Trichothiodystrophy
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

De Barsy Syndrome: Orthopedic Case Report and Literature Review
MOJ Orthopedics & Rheumatology De Barsy Syndrome: Orthopedic Case report and Literature Review Introduction Case Report Volume 7 Issue 5 - 2017 This condition was first described in 1968 by De Barsy who and degeneration of the elastic tissue of the cornea and skin, Jose de Jesus Guerra Jasso1*, Douglas reported a case of a patient with progeria, dwarfism, oligofrenia and since then, it is known as Barsy Syndrome or Barsy- Colmenares Bonilla2 and Loreett Ocampo Perez3 of progeroid aspect, cutis laxa, corneal opacity, intrauterine 1Pediatric Orthopedics, Hospital Regional de Alta Especialidad growthMoens-Dierckx retardation Syndrome. and severe This ismental defined retardation as the combination (although del Bajio, Mexico some will learn to speak, intelligence is less than normal) [1]. 2Pediatric Orthopedic Service, Hospital regional de alta especialidad del bajio The orthopedic manifestations are dysplasia of hip development, 3Fellow of Pediatric Orthopedics, Hospital Regional de Alta hyper laxity of severe joints, athetoid movements, scoliosis and Especialidad del Bajio, Mexico severe deformities of the foot. Epidemiology in Latin America is unknown because of its underdiagnosis and when confused *Corresponding author: Jesus Guerra Jasso, Hospital with other connective tissue pathologies (Hutchinson-Gilford Regional de Alta Especialidad del Bajio, Boulevard Milenio No. 130. Col, San Carlos la Roncha, C.P. 37660, Guanajuato, syndrome, gerodermic osteodiplasia, even Ehlers-Danlos), the Mexico, Tel: 477-267 2000; Ext-1403; life expectancy of these patients varies according to the degree of Email: penetrance and in the world literature, there are very few reports (about 50), so the diagnosis requires a challenge [2]. Received: January 13, 2017 | Published: March 21, 2017 Clinical Case and thick clamp. -

Open Full Page
CCR PEDIATRIC ONCOLOGY SERIES CCR Pediatric Oncology Series Recommendations for Childhood Cancer Screening and Surveillance in DNA Repair Disorders Michael F. Walsh1, Vivian Y. Chang2, Wendy K. Kohlmann3, Hamish S. Scott4, Christopher Cunniff5, Franck Bourdeaut6, Jan J. Molenaar7, Christopher C. Porter8, John T. Sandlund9, Sharon E. Plon10, Lisa L. Wang10, and Sharon A. Savage11 Abstract DNA repair syndromes are heterogeneous disorders caused by around the world to discuss and develop cancer surveillance pathogenic variants in genes encoding proteins key in DNA guidelines for children with cancer-prone disorders. Herein, replication and/or the cellular response to DNA damage. The we focus on the more common of the rare DNA repair dis- majority of these syndromes are inherited in an autosomal- orders: ataxia telangiectasia, Bloom syndrome, Fanconi ane- recessive manner, but autosomal-dominant and X-linked reces- mia, dyskeratosis congenita, Nijmegen breakage syndrome, sive disorders also exist. The clinical features of patients with DNA Rothmund–Thomson syndrome, and Xeroderma pigmento- repair syndromes are highly varied and dependent on the under- sum. Dedicated syndrome registries and a combination of lying genetic cause. Notably, all patients have elevated risks of basic science and clinical research have led to important in- syndrome-associated cancers, and many of these cancers present sights into the underlying biology of these disorders. Given the in childhood. Although it is clear that the risk of cancer is rarity of these disorders, it is recommended that centralized increased, there are limited data defining the true incidence of centers of excellence be involved directly or through consulta- cancer and almost no evidence-based approaches to cancer tion in caring for patients with heritable DNA repair syn- surveillance in patients with DNA repair disorders. -

EXTENDED CARRIER SCREENING Peace of Mind for Planned Pregnancies
Focusing on Personalised Medicine EXTENDED CARRIER SCREENING Peace of Mind for Planned Pregnancies Extended carrier screening is an important tool for prospective parents to help them determine their risk of having a child affected with a heritable disease. In many cases, parents aren’t aware they are carriers and have no family history due to the rarity of some diseases in the general population. What is covered by the screening? Genomics For Life offers a comprehensive Extended Carrier Screening test, providing prospective parents with the information they require when planning their pregnancy. Extended Carrier Screening has been shown to detect carriers who would not have been considered candidates for traditional risk- based screening. With a simple mouth swab collection, we are able to test for over 419 genes associated with inherited diseases, including Fragile X Syndrome, Cystic Fibrosis and Spinal Muscular Atrophy. The assay has been developed in conjunction with clinical molecular geneticists, and includes genes listed in the NIH Genetic Test Registry. For a list of genes and disorders covered, please see the reverse of this brochure. If your gene of interest is not covered on our Extended Carrier Screening panel, please contact our friendly team to assist you in finding a gene test panel that suits your needs. Why have Extended Carrier Screening? Extended Carrier Screening prior to pregnancy enables couples to learn about their reproductive risk and consider a complete range of reproductive options, including whether or not to become pregnant, whether to use advanced reproductive technologies, such as preimplantation genetic diagnosis, or to use donor gametes. -

The Progeria Syndrome Fact Sheet
HUTCHINSON-GILFORD PROGERIA SYNDROME FREQUENTLY ASKED QUESTIONS WHAT IS PROGERIA? Hutchinson-Gilford Progeria Syndrome “Progeria” or “HGPS” is a rare, fatal genetic condition characterized by an appearance of accelerated aging in children. Its name is derived from the Greek and means "prematurely old." While there are different forms of Progeria*, the classic type is Hutchinson- Gilford Progeria Syndrome, which was named after the doctors who first described it in England: in 1886 by Dr. Jonathan Hutchinson, and in 1897 by Dr. Hastings Gilford. HOW COMMON IS PROGERIA? Progeria affects approximately 1 in 4 - 8 million newborns. It affects both sexes equally and all races. In the past 15 years, children with Progeria have been reported all over the world , including in: Algeria Cuba Ireland Peru Sweden Argentina Denmark Israel Philippines Switzerland Australia Dominican Italy Poland Turkey Austria Republic Japan Portugal United States Belgium Egypt Libya Puerto Rico Venezuela Brazil England Mexico Romania Vietnam Canada France Morocco South Africa Yugoslavia China Germany Netherlands South Korea Columbia India Pakistan Spain WHAT ARE THE FEATURES OF PROGERIA? Although they are born looking healthy, most children with Progeria begin to display many characteristics of Progeria within the first year of life. Progeria signs include growth failure, loss of body fat and hair, aged-looking skin, stiffness of joints, hip dislocation, generalized atherosclerosis, cardiovascular (heart) disease and stroke. The children have a remarkably similar appearance, despite differing ethnic backgrounds. Children with Progeria die of atherosclerosis (heart disease) at an average age of thirteen years (with a range of about 8 – 21 years). WHAT DOES PROGERIA HAVE TO DO WITH AGING? Children with Progeria are genetically predisposed to premature, progressive heart disease. -

Disease Reference Book
The Counsyl Foresight™ Carrier Screen 180 Kimball Way | South San Francisco, CA 94080 www.counsyl.com | [email protected] | (888) COUNSYL The Counsyl Foresight Carrier Screen - Disease Reference Book 11-beta-hydroxylase-deficient Congenital Adrenal Hyperplasia .................................................................................................................................................................................... 8 21-hydroxylase-deficient Congenital Adrenal Hyperplasia ...........................................................................................................................................................................................10 6-pyruvoyl-tetrahydropterin Synthase Deficiency ..........................................................................................................................................................................................................12 ABCC8-related Hyperinsulinism........................................................................................................................................................................................................................................ 14 Adenosine Deaminase Deficiency .................................................................................................................................................................................................................................... 16 Alpha Thalassemia............................................................................................................................................................................................................................................................. -
Blueprint Genetics Ectodermal Dysplasia Panel
Ectodermal Dysplasia Panel Test code: DE0401 Is a 25 gene panel that includes assessment of non-coding variants. Is ideal for patients with a clinical suspicion of ectodermal dysplasia (hidrotic or hypohidrotic) or Ellis-van Creveld syndrome. About Ectodermal Dysplasia Ectodermal Dysplasia (ED) is a group of closely related conditions of which more than 150 different syndromes have been identified. EDs affects the development or function of teeth, hair, nails and sweat glands. ED may present as isolated or as part of a syndromic disease and is commonly subtyped according to sweating ability. The clinical features of the X-linked and autosomal forms of hypohidrotic ectodermal dysplasia (HED) can be indistinguishable and many of the involved genes may lead to phenotypically distinct outcomes depending on number of defective alleles. The most common EDs are hypohidrotic ED and hydrotic ED. X-linked hypohidrotic ectodermal dysplasia (HED) is caused by EDA mutations and explain 75%-95% of familial HED and 50% of sporadic cases. HED is characterized by three cardinal features: hypotrichosis (sparse, slow-growing hair and sparse/missing eyebrows), reduced sweating and hypodontia (absence or small teeth). Reduced sweating poses risk for episodes of hyperthermia. Female carriers may have some degree of hypodontia and mild hypotrichosis. Isolated dental phenotypes have also been described. Mutations in WNT10A have been reported in up to 9% of individuals with HED and in 25% of individuals with HED who do not have defective EDA. Approximately 50% of individuals with heterozygous WNT10A mutation have HED and the most consistent clinical feature is severe oligodontia of permanent teeth. -

Xeroderma Pigmentosum
Xeroderma pigmentosum Description Xeroderma pigmentosum, which is commonly known as XP, is an inherited condition characterized by an extreme sensitivity to ultraviolet (UV) rays from sunlight. This condition mostly affects the eyes and areas of skin exposed to the sun. Some affected individuals also have problems involving the nervous system. The signs of xeroderma pigmentosum usually appear in infancy or early childhood. Many affected children develop a severe sunburn after spending just a few minutes in the sun. The sunburn causes redness and blistering that can last for weeks. Other affected children do not get sunburned with minimal sun exposure, but instead tan normally. By age 2, almost all children with xeroderma pigmentosum develop freckling of the skin in sun-exposed areas (such as the face, arms, and lips); this type of freckling rarely occurs in young children without the disorder. In affected individuals, exposure to sunlight often causes dry skin (xeroderma) and changes in skin coloring (pigmentation). This combination of features gives the condition its name, xeroderma pigmentosum. People with xeroderma pigmentosum have a greatly increased risk of developing skin cancer. Without sun protection, about half of children with this condition develop their first skin cancer by age 10. Most people with xeroderma pigmentosum develop multiple skin cancers during their lifetime. These cancers occur most often on the face, lips, and eyelids. Cancer can also develop on the scalp, in the eyes, and on the tip of the tongue. Studies suggest that people with xeroderma pigmentosum may also have an increased risk of other types of cancer, including brain tumors. -
Neurodegeneration in Accelerated Aging
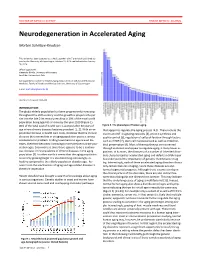
DOCTOR OF MEDICAL SCIENCE DANISH MEDICAL JOURNAL Neurodegeneration in Accelerated Aging Morten Scheibye-Knudsen This review has been accepted as a thesis together with 7 previously published pa- pers by the University of Copenhagen, October 16, 2014 and defended on January 14, 2016 Official opponents: Alexander Bürkle, University of Konstanz Lars Eide, University of Oslo Correspondence: Center for Healthy Aging, Department of Cellular and Molecular Medicine, Faculty of Health and Medical Sciences, University of Copenhagen E-mail: [email protected] Dan Med J 2016;63(11):B5308 INTRODUCTION The global elderly population has been progressively increasing throughout the 20th century and this growth is projected to per- sist into the late 21st century resulting in 20% of the total world population being aged 65 or more by the year 2100 (Figure 1). 80% of the total cost of health care is accrued after 40 years of Figure 2. The phenotype of human aging. age where chronic diseases become prevalent [1, 2]. With an ex- that appear to regulate the aging process [4,5]. These include the ponential increase in health care costs, it follows that the chronic insulin and IGF-1 signaling cascades [4], protein synthesis and diseases that accumulate in an aging population poses a serious quality control [6], regulation of cell proliferation through factors socioeconomic problem. Finding treatments to age related dis- such as mTOR [7], stem cell maintenance 8 as well as mitochon- eases, therefore becomes increasingly more pertinent as the pop- drial preservation [9]. Most of these pathways are conserved ulation ages. Even more so since there appears to be a continu- through evolution and appear to regulate aging in many lower or- ous increase in the prevalence of chronic diseases in the aging ganisms. -

Predisposition to Hematologic Malignancies in Patients With
LETTERS TO THE EDITOR carcinomas but no internal cancer by the age of 29 years Predisposition to hematologic malignancies in and 9 years, respectively. patients with xeroderma pigmentosum Case XP540BE . This patient had a highly unusual pres - entation of MPAL. She was diagnosed with XP at the age Germline predisposition is a contributing etiology of of 18 months with numerous lentigines on sun-exposed hematologic malignancies, especially in children and skin, when her family emigrated from Morocco to the young adults. Germline predisposition in myeloid neo - USA. The homozygous North African XPC founder muta - plasms was added to the World Health Organization tion was present. 10 She had her first skin cancer at the age 1 2016 classification, and current management recommen - of 8 years, and subsequently developed more than 40 cuta - dations emphasize the importance of screening appropri - neous basal and squamous cell carcinomas, one melanoma 2 ate patients. Rare syndromes of DNA repair defects can in situ , and one ocular surface squamous neoplasm. She 3 lead to myeloid and/or lymphoid neoplasms. Here, we was diagnosed with a multinodular goiter at the age of 9 describe our experience with hematologic neoplasms in years eight months, with several complex nodules leading the defective DNA repair syndrome, xeroderma pigmen - to removal of her thyroid gland. Histopathology showed tosum (XP), including myelodysplastic syndrome (MDS), multinodular adenomatous/papillary hyperplasia. At the secondary acute myeloid leukemia (AML), high-grade age of 19 years, she presented with night sweats, fatigue, lymphoma, and an extremely unusual presentation of and lymphadenopathy. Laboratory studies revealed pancy - mixed phenotype acute leukemia (MPAL) with B, T and topenia with hemoglobin 6.8 g/dL, platelet count myeloid blasts. -

1. Progeria 101: Frequently Asked Questions
1. PROGERIA 101: FREQUENTLY ASKED QUESTIONS 1. Progeria 101: Frequently Asked Questions What is Hutchinson-Gilford Progeria Syndrome? What is PRF’s history and mission? What causes Progeria? How is Progeria diagnosed? Are there different types of Progeria? Is Progeria contagious or inherited? What is Hutchinson-Gilford Progeria Syndrome (HGPS or Progeria)? Progeria is also known as Hutchinson-Gilford Progeria Syndrome (HGPS). Genetic testing for It was first described in 1886 by Dr. Jonathan Hutchinson and in 1897 by Progeria can be Dr. Hastings Gilford. Progeria is a rare, fatal, “premature aging” syndrome. It’s called a syndrome performed from a because all the children have very similar symptoms that “go together”. The small sample of blood children have a remarkably similar appearance, even though Progeria affects children of all different ethnic backgrounds. Although most babies with (1-2 tsp) or sometimes Progeria are born looking healthy, they begin to display many characteristics from a sample of saliva. of accelerated aging by 18-24 months of age, or even earlier. Progeria signs include growth failure, loss of body fat and hair, skin changes, stiffness of joints, hip dislocation, generalized atherosclerosis, cardiovascular (heart) disease, and stroke. Children with Progeria die of atherosclerosis (heart disease) or stroke at an average age of 13 years (with a range of about 8-21 years). Remarkably, the intellect of children with Progeria is unaffected, and despite the physical changes in their young bodies, these extraordinary children are intelligent, courageous, and full of life. 1.2 THE PROGERIA HANDBOOK What is PRF’s history and mission? The Progeria Research Foundation (PRF) was established in the United States in 1999 by the parents of a child with Progeria, Drs. -

Hereditary Hearing Impairment with Cutaneous Abnormalities
G C A T T A C G G C A T genes Review Hereditary Hearing Impairment with Cutaneous Abnormalities Tung-Lin Lee 1 , Pei-Hsuan Lin 2,3, Pei-Lung Chen 3,4,5,6 , Jin-Bon Hong 4,7,* and Chen-Chi Wu 2,3,5,8,* 1 Department of Medical Education, National Taiwan University Hospital, Taipei City 100, Taiwan; [email protected] 2 Department of Otolaryngology, National Taiwan University Hospital, Taipei 11556, Taiwan; [email protected] 3 Graduate Institute of Clinical Medicine, National Taiwan University College of Medicine, Taipei City 100, Taiwan; [email protected] 4 Graduate Institute of Medical Genomics and Proteomics, National Taiwan University College of Medicine, Taipei City 100, Taiwan 5 Department of Medical Genetics, National Taiwan University Hospital, Taipei 10041, Taiwan 6 Department of Internal Medicine, National Taiwan University Hospital, Taipei 10041, Taiwan 7 Department of Dermatology, National Taiwan University Hospital, Taipei City 100, Taiwan 8 Department of Medical Research, National Taiwan University Biomedical Park Hospital, Hsinchu City 300, Taiwan * Correspondence: [email protected] (J.-B.H.); [email protected] (C.-C.W.) Abstract: Syndromic hereditary hearing impairment (HHI) is a clinically and etiologically diverse condition that has a profound influence on affected individuals and their families. As cutaneous findings are more apparent than hearing-related symptoms to clinicians and, more importantly, to caregivers of affected infants and young individuals, establishing a correlation map of skin manifestations and their underlying genetic causes is key to early identification and diagnosis of syndromic HHI. In this article, we performed a comprehensive PubMed database search on syndromic HHI with cutaneous abnormalities, and reviewed a total of 260 relevant publications. -

Pediatric Photosensitivity Disorders Dr
FAST FACTS FOR BOARD REVIEW Series Editor: William W. Huang,MD,MPH W. Series Editor:William Swetha N.Pathak,MD;JacquelineDeLuca,MD Pediatric PhotosensitivityDisorders Table 1. Pediatric Photosensitivity Disorders Disease Pathophysiology Clinical Features Management/Prognosis Other/Pearls Actinic prurigo Strong association Pruritic crusted papules Phototesting: lesions Native Americans, (hydroa aestivale, with HLA-DR4 and nodules in both provoked by UVA or UVB; especially mestizos; Hutchinson (HLA-DRB1*0401/0407); sun-exposed and less spontaneous resolution hardening does not summer prurigo) may be a persistent frequently nonexposed may occur during late occur; histopathology: variant of PMLE sites (ie, buttocks); heal adolescence; may follow dermal perivascular (delayed-type with scarring; mucosal a chronic course that mononuclear cell hypersensitivity) and conjunctival persists in adulthood; infiltrate, lacks papillary from UVA or UVB involvement, with cheilitis photoprotection; topical dermal edema, can see often an initial or only corticosteroids and lymphoid follicles feature; worse in summer topical tacrolimus; from lip biopsies; but can extend to winter NB-UVB or PUVA; occurs hours to cyclosporine or days following azathioprine; thalidomide sun exposure (treatment of choice) for (vs solar urticaria) resistant disease noconflictofinterest. The authorsreport Long Beach,California. Center, LaserSkinCare DeLucaisfrom Dr. North Carolina. Winston-Salem, University, Forest Wake Pathakisfrom Dr. Bloom syndrome AR; BLM (encodes Malar telangiectatic