Eponyms Related to Genetic Disorders Associated with Gingival Enlargement; Part I
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Benign Fibro-Osseous Lesions Plus…
“Vision is the art of seeing things invisible.” Jonathan Swift 1667 - 1745 Benign Fibro-osseous Lesions Plus… Steven R. Singer, DDS [email protected] 212.305.5674 Benign Fibro-osseous Lesions Fibrous Dysplasia A group of lesions in which normal bone is Localized change in bone metabolism replaced initially by fibrous connective tissue Normal cancellous bone is replaced by Over time, the lesion is infiltrated by osteoid fibrous connective tissue and cementoid tissue The connective tissue contains varying amounts of abnormal bone with irregular This is a benign and idiopathic process trabeculae Trabeculae are randomly oriented. (Remember that normal trabeculae are aligned to respond to stress) Fibrous Dysplasia Fibrous Dysplasia Lesions may be solitary (monostotic) or Fibrous dysplasia is non-hereditary involve more than one bone (polyostotic) Caused by a mutation in a somatic cell. Monostotic form accounts for 70% of all Extent of lesions depends on the timing of cases the mutation. Polyostotic form is more common in the first If the mutation occurs earlier, the disease decade will be more widespread throughout the M=F except in McCune-Albright syndrome, body. An example is McCune-Albright which is almost exclusively found in females Syndrome 1 Fibrous Dysplasia Fibrous Dysplasia McCune-Albright Syndrome • Monostotic and polyostotic forms usually -Almost exclusively begins in the second decade of life females -Polyostotic fibrous • Slow, painless expansion of the jaws dysplasia • Patients may complain of swelling or have -

PTEN Mutations the PTEN Hamartoma Tumor Synd
Updated December 2019 (NCCN v1.2020) Cowden Syndrome/PTEN Hamartoma Tumor Syndrome: PTEN Mutations The PTEN Hamartoma Tumor Syndrome (PHTS) is a spectrum of highly variable conditions with overlapping features. This spectrum includes Cowden syndrome (CS), Bannayan-Riley-Ruvalcaba syndrome (BRRS), and PTEN-related autism spectrum disorder.1-3 The term PHTS describes any individual with a germline pathogenic PTEN mutation, regardless of their clinical presentation.4 PHTS is a multisystem syndrome primarily characterized by noncancerous (benign), tumor-like growths called hamartomas that can develop throughout the body. There is also an increased risk of adult-onset cancers.5 Cancer Risks and General Management Recommendations PTEN Mutation General Surveillance/Management Recommendations9 Carrier Cancer Population Risks2,4-8 Lifetime Cancer Risks Female Breast: 12.4% Surveillance Primary: 33-60% Breast awareness, including periodic, consistent breast self exams, Second Primary: starting at age 18 years 29% within 10 Clinical breast exam every 6-12 months starting at age 25 years, or 5- years10 10 years before the earliest breast cancer diagnosis in the family (whichever comes first) Annual mammogram with consideration of tomosynthesis and breast MRI with contrast at age 30-35 years, or 5-10 years before the earliest breast cancer diagnosis in the family (whichever comes first) Age >75 years: Management should be considered on an individual basis Surgery Discuss option of risk-reducing mastectomy, including degree of protection, reconstruction -

Phenotypic and Genotypic Characterisation of Noonan-Like
1of5 ELECTRONIC LETTER J Med Genet: first published as 10.1136/jmg.2004.024091 on 2 February 2005. Downloaded from Phenotypic and genotypic characterisation of Noonan-like/ multiple giant cell lesion syndrome J S Lee, M Tartaglia, B D Gelb, K Fridrich, S Sachs, C A Stratakis, M Muenke, P G Robey, M T Collins, A Slavotinek ............................................................................................................................... J Med Genet 2005;42:e11 (http://www.jmedgenet.com/cgi/content/full/42/2/e11). doi: 10.1136/jmg.2004.024091 oonan-like/multiple giant cell lesion syndrome (NL/ MGCLS; OMIM 163955) is a rare condition1–3 with Key points Nphenotypic overlap with Noonan’s syndrome (OMIM 163950) and cherubism (OMIM 118400) (table 1). N Noonan-like/multiple giant cell lesion syndrome (NL/ Recently, missense mutations in the PTPN11 gene on MGCLS) has clinical similarities with Noonan’s syn- chromosome 12q24.1 have been identified as the cause of drome and cherubism. It is unclear whether it is a Noonan’s syndrome in 45% of familial and sporadic cases,45 distinct entity or a variant of Noonan’s syndrome or indicating genetic heterogeneity within the syndrome. In the cherubism. 5 study by Tartaglia et al, there was a family in which three N Three unrelated patients with NL/MGCLS were char- members had features of Noonan’s syndrome; two of these acterised, two of whom were found to have mutations had incidental mandibular giant cell lesions.3 All three in the PTPN11 gene, the mutation found in 45% of members were found to have a PTPN11 mutation known to patients with Noonan’s syndrome. -

Cherubism As a Systemic Skeletal Disease
Morice et al. BMC Musculoskeletal Disorders (2020) 21:564 https://doi.org/10.1186/s12891-020-03580-z CASE REPORT Open Access Cherubism as a systemic skeletal disease: evidence from an aggressive case Anne Morice1,2,3,4*, Aline Joly3,4, Manon Ricquebourg5,6, Gérard Maruani2,7,8, Emmanuel Durand9, Louise Galmiche2,10, Jeanne Amiel2,11, Yoann Vial12,13, Hélène Cavé12,13, Kahina Belhous14, Marie Piketty15, Martine Cohen-Solal6, Ariane Berdal1,16, Corinne Collet5,6, Arnaud Picard1,2,3,4, Amelie E. Coudert1,6,16† and Natacha Kadlub1,2,3,4† Abstract Background: Cherubism is a rare autosomal dominant genetic condition caused by mutations in the SH3BP2 gene. This disease is characterized by osteolysis of the jaws, with the bone replaced by soft tissue rich in fibroblasts and multinuclear giant cells. SH3BP2 is a ubiquitous adaptor protein yet the consequences of SH3BP2 mutation have so far been described as impacting only face. Cherubism mouse models have been generated and unlike human patients, the knock-in mice exhibit systemic bone loss together with a systemic inflammation. Case presentation: In light of these observations, we decided to search for a systemic cherubism phenotype in a 6-year-old girl with an aggressive cherubism. We report here the first case of cherubism with systemic manifestations. Bone densitometry showed low overall bone density (total body Z-score = − 4.6 SD). Several markers of bone remodelling (CTx,BALP,P1NP)aswellasinflammation(TNFα and IL-1) were elevated. A causative second-site mutation in other genes known to influence bone density was ruled out by sequencing a panel of such genes. -

Prevalence and Incidence of Rare Diseases: Bibliographic Data
Number 1 | January 2019 Prevalence and incidence of rare diseases: Bibliographic data Prevalence, incidence or number of published cases listed by diseases (in alphabetical order) www.orpha.net www.orphadata.org If a range of national data is available, the average is Methodology calculated to estimate the worldwide or European prevalence or incidence. When a range of data sources is available, the most Orphanet carries out a systematic survey of literature in recent data source that meets a certain number of quality order to estimate the prevalence and incidence of rare criteria is favoured (registries, meta-analyses, diseases. This study aims to collect new data regarding population-based studies, large cohorts studies). point prevalence, birth prevalence and incidence, and to update already published data according to new For congenital diseases, the prevalence is estimated, so scientific studies or other available data. that: Prevalence = birth prevalence x (patient life This data is presented in the following reports published expectancy/general population life expectancy). biannually: When only incidence data is documented, the prevalence is estimated when possible, so that : • Prevalence, incidence or number of published cases listed by diseases (in alphabetical order); Prevalence = incidence x disease mean duration. • Diseases listed by decreasing prevalence, incidence When neither prevalence nor incidence data is available, or number of published cases; which is the case for very rare diseases, the number of cases or families documented in the medical literature is Data collection provided. A number of different sources are used : Limitations of the study • Registries (RARECARE, EUROCAT, etc) ; The prevalence and incidence data presented in this report are only estimations and cannot be considered to • National/international health institutes and agencies be absolutely correct. -

Jaffe–Campanacci Syndrome, Revisited
ORIGINAL RESEARCH ARTICLE © American College of Medical Genetics and Genomics Jaffe–Campanacci syndrome, revisited: detailed clinical and molecular analyses determine whether patients have neurofibromatosis type 1, coincidental manifestations, or a distinct disorder Douglas R. Stewart, MD1, Hilde Brems, PhD2,3, Alicia G. Gomes, MS, CGC4, Sarah L. Ruppert, MS, CGC5, Tom Callens, BSc4, Jennifer Williams, MS4, Kathleen Claes, PhD6, Michael B. Bober, MD, PhD7, Rachel Hachen, MD, MPH8, Leonard B. Kaban, MD, DDS9, Hua Li, PhD10, Angela Lin, MD11, Marie McDonald, MD, MBBCh12,13, Serge Melancon, MD14,15, June Ortenberg, MDCM, FRCPC14,15, Heather B. Radtke, MS, CGC16, Ignace Samson, MD17, Robert A. Saul, MD18, Joseph Shen, MD, PhD19, Elizabeth Siqveland, RN, CNP20, Tomi L. Toler, MS, CGC21, Merel van Maarle, MD, PhD22, Margaret Wallace, PhD10, Misti Williams, PhD23, Eric Legius, MD, PhD2,3 and Ludwine Messiaen, PhD4 Purpose: “Jaffe–Campanacci syndrome” describes the complex of diagnostic criteria for neurofibromatosis type 1. Somatic NF1 muta- multiple nonossifying fibromas of the long bones, mandibular giant tions were detected in two giant cell lesions but not in two nonos- cell lesions, and café-au-lait macules in individuals without neuro- sifying fibromas. No SPRED1 or GNAS1 (exon 8) mutations were fibromas. We sought to determine whether Jaffe–Campanacci syn- detected in the seven NF1-negative patients with Jaffe–Campanacci drome is a distinct genetic entity or a variant of neurofibromatosis syndrome, nonossifying fibromas, or giant cell lesions. type 1. Conclusion: In this study, the majority of patients with café-au-lait Methods: We performed germline NF1, SPRED1, and GNAS1 (exon macules and nonossifying fibromas or giant cell lesions harbored a 8) mutation testing on patients with Jaffe–Campanacci syndrome or pathogenic germline NF1 mutation, suggesting that many Jaffe–Cam- Jaffe–Campanacci syndrome–related features. -

An Unusual Case of Cowden Syndrome Associated With
Pistorius et al. Hereditary Cancer in Clinical Practice (2016) 14:11 DOI 10.1186/s13053-016-0051-8 CASE REPORT Open Access An unusual case of Cowden syndrome associated with ganglioneuromatous polyposis Steffen Pistorius1,6*†, Barbara Klink2,7*†, Jessica Pablik3, Andreas Rump2, Daniela Aust3,7, Marlene Garzarolli4, Evelin Schröck2,7 and Hans K. Schackert5,6,7 Abstract Background: Ganglioneuromatous polyposis (GP) is a very rare disorder which may be associated with other clinical manifestations and syndromes, such as Cowden syndrome, multiple endocrine neoplasia (MEN) type II and neurofibromatosis (NF) 1. The risk for malignant transformation of ganglioneuromas is unknown, and the combination of GP with colon cancer has been only very seldom reported. Methods and results: We report the case of a 60-year old male patient with adenocarcinoma, adenomas and lipomas of the colon and multiple gastroduodenal lesions combined with generalised lipomatosis and macrocephaly. Based on the initial endoscopic and histological findings, a (restorative) proctocolectomy was recommended but declined by the patient. Instead, a colectomy was performed. The histological examination revealed an unforeseen GP in addition to the colon cancer. Extensive molecular diagnostics allowed for the differential diagnosis of the causes of the clinical manifestations, and the clinical suspicion of Cowden syndrome could not be confirmed using Sanger Sequencing and MLPA for the analysis of PTEN. Finally, a pathogenic germline mutation in PTEN (heterozygous stop mutation in exon 2: NM_000314 (PTEN):c.138C > A; p.Tyr46*) could be detected by next-generation sequencing (NGS), confirming an unusual presentation of Cowden syndrome with GP. Conclusions: Cowden syndrome should be considered in cases of GP with extracolonic manifestation and verified by combined clinical and molecular diagnostics. -
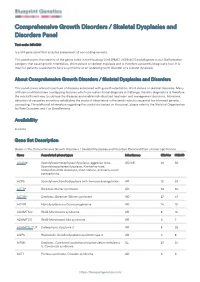
Blueprint Genetics Comprehensive Growth Disorders / Skeletal
Comprehensive Growth Disorders / Skeletal Dysplasias and Disorders Panel Test code: MA4301 Is a 374 gene panel that includes assessment of non-coding variants. This panel covers the majority of the genes listed in the Nosology 2015 (PMID: 26394607) and all genes in our Malformation category that cause growth retardation, short stature or skeletal dysplasia and is therefore a powerful diagnostic tool. It is ideal for patients suspected to have a syndromic or an isolated growth disorder or a skeletal dysplasia. About Comprehensive Growth Disorders / Skeletal Dysplasias and Disorders This panel covers a broad spectrum of diseases associated with growth retardation, short stature or skeletal dysplasia. Many of these conditions have overlapping features which can make clinical diagnosis a challenge. Genetic diagnostics is therefore the most efficient way to subtype the diseases and enable individualized treatment and management decisions. Moreover, detection of causative mutations establishes the mode of inheritance in the family which is essential for informed genetic counseling. For additional information regarding the conditions tested on this panel, please refer to the National Organization for Rare Disorders and / or GeneReviews. Availability 4 weeks Gene Set Description Genes in the Comprehensive Growth Disorders / Skeletal Dysplasias and Disorders Panel and their clinical significance Gene Associated phenotypes Inheritance ClinVar HGMD ACAN# Spondyloepimetaphyseal dysplasia, aggrecan type, AD/AR 20 56 Spondyloepiphyseal dysplasia, Kimberley -

Blueprint Genetics Comprehensive Skeletal Dysplasias and Disorders
Comprehensive Skeletal Dysplasias and Disorders Panel Test code: MA3301 Is a 251 gene panel that includes assessment of non-coding variants. Is ideal for patients with a clinical suspicion of disorders involving the skeletal system. About Comprehensive Skeletal Dysplasias and Disorders This panel covers a broad spectrum of skeletal disorders including common and rare skeletal dysplasias (eg. achondroplasia, COL2A1 related dysplasias, diastrophic dysplasia, various types of spondylo-metaphyseal dysplasias), various ciliopathies with skeletal involvement (eg. short rib-polydactylies, asphyxiating thoracic dysplasia dysplasias and Ellis-van Creveld syndrome), various subtypes of osteogenesis imperfecta, campomelic dysplasia, slender bone dysplasias, dysplasias with multiple joint dislocations, chondrodysplasia punctata group of disorders, neonatal osteosclerotic dysplasias, osteopetrosis and related disorders, abnormal mineralization group of disorders (eg hypopohosphatasia), osteolysis group of disorders, disorders with disorganized development of skeletal components, overgrowth syndromes with skeletal involvement, craniosynostosis syndromes, dysostoses with predominant craniofacial involvement, dysostoses with predominant vertebral involvement, patellar dysostoses, brachydactylies, some disorders with limb hypoplasia-reduction defects, ectrodactyly with and without other manifestations, polydactyly-syndactyly-triphalangism group of disorders, and disorders with defects in joint formation and synostoses. Availability 4 weeks Gene Set Description -

On the Genetics of Hypodontia and Microdontia: Synergism Or Allelism of Major Genes in a Family with Six Affected Members
JMed Genet 1996;33:137-142 137 On the genetics of hypodontia and microdontia: synergism or allelism of major genes in a family J Med Genet: first published as 10.1136/jmg.33.2.137 on 1 February 1996. Downloaded from with six affected members S P Lyngstadaas, H Nordbo, T Gedde-Dahl Jr, P S Thrane Abstract and epigenetic factors.7 In a large study oftooth Familial severe hypodontia of the per- number and size in British schoolchildren, ex- manent dentition is a rare condition. The cluding patients with more widespread ab- genetics ofthis entity remains unclear and normalities, Brook3 favoured a multifactorial several modes of inheritance have been model with a continuous spectrum, related to suggested. We report here an increase in tooth number and size, with thresholds, and the number of congenitally missing teeth where position on the scale depends upon the after the mating of affected subjects from combination of numerous genetic and en- two unrelated Norwegian families. This vironmental factors, each with a small effect. condition may be the result of allelic mut- In this study the proportion ofaffected relatives ations at a single gene locus. Alternatively, varied with the severity of the condition in the incompletely penetrant non-allelic genes probands and an association between hy- may show a synergistic effect as expected podontia and microdontia was noted. for a multifactorial trait with interacting Other causes of hypodontia have been sug- gene products. This and similar kindreds gested and include an evolutionary trend to- may allow identification of genes involved wards fewer teeth,28 infections during in growth and differentiation of dental tis- pregnancy and early childhood, hormonal dys- sues by linkage and haplotype association function, which itself may be inherited, and analysis. -

Cowden Syndrome
Update No.4 - 2017 Cowden syndrome Cowden syndrome is a rare inherited multiple hamartoma syndrome with a reported, but likely underestimated, prevalence of 1 in 200,000. Affected individuals usually have macrocephaly and develop benign mucocutaneous lesions (trichilemmomas, papillomatous papules and acral keratosis) by early adulthood. The clinical diagnosis of Cowden syndrome is complex and based on diagnostic criteria divided into 3 categories (pathognomonic, major and minor). Gastrointestinal manifestations are common and can be suggestive of Cowden syndrome in a patient with other manifestations of the disease. Genetics: Autosomal dominant inheritance. Up to 85% of cases are caused by mutations in the PTEN gene on chromosome 10 or its promoter. Mutation of the gene and altered protein product leads to unchecked cellular proliferation. Gastrointestinal tract manifestations: More recent studies suggest that 75-95% of patients with Cowden syndrome will have gastrointestinal manifestations. These can include: Oesophageal glycogenic acanthosis, which often presents as small white lesions endoscopically Multiple hamartomatous polyps of the GI tract Small sessile hamartomatous polyps of the large bowel frequently containing adipose tissue and lymphoid follicles (Fig. 1) Ganglioneuroma (Fig. 2), lipoma, and fibrolipoma of the large bowel Inflammatory/hyperplastic polyps of the stomach Increased risk of adenomas in the large bowel Fig. 1 Hamartomatous polyp Fig. 2 Ganglioneuroma Malignant risk: It is important to recognise Cowden syndrome -

Living with Orofacial Conditions: Psychological Distress
Qual Life Res DOI 10.1007/s11136-014-0826-1 Living with orofacial conditions: psychological distress and quality of life in adults affected with Treacher Collins syndrome, cherubism, or oligodontia/ectodermal dysplasia—a comparative study Amy Østertun Geirdal • Solfrid Sørgjerd Saltnes • Kari Storhaug • Pamela A˚ sten • Hilde Nordgarden • Janicke Liaaen Jensen Accepted: 10 October 2014 Ó The Author(s) 2014. This article is published with open access at Springerlink.com Abstract Conclusions Psychological distress and quality of life Purpose The relationship between quality of life, psy- differed in various orofacial conditions. This study pro- chological distress, and orofacial syndromes in children vided insight into these aspects that may contribute to and adolescents has been reported in several studies. improved care. However, little is known about differences in psychological distress and quality of life among adults with different Keywords Psychological distress Á Quality of life Á orofacial conditions. Therefore, the aims of this study were Treacher Collins syndrome Á Cherubism Á Oligodontia/ to examine and compare these factors among three groups ectodermal dysplasia of adults affected by Treacher Collins syndrome (TCS), cherubism, and oligodontia/ectodermal dysplasia (ED). Methods We included 11 individuals with TCS (mean Introduction age 46.9, SD 12.9 years), 15 with cherubism (mean age 50.3, SD 16.8 years), and 49 with oligodontia/ED (mean Treacher Collins syndrome (TCS), cherubism, oligodontia, age 30.7, SD 15.6 years). The respondents completed and ectodermal dysplasias (EDs) are all examples of rare questionnaires related to psychological distress and quality genetic conditions that affect the orofacial complex. These of life.