Cephalosporins: a Focus on Side Chains and -Lactam Cross-Reactivity
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Medical Review(S) Clinical Review
CENTER FOR DRUG EVALUATION AND RESEARCH APPLICATION NUMBER: 200327 MEDICAL REVIEW(S) CLINICAL REVIEW Application Type NDA Application Number(s) 200327 Priority or Standard Standard Submit Date(s) December 29, 2009 Received Date(s) December 30, 2009 PDUFA Goal Date October 30, 2010 Division / Office Division of Anti-Infective and Ophthalmology Products Office of Antimicrobial Products Reviewer Name(s) Ariel Ramirez Porcalla, MD, MPH Neil Rellosa, MD Review Completion October 29, 2010 Date Established Name Ceftaroline fosamil for injection (Proposed) Trade Name Teflaro Therapeutic Class Cephalosporin; ß-lactams Applicant Cerexa, Inc. Forest Laboratories, Inc. Formulation(s) 400 mg/vial and 600 mg/vial Intravenous Dosing Regimen 600 mg every 12 hours by IV infusion Indication(s) Acute Bacterial Skin and Skin Structure Infection (ABSSSI); Community-acquired Bacterial Pneumonia (CABP) Intended Population(s) Adults ≥ 18 years of age Template Version: March 6, 2009 Reference ID: 2857265 Clinical Review Ariel Ramirez Porcalla, MD, MPH Neil Rellosa, MD NDA 200327: Teflaro (ceftaroline fosamil) Table of Contents 1 RECOMMENDATIONS/RISK BENEFIT ASSESSMENT ......................................... 9 1.1 Recommendation on Regulatory Action ........................................................... 10 1.2 Risk Benefit Assessment.................................................................................. 10 1.3 Recommendations for Postmarketing Risk Evaluation and Mitigation Strategies ........................................................................................................................ -

Activity of Aztreonam in Combination with Ceftazidime-Avibactam Against
Diagnostic Microbiology and Infectious Disease 99 (2021) 115227 Contents lists available at ScienceDirect Diagnostic Microbiology and Infectious Disease journal homepage: www.elsevier.com/locate/diagmicrobio Activity of aztreonam in combination with ceftazidime–avibactam against serine- and metallo-β-lactamase–producing ☆ ☆☆ ★ Pseudomonas aeruginosa , , Michelle Lee a, Taylor Abbey a, Mark Biagi b, Eric Wenzler a,⁎ a College of Pharmacy, University of Illinois at Chicago, Chicago, IL, USA b College of Pharmacy, University of Illinois at Chicago, Rockford, IL, USA article info abstract Article history: Existing data support the combination of aztreonam and ceftazidime–avibactam against serine-β-lactamase Received 29 June 2020 (SBL)– and metallo-β-lactamase (MBL)–producing Enterobacterales, although there is a paucity of data against Received in revised form 15 September 2020 SBL- and MBL-producing Pseudomonas aeruginosa. In this study, 5 SBL- and MBL-producing P. aeruginosa (1 Accepted 19 September 2020 IMP, 4 VIM) were evaluated against aztreonam and ceftazidime–avibactam alone and in combination via broth Available online xxxx microdilution and time-kill analyses. All 5 isolates were nonsusceptible to aztreonam, aztreonam–avibactam, – – Keywords: and ceftazidime avibactam. Combining aztreonam with ceftazidime avibactam at subinhibitory concentrations Metallo-β-lactamase produced synergy and restored bactericidal activity in 4/5 (80%) isolates tested. These results suggest that the VIM combination of aztreonam and ceftazidime–avibactam may be a viable treatment option against SBL- and IMP MBL-producing P. aeruginosa. Aztreonam © 2020 Elsevier Inc. All rights reserved. Ceftazidime–avibactam Synergy 1. Introduction of SBLs and MBLs harbored by P. aeruginosa are fundamentally different than those in Enterobacterales (Alm et al., 2015; Kazmierczak et al., The rapid global dissemination of Ambler class B metallo-β- 2016; Periasamy et al., 2020; Poirel et al., 2000; Watanabe et al., lactamase (MBL) enzymes along with their increasing diversity across 1991). -

Use of Ceftaroline Fosamil in Children: Review of Current Knowledge and Its Application
Infect Dis Ther (2017) 6:57–67 DOI 10.1007/s40121-016-0144-8 REVIEW Use of Ceftaroline Fosamil in Children: Review of Current Knowledge and its Application Juwon Yim . Leah M. Molloy . Jason G. Newland Received: November 10, 2016 / Published online: December 30, 2016 Ó The Author(s) 2016. This article is published with open access at Springerlink.com ABSTRACT infections, CABP caused by penicillin- and ceftriaxone-resistant S. pneumoniae and Ceftaroline is a novel cephalosporin recently resistant Gram-positive infections that fail approved in children for treatment of acute first-line antimicrobial agents. However, bacterial skin and soft tissue infections and limited data are available on tolerability in community-acquired bacterial pneumonia neonates and infants younger than 2 months (CABP) caused by methicillin-resistant of age, and on pharmacokinetic characteristics Staphylococcus aureus, Streptococcus pneumoniae in children with chronic medical conditions and other susceptible bacteria. With a favorable and those with invasive, complicated tolerability profile and efficacy proven in infections. In this review, the microbiological pediatric patients and excellent in vitro profile of ceftaroline, its mechanism of action, activity against resistant Gram-positive and and pharmacokinetic profile will be presented. Gram-negative bacteria, ceftaroline may serve Additionally, clinical evidence for use in as a therapeutic option for polymicrobial pediatric patients and proposed place in therapy is discussed. Enhanced content To view enhanced content for this article go to http://www.medengine.com/Redeem/ 1F47F0601BB3F2DD. Keywords: Antibiotic resistance; Ceftaroline J. Yim (&) fosamil; Children; Methicillin-resistant St. John Hospital and Medical Center, Detroit, MI, Staphylococcus aureus; Streptococcus pneumoniae USA e-mail: [email protected] L. -

Empiric Antimicrobial Therapy for Diabetic Foot Infection
Empiric Antimicrobial Therapy for Diabetic Foot Infection (NB Provincial Health Authorities Anti-Infective Stewardship Committee, September 2019) Infection Severity Preferred Empiric Regimens Alternative Regimens Comments Mild Wound less than 4 weeks duration:d Wound less than 4 weeks duration:e • Outpatient management • Cellulitis less than 2 cm and • cephalexin 500 – 1000 mg PO q6h*,a OR • clindamycin 300 – 450 mg PO q6h (only if recommended ,a • cefadroxil 500 – 1000 mg PO q12h* severe delayed reaction to a beta-lactam) without involvement of deeper • Tailor regimen based on culture tissues and susceptibility results and True immediate allergy to a beta-lactam at MRSA Suspected: • Non-limb threatening patient response risk of cross reactivity with cephalexin or • doxycycline 200 mg PO for 1 dose then • No signs of sepsis cefadroxil: 100 mg PO q12h OR • cefuroxime 500 mg PO q8–12h*,b • sulfamethoxazole+trimethoprim 800+160 mg to 1600+320 mg PO q12h*,f Wound greater than 4 weeks duration:d Wound greater than 4 weeks duratione • amoxicillin+clavulanate 875/125 mg PO and MRSA suspected: q12h*,c OR • doxycycline 200 mg PO for 1 dose then • cefuroxime 500 mg PO q8–12h*,b AND 100 mg PO q12h AND metroNIDAZOLE metroNIDAZOLE 500 mg PO q12h 500 mg PO q12h OR • sulfamethoxazole+trimethoprim 800+160 mg to 1600/320 mg PO q12h*,f AND metroNIDAZOLE 500 mg PO q12h Moderate Wound less than 4 weeks duration:d Wound less than 4 weeks duration:e • Initial management with • Cellulitis greater than 2 cm or • ceFAZolin 2 g IV q8h*,b OR • levoFLOXacin 750 -

FDA Drug Safety Communication: FDA Cautions About Dose Confusion and Medication Error with Antibacterial Drug Avycaz (Ceftazidime and Avibactam)
FDA Drug Safety Communication: FDA cautions about dose confusion and medication error with antibacterial drug Avycaz (ceftazidime and avibactam) Safety Announcement [09-22-2015] The U.S. Food and Drug Administration (FDA) is warning health care professionals about the risk for dosing errors with the intravenous antibacterial drug Avycaz (ceftazidime and avibactam) due to confusion about the drug strength displayed on the vial and carton labels. Avycaz was initially approved with the vial and carton labels displaying the individual strengths of the two active ingredients (i.e., 2 gram/0.5 gram); however, the product is dosed based on the sum of the active ingredients (i.e., 2.5 gram). To prevent medication errors, we have revised the labels to indicate that each vial contains Avycaz 2.5 gram, equivalent to ceftazidime 2 gram and avibactam 0.5 gram (see Photos). Avycaz is approved for intravenous administration to treat complicated infections in the urinary tract, or in combination with the antibacterial drug metronidazole to treat complicated infections in the abdomen in patients with limited or no alternative treatment options. Antibacterial drugs work by killing or stopping the growth of bacteria that can cause illness. Since Avycaz’s approval in February 2015, we have received reports of three medication error cases related to confusion on how the strength was displayed on the Avycaz vial and carton labels. Two cases stated that the errors occurred during preparation of the dose in the pharmacy. The third case described concern about the potential for confusion because the strength displayed for Avycaz differs from how the strength is displayed for other beta-lactam/beta-lactamase antibacterial drugs. -

Cefalexin in the WHO Essential Medicines List for Children Reject
Reviewer No. 1: checklist for application of: Cefalexin In the WHO Essential Medicines List for Children (1) Have all important studies that you are aware of been included? Yes No 9 (2) Is there adequate evidence of efficacy for the proposed use? Yes 9 No (3) Is there evidence of efficacy in diverse settings and/or populations? Yes 9 No (4) Are there adverse effects of concern? Yes 9 No (5) Are there special requirements or training needed for safe/effective use? Yes No 9 (6) Is this product needed to meet the majority health needs of the population? Yes No 9 (7) Is the proposed dosage form registered by a stringent regulatory authority? Yes 9 No (8) What action do you propose for the Committee to take? Reject the application for inclusion of the following presentations of cefalexin: • Tablets/ capsules 250mg • Oral suspensions 125mg/5ml and 125mg/ml (9) Additional comment, if any. In order to identify any additional literature, the following broad and sensitive search was conducted using the PubMed Clinical Query application: (cephalexin OR cefalexin AND - 1 - pediatr*) AND ((clinical[Title/Abstract] AND trial[Title/Abstract]) OR clinical trials[MeSH Terms] OR clinical trial[Publication Type] OR random*[Title/Abstract] OR random allocation[MeSH Terms] OR therapeutic use[MeSH Subheading]) Only one small additional study was identified, which looked at the provision of prophylactic antibiotics in patients presenting to an urban children's hospital with trauma to the distal fingertip, requiring repair.1 In a prospective randomised control trial, 146 patients were enrolled, of which 69 were randomised to the no-antibiotic group, and 66 were randomised to the antibiotic (cefalexin) group. -

Severe Sepsis and Septic Shock Antibiotic Guide
Stanford Health Issue Date: 05/2017 Stanford Antimicrobial Safety and Sustainability Program Severe Sepsis and Septic Shock Antibiotic Guide Table 1: Antibiotic selection options for healthcare associated and/or immunocompromised patients • Healthcare associated: intravenous therapy, wound care, or intravenous chemotherapy within the prior 30 days, residence in a nursing home or other long-term care facility, hospitalization in an acute care hospital for two or more days within the prior 90 days, attendance at a hospital or hemodialysis clinic within the prior 30 days • Immunocompromised: Receiving chemotherapy, known systemic cancer not in remission, ANC <500, severe cell-mediated immune deficiency Table 2: Antibiotic selection options for community acquired, immunocompetent patients Table 3: Antibiotic selection options for patients with simple sepsis, community acquired, immunocompetent patients requiring hospitalization. Risk Factors for Select Organisms P. aeruginosa MRSA Invasive Candidiasis VRE (and other resistant GNR) Community acquired: • Known colonization with MDROs • Central venous catheter • Liver transplant • Prior IV antibiotics within 90 day • Recent MRSA infection • Broad-spectrum antibiotics • Known colonization • Known colonization with MDROs • Known MRSA colonization • + 1 of the following risk factors: • Prolonged broad antibacterial • Skin & Skin Structure and/or IV access site: ♦ Parenteral nutrition therapy Hospital acquired: ♦ Purulence ♦ Dialysis • Prolonged profound • Prior IV antibiotics within 90 days ♦ Abscess -
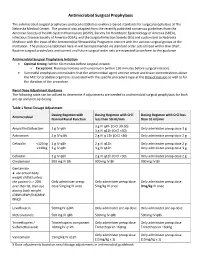
Antimicrobial Surgical Prophylaxis
Antimicrobial Surgical Prophylaxis The antimicrobial surgical prophylaxis protocol establishes evidence-based standards for surgical prophylaxis at The Nebraska Medical Center. The protocol was adapted from the recently published consensus guidelines from the American Society of Health-System Pharmacists (ASHP), Society for Healthcare Epidemiology of America (SHEA), Infectious Disease Society of America (IDSA), and the Surgical Infection Society (SIS) and customized to Nebraska Medicine with the input of the Antimicrobial Stewardship Program in concert with the various surgical groups at the institution. The protocol established here-in will be implemented via standard order sets utilized within One Chart. Routine surgical prophylaxis and current and future surgical order sets are expected to conform to this guidance. Antimicrobial Surgical Prophylaxis Initiation Optimal timing: Within 60 minutes before surgical incision o Exceptions: Fluoroquinolones and vancomycin (within 120 minutes before surgical incision) Successful prophylaxis necessitates that the antimicrobial agent achieve serum and tissue concentrations above the MIC for probable organisms associated with the specific procedure type at the time of incision as well as for the duration of the procedure. Renal Dose Adjustment Guidance The following table can be utilized to determine if adjustments are needed to antimicrobial surgical prophylaxis for both pre-op and post-op dosing. Table 1 Renal Dosage Adjustment Dosing Regimen with Dosing Regimen with CrCl Dosing Regimen with -

Product Monograph
Product Monograph PrORB-CEFUROXIME Cefuroxime Axetil Tablets, USP 250 mg and 500 mg cefuroxime/tablet Antibiotic Orbus Pharma Inc. Date of Preparation: February 25, 2009 20 Konrad Crescent Markham, Ontario Control #: 117041 L3R8T4 1 Product Monograph PrORB-CEFUROXIME Cefuroxime Axetil Tablets, USP 250 mg and 500 mg cefuroxime/tablet Antibiotic Actions and Clinical Pharmacology Cefuroxime axetil is an orally active prodrug of cefuroxime. After oral administration, cefuroxime axetil is absorbed from the gastrointestinal tract and rapidly hydrolyzed by nonspecific esterases in the intestinal mucosa and blood to release cefuroxime into the blood stream. Conversion to cefuroxime, the microbiologically active form, occurs rapidly. The inherent properties of cefuroxime are unaltered after its administration as cefuroxime axetil. Cefuroxime exerts its bactericidal effect by binding to an enzyme or enzymes referred to as penicillin-binding proteins (PBPs) involved in bacterial cell wall synthesis. This binding results in inhibition of bacterial cell wall synthesis and subsequent cell death. Specifically, cefuroxime shows high affinity for PBP 3, a primary target for cefuroxime in gram- negative organisms such as E. coli. Comparative Bioavailability Studies A two-way crossover, randomized, blinded, single-dose bioequivalence study was performed on 22 normal, healthy, non-smoking male subjects under fasting conditions. The rate and extent of absorption of cefuroxime axetil was measured and compared following a single oral dose (1 x 500 mg tablet) -

In Vitro Susceptibilities of Escherichia Coli and Klebsiella Spp. To
Jpn. J. Infect. Dis., 60, 227-229, 2007 Short Communication In Vitro Susceptibilities of Escherichia coli and Klebsiella Spp. to Ampicillin-Sulbactam and Amoxicillin-Clavulanic Acid Birgul Kacmaz* and Nedim Sultan1 Department of Central Microbiology and 1Department of Microbiology, Faculty of Medicine, Gazi University, Ankara, Turkey (Received January 30, 2007. Accepted April 13, 2007) SUMMARY: Ampicillin-sulbactam (A/S) and amoxicillin-clavulanic acid (AUG) are thought to be equally efficacious clinically against the Enterobacteriaceae family. In this study, the in vitro activities of the A/S and AUG were evaluated and compared against Escherichia coli and Klebsiella spp. Antimicrobial susceptibility tests were performed by standard agar dilution and disc diffusion techniques according to the Clinical and Laboratory Standards Institute (CLSI). During the study period, 973 strains were isolated. Of the 973 bacteria isolated, 823 were E. coli and 150 Klebsiella spp. More organisms were found to be susceptible to AUG than A/S, regardless of the susceptibility testing methodology. The agar dilution results of the isolates that were found to be sensitive or resistant were also compatible with the disc diffusion results. However, some differences were seen in the agar dilution results of some isolates that were found to be intermediately resistant with disc diffusion. In E. coli isolates, 17 of the 76 AUG intermediately resistant isolates (by disc diffusion), and 17 of the 63 A/S intermediately resistant isolates (by disc diffusion) showed different resistant patterns by agar dilution. When the CLSI breakpoint criteria are applied it should be considered that AUG and A/S sensitivity in E. coli and Klebsiella spp. -

Zinforo, INN Ceftaroline Fosamil
ANNEX I SUMMARY OF PRODUCT CHARACTERISTICS 1 1. NAME OF THE MEDICINAL PRODUCT Zinforo 600 mg powder for concentrate for solution for infusion 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Each vial contains ceftaroline fosamil acetic acid solvate monohydrate equivalent to 600 mg ceftaroline fosamil. After reconstitution, 1 ml of the solution contains 30 mg of ceftaroline fosamil. For the full list of excipients, see section 6.1. 3. PHARMACEUTICAL FORM Powder for concentrate for solution for infusion. A pale yellowish-white to light yellow powder. 4. CLINICAL PARTICULARS 4.1 Therapeutic indications Zinforo is indicated in adults for the treatment of the following infections (see sections 4.4 and 5.1): • Complicated skin and soft tissue infections (cSSTI) • Community-acquired pneumonia (CAP) Consideration should be given to official guidance on the appropriate use of antibacterial agents. 4.2 Posology and method of administration Posology For the treatment of cSSTI and CAP, the recommended dose is 600 mg administered every 12 hours by intravenous infusion over 60 minutes in patients aged 18 years or older. The recommended treatment duration for cSSTI is 5 to 14 days and the recommended duration of treatment for CAP is 5 to 7 days. Special populations Elderly patients (≥ 65 years) No dosage adjustment is required for the elderly with creatinine clearance values > 50 ml/min (see section 5.2). Renal impairment The dose should be adjusted when creatinine clearance (CrCL) is ≤ 50 ml/min, as shown below (see sections 4.4 and 5.2). Creatinine clearance Dosage regimen Frequency (ml/min) > 30 to ≤ 50 400 mg intravenously (over 60 minutes) every 12 hours 2 There is insufficient data to make specific dosage adjustment recommendations for patients with severe renal impairment (CrCL ≤ 30 ml/min) and end-stage renal disease (ESRD), including patients undergoing haemodialysis (see section 4.4). -

Summary of Product Characteristics
SUMMARY OF PRODUCT CHARACTERISTICS 1 1. NAME OF THE MEDICINAL PRODUCT Augmentin 125 mg/31.25 mg/5 ml powder for oral suspension Augmentin 250 mg/62.5 mg/5 ml powder for oral suspension 2. QUALITATIVE AND QUANTITATIVE COMPOSITION When reconstituted, every ml of oral suspension contains amoxicillin trihydrate equivalent to 25 mg amoxicillin and potassium clavulanate equivalent to 6.25 mg of clavulanic acid. Excipients with known effect Every ml of oral suspension contains 2.5 mg aspartame (E951). The flavouring in Augmentin contains maltodextrin (glucose) (see section 4.4). This medicine contains less than 1 mmol sodium (23 mg) per ml, that is to say essentially ‘sodium- free’. When reconstituted, every ml of oral suspension contains amoxicillin trihydrate equivalent to 50 mg amoxicillin and potassium clavulanate equivalent to 12.5 mg of clavulanic acid. Excipients with known effect Every ml of oral suspension contains 2.5 mg aspartame (E951). The flavouring in Augmentin contains maltodextrin (glucose) (see section 4.4). This medicine contains less than 1 mmol sodium (23 mg) per ml, that is to say essentially ‘sodium- free’. For the full list of excipients, see section 6.1. 3. PHARMACEUTICAL FORM Powder for oral suspension. Off-white powder. 4. CLINICAL PARTICULARS 4.1 Therapeutic indications Augmentin is indicated for the treatment of the following infections in adults and children (see sections 4.2, 4.4 and 5.1): • Acute bacterial sinusitis (adequately diagnosed) • Acute otitis media • Acute exacerbations of chronic bronchitis (adequately diagnosed) • Community acquired pneumonia • Cystitis • Pyelonephritis 2 • Skin and soft tissue infections in particular cellulitis, animal bites, severe dental abscess with spreading cellulitis • Bone and joint infections, in particular osteomyelitis.