Cherubism: Best Clinical Practice
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Benign Fibro-Osseous Lesions Plus…
“Vision is the art of seeing things invisible.” Jonathan Swift 1667 - 1745 Benign Fibro-osseous Lesions Plus… Steven R. Singer, DDS [email protected] 212.305.5674 Benign Fibro-osseous Lesions Fibrous Dysplasia A group of lesions in which normal bone is Localized change in bone metabolism replaced initially by fibrous connective tissue Normal cancellous bone is replaced by Over time, the lesion is infiltrated by osteoid fibrous connective tissue and cementoid tissue The connective tissue contains varying amounts of abnormal bone with irregular This is a benign and idiopathic process trabeculae Trabeculae are randomly oriented. (Remember that normal trabeculae are aligned to respond to stress) Fibrous Dysplasia Fibrous Dysplasia Lesions may be solitary (monostotic) or Fibrous dysplasia is non-hereditary involve more than one bone (polyostotic) Caused by a mutation in a somatic cell. Monostotic form accounts for 70% of all Extent of lesions depends on the timing of cases the mutation. Polyostotic form is more common in the first If the mutation occurs earlier, the disease decade will be more widespread throughout the M=F except in McCune-Albright syndrome, body. An example is McCune-Albright which is almost exclusively found in females Syndrome 1 Fibrous Dysplasia Fibrous Dysplasia McCune-Albright Syndrome • Monostotic and polyostotic forms usually -Almost exclusively begins in the second decade of life females -Polyostotic fibrous • Slow, painless expansion of the jaws dysplasia • Patients may complain of swelling or have -

Segmental Overvekst Og Vaskulærmalformasjoner V02
2/1/2021 Segmental overvekst og vaskulærmalformasjoner v02 Avdeling for medisinsk genetikk Segmental overvekst og vaskulærmalformasjoner Genpanel, versjon v02 * Enkelte genomiske regioner har lav eller ingen sekvensdekning ved eksomsekvensering. Dette skyldes at de har stor likhet med andre områder i genomet, slik at spesifikk gjenkjennelse av disse områdene og påvisning av varianter i disse områdene, blir vanskelig og upålitelig. Disse genetiske regionene har vi identifisert ved å benytte USCS segmental duplication hvor områder større enn 1 kb og ≥90% likhet med andre regioner i genomet, gjenkjennes (https://genome.ucsc.edu). Vi gjør oppmerksom på at ved identifiseringav ekson oppstrøms for startkodon kan eksonnummereringen endres uten at transkript ID endres. Avdelingens websider har en full oversikt over områder som er affisert av segmentale duplikasjoner. ** Transkriptets kodende ekson. Ekson Gen Gen affisert (HGNC (HGNC Transkript Ekson** Fenotype av symbol) ID) segdup* ACVRL1 175 NM_000020.3 2-10 Telangiectasia, hereditary hemorrhagic, type 2 OMIM ADAMTS3 219 NM_014243.3 1-22 Hennekam lymphangiectasia- lymphedema syndrome 3 OMIM AKT1 391 NM_005163.2 2-14 Cowden syndrome 6 OMIM Proteus syndrome, somatic OMIM AKT2 392 NM_001626.6 2-14 Diabetes mellitus, type II OMIM Hypoinsulinemic hypoglycemia with hemihypertrophy OMIM AKT3 393 NM_005465.7 2-14 Megalencephaly-polymicrogyria- polydactyly-hydrocephalus syndrome 2 OMIM file:///data/SegOv_v02-web.html 1/7 2/1/2021 Segmental overvekst og vaskulærmalformasjoner v02 Ekson Gen Gen affisert (HGNC (HGNC -

Phenotypic and Genotypic Characterisation of Noonan-Like
1of5 ELECTRONIC LETTER J Med Genet: first published as 10.1136/jmg.2004.024091 on 2 February 2005. Downloaded from Phenotypic and genotypic characterisation of Noonan-like/ multiple giant cell lesion syndrome J S Lee, M Tartaglia, B D Gelb, K Fridrich, S Sachs, C A Stratakis, M Muenke, P G Robey, M T Collins, A Slavotinek ............................................................................................................................... J Med Genet 2005;42:e11 (http://www.jmedgenet.com/cgi/content/full/42/2/e11). doi: 10.1136/jmg.2004.024091 oonan-like/multiple giant cell lesion syndrome (NL/ MGCLS; OMIM 163955) is a rare condition1–3 with Key points Nphenotypic overlap with Noonan’s syndrome (OMIM 163950) and cherubism (OMIM 118400) (table 1). N Noonan-like/multiple giant cell lesion syndrome (NL/ Recently, missense mutations in the PTPN11 gene on MGCLS) has clinical similarities with Noonan’s syn- chromosome 12q24.1 have been identified as the cause of drome and cherubism. It is unclear whether it is a Noonan’s syndrome in 45% of familial and sporadic cases,45 distinct entity or a variant of Noonan’s syndrome or indicating genetic heterogeneity within the syndrome. In the cherubism. 5 study by Tartaglia et al, there was a family in which three N Three unrelated patients with NL/MGCLS were char- members had features of Noonan’s syndrome; two of these acterised, two of whom were found to have mutations had incidental mandibular giant cell lesions.3 All three in the PTPN11 gene, the mutation found in 45% of members were found to have a PTPN11 mutation known to patients with Noonan’s syndrome. -

Megalencephaly and Macrocephaly
277 Megalencephaly and Macrocephaly KellenD.Winden,MD,PhD1 Christopher J. Yuskaitis, MD, PhD1 Annapurna Poduri, MD, MPH2 1 Department of Neurology, Boston Children’s Hospital, Boston, Address for correspondence Annapurna Poduri, Epilepsy Genetics Massachusetts Program, Division of Epilepsy and Clinical Electrophysiology, 2 Epilepsy Genetics Program, Division of Epilepsy and Clinical Department of Neurology, Fegan 9, Boston Children’s Hospital, 300 Electrophysiology, Department of Neurology, Boston Children’s Longwood Avenue, Boston, MA 02115 Hospital, Boston, Massachusetts (e-mail: [email protected]). Semin Neurol 2015;35:277–287. Abstract Megalencephaly is a developmental disorder characterized by brain overgrowth secondary to increased size and/or numbers of neurons and glia. These disorders can be divided into metabolic and developmental categories based on their molecular etiologies. Metabolic megalencephalies are mostly caused by genetic defects in cellular metabolism, whereas developmental megalencephalies have recently been shown to be caused by alterations in signaling pathways that regulate neuronal replication, growth, and migration. These disorders often lead to epilepsy, developmental disabilities, and Keywords behavioral problems; specific disorders have associations with overgrowth or abnor- ► megalencephaly malities in other tissues. The molecular underpinnings of many of these disorders are ► hemimegalencephaly now understood, providing insight into how dysregulation of critical pathways leads to ► -

Cardiomyopathy Precision Panel Overview Indications
Cardiomyopathy Precision Panel Overview Cardiomyopathies are a group of conditions with a strong genetic background that structurally hinder the heart to pump out blood to the rest of the body due to weakness in the heart muscles. These diseases affect individuals of all ages and can lead to heart failure and sudden cardiac death. If there is a family history of cardiomyopathy it is strongly recommended to undergo genetic testing to be aware of the family risk, personal risk, and treatment options. Most types of cardiomyopathies are inherited in a dominant manner, which means that one altered copy of the gene is enough for the disease to present in an individual. The symptoms of cardiomyopathy are variable, and these diseases can present in different ways. There are 5 types of cardiomyopathies, the most common being hypertrophic cardiomyopathy: 1. Hypertrophic cardiomyopathy (HCM) 2. Dilated cardiomyopathy (DCM) 3. Restrictive cardiomyopathy (RCM) 4. Arrhythmogenic Right Ventricular Cardiomyopathy (ARVC) 5. Isolated Left Ventricular Non-Compaction Cardiomyopathy (LVNC). The Igenomix Cardiomyopathy Precision Panel serves as a diagnostic and tool ultimately leading to a better management and prognosis of the disease. It provides a comprehensive analysis of the genes involved in this disease using next-generation sequencing (NGS) to fully understand the spectrum of relevant genes. Indications The Igenomix Cardiomyopathy Precision Panel is indicated in those cases where there is a clinical suspicion of cardiomyopathy with or without the following manifestations: - Shortness of breath - Fatigue - Arrythmia (abnormal heart rhythm) - Family history of arrhythmia - Abnormal scans - Ventricular tachycardia - Ventricular fibrillation - Chest Pain - Dizziness - Sudden cardiac death in the family 1 Clinical Utility The clinical utility of this panel is: - The genetic and molecular diagnosis for an accurate clinical diagnosis of a patient with personal or family history of cardiomyopathy, channelopathy or sudden cardiac death. -

Cherubism As a Systemic Skeletal Disease
Morice et al. BMC Musculoskeletal Disorders (2020) 21:564 https://doi.org/10.1186/s12891-020-03580-z CASE REPORT Open Access Cherubism as a systemic skeletal disease: evidence from an aggressive case Anne Morice1,2,3,4*, Aline Joly3,4, Manon Ricquebourg5,6, Gérard Maruani2,7,8, Emmanuel Durand9, Louise Galmiche2,10, Jeanne Amiel2,11, Yoann Vial12,13, Hélène Cavé12,13, Kahina Belhous14, Marie Piketty15, Martine Cohen-Solal6, Ariane Berdal1,16, Corinne Collet5,6, Arnaud Picard1,2,3,4, Amelie E. Coudert1,6,16† and Natacha Kadlub1,2,3,4† Abstract Background: Cherubism is a rare autosomal dominant genetic condition caused by mutations in the SH3BP2 gene. This disease is characterized by osteolysis of the jaws, with the bone replaced by soft tissue rich in fibroblasts and multinuclear giant cells. SH3BP2 is a ubiquitous adaptor protein yet the consequences of SH3BP2 mutation have so far been described as impacting only face. Cherubism mouse models have been generated and unlike human patients, the knock-in mice exhibit systemic bone loss together with a systemic inflammation. Case presentation: In light of these observations, we decided to search for a systemic cherubism phenotype in a 6-year-old girl with an aggressive cherubism. We report here the first case of cherubism with systemic manifestations. Bone densitometry showed low overall bone density (total body Z-score = − 4.6 SD). Several markers of bone remodelling (CTx,BALP,P1NP)aswellasinflammation(TNFα and IL-1) were elevated. A causative second-site mutation in other genes known to influence bone density was ruled out by sequencing a panel of such genes. -

Prevalence and Incidence of Rare Diseases: Bibliographic Data
Number 1 | January 2019 Prevalence and incidence of rare diseases: Bibliographic data Prevalence, incidence or number of published cases listed by diseases (in alphabetical order) www.orpha.net www.orphadata.org If a range of national data is available, the average is Methodology calculated to estimate the worldwide or European prevalence or incidence. When a range of data sources is available, the most Orphanet carries out a systematic survey of literature in recent data source that meets a certain number of quality order to estimate the prevalence and incidence of rare criteria is favoured (registries, meta-analyses, diseases. This study aims to collect new data regarding population-based studies, large cohorts studies). point prevalence, birth prevalence and incidence, and to update already published data according to new For congenital diseases, the prevalence is estimated, so scientific studies or other available data. that: Prevalence = birth prevalence x (patient life This data is presented in the following reports published expectancy/general population life expectancy). biannually: When only incidence data is documented, the prevalence is estimated when possible, so that : • Prevalence, incidence or number of published cases listed by diseases (in alphabetical order); Prevalence = incidence x disease mean duration. • Diseases listed by decreasing prevalence, incidence When neither prevalence nor incidence data is available, or number of published cases; which is the case for very rare diseases, the number of cases or families documented in the medical literature is Data collection provided. A number of different sources are used : Limitations of the study • Registries (RARECARE, EUROCAT, etc) ; The prevalence and incidence data presented in this report are only estimations and cannot be considered to • National/international health institutes and agencies be absolutely correct. -

MECHANISMS in ENDOCRINOLOGY: Novel Genetic Causes of Short Stature
J M Wit and others Genetics of short stature 174:4 R145–R173 Review MECHANISMS IN ENDOCRINOLOGY Novel genetic causes of short stature 1 1 2 2 Jan M Wit , Wilma Oostdijk , Monique Losekoot , Hermine A van Duyvenvoorde , Correspondence Claudia A L Ruivenkamp2 and Sarina G Kant2 should be addressed to J M Wit Departments of 1Paediatrics and 2Clinical Genetics, Leiden University Medical Center, PO Box 9600, 2300 RC Leiden, Email The Netherlands [email protected] Abstract The fast technological development, particularly single nucleotide polymorphism array, array-comparative genomic hybridization, and whole exome sequencing, has led to the discovery of many novel genetic causes of growth failure. In this review we discuss a selection of these, according to a diagnostic classification centred on the epiphyseal growth plate. We successively discuss disorders in hormone signalling, paracrine factors, matrix molecules, intracellular pathways, and fundamental cellular processes, followed by chromosomal aberrations including copy number variants (CNVs) and imprinting disorders associated with short stature. Many novel causes of GH deficiency (GHD) as part of combined pituitary hormone deficiency have been uncovered. The most frequent genetic causes of isolated GHD are GH1 and GHRHR defects, but several novel causes have recently been found, such as GHSR, RNPC3, and IFT172 mutations. Besides well-defined causes of GH insensitivity (GHR, STAT5B, IGFALS, IGF1 defects), disorders of NFkB signalling, STAT3 and IGF2 have recently been discovered. Heterozygous IGF1R defects are a relatively frequent cause of prenatal and postnatal growth retardation. TRHA mutations cause a syndromic form of short stature with elevated T3/T4 ratio. Disorders of signalling of various paracrine factors (FGFs, BMPs, WNTs, PTHrP/IHH, and CNP/NPR2) or genetic defects affecting cartilage extracellular matrix usually cause disproportionate short stature. -

Jaffe–Campanacci Syndrome, Revisited
ORIGINAL RESEARCH ARTICLE © American College of Medical Genetics and Genomics Jaffe–Campanacci syndrome, revisited: detailed clinical and molecular analyses determine whether patients have neurofibromatosis type 1, coincidental manifestations, or a distinct disorder Douglas R. Stewart, MD1, Hilde Brems, PhD2,3, Alicia G. Gomes, MS, CGC4, Sarah L. Ruppert, MS, CGC5, Tom Callens, BSc4, Jennifer Williams, MS4, Kathleen Claes, PhD6, Michael B. Bober, MD, PhD7, Rachel Hachen, MD, MPH8, Leonard B. Kaban, MD, DDS9, Hua Li, PhD10, Angela Lin, MD11, Marie McDonald, MD, MBBCh12,13, Serge Melancon, MD14,15, June Ortenberg, MDCM, FRCPC14,15, Heather B. Radtke, MS, CGC16, Ignace Samson, MD17, Robert A. Saul, MD18, Joseph Shen, MD, PhD19, Elizabeth Siqveland, RN, CNP20, Tomi L. Toler, MS, CGC21, Merel van Maarle, MD, PhD22, Margaret Wallace, PhD10, Misti Williams, PhD23, Eric Legius, MD, PhD2,3 and Ludwine Messiaen, PhD4 Purpose: “Jaffe–Campanacci syndrome” describes the complex of diagnostic criteria for neurofibromatosis type 1. Somatic NF1 muta- multiple nonossifying fibromas of the long bones, mandibular giant tions were detected in two giant cell lesions but not in two nonos- cell lesions, and café-au-lait macules in individuals without neuro- sifying fibromas. No SPRED1 or GNAS1 (exon 8) mutations were fibromas. We sought to determine whether Jaffe–Campanacci syn- detected in the seven NF1-negative patients with Jaffe–Campanacci drome is a distinct genetic entity or a variant of neurofibromatosis syndrome, nonossifying fibromas, or giant cell lesions. type 1. Conclusion: In this study, the majority of patients with café-au-lait Methods: We performed germline NF1, SPRED1, and GNAS1 (exon macules and nonossifying fibromas or giant cell lesions harbored a 8) mutation testing on patients with Jaffe–Campanacci syndrome or pathogenic germline NF1 mutation, suggesting that many Jaffe–Cam- Jaffe–Campanacci syndrome–related features. -

Fetal Hydrops in Combination with Gonadoblastoid Testicular Dysplasia May Represent a Lethal Type of Noonan Syndrome
etics & E en m G b ry n o a l o Reischer et al., Human Genet Embryol 2016, 6:3 m g u y H Human Genetics & Embryology DOI: 10.4172/2161-0436.1000137 ISSN: 2161-0436 Research Article Open Access Fetal Hydrops in Combination with Gonadoblastoid Testicular Dysplasia May Represent a Lethal Type of Noonan Syndrome Theresa Reischer1, Maximilian Schmid1, Sukirthini Balendran1, Manuel Nistal2, Julia Vodopiutz3, Elisabeth Krampl-Bettelheim4, Niko Popitsch5, Sandra Liebmann-Reindl6 and Berthold Streubel6,7* 1Department of Obstetrics and Feto-Maternal Medicine, Medical University of Vienna, Vienna, Austria 2Department of Pathology, Hospital La Paz, Universidad Autónoma de Madrid, Spain 3Department of Pediatrics, Medical University of Vienna, Vienna, Austria 4Fetomed - Center for Fetal Medicine, Doebling Private Hospital, Vienna, Austria 5Wellcome Trust Centre for Human Genetics, University of Oxford, Oxford, UK 6Core Facility Genomics, Medical University of Vienna, Vienna, Austria 7Department of Pathology, Medical University of Vienna, Austria Abstract Objectives: Fetal gonadoblastoid testicular dysplasia is a rare finding. The combination with typical features of Noonan syndrome has never been described so far. We performed genetic testing including whole exome sequencing in two cases with fetal hydrops, congenital heart disease and gonadoblastoid testicular dysplasia. Methods: Exome sequencing was performed in the index case, where high quality DNA was isolated from fetal blood. In the second case and in five further gonadoblastoma samples, conventional Sanger sequencing was performed on DNA isolated from formalin fixed, paraffin embedded tissue. Results: Whole exome sequencing of the index case revealed a pathogenic mutation in the RIT1 gene (c.270G>A (p.Met90Ile)), leading to the diagnosis of Noonan syndrome type 8. -
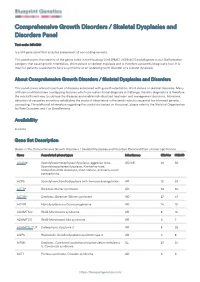
Blueprint Genetics Comprehensive Growth Disorders / Skeletal
Comprehensive Growth Disorders / Skeletal Dysplasias and Disorders Panel Test code: MA4301 Is a 374 gene panel that includes assessment of non-coding variants. This panel covers the majority of the genes listed in the Nosology 2015 (PMID: 26394607) and all genes in our Malformation category that cause growth retardation, short stature or skeletal dysplasia and is therefore a powerful diagnostic tool. It is ideal for patients suspected to have a syndromic or an isolated growth disorder or a skeletal dysplasia. About Comprehensive Growth Disorders / Skeletal Dysplasias and Disorders This panel covers a broad spectrum of diseases associated with growth retardation, short stature or skeletal dysplasia. Many of these conditions have overlapping features which can make clinical diagnosis a challenge. Genetic diagnostics is therefore the most efficient way to subtype the diseases and enable individualized treatment and management decisions. Moreover, detection of causative mutations establishes the mode of inheritance in the family which is essential for informed genetic counseling. For additional information regarding the conditions tested on this panel, please refer to the National Organization for Rare Disorders and / or GeneReviews. Availability 4 weeks Gene Set Description Genes in the Comprehensive Growth Disorders / Skeletal Dysplasias and Disorders Panel and their clinical significance Gene Associated phenotypes Inheritance ClinVar HGMD ACAN# Spondyloepimetaphyseal dysplasia, aggrecan type, AD/AR 20 56 Spondyloepiphyseal dysplasia, Kimberley -

Blueprint Genetics Comprehensive Skeletal Dysplasias and Disorders
Comprehensive Skeletal Dysplasias and Disorders Panel Test code: MA3301 Is a 251 gene panel that includes assessment of non-coding variants. Is ideal for patients with a clinical suspicion of disorders involving the skeletal system. About Comprehensive Skeletal Dysplasias and Disorders This panel covers a broad spectrum of skeletal disorders including common and rare skeletal dysplasias (eg. achondroplasia, COL2A1 related dysplasias, diastrophic dysplasia, various types of spondylo-metaphyseal dysplasias), various ciliopathies with skeletal involvement (eg. short rib-polydactylies, asphyxiating thoracic dysplasia dysplasias and Ellis-van Creveld syndrome), various subtypes of osteogenesis imperfecta, campomelic dysplasia, slender bone dysplasias, dysplasias with multiple joint dislocations, chondrodysplasia punctata group of disorders, neonatal osteosclerotic dysplasias, osteopetrosis and related disorders, abnormal mineralization group of disorders (eg hypopohosphatasia), osteolysis group of disorders, disorders with disorganized development of skeletal components, overgrowth syndromes with skeletal involvement, craniosynostosis syndromes, dysostoses with predominant craniofacial involvement, dysostoses with predominant vertebral involvement, patellar dysostoses, brachydactylies, some disorders with limb hypoplasia-reduction defects, ectrodactyly with and without other manifestations, polydactyly-syndactyly-triphalangism group of disorders, and disorders with defects in joint formation and synostoses. Availability 4 weeks Gene Set Description