Palpation Techniques
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

List: Bones & Bone Markings of Appendicular Skeleton and Knee
List: Bones & Bone markings of Appendicular skeleton and Knee joint Lab: Handout 4 Superior Appendicular Skeleton I. Clavicle (Left or Right?) A. Acromial End B. Conoid Tubercle C. Shaft D. Sternal End II. Scapula (Left or Right?) A. Superior border (superior margin) B. Medial border (vertebral margin) C. Lateral border (axillary margin) D. Scapular notch (suprascapular notch) E. Acromion Process F. Coracoid Process G. Glenoid Fossa (cavity) H. Infraglenoid tubercle I. Subscapular fossa J. Superior & Inferior Angle K. Scapular Spine L. Supraspinous Fossa M. Infraspinous Fossa III. Humerus (Left or Right?) A. Head of Humerus B. Anatomical Neck C. Surgical Neck D. Greater Tubercle E. Lesser Tubercle F. Intertubercular fossa (bicipital groove) G. Deltoid Tuberosity H. Radial Groove (groove for radial nerve) I. Lateral Epicondyle J. Medial Epicondyle K. Radial Fossa L. Coronoid Fossa M. Capitulum N. Trochlea O. Olecranon Fossa IV. Radius (Left or Right?) A. Head of Radius B. Neck C. Radial Tuberosity D. Styloid Process of radius E. Ulnar Notch of radius V. Ulna (Left or Right?) A. Olecranon Process B. Coronoid Process of ulna C. Trochlear Notch of ulna Human Anatomy List: Bones & Bone markings of Appendicular skeleton and Knee joint Lab: Handout 4 D. Radial Notch of ulna E. Head of Ulna F. Styloid Process VI. Carpals (8) A. Proximal row (4): Scaphoid, Lunate, Triquetrum, Pisiform B. Distal row (4): Trapezium, Trapezoid, Capitate, Hamate VII. Metacarpals: Numbered 1-5 A. Base B. Shaft C. Head VIII. Phalanges A. Proximal Phalanx B. Middle Phalanx C. Distal Phalanx ============================================================================= Inferior Appendicular Skeleton IX. Os Coxae (Innominate bone) (Left or Right?) A. -

Musculoskeletal Morphing from Human to Mouse
Procedia IUTAM Procedia IUTAM 00 (2011) 1–9 2011 Symposium on Human Body Dynamics Musculoskeletal Morphing from Human to Mouse Yoshihiko Nakamuraa,∗, Yosuke Ikegamia, Akihiro Yoshimatsua, Ko Ayusawaa, Hirotaka Imagawaa, and Satoshi Ootab aDepartment of Mechano-Informatics, Graduate School of Information and Science and Technology, University of Tokyo, 7-3-1, Hongo, Bunkyo-ku, Tokyo, Japan bBioresource Center, Riken, 3-1-1 Takanodai, Tsukuba-shi, Ibaragi, Japan Abstract The analysis of movement provides various insights of human body such as biomechanical property of muscles, function of neural systems, physiology of sensory-motor system, skills of athletic movements, and more. Biomechan- ical modeling and robotics computation have been integrated to extend the applications of musculoskeletal analysis of human movements. The analysis would also provide valuable means for the other mammalian animals. One of current approaches of post-genomic research focuses to find connections between the phenotype and the genotype. The former means the visible morphological or behavioral expression of an animal, while the latter implies its genetic expression. Knockout mice allows to study the developmental pathway from the genetic disorders to the behavioral disorders. Would musculoskeletal analysis of mice also offer scientific means for such study? This paper reports our recent technological development to build the musculoskeletal model of a laboratory mouse. We propose mapping the musculoskeletal model of human to a laboratory mouse based on the morphological similarity between the two mammals. Although the model will need fine adjustment based on the CT data or else, we can still use the mapped musculoskeletal model as an approximate model of the mouse’s musculoskeletal system. -
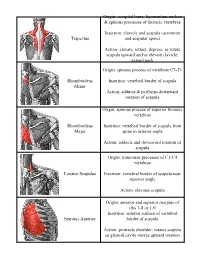
Trapezius Origin: Occipital Bone, Ligamentum Nuchae & Spinous Processes of Thoracic Vertebrae Insertion: Clavicle and Scapul
Origin: occipital bone, ligamentum nuchae & spinous processes of thoracic vertebrae Insertion: clavicle and scapula (acromion Trapezius and scapular spine) Action: elevate, retract, depress, or rotate scapula upward and/or elevate clavicle; extend neck Origin: spinous process of vertebrae C7-T1 Rhomboideus Insertion: vertebral border of scapula Minor Action: adducts & performs downward rotation of scapula Origin: spinous process of superior thoracic vertebrae Rhomboideus Insertion: vertebral border of scapula from Major spine to inferior angle Action: adducts and downward rotation of scapula Origin: transverse precesses of C1-C4 vertebrae Levator Scapulae Insertion: vertebral border of scapula near superior angle Action: elevates scapula Origin: anterior and superior margins of ribs 1-8 or 1-9 Insertion: anterior surface of vertebral Serratus Anterior border of scapula Action: protracts shoulder: rotates scapula so glenoid cavity moves upward rotation Origin: anterior surfaces and superior margins of ribs 3-5 Insertion: coracoid process of scapula Pectoralis Minor Action: depresses & protracts shoulder, rotates scapula (glenoid cavity rotates downward), elevates ribs Origin: supraspinous fossa of scapula Supraspinatus Insertion: greater tuberacle of humerus Action: abduction at the shoulder Origin: infraspinous fossa of scapula Infraspinatus Insertion: greater tubercle of humerus Action: lateral rotation at shoulder Origin: clavicle and scapula (acromion and adjacent scapular spine) Insertion: deltoid tuberosity of humerus Deltoid Action: -

Morphometric Study of Tibial Condylar Area in the North Indian Population. Ankit Srivastava1, Dr
JMSCR Volume||2||Issue||3||Page515-519||March 2014 2014 www.jmscr.igmpublication.org Impact Factcor-1.1147 ISSN (e)-2347-176x Morphometric Study of Tibial Condylar area in the North Indian Population. Ankit Srivastava1, Dr. Anjoo Yadav2, Prof. R.J. Thomas3, Ms. Neha Gupta4 1Tutor in AIIMS Bhopal. 2Lecturer in Govt. medical college, Kannauj. 3Professor in Govt. medical college, Kannauj. 4Tutor in Govt. medical college, Kannauj. Email: [email protected] Abstract: The upper end of tibia is expanded to form a mass that consists of two parts: lateral and medial condyles which articulate with the corresponding condylar surfaces of the femur. Separating these two condyles is the intercondylar area whose central part is raised to form the intercondylar eminence. The present study will give information of the exact dimensions and percentage covered by medial and lateral condyles out of total condylar area. This study was undertaken to collect metrical data about the medial and lateral condyles of tibia. The present study was performed on 150 dry tibia of north Indian subjects, Out of which 70 tibia belonged to right side and 80 were of left side. The age and sex of these bones were not known. The anteroposterior length of medial and lateral tibial condylar area was measured along with their transverse diameter. The data was statistically analyzed to hold comparisons between tibia of right and left side and also between medial and lateral tibial condyles of the same side. The area covered by MTC is 38.56% and by LTC is 35.97% out of total condylar area in right side. -

Sesamoid Bone of the Medial Collateral Ligament of the Knee Joint
CASE REPORT Eur. J. Anat. 21 (4): 309-313 (2017) Sesamoid bone of the medial collateral ligament of the knee joint Omar M. Albtoush, Konstantin Nikolaou, Mike Notohamiprodjo Department of Diagnostic and Interventional Radiology, Karls Eberhard Universität Tübingen, Hoppe-Seyler-Str. 3, 72076 Tübingen, Germany SUMMARY tomical relations and the exclusion of other possi- bilities. The variable occurrence of the sesamoid bones This article supports the theory stating that the supports the theory stating that the development development and evolution of the sesamoid bones and evolution of these bones are controlled are controlled through the interaction between in- through the interaction between intrinsic genetic trinsic genetic factors and extrinsic epigenetic stim- factors and extrinsic stimuli. In the present article uli, which can explain their variable occurrence. we report a sesamoid bone at the medial collateral ligament of the knee joint, a newly discovered find- CASE REPORT ing in human and veterinary medicine. We present a case of a 51-year-old female pa- Key words: Sesamoid – MCL – Knee – Fabella – tient, who presented with mild pain at the medial Cyamella aspect of the left knee. No trauma has been re- ported. An unenhanced spiral CT-Scan was per- INTRODUCTION formed with 2 mm thickness, 120 kvp and 100 mAs, which showed preserved articulation of the New structural anatomical discoveries are not so knee joint with neither joint effusion, nor narrowing often encountered. However, their potential occur- of the joint space nor articulating cortical irregulari- rence should be kept in mind, which can eventually ties (Fig. 1). Mild subchondral sclerosis was de- help in a better understanding of patients’ symp- picted at the medial tibial plateau as a sign of early toms and subsequently improve the management osteoarthritis. -

The Anatomy of the Medial Part of the Knee
LaPrade.fm Page 2000 Thursday, August 16, 2007 12:24 PM COPYRIGHT © 2007 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED The Anatomy of the Medial Part of the Knee By Robert F. LaPrade, MD, PhD, Anders Hauge Engebretsen, Medical Student, Thuan V. Ly, MD, Steinar Johansen, MD, Fred A. Wentorf, MS, and Lars Engebretsen, MD, PhD Investigation performed at the University of Minnesota, Minneapolis, Minnesota Background: While the anatomy of the medial part of the knee has been described qualitatively, quantitative de- scriptions of the attachment sites of the main medial knee structures have not been reported. The purpose of the present study was to verify the qualitative anatomy of medial knee structures and to perform a quantitative evaluation of their anatomic attachment sites as well as their relationships to pertinent osseous landmarks. Methods: Dissections were performed and measurements were made for eight nonpaired fresh-frozen cadaveric knees with use of an electromagnetic three-dimensional tracking sensor system. Results: In addition to the medial epicondyle and the adductor tubercle, a third osseous prominence, the gastrocne- mius tubercle, which corresponded to the attachment site of the medial gastrocnemius tendon, was identified. The average length of the superficial medial (tibial) collateral ligament was 94.8 mm. The superficial medial collateral lig- ament femoral attachment was 3.2 mm proximal and 4.8 mm posterior to the medial epicondyle. The superficial me- dial collateral ligament had two separate attachments on the tibia. The distal attachment of the superficial medial collateral ligament on the tibia was 61.2 mm distal to the knee joint. -

The Patellofemoral Joint
The Patellofemoral Joint Tal Laor, MD Department of Radiology Cincinnati Children’s Hospital Medical Center Patellofemoral Joint Disorders • Overuse pain • Transient patellar dislocation • Arthritis Patellofemoral Joint Disorders • Overuse pain • Transient patellar dislocation • Arthritis Transient Patellar Dislocation • Common in children, adolescents • Lateral dislocation • Spontaneous reduction • Predisposing factors • Associated injuries http://ortho-teaching.feinberg.northwestern.edu/ Transient Patellar Dislocation • Highest incidence 10-17 year olds • Half experience anterior knee pain after episode managed conservatively • High rate of recurrent dislocations • Persistent symptoms, degenerative changes Predisposing Factors • Most factors are congenital/developmental • Osseous –Patellar configuration, location –Femoral (trochlea) –Tibial (tubercle) • Soft tissue Patellar Factors www.boundless.com Patella • Sesamoid bone • Medial, lateral facets • Odd facet (80%): far medial O L M Goodfellow J, et al. JBJS 58-B 1976 Patella • Sesamoid bone • Medial, lateral facets • Odd facet (80%): far medial • Shape medial, lateral facets (Wiberg classification) I II L M III Patella Alta • Associated with instability • Insall-Salvati ratio – Patellar tendon/patellar length – Lateral radiograph in 30° flexion – Standing increases quadriceps contraction and adds to “alta” Modified Insall-Salvati ratio (mIS) Insall-Salvati ratio (IS) Caton-Deschamps Index (CDI) PL TL Normal: IS = 0.8-1.2 Normal: mIS = mean 1.25 (>2 is alta) Normal: CDI = 0.8-1.2 Caton -

OSGOOD-SCHLATTER DISEASE (Osteochondrosis, Apophysitis of the Tibial Tubercle)
Montefiore Pediatric Orthopedic and Scoliosis Center Children’s Hospital at Montefiore Norman Otsuka MD – Eric Fornari MD Jacob Schulz MD – Jaime Gomez MD – Christine Moloney PA th 3400 Bainbridge Avenue, 6 Fl, Bronx, NY 10467 phone 718 920 2060 / fax 718 920 7799 1250 Waters Place, 11th Fl, Bronx, NY 10461 OSGOOD-SCHLATTER DISEASE (Osteochondrosis, Apophysitis of the Tibial Tubercle) Description Osgood-Schlatter disease is characterized by inflammation of the growth plate of the leg just below the knee at the tibial tubercle, a prominence just below the kneecap. The tibial tubercle is the bony attachment on the large bone of the lower leg (tibia) of the big, powerful thigh muscle (quadriceps). The growth plate is an area of relative weakness, and injury to it occurs due to repeated stress or vigorous exercise. It is a temporary condition of the tibial tubercle that is uncommon after age 16. Common Signs and Symptoms • A slightly swollen, warm, and tender bump below the knee • Pain with activity, especially straightening the leg against force (stair climbing, jumping, deep knee bends, or weight-lifting) or following an extended period of vigorous exercise in an adolescent. In more severe cases, pain occurs during less vigorous activity. Causes Osgood-Schlatter disease results from stress or injury to the tibial tubercle growth plate (which is still developing during adolescence), causing a flare-up. Repeated stress or injury interferes with development, causing inflammation. Risk Increases With • Overzealous conditioning routines, such as running, jumping, or jogging • Being overweight • Boys between 11 and 18 • Rapid skeletal growth • Poor physical conditioning (strength and flexibility) Preventive Measures • Lose weight or maintain ideal body weight. -

Axial Skeleton- Skull, Spinal Column Appendicular Skeleton – Limbs and Girdle
How many bones do humans have? • When you were born you had over 300 bones. As you grew, some of these bones began to fuse together. The result? An adult has only 206 bones! Factoids: • The human hand has 27 bones; your face has 14! • The longest bone in your body? Your thigh bone, the femur -- it's about 1/4 of your height. The smallest is the stirrup bone in the ear which can measure 1/10 of an inch. • Did you know that humans and giraffes have the same number of bones in their necks? Giraffe neck vertebrae are just much, much longer! • You have over 230 moveable and semi-moveable joints in your body. The Skeletal System Parts of the skeletal system Bones (skeleton) Joints Cartilages Ligaments (bone to bone)(tendon=bone to muscle) Divided into two divisions Axial skeleton- skull, spinal column Appendicular skeleton – limbs and girdle Copyright © 2003 Pearson Education, Inc. publishing as Benjamin Cummings Functions of Bones Support of the body Protection of soft organs Movement due to attached skeletal muscles Storage of minerals and fats Blood cell formation Copyright © 2003 Pearson Education, Inc. publishing as Benjamin Cummings Bones of the Human Body The skeleton has 206 bones Two basic types of bone tissue Compact bone Homogeneous Spongy bone Small needle-like pieces of bone Figure 5.2b Many open spaces Copyright © 2003 Pearson Education, Inc. publishing as Benjamin Cummings Bones are classified by their shape: 1. Long- bones are longer than they are wide (arms, legs) 2. Short- usually square in shape, cube like (wrist, ankle) 3. -

Anteromedial Tibial Tubercle Osteotomy 1 3 (Fulkerson Osteotomy) 40
2 Anteromedial Tibial Tubercle Osteotomy 1 3 (Fulkerson Osteotomy) 40 4 Jack Farr, Brian J. Cole, James Kercher, Lachlan Batty, [AU1] 5 and Sarvottam Bajaj 6 40.1 Introduction nature of the Fulkerson osteotomy allows for simul- 34 taneous anteriorization and medialization of the tib- 35 ial tubercle. By varying the angle of the osteotomy, the 36 7 The tibial tubercle (interchangeable with tuberosity) tubercle can be biased to a more anterior or more medial 37 8 is the most distal anchor of the extensor mechanism position. Since his initial description, the indications for 38 9 and can serve as a tool in altering patellofemoral (PF) this procedure have evolved significantly and continue 39 10 mechanics. Known collectively as distal realignment to be refined. This has been primarily driven by the evo- 40 11 procedures, osteotomies of the tibial tubercle are a use- lution and outcomes of patellofemoral resurfacing 41 12 ful method to treat a variety of PF conditions by allow- procedures as well as improved objective measures of 42 13 ing coronal, axial, and sagittal plane adjustments of the patellar alignment, contact area, and forces. 43 14 patellofemoral articulation which redistribute patellar The tibial tuberosity to trochlear groove (TT–TG) 44 15 contact pressures (force and contact area) and poten- distance, popularized by Dejour et al.8 as an objective 45 [AU2]16 tially improve tracking. Numerous tibial tubercle osteot- measure of tuberosity position, has helped quantify 46 17 omies have been described in the literature to treat PF abnormal tuberosity position and enhanced appropri- 47 18 pain, chondrosis, and instability. -

Injuries and Normal Variants of the Pediatric Knee
Revista Chilena de Radiología, año 2016. ARTÍCULO DE REVISIÓN Injuries and normal variants of the pediatric knee Cristián Padilla C.a,* , Cristián Quezada J.a,b, Nelson Flores N.a, Yorky Melipillán A.b and Tamara Ramírez P.b a. Imaging Center, Hospital Clínico Universidad de Chile, Santiago, Chile. b. Radiology Service, Hospital de Niños Roberto del Río, Santiago, Chile. Abstract: Knee pathology is a reason for consultation and a prevalent condition in children, which is why it is important to know both the normal variants as well as the most frequent pathologies. In this review a brief description is given of the main pathologies and normal variants that affect the knee in children, not only the main clinical characteristics but also the findings described in the different, most used imaging techniques (X-ray, ultrasound, computed tomography and magnetic resonance imaging [MRI]). Keywords: Knee; Paediatrics; Bone lesions. Introduction posteromedial distal femoral metaphysis, near the Pediatric knee imaging studies are used to evaluate insertion site of the medial twin muscle or adductor different conditions, whether traumatic, inflammatory, magnus1. It is a common finding on radiography and developmental or neoplastic. magnetic resonance imaging (MRI), incidental, with At a younger age the normal evolution of the more frequency between ages 10-15 years, although images during the skeletal development of the distal it can be present at any age until the physeal closure, femur, proximal tibia and proximal fibula should be after which it resolves1. In frontal radiography, it ap- known to avoid diagnostic errors. Older children and pears as a radiolucent, well circumscribed, cortical- adolescents present a higher frequency of traumatic based lesion with no associated soft tissue mass, with and athletic injuries. -

(AMIC) and Microfractures for Focal Chondral Defects of the Knee: a Medium-Term Comparative Study
life Communication Autologous Matrix-Induced Chondrogenesis (AMIC) and Microfractures for Focal Chondral Defects of the Knee: A Medium-Term Comparative Study Filippo Migliorini 1 , Jörg Eschweiler 1, Nicola Maffulli 2,3,4,* , Hanno Schenker 1, Alice Baroncini 1 , Markus Tingart 1 and Björn Rath 1,5 1 Department of Orthopedics and Trauma Surgery, University Clinic Aachen, RWTH Aachen University Clinic, 52064 Aachen, Germany; [email protected] (F.M.); [email protected] (J.E.); [email protected] (H.S.); [email protected] (A.B.); [email protected] (M.T.); [email protected] (B.R.) 2 Department of Medicine, Surgery and Dentistry, University of Salerno, Via S. Allende, 84081 Baronissi, Italy 3 School of Pharmacy and Bioengineering, Keele University School of Medicine, Thornburrow Drive, Stoke-on-Trent ST5 5BG, UK 4 Centre for Sports and Exercise Medicine, Barts and the London School of Medicine and Dentistry, Queen Mary University of London, Mile End Hospital, 275 Bancroft Road, London E1 4DG, UK 5 Department of Orthopedics, Klinikum Wels-Grieskirchen, A-4600 Wels, Austria * Correspondence: [email protected] Abstract: Introduction: The potential of autologous matrix-induced chondrogenesis (AMIC) to restore unipolar focal chondral defects of the knee is promising. However, the outcome compared to Citation: Migliorini, F.; Eschweiler, J.; microfracturing (MFx) for certain defect sizes (2–3 cm2) is still uncertain. Therefore, the present study Maffulli, N.; Schenker, H.; Baroncini, compared primary isolated AMIC versus MFx in a cohort of patients with borderline sized focal A.; Tingart, M.; Rath, B. Autologous unipolar chondral defects of the knee at midterm follow-up.