Normal Cells Neuron
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Strategies to Improve Nerve Regeneration After Radical Prostatectomy: a Narrative Review
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Institutional Research Information System University of Turin Strategies to improve nerve regeneration after radical prostatectomy: a narrative review Stefano Geuna 1, 2, Luisa Muratori1, 2, Federica Fregnan 1, 2, Matteo Manfredi4 , Riccardo Bertolo 3, 4 , Francesco Porpiglia4. 1 Department of Clinical and Biological Sciences, University of Turin, Orbassano (To), 10043, Italy. 2 Neuroscience Institute Cavalieri Ottolenghi (NICO), Orbassano (To), 10043, Italy. 3 Urological and Kidney Institute, Cleveland Clinic, Cleveland, OH, US. 4 Department of Oncology, University of Turin, Orbassano (To), 10043, Italy. Abstract Peripheral nerves are complex organs that spread throughout the entire human body. They are frequently affected by lesions not only as a result of trauma but also following radical tumor resection. In fact, despite the advancement in surgical techniques, such as nerve- sparing robot assisted radical prostatectomy, some degree of nerve injury may occur resulting in erectile dysfunction with significant impairment of the quality of life. The aim of this review is to provide an overview on the mechanisms of the regeneration of injured peripheral nerves and to describe the potential strategies to improve the regeneration process and the functional recovery. Yet, the recent advances in bio- engineering strategies to promote nerve regeneration in the urological field are outlined with a view on the possible future regenerative therapies which might ameliorate the functional outcome after radical prostatectomy. 1 Introduction Radical prostatectomy is the gold standard surgical treatment for organ-confined prostate cancer. The employment of innovative surgical technique such as nerve-sparing robot assisted radical prostatectomy allowed to magnify the anatomical field leading to a three- dimensional perspective obtained through the robotic lenses and a better anatomical knowledge. -
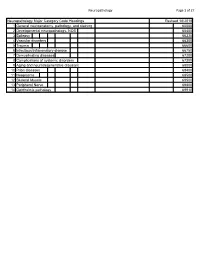
Neuropathology Category Code List
Neuropathology Page 1 of 27 Neuropathology Major Category Code Headings Revised 10/2018 1 General neuroanatomy, pathology, and staining 65000 2 Developmental neuropathology, NOS 65400 3 Epilepsy 66230 4 Vascular disorders 66300 5 Trauma 66600 6 Infectious/inflammatory disease 66750 7 Demyelinating diseases 67200 8 Complications of systemic disorders 67300 9 Aging and neurodegenerative diseases 68000 10 Prion diseases 68400 11 Neoplasms 68500 12 Skeletal Muscle 69500 13 Peripheral Nerve 69800 14 Ophthalmic pathology 69910 Neuropathology Page 2 of 27 Neuropathology 1 General neuroanatomy, pathology, and staining 65000 A Neuroanatomy, NOS 65010 1 Neocortex 65011 2 White matter 65012 3 Entorhinal cortex/hippocampus 65013 4 Deep (basal) nuclei 65014 5 Brain stem 65015 6 Cerebellum 65016 7 Spinal cord 65017 8 Pituitary 65018 9 Pineal 65019 10 Tracts 65020 11 Vascular supply 65021 12 Notochord 65022 B Cell types 65030 1 Neurons 65031 2 Astrocytes 65032 3 Oligodendroglia 65033 4 Ependyma 65034 5 Microglia and mononuclear cells 65035 6 Choroid plexus 65036 7 Meninges 65037 8 Blood vessels 65038 C Cerebrospinal fluid 65045 D Pathologic responses in neurons and axons 65050 1 Axonal degeneration/spheroid/reaction 65051 2 Central chromatolysis 65052 3 Tract degeneration 65053 4 Swollen/ballooned neurons 65054 5 Trans-synaptic neuronal degeneration 65055 6 Olivary hypertrophy 65056 7 Acute ischemic (hypoxic) cell change 65057 8 Apoptosis 65058 9 Protein aggregation 65059 10 Protein degradation/ubiquitin pathway 65060 E Neuronal nuclear inclusions 65100 -

OIICS Manual 2012
SECTION 2 Definitions, Rules of Selection, and Titles and Descriptions SECTION CONTENTS 2.1 Nature of Injury or Illness 2.2 Part of Body Affected 2.3 Source and Secondary Source of Injury or Illness 2.4 Event or Exposure *-Asterisks denote a summary level code not assigned to individual cases. _____________________________________________________________________________________________ 01/12 6 SECTION 2.1 Nature of Injury or Illness SECTION CONTENTS 2.1.1 Definition, Rules of Selection 2.1.2 Titles and Descriptions *-Asterisks denote a summary level code not assigned to individual cases. _____________________________________________________________________________________________ 01/12 7 2.1.1 Nature of Injury or Illness—Definition, Rules of Selection 1.0 DEFINITION The nature of injury or illness identifies the principal physical characteristic(s) of the work related injury or illness. RULES OF SELECTION: 1.1 Name the injury or illness indicated on the source document. Example: For strained back, choose Strains. 1.2 When two or more injuries or illnesses are indicated, and one is a sequela, aftereffect, complication due to medical treatment, or re-injury, choose the initial injury or illness. Example: If a laceration became infected developing into septicemia, choose Cuts, lacerations. 1.3 When two or more injuries or illnesses are indicated and one is more severe than the other(s) and is not a sequela or complication of the other injury or illness, select the more severe injury or illness. Example: For sprained finger and fractured wrist, choose Fractures. 1.3.1 When a single event or exposure produces an injury and transmits a disease simultaneously, and one is more severe than the other(s), select the more severe injury or disease. -

Novel Cryoneurolysis Device for the Treatment of Sensory and Motor Peripheral Nerves
UC San Diego UC San Diego Previously Published Works Title Novel cryoneurolysis device for the treatment of sensory and motor peripheral nerves. Permalink https://escholarship.org/uc/item/7s25k7xt Journal Expert review of medical devices, 13(8) ISSN 1743-4440 Authors Ilfeld, Brian M Preciado, Jessica Trescot, Andrea M Publication Date 2016-08-01 DOI 10.1080/17434440.2016.1204229 Peer reviewed eScholarship.org Powered by the California Digital Library University of California EXPERT REVIEW OF MEDICAL DEVICES, 2016 VOL. 13, NO. 8, 713–725 http://dx.doi.org/10.1080/17434440.2016.1204229 REVIEW Novel cryoneurolysis device for the treatment of sensory and motor peripheral nerves Brian M. Ilfelda, Jessica Preciadob and Andrea M. Trescotc aDepartment of Anesthesiology, University California San Diego, San Diego, CA, USA; bMyoscience, Inc., Fremont, CA, USA; cAlaska Pain Management Center, Wasilla, AK, USA ABSTRACT ARTICLE HISTORY Introduction: Cryoneurolysis is the direct application of low temperatures to reversibly ablate periph- Received 5 January 2016 eral nerves to provide pain relief. Recent development of a handheld cryoneurolysis device with small Accepted 17 June 2016 gauge probes and an integrated skin warmer broadens the clinical applications to include treatment of Published online superficial nerves, further enabling treatments for pre-operative pain, post-surgical pain, chronic pain, 13 July 2016 and muscle movement disorders. KEYWORDS Areas covered: Cryoneurolysis is the direct application of cold temperatures to a peripheral nerve, Cryoneurolysis; resulting in reversible ablation due to Wallerian degeneration and nerve regeneration. Use over the last cryoanalgesia; 50 years attests to a very low incidence of complications and adverse effects. -

OIICS Manual 2012
SECTION 4.1 Nature of Injury or Illness Index *-Asterisks denote a summary level code not assigned to individual cases. _____________________________________________________________________________________________ 01/12 447 NATURE CODE INDEX A 2831 Acne 2831 Acne varioliformis 3221 Abacterial meningitis 3211 Acquired immune deficiency syndrome 253 Abdominal hernia from repeated exertions (AIDS)—diagnosed 124 Abdominal hernia from single or short term 3199 Actinomycotic infections exertion 2819 Acute abscess of lymph gland or node 5174 Abdominal pain, unspecified 2359 Acute and subacute endocarditis 521 Abnormal blood-gas level 241 Acute bronchitis and bronchiolitis 521 Abnormal blood-lead level 2341 Acute cor pulmonale 525 Abnormal electrocardiogram (EKG, ECG), 195* Acute dermatitis electroencephalogram (EEG), 2819 Acute lymphadenitis electroretinogram (ERG) 2351 Acute myocarditis 52* Abnormal findings 2359 Acute pericarditis 521 Abnormal findings from examination of 2342 Acute pulmonary artery or vein embolism, blood nontraumatic 522 Abnormal findings from examination of 241 Acute respiratory infections (including urine common cold) 525 Abnormal findings from function studies 2422 Adenoids—chronic condition 526* Abnormal findings from histological and 6212 Adjustment disorder immunological studies 1731 Aero-otitis media 5269 Abnormal findings from histological and 1732 Aero-sinusitis immunological studies, n.e.c. 21 Agranulocytosis and neutropenia 5260 Abnormal findings from histological and 3212 AIDS-like syndrome immunological studies, unspecified 3212 AIDS-related complex (ARC) 523 Abnormal findings from body 3211 AIDS (acquired immune deficiency substances other than blood and urine syndrome)—diagnosed 524 Abnormal findings from radiological and 399 Ainhum other examination of body structure 1733 Air or gas embolisms due to diving 520 Abnormal findings, unspecified 1738 Air pressure effects, multiple 5129 Abnormal gait 1739 Air pressure effects, n.e.c. -
Trauma to the Nervous System (Dr. Merchut) 1. Pathophysiology Of
Trauma to the Nervous System (Dr. Merchut) 1. Pathophysiology of head trauma A more diffuse force applied to the skull typically produces a linear skull fracture, while a more focal or localized force causes a depressed skull fracture. A severe skull fracture may be associated with an underlying contusion (bruise) or laceration of the brain. Fractures at the skull base, face or orbit can entrap or compress cranial nerves. Leakage of cerebrospinal fluid (CSF) from the ear or nose may signal a greater risk of infection developing in the CSF or brain itself. Treatment involves surgical removal of bone fragments and debris, and closure of any dural tears. Brain contusions are superficial hemorrhages at the tops of cortical gyri, near the point of impact (coup) or more remotely in the brain (contrecoup) from movement of the brain within the skull. They occur most often at the basal or ventral surfaces of the frontal and anterior temporal lobes (Figure 1), where the bony skull is roughened (orbital surface of frontal bone) or protuberant (edges of sphenoidal wings). Brain contusions are caused by angular or rotational, not linear, acceleration of the brain (which explains why the woodpecker survives without brain injury). Figure 1. Frequency distribution of brain contusions. Individual cases are outlined and superimposed. (From Gurdjian ES. J Trauma 16[1]:35-51, 1976.) © Dr. Michael P. Merchut Page 1 1/23/2014 Contusions or more severe intracranial hemorrhages are often associated with brain edema, due to local metabolic or ischemic processes in addition to the presence of blood. Increased intracranial pressure (ICP) decreases cerebral blood flow, creating ischemia, and compensatory cerebral autoregulation eventually fails if the edema progresses. -
Spinal Cord Injury (SCI) Is Damage Or Trauma to the Spinal Cord That Results in a Loss Or Impaired Function Causing Reduced Mobility Or Feeling
A Spinal Cord Injury (SCI) is damage or trauma to the spinal cord that results in a loss or impaired function causing reduced mobility or feeling. Common causes of damage are trauma (car accident, gunshot, falls, sports injuries, etc.) or disease (Transverse Myelitis, Polio, Spina Bifida, Friedreich's Ataxia, etc.). The spinal cord does not have to be severed in order for a loss of functioning to occur. In most people with SCI, the spinal cord is intact, but the cellular damage to it results in loss of functioning. SCI is very different from back injuries such as ruptured disks, spinal stenosis or pinched nerves. It is possible for a person to "break their back or neck" yet not sustain a spinal cord injury as long as only the bones (the vertebrae) around the spinal cord are damaged, but the spinal cord is not affected. In these cases, the person may not experience paralysis after the vertebrae are stabilized. What is the spinal Spinal cord injury (SCI) refers to an injury to the spinal cord. It can cause myelopathy or damage to nerve roots or myelinated fiber tracts that carry signals to and from the brain.[1][2 Please read: A personal appeal from Wikipedia founder Jimmy Wales Spinal cord injury From Wikipedia, the free encyclopedia Jump to: navigation, search This article has multiple issues. Please help improve it or discuss these issues on the talk page. It is missing citations or footnotes. Please help improve it by adding inline citations. Tagged since September 2010. It may require general cleanup to meet Wikipedia's quality standards. -

Evaluating the Use of Engineered Nervous Tissue Constructs in the Repair of Peripheral Nerve Lesions and Amputations
University of Pennsylvania ScholarlyCommons Publicly Accessible Penn Dissertations Spring 2010 Evaluating the Use of Engineered Nervous Tissue Constructs in the Repair of Peripheral Nerve Lesions and Amputations Niranjan Kameswaran University of Pennsylvania, [email protected] Follow this and additional works at: https://repository.upenn.edu/edissertations Part of the Bioelectrical and Neuroengineering Commons Recommended Citation Kameswaran, Niranjan, "Evaluating the Use of Engineered Nervous Tissue Constructs in the Repair of Peripheral Nerve Lesions and Amputations" (2010). Publicly Accessible Penn Dissertations. 171. https://repository.upenn.edu/edissertations/171 This paper is posted at ScholarlyCommons. https://repository.upenn.edu/edissertations/171 For more information, please contact [email protected]. Evaluating the Use of Engineered Nervous Tissue Constructs in the Repair of Peripheral Nerve Lesions and Amputations Abstract Severe trauma to the limbs can often result in the lesioning, or even amputation, of the underlying peripheral nerves. In these cases, endogenous neural repair mechanisms are compromised and a path to the end target may be lost, resulting in the need for surgical intervention. Current repair strategies are incapable of maintaining this regenerative pathway, or providing a bridge to a surrogate end target, often resulting in incomplete repair. This thesis describes the development and evaluation of a novel method of addressing peripheral nerve lesions and amputations that utilizes living tissue-engineered neural grafts. These grafts are created by the controlled mechanical separation of axons spanning integrated neuron populations in vitro, resulting in axon tracts spanning several centimeters in length. Techniques were developed to encapsulate and transplant these tracts, with the goal of providing structural and nutrient support, while minimizing macrophage infiltration. -

Occupational Injury and Illness Classification Manual
Occupational Injury and Illness Classification Manual U.S. Department of Labor Bureau of Labor Statistics December 1992 This document has been modified from its original state by using Adobe Acrobat to make it 508 compliant. 1/8/2009. THIS PAGE INTENTIONALLY LEFT BLANK i OCCUPATIONAL INJURY AND ILLNESS CLASSIFICATION MANUAL Table of Contents Section Page 1. Introduction to the Occupational Injury and Illness Classification Manual 1-1 2. Definitions, Rules of Selection, and Titles and Descriptions 2-1 2.1 Nature of Injury or Illness 2.1-1 2.1.1 Definition, Rules of Selection 2.1-2 2.1.2 Titles and Descriptions 2.1-3 2.2 Part of Body Affected 2.2-1 2.2.1 Definition, Rules of Selection 2.2-2 2.2.2 Titles and Descriptions 2.2-3 2.3 Source of Injury or Illness; Secondary Source of Injury or Illness 2.3-1 2.3.1 Source of Injury Definition, Rules of Selection 2.3-2 2.3.2 Secondary Source of Injury Definition, Rules of Selection 2.3-4 2.3.3 Titles and Descriptions 2.3-6 2.4 Event or Exposure 2.4-1 2.4.1 Definition, Rules of Selection 2.4-2 2.4.2 Titles and Descriptions 2.4-3 3. Code Titles 3-1 3.1 Nature of Injury or Illness 3.1-1 3.2 Part of Body Affected 3.2-1 3.3 Source of Injury or Illness; Secondary Source of Injury or Illness 3.3-1 3.4 Event or Exposure 3.4-1 4. -

2018 Oral Presentations PN 1. Time to Intervention Affecting Outcomes In
2018 Oral Presentations PN 1. Time to Intervention Affecting Outcomes in Pediatric Nerve Injuries following Supracondylar Humerus Fractures Megan E Friend, MD; Elizabeth A Newman, MD; Daniel Bracey, MD, PhD; Shea Comadoll, BS; Rebecca Senehi, BS; Zhongyu Li, MD, PhD Wake Forest, Winston-Salem, NC Introduction: Supracondylar humerus fractures are the most common pediatric elbow fractures, and nerve injury is a well-documented complication associated with these fractures. While most nerve injuries following supracondylar humerus fractures spontaneously resolve, other injuries require operative intervention by a nerve specialist. The aim of this study was to determine if time from injury to surgical intervention affects clinical outcomes in nerve injuries following pediatric supracondylar humerus fractures. Materials and Methods: We performed a retrospective chart review of pediatric patients treated by the senior author for nerve injuries following supracondylar humerus fractures between 2006 and 2016. Sixteen patients with nerve injury requiring surgical intervention were identified. Chart review was performed to identify date of injury, fracture pattern, time to intervention by the senior author, and neurologic outcomes. British Medical Research Council scores for muscle strength and sensation were used to gauge recovery. A correlation analysis was performed to determine the effect on time to intervention on neurologic recovery. Results: Average time to treatment by the senior author was 8.2 ± 5.5 mo. The majority of fractures in this group were Gartland type III supracondylar fractures (62.5%). The most commonly injured nerve was the ulnar (56%), followed by the median (31%), and radial (19%). Surgical indications included neuropathic pain, worsened neurologic exam after initial reduction, muscle atrophy, nerve conduction study findings, and lack of recovery at the time of referral. -

Imaging of Traumatic Brain Injury
Imaging of Traumatic Brain Injury Yoshimi Anzai, MD, MPH Professor of Radiology Director of Neuroradiology Director of Head and Neck Imaging Co-Director of the Radiology Health Service Research Section Department of Radiology University of Washington Seattle, Washington Kathleen R. Fink, MD Assistant Professor of Neuroradiology Department of Radiology Harborview Medical Center University of Washington Seattle, Washington Thieme New York " Stuttgart " Delhi " Rio de Janiero Thieme Medical Publishers, Inc. Important note:Medicine is an ever-changing science undergoing 333 Seventh Ave. continual development. Research and clinical experience are con New York, NY 10001 tinually expanding our knowledge, in particular our knowledge of proper treatment and drug therapy. Insofar as this book mentions Executive Editor: William Lamsback any dosage or application, readers may rest assured that the Managing Editor: J. Owen Zurhellen IV authors, editors, and publishers have made every effort to ensure Assistant Managing Editor: Heather Allen that such references are in accordance thewith state of knowledge Senior Vice President, Editorial and Electronic Product Development: at the time of production of the book. Cornelia Schulze Nevertheless, this does not involve, imply, or express any guar Production Editor: Sean Woznicki antee or responsibility on the part of the publishers in respect to any International Production Director: Andreas Schabert dosage instructions and forms of applications stated in the book. International Marketing Director: Fiona Henderson Every user is requested to examine thecarefully manufacturers ’ Director of Sales, North America: Mike Roseman leaflets accompanying each drug and to check, if necessary in con International Sales Director: Louisa Turrell sultation with a physician or specialist, whether the dosage sche Vice President, Finance and Accounts: Sarah Vanderbilt dules mentioned therein or the contraindications stated by the President: Brian D. -

Nerve Ultrasound in Traumatic and Iatrogenic Peripheral Nerve Injury
diagnostics Review Nerve Ultrasound in Traumatic and Iatrogenic Peripheral Nerve Injury Juerd Wijntjes 1, Alexandra Borchert 2 and Nens van Alfen 1,* 1 Department of Neurology and Clinical Neurophysiology, Donders Institute for Brain, Cognition and Behavior, Radboud University Medical Center, 6500 HB Nijmegen, The Netherlands; [email protected] 2 Nervenultraschall Euregio, Pauwelsklinik, 52064 Aachen, Germany; [email protected] * Correspondence: [email protected]; Tel.: +31-24-3616600 Abstract: Peripheral nerve injury is a potentially debilitating disorder that occurs in an estimated 2–3% of all patients with major trauma, in a similar percentage of medical procedures. The workup of these injuries has traditionally been clinical, combined with electrodiagnostic testing. However, this has limitations, especially in the acute phase of the trauma or lack of any recovery, when it is very important to determine nerve continuity and perform surgical exploration and repair in the case of the complete transection or intraneural fibrosis. Ultrasound can help in those situations. It is a versatile imaging technique with a high sensitivity of 93% for detecting focal nerve lesions. Ultrasound can assess the structural integrity of the nerve, neuroma formation and other surrounding abnormalities of bone or foreign bodies impeding the nerve. In addition, this can help to prevent iatrogenic nerve injury by marking the nerve before the procedure. This narrative review gives an overview of why and how nerve ultrasound can play a role in the detection, management and prevention of peripheral nerve injury. Keywords: peripheral nerve; fascicle; nerve injury; nerve trauma; nerve ultrasound; ultrasonography; imaging; neuroma; iatrogenic; nerve surgery Citation: Wijntjes, J.; Borchert, A.; van 1.