Sensory Conduction in Medial Plantar Nerve
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Clinical Presentations of Lumbar Disc Degeneration and Lumbosacral Nerve Lesions
Hindawi International Journal of Rheumatology Volume 2020, Article ID 2919625, 13 pages https://doi.org/10.1155/2020/2919625 Review Article Clinical Presentations of Lumbar Disc Degeneration and Lumbosacral Nerve Lesions Worku Abie Liyew Biomedical Science Department, School of Medicine, Debre Markos University, Debre Markos, Ethiopia Correspondence should be addressed to Worku Abie Liyew; [email protected] Received 25 April 2020; Revised 26 June 2020; Accepted 13 July 2020; Published 29 August 2020 Academic Editor: Bruce M. Rothschild Copyright © 2020 Worku Abie Liyew. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Lumbar disc degeneration is defined as the wear and tear of lumbar intervertebral disc, and it is mainly occurring at L3-L4 and L4-S1 vertebrae. Lumbar disc degeneration may lead to disc bulging, osteophytes, loss of disc space, and compression and irritation of the adjacent nerve root. Clinical presentations associated with lumbar disc degeneration and lumbosacral nerve lesion are discogenic pain, radical pain, muscular weakness, and cutaneous. Discogenic pain is usually felt in the lumbar region, or sometimes, it may feel in the buttocks, down to the upper thighs, and it is typically presented with sudden forced flexion and/or rotational moment. Radical pain, muscular weakness, and sensory defects associated with lumbosacral nerve lesions are distributed on -

Piriformis Syndrome Is Overdiagnosed 11 Robert A
American Association of Neuromuscular & Electrodiagnostic Medicine AANEM CROSSFIRE: CONTROVERSIES IN NEUROMUSCULAR AND ELECTRODIAGNOSTIC MEDICINE Loren M. Fishman, MD, B.Phil Robert A.Werner, MD, MS Scott J. Primack, DO Willam S. Pease, MD Ernest W. Johnson, MD Lawrence R. Robinson, MD 2005 AANEM COURSE F AANEM 52ND Annual Scientific Meeting Monterey, California CROSSFIRE: Controversies in Neuromuscular and Electrodiagnostic Medicine Loren M. Fishman, MD, B.Phil Robert A.Werner, MD, MS Scott J. Primack, DO Willam S. Pease, MD Ernest W. Johnson, MD Lawrence R. Robinson, MD 2005 COURSE F AANEM 52nd Annual Scientific Meeting Monterey, California AANEM Copyright © September 2005 American Association of Neuromuscular & Electrodiagnostic Medicine 421 First Avenue SW, Suite 300 East Rochester, MN 55902 PRINTED BY JOHNSON PRINTING COMPANY, INC. ii CROSSFIRE: Controversies in Neuromuscular and Electrodiagnostic Medicine Faculty Loren M. Fishman, MD, B.Phil Scott J. Primack, DO Assistant Clinical Professor Co-director Department of Physical Medicine and Rehabilitation Colorado Rehabilitation and Occupational Medicine Columbia College of Physicians and Surgeons Denver, Colorado New York City, New York Dr. Primack completed his residency at the Rehabilitation Institute of Dr. Fishman is a specialist in low back pain and sciatica, electrodiagnosis, Chicago in 1992. He then spent 6 months with Dr. Larry Mack at the functional assessment, and cognitive rehabilitation. Over the last 20 years, University of Washington. Dr. Mack, in conjunction with the Shoulder he has lectured frequently and contributed over 55 publications. His most and Elbow Service at the University of Washington, performed some of the recent work, Relief is in the Stretch: End Back Pain Through Yoga, and the original research utilizing musculoskeletal ultrasound in order to diagnose earlier book, Back Talk, both written with Carol Ardman, were published shoulder pathology. -

Sensory Conduction in Medial and Lateral Plantar Nerves
J Neurol Neurosurg Psychiatry: first published as 10.1136/jnnp.51.2.188 on 1 February 1988. Downloaded from Journal ofNeurology, Neurosurgery, and Psychiatry 1988;51:188-191 Sensory conduction in medial and lateral plantar nerves S N PONSFORD From the Department of Clinical Neurophysiology, Walsgrave Hospital, Coventry, UK SUMMARY A simple and reliable method of recording medial and lateral plantar nerve sensory action potentials is described. Potentials are recorded with surface electrodes at the ankle using surface electrodes stimulating orthodromically at the sole. The normal values obtained are higher in amplitude than those obtained by the method described by Guiloff and Sherratt and are detectable in older subjects aged over 80 years. The procedure is valuable in the diagnosis of early peripheral neuropathy, mononeuritig multiplex; tarsal tunnel syndrome and in differentiation between pre and post ganglionic L5 SI lesions. The value of medial plantar sensory action potential EL53051 applied to the sole just lateral to the first meta-guest. Protected by copyright. (SAP) recording in the diagnosis of peripheral neuro- tarsal, the anode level with metatarsophalangeal joint, the pathy and investigation of root or individual nerve cathode thus overlying the first common digital nerve sub- lesions involving the leg or foot was clearly estab- serving contiguous surfaces ofthe great and second toes. For the lateral plantar, the stimulator was placed between the lished by Guiloff and Sherratt.1 However, their fourth and fifth metatarsals, the anode-again level with the method of stimulating at the big toe and recording at metatarsophalangeal joint, overlying the fourth common the ankle gives potentials of relatively small ampli- digital nerve supplying contiguous surfaces of the fourth and tude (mean amplitude 2-3 pv, range 0-8- 1). -
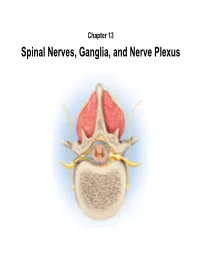
Spinal Nerves, Ganglia, and Nerve Plexus Spinal Nerves
Chapter 13 Spinal Nerves, Ganglia, and Nerve Plexus Spinal Nerves Posterior Spinous process of vertebra Posterior root Deep muscles of back Posterior ramus Spinal cord Transverse process of vertebra Posterior root ganglion Spinal nerve Anterior ramus Meningeal branch Communicating rami Anterior root Vertebral body Sympathetic ganglion Anterior General Anatomy of Nerves and Ganglia • Spinal cord communicates with the rest of the body by way of spinal nerves • nerve = a cordlike organ composed of numerous nerve fibers (axons) bound together by connective tissue – mixed nerves contain both afferent (sensory) and efferent (motor) fibers – composed of thousands of fibers carrying currents in opposite directions Anatomy of a Nerve Copyright © The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Epineurium Perineurium Copyright © The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Endoneurium Nerve Rootlets fiber Posterior root Fascicle Posterior root ganglion Anterior Blood root vessels Spinal nerve (b) Copyright by R.G. Kessel and R.H. Kardon, Tissues and Organs: A Text-Atlas of Scanning Electron Microscopy, 1979, W.H. Freeman, All rights reserved Blood vessels Fascicle Epineurium Perineurium Unmyelinated nerve fibers Myelinated nerve fibers (a) Endoneurium Myelin General Anatomy of Nerves and Ganglia • nerves of peripheral nervous system are ensheathed in Schwann cells – forms neurilemma and often a myelin sheath around the axon – external to neurilemma, each fiber is surrounded by -

Compiled for Lower Limb
Updated: December, 9th, 2020 MSI ANATOMY LAB: STRUCTURE LIST Lower Extremity Lower Extremity Osteology Hip bone Tibia • Greater sciatic notch • Medial condyle • Lesser sciatic notch • Lateral condyle • Obturator foramen • Tibial plateau • Acetabulum o Medial tibial plateau o Lunate surface o Lateral tibial plateau o Acetabular notch o Intercondylar eminence • Ischiopubic ramus o Anterior intercondylar area o Posterior intercondylar area Pubic bone (pubis) • Pectineal line • Tibial tuberosity • Pubic tubercle • Medial malleolus • Body • Superior pubic ramus Patella • Inferior pubic ramus Fibula Ischium • Head • Body • Neck • Ramus • Lateral malleolus • Ischial tuberosity • Ischial spine Foot • Calcaneus Ilium o Calcaneal tuberosity • Iliac fossa o Sustentaculum tali (talar shelf) • Anterior superior iliac spine • Anterior inferior iliac spine • Talus o Head • Posterior superior iliac spine o Neck • Posterior inferior iliac spine • Arcuate line • Navicular • Iliac crest • Cuboid • Body • Cuneiforms: medial, intermediate, and lateral Femur • Metatarsals 1-5 • Greater trochanter • Phalanges 1-5 • Lesser trochanter o Proximal • Head o Middle • Neck o Distal • Linea aspera • L • Lateral condyle • L • Intercondylar fossa (notch) • L • Medial condyle • L • Lateral epicondyle • L • Medial epicondyle • L • Adductor tubercle • L • L • L • L • 1 Updated: December, 9th, 2020 Lab 3: Anterior and Medial Thigh Anterior Thigh Medial thigh General Structures Muscles • Fascia lata • Adductor longus m. • Anterior compartment • Adductor brevis m. • Medial compartment • Adductor magnus m. • Great saphenous vein o Adductor hiatus • Femoral sheath o Compartments and contents • Pectineus m. o Femoral canal and ring • Gracilis m. Muscles & Associated Tendons Nerves • Tensor fasciae lata • Obturator nerve • Iliotibial tract (band) • Femoral triangle: Boundaries Vessels o Inguinal ligament • Obturator artery o Sartorius m. • Femoral artery o Adductor longus m. -

M34 M34/1 Latin M34, M34/1
M34 M34/1 M34 M34/1 Latin M34, M34/1 1 Tibia 34 Retinaculum 62 Vagina tendinum musculi 2 Malleolus medialis musculorum fibularium extensoris hallucis longi 3 Talus inferius [Retinaculum 63 A. dorsalis pedis 4 Lig. collaterale mediale musculorum peroneorum 64 M. extensor hallucis brevis [Lig. deltoideum] inferius] 65 N. cutaneus dorsalis 5 Lig. talonaviculare 35 Tendo musculi fibularis medialis 6 Os naviculare longus [Tendo musculi 66 Mm. interossei dorsales 7 Ligg. tarsi dorsalia fibularis longus] 67 Tendines musculi 8 Os metatarsi I 36 Lig. calcaneofibulare extensoris digitorum longi [Os metatarsale I] 37 Tendo calcaneus 68 Tendo musculi extensoris 9 Articualtio 38 Retinaculum musculo- hallucis longi metatarsophalangeae I rum fibularium superius 69 Nn. digitales dorsales pedis 10 Phalanx proximalis I [Retinaculum musculorum 70 Aa. digitales dorsales 11 Phalanx distalis I peroneorum superius] 71 M. abductor digiti minimi 12 Ligg. metatarsalia dorsalia 39 Lig. talocalcaneum 72 Tendines musculi 13 Os cuboideum interosseum extensoris digitorum brevis 14 Lig. bifurcatum 40 Lig. talofibulare posterius 73 Aa. metatarsales dorsales 15 Lig. talofibulare anterius 41 Articulationes metatarsop- 74 A. arcuata 16 Malleolus lateralis halangeae, Ligg. plantaria 75 M. fibularis tertius 17 Lig. tibio-fibulare anterius 42 Basis ossis metatarsi I [M. peroneus tertius] 18 Fibula 43 Ligg. tarsometatarsalia 76 Tendo musculi fibularis 19 Membrana interossea cruris plantaria brevis [Tendo musculi 20 Lig. collaterale mediale 44 Lig. cuboideonaviculare peronei brevis] [Lig. deltoideum], pars plantare 77® A. tarsalis lateralis tibiotalaris anterior 45 Lig. calcaneonaviculare 78 N. cutaneus dorsalis inter- 21 Lig. collaterale mediale plantare medius [Lig. deltoideum], pars 46 Sustentaculum tali 79 Retinaculum musculorum tibiocalcanea 47 Tuber calcanei extensorum superius 22 Lig. -

Lower Extremity Focal Neuropathies
LOWER EXTREMITY FOCAL NEUROPATHIES Lower Extremity Focal Neuropathies Arturo A. Leis, MD S.H. Subramony, MD Vettaikorumakankav Vedanarayanan, MD, MBBS Mark A. Ross, MD AANEM 59th Annual Meeting Orlando, Florida Copyright © September 2012 American Association of Neuromuscular & Electrodiagnostic Medicine 2621 Superior Drive NW Rochester, MN 55901 Printed by Johnson Printing Company, Inc. 1 Please be aware that some of the medical devices or pharmaceuticals discussed in this handout may not be cleared by the FDA or cleared by the FDA for the specific use described by the authors and are “off-label” (i.e., a use not described on the product’s label). “Off-label” devices or pharmaceuticals may be used if, in the judgment of the treating physician, such use is medically indicated to treat a patient’s condition. Information regarding the FDA clearance status of a particular device or pharmaceutical may be obtained by reading the product’s package labeling, by contacting a sales representative or legal counsel of the manufacturer of the device or pharmaceutical, or by contacting the FDA at 1-800-638-2041. 2 LOWER EXTREMITY FOCAL NEUROPATHIES Lower Extremity Focal Neuropathies Table of Contents Course Committees & Course Objectives 4 Faculty 5 Basic and Special Nerve Conduction Studies of the Lower Limbs 7 Arturo A. Leis, MD Common Peroneal Neuropathy and Foot Drop 19 S.H. Subramony, MD Mononeuropathies Affecting Tibial Nerve and its Branches 23 Vettaikorumakankav Vedanarayanan, MD, MBBS Femoral, Obturator, and Lateral Femoral Cutaneous Neuropathies 27 Mark A. Ross, MD CME Questions 33 No one involved in the planning of this CME activity had any relevant financial relationships to disclose. -

A Step Towards Stereotactic Navigation During Pelvic Surgery: 3D Nerve Topography
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Erasmus University Digital Repository Surgical Endoscopy and Other Interventional Techniques https://doi.org/10.1007/s00464-018-6086-3 A step towards stereotactic navigation during pelvic surgery: 3D nerve topography A. R. Wijsmuller1,2 · C. Giraudeau3 · J. Leroy4 · G. J. Kleinrensink5 · E. Rociu6 · L. G. Romagnolo7 · A. G. F. Melani7,8,9 · V. Agnus2 · M. Diana3 · L. Soler3 · B. Dallemagne2 · J. Marescaux2 · D. Mutter2 Received: 10 May 2017 / Accepted: 1 February 2018 © The Author(s) 2018. This article is an open access publication Abstract Background Long-term morbidity after multimodal treatment for rectal cancer is suggested to be mainly made up by nerve- injury-related dysfunctions. Stereotactic navigation for rectal surgery was shown to be feasible and will be facilitated by highlighting structures at risk of iatrogenic damage. The aim of this study was to investigate the ability to make a 3D map of the pelvic nerves with magnetic resonance imaging (MRI). Methods A systematic review was performed to identify a main positional reference for each pelvic nerve and plexus. The nerves were manually delineated in 20 volunteers who were scanned with a 3-T MRI. The nerve identifiability rate and the likelihood of nerve identification correctness were determined. Results The analysis included 61 studies on pelvic nerve anatomy. A main positional reference was defined for each nerve. On MRI, the sacral nerves, the lumbosacral plexus, and the obturator nerve could be identified bilaterally in all volunteers. The sympathetic trunk could be identified in 19 of 20 volunteers bilaterally (95%). -

35. Lumbar Plexus. Sacral Plexus. Coccygeal Plexus
GUIDELINES Students’ independent work during preparation to practical lesson Academic discipline HUMAN ANATOMY Topic LUMBAR PLEXUS. SACRAL PLEXUS. COCCYGEAL PLEXUS 1. Relevance of the topic Lumbar, sacral and coccygeal plexuses innervate the skin of the abdomen, lower back and lower extremities and all the muscles of the lower limbs. Acquired knowledge is the basis for many fields of practical medicine, such as neurology, surgery and traumatology. 2. Specific objectives After the lesson the student should know and be able to: - describe the sources of the formation of the lumbar plexus; - classify the nerves of the lumbar plexus; - to be able to demonstrate and define the branches of the lumbar plexus; - describe sources of sacral plexus formation; - classify sacral plexus nerves; - be able to demonstrate and identify short and long branches of the sacral plexus; - describe the sources of formation coccygeal plexus; - classify coccygeal plexus nerves; - be able to demonstrate and identify branches of coccygeal plexus; - to explain the innervation of muscles and skin in the areas of the lower back and lower extremity. 3. Basic level of preparation For practical this lesson a student should know and be able: - to know the anatomy of the spine, pelvis, lower extremities; - to analyze and show large and small pelvis, their bones; - to analyze and demonstrate bones and joints of the lower limbs; - to demonstrate muscles of the abdomen, perineum, pelvic girdle and lower limbs; - to know the anatomy (external and internal structure) of the spinal cord; - to know the spinal nerve anatomy. 4. Tasks for independent work during preparation for the classes 4.1. -

Management of Metastatic Tumors Invading the Peripheral Nervous System
Neurosurg Focus 22 (6):E14, 2007 Management of metastatic tumors invading the peripheral nervous system JOHN GACHIANI, M.D.,1 DANIEL H. KIM, M.D.,3 ADRIANE NELSON, M.D.,2 AND DAVID KLINE, M.D.1 Departments of 1Neurosurgery and 2Pathology, Louisiana State University Health Sciences Center; 3Department of Neurosurgery, Ochsner Clinic Foundation, New Orleans, Louisiana Object. The authors present the results of a retrospective review of 37 surgically treated metastases to nerve (malignant peripheral non–neural sheath nerve tumors). Tumor frequencies, presentations, management, and prognosis are discussed. Methods. Thirty-seven patients who were treated for metastases to nerve between 1969 and 2006 at the Louisiana State University Health Sciences Center were identified in a review of patient records. Notes regarding patient history and physical examination findings were reviewed to provide informa- tion on presenting symptoms and signs. Imaging and histopathological examination results were also reviewed. Cases were analyzed depending on the primary tumor and the location of metastasis. Results. There included 37 surgically treated lesions, 16 of which originated in the breast and 10 of which originated in the lung. In two cases melanomas had metastasized to nerve, and one tumor each had metastasized from the bladder, rectum, skin, head and neck, and thyroid, and from a primary Ewing sarcoma. There was a single lymphoma that had metastasized to the radial nerve and one chor- doma and one osteosarcoma, each of which had metastasized to the brachial plexus. Conclusions. The nervous system is involved in numerous ways by oncological process. Direct involvement of the peripheral nervous system occurs mostly from direct extension, although it occa- sionally occurs because of distant spread from the primary tumor to nerve. -
Spinal Nerves and Reflexes
Central Nervous System - Spinal Nerves and Reflexes Chapter 13B Spinal Nerves - Number There are 31 pairs of spinal nerves…a total of 62 nerves. Spinal cord is located in the vertebral canal. Spinal nerves exit vertebral column through intervertebral foramina. Intervertebral foramen Vertebral canal Spinal Nerves Interneuron Sensory neuron Sensory fiber Spinal nerve Motor neuron Motor fiber All spinal nerves are mixed nerves….contain sensory and motor fibers. Spinal Nerves - Supply N V C2–C3 C2 C 3 C3 C4 Spinal nerves go to skin, muscles and some T2 C4 C5 T3 T1 of the internal organs. T4 T2 T5 C5 T3 T T 6 4 T7 T5 T8 Dermatomes: areas of the skin that is T2 T6 T9 T T2 T7 10 connected to a specific spinal nerve. T11 T8 T12 T9 C L1 6 T10 L2 T T L3 1 11 L4 C Myotomes: specific muscles that are C6 L 7 T12 5 L1 supplied by a specific spinal nerve. S4S L 3 2 S2 C8 C8 T L3 L1 1 1 S5 C7 S1 L5 L4 S2 L2 KEY L5 L Spinal cord regions 3 = Cervical = Thoracic S = Lumbar 1 = Sacral L4 ANTERIOR POSTERIOR Spinal Nerves - Branches Spinal nerve Dorsal Dorsal root Dorsal root ganglion ramus Spinal nerve Ventral Dorsal horn ramus Ventral Ventral root horn Rami communicantes After exiting vertebral column, EACH spinal nerve splits into branches, called rami: 1. Dorsal ramus: contains nerves that serve the dorsal portions of the trunk- carry visceral motor, somatic motor, and sensory information to and from the skin and muscles of the back. -

Tibial Nerve Block: Supramalleolar Or Retromalleolar Approach? a Randomized Trial in 110 Participants
International Journal of Environmental Research and Public Health Article Tibial Nerve Block: Supramalleolar or Retromalleolar Approach? A Randomized Trial in 110 Participants María Benimeli-Fenollar 1,* , José M. Montiel-Company 2 , José M. Almerich-Silla 2 , Rosa Cibrián 3 and Cecili Macián-Romero 1 1 Department of Nursing, University of Valencia, c/Jaume Roig s/n, 46010 Valencia, Spain; [email protected] 2 Department of Stomatology, University of Valencia, c/Gascó Oliag, 1, 46010 Valencia, Spain; [email protected] (J.M.M.-C.); [email protected] (J.M.A.-S.) 3 Department of Physiology, University of Valencia, c/Blasco Ibánez, 15, 46010 Valencia, Spain; [email protected] * Correspondence: [email protected] Received: 26 April 2020; Accepted: 23 May 2020; Published: 29 May 2020 Abstract: Of the five nerves that innervate the foot, the one in which anesthetic blocking presents the greatest difficulty is the tibial nerve. The aim of this clinical trial was to establish a protocol for two tibial nerve block anesthetic techniques to later compare the anesthetic efficiency of retromalleolar blocking and supramalleolar blocking in order to ascertain whether the supramalleolar approach achieved a higher effective blocking rate. A total of 110 tibial nerve blocks were performed. Location of the injection site was based on a prior ultrasound assessment of the tibial nerve. The block administered was 3 mL of 2% mepivacaine. The two anesthetic techniques under study provided very similar clinical results. The tibial nerve success rate was 81.8% for the retromalleolar technique and 78.2% for the supramalleolar technique.