is very little information in the literature on this rather enigmatic structure, with no evidence as to whether it is a consistent and reliable marker, or if it varies significantly in the population. Materials and Methods. In this study, data were gathered from 79 pairs of adult, post-medieval skeletal femora to investigate the effects of sex, age, femoral side, femoral length, femoral neck length, and femoral neck-shaft angle on the width, length, and height of the innominate tubercle. -
Bones of the Lower Limb Doctors Notes Notes/Extra Explanation Editing File Objectives
Color Code Important Bones of the Lower Limb Doctors Notes Notes/Extra explanation Editing File Objectives Classify the bones of the three regions of the lower limb (thigh, leg and foot). Memorize the main features of the – Bones of the thigh (femur & patella) – Bones of the leg (tibia & Fibula) – Bones of the foot (tarsals, metatarsals and phalanges) Recognize the side of the bone. ﻻ تنصدمون من عدد ال رشائح نصها رشح زائد وملخصات واسئلة Some pictures in the original slides have been replaced with other pictures which are more clear BUT they have the same information and labels. Terminology (Team 434) شيء مرتفع /Eminence a small projection or bump Terminology (Team 434) Bones of thigh (Femur and Patella) Femur o Articulates (joins): (1) above with Acetabulum of hip bone to form the hip joint, (2) below with tibia and patella to form the knee joint. Body of femur (shaft) o Femur consists of: I. Upper end. II. Shaft. III. Lower end. Note: All long bones consist of three things: 1- upper/proximal end posterior 2- shaft anterior 3- lower/distal end I. Upper End of Femur The upper end contains: A. Head B. Neck C. Greater trochanter & D. Lesser trochanter A. Head: o Articulates (joins) with acetabulum of hip bone to form the hip joint. o Has a depression in the center called Fovea Capitis. o The fovea capitis is for the attachment of ligament of the head of Femur. o An artery called Obturator Artery passes along this ligament to supply head of Femur. B. Neck: o Connects head to the shaft. -

Bone Handout”)
The Skeletal System (“Bone Handout”) Bone Markings - as in Table 6.1, know categories, names, descriptions and categories of bone markings Common Fractures - as in Table 6.2, identify type from pictures The Axial Skeleton Skull Cranial bones frontal (supraorbital foramen) parietal temporal (mastoid process, external auditory(acoustic) meatus, styloid process, zygomatic process, stylomastoid foramen) occipital (foramen magnum, hypoglossal canal, occipital condyles) sphenoid (optic canal, superior orbital fissure, sella turcica, foramen rotundum, foramen ovale, foramen spinosum , greater wings, lesser wings) ethmoid (olfactory foramina) Relevant Figures: 7.4, 7.6, 7.7a, 7.9 Facial bones nasal maxilla (infraorbital foramen, inferior orbital fissure) zygomatic mandible (mental foramen, body, ramus, mandibular condyle) lacrimal (lacrimal fossa) palatine inferior nasal conchae vomer Relevant Figures: 7.4, 7.6, 7.7a Sutures coronal sagittal lambdoid squamous Relevant Figures: 7.4, 7.5 Paranasal Sinuses frontal sphenoidal maxillary ethmoidal Relevant Figures: 7.15 Fontanels anterior posterior sphenoidal mastoid Relevant Figures: 7.28 Hyoid bone Relevant Figures: 7.17 1 Vertebrae Parts of a “typical vertebra” using thoracic as example body vertebral arch (pedicle, lamina, vertebral foramen) intervertebral foramen transverse process spinous process superior articular process inferior articular process Divisions of vertebral column cervical (transverse foramina) thoracic (transverse costal facet - for tubercle of rib, superior and inferior costal