Pediatric Photosensitivity Disorders Dr
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Causes of Short Stature Author Alan D Rogol, MD, Phd Section Editors
Causes of short stature Author Alan D Rogol, MD, PhD Section Editors Peter J Snyder, MD Mitchell Geffner, MD Deputy Editor Alison G Hoppin, MD Contributor disclosures All topics are updated as new evidence becomes available and our peer review process is complete. Literature review current through: Mar 2016. | This topic last updated: Aug 13, 2015. INTRODUCTION — Short stature is a term applied to a child whose height is 2 standard deviations (SD) or more below the mean for children of that sex and chronologic age (and ideally of the same racial-ethnic group). This corresponds to a height that is below the 2.3rd percentile. Short stature may be either a variant of normal growth or caused by a disease. The most common causes of short stature beyond the first year or two of life are familial (genetic) short stature and delayed (constitutional) growth, which are normal non-pathologic variants of growth. The goal of the evaluation of a child with short stature is to identify the subset of children with pathologic causes (such as Turner syndrome, inflammatory bowel disease or other underlying systemic disease, or growth hormone deficiency). The evaluation also assesses the severity of the short stature and likely growth trajectory, to facilitate decisions about intervention, if appropriate. This topic will review the main causes of short stature. The diagnostic approach to children with short stature is discussed separately. (See "Diagnostic approach to children and adolescents with short stature".) NORMAL VARIANTS OF GROWTH Familial short stature — Familial or genetic short stature is most often a normal variant, termed familial or genetic short stature (figure 1). -

Open Full Page
CCR PEDIATRIC ONCOLOGY SERIES CCR Pediatric Oncology Series Recommendations for Childhood Cancer Screening and Surveillance in DNA Repair Disorders Michael F. Walsh1, Vivian Y. Chang2, Wendy K. Kohlmann3, Hamish S. Scott4, Christopher Cunniff5, Franck Bourdeaut6, Jan J. Molenaar7, Christopher C. Porter8, John T. Sandlund9, Sharon E. Plon10, Lisa L. Wang10, and Sharon A. Savage11 Abstract DNA repair syndromes are heterogeneous disorders caused by around the world to discuss and develop cancer surveillance pathogenic variants in genes encoding proteins key in DNA guidelines for children with cancer-prone disorders. Herein, replication and/or the cellular response to DNA damage. The we focus on the more common of the rare DNA repair dis- majority of these syndromes are inherited in an autosomal- orders: ataxia telangiectasia, Bloom syndrome, Fanconi ane- recessive manner, but autosomal-dominant and X-linked reces- mia, dyskeratosis congenita, Nijmegen breakage syndrome, sive disorders also exist. The clinical features of patients with DNA Rothmund–Thomson syndrome, and Xeroderma pigmento- repair syndromes are highly varied and dependent on the under- sum. Dedicated syndrome registries and a combination of lying genetic cause. Notably, all patients have elevated risks of basic science and clinical research have led to important in- syndrome-associated cancers, and many of these cancers present sights into the underlying biology of these disorders. Given the in childhood. Although it is clear that the risk of cancer is rarity of these disorders, it is recommended that centralized increased, there are limited data defining the true incidence of centers of excellence be involved directly or through consulta- cancer and almost no evidence-based approaches to cancer tion in caring for patients with heritable DNA repair syn- surveillance in patients with DNA repair disorders. -

EXTENDED CARRIER SCREENING Peace of Mind for Planned Pregnancies
Focusing on Personalised Medicine EXTENDED CARRIER SCREENING Peace of Mind for Planned Pregnancies Extended carrier screening is an important tool for prospective parents to help them determine their risk of having a child affected with a heritable disease. In many cases, parents aren’t aware they are carriers and have no family history due to the rarity of some diseases in the general population. What is covered by the screening? Genomics For Life offers a comprehensive Extended Carrier Screening test, providing prospective parents with the information they require when planning their pregnancy. Extended Carrier Screening has been shown to detect carriers who would not have been considered candidates for traditional risk- based screening. With a simple mouth swab collection, we are able to test for over 419 genes associated with inherited diseases, including Fragile X Syndrome, Cystic Fibrosis and Spinal Muscular Atrophy. The assay has been developed in conjunction with clinical molecular geneticists, and includes genes listed in the NIH Genetic Test Registry. For a list of genes and disorders covered, please see the reverse of this brochure. If your gene of interest is not covered on our Extended Carrier Screening panel, please contact our friendly team to assist you in finding a gene test panel that suits your needs. Why have Extended Carrier Screening? Extended Carrier Screening prior to pregnancy enables couples to learn about their reproductive risk and consider a complete range of reproductive options, including whether or not to become pregnant, whether to use advanced reproductive technologies, such as preimplantation genetic diagnosis, or to use donor gametes. -

CCR PEDIATRIC ONCOLOGY SERIES CCR Pediatric Oncology Series Recommendations for Surveillance for Children with Leukemia-Predisposing Conditions Christopher C
CCR PEDIATRIC ONCOLOGY SERIES CCR Pediatric Oncology Series Recommendations for Surveillance for Children with Leukemia-Predisposing Conditions Christopher C. Porter1, Todd E. Druley2, Ayelet Erez3, Roland P. Kuiper4, Kenan Onel5, Joshua D. Schiffman6, Kami Wolfe Schneider7, Sarah R. Scollon8, Hamish S. Scott9, Louise C. Strong10, Michael F. Walsh11, and Kim E. Nichols12 Abstract Leukemia, the most common childhood cancer, has long been patients. The panel recognized that for several conditions, recognized to occasionally run in families. The first clues about routine monitoring with complete blood counts and bone the genetic mechanisms underlying familial leukemia emerged marrow evaluations is essential to identify disease evolution in 1990 when Li-Fraumeni syndrome was linked to TP53 muta- and enable early intervention with allogeneic hematopoietic tions. Since this discovery, many other genes associated with stem cell transplantation. However, for others, less intensive hereditary predisposition to leukemia have been identified. surveillance may be considered. Because few reports describ- Although several of these disorders also predispose individuals ing the efficacy of surveillance exist, the recommendations to solid tumors, certain conditions exist in which individuals are derived by this panel are based on opinion, and local expe- specifically at increased risk to develop myelodysplastic syn- rience and will need to be revised over time. The development drome (MDS) and/or acute leukemia. The increasing identifica- of registries and clinical trials is urgently needed to enhance tion of affected individuals and families has raised questions understanding of the natural history of the leukemia-predis- around the efficacy, timing, and optimal methods of surveil- posing conditions, such that these surveillance recommenda- lance. -
Turner Syndrome (TS) Is a Genetic Disease That Affects About Physical Signs of TS May Include: 1 in Every 2,500 Female Live Births
Notes: A Guide for Caregivers For easily accessible answers, education, and support, visit Nutropin.com or call 1-866-NUTROPIN (1-866-688-7674). 18 19 of patients with Your healthcare team is your primary source Turner Syndrome of information about your child’s treatment. Please see the accompanying full Prescribing Information, including Instructions for Use, and additional Important Safety Information througout and on pages 16-18. Models used for illustrative purposes only. Nutropin, Nutropin AQ, and NuSpin are registered trademarks, Nutropin GPS is a trademark, and NuAccess is a service mark of Genentech, Inc. © 2020 Genentech USA, Inc., 1 DNA Way, So. San Francisco, CA 94080 M-US-00005837(v1.0) 06/20 FPO Understanding Turner Syndrome What is Turner Syndrome? Turner Syndrome (TS) is a genetic disease that affects about Physical signs of TS may include: 1 in every 2,500 female live births. TS occurs when one • Short stature of a girl’s two X chromosomes is absent or incomplete. • Webbing of the neck Chromosomes are found in all cells of the human body. They contain the genes that determine the characteristics of a • Low-set, rotated ears person such as the color of hair or eyes. Every person has • Arms that turn out slightly at the elbows 22 pairs of chromosomes containing these characteristics, • Low hairline at the back of the head and one pair of sex chromosomes. • A high, arched palate in the mouth Normally cells in a female’s body contain two “X” chromosomes Biological signs of TS may include: (Fig. 1). • Underdevelopment of the ovaries In girls with TS, part or • Not reaching sexual maturity or starting all of one X chromosome a menstrual period (Fig. -
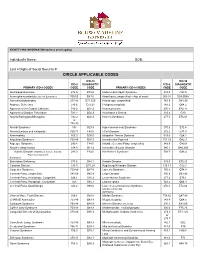
Circle Applicable Codes
IDENTIFYING INFORMATION (please print legibly) Individual’s Name: DOB: Last 4 Digits of Social Security #: CIRCLE APPLICABLE CODES ICD-10 ICD-10 ICD-9 DIAGNOSTIC ICD-9 DIAGNOSTIC PRIMARY ICD-9 CODES CODE CODE PRIMARY ICD-9 CODES CODE CODE Abetalipoproteinemia 272.5 E78.6 Hallervorden-Spatz Syndrome 333.0 G23.0 Acrocephalosyndactyly (Apert’s Syndrome) 755.55 Q87.0 Head Injury, unspecified – Age of onset: 959.01 S09.90XA Adrenaleukodystrophy 277.86 E71.529 Hemiplegia, unspecified 342.9 G81.90 Arginase Deficiency 270.6 E72.21 Holoprosencephaly 742.2 Q04.2 Agenesis of the Corpus Callosum 742.2 Q04.3 Homocystinuria 270.4 E72.11 Agenesis of Septum Pellucidum 742.2 Q04.3 Huntington’s Chorea 333.4 G10 Argyria/Pachygyria/Microgyria 742.2 Q04.3 Hurler’s Syndrome 277.5 E76.01 or 758.33 Aicardi Syndrome 333 G23.8 Hyperammonemia Syndrome 270.6 E72.4 Alcohol Embryo and Fetopathy 760.71 F84.5 I-Cell Disease 272.2 E77.0 Anencephaly 655.0 Q00.0 Idiopathic Torsion Dystonia 333.6 G24.1 Angelman Syndrome 759.89 Q93.5 Incontinentia Pigmenti 757.33 Q82.3 Asperger Syndrome 299.8 F84.5 Infantile Cerebral Palsy, unspecified 343.9 G80.9 Ataxia-Telangiectasia 334.8 G11.3 Intractable Seizure Disorder 345.1 G40.309 Autistic Disorder (Childhood Autism, Infantile 299.0 F84.0 Klinefelter’s Syndrome 758.7 Q98.4 Psychosis, Kanner’s Syndrome) Biotinidase Deficiency 277.6 D84.1 Krabbe Disease 333.0 E75.23 Canavan Disease 330.0 E75.29 Kugelberg-Welander Disease 335.11 G12.1 Carpenter Syndrome 759.89 Q87.0 Larsen’s Syndrome 755.8 Q74.8 Cerebral Palsy, unspecified 343.69 G80.9 -

2018 Etiologies by Frequencies
2018 Etiologies in Order of Frequency by Category Hereditary Syndromes and Disorders Count CHARGE Syndrome 958 Down syndrome (Trisomy 21 syndrome) 308 Usher I syndrome 252 Stickler syndrome 130 Dandy Walker syndrome 119 Cornelia de Lange 102 Goldenhar syndrome 98 Usher II syndrome 83 Wolf-Hirschhorn syndrome (Trisomy 4p) 68 Trisomy 13 (Trisomy 13-15, Patau syndrome) 60 Pierre-Robin syndrome 57 Moebius syndrome 55 Trisomy 18 (Edwards syndrome) 52 Norrie disease 38 Leber congenital amaurosis 35 Chromosome 18, Ring 18 31 Aicardi syndrome 29 Alstrom syndrome 27 Pfieffer syndrome 27 Treacher Collins syndrome 27 Waardenburg syndrome 27 Marshall syndrome 25 Refsum syndrome 21 Cri du chat syndrome (Chromosome 5p- synd) 16 Bardet-Biedl syndrome (Laurence Moon-Biedl) 15 Hurler syndrome (MPS I-H) 15 Crouzon syndrome (Craniofacial Dysotosis) 13 NF1 - Neurofibromatosis (von Recklinghausen dis) 13 Kniest Dysplasia 12 Turner syndrome 11 Usher III syndrome 10 Cockayne syndrome 9 Apert syndrome/Acrocephalosyndactyly, Type 1 8 Leigh Disease 8 Alport syndrome 6 Monosomy 10p 6 NF2 - Bilateral Acoustic Neurofibromatosis 6 Batten disease 5 Kearns-Sayre syndrome 5 Klippel-Feil sequence 5 Hereditary Syndromes and Disorders Count Prader-Willi 5 Sturge-Weber syndrome 5 Marfan syndrome 3 Hand-Schuller-Christian (Histiocytosis X) 2 Hunter Syndrome (MPS II) 2 Maroteaux-Lamy syndrome (MPS VI) 2 Morquio syndrome (MPS IV-B) 2 Optico-Cochleo-Dentate Degeneration 2 Smith-Lemli-Opitz (SLO) syndrome 2 Wildervanck syndrome 2 Herpes-Zoster (or Hunt) 1 Vogt-Koyanagi-Harada -

Disease Reference Book
The Counsyl Foresight™ Carrier Screen 180 Kimball Way | South San Francisco, CA 94080 www.counsyl.com | [email protected] | (888) COUNSYL The Counsyl Foresight Carrier Screen - Disease Reference Book 11-beta-hydroxylase-deficient Congenital Adrenal Hyperplasia .................................................................................................................................................................................... 8 21-hydroxylase-deficient Congenital Adrenal Hyperplasia ...........................................................................................................................................................................................10 6-pyruvoyl-tetrahydropterin Synthase Deficiency ..........................................................................................................................................................................................................12 ABCC8-related Hyperinsulinism........................................................................................................................................................................................................................................ 14 Adenosine Deaminase Deficiency .................................................................................................................................................................................................................................... 16 Alpha Thalassemia............................................................................................................................................................................................................................................................. -

Current Dosing of Growth Hormone in Children with Growth Hormone Deficiency: How Physiologic?
Current Dosing of Growth Hormone in Children With Growth Hormone Deficiency: How Physiologic? Margaret H. MacGillivray, MD*; Sandra L. Blethen, MD, PhD‡; John G. Buchlis, MD*; Richard R. Clopper, ScD*; David E. Sandberg, PhD*; and Thomas A. Conboy, MS* ABSTRACT. The current doses of recombinant growth ARE THE APPROVED RECOMBINANT HUMAN GH hormone (rGH) are two to three times those used in the DOSING REGIMENS PHYSIOLOGIC? pituitary growth hormone era. These rGH doses (0.025 to A standard method for determining whether hor- 0.043 mg/kg/d) are similar to or moderately greater than mone replacement is physiologic is to compare the the physiologic requirements. Growth velocity and dose of hormone administered with the amount of height gains have been shown to be greater with 0.05 that hormone produced daily in healthy persons. For mg/kg/d of rGH than with 0.025 mg/kg/d. Larger doses of human GH, this is not an easy task because of its GH and early initiation of treatment result in greater short half-life, multicompartmental distribution, and heights at the onset of puberty and greater adult heights. Earlier onset of puberty and more rapid maturation, as episodic pulsatile pattern of secretion. In addition, indicated by bone age, were not observed in children GH has a variable secretion profile that is influenced who were given 0.18 to 0.3 mg/kg/wk of rGH. The fre- by age, diurnal rhythm, sleep, stress, nutrition, body quency of adverse events is very low, but diligent sur- weight, and sex hormones. One approach to calcu- veillance of all children who are treated with rGH is lating daily levels of endogenously produced GH essential. -

Obese Children and Adolescents: a Risk Group for Low Vitamin B12
ARTICLE Obese Children and Adolescents A Risk Group for Low Vitamin B12 Concentration Orit Pinhas-Hamiel, MD; Noa Doron-Panush, RD; Brian Reichman, MD; Dorit Nitzan-Kaluski, MD, MPH, RD; Shlomit Shalitin, MD; Liat Geva-Lerner, MD Objective: To assess whether overweight children and Results: Median concentration of serum B12 in normal- adolescents are at an increased risk for vitamin B12 deficiency. weight children was 530 pg/mL and in obese children, Ͻ 400 pg/mL (P .001). Low B12 concentrations were noted Design: Prospective descriptive study. in 10.4% of the obese children compared with only 2.2% Ͻ of the normal weight group (P .001). Vitamin B12 defi- Setting: Two pediatric endocrine centers in Israel. ciency was noted in 12 children, 8 (4.9%) of the obese subjects and 4 (1.8%) of the normal weight group (P=.08). Participants: Three hundred ninety-two children and After we adjusted for age and sex, obesity was associ- adolescents were divided into 2 groups as follows: the ated with a 4.3-fold risk for low serum B12, and each unit normal-weight group had body mass indexes, calcu- increase in body mass index standard deviation score re- lated as weight in kilograms divided by height in meters sulted in an increased risk of 1.24 (95% confidence in- squared, under the 95th percentile (Ͻ1.645 standard de- terval, 0.99-1.56). viation scores; n=228); the obese group had body mass indexes equal to or above the 95th percentile (Ն1.645 standard deviation scores; n=164). Conclusions: Obesity in children and adolescents was associated with an increased risk of low vitamin B12 con- Intervention: We measured vitamin B12 concentra- centration. -

Diseases of the Digestive System (KOO-K93)
CHAPTER XI Diseases of the digestive system (KOO-K93) Diseases of oral cavity, salivary glands and jaws (KOO-K14) lijell Diseases of pulp and periapical tissues 1m Dentofacial anomalies [including malocclusion] Excludes: hemifacial atrophy or hypertrophy (Q67.4) K07 .0 Major anomalies of jaw size Hyperplasia, hypoplasia: • mandibular • maxillary Macrognathism (mandibular)(maxillary) Micrognathism (mandibular)( maxillary) Excludes: acromegaly (E22.0) Robin's syndrome (087.07) K07 .1 Anomalies of jaw-cranial base relationship Asymmetry of jaw Prognathism (mandibular)( maxillary) Retrognathism (mandibular)(maxillary) K07.2 Anomalies of dental arch relationship Cross bite (anterior)(posterior) Dis to-occlusion Mesio-occlusion Midline deviation of dental arch Openbite (anterior )(posterior) Overbite (excessive): • deep • horizontal • vertical Overjet Posterior lingual occlusion of mandibular teeth 289 ICO-N A K07.3 Anomalies of tooth position Crowding Diastema Displacement of tooth or teeth Rotation Spacing, abnormal Transposition Impacted or embedded teeth with abnormal position of such teeth or adjacent teeth K07.4 Malocclusion, unspecified K07.5 Dentofacial functional abnormalities Abnormal jaw closure Malocclusion due to: • abnormal swallowing • mouth breathing • tongue, lip or finger habits K07.6 Temporomandibular joint disorders Costen's complex or syndrome Derangement of temporomandibular joint Snapping jaw Temporomandibular joint-pain-dysfunction syndrome Excludes: current temporomandibular joint: • dislocation (S03.0) • strain (S03.4) K07.8 Other dentofacial anomalies K07.9 Dentofacial anomaly, unspecified 1m Stomatitis and related lesions K12.0 Recurrent oral aphthae Aphthous stomatitis (major)(minor) Bednar's aphthae Periadenitis mucosa necrotica recurrens Recurrent aphthous ulcer Stomatitis herpetiformis 290 DISEASES OF THE DIGESTIVE SYSTEM Diseases of oesophagus, stomach and duodenum (K20-K31) Ill Oesophagitis Abscess of oesophagus Oesophagitis: • NOS • chemical • peptic Use additional external cause code (Chapter XX), if desired, to identify cause. -
Blueprint Genetics Ectodermal Dysplasia Panel
Ectodermal Dysplasia Panel Test code: DE0401 Is a 25 gene panel that includes assessment of non-coding variants. Is ideal for patients with a clinical suspicion of ectodermal dysplasia (hidrotic or hypohidrotic) or Ellis-van Creveld syndrome. About Ectodermal Dysplasia Ectodermal Dysplasia (ED) is a group of closely related conditions of which more than 150 different syndromes have been identified. EDs affects the development or function of teeth, hair, nails and sweat glands. ED may present as isolated or as part of a syndromic disease and is commonly subtyped according to sweating ability. The clinical features of the X-linked and autosomal forms of hypohidrotic ectodermal dysplasia (HED) can be indistinguishable and many of the involved genes may lead to phenotypically distinct outcomes depending on number of defective alleles. The most common EDs are hypohidrotic ED and hydrotic ED. X-linked hypohidrotic ectodermal dysplasia (HED) is caused by EDA mutations and explain 75%-95% of familial HED and 50% of sporadic cases. HED is characterized by three cardinal features: hypotrichosis (sparse, slow-growing hair and sparse/missing eyebrows), reduced sweating and hypodontia (absence or small teeth). Reduced sweating poses risk for episodes of hyperthermia. Female carriers may have some degree of hypodontia and mild hypotrichosis. Isolated dental phenotypes have also been described. Mutations in WNT10A have been reported in up to 9% of individuals with HED and in 25% of individuals with HED who do not have defective EDA. Approximately 50% of individuals with heterozygous WNT10A mutation have HED and the most consistent clinical feature is severe oligodontia of permanent teeth.