Antimicrobial Stewardship Guidance
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
Therapeutic Alternatives for Drug-Resistant Cabapenemase- Producing Enterobacteria
THERAPEUTIC ALTERNATIVES FOR MULTIDRUG-RESISTANT AND EXTREMELY All isolates resistant to carbapenems were evaluated Fig. 1: Susceptibility (%) of Carbapenemase-producing MDRE Fig. 3: Susceptibility (%) of VIM-producing MDRE to Alternative DRUG-RESISTANT CABAPENEMASE- for the presence of genes encoding carbapenemases to Alternative Antibiotics Antibiotics PRODUCING ENTEROBACTERIA OXA-48-like, KPC, GES, NDM, VIM, IMP and GIM. M. Almagro*, A. Kramer, B. Gross, S. Suerbaum, S. Schubert. Max Von Pettenkofer Institut, Faculty of Medicine. LMU Munich, München, Germany. RESULTS BACKROUND 44 isolates of CPE were collected: OXA-48 (n=29), VIM (n=9), NDM-1 (n=5), KPC (n=1) and GES (n=1). The increasing emergence and dissemination of carbapenem-resistant gram-negative bacilli has From the 44 CPE isolates, 26 isolates were identified reduced significantly the options for sufficient as Klebsiella pneumoniae (68% of the OXA-48 CPE), 8 Fig. 2: Susceptibility (%) of OXA-48-producing MDRE to Fig. 4: Susceptibility (%) of NDM-producing MDRE to Alternative antibiotic therapy. The genes encoding most of these as Escherichia coli, 6 as Enterobacter cloacae, 2 as Alternative Antibiotics Antibiotics carbapenemases reside on plasmids or transposons Citrobacter freundii,1 as Providencia stuartii and 1 as carrying additional resistance genes which confer Morganella morganii. multidrug resistance to the isolates. 31 isolates (70%) were causing an infection, including urinary tract infection (20%), respiratory tract MATERIALS AND METHODS infection (18%), abdominal infection (18%), bacteraemia (9%) and skin and soft tissue infection In the present study, we tested the in vitro activity of (5%). 13 isolates were believed to be colonizers. antimicrobial agents against a well-characterized c o l l e c t i o n o f c a r b a p e n e m a s e - p r o d u c i n g Isolates were classified as 32 MDRE and 13 XDRE. -

Medical Review(S) Clinical Review
CENTER FOR DRUG EVALUATION AND RESEARCH APPLICATION NUMBER: 200327 MEDICAL REVIEW(S) CLINICAL REVIEW Application Type NDA Application Number(s) 200327 Priority or Standard Standard Submit Date(s) December 29, 2009 Received Date(s) December 30, 2009 PDUFA Goal Date October 30, 2010 Division / Office Division of Anti-Infective and Ophthalmology Products Office of Antimicrobial Products Reviewer Name(s) Ariel Ramirez Porcalla, MD, MPH Neil Rellosa, MD Review Completion October 29, 2010 Date Established Name Ceftaroline fosamil for injection (Proposed) Trade Name Teflaro Therapeutic Class Cephalosporin; ß-lactams Applicant Cerexa, Inc. Forest Laboratories, Inc. Formulation(s) 400 mg/vial and 600 mg/vial Intravenous Dosing Regimen 600 mg every 12 hours by IV infusion Indication(s) Acute Bacterial Skin and Skin Structure Infection (ABSSSI); Community-acquired Bacterial Pneumonia (CABP) Intended Population(s) Adults ≥ 18 years of age Template Version: March 6, 2009 Reference ID: 2857265 Clinical Review Ariel Ramirez Porcalla, MD, MPH Neil Rellosa, MD NDA 200327: Teflaro (ceftaroline fosamil) Table of Contents 1 RECOMMENDATIONS/RISK BENEFIT ASSESSMENT ......................................... 9 1.1 Recommendation on Regulatory Action ........................................................... 10 1.2 Risk Benefit Assessment.................................................................................. 10 1.3 Recommendations for Postmarketing Risk Evaluation and Mitigation Strategies ........................................................................................................................ -
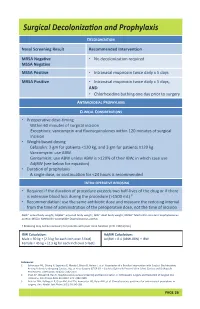

Surgical Decolonization and Prophylaxis
Surgical Decolonization and Prophylaxis SurgicalSurgical Decolonization Decolonization and Prophylaxis and Prophylaxis DECOLONIZATION DECOLONIZATION Nasal Screening Result Recommended Intervention Nasal Screening Result Recommended Intervention MRSA Negative • No decolonization required MSSAMRSA NegativeNegative • No decolonization required MSSA PositiveNegative • Intranasal mupirocin twice daily x 5 days MSSA Positive • Intranasal mupirocin twice daily x 5 days MRSA Positive • Intranasal mupirocin twice daily x 5 days, MRSA Positive AND• Intranasal mupirocin twice daily x 5 days, •ANDChlorhexidine bathing one day prior to surgery ANTIMICROBIAL• ChlorhexidinePROPHYLAXISbathing one day prior to surgery ANTIMICROBIAL PROPHYLAXIS CLINICAL CONSIDERATIONS • Preoperative dose-timing CLINICAL CONSIDERATIONS • PreoperativeWithin 60 minutesdose-timing of surgical incision WithinExceptions: 60 minutes vancomycin of surgicaland fluoroquinolones incision within 120 minutes of surgical incisionExceptions: vancomycin and fluoroquinolones within 120 minutes of surgical • Weightincision-based dosing • WeightCefazolin-based: 2 gm dosingfor patients <120 kg, and 3 gm for patients ≥120 kg Vancomycin:Cefazolin: 2 gm usefor ABW patients <120 kg, and 3 gm for patients ≥120 kg Gentamicin:Vancomycin: use use ABW ABW unless ABW is >120% of their IBW, in which case use AdjBWGentamicin:(see below use ABW for equation)unless ABW is >120% of their IBW, in which case use • DurationAdjBW of(see prophylaxis below for equation) • DurationA single of dose, prophylaxis -

Empiric Antimicrobial Therapy for Diabetic Foot Infection
Empiric Antimicrobial Therapy for Diabetic Foot Infection (NB Provincial Health Authorities Anti-Infective Stewardship Committee, September 2019) Infection Severity Preferred Empiric Regimens Alternative Regimens Comments Mild Wound less than 4 weeks duration:d Wound less than 4 weeks duration:e • Outpatient management • Cellulitis less than 2 cm and • cephalexin 500 – 1000 mg PO q6h*,a OR • clindamycin 300 – 450 mg PO q6h (only if recommended ,a • cefadroxil 500 – 1000 mg PO q12h* severe delayed reaction to a beta-lactam) without involvement of deeper • Tailor regimen based on culture tissues and susceptibility results and True immediate allergy to a beta-lactam at MRSA Suspected: • Non-limb threatening patient response risk of cross reactivity with cephalexin or • doxycycline 200 mg PO for 1 dose then • No signs of sepsis cefadroxil: 100 mg PO q12h OR • cefuroxime 500 mg PO q8–12h*,b • sulfamethoxazole+trimethoprim 800+160 mg to 1600+320 mg PO q12h*,f Wound greater than 4 weeks duration:d Wound greater than 4 weeks duratione • amoxicillin+clavulanate 875/125 mg PO and MRSA suspected: q12h*,c OR • doxycycline 200 mg PO for 1 dose then • cefuroxime 500 mg PO q8–12h*,b AND 100 mg PO q12h AND metroNIDAZOLE metroNIDAZOLE 500 mg PO q12h 500 mg PO q12h OR • sulfamethoxazole+trimethoprim 800+160 mg to 1600/320 mg PO q12h*,f AND metroNIDAZOLE 500 mg PO q12h Moderate Wound less than 4 weeks duration:d Wound less than 4 weeks duration:e • Initial management with • Cellulitis greater than 2 cm or • ceFAZolin 2 g IV q8h*,b OR • levoFLOXacin 750 -

Cusumano-Et-Al-2017.Pdf
International Journal of Infectious Diseases 63 (2017) 1–6 Contents lists available at ScienceDirect International Journal of Infectious Diseases journal homepage: www.elsevier.com/locate/ijid Rapidly growing Mycobacterium infections after cosmetic surgery in medical tourists: the Bronx experience and a review of the literature a a b c b Lucas R. Cusumano , Vivy Tran , Aileen Tlamsa , Philip Chung , Robert Grossberg , b b, Gregory Weston , Uzma N. Sarwar * a Albert Einstein College of Medicine, Montefiore Medical Center, Bronx, New York, USA b Division of Infectious Diseases, Department of Medicine, Albert Einstein College of Medicine, Montefiore Medical Center, Bronx, New York, USA c Department of Pharmacy, Nebraska Medicine, Omaha, Nebraska, USA A R T I C L E I N F O A B S T R A C T Article history: Background: Medical tourism is increasingly popular for elective cosmetic surgical procedures. However, Received 10 May 2017 medical tourism has been accompanied by reports of post-surgical infections due to rapidly growing Received in revised form 22 July 2017 mycobacteria (RGM). The authors’ experience working with patients with RGM infections who have Accepted 26 July 2017 returned to the USA after traveling abroad for cosmetic surgical procedures is described here. Corresponding Editor: Eskild Petersen, Methods: Patients who developed RGM infections after undergoing cosmetic surgeries abroad and who ?Aarhus, Denmark presented at the Montefiore Medical Center (Bronx, New York, USA) between August 2015 and June 2016 were identified. A review of patient medical records was performed. Keywords: Results: Four patients who presented with culture-proven RGM infections at the sites of recent cosmetic Mycobacterium abscessus complex procedures were identified. -

Cefalexin in the WHO Essential Medicines List for Children Reject
Reviewer No. 1: checklist for application of: Cefalexin In the WHO Essential Medicines List for Children (1) Have all important studies that you are aware of been included? Yes No 9 (2) Is there adequate evidence of efficacy for the proposed use? Yes 9 No (3) Is there evidence of efficacy in diverse settings and/or populations? Yes 9 No (4) Are there adverse effects of concern? Yes 9 No (5) Are there special requirements or training needed for safe/effective use? Yes No 9 (6) Is this product needed to meet the majority health needs of the population? Yes No 9 (7) Is the proposed dosage form registered by a stringent regulatory authority? Yes 9 No (8) What action do you propose for the Committee to take? Reject the application for inclusion of the following presentations of cefalexin: • Tablets/ capsules 250mg • Oral suspensions 125mg/5ml and 125mg/ml (9) Additional comment, if any. In order to identify any additional literature, the following broad and sensitive search was conducted using the PubMed Clinical Query application: (cephalexin OR cefalexin AND - 1 - pediatr*) AND ((clinical[Title/Abstract] AND trial[Title/Abstract]) OR clinical trials[MeSH Terms] OR clinical trial[Publication Type] OR random*[Title/Abstract] OR random allocation[MeSH Terms] OR therapeutic use[MeSH Subheading]) Only one small additional study was identified, which looked at the provision of prophylactic antibiotics in patients presenting to an urban children's hospital with trauma to the distal fingertip, requiring repair.1 In a prospective randomised control trial, 146 patients were enrolled, of which 69 were randomised to the no-antibiotic group, and 66 were randomised to the antibiotic (cefalexin) group. -

Structure of a Penicillin Binding Protein Complexed with a Cephalosporin-Peptidoglycan Mimic M.A
Structure of a Penicillin Binding Protein Complexed with a Cephalosporin-Peptidoglycan Mimic M.A. McDonough1, W. Lee2, N.R. Silvaggi1, L.P. Kotra 2, Z-H. Li2, Y. Takeda2, S .O. Mobashery2, and J.A. Kelly1 1Department of Molecular and Cell Biology and Institute for Materials Science, Univ. of Connecticut, Storrs, CT 2Institute for Drug Design and the Department of Chemistry, Wayne State Univ., Detroit, MI Many bacteria that are responsible for causing dis- lactams. Also, one questions why ß-lactamases hydro- eases in humans are rapidly developing mutant strains lyze ß-lactams and release them rapidly but they do resistant to existing antibiotics. Proliferation of these not react with peptide substrates. mutant strains is likely to be a serious health-care prob- To help answer these questions, structural studies lem of increasing proportions. Almost sixty percent of of the Streptomyces sp. R61 D-Ala-D-Ala-peptidase all clinically used antibiotics are beta-lactams, which have been undertaken to investigate how the enzyme stop the growth of bacteria by interfering with their cell- wall biosynthesis. The cell walls are made of glycan chains that polymerize to form a structure that gives strength and shape to the bacteria. An understanding of the process how the cell wall is synthesized may help in designing more potent antibiotics. D-Ala-D-Ala-carboxypeptidase/transpeptidases (DD-peptidases) are penicillin-binding proteins (PBPs), the targets of ß-lactam antibiotics such as penicillins and cephalosporins (Figure 1A). These enzymes cata- lyze the final cross-linking step of bacterial cell wall bio- synthesis. In vivo inhibition of PBPs by ß-lactams re- sults in the cessation of bacterial growth. -

UNASYN® (Ampicillin Sodium/Sulbactam Sodium)
® UNASYN (ampicillin sodium/sulbactam sodium) To reduce the development of drug-resistant bacteria and maintain the effectiveness of UNASYN® and other antibacterial drugs, UNASYN should be used only to treat infections that are proven or strongly suspected to be caused by bacteria. DESCRIPTION UNASYN is an injectable antibacterial combination consisting of the semisynthetic antibacterial ampicillin sodium and the beta-lactamase inhibitor sulbactam sodium for intravenous and intramuscular administration. Ampicillin sodium is derived from the penicillin nucleus, 6-aminopenicillanic acid. Chemically, it is monosodium (2S, 5R, 6R)-6-[(R)-2-amino-2-phenylacetamido]-3, 3-dimethyl-7-oxo-4-thia-1-azabicyclo[3.2.0]heptane-2-carboxylate and has a molecular weight of 371.39. Its chemical formula is C16H18N3NaO4S. The structural formula is: COONa O CH 3 N CH O 3 NH S NH 2 1 Reference ID: 4053909 Sulbactam sodium is a derivative of the basic penicillin nucleus. Chemically, sulbactam sodium is sodium penicillinate sulfone; sodium (2S, 5R)-3,3-dimethyl-7-oxo-4-thia- 1-azabicyclo [3.2.0] heptane-2-carboxylate 4,4-dioxide. Its chemical formula is C8H10NNaO5S with a molecular weight of 255.22. The structural formula is: COONa CH 3 O N CH 3 S O O UNASYN, ampicillin sodium/sulbactam sodium parenteral combination, is available as a white to off-white dry powder for reconstitution. UNASYN dry powder is freely soluble in aqueous diluents to yield pale yellow to yellow solutions containing ampicillin sodium and sulbactam sodium equivalent to 250 mg ampicillin per mL and 125 mg sulbactam per mL. The pH of the solutions is between 8.0 and 10.0. -

The Antibacterial Activity of Cefpodoxime and the Novel Β
Session-198 b SATURDAY-279 The Antibacterial Activity of Cefpodoxime and the Novel -lactamase Inhibitor ETX1317 Against Recent Clinical Isolates of b-lactamase-producing Enterobacteriaceae Entasis Therapeutics S. McLeod1, M. Hackel2, R. Badal2, A. Shapiro1, J. Mueller1, R. Tommasi1, and A. Miller1 1-781-810-0120 1Entasis Therapeutics, Waltham, MA and 2IHMA, International Health Management Associates, Schaumburg, IL USA www.entasistx.com Abstract In vitro activity of ETX1317 vs. comparator BLIs Cumulative activity vs. 911 ESBL-enriched Enterobacteriaceae from 2013-2015 Activity vs. 35 sequenced KPC+ and/or MBL+ Enterobacteriaceae MIC (mg/L) Background β-lactamase inhibition (IC50, µM) Strain ID Species encoded bla genes IPM CAZ-AVI CPD-ETX1317 ETX1317 ETX1317 is a novel, diazabicyclooctenone inhibitor of serine β-lactamases that Number (cumulative %) of isolates inhibited at MIC (mg/L) Class A Class C Class D Drug %S* ARC3528*¥ E. cloacae AmpC [∆308-313(SKVALA)] 0.25 32 0.125 4 restores β-lactam activity against multidrug-resistant Enterobacteriaceae. ETX0282, < 0.03 0.06 0.12 0.25 0.5 1 2 4 8 16 32 > 32 ARC4165*¥ C. freundii CMY-2; AmpC [N366Y]; TEM-1; SHV-5 2 32 ≤0.03 4 the oral prodrug of ETX1317, is currently under investigation in combination with BLI CTX-M-15 SHV-5 KPC-2 TEM-1 AmpC* P99 OXA-24/40 OXA-48 0 5 6 14 19 34 20 27 17 18 18 733 3 CPD 10.8 ARC6479* K. oxytoca NDM-1 16 >32 32 32 cefpodoxime proxetil (CPDP), which is hydrolyzed in vivo to release cefpodoxime 0% 0.5% 1% 3% 5% 9% 11% 14% 16% 18% 20% 100% (CPD). -

Antibiotic Assay Medium No. 3 (Assay Broth) Is Used for Microbiological Assay of Antibiotics. M042
HiMedia Laboratories Technical Data Antibiotic Assay Medium No. 3 (Assay Broth) is used for M042 microbiological assay of antibiotics. Antibiotic Assay Medium No. 3 (Assay Broth) is used for microbiological assay of antibiotics. Composition** Ingredients Gms / Litre Peptic digest of animal tissue (Peptone) 5.000 Beef extract 1.500 Yeast extract 1.500 Dextrose 1.000 Sodium chloride 3.500 Dipotassium phosphate 3.680 Potassium dihydrogen phosphate 1.320 Final pH ( at 25°C) 7.0±0.2 **Formula adjusted, standardized to suit performance parameters Directions Suspend 17.5 grams in 1000 ml distilled water. Heat if necessary to dissolve the medium completely. Sterilize by autoclaving at 15 lbs pressure (121°C) for 15 minutes. Advice:Recommended for the Microbiological assay of Amikacin, Bacitracin, Capreomycin, Chlortetracycline,Chloramphenicol,Cycloserine,Demeclocycline,Dihydrostreptomycin, Doxycycline, Gentamicin, Gramicidin, Kanamycin, Methacycline, Neomycin, Novobiocin, Oxytetracycline, Rolitetracycline, Streptomycin, Tetracycline, Tobramycin, Trolendomycin and Tylosin according to official methods . Principle And Interpretation Antibiotic Assay Medium is used in the performance of antibiotic assays. Grove and Randall have elucidated those antibiotic assays and media in their comprehensive treatise on antibiotic assays (1). Antibiotic Assay Medium No. 3 (Assay Broth) is used in the microbiological assay of different antibiotics in pharmaceutical and food products by the turbidimetric method. Ripperre et al reported that turbidimetric methods for determining the potency of antibiotics are inherently more accurate and more precise than agar diffusion procedures (2). Turbidimetric antibiotic assay is based on the change or inhibition of growth of a test microorganims in a liquid medium containing a uniform concentration of an antibiotic. After incubation of the test organism in the working dilutions of the antibiotics, the amount of growth is determined by measuring the light transmittance using spectrophotometer. -
Antimicrobial Surgical Prophylaxis
Antimicrobial Surgical Prophylaxis The antimicrobial surgical prophylaxis protocol establishes evidence-based standards for surgical prophylaxis at The Nebraska Medical Center. The protocol was adapted from the recently published consensus guidelines from the American Society of Health-System Pharmacists (ASHP), Society for Healthcare Epidemiology of America (SHEA), Infectious Disease Society of America (IDSA), and the Surgical Infection Society (SIS) and customized to Nebraska Medicine with the input of the Antimicrobial Stewardship Program in concert with the various surgical groups at the institution. The protocol established here-in will be implemented via standard order sets utilized within One Chart. Routine surgical prophylaxis and current and future surgical order sets are expected to conform to this guidance. Antimicrobial Surgical Prophylaxis Initiation Optimal timing: Within 60 minutes before surgical incision o Exceptions: Fluoroquinolones and vancomycin (within 120 minutes before surgical incision) Successful prophylaxis necessitates that the antimicrobial agent achieve serum and tissue concentrations above the MIC for probable organisms associated with the specific procedure type at the time of incision as well as for the duration of the procedure. Renal Dose Adjustment Guidance The following table can be utilized to determine if adjustments are needed to antimicrobial surgical prophylaxis for both pre-op and post-op dosing. Table 1 Renal Dosage Adjustment Dosing Regimen with Dosing Regimen with CrCl Dosing Regimen with -
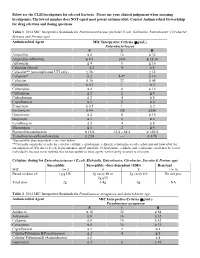
Below Are the CLSI Breakpoints for Selected Bacteria. Please Use Your Clinical Judgement When Assessing Breakpoints
Below are the CLSI breakpoints for selected bacteria. Please use your clinical judgement when assessing breakpoints. The lowest number does NOT equal most potent antimicrobial. Contact Antimicrobial Stewardship for drug selection and dosing questions. Table 1: 2014 MIC Interpretive Standards for Enterobacteriaceae (includes E.coli, Klebsiella, Enterobacter, Citrobacter, Serratia and Proteus spp) Antimicrobial Agent MIC Interpretive Criteria (g/mL) Enterobacteriaceae S I R Ampicillin ≤ 8 16 ≥ 32 Ampicillin-sulbactam ≤ 8/4 16/8 ≥ 32/16 Aztreonam ≤ 4 8 ≥ 16 Cefazolin (blood) ≤ 2 4 ≥ 8 Cefazolin** (uncomplicated UTI only) ≤ 16 ≥ 32 Cefepime* ≤ 2 4-8* ≥ 16 Cefotetan ≤ 16 32 ≥ 64 Ceftaroline ≤ 0.5 1 ≥ 2 Ceftazidime ≤ 4 8 ≥ 16 Ceftriaxone ≤ 1 2 ≥ 4 Cefpodoxime ≤ 2 4 ≥ 8 Ciprofloxacin ≤ 1 2 ≥ 4 Ertapenem ≤ 0.5 1 ≥ 2 Fosfomycin ≤ 64 128 ≥256 Gentamicin ≤ 4 8 ≥ 16 Imipenem ≤ 1 2 ≥ 4 Levofloxacin ≤ 2 4 ≥ 8 Meropenem ≤ 1 2 ≥ 4 Piperacillin-tazobactam ≤ 16/4 32/4 – 64/4 ≥ 128/4 Trimethoprim-sulfamethoxazole ≤ 2/38 --- ≥ 4/76 *Susceptibile dose-dependent – see chart below **Cefazolin can predict results for cefaclor, cefdinir, cefpodoxime, cefprozil, cefuroxime axetil, cephalexin and loracarbef for uncomplicated UTIs due to E.coli, K.pneumoniae, and P.mirabilis. Cefpodoxime, cefinidir, and cefuroxime axetil may be tested individually because some isolated may be susceptible to these agents while testing resistant to cefazolin. Cefepime dosing for Enterobacteriaceae ( E.coli, Klebsiella, Enterobacter, Citrobacter, Serratia & Proteus spp) Susceptible Susceptible –dose-dependent (SDD) Resistant MIC </= 2 4 8 >/= 16 Based on dose of: 1g q12h 1g every 8h or 2g every 8 h Do not give 2g q12 Total dose 2g 3-4g 6g NA Table 2: 2014 MIC Interpretive Standards for Pseudomonas aeruginosa and Acinetobacter spp.