In Vitro Susceptibilities of Escherichia Coli and Klebsiella Spp. To
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Medical Review(S) Clinical Review
CENTER FOR DRUG EVALUATION AND RESEARCH APPLICATION NUMBER: 200327 MEDICAL REVIEW(S) CLINICAL REVIEW Application Type NDA Application Number(s) 200327 Priority or Standard Standard Submit Date(s) December 29, 2009 Received Date(s) December 30, 2009 PDUFA Goal Date October 30, 2010 Division / Office Division of Anti-Infective and Ophthalmology Products Office of Antimicrobial Products Reviewer Name(s) Ariel Ramirez Porcalla, MD, MPH Neil Rellosa, MD Review Completion October 29, 2010 Date Established Name Ceftaroline fosamil for injection (Proposed) Trade Name Teflaro Therapeutic Class Cephalosporin; ß-lactams Applicant Cerexa, Inc. Forest Laboratories, Inc. Formulation(s) 400 mg/vial and 600 mg/vial Intravenous Dosing Regimen 600 mg every 12 hours by IV infusion Indication(s) Acute Bacterial Skin and Skin Structure Infection (ABSSSI); Community-acquired Bacterial Pneumonia (CABP) Intended Population(s) Adults ≥ 18 years of age Template Version: March 6, 2009 Reference ID: 2857265 Clinical Review Ariel Ramirez Porcalla, MD, MPH Neil Rellosa, MD NDA 200327: Teflaro (ceftaroline fosamil) Table of Contents 1 RECOMMENDATIONS/RISK BENEFIT ASSESSMENT ......................................... 9 1.1 Recommendation on Regulatory Action ........................................................... 10 1.2 Risk Benefit Assessment.................................................................................. 10 1.3 Recommendations for Postmarketing Risk Evaluation and Mitigation Strategies ........................................................................................................................ -

“Ceftriaxone– Sulbactam–EDTA” and Various Antibiotics Against Gram
ORIGINAL ARTICLE A Comparative In Vitro Sensitivity Study of “Ceftriaxone– Sulbactam–EDTA” and Various Antibiotics against Gram- negative Bacterial Isolates from Intensive Care Unit Sweta Singh1, Chinmoy Sahu2, Sangram Singh Patel3, Abhay Singh4, Nidhi Yaduvanshi5 ABSTRACT Introduction: A rapid increase in multidrug-resistant (MDR) strains is being seen across the globe especially in the Southeast Asian region, including India. Carbapenems and colistin form the mainstay of treatment against gram-negative pathogens, especially extended-spectrum beta-lactamase (ESBL)- and metallo-beta-lactamse (MBL)-producing isolates. However, due to increased resistance to carbapenems and toxicity of colistin, especially in intensive care units (ICUs), carbapenem-sparing antibiotics like ceftriaxone–sulbactam–EDTA (CSE) combination needs to be evaluated. Materials and methods: Bacterial isolates cultured from various clinical samples from all ICUs for a period of 9 months were evaluated. Bacterial identification was performed by matrix assisted laser desorption ionization time of flight mass spectrometry (MALDI-TOF MS) and antibiotic susceptibility testing were performed by disk diffusion and E test method. Antibiogram of various antibiotics was noted. Extended-spectrum beta-lactamase- and MBL-producing bacteria were identified by phenotypic methods. Antibiotic sensitivity results of CSE were compared with the comparator drugs like colistin, carbapenems, and tigecycline in Enterobacteriaceae, Acinetobacter spp., and Pseudomonas spp. along with ESBL and MBL producers. Results: A total of 2,760 samples of blood, cerebrospinal fluid (CSF), respiratory samples, tissue, and pus were collected from ICUs with maximum isolates from pus (37%) followed by respiratory samples (31%) and blood (27%). Escherichia coli and Klebsiella pneumoniae were the predominant gram-negative pathogens accounting for 56% of the isolates followed by Acinetobacter spp. -

Antimicrobial Susceptibility Among Colistin, Sulbactam, And
Hindawi Journal of Pathogens Volume 2018, Article ID 3893492, 5 pages https://doi.org/10.1155/2018/3893492 Research Article Antimicrobial Susceptibility among Colistin, Sulbactam, and Fosfomycin and a Synergism Study of Colistin in Combination with Sulbactam or Fosfomycin against Clinical Isolates of Carbapenem-Resistant Acinetobacter baumannii Sombat Leelasupasri,1 Wichai Santimaleeworagun ,2,3 and Tossawan Jitwasinkul3,4 1 Internal Medicine Unit, Phyathai II International Hospital, Bangkok, Tailand 2Department of Pharmacy, Faculty of Pharmacy, Silpakorn University, Nakhon Pathom, Tailand 3Antibiotic Optimization and Patient Care Project by Pharmaceutical Initiative for Resistant Bacteria and Infectious Diseases Working Group (PIRBIG), Silpakorn University, Nakhon Pathom, Tailand 4Department of Biopharmacy, Faculty of Pharmacy, Silpakorn University, Nakhon Pathom, Tailand Correspondence should be addressed to Wichai Santimaleeworagun; [email protected] Received 28 August 2017; Revised 9 December 2017; Accepted 25 December 2017; Published 18 January 2018 Academic Editor: Jose Yuste Copyright © 2018 Sombat Leelasupasri et al. Tis is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Tis in vitro study aimed to determine the activity of colistin plus sulbactam and colistin plus fosfomycin against carbapenem- resistant A. baumannii (CRAB). Fifeen clinical isolates were obtained from patients admitted to Phyathai II International Hospital, Bangkok, Tailand, from August 2014 to April 2015. Te antimicrobial susceptibilities of colistin, sulbactam, and fosfomycin were evaluated using the E-test or broth microdilution and the synergistic activity of the antibacterial combinations (colistin plus sulbactam or fosfomycin) was determined using the chequerboard method. Clonal relationships were explored using repetitive element palindromic- (REP-) PCR. -

General Items
Essential Medicines List (EML) 2019 Application for the inclusion of imipenem/cilastatin, meropenem and amoxicillin/clavulanic acid in the WHO Model List of Essential Medicines, as reserve second-line drugs for the treatment of multidrug-resistant tuberculosis (complementary lists of anti-tuberculosis drugs for use in adults and children) General items 1. Summary statement of the proposal for inclusion, change or deletion This application concerns the updating of the forthcoming WHO Model List of Essential Medicines (EML) and WHO Model List of Essential Medicines for Children (EMLc) to include the following medicines: 1) Imipenem/cilastatin (Imp-Cln) to the main list but NOT the children’s list (it is already mentioned on both lists as an option in section 6.2.1 Beta Lactam medicines) 2) Meropenem (Mpm) to both the main and the children’s lists (it is already on the list as treatment for meningitis in section 6.2.1 Beta Lactam medicines) 3) Clavulanic acid to both the main and the children’s lists (it is already listed as amoxicillin/clavulanic acid (Amx-Clv), the only commercially available preparation of clavulanic acid, in section 6.2.1 Beta Lactam medicines) This application makes reference to amendments recommended in particular to section 6.2.4 Antituberculosis medicines in the latest editions of both the main EML (20th list) and the EMLc (6th list) released in 2017 (1),(2). On the basis of the most recent Guideline Development Group advising WHO on the revision of its guidelines for the treatment of multidrug- or rifampicin-resistant (MDR/RR-TB)(3), the applicant considers that the three agents concerned be viewed as essential medicines for these forms of TB in countries. -

Activity of Imipenem, Meropenem, Cefepime, and Sulbactam in Combination with the Β-Lactamase Inhibitor LN-1-255 Against Acinetobacter Spp
antibiotics Article Activity of Imipenem, Meropenem, Cefepime, and Sulbactam in Combination with the β-Lactamase Inhibitor LN-1-255 against Acinetobacter spp. Cristina Lasarte-Monterrubio 1,† , Juan C. Vázquez-Ucha 1,† , Maria Maneiro 2, Jorge Arca-Suárez 1,*, Isaac Alonso 3, Paula Guijarro-Sánchez 1 , John D. Buynak 4, Germán Bou 1, Concepción González-Bello 2 and Alejandro Beceiro 1,* 1 Servicio de Microbiología, Instituto de Investigación Biomédica de A Coruña (INIBIC-CICA), Complejo Hospitalario Universitario A Coruña (CHUAC), As Xubias 84, 15006 A Coruña, Spain; [email protected] (C.L.-M.); [email protected] (J.C.V.-U.); [email protected] (P.G.-S.); [email protected] (G.B.) 2 Centro Singular de Investigación en Química Biolóxica e Materiais Moleculares (CIQUS), Departamento de Química Orgánica, Universidade de Santiago de Compostela, Jenaro de la Fuente s/n, 15782 Santiago de Compostela, Spain; [email protected] (M.M.); [email protected] (C.G.-B.) 3 Servicio de Microbiología, Hospital Provincial Pontevedra, Loureiro Crespo 2, 36002 Pontevedra, Spain; Citation: Lasarte-Monterrubio, C.; [email protected] 4 Vázquez-Ucha, J.C.; Maneiro, M.; Department of Chemistry, Southern Methodist University, Dallas, TX 75275, USA; [email protected] Arca-Suárez, J.; Alonso, I.; * Correspondence: [email protected] (J.A.-S.); [email protected] (A.B.); Tel.: +34-981-176-087 (J.A.-S.); +34-981-176-087 (A.B.) Guijarro-Sánchez, P.; Buynak, J.D.; † Cristina Lasarte-Monterrubio and Juan C. Vázquez-Ucha contributed equally to the study. Bou, G.; González-Bello, C.; Beceiro, A. -

Antimicrobial Stewardship Guidance
Antimicrobial Stewardship Guidance Federal Bureau of Prisons Clinical Practice Guidelines March 2013 Clinical guidelines are made available to the public for informational purposes only. The Federal Bureau of Prisons (BOP) does not warrant these guidelines for any other purpose, and assumes no responsibility for any injury or damage resulting from the reliance thereof. Proper medical practice necessitates that all cases are evaluated on an individual basis and that treatment decisions are patient-specific. Consult the BOP Clinical Practice Guidelines Web page to determine the date of the most recent update to this document: http://www.bop.gov/news/medresources.jsp Federal Bureau of Prisons Antimicrobial Stewardship Guidance Clinical Practice Guidelines March 2013 Table of Contents 1. Purpose ............................................................................................................................................. 3 2. Introduction ...................................................................................................................................... 3 3. Antimicrobial Stewardship in the BOP............................................................................................ 4 4. General Guidance for Diagnosis and Identifying Infection ............................................................. 5 Diagnosis of Specific Infections ........................................................................................................ 6 Upper Respiratory Infections (not otherwise specified) .............................................................................. -
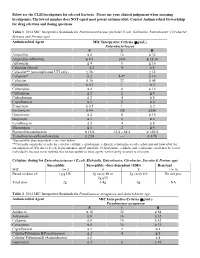
Below Are the CLSI Breakpoints for Selected Bacteria. Please Use Your Clinical Judgement When Assessing Breakpoints
Below are the CLSI breakpoints for selected bacteria. Please use your clinical judgement when assessing breakpoints. The lowest number does NOT equal most potent antimicrobial. Contact Antimicrobial Stewardship for drug selection and dosing questions. Table 1: 2014 MIC Interpretive Standards for Enterobacteriaceae (includes E.coli, Klebsiella, Enterobacter, Citrobacter, Serratia and Proteus spp) Antimicrobial Agent MIC Interpretive Criteria (g/mL) Enterobacteriaceae S I R Ampicillin ≤ 8 16 ≥ 32 Ampicillin-sulbactam ≤ 8/4 16/8 ≥ 32/16 Aztreonam ≤ 4 8 ≥ 16 Cefazolin (blood) ≤ 2 4 ≥ 8 Cefazolin** (uncomplicated UTI only) ≤ 16 ≥ 32 Cefepime* ≤ 2 4-8* ≥ 16 Cefotetan ≤ 16 32 ≥ 64 Ceftaroline ≤ 0.5 1 ≥ 2 Ceftazidime ≤ 4 8 ≥ 16 Ceftriaxone ≤ 1 2 ≥ 4 Cefpodoxime ≤ 2 4 ≥ 8 Ciprofloxacin ≤ 1 2 ≥ 4 Ertapenem ≤ 0.5 1 ≥ 2 Fosfomycin ≤ 64 128 ≥256 Gentamicin ≤ 4 8 ≥ 16 Imipenem ≤ 1 2 ≥ 4 Levofloxacin ≤ 2 4 ≥ 8 Meropenem ≤ 1 2 ≥ 4 Piperacillin-tazobactam ≤ 16/4 32/4 – 64/4 ≥ 128/4 Trimethoprim-sulfamethoxazole ≤ 2/38 --- ≥ 4/76 *Susceptibile dose-dependent – see chart below **Cefazolin can predict results for cefaclor, cefdinir, cefpodoxime, cefprozil, cefuroxime axetil, cephalexin and loracarbef for uncomplicated UTIs due to E.coli, K.pneumoniae, and P.mirabilis. Cefpodoxime, cefinidir, and cefuroxime axetil may be tested individually because some isolated may be susceptible to these agents while testing resistant to cefazolin. Cefepime dosing for Enterobacteriaceae ( E.coli, Klebsiella, Enterobacter, Citrobacter, Serratia & Proteus spp) Susceptible Susceptible –dose-dependent (SDD) Resistant MIC </= 2 4 8 >/= 16 Based on dose of: 1g q12h 1g every 8h or 2g every 8 h Do not give 2g q12 Total dose 2g 3-4g 6g NA Table 2: 2014 MIC Interpretive Standards for Pseudomonas aeruginosa and Acinetobacter spp. -

Ampicillin (Ampicillin Sodium) INJECTION, POWDER, FOR
Ampicillin for Injection, USP Rx Only (For Intramuscular or Intravenous Injection) To reduce the development of drug-resistant bacteria and maintain the effectiveness of ampicillin and other antibacterial drugs, ampicillin should be used only to treat or prevent infections that are proven or strongly suspected to be caused by bacteria. DESCRIPTION Ampicillin for injection, USP the monosodium salt of [2S-[2α,5α,6β(S*)]]-6- [(aminophenylacetyl)amino]-3,3-dimethyl-7-oxo-4-thia-1-azabicyclo[3.2.0]heptane-2-carboxylic acid, is a synthetic penicillin. It is an antibacterial agent with a broad spectrum of bactericidal activity against both penicillin-susceptible Gram-positive organisms and many common Gram-negative pathogens. Ampicillin for injection, USP is a white to cream-tinged, crystalline powder. The reconstituted solution is clear, colorless and free from visible particulates. Each vial of Ampicillin for injection, USP contains ampicillin sodium equivalent to 250 mg, 500 mg, 1 gram or 2 grams ampicillin. Ampicillin for injection, USP contains 65.8 mg [2.9 mEq] sodium per gram ampicillin. It has the following molecular structure: The molecular formula is C16H18N3NaO4S, and the molecular weight is 371.39. The pH range of the reconstituted solution is 8 to 10. CLINICAL PHARMACOLOGY Ampicillin for injection diffuses readily into most body tissues and fluids. However, penetration into the cerebrospinal fluid and brain occurs only when the meninges are inflamed. Ampicillin is excreted largely unchanged in the urine and its excretion can be delayed by concurrent administration of probenecid. Due to maturational changes in renal function, ampicillin half-life decreases as postmenstrual age (a sum of gestational age and postnatal age) increases for infants with postnatal age of less than 28 days. -

Eml-2017-Antibacterials-Eng.Pdf
Consideration of antibacterial medicines as part of the revisions to 2017 WHO Model List of Essential Medicines for adults (EML) and Model List of Essential Medicines for children (EMLc) Section 6.2 Antibacterials including Access, Watch and Reserve Lists of antibiotics This summary has been prepared by the Health Technologies and Pharmaceuticals (HTP) programme at the WHO Regional Office for Europe. It is intended to communicate changes to the 2017 WHO Model List of Essential Medicines for adults (EML) and Model List of Essential Medicines for children (EMLc) to national counterparts involved in the evidence-based selection of medicines for inclusion in national essential medicines lists (NEMLs), lists of medicines for inclusion in reimbursement programs, and medicine formularies for use in primary, secondary and tertiary care. This document does not replace the full report of the WHO Expert Committee, 2017 and this summary should be read in conjunction with the full report (WHO Technical Report Series, No. 1006; http://apps.who.int/iris/bitstream/10665/259481/1/9789241210157-eng.pdf?ua=1). The revised lists of essential medicines (in English) are available as follows: 2017 WHO Model List of Essential Medicines for adults (EML) http://www.who.int/medicines/publications/essentialmedicines/20th_EML2017_FINAL_amend edAug2017.pdf?ua=1 2017 Model List of Essential Medicines for children (EMLc) http://www.who.int/medicines/publications/essentialmedicines/6th_EMLc2017_FINAL_amend edAug2017.pdf?ua=1 Summary of changes to Section 6.2 Antibacterials: Section 6 of the EML covers anti-infective medicines. Disease-specific subsections within Section 6, such as those covering medicines for tuberculosis, HIV, hepatitis and malaria, have been regularly reviewed and updated, taking into consideration relevant WHO treatment guidelines. -

Amoxicillin and Clavulanic Acid)
European Medicines Agency London, 19 October 2009 Doc. Ref. EMEA/CHMP/97898/2009 rev 1 EMEA/H/A-30/979 Questions and answers on the referral for Augmentin (amoxicillin and clavulanic acid) The European Medicines Agency has completed a review of Augmentin. The Agency’s Committee for Medicinal Products for Human Use (CHMP) has concluded that there is a need to harmonise the prescribing information for Augmentin in the European Union (EU). The review was carried out under an ‘Article 30’ referral1. What is Augmentin? Augmentin is an antibiotic. It is used for the short-term treatment of a number of common infections: • infections of the respiratory tract (airways and lungs) such as tonsillitis, sinusitis, otitis media (infection of the middle ear), exacerbation (flare up) of bronchitis and pneumonia; • infections of the urinary tract (the structures that carry urine in the body); • infections of the skin and soft tissues (the structures just below the skin); It can also be used for more serious infections, such as bone or intra-abdominal infections. It can be used in the prevention of some infections. Augmentin, also known as ‘coamoxiclav’, contains two active substances: amoxicillin, which is an antibiotic belonging to the beta-lactam family (the same family as penicillins), and clavulanic acid, which is a ‘beta-lactamase inhibitor’. When Augmentin is absorbed in the body, the amoxicillin component kills the bacteria that are causing the infection, while the clavulanic acid component blocks an enzyme, betalactamase that enable the bacteria to destroy amoxicillin. As a result, the antibiotic can work for longer, and is more effective in killing bacteria. -

Amoxicillin-Clavulanic Acid
HIGHLIGHTS OF PRESCRIBING INFORMATION ------------------------------ CONTRAINDICATIONS ---------------------- These highlights do not include all the information needed to use • History of a serious hypersensitivity reaction (e.g., anaphylaxis or AUGMENTIN safely and effectively. See full prescribing Stevens-Johnson syndrome) to AUGMENTIN or to other information for AUGMENTIN. beta-lactams (e.g., penicillins or cephalosporins) (4) • History of cholestatic jaundice/hepatic dysfunction associated with AUGMENTIN (amoxicillin/clavulanate potassium) Tablets, AUGMENTIN. (4) Powder for Oral Suspension, and Chewable Tablets ----------------------- WARNINGS AND PRECAUTIONS --------------- Initial U.S. Approval: 1984 • Serious (including fatal) hypersensitivity reactions: Discontinue To reduce the development of drug-resistant bacteria and maintain the AUGMENTIN if a reaction occurs. (5.1) effectiveness of AUGMENTIN and other antibacterial drugs, • Hepatic dysfunction and cholestatic jaundice: Discontinue if AUGMENTIN should be used only to treat infections that are proven signs/symptoms of hepatitis occur. Monitor liver function tests in or strongly suspected to be caused by bacteria. patients with hepatic impairment. (5.2) ---------------------------- INDICATIONS AND USAGE ------------------- • Clostridium difficile-associated diarrhea (CDAD): Evaluate AUGMENTIN is a combination penicillin-class antibacterial and patients if diarrhea occurs. (5.3) beta-lactamase inhibitor indicated for treatment of the following: • Patients with mononucleosis -

The Prevalence and Antimicrobial Resistance of Haemophilus Infuenzae in Prepubertal Girls with Vulvovaginitis
The prevalence and antimicrobial resistance of Haemophilus inuenzae in prepubertal girls with vulvovaginitis Mingming Zhou The Children's Hospital, Zhejiang University School of Medicine Liying Sun The Children's Hospital, Zhejiang University School of Medicine Xuejun Chen ( [email protected] ) Chao Fang The Children's Hospital, Zhejiang University School of Medicine Jianping Li The Children's Hospital, Zhejiang University School of Medicine Chunzhen Hua The Children's Hospital, Zhejiang University School of Medicne Research article Keywords: Haemophilus inuenzae, Vulvovaginitis, Prepubertal, Antimicrobial resistance, Vulval Posted Date: July 16th, 2020 DOI: https://doi.org/10.21203/rs.3.rs-41705/v1 License: This work is licensed under a Creative Commons Attribution 4.0 International License. Read Full License Page 1/16 Abstract Background: To determine the prevalence of Haemophilus inuenzae vulvovaginitis in prepubertal girls and the antimicrobial resistance of H.inuenzae strains isolated from vulval specimens. Methods: Isolates of H.inuenzae from vulval swabs of prepubertal girls with vulvovaginitis received at The Children's Hospital, Zhejiang University School of Medicine during 2016-2019 were studied. Vulval specimens were inoculated on Haemophilus selective chocolate agar. Antimicrobial susceptibility tests were performed using the disk diffusion method. A cenase disk was used to detect β-lactamase. Results: A total of 4142 vulval specimens were received during the 4 years, 649 isolates of H. inuenzae were isolated from 642 girls aged 6 months to 13 years, with a median of 5y. There were peaks of isolates from April to July seen in the vulval isolates. In total, the ampicillin resistance rate was 39.1% (250/640); 33.2% strains (211/636) were for β-lactamase-positive isolates, 6.6% strains (42/635) were β- lactamase-negative and ampicillin-resistant (BLNAR) isolates.