Autonomic Nervous System
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Variations of Thoracic Splanchnic Nerves and Its Clinical Implications
Int. J. Morphol., 23(3):247-251, 2005. Variations of Thoracic Splanchnic Nerves and its Clinical Implications Variaciones de los Nervios Esplácnicos Torácicos y sus Implicancias Clínicas *Tony George Jacob; ** Surbhi Wadhwa; ***Shipra Paul & ****Srijit Das JACOB, G. T.; WADHWA, S.; PAUL, S. & DAS, S. Variations of thoracic splanchnic nerves and its clinical implications. Int. J. Morphol., 23(3):247-251, 2005. SUMMARY:The present study reports an anomalous branching pattern of the thoracic sympathetic chain. At the level of T3 ganglion, an anomalous branch i.e accessory sympathetic chain (ASC) descended anteromedial to the main sympathetic chain (MSC). The MSC and the ASC communicated with each other at the level of T9, T10 and T11 ganglion, indicating the absence of classical pattern of greater, lesser and least splanchnic nerves on the right side. However, on the left side, the sympathetic chain displayed normal branching pattern. We opine that the ASC may be representing a higher origin of greater splanchnic nerve at the level of T3 ganglion and the branches from MSC at T9, T10 and T11 ganglion may be the lesser and least splanchnic nerves, which further joined the ASC (i.e presumably the greater splanchnic nerve) to form a common trunk. This common trunk pierced the right crus of diaphragm to reach the right suprarenal plexus after giving few branches to the celiac plexus. Awareness and knowledge of such anatomical variants of thoracic sympathetic chain may be helpful to surgeons in avoiding any incomplete denervation or preventing any inadvertent injury during thoracic sympathectomy. KEY WORDS: Splanchnic nerves; Sympathetic chain; Trunk thoracic; Ganglion. -

The Baseline Structure of the Enteric Nervous System and Its Role in Parkinson’S Disease
life Review The Baseline Structure of the Enteric Nervous System and Its Role in Parkinson’s Disease Gianfranco Natale 1,2,* , Larisa Ryskalin 1 , Gabriele Morucci 1 , Gloria Lazzeri 1, Alessandro Frati 3,4 and Francesco Fornai 1,4 1 Department of Translational Research and New Technologies in Medicine and Surgery, University of Pisa, 56126 Pisa, Italy; [email protected] (L.R.); [email protected] (G.M.); [email protected] (G.L.); [email protected] (F.F.) 2 Museum of Human Anatomy “Filippo Civinini”, University of Pisa, 56126 Pisa, Italy 3 Neurosurgery Division, Human Neurosciences Department, Sapienza University of Rome, 00135 Rome, Italy; [email protected] 4 Istituto di Ricovero e Cura a Carattere Scientifico (I.R.C.C.S.) Neuromed, 86077 Pozzilli, Italy * Correspondence: [email protected] Abstract: The gastrointestinal (GI) tract is provided with a peculiar nervous network, known as the enteric nervous system (ENS), which is dedicated to the fine control of digestive functions. This forms a complex network, which includes several types of neurons, as well as glial cells. Despite extensive studies, a comprehensive classification of these neurons is still lacking. The complexity of ENS is magnified by a multiple control of the central nervous system, and bidirectional communication between various central nervous areas and the gut occurs. This lends substance to the complexity of the microbiota–gut–brain axis, which represents the network governing homeostasis through nervous, endocrine, immune, and metabolic pathways. The present manuscript is dedicated to Citation: Natale, G.; Ryskalin, L.; identifying various neuronal cytotypes belonging to ENS in baseline conditions. -

Anatomical Planes in Rectal Cancer Surgery
DOI: 10.4274/tjcd.galenos.2019.2019-10-2 Turk J Colorectal Dis 2019;29:165-170 REVIEW Anatomical Planes in Rectal Cancer Surgery Rektum Kanser Cerrahisinde Anatomik Planlar Halil İbrahim Açar, Mehmet Ayhan Kuzu Ankara University Faculty of Medicine, Department of General Surgery, Ankara, Turkey ABSTRACT This review outlines important anatomical landmarks not only for rectal cancer surgery but also for pelvic exentration. Keywords: Anorectal anatomy, pelvic anatomy, surgical anatomy of rectum ÖZ Pelvis anatomisini derleme halinde özetleyen bu makale rektum kanser cerrahisi ve pelvik ezantrasyon için önemli topografik noktaları gözden geçirmektedir. Anahtar Kelimeler: Anorektal anatomi, pelvik anatomi, rektumun cerrahi anatomisi Introduction Surgical Anatomy of the Rectum The rectum extends from the promontory to the anal canal Pelvic Anatomy and is approximately 12-15 cm long. It fills the sacral It is essential to know the pelvic anatomy because of the concavity and ends with an anal canal 2-3 cm anteroinferior intestinal and urogenital complications that may develop to the tip of the coccyx. The rectum contains three folds in after the surgical procedures applied to the pelvic region. the coronal plane laterally. The upper and lower are convex The pelvis, encircled by bone tissue, is surrounded by the to the right, and the middle is convex to the left. The middle main vessels, ureters, and autonomic nerves. Success in the fold is aligned with the peritoneal reflection. Intraluminal surgical treatment of pelvic organs is only possible with a projections of the lower boundaries of these folds are known as Houston’s valves. Unlike the sigmoid colon, taenia, good knowledge of the embryological development of the epiploic appendices, and haustra are absent in the rectum. -

Autonomic Nerve Activity and Cardiac Arrhythmias
ACORP Complete (with appendices) Last Name of PI► Protocol No. Assigned by the IACUC►02002 Official Date of Approval► 1. Caging needs. Complete the table below to describe the housing that will have to be accommodated by the housing sites for this protocol: d. Is this housing e. Estimated c. Number of consistent with the maximum number a. Species b. Type of housing* individuals per Guide and USDA of housing units housing unit** regulations? needed at any one (yes/no***) time Chain link run, 3x6 Canines 1 no 7 and 4x10 feet cage *See ACORP Instructions, for guidance on describing the type of housing needed. If animals are to be housed according to a local Standard Operating Procedure (SOP), enter “standard (see SOP)” here, and enter the SOP into the table in Item Y. If the local standard housing is not described in a SOP, enter “standard, see below” in the table and describe the standard housing here: Chain link run, 3x6 feet cages ** The Guide states that social animals should generally be housed in stable pairs or groups. Provide a justification if any animals will be housed singly (if species is not considered “social”, then so note) Dogs are housed singly in chain link runs but can socialize with one another since each room has two to five dog runs. In addition, while their runs are being cleaned on a daily basis, pairs of dogs are allowed to exercise and play together in a designated "romper room". Animals are fitted with DSI transmitters and need to be housed singly in a cage for which DSI receivers are installed to receive signals from the transmitters. -

Clinical Presentations of Lumbar Disc Degeneration and Lumbosacral Nerve Lesions
Hindawi International Journal of Rheumatology Volume 2020, Article ID 2919625, 13 pages https://doi.org/10.1155/2020/2919625 Review Article Clinical Presentations of Lumbar Disc Degeneration and Lumbosacral Nerve Lesions Worku Abie Liyew Biomedical Science Department, School of Medicine, Debre Markos University, Debre Markos, Ethiopia Correspondence should be addressed to Worku Abie Liyew; [email protected] Received 25 April 2020; Revised 26 June 2020; Accepted 13 July 2020; Published 29 August 2020 Academic Editor: Bruce M. Rothschild Copyright © 2020 Worku Abie Liyew. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Lumbar disc degeneration is defined as the wear and tear of lumbar intervertebral disc, and it is mainly occurring at L3-L4 and L4-S1 vertebrae. Lumbar disc degeneration may lead to disc bulging, osteophytes, loss of disc space, and compression and irritation of the adjacent nerve root. Clinical presentations associated with lumbar disc degeneration and lumbosacral nerve lesion are discogenic pain, radical pain, muscular weakness, and cutaneous. Discogenic pain is usually felt in the lumbar region, or sometimes, it may feel in the buttocks, down to the upper thighs, and it is typically presented with sudden forced flexion and/or rotational moment. Radical pain, muscular weakness, and sensory defects associated with lumbosacral nerve lesions are distributed on -

Of the Pediatric Mediastinum
MRI of the Pediatric Mediastinum Dianna M. E. Bardo, MD Director of Body MR & Co-Director of the 3D Innovation Lab Disclosures Consultant & Speakers Bureau – honoraria Koninklijke Philips Healthcare N V Author – royalties Thieme Publishing Springer Publishing Mediastinum - Anatomy Superior Mediastinum thoracic inlet to thoracic plane thoracic plane to diaphragm Inferior Mediastinum lateral – pleural surface anterior – sternum posterior – vertebral bodies Mediastinum - Anatomy Anterior T4 Mediastinum pericardium to sternum Middle Mediastinum pericardial sac Posterior Mediastinum vertebral bodies to pericardium lateral – pleural surface superior – thoracic inlet inferior - diaphragm Mediastinum – MR Challenges Motion Cardiac ECG – gating/triggering Breathing Respiratory navigation Artifacts Intubation – LMA Surgical / Interventional materials Mediastinum – MR Sequences ECG gated/triggered sequences SSFP – black blood SE – IR – GRE Non- ECG gated/triggered sequences mDIXON (W, F, IP, OP), eTHRIVE, turbo SE, STIR, DWI Respiratory – triggered, radially acquired T2W MultiVane, BLADE, PROPELLER Mediastinum – MR Sequences MRA / MRV REACT – non Gd enhanced Gd enhanced sequences THRIVE, mDIXON, mDIXON XD Mediastinum – Contents Superior Mediastinum PVT Left BATTLE: Phrenic nerve Vagus nerve Structures at the level of the sternal angle Thoracic duct Left recurrent laryngeal nerve (not the right) CLAPTRAP Brachiocephalic veins Cardiac plexus Aortic arch (and its 3 branches) Ligamentum arteriosum Thymus Aortic arch (inner concavity) Trachea Pulmonary -

Vagus Nerve (CN X) That Supply All of the Thoracic and Abdominal Viscera, Except the Descending and Sigmoid Colons and Other Pelvic Viscera
DR. HAYTHEM ALI ALSAYIGH Assistant prof. BOARD CLINICAL SURGICAL ANATOMY F.I.M.B.S.-MB.CH,B COLLEGE OF MEDICINE –UNIVERSITY OF BABYLON III. Autonomic Nervous System in the Thorax Is composed of motor, or efferent, nerves through which cardiac muscle, smooth muscle , and glands are innervated. Involves two neurons: preganglionic and postganglionic. It may include general visceral afferent (GVA) fibers because they run along with general visceral efferent (GVE) fibers . Consists of sympathetic (or thoracolumbar outflow) and parasympathetic (or craniosacral outflow)systems. Consists of cholinergic fibers (sympathetic preganglionic, parasympathetic preganglionic, and postganglionic) that use acetylcholine as the neurotransmitter and adrenergic fibers (sympathetic postganglionic) that use norepinephrine as the neurotransmitter (except those to sweat glands [cholinergic]). A. Sympathetic nervous system Enables the body to cope with crises or emergencies and thus often is referred to as the fight-or-flight division. Contains preganglionic cell bodies that are located in the lateral horn or intermediolateral cell column of the spinal cord segments between T1 and L2. Has preganglionic fibers that pass through the white rami communicantes and enter the sympathetic chain ganglion, where they synapse. Has postganglionic fibers that join each spinal nerve by way of the gray rami communicantes and supply the blood vessels, hair follicles (arrector pili muscles), and sweat glands. Increases the heart rate , dilates the bronchial lumen , and dilates the coronary arteries. 1. Sympathetic trunk Is composed primarily of ascending and descending preganglionic sympathetic fibers and visceral afferent fibers, and contains the cell bodies of the postganglionic sympathetic (GVE) fibers. Descends in front of the neck of the ribs and the posterior intercostal vessels. -
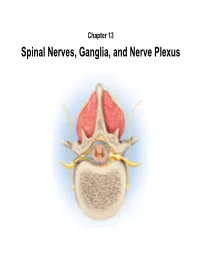
Spinal Nerves, Ganglia, and Nerve Plexus Spinal Nerves
Chapter 13 Spinal Nerves, Ganglia, and Nerve Plexus Spinal Nerves Posterior Spinous process of vertebra Posterior root Deep muscles of back Posterior ramus Spinal cord Transverse process of vertebra Posterior root ganglion Spinal nerve Anterior ramus Meningeal branch Communicating rami Anterior root Vertebral body Sympathetic ganglion Anterior General Anatomy of Nerves and Ganglia • Spinal cord communicates with the rest of the body by way of spinal nerves • nerve = a cordlike organ composed of numerous nerve fibers (axons) bound together by connective tissue – mixed nerves contain both afferent (sensory) and efferent (motor) fibers – composed of thousands of fibers carrying currents in opposite directions Anatomy of a Nerve Copyright © The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Epineurium Perineurium Copyright © The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Endoneurium Nerve Rootlets fiber Posterior root Fascicle Posterior root ganglion Anterior Blood root vessels Spinal nerve (b) Copyright by R.G. Kessel and R.H. Kardon, Tissues and Organs: A Text-Atlas of Scanning Electron Microscopy, 1979, W.H. Freeman, All rights reserved Blood vessels Fascicle Epineurium Perineurium Unmyelinated nerve fibers Myelinated nerve fibers (a) Endoneurium Myelin General Anatomy of Nerves and Ganglia • nerves of peripheral nervous system are ensheathed in Schwann cells – forms neurilemma and often a myelin sheath around the axon – external to neurilemma, each fiber is surrounded by -

Detailed and Applied Anatomy for Improved Rectal Cancer Treatment
REVIEW ARTICLE Annals of Gastroenterology (2019) 32, 1-10 Detailed and applied anatomy for improved rectal cancer treatment Τaxiarchis Κonstantinos Νikolouzakisa, Theodoros Mariolis-Sapsakosb, Chariklia Triantopoulouc, Eelco De Breed, Evaghelos Xynose, Emmanuel Chrysosf, John Tsiaoussisa Medical School of Heraklion, University of Crete; National and Kapodistrian University of Athens, Agioi Anargyroi General and Oncologic Hospital of Kifisia, Athens; Konstantopouleio General Hospital, Athens; Medical School of Crete University Hospital, Heraklion, Crete; Creta Interclinic, Heraklion, Crete; University Hospital of Heraklion, Crete, Greece Abstract Rectal anatomy is one of the most challenging concepts of visceral anatomy, even though currently there are more than 23,000 papers indexed in PubMed regarding this topic. Nonetheless, even though there is a plethora of information meant to assist clinicians to achieve a better practice, there is no universal understanding of its complexity. This in turn increases the morbidity rates due to iatrogenic causes, as mistakes that could be avoided are repeated. For this reason, this review attempts to gather current knowledge regarding the detailed anatomy of the rectum and to organize and present it in a manner that focuses on its clinical implications, not only for the colorectal surgeon, but most importantly for all colorectal cancer-related specialties. Keywords Anatomy, rectum, cancer, surgery Ann Gastroenterol 2019; 32 (5): 1-10 Introduction the anal verge [AV]) to a given landmark (e.g., the part from the sacral promontory) [1]. This study can be considered as Even though rectal anatomy is considered by most indicative of the current overall knowledge on rectal anatomy clinicians to be a well-known subject, it is still treated as a hot across CRC-related specialties. -

What Is the Autonomic Nervous System?
J Neurol Neurosurg Psychiatry: first published as 10.1136/jnnp.74.suppl_3.iii31 on 21 August 2003. Downloaded from AUTONOMIC DISEASES: CLINICAL FEATURES AND LABORATORY EVALUATION *iii31 Christopher J Mathias J Neurol Neurosurg Psychiatry 2003;74(Suppl III):iii31–iii41 he autonomic nervous system has a craniosacral parasympathetic and a thoracolumbar sym- pathetic pathway (fig 1) and supplies every organ in the body. It influences localised organ Tfunction and also integrated processes that control vital functions such as arterial blood pres- sure and body temperature. There are specific neurotransmitters in each system that influence ganglionic and post-ganglionic function (fig 2). The symptoms and signs of autonomic disease cover a wide spectrum (table 1) that vary depending upon the aetiology (tables 2 and 3). In some they are localised (table 4). Autonomic dis- ease can result in underactivity or overactivity. Sympathetic adrenergic failure causes orthostatic (postural) hypotension and in the male ejaculatory failure, while sympathetic cholinergic failure results in anhidrosis; parasympathetic failure causes dilated pupils, a fixed heart rate, a sluggish urinary bladder, an atonic large bowel and, in the male, erectile failure. With autonomic hyperac- tivity, the reverse occurs. In some disorders, particularly in neurally mediated syncope, there may be a combination of effects, with bradycardia caused by parasympathetic activity and hypotension resulting from withdrawal of sympathetic activity. The history is of particular importance in the consideration and recognition of autonomic disease, and in separating dysfunction that may result from non-autonomic disorders. CLINICAL FEATURES c copyright. General aspects Autonomic disease may present at any age group; at birth in familial dysautonomia (Riley-Day syndrome), in teenage years in vasovagal syncope, and between the ages of 30–50 years in familial amyloid polyneuropathy (FAP). -

The Neuroanatomy of Female Pelvic Pain
Chapter 2 The Neuroanatomy of Female Pelvic Pain Frank H. Willard and Mark D. Schuenke Introduction The female pelvis is innervated through primary afferent fi bers that course in nerves related to both the somatic and autonomic nervous systems. The somatic pelvis includes the bony pelvis, its ligaments, and its surrounding skeletal muscle of the urogenital and anal triangles, whereas the visceral pelvis includes the endopelvic fascial lining of the levator ani and the organ systems that it surrounds such as the rectum, reproductive organs, and urinary bladder. Uncovering the origin of pelvic pain patterns created by the convergence of these two separate primary afferent fi ber systems – somatic and visceral – on common neuronal circuitry in the sacral and thoracolumbar spinal cord can be a very dif fi cult process. Diagnosing these blended somatovisceral pelvic pain patterns in the female is further complicated by the strong descending signals from the cerebrum and brainstem to the dorsal horn neurons that can signi fi cantly modulate the perception of pain. These descending systems are themselves signi fi cantly in fl uenced by both the physiological (such as hormonal) and psychological (such as emotional) states of the individual further distorting the intensity, quality, and localization of pain from the pelvis. The interpretation of pelvic pain patterns requires a sound knowledge of the innervation of somatic and visceral pelvic structures coupled with an understand- ing of the interactions occurring in the dorsal horn of the lower spinal cord as well as in the brainstem and forebrain. This review will examine the somatic and vis- ceral innervation of the major structures and organ systems in and around the female pelvis. -

Dear Subscribers! This Issue of Our Magazine Is Devoted to Cooperation of Our Editorial Board with Ukrainian Medical Scientists
Deutscher Wissenschaftsherold • German Science Herald, N 4/2016 Dear subscribers! This issue of our magazine is devoted to cooperation of our editorial board with Ukrainian medical scientists. We present you the results of their researches. UDC: 611.831.1:611.216-018.73 Boichuk O.M. Higher State Educational Institution of Ukraine “Bukovinian State Medical University”, M.H. Turkevych Department of Human Anatomy, Chernivtsi, Ukraine, [email protected] Kryvetska I.I. Higher State Educational Institution of Ukraine “Bukovinian State Medical University”, S.M. Savenko Department of Neurology, Psychiatry and Medical Psychology Chernivtsi, Ukraine Bambuliak A.V. Higher State Educational Institution of Ukraine “Bukovinian State Medical University”, Department of Surgical and Pediatric Dentistry, Chernivtsi, Ukraine, [email protected] Sapunkov O.D. Higher State Educational Institution of Ukraine “Bukovinian State Medical University”, Department of Pediatric Surgery and Otolaryngology, Chernivtsi, Ukraine STRUCTURAL COMPONENTS OF AUTONOMIC INNERVATION OF MUCOSA OF NASAL CAVITY AND PARANASAL SINUSES Abstract. Autonomic innervation of mucosa of the nasal cavity and paranasal sinuses has been studied using complex morphological methods. It was determined that autonomic innervation of the nasal cavity and paranasal sinuses mostly occurs due to the branches of the pterygopalatine ganglion Keywords: nasal cavity, paranasal sinuses, innervation, pterygopalatine ganglion, mucosa, anatomy. Introduction. Mucosa of nasal cavity is peripheral element of olfactory analyzer functionally large receptor surface with a very consists of highly specialized epithelium of the complex and various reflex connections. It is upper nasal passage, short dendrites, which equipped with lots of blood and lymphatic ends with receptors, and axons form olfactory vessels, which are surrounded with numerous filaments that enter the olfactory bulb where nerve endings.