Upper Extremity Compression Neuropathies
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Dental Plexopathy Vesta Guzeviciene, Ricardas Kubilius, Gintautas Sabalys
SCIENTIFIC ARTICLES Stomatologija, Baltic Dental and Maxillofacial Journal, 5:44-47, 2003 Dental Plexopathy Vesta Guzeviciene, Ricardas Kubilius, Gintautas Sabalys SUMMARY Aim and purpose of the study were: 1) to study and compare unfavorable factors playing role in the development of upper teeth plexitis and upper teeth plexopathy; 2) to study peculiarities of clinical manifestation of upper teeth plexitis and upper teeth plexopathy, and to establish their diagnostic value; 3) to optimize the treatment. The results of examination and treatment of 79 patients with upper teeth plexitis (UTP-is) and 63 patients with upper teeth plexopathy (UTP-ty) are described in the article. Questions of the etiology, pathogenesis and differential diagnosis are discussed, methods of complex medicamental and surgical treatment are presented. Keywords: atypical facial neuralgia, atypical odontalgia, atypical facial pain, vascular toothache. PREFACE Besides the common clinical tests, in order to ana- lyze in detail the etiology and pathogenesis of the afore- Usually the injury of the trigeminal nerve is re- mentioned disease, its clinical manifestation and pecu- lated to the pathology of the teeth neural plexuses. liarities, we performed specific examinations such as According to the literature data, injury of the upper orthopantomography of the infraorbital canals, mea- teeth neural plexuses makes more than 7% of all sured the velocity of blood flow in the infraorbital blood neurostomatologic diseases. Many terms are used in vessels (doplerography), examined the pain threshold literature to characterize the clinical symptoms com- of facial skin and oral mucous membrane in acute pe- plex of the above-mentioned pathology. Some authors riod and remission, and evaluated the role that the state (1, 2, 3) named it dental plexalgia or dental plexitis. -

Brachial-Plexopathy.Pdf
Brachial Plexopathy, an overview Learning Objectives: The brachial plexus is the network of nerves that originate from cervical and upper thoracic nerve roots and eventually terminate as the named nerves that innervate the muscles and skin of the arm. Brachial plexopathies are not common in most practices, but a detailed knowledge of this plexus is important for distinguishing between brachial plexopathies, radiculopathies and mononeuropathies. It is impossible to write a paper on brachial plexopathies without addressing cervical radiculopathies and root avulsions as well. In this paper will review brachial plexus anatomy, clinical features of brachial plexopathies, differential diagnosis, specific nerve conduction techniques, appropriate protocols and case studies. The reader will gain insight to this uncommon nerve problem as well as the importance of the nerve conduction studies used to confirm the diagnosis of plexopathies. Anatomy of the Brachial Plexus: To assess the brachial plexus by localizing the lesion at the correct level, as well as the severity of the injury requires knowledge of the anatomy. An injury involves any condition that impairs the function of the brachial plexus. The plexus is derived of five roots, three trunks, two divisions, three cords, and five branches/nerves. Spinal roots join to form the spinal nerve. There are dorsal and ventral roots that emerge and carry motor and sensory fibers. Motor (efferent) carries messages from the brain and spinal cord to the peripheral nerves. This Dorsal Root Sensory (afferent) carries messages from the peripheral to the Ganglion is why spinal cord or both. A small ganglion containing cell bodies of sensory NCS’s sensory fibers lies on each posterior root. -

Ultrasound of Radial, Ulnar, and Median Nerves
Ultrasound of Radial, Ulnar, Disclosures • Consultant: Bioclinica and Median Nerves • Contractor: POCUS PRO • Advisory Board: Philips Jon A. Jacobson, M.D. • Book Royalties: Elsevier • Not relevant to this lecture Professor of Radiology See www.jacobsonmskus.com for syllabus other educational material Nerve Compression Nerve Entrapment • Experimental model (rat, sciatic nv): • US findings: – Compression causes ischemia – Nerve enlargement proximal to entrapment – First pathologic change: edema • Best appreciated transverse to nerve • Correlated with severity of axonal injury – Abnormally hypoechoic – Mild compression: demyelination • Especially the connective tissue layers – Severe compression: axonal damage – Variable enlargement or flattening at entrapment site Powell, Laboratory Investigation 1986; 55:91 Atrophy Denervation Nerve Entrapment Syndromes • Edema: hyperechoic • Fatty degeneration: • Median: – Hyperechoic – Carpal tunnel syndrome – Echogenic interfaces – Pronator teres syndrome • Atrophy: Asymptomatic – Hyperechoic with • Ulnar: decreased muscle size – Ulnar tunnel syndrome • Compare to other side! – Cubital tunnel syndrome J Ultrasound Med 1993; 2:73 Extensor Muscles: leg 1 Volar Wrist Normal Peripheral Nerve • Ultrasound appearance: – Hypoechoic nerve fascicles – Hyperechoic connective tissue • Transverse: – Honeycomb appearance Silvestri et al. Radiology 1995; 197:291 Median Nerve From: Netter’s Atlas of Human Anatomy Volar Wrist: median nerve & flexors Peripheral Nerves • More coarse compared to tendon T – Fascicular -

Piriformis Syndrome Is Overdiagnosed 11 Robert A
American Association of Neuromuscular & Electrodiagnostic Medicine AANEM CROSSFIRE: CONTROVERSIES IN NEUROMUSCULAR AND ELECTRODIAGNOSTIC MEDICINE Loren M. Fishman, MD, B.Phil Robert A.Werner, MD, MS Scott J. Primack, DO Willam S. Pease, MD Ernest W. Johnson, MD Lawrence R. Robinson, MD 2005 AANEM COURSE F AANEM 52ND Annual Scientific Meeting Monterey, California CROSSFIRE: Controversies in Neuromuscular and Electrodiagnostic Medicine Loren M. Fishman, MD, B.Phil Robert A.Werner, MD, MS Scott J. Primack, DO Willam S. Pease, MD Ernest W. Johnson, MD Lawrence R. Robinson, MD 2005 COURSE F AANEM 52nd Annual Scientific Meeting Monterey, California AANEM Copyright © September 2005 American Association of Neuromuscular & Electrodiagnostic Medicine 421 First Avenue SW, Suite 300 East Rochester, MN 55902 PRINTED BY JOHNSON PRINTING COMPANY, INC. ii CROSSFIRE: Controversies in Neuromuscular and Electrodiagnostic Medicine Faculty Loren M. Fishman, MD, B.Phil Scott J. Primack, DO Assistant Clinical Professor Co-director Department of Physical Medicine and Rehabilitation Colorado Rehabilitation and Occupational Medicine Columbia College of Physicians and Surgeons Denver, Colorado New York City, New York Dr. Primack completed his residency at the Rehabilitation Institute of Dr. Fishman is a specialist in low back pain and sciatica, electrodiagnosis, Chicago in 1992. He then spent 6 months with Dr. Larry Mack at the functional assessment, and cognitive rehabilitation. Over the last 20 years, University of Washington. Dr. Mack, in conjunction with the Shoulder he has lectured frequently and contributed over 55 publications. His most and Elbow Service at the University of Washington, performed some of the recent work, Relief is in the Stretch: End Back Pain Through Yoga, and the original research utilizing musculoskeletal ultrasound in order to diagnose earlier book, Back Talk, both written with Carol Ardman, were published shoulder pathology. -

Identification and Surgical Management of Upper Arm and Forearm Compartment Syndrome
Open Access Case Report DOI: 10.7759/cureus.5862 Identification and Surgical Management of Upper Arm and Forearm Compartment Syndrome Adel Hanandeh 1 , Vishnu R. Mani 2 , Paul Bauer 1 , Alexius Ramcharan 3 , Brian Donaldson 1 1. General Surgery, Columbia University College of Physicians and Surgeons at Harlem Hospital Center, New York, USA 2. Surgery, Columbia University College of Physicians and Surgeons at Harlem Hospital Center, New York, USA 3. Surgery, Harlem Hospital Center, New York, USA Corresponding author: Adel Hanandeh, [email protected] Abstract Extremity muscles are grouped and divided by strong fascial membranes into compartments. Multiple pathological processes can result in an increase in the pressure within a muscle compartment. An increase in the compartment pressure beyond the adequate perfusion pressure has the potential to cause extremity compartment syndrome. There are multiple sites where compartment syndrome can occur. In this article, an arm and forearm compartment syndrome ensued secondary to a minor crushing injury that lead to supracondylar and medial epicondylar non-displaced fractures. A pure motor radial and ulnar nerve deficits noted on presentation, worsened with progression of the compartment syndrome. Ultimately, a surgical fasciotomy was carried out to release all compartments of the right upper arm and forearm. Categories: General Surgery, Orthopedics, Anatomy Keywords: upper arm compartment syndrome, fasciotomy, forearm compartment syndrome, condylar fracture, pediatric supracondylar humerus fracture Introduction In 1872, the first description of compartment syndrome was published by Richard von Volkmann. His publication described an irreversible contracture of muscles due to ischemic process resulting in the first documented nerve injury and contracture from compartment syndrome. -

Exposure of the Forearm and Distal Radius
Exposure of the Forearm and Distal Radius Melissa A. Klausmeyer, MDa, Chaitanya Mudgal, MDb,* KEYWORDS Henry approach Thompson approach Flexor carpi radialis approach Dorsal distal radius approach Distal radius approach KEY POINTS The use of internervous planes allow access to the underlying bone without risk of denervating the overlying muscles. The choice of approach is based on the injury pattern and need for exposure. The Henry and Thompson approaches are useful for radial shaft fractures. The distal radius can be approached volarly through the flexor carpi radialis (FCR) approach or dorsally through the extended Thompson approach. The extended FCR approach is useful for intraarticular fractures of the distal radius as well as mal- unions and subacute fractures. INTRODUCTION ANATOMY OF THE FOREARM Muscles Safe operative approaches to the bones of the forearm and wrist include the use of internervous The muscles of the forearm are split into 4 compart- planes. These planes lie between muscles that ments: The superficial volar, the deep volar, the are innervated by different nerves. By utilizing extensor, and the mobile wad (Table 1). The median these planes for dissection, extensive mobilization nerve supplies all of the volar muscles of the forearm of muscles and therefore large areas of exposure except the ulnar half of the flexor digitorum profun- may be obtained without the risk of muscle dus and the flexor carpi ulnaris that are supplied denervation. by the ulnar nerve. The radial nerve proper supplies A successful operative plan also must include the brachioradialis and extensor carpi radialis lon- consideration of the soft tissues, particularly gus. -

Sensory Conduction in Medial and Lateral Plantar Nerves
J Neurol Neurosurg Psychiatry: first published as 10.1136/jnnp.51.2.188 on 1 February 1988. Downloaded from Journal ofNeurology, Neurosurgery, and Psychiatry 1988;51:188-191 Sensory conduction in medial and lateral plantar nerves S N PONSFORD From the Department of Clinical Neurophysiology, Walsgrave Hospital, Coventry, UK SUMMARY A simple and reliable method of recording medial and lateral plantar nerve sensory action potentials is described. Potentials are recorded with surface electrodes at the ankle using surface electrodes stimulating orthodromically at the sole. The normal values obtained are higher in amplitude than those obtained by the method described by Guiloff and Sherratt and are detectable in older subjects aged over 80 years. The procedure is valuable in the diagnosis of early peripheral neuropathy, mononeuritig multiplex; tarsal tunnel syndrome and in differentiation between pre and post ganglionic L5 SI lesions. The value of medial plantar sensory action potential EL53051 applied to the sole just lateral to the first meta-guest. Protected by copyright. (SAP) recording in the diagnosis of peripheral neuro- tarsal, the anode level with metatarsophalangeal joint, the pathy and investigation of root or individual nerve cathode thus overlying the first common digital nerve sub- lesions involving the leg or foot was clearly estab- serving contiguous surfaces ofthe great and second toes. For the lateral plantar, the stimulator was placed between the lished by Guiloff and Sherratt.1 However, their fourth and fifth metatarsals, the anode-again level with the method of stimulating at the big toe and recording at metatarsophalangeal joint, overlying the fourth common the ankle gives potentials of relatively small ampli- digital nerve supplying contiguous surfaces of the fourth and tude (mean amplitude 2-3 pv, range 0-8- 1). -

Ultrasound of Peripheral Nerve and Muscle
ULTRASOUND OF PERIPHERAL NERVE AND MUSCLE Steven Shook, MD Cleveland Clinic Cleveland, OH INTRODUCTION Advances in field of ultrasound over the past twenty years have generated increasing interest in utilizing the technology in neuromuscular assessment and diagnosis. High-resolution ultrasound offers a noninvasive, real- time, static and dynamic examination of the peripheral nervous system, yielding information which complements the neurological examination, electrodiagnostic testing (EDX), and other established imaging modalities such as Magnetic Resonance Imaging (MRI). ULTRASOUND BASICS Ultrasonography involves transmitting sound-wave pulses into tissue and analyzing the temporal and acoustic properties of the reflected wave, or echo. Echoes occur at tissue interfaces. Reflected energy is a product of the difference in adjacent tissue densities (acoustic impedance), as well the angle of the ultrasound beam (angle of incidence) relative to the interface.(1) A fraction of a transmitted sound-wave energy is reflected whenever there is a change in acoustic impedance within tissue. Larger differences in acoustic impedance result in more profound reflection. Unreflected sound travels deeper into the tissue, generating echos from layers at a greater depth. A portion of the ultrasound energy never returns to the transducer, either being transformed into heat (absorption), refracted or scattered at nonperpendicular tissue interfaces. When the sound wave encounters a significantly different tissue density, analysis of deeper structures is not possible. For example, ultrasound cannot evaluate structures deep to air- filled cavities or bone due to the acoustic impedance of these regions.(2) An ultrasound probe (transducer) is capable of both emitting and receiving these pulses and converting them into electrical signals for analysis. -

Risk of Encountering Dorsal Scapular and Long Thoracic Nerves During Ultrasound-Guided Interscalene Brachial Plexus Block with Nerve Stimulator
Korean J Pain 2016 July; Vol. 29, No. 3: 179-184 pISSN 2005-9159 eISSN 2093-0569 http://dx.doi.org/10.3344/kjp.2016.29.3.179 | Original Article | Risk of Encountering Dorsal Scapular and Long Thoracic Nerves during Ultrasound-guided Interscalene Brachial Plexus Block with Nerve Stimulator Department of Anesthesiology and Pain Medicine, Wonkwang University College of Medicine, Wonkwang Institute of Science, Iksan, *Department of Anesthesiology and Pain Medicine, Presbyterian Medical Center, University of Seonam College of Medicine, Jeonju, Korea Yeon Dong Kim, Jae Yong Yu*, Junho Shim*, Hyun Joo Heo*, and Hyungtae Kim* Background: Recently, ultrasound has been commonly used. Ultrasound-guided interscalene brachial plexus block (IBPB) by posterior approach is more commonly used because anterior approach has been reported to have the risk of phrenic nerve injury. However, posterior approach also has the risk of causing nerve injury because there are risks of encountering dorsal scapular nerve (DSN) and long thoracic nerve (LTN). Therefore, the aim of this study was to evaluate the risk of encountering DSN and LTN during ultrasound-guided IBPB by posterior approach. Methods: A total of 70 patients who were scheduled for shoulder surgery were enrolled in this study. After deciding insertion site with ultrasound, awake ultrasound-guided IBPB with nerve stimulator by posterior approach was performed. Incidence of muscle twitches (rhomboids, levator scapulae, and serratus anterior muscles) and current intensity immediately before muscle twitches disappeared were recorded. Results: Of the total 70 cases, DSN was encountered in 44 cases (62.8%) and LTN was encountered in 15 cases (21.4%). Both nerves were encountered in 10 cases (14.3%). -

The Branching and Innervation Pattern of the Radial Nerve in the Forearm: Clarifying the Literature and Understanding Variations and Their Clinical Implications
diagnostics Article The Branching and Innervation Pattern of the Radial Nerve in the Forearm: Clarifying the Literature and Understanding Variations and Their Clinical Implications F. Kip Sawyer 1,2,* , Joshua J. Stefanik 3 and Rebecca S. Lufler 1 1 Department of Medical Education, Tufts University School of Medicine, Boston, MA 02111, USA; rebecca.lufl[email protected] 2 Department of Anesthesiology, Stanford University School of Medicine, Stanford, CA 94305, USA 3 Department of Physical Therapy, Movement and Rehabilitation Science, Bouve College of Health Sciences, Northeastern University, Boston, MA 02115, USA; [email protected] * Correspondence: [email protected] Received: 20 May 2020; Accepted: 29 May 2020; Published: 2 June 2020 Abstract: Background: This study attempted to clarify the innervation pattern of the muscles of the distal arm and posterior forearm through cadaveric dissection. Methods: Thirty-five cadavers were dissected to expose the radial nerve in the forearm. Each muscular branch of the nerve was identified and their length and distance along the nerve were recorded. These values were used to determine the typical branching and motor entry orders. Results: The typical branching order was brachialis, brachioradialis, extensor carpi radialis longus, extensor carpi radialis brevis, supinator, extensor digitorum, extensor carpi ulnaris, abductor pollicis longus, extensor digiti minimi, extensor pollicis brevis, extensor pollicis longus and extensor indicis. Notably, the radial nerve often innervated brachialis (60%), and its superficial branch often innervated extensor carpi radialis brevis (25.7%). Conclusions: The radial nerve exhibits significant variability in the posterior forearm. However, there is enough consistency to identify an archetypal pattern and order of innervation. These findings may also need to be considered when planning surgical approaches to the distal arm, elbow and proximal forearm to prevent an undue loss of motor function. -
Neurology of the Upper Limb
Neurology of the Upper limb Donald Sammut Hand Surgeon Kings Upper Limb Anatomy plus lecture notes The$Neck$ The$Nerve$roots$which$supply$the$Upper$Limb$are$C5$to$T1$ Pre<fixed$(C4$to$C8)$and$Post<fixed$(C6$to$T2)$plexus$not$uncommon.$ Also$common$contributions$from$C4$and$from$T2$in$a$normally$rooted$plexus.$ $ The$anterior$nerve$roots$emerge$between$the$vertebrae$and$immediately$pass$ $through$the$first$area$of$possible$compression:$ The$root$nerve$canal$is$bounded$$ Anteriorly$by$the$posterior$margin$of$the$intervertebral$disc$and$$ Posteriorly,$by$the$facet$joint$between$vertebrae.$ $ Pathology$of$the$disc,$or$joint,$or$both,$can$narrow$this$channel$and$compress$ $the$nerve$root$ The$roots$emerge$from$the$cervical$spine$into$the$plane$between$$ Scalenius$Anterior$and$Scalenius$Medius.$$ $ Scalenius*Anterior:** Origin:$Anterior$tubercles$of$Cervical$vertebae$C3$to$6$(C6$tubercle$is$the$Carotid$tubercle)$ Insertion:$The$scalene$tubercle$on$inner$border/upper$surface$1st$rib$ $ Scalenius*Medius:* Origin:$Posterior$tubercles$of$all$cervical$vertebrae$ Insertion:$Quadrangular$area$between$the$neck$and$subclavian$groove$1st$rib$ $ Exiting$from$the$Scalenes,$the$trunks$lie$in$the$posterior$triangle$of$the$neck.$ The$posterior$triangle$is$bounded$anteriorly$by$SternoCleidoMastoid$and$$ posteriorly$by$the$Trapezius.$ The$inferior$border$is$the$clavicle$.$ The$apex$of$the$triangle$superiorly$is$at$the$back$of$the$skull$on$the$superior$nuchal$line$ $ $ The$Posterior$Triangle$ SternoCleidoMastoid$ Trapezius$ Scalenius$Medius$ Scalenius$Anterior$ -
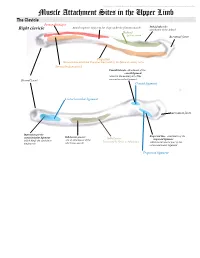
Muscle Attachment Sites in the Upper Limb
This document was created by Alex Yartsev ([email protected]); if I have used your data or images and forgot to reference you, please email me. Muscle Attachment Sites in the Upper Limb The Clavicle Pectoralis major Smooth superior surface of the shaft, under the platysma muscle Deltoid tubercle: Right clavicle attachment of the deltoid Deltoid Axillary nerve Acromial facet Trapezius Sternocleidomastoid and Trapezius innervated by the Spinal Accessory nerve Sternocleidomastoid Conoid tubercle, attachment of the conoid ligament which is the medial part of the Sternal facet coracoclavicular ligament Conoid ligament Costoclavicular ligament Acromial facet Impression for the Trapezoid line, attachment of the costoclavicular ligament Subclavian groove: Subclavius trapezoid ligament which binds the clavicle to site of attachment of the Innervated by Nerve to Subclavius which is the lateral part of the the first rib subclavius muscle coracoclavicular ligament Trapezoid ligament This document was created by Alex Yartsev ([email protected]); if I have used your data or images and forgot to reference you, please email me. The Scapula Trapezius Right scapula: posterior Levator scapulae Supraspinatus Deltoid Deltoid and Teres Minor are innervated by the Axillary nerve Rhomboid minor Levator Scapulae, Rhomboid minor and Rhomboid Major are innervated by the Dorsal Scapular Nerve Supraspinatus and Infraspinatus innervated by the Suprascapular nerve Infraspinatus Long head of triceps Rhomboid major Teres Minor Teres Major Teres Major