Immersion Course Lecture Kelly
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Regulation of the Mammalian Target of Rapamycin Complex 2 (Mtorc2)
Regulation of the Mammalian Target Of Rapamycin Complex 2 (mTORC2) Inauguraldissertation Zur Erlangung der Würde eines Doktors der Philosophie vorgelegt der Philosophisch-Naturwissenschaftlichen Fakultät der Universität Basel von Klaus-Dieter Molle aus Heilbronn, Deutschland Basel, 2006 Genehmigt von der Philosophisch-Naturwissenschaftlichen Fakultät Auf Antrag von Prof. Michael N. Hall und Prof. Markus Affolter. Basel, den 21.11.2006 Prof. Hans-Peter Hauri Dekan Summary The growth controlling mammalian Target of Rapamycin (mTOR) is a conserved Ser/Thr kinase found in two structurally and functionally distinct complexes, mTORC1 and mTORC2. The tumor suppressor TSC1-TSC2 complex inhibits mTORC1 by acting on the small GTPase Rheb, but the role of TSC1-TSC2 and Rheb in the regulation of mTORC2 is unclear. Here we examined the role of TSC1-TSC2 in the regulation of mTORC2 in human embryonic kidney 293 cells. Induced knockdown of TSC1 and TSC2 (TSC1/2) stimulated mTORC2-dependent actin cytoskeleton organization and Paxillin phosphorylation. Furthermore, TSC1/2 siRNA increased mTORC2-dependent Ser473 phosphorylation of plasma membrane bound, myristoylated Akt/PKB. This suggests that loss of Akt/PKB Ser473 phosphorylation in TSC mutant cells, as reported previously, is due to inhibition of Akt/PKB localization rather than inhibition of mTORC2 activity. Amino acids and overexpression of Rheb failed to stimulate mTORC2 signaling. Thus, TSC1-TSC2 also inhibits mTORC2, but possibly independently of Rheb. Our results suggest that mTORC2 hyperactivation may contribute to the pathophysiology of diseases such as cancer and Tuberous Sclerosis Complex. i Acknowledgement During my PhD studies in the Biozentrum I received a lot of support from many people around me who I mention here to express my gratefulness. -

Lymphocyte/WBC-Based Comprehensive Testing Via Next-Gen Sequencing NF1/SPRED1 and Other Rasopathy Related Conditions on Blood/Saliva
Last Updated October 2019 Institutional Price TAT Genetic Test CPT Codes Z codes Specimen Requirements (USD$) (working days) Lymphocyte/WBC-based Comprehensive Testing via Next-Gen Sequencing NF1/SPRED1 and Other RASopathy Related Conditions on Blood/Saliva NF1- only NGS testing and copy number analysis for the NF1 gene (NF1-NG) This testing includes an average coverage of >1600x to allow for the identification of (1) 3-6ml whole blood in EDTA (purple topped) tubes mosaicism as low as 3-5% of the alleles. In addition, novel variants identified in the $1,000 81408 25 (2) Oragene 575 saliva kit (provided by the MGL) ZB6A9 NF1 gene will be confirmed via RNA-based analysis at no additional charge. RNA- $1,600 (RUSH) 81479 15 (RUSH) (3) DNA sample (25ul volume at 3ug, O.D. value at based testing will also be provided to non-founder, multigenerational families with 260:280 ≥1.8) “classic” NF1 at no additional charge if next-generation sequencing is found negative. (1) 3-6ml whole blood in EDTA (purple topped) tubes SPRED1-only NGS testing and copy number analysis for SPRED1 (SPD1-NG) $800 81405 25 (2) Oragene 575 saliva kit (provided by the MGL) This testing includes an average coverage of >1600x to allow for the identification of ZB6AC $1,400 (RUSH) 81479 15 (RUSH) (3) DNA sample (25ul volume at 3ug, O.D. value at mosaicism as low as 3-5% of the alleles after comprehensive NF1 analysis. 260:280 ≥1.8) NF1/SPRED1 NGS testing and copy number analysis for NF1 and SPRED1 (NFSP-NG) (1) 3-6ml whole blood in EDTA (purple topped) tubes 81408 This testing includes an average coverage of >1600x to allow for the identification of $1,100 25 (2) Oragene 575 saliva kit (provided by the MGL) 81405 ZB6A8 mosaicism as low as 3-5% of the alleles. -

Related Malignant Phenotypes in the Nf1-Deficient MPNST
Published OnlineFirst February 19, 2013; DOI: 10.1158/1541-7786.MCR-12-0593 Molecular Cancer Genomics Research RAS/MEK–Independent Gene Expression Reveals BMP2- Related Malignant Phenotypes in the Nf1-Deficient MPNST Daochun Sun1, Ramsi Haddad2,3, Janice M. Kraniak2, Steven D. Horne1, and Michael A. Tainsky1,2 Abstract Malignant peripheral nerve sheath tumor (MPNST) is a type of soft tissue sarcoma that occurs in carriers of germline mutations in Nf1 gene as well as sporadically. Neurofibromin, encoded by the Nf1 gene, functions as a GTPase-activating protein (GAP) whose mutation leads to activation of wt-RAS and mitogen-activated protein kinase (MAPK) signaling in neurofibromatosis type I (NF1) patients' tumors. However, therapeutic targeting of RAS and MAPK have had limited success in this disease. In this study, we modulated NRAS, mitogen-activated protein/extracellular signal–regulated kinase (MEK)1/2, and neurofibromin levels in MPNST cells and determined gene expression changes to evaluate the regulation of signaling pathways in MPNST cells. Gene expression changes due to neurofibromin modulation but independent of NRAS and MEK1/2 regulation in MPNST cells indicated bone morphogenetic protein 2 (Bmp2) signaling as a key pathway. The BMP2-SMAD1/5/8 pathway was activated in NF1-associated MPNST cells and inhibition of BMP2 signaling by LDN-193189 or short hairpin RNA (shRNA) to BMP2 decreased the motility and invasion of NF1-associated MPNST cells. The pathway-specific gene changes provide a greater understanding of the complex role of neurofibromin in MPNST pathology and novel targets for drug discovery. Mol Cancer Res; 11(6); 616–27. -

TSC1/TSC2 Signaling in the CNS ⇑ Juliette M
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Elsevier - Publisher Connector FEBS Letters 585 (2011) 973–980 journal homepage: www.FEBSLetters.org Review TSC1/TSC2 signaling in the CNS ⇑ Juliette M. Han, Mustafa Sahin The F.M. Kirby Neurobiology Center, Department of Neurology, Children’s Hospital Boston, Harvard Medical School, Boston, MA 02115, USA article info abstract Article history: Over the past several years, the study of a hereditary tumor syndrome, tuberous sclerosis complex Received 5 January 2011 (TSC), has shed light on the regulation of cellular proliferation and growth. TSC is an autosomal Revised 1 February 2011 dominant disorder that is due to inactivating mutations in TSC1 or TSC2 and characterized by benign Accepted 1 February 2011 tumors (hamartomas) involving multiple organ systems. The TSC1/2 complex has been found to play Available online 15 February 2011 a crucial role in an evolutionarily-conserved signaling pathway that regulates cell growth: the Edited by Wilhelm Just mTORC1 pathway. This pathway promotes anabolic processes and inhibits catabolic processes in response to extracellular and intracellular factors. Findings in cancer biology have reinforced the critical role for TSC1/2 in cell growth and proliferation. In contrast to cancer cells, in the CNS, the Keywords: mTOR TSC1/2 complex not only regulates cell growth/proliferation, but also orchestrates an intricate and Autism finely tuned system that has distinctive roles under different conditions, depending on cell type, Translation stage of development, and subcellular localization. Overall, TSC1/2 signaling in the CNS, via its multi-faceted roles, contributes to proper neural connectivity. -

Mtor: a Pharmacologic Target for Autophagy Regulation
mTOR: a pharmacologic target for autophagy regulation Young Chul Kim, Kun-Liang Guan J Clin Invest. 2015;125(1):25-32. https://doi.org/10.1172/JCI73939. Review mTOR, a serine/threonine kinase, is a master regulator of cellular metabolism. mTOR regulates cell growth and proliferation in response to a wide range of cues, and its signaling pathway is deregulated in many human diseases. mTOR also plays a crucial role in regulating autophagy. This Review provides an overview of the mTOR signaling pathway, the mechanisms of mTOR in autophagy regulation, and the clinical implications of mTOR inhibitors in disease treatment. Find the latest version: https://jci.me/73939/pdf The Journal of Clinical Investigation REVIEW SERIES: AUTOPHAGY Series Editor: Guido Kroemer mTOR: a pharmacologic target for autophagy regulation Young Chul Kim and Kun-Liang Guan Department of Pharmacology and Moores Cancer Center, UCSD, La Jolla, California, USA. mTOR, a serine/threonine kinase, is a master regulator of cellular metabolism. mTOR regulates cell growth and proliferation in response to a wide range of cues, and its signaling pathway is deregulated in many human diseases. mTOR also plays a crucial role in regulating autophagy. This Review provides an overview of the mTOR signaling pathway, the mechanisms of mTOR in autophagy regulation, and the clinical implications of mTOR inhibitors in disease treatment. Overview of mTOR signaling pathway such as insulin and IGF activate their cognate receptors (recep- Nutrients, growth factors, and cellular energy levels are key deter- tor tyrosine kinases [RTKs]) and subsequently activate the PI3K/ minants of cell growth and proliferation. mTOR, a serine/threon- AKT signaling axis. -
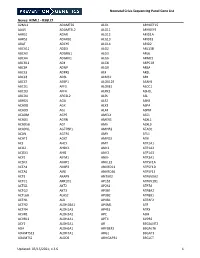
NICU Gene List Generator.Xlsx
Neonatal Crisis Sequencing Panel Gene List Genes: A2ML1 - B3GLCT A2ML1 ADAMTS9 ALG1 ARHGEF15 AAAS ADAMTSL2 ALG11 ARHGEF9 AARS1 ADAR ALG12 ARID1A AARS2 ADARB1 ALG13 ARID1B ABAT ADCY6 ALG14 ARID2 ABCA12 ADD3 ALG2 ARL13B ABCA3 ADGRG1 ALG3 ARL6 ABCA4 ADGRV1 ALG6 ARMC9 ABCB11 ADK ALG8 ARPC1B ABCB4 ADNP ALG9 ARSA ABCC6 ADPRS ALK ARSL ABCC8 ADSL ALMS1 ARX ABCC9 AEBP1 ALOX12B ASAH1 ABCD1 AFF3 ALOXE3 ASCC1 ABCD3 AFF4 ALPK3 ASH1L ABCD4 AFG3L2 ALPL ASL ABHD5 AGA ALS2 ASNS ACAD8 AGK ALX3 ASPA ACAD9 AGL ALX4 ASPM ACADM AGPS AMELX ASS1 ACADS AGRN AMER1 ASXL1 ACADSB AGT AMH ASXL3 ACADVL AGTPBP1 AMHR2 ATAD1 ACAN AGTR1 AMN ATL1 ACAT1 AGXT AMPD2 ATM ACE AHCY AMT ATP1A1 ACO2 AHDC1 ANK1 ATP1A2 ACOX1 AHI1 ANK2 ATP1A3 ACP5 AIFM1 ANKH ATP2A1 ACSF3 AIMP1 ANKLE2 ATP5F1A ACTA1 AIMP2 ANKRD11 ATP5F1D ACTA2 AIRE ANKRD26 ATP5F1E ACTB AKAP9 ANTXR2 ATP6V0A2 ACTC1 AKR1D1 AP1S2 ATP6V1B1 ACTG1 AKT2 AP2S1 ATP7A ACTG2 AKT3 AP3B1 ATP8A2 ACTL6B ALAS2 AP3B2 ATP8B1 ACTN1 ALB AP4B1 ATPAF2 ACTN2 ALDH18A1 AP4M1 ATR ACTN4 ALDH1A3 AP4S1 ATRX ACVR1 ALDH3A2 APC AUH ACVRL1 ALDH4A1 APTX AVPR2 ACY1 ALDH5A1 AR B3GALNT2 ADA ALDH6A1 ARFGEF2 B3GALT6 ADAMTS13 ALDH7A1 ARG1 B3GAT3 ADAMTS2 ALDOB ARHGAP31 B3GLCT Updated: 03/15/2021; v.3.6 1 Neonatal Crisis Sequencing Panel Gene List Genes: B4GALT1 - COL11A2 B4GALT1 C1QBP CD3G CHKB B4GALT7 C3 CD40LG CHMP1A B4GAT1 CA2 CD59 CHRNA1 B9D1 CA5A CD70 CHRNB1 B9D2 CACNA1A CD96 CHRND BAAT CACNA1C CDAN1 CHRNE BBIP1 CACNA1D CDC42 CHRNG BBS1 CACNA1E CDH1 CHST14 BBS10 CACNA1F CDH2 CHST3 BBS12 CACNA1G CDK10 CHUK BBS2 CACNA2D2 CDK13 CILK1 BBS4 CACNB2 CDK5RAP2 -

Abnormal Protein Phosphorylation in Human Amyotrophic Lateral Sclerosis
ABNORMAL PROTEIN PHOSPHORYLATION IN HUMAN AMYOTROPHIC LATERAL SCLEROSIS Jie Hong Hu B.Sc., Zhongshan (Sun Yat-sen) University, 1993 M.Sc., Zhongshan (Sun Yat-sen) University, 1996 THESIS SUBMITTED IN PARTIAL FULFILLMENT OF THE REQUIREMENTS FOR THE DEGREE OF DOCTOR OF PHILOSOPHY In the School of KINESIOLOGY O Jie Hong Hu, 2003 SIMON FRASER UNIVERSITY September, 2003 All rights reserved. This work may not be reproduced in whole or in part, by photocopy or other means, without permission of the author. APPROVAL NAME: Jie Hong Hu DEGREE: Doctor of Philosophy TITLE OF THESIS: Abnormal protein phosphorylation in human amyotrophic lateral sclerosis (ALS) EXAMINING COMMITTEE: Chair: Dr. Parveen Bawa Professor Dr. Charles krieger Senior Supervisor Professor, School of Kinesiology BimeUraser University Dr. Wade Parkhouse Supervisor Professor, School of Kinesiology Simon Fraser University - Dr. Nick Harden Internal Examiner Assistant Professor, Department Molecular Biology and Biochemstry Simon Fraser University ~r.6rDurham External Examiner Professor, Department Neurology/Neurosurgery McGill University Date Approved: 16"' September 2003 PARTIAL COPYRIGHT LICENCE I hereby grant to Simon Fraser University the right to lend my thesis, project or extended essay (the title of which is shown below) to users of the Simon Fraser University Library, and to make partial or single copies only for such users or in response to a request from the library of any other university, or other educational institution, on its own behalf or for one of its users. I further agree that permission for multiple copying of this work for scholarly purposes may be granted by me or the Dean of Graduate Studies. It is understood that copying or publication of this work for financial gain shall not be allowed without my written permission. -

Mutational Spectrum of the TSC1 Gene in a Cohort of 225 Tuberous Sclerosis Complex Patients: J Med Genet: First Published As 10.1136/Jmg.36.4.285 on 1 April 1999
J Med Genet 1999;36:285–289 285 Mutational spectrum of the TSC1 gene in a cohort of 225 tuberous sclerosis complex patients: J Med Genet: first published as 10.1136/jmg.36.4.285 on 1 April 1999. Downloaded from no evidence for genotype-phenotype correlation Marjon van Slegtenhorst, Senno Verhoef, Anita Tempelaars, Lida Bakker, Qi Wang, Marja Wessels, Remco Bakker, Mark Nellist, Dick Lindhout, Dicky Halley, Ans van den Ouweland Abstract TSC1 locus on chromosome 9q34 and the Tuberous sclerosis complex is an inherited other half to the TSC2 locus on chromosome tumour suppressor syndrome, caused by a 16p13.67 The TSC1 and TSC2 genes were mutation in either the TSC1 or TSC2 identified by positional cloning89 and there is gene. The disease is characterised by a abundant evidence that both genes act as broad phenotypic spectrum that can in- tumour suppressor genes.10–13 clude seizures, mental retardation, renal The TSC2 gene consists of 41 exons, dysfunction, and dermatological abnor- spanning 43 kb of genomic DNA.14 It encodes malities. The TSC1 gene was recently a 200 kDa protein, tuberin, which has a identified and has 23 exons, spanning 45 putative GAP activity for rab515 and rap1,16 two kb of genomic DNA, and encoding an 8.6 members of the ras superfamily of small kb mRNA. After screening all 21 coding GTPases. The mutational spectrum of TSC2 exons in our collection of 225 unrelated includes a number of large deletions often dis- 17 18 patients, only 29 small mutations were rupting the PKD1 gene as well, but also 19–27 detected, suggesting that TSC1 mutations point mutations and a number of missense 28 are under-represented among TSC pa- changes. -

Whole Exome Sequencing in Families at High Risk for Hodgkin Lymphoma: Identification of a Predisposing Mutation in the KDR Gene
Hodgkin Lymphoma SUPPLEMENTARY APPENDIX Whole exome sequencing in families at high risk for Hodgkin lymphoma: identification of a predisposing mutation in the KDR gene Melissa Rotunno, 1 Mary L. McMaster, 1 Joseph Boland, 2 Sara Bass, 2 Xijun Zhang, 2 Laurie Burdett, 2 Belynda Hicks, 2 Sarangan Ravichandran, 3 Brian T. Luke, 3 Meredith Yeager, 2 Laura Fontaine, 4 Paula L. Hyland, 1 Alisa M. Goldstein, 1 NCI DCEG Cancer Sequencing Working Group, NCI DCEG Cancer Genomics Research Laboratory, Stephen J. Chanock, 5 Neil E. Caporaso, 1 Margaret A. Tucker, 6 and Lynn R. Goldin 1 1Genetic Epidemiology Branch, Division of Cancer Epidemiology and Genetics, National Cancer Institute, NIH, Bethesda, MD; 2Cancer Genomics Research Laboratory, Division of Cancer Epidemiology and Genetics, National Cancer Institute, NIH, Bethesda, MD; 3Ad - vanced Biomedical Computing Center, Leidos Biomedical Research Inc.; Frederick National Laboratory for Cancer Research, Frederick, MD; 4Westat, Inc., Rockville MD; 5Division of Cancer Epidemiology and Genetics, National Cancer Institute, NIH, Bethesda, MD; and 6Human Genetics Program, Division of Cancer Epidemiology and Genetics, National Cancer Institute, NIH, Bethesda, MD, USA ©2016 Ferrata Storti Foundation. This is an open-access paper. doi:10.3324/haematol.2015.135475 Received: August 19, 2015. Accepted: January 7, 2016. Pre-published: June 13, 2016. Correspondence: [email protected] Supplemental Author Information: NCI DCEG Cancer Sequencing Working Group: Mark H. Greene, Allan Hildesheim, Nan Hu, Maria Theresa Landi, Jennifer Loud, Phuong Mai, Lisa Mirabello, Lindsay Morton, Dilys Parry, Anand Pathak, Douglas R. Stewart, Philip R. Taylor, Geoffrey S. Tobias, Xiaohong R. Yang, Guoqin Yu NCI DCEG Cancer Genomics Research Laboratory: Salma Chowdhury, Michael Cullen, Casey Dagnall, Herbert Higson, Amy A. -

The Role of the Rho Gtpases in Neuronal Development
Downloaded from genesdev.cshlp.org on September 24, 2021 - Published by Cold Spring Harbor Laboratory Press REVIEW The role of the Rho GTPases in neuronal development Eve-Ellen Govek,1,2, Sarah E. Newey,1 and Linda Van Aelst1,2,3 1Cold Spring Harbor Laboratory, Cold Spring Harbor, New York, 11724, USA; 2Molecular and Cellular Biology Program, State University of New York at Stony Brook, Stony Brook, New York, 11794, USA Our brain serves as a center for cognitive function and and an inactive GDP-bound state. Their activity is de- neurons within the brain relay and store information termined by the ratio of GTP to GDP in the cell and can about our surroundings and experiences. Modulation of be influenced by a number of different regulatory mol- this complex neuronal circuitry allows us to process that ecules. Guanine nucleotide exchange factors (GEFs) ac- information and respond appropriately. Proper develop- tivate GTPases by enhancing the exchange of bound ment of neurons is therefore vital to the mental health of GDP for GTP (Schmidt and Hall 2002); GTPase activat- an individual, and perturbations in their signaling or ing proteins (GAPs) act as negative regulators of GTPases morphology are likely to result in cognitive impairment. by enhancing the intrinsic rate of GTP hydrolysis of a The development of a neuron requires a series of steps GTPase (Bernards 2003; Bernards and Settleman 2004); that begins with migration from its birth place and ini- and guanine nucleotide dissociation inhibitors (GDIs) tiation of process outgrowth, and ultimately leads to dif- prevent exchange of GDP for GTP and also inhibit the ferentiation and the formation of connections that allow intrinsic GTPase activity of GTP-bound GTPases (Zalc- it to communicate with appropriate targets. -

Structural, Biochemical, and Cell Biological Characterization of Rab7 Mutants That Cause Peripheral Neuropathy
University of Pennsylvania ScholarlyCommons Publicly Accessible Penn Dissertations Spring 2010 Structural, Biochemical, and Cell Biological Characterization of Rab7 Mutants That Cause Peripheral Neuropathy Brett A. McCray University of Pennsylvania, [email protected] Follow this and additional works at: https://repository.upenn.edu/edissertations Part of the Molecular and Cellular Neuroscience Commons Recommended Citation McCray, Brett A., "Structural, Biochemical, and Cell Biological Characterization of Rab7 Mutants That Cause Peripheral Neuropathy" (2010). Publicly Accessible Penn Dissertations. 145. https://repository.upenn.edu/edissertations/145 This paper is posted at ScholarlyCommons. https://repository.upenn.edu/edissertations/145 For more information, please contact [email protected]. Structural, Biochemical, and Cell Biological Characterization of Rab7 Mutants That Cause Peripheral Neuropathy Abstract Coordinated trafficking of intracellular vesicles is of critical importance for the maintenance of cellular health and homeostasis. Members of the Rab GTPase family serve as master regulators of vesicular trafficking, maturation, and fusion by reversibly associating with distinct target membranes and recruiting specific effector proteins. Rabs act as molecular switches by cycling between an active, GTP-bound form and an inactive, GDP-bound form. The activity cycle is coupled to GTP hydrolysis and is tightly controlled by regulatory proteins such as guanine nucleotide exchange factors and GTPase activating proteins. Rab7 specifically regulates the trafficking and maturation of vesicle populations that are involved in protein degradation including late endosomes, lysosomes, and autophagic vacuoles. Missense mutations of Rab7 cause a dominantly-inherited axonal degeneration known as Charcot-Marie-Tooth type 2B (CMT2B) through an unknown mechanism. Patients with CMT2B present with length-dependent degeneration of peripheral sensory and motor neurons that leads to weakness and profound sensory loss. -
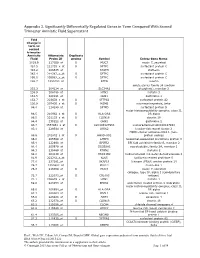
Appendix 2. Significantly Differentially Regulated Genes in Term Compared with Second Trimester Amniotic Fluid Supernatant
Appendix 2. Significantly Differentially Regulated Genes in Term Compared With Second Trimester Amniotic Fluid Supernatant Fold Change in term vs second trimester Amniotic Affymetrix Duplicate Fluid Probe ID probes Symbol Entrez Gene Name 1019.9 217059_at D MUC7 mucin 7, secreted 424.5 211735_x_at D SFTPC surfactant protein C 416.2 206835_at STATH statherin 363.4 214387_x_at D SFTPC surfactant protein C 295.5 205982_x_at D SFTPC surfactant protein C 288.7 1553454_at RPTN repetin solute carrier family 34 (sodium 251.3 204124_at SLC34A2 phosphate), member 2 238.9 206786_at HTN3 histatin 3 161.5 220191_at GKN1 gastrokine 1 152.7 223678_s_at D SFTPA2 surfactant protein A2 130.9 207430_s_at D MSMB microseminoprotein, beta- 99.0 214199_at SFTPD surfactant protein D major histocompatibility complex, class II, 96.5 210982_s_at D HLA-DRA DR alpha 96.5 221133_s_at D CLDN18 claudin 18 94.4 238222_at GKN2 gastrokine 2 93.7 1557961_s_at D LOC100127983 uncharacterized LOC100127983 93.1 229584_at LRRK2 leucine-rich repeat kinase 2 HOXD cluster antisense RNA 1 (non- 88.6 242042_s_at D HOXD-AS1 protein coding) 86.0 205569_at LAMP3 lysosomal-associated membrane protein 3 85.4 232698_at BPIFB2 BPI fold containing family B, member 2 84.4 205979_at SCGB2A1 secretoglobin, family 2A, member 1 84.3 230469_at RTKN2 rhotekin 2 82.2 204130_at HSD11B2 hydroxysteroid (11-beta) dehydrogenase 2 81.9 222242_s_at KLK5 kallikrein-related peptidase 5 77.0 237281_at AKAP14 A kinase (PRKA) anchor protein 14 76.7 1553602_at MUCL1 mucin-like 1 76.3 216359_at D MUC7 mucin 7,