International Clinical Classification of Diabetic Retinopathy Severity of Diabetic Macular Edema
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Post-Cataract Cystoid Macular Oedema Prevention – Update 2019
Review Cystoid Macular Oedema Post-cataract Cystoid Macular Oedema Prevention – Update 2019 Andrzej Grzybowski,1,2 Reda Zemaitiene,3 Lina Mikalauskiene3 1. Department of Ophthalmology, University of Warmia and Mazury, Olsztyn, Poland; 2. Institute for Research in Ophthalmology, Foundation for Ophthalmology Development, Poznan, Poland; 3. Department of Ophthalmology, Medical Academy, Lithuanian University of Health Sciences, Kaunas, Lithuania DOI: https://doi.org/10.17925/EOR.2019.13.1.37 seudophakic cystoid macular oedema (PCMO) is a common complication following both uncomplicated and complicated cataract surgery, becoming apparent about 6 weeks following surgery. PCMO may be asymptomatic in some cases, but in others is associated Pwith a reduction in visual acuity. The pathogenesis of PCMO is linked to postoperative inflammation and the release of inflammatory mediators. The use of topical steroids and/or nonsteroidal anti-inflammatory drugs can reduce the adverse effects of inflammation and have been used for the prevention and treatment of PCMO. However, the therapeutic effectiveness of these drugs is currently not well understood, partially because PCMO can spontaneously resolve as well as the multiple treatment protocols and the paucity of robust data exist. In this review we compare the various prophylactic options for PCMO and provide commentary on their efficacy. Keywords Various options for the prevention of pseudophakic cystoid macular oedema (PCMO) have been Pseudophakic cystoid macular oedema, offered. Nonsteroidal anti-inflammatory drugs (NSAIDs) seem to be beneficial in preventing post-operative inflammation, cataract surgery, postoperative inflammation; however, there is lack of evidence for long-term benefit after cataract nonsteroidal anti-inflammatory drugs surgery. What is more, topical NSAID preparations are difficult to compare, as studies differ in Disclosure: Andrzej Grzybowski, Reda inclusion criteria, patient characteristics, prescription and duration of treatment. -

Treat Cataracts and Astigmatism with One
TREAT CATARACTS Cataract patients have a choice Eye with cataract See life through the AcrySof® IQ Toric IOL. of treatments, including the As the eye ages, the lens becomes AND ASTIGMATISM WITH breakthrough AcrySof® IQ Toric cloudier, allowing less light to pass Ask your doctor about your options. intraocular lens (IOL) that treats through. The light that doesn’t make ONE PROCEDURE pre-existing corneal astigmatism at the it to the retina is diffused or scattered, same time that it corrects cataracts. leaving vision defocused and blurry. With a single procedure, you have the potential to enjoy freedom from glasses or contacts for distance vision with enhanced image quality – and see life through a new lens. 1. Independent third party research; Data on File, December 2011. Cataracts and astigmatism defined. Important Product Information A cataract is like a cloud over the eye’s lens, Eye with astigmatism CAUTION: Restricted by law to sale by or on the order of a physician. DESCRIPTION: interfering with quality of vision and making The AcrySof® IQ Toric Intraocular Lenses (IOLs) are artificial lenses implanted in the normal activities, such as driving a car, reading When the surface of the cornea has eye of adult patients following cataract surgery. These lenses are designed to correct pre-existing corneal astigmatism, which is the inability of the eye to focus clearly at a newspaper or seeing people’s faces, an uneven curvature, shaped more any distance because of difference curvatures on the cornea, and provide distance vision. WARNINGS / PRECAUTIONS: You may experience and need to contact your increasingly difficult. -

The Usefulness of Systemic Inflammatory Markers As Diagnostic
A RQUIVOS B RASILEIROS DE ORIGINAL ARTICLE The usefulness of systemic inflammatory markers as diagnostic indicators of the pathogenesis of diabetic macular edema A utilidade de marcadores inflamatórios sistêmicos como indicadores diagnósticos da patogênese do edema macular diabético Cagri Ilhan1 , Mehmet Citirik2, Mehmet Murat Uzel3, Hasan Kiziltoprak4, Kemal Tekin5 1. Department of Ophthalmology, Hatay State Hospital, Hatay, Turkey. 2. Department of Ophthalmology, University of Health Sciences, Ankara Ulucanlar Eye Education and Research Hospital, Ankara, Turkey. 3. Department of Ophthalmology, Balikesir University, Balikesir, Turkey. 4. Department of Ophthalmology, Bingol Maternity and Child Hospital, Bingol, Turkey. 5. Department of Ophthalmology, Ercis State Hospital, Van, Turkey. ABSTRACT | Purpose: To investigate the usefulness of sys- groups were similar (diabetic macular edema vs. non-diabetic temic inflammatory markers [i.e., white blood cell and platelet macular edema, p=0.08; diabetic macular edema vs. control, counts, mean platelet volume, and their ratios] as diagnostic p=0.02; and non- diabetic macular edema vs. control, p=0.78). markers of the pathogenesis of diabetic macular edema. Me- All other parameters were similar between groups (all p>0.05). thods: The study cohort included 80 diabetic macular edema Conclusion: The neutrophil/lymphocyte ratio and mean platelet patients (40 with diabetic retinopathy and 40 without) and 40 volume of the diabetic macular edema group were higher than healthy age- and sex-matched controls. Neutrophil, lymphocyte, those of the non-diabetic macular edema and control groups. monocyte, and platelet counts, and the mean platelet volume A neutrophil/lymphocyte ratio cutoff value of ≥2.26 was identified were determined from peripheral blood samples, and the as an indicator of the pathogenesis of diabetic macular edema monocyte/lymphocyte, platelet/lymphocyte, and mean platelet with high sensitivity and specificity. -

Proposed International Clinical Diabetic Retinopathy and Diabetic Macular Edema Disease Severity Scales
Proposed International Clinical Diabetic Retinopathy and Diabetic Macular Edema Disease Severity Scales C. P. Wilkinson, MD,1 Frederick L. Ferris, III, MD,2 Ronald E. Klein, MD, MPH,3 Paul P. Lee, MD, JD,4 Carl David Agardh, MD,5 Matthew Davis, MD,3 Diana Dills, MD,6 Anselm Kampik, MD,7 R. Pararajasegaram, MD,8 Juan T. Verdaguer, MD,9 representing the Global Diabetic Retinopathy Project Group Purpose: To develop consensus regarding clinical disease severity classification systems for diabetic retinopathy and diabetic macular edema that can be used around the world, and to improve communication and coordination of care among physicians who care for patients with diabetes. Design: Report regarding the development of clinical diabetic retinopathy disease severity scales. Participants: A group of 31 individuals from 16 countries, representing comprehensive ophthalmology, retina subspecialties, endocrinology, and epidemiology. Methods: An initial clinical classification system, based on the Early Treatment Diabetic Retinopathy Study and the Wisconsin Epidemiologic Study of Diabetic Retinopathy publications, was circulated to the group in advance of a workshop. Each member reviewed this using e-mail, and a modified Delphi system was used to stratify responses. At a later workshop, separate systems for diabetic retinopathy and macular edema were developed. These were then reevaluated by group members, and the modified Delphi system was again used to measure degrees of agreement. Main Outcome Measures: Consensus regarding specific classification systems was achieved. Results: A five-stage disease severity classification for diabetic retinopathy includes three stages of low risk, afourthstageofseverenonproliferativeretinopathy,andafifthstageofproliferativeretinopathy.Diabeticmacular edema is classified as apparently present or apparently absent. If training and equipment allow the screener to make a valid decision, macular edema is further categorized as a function of its distance from the central macula. -

Optical Coherence Tomography Demonstrates Subretinal Macular Edema from Papilledema
CLINICAL SCIENCES Optical Coherence Tomography Demonstrates Subretinal Macular Edema From Papilledema Vincent J. Hoye III, MD; Audina M. Berrocal, MD; Thomas R. Hedges III, MD; Maria Luz Amaro-Quireza, OD Objective: To evaluate macular changes in eyes with duction in visual acuity. The subretinal fluid appeared papilledema from increased intracranial pressure using to arise from the peripapillary region, and all showed optical coherence tomography (OCT). some improvement in central vision as the fluid re- solved. Methods: Fifty-five patients with papilledema seen dur- ing 1998 and 1999 were studied with OCT of the optic Conclusions: Subretinal fluid accumulations can cause nerve and retinal nerve fiber layer. Nineteen of these also decreased visual acuity in patients with papilledema. Op- had OCT of the macula during periods of acute, sub- tical coherence tomography can demonstrate subretinal acute, or recurrent papilledema and were evaluated in fluid and can be used to follow the course of this impor- detail for this report. tant visual complication of papilledema. Results: Seven patients had OCT evidence of sub- retinal fluid involving the macula. All had some re- Arch Ophthalmol. 2001;119:1287-1290 OSS OF visual acuity from pap- mal findings on neuroimaging scans and illedema or optic nerve head elevated opening pressures on lumbar swelling due to increased in- puncture. Two patients had brain metas- tracranial pressure is uncom- tases, one from breast cancer and the other mon. The visual conse- from testicular cancer. Six patients were Lquences of papilledema usually are limited treated medically with acetazolamide to visual field defects and enlargement of and/or furosemide. -

Diabetic Retinopathy
RETINA HEALTH SERIES | Facts from the ASRS The Foundation American Society of Retina Specialists Committed to improving the quality of life of all people with retinal disease. Diabetic Retinopathy: Diabetic retinopathy (pronounced ret in OP uh thee) is a complication of diabetes that causes damage to the blood vessels of the retina— the light-sensitive tissue that lines the back part of the eye, allowing you to see fine detail. Diabetic retinopathy is the most common cause of irreversible blindness in working-age Americans. As many people with type 1 diabetes suffer blindness SYMPTOMS as those with the more common type 2 disease. Diabetic retinopathy occurs in more than half of the people who develop diabetes. It is possible to have diabetic retinopathy for a long time Causes: The primary cause of diabetic retinopathy is diabetes—a condition in without noticing symptoms until which the levels of glucose (sugar) in the blood are too high. Elevated sugar substantial damage has occurred. levels from diabetes can damage the small blood vessels that nourish the Symptoms of diabetic retinopathy retina and may, in some cases, block them completely. may occur in one or both eyes. When damaged blood vessels leak fluid into the retina it results in a Symptoms may include: condition known as diabetic macular edema which causes swelling in the • Blurred or double vision center part of the eye (macula) that provides the sharp vision needed for • Difficulty reading reading and recognizing faces. • The appearance of spots— Prolonged damage to the small blood vessels in the retina results in poor commonly called “floaters”— circulation to the retina and macula prompting the development of growth in your vision factors that cause new abnormal blood vessels (neovascularization) and scar • A shadow across the field of vision tissue to grow on the surface of the retina. -

Fact Sheet About Diabetic Macular Edema (Dme)
FACT SHEET ABOUT DIABETIC MACULAR EDEMA (DME) WHAT IS DME? Diabetic Macular Edema (DME) or "swelling of the macula" is a common complication in the eyes of patients with diabetes. It is a frequent cause of vision loss in patients with diabetes, and can eventually lead to blindness.1,2 The macula is the part of the retina responsible for central or fine vision. In DME, blood vessels in the retina are damaged by chronic high blood sugar levels. A breakdown in the blood-retinal barrier and increased vascular permeability allows fluid from blood vessels to leak into the retina, causing macular swelling.2 Fluid in the macula can cause severe vision loss or blindness.2 Vascular endothelial growth factor (VEGF), a naturally occurring family of growth factors in the body, appears to play a critical role in the development of DME.3 Increased VEGF production contributes to the vascular disruptions and leakage that characterize DME, as well as the formation of new blood vessels (a process known as angiogenesis) seen in more advanced forms of diabetic retinopathy (DR).2 DME STATISTICS According to the Centers for Disease Control and Prevention, approximately 29.1 million adults are living with diabetes (types I & II) in the U.S. 4 Of those, approximately 1.5 million people are diagnosed with DME.5 o The prevalence of DME is especially high among racial and ethnic minorities, particularly in African Americans.6 DME is the leading cause of blindness in young adults in developed countries.7 The increasing number of individuals with diabetes worldwide suggests that DME will continue to be a major contributor to vision loss and associated functional impairment. -
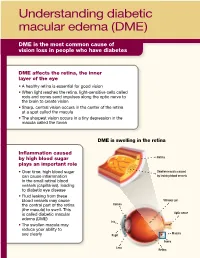
Understanding Diabetic Macular Edema (DME)
Understanding diabetic macular edema (DME) DME is the most common cause of vision loss in people who have diabetes DME affects the retina, the inner layer of the eye • A healthy retina is essential for good vision • When light reaches the retina, light-sensitive cells called rods and cones send impulses along the optic nerve to the brain to create vision • Sharp, central vision occurs in the center of the retina at a spot called the macula • The sharpest vision occurs in a tiny depression in the macula called the fovea DME is swelling in the retina Inflammation caused by high blood sugar Retina plays an important role • Over time, high blood sugar Swollen macula caused can cause inflammation by leaking blood vessels in the small retinal blood vessels (capillaries), leading to diabetic eye disease • Fluid leaking from these blood vessels may cause Vitreous gel Cornea the central part of the retina (the macula) to swell. This Optic nerve is called diabetic macular edema (DME) Iris • The swollen macula may reduce your ability to Macula see clearly Pupil Fovea Lens Retina Understanding DME (continued) Symptoms of DME • Early DME may not have any symptoms • As DME worsens, it can cause blurry central vision ranging from mild to severe • DME can cause significant vision loss over time How DME can affect vision Mild blurriness Moderate blurriness Severe blurriness Untreated DME can lead to vision loss • Talk to your doctor about treatment options • If you develop cataracts (hazy spots that can affect vision) in the lenses of your eyes, the natural lenses may be surgically removed and replaced with artificial ones • Having cataracts or artificial lenses can affect your treatment options ©2014 Allergan, Inc., Irvine, CA 92612 APC67SH14 141256. -

Dry Eye Syndrome in Type II Diabetic Patients Attending a Medical College Teaching Hospital
12 Ophthalmology and Allied Sciences Volume 4 Number 1, January - April 2018 Original Article DOI: http://dx.doi.org/10.21088/oas.2454.7816.4118.2 Dry Eye Syndrome in Type II Diabetic Patients Attending A Medical College Teaching Hospital Gnanajyothi C. Bada*, Satish S. Patil** *Assistant Professor, Department of Ophthalmology, Khaja Banda Nawaz Institute of Medical Sciences, Kalaburagi, Karnataka 585104, India. **Assistant ProfessorDepartment of Physiology, M R Medical College, Kalaburagi, Karnataka 585105, India. Abstract Introduction: Diabetes mellitus is one of the leading health problem all over the world. Dry eye syndrome (DES) is common in diabetes mellitus. The study was done to detect theprevalence of DES in type II diabetic patients and to determine the association of dry eyes with diabetic retinopathy. Methodology: Diabetic patients(n=200) attending Ophthalmology OPD at Khaja Bande Nawaz Institute of Medical Sciences (KBNIMS), Kalaburagi during the period fromApril to December 2017 were included in the study group, basedon the inclusion & exclusion criteria. Results: Our study showed that the prevalence of DES in diabetes was 51%, with higher rate in females and older age group. 33% of diabetic retinopathy patients had DES even though it was not statistically significant. Conclusion: Since there exists an association between diabetes and DES, all diabetic patients should be screened for DES to prevent ocular surface damage. Keywords: Diabetes Mellitus; Diabetic Retinopathy; Dry Eye Syndrome (DES). Introduction itchiness, redness, pain, ocular fatigue and visual disturbance [6]. DES results in corneal and conjunctival epithelial alterations such as punctate Diabetes mellitus is one of the leading health keratopathy, recurrent erosions, persistent epithelial problem all over the world [1]. -

Introduction to Micropulse for Central Serous Chorioretinopathy
Advertorial MicroPulse for Central Serous Chorioretinopathy Sponsored by Quantel Medical Introduction to MicroPulse for Central Serous Chorioretinopathy MicroPulse laser has become one of our hospital’s standard treatments for CSCR. BY PROF. DR. SASCHA FAUSER, MD I would like to introduce you to the principle of One of the challenges with MicroPulse laser treatment is MicroPulse laser therapy. that you cannot visualize any laser effect during the treatment, To understand MicroPulse laser technology, we must which could give you the feeling that the treatment is not effec- first understand conventional photocoagulation. tive. Overall, the problem is overtreating, but undertreatment With conventional photocoagulation, the laser trans- can also be an issue. To avoid undertreating, surgeons should fers energy to the retina. The longer the laser beam is on, the more apply dense treatment and focus the laser carefully. The yel- heat is generated. This heat may result in tissue damage by coagu- low 577 nm wavelength has an advantage in these situations lating the proteins. It is similar to how an egg loses its transparency because, due to its absorption characteristics, it can be titrated. when heat is applied to it. Basically, you apply the laser to the periphery of the edematous We do not yet know the exact mechanism of action of laser, but area (in a nonedematous area) on low power that is increased one hypothesis is that the damaged photoreceptors are replaced by gradually until a just-visible effect appears. Once the thermal glial cells, which have less oxygen consumption, less vascular endo- threshold is determined for a patient, you reduce the power to thelial growth factor, less edema, and less neovascularization. -

Effect of Glaucoma on Development of Diabetic Retinopathy in Long Standing Diabetics
Research Article Journal of Clinical Ophthalmology and Eye Disorders Published: 01 Mar, 2021 Effect of Glaucoma on Development of Diabetic Retinopathy in Long Standing Diabetics Anuj Kumar Singal* Department of Ophthalmology, JSS Medical College, India Abstract Aim: To compare the prevalence and severity of diabetic retinopathy in patients with glaucoma and compare it with patients without any evidence of glaucoma. Methods and Materials: In this retrospective observational study, a total of 70 diabetics with a history of diabetes since a minimum of ten years and under regular treatment presenting to the ophthalmology OPD were taken for the study. The right eye was taken into the study. These 70 eyes of 70 patients underwent detailed ophthalmic examination and the presence or absences of retinopathy (as per Modified Airlie House classification of diabetic retinopathy) as well as severity of retinopathy and glaucoma were noted. Results: Mean age of the patients was 60.39 ± 10 years. Males were predominant in the study. Among the 70 eyes, 38 eyes were diagnosed with glaucoma. The remaining 32 eyes did not show any signs of glaucoma. The mean duration of diabetes was similar in both glaucomatous and non-glaucomatous patients (12.2 vs. 12.7 yrs). Most patients (63%) with glaucoma had no retinopathy changes and none of these patients had severe retinopathy. On the other hand, most patients without any signs of glaucoma were found to have some retinopathy changes (72%) with nearly half of them having severe retinopathy changes. This was statistically highly significant (p<0.0001). The Intraocular pressure was found to be lower in patients with retinopathy changes. -

Healthy Vision
Healthy Vision Watch out for your vision. Watch out for your vision! The National Eye Institute (NEI) conducts and supports research that leads to sight-saving treatments and plays a vital role in reducing vision loss and blindness. NEI is part of the National Institutes of Health (NIH), an agency of the U.S. Department of Health and Human Services. Healthy Vision | 1 Healthy Vision Watch out for your vision. Healthy Vision | 2 Healthy Vision | 3 Your vision is very important. Every year, millions of people have problems with their vision. Some of these problems cause permanent vision loss, even blindness. Some groups, such as Hispanics/Latinos and African Americans, are at a higher risk for vision loss because of their increased risk of diabetes, high blood pressure or high cholesterol. As people age, their risk also increases for eye diseases and conditions such as age-related macular degeneration, cataract, diabetic retinopathy, dry eye, glaucoma, and low vision. But there are steps you can take to protect your vision. This booklet discusses the importance of early detection of eye disease in adults and offers general information on eye health for you and your family. We often don’t appreciate what we have until it’s gone. Healthy Vision | 4 Lens Vitreous humor Pupil Macula Cornea Fovea Iris Optic nerve Retina Sclera How we see The eye has many parts that help create vision. For you to be able to see, light first passes through the cornea, the clear, dome- shaped surface that covers the front of the eye. The cornea bends, or refracts, the light entering the eye.