Dry Eye Syndrome: Excessive Tear Evaporation
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Altered Hyaluronic Acid Content in Tear Fluid of Patients with Adenoviral Conjunctivitis
Anais da Academia Brasileira de Ciências (2015) 87(1): 455-462 (Annals of the Brazilian Academy of Sciences) Printed version ISSN 0001-3765 / Online version ISSN 1678-2690 http://dx.doi.org/10.1590/0001-3765201520140122 www.scielo.br/aabc Altered hyaluronic acid content in tear fluid of patients with adenoviral conjunctivitis JULIANA L. DREYFUSS1,2*, CAIO V. REGATIERI1,3,5*, BRUNO COELHO1, JOSÉ B. BARBOSA3, DENISE DE FREITAS3, HELENA B. NADER1 and JOÃO R. MARTINS1,4 1Departamento de Bioquímica, Disciplina de Biologia Molecular, Universidade Federal de São Paulo, Rua Três de Maio, 100, 4º andar, 04044-020 São Paulo, SP, Brasil 2Departamento de Informática em Saúde, Grupo Interdisciplinar de Ciências Exatas em Saúde, Universidade Federal de São Paulo, Rua Botucatu, 862, 04023-062 São Paulo, SP, Brasil 3Departamento de Oftalmologia, Universidade Federal de São Paulo, Rua Botucatu, 821, 04023-062 São Paulo, SP, Brasil 4Departamento de Medicina, Disciplina de Endocrinologia, Universidade Federal de São Paulo, Rua Borges Lagoa, 800, 04038-001 São Paulo, SP, Brasil 5Department of Ophthalmology, New England Eye Center, Tufts Medical Center, 800 Washington Street, 02111 Boston, MA, USA Manuscript received on March 13, 2014; accepted for publication on October 24, 2014 ABSTRACT The adenoviral conjunctivitis is one of the biggest causes of conjunctival infection in the world. Conjunctivitis causes relatively nonspecific symptoms, as hyperaemia and chemosis. Even after biomicroscopy, complex laboratory tests, such as viral culture, are necessary to identify the pathogen or its etiology. To contribute to the better understanding of the pathobiology of the adenoviral conjunctivitis, the tear fluids of patients with unilateral acute adenovirus conjunctivitis (UAAC), normal donors (control) and patients with allergic conjunctivitis were analyzed. -

Ν Prefit Examination
Cosmetics and the Contact Lens Wearer - What and Why By Diane F. Drake, LDO, ABOM, FCLSA Mission Statement Better Quality of Life Through Better Vision Course Description This presentation discusses cosmetics offered for the male and female contact lens wearers. Obvious and not so obvious cosmetics such as hairsprays, aftershaves, colognes, and soaps will be discussed. Proper handling and hygiene of contact lenses and the various structures of the tear layer and ocular structure will be included. Discover how improper cosmetic use can affect tear layers and the success or lack of success of the contact lens wearer. Introduction ν Tear layers ν Cosmetic usage ν Importance of tear film ν Patient instructions ν Types of cosmetics ν Conclusion - Communication ν Prefit examination Anatomy of the Eye Cornea Eyelids ν Five distinct layers ν Important in health of eye – Epithelium – Help to keep eye moist – Bowman’s layer – Help to distribute tears, oxygen and – Stroma nutrients – Descemets membrane – Protects the eye from light and injury – Endothelium – Lids are elastic ν Lose elasticity with age Tissues of Eyelids Conjunctiva ν Conjunctiva ν Thin mucous membrane, running ν Termed palpebral aperture continuous from lid to corneal limbus – While opened – Not always same size – Palpebral - lids – Bulbar - Globe of eye ν Contain Meibomian glands ν Contain Sebaceous glands ν Muscles of eyelid – Levator Muscle ν Pumps tears away – Orbicularis Oculi Muscle Contact lenses cannot get lost behind the eye Lacrimal Apparatus - Tear Production ν The conjunctival -

Epiphora (Excessive Tearing)
EPIPHORA (EXCESSIVE TEARING) INTRODUCTION Epiphora, or excessive tearing, is the overflow of tears from one or both eyes. Epiphora can occur all the time or only sometimes. It can be split into two categories. Either too many tears are produced or not enough of the tears are cleared. The following information will focus on tears not being cleared. ANATOMY The part of your body that makes tears is the lacrimal apparatus (See Figure 1). It is a system of tubes and sacs. It begins at the outer corner of your eyes in the lacrimal gland. This is the gland that produces tears. Tears then wash across the surface of the eye from the outer to inner corner, protecting, moistening and cleaning the outer layer of the eye. The upper and lower eyelids each have a single opening near the inner corner. These openings are on slightly raised mounds called puncta (See Figure 2). Each punctum drains tears into a tube called the canaliculus. There is an upper and lower canaliculus. Each of these small tubes drains tears into a larger tube called the common canaliculus. The common canaliculus delivers tears to the lacrimal sac, which is under the inner corner of the eye near the nose. The duct then drains tears from the lacrimal sac into the nose. Tears enter the nasal cavity through an opening near the bottom known as Hasner's valve. Too much tearing can result from problems that happen anywhere along this path. A common area to see obstruction is in the nasolacrimal duct. Figure 1. -

Sympathy Crying: Insights from Infrared Thermal Imaging on a Female Sample
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Portsmouth University Research Portal (Pure) RESEARCH ARTICLE Sympathy Crying: Insights from Infrared Thermal Imaging on a Female Sample Stephanos Ioannou1*, Paul Morris2, Samantha Terry2, Marc Baker2, Vittorio Gallese3,4, Vasudevi Reddy2 1 Alfaisal University, Department of Physiological Sciences, College of Medicine, Riyadh, Kingdom of Saudi Arabia, 2 Department of Psychology-Centre for Situated Action and Communication, University of Portsmouth, Portsmouth, United Kingdom, 3 Parma University, Department of Neuroscience, Section of Human Physiology, Parma, Italy, 4 Institute of Philosophy, School of Advanced Study, University of London, London, United Kingdom * [email protected] a11111 Abstract Sympathy crying is an odd and complex mixture of physiological and emotional phenom- ena. Standard psychophysiological theories of emotion cannot attribute crying to a single subdivision of the autonomic nervous system (ANS) and disagreement exists regarding the emotional origin of sympathy crying. The current experiment examines sympathy crying OPEN ACCESS using functional thermal infrared imaging (FTII), a novel contactless measure of ANS activ- Citation: Ioannou S, Morris P, Terry S, Baker M, ity. To induce crying female participants were given the choice to decide which film they Gallese V, Reddy V (2016) Sympathy Crying: Insights wanted to cry to. Compared to baseline, temperature started increasing on the forehead, from Infrared Thermal Imaging on a Female Sample. PLoS ONE 11(10): e0162749.doi:10.1371/journal. the peri-orbital region, the cheeks and the chin before crying and reached even higher tem- pone.0162749 peratures during crying. The maxillary area showed the opposite pattern and a gradual tem- Editor: Alessio Avenanti, University of Bologna, perature decrease was observed compared to baseline as a result of emotional sweating. -

Eye External Anatomy of Eye Accessory Structures
4/22/16 Eye Bio 40B Dr. Kandula External Anatomy of Eye Accessory Structures l Eyebrows l Levator Palpebrae Superioris - opens eye l Eyelashes l Ciliary glands – modified sweat glands l Small sebaceous glands l Sty is inflamed ciliary glands or small sebaceous glands 1 4/22/16 Terms: Lacrimal gland and duct Surface of eye Lacrimal puncta Lacrimal sac Nasolacrimal duct Nasal cavity Tears / Lacrimal fluid l a watery physiologic saline, with a plasma-like consistency, l contains the bactericidal enzyme lysozyme; l it moistens the conjunctiva and cornea, l provides nutrients and dissolved O2 to the cornea. Extrinsic Muscles of the Eye: Lateral/medial rectus Important to know Superior/inferior rectus actions and nerve Superior/inferior oblique supply in table 2 4/22/16 Extrinsic Eye Muscles • Eye movements controlled by six extrinsic eye muscles Four recti muscles § Superior rectus – moves eyeball superiorly supplied by Cranial Nerve III § Inferior rectus - moves eyeball inferiorly supplied by Cranial Nerve III § Lateral rectus - moves eyeball laterally supplied by Cranial Nerve VI § Medial rectus - moves eyeball medially supplied by Cranial Nerve III Extrinsic Eye Muscles Two oblique muscles rotate eyeball on its axis § Superior oblique rotates eyeball inferiorly and laterally and is supplied by Cranial Nerve IV § Inferior oblique rotates superiorly and laterally and is supplied by Cranial Nerve III Convergence of the Eyes l Binocular vision in humans has both eyes looking at the same object l As you look at an object close to your face, -
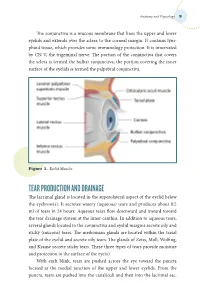
TEAR PRODUCTION and DRAINAGE the Lacrimal Gland Is Located in the Superolateral Aspect of the Eyelid Below the Eyebrow(S)
Anatomy and Physiology 9 The conjunctiva is a mucous membrane that lines the upper and lower eyelids and extends over the sclera to the corneal margin. It contains lym- phoid tissue, which provides some immunology protection. It is innervated by CN V, the trigeminal nerve. The portion of the conjunctiva that covers the sclera is termed the bulbar conjunctiva; the portion covering the inner surface of the eyelids is termed the palpebral conjunctiva. Figure 1. Eyelid Muscles TEAR PRODUCTION AND DRAINAGE The lacrimal gland is located in the superolateral aspect of the eyelid below the eyebrow(s). It secretes watery (aqueous) tears and produces about 0.2 ml of tears in 24 hours. Aqueous tears flow downward and inward toward the tear drainage system at the inner canthus. In addition to aqueous tears, several glands located in the conjunctiva and eyelid margins secrete oily and sticky (mucous) tears. The meibomian glands are located within the tarsal plate of the eyelid and secrete oily tears. The glands of Zeiss, Moll, Wolfing, and Krause secrete sticky tears. These three types of tears provide moisture and protection to the surface of the eye(s). With each blink, tears are pushed across the eye toward the puncta located at the medial junction of the upper and lower eyelids. From the puncta, tears are pushed into the canaliculi and then into the lacrimal sac. 10 Essentials of Ophthalmic Nursing They are drained from the lacrimal sac and nasolacrimal duct to the inside of the nose and down the throat (see Figure 2). Figure 2. Lacrimal System TEAR FILM The tear film has three distinct layers. -

Excessive Tearing (Epiphora ))
EExxcceessssiivvee TTeeaarriinngg ((EEppiipphhoorraa)) www.theeyecenter.com A healthy eye is a wet eye, thanks to the workings of the lacrimal (tear duct) system around the eyes. The lacrimal gland is found above the outer edge of the eye under the eyebrow. The lacrimal duct, which forms tears, is found on the inside corner of your eye and down the side of the nose. For various reasons, this system can malfunction and cause the eye(s) to be continuously wet. Symptoms The tear duct is the passage through which the tears drain off the eye. When it becomes blocked or plugged, it may lead to: • Constant tearing • Redness and swelling in and around the eyes • Infection • Pain Alexandria Fairfax Sterling Leesburg 703-931-9100 703-573-8080 703-430-4400 703-858-3170 The blockage may be due to: • Mucous buildup in the lacrimal duct at birth and in infancy • Ingrown eyelashes • Thick or hardened discharge from an eye infection such as conjunctivitis (pink eye) • Continued exposure to allergens that irritate the eyes • Obstruction due to airborne irritants especially in the work environment (i.e. dust, chemicals, smoke or pollution) • Other eye conditions, such as a stye, that cause the eye to have an unusual discharge that can harden and plug the lacrimal duct. Treatment The ophthalmologist will examine the eye and may probe the tear duct to determine if a blockage exists. Initially, antibiotic drops may be prescribed to treat the infection, and possibly corticosteroid drops to treat any swelling. The blockage can often be worked loose by massaging the tear duct along the side of the eye and down the nose. -

The Lacrimal System Terms
The Lacrimal System Lynn E. Lawrence, CPOT, ABOC, COA, OSC Terms • Etiology – the cause of a disease or abnormal condition • Dacryocystitis – inflammation of the lacrimal sac • Epiphora – watering of eyes due to excess secretion of tears or obstruction of the lacrimal passage Tear Film Layers oil aqueous snot What functions does each layer of the tear perform? Lacrimal System: Tear Film Layers LIPID DEFICIENCY ‐ evaporates TEAR DEFICIENCY – fails to hydrate properly oil aqueous snot What functions does each layer of the tear perform? What are functions of tears? Tear Components • Lipid Layer – prevents evaporation • Aqueous Layer ‐ hydration • Mucus Layer – sticks tear to the eye • Other components Lacrimal Apparatus • Sometimes a person cannot produce natural tears they might need punctal plugs to prevent the tears from draining off the eye. • Faucet • Action • Drain Obstructive – vs‐ non‐obstructive Tear Production – Secretory • Lacrimal gland – Reflex tearing – Too much tearing…epiphora • Gland of Krause – Superior fornix • Gland of Wolfring – Superior tarsal plate Two Primary Forms of Dry Eye 800 nm 8,000 nm 100 nm The two primary forms of dry eye are Evaporative Dry Eye, also known as Meibomian Gland Dysfunction or MGD and Aqueous Dry Eye. The majority of dry eye sufferers have MGD. Oil & Water Remember science class? Oil floats. Oil does not mix with water, but rather sits on top of water. Oil is what keeps water from evaporating. Need three volunteers TEST TIME http://optometrytimes.modernmedicine.com/optometrytimes/news/treating‐dry‐eye‐ lipid‐based‐eye‐drops Lipid Secretion: Meibomian Glands Left: Transillumination of eyelid showing meibomian glands Right: Secretion of lipid at lid margin • The lipid layer restricts evaporation to 5‐10% of tear flow – Also helps lubricate Mucin Secretion: Goblet Cells Superficial layer of bulbar conjunctiva. -

The Pathologization, Psychologization, and Privatization
1 BOTTLED TEARS: THE PATHOLOGIZATION, PSYCHOLOGIZATION, AND PRIVATIZATION OF GRIEF LEEAT GRANEK A DISSERTATION SUBMITTED TO THE FACULTY OF GRADUATE STUDIES IN PARTIAL FULFILMENT OF THE REQUIREMENTS FOR THE DEGREE OF DOCTOR OF PHILOSOPHY GRADUATE PROGRAM IN PSYCHOLOGY YORK UNIVERSITY, TORONTO, ONTARIO OCTOBER 2008 Library and Archives Bibliotheque et Canada Archives Canada Published Heritage Direction du Branch Patrimoine de I'edition 395 Wellington Street 395, rue Wellington Ottawa ON K1A0N4 Ottawa ON K1A 0N4 Canada Canada Your file Votre reference ISBN: 978-0-494-90378-0 Our file Notre reference ISBN: 978-0-494-90378-0 NOTICE: AVIS: The author has granted a non L'auteur a accorde une licence non exclusive exclusive license allowing Library and permettant a la Bibliotheque et Archives Archives Canada to reproduce, Canada de reproduire, publier, archiver, publish, archive, preserve, conserve, sauvegarder, conserver, transmettre au public communicate to the public by par telecommunication ou par I'lnternet, preter, telecommunication or on the Internet, distribuer et vendre des theses partout dans le loan, distrbute and sell theses monde, a des fins commerciales ou autres, sur worldwide, for commercial or non support microforme, papier, electronique et/ou commercial purposes, in microform, autres formats. paper, electronic and/or any other formats. The author retains copyright L'auteur conserve la propriete du droit d'auteur ownership and moral rights in this et des droits moraux qui protege cette these. Ni thesis. Neither the thesis nor la these ni des extraits substantiels de celle-ci substantial extracts from it may be ne doivent etre imprimes ou autrement printed or otherwise reproduced reproduits sans son autorisation. -

Coronavirus in Tears and Conjunctival Secretions of Patients with COVID-19
Received: 19 February 2020 | Accepted: 24 February 2020 DOI: 10.1002/jmv.25725 RESEARCH ARTICLE Evaluation of coronavirus in tears and conjunctival secretions of patients with SARS‐CoV‐2 infection Jianhua Xia MM | Jianping Tong MD | Mengyun Liu MM | Ye Shen MD | Dongyu Guo MD Department of Ophthalmology, Zhejiang University School of Medicine First Affiliated Abstract Hospital, Hangzhou, Zhejiang, China, Objective: This study aimed to assess the presence of novel coronavirus in tears Correspondence and conjunctival secretions of SARS–CoV‐2‐infected patients. Ye Shen, MD and Dongyu Guo, MD, Department of Ophthalmology, Zhejiang Methods: A prospective interventional case series study was performed, and University School of Medicine First Affiliated 30 confirmed novel coronavirus pneumonia (NCP) patients were selected at the Hospital, Hangzhou, 310003 Zhejiang, China. Email: [email protected] (Y. S.) and First Affiliated Hospital of Zhejiang University from 26 January 2020 to 9 February [email protected] (D. G.) 2020. At an interval of 2 to 3 days, tear and conjunctival secretions were collected twice with disposable sampling swabs for reverse‐transcription polymerase chain reaction (RT‐PCR) assay. Results: Twenty‐one common‐type and nine severe‐type NCP patients were enrolled. Two samples of tear and conjunctival secretions were obtained from the only one patient with conjunctivitis yielded positive RT‐PCR results. Fifty‐eight samples from other patents were all negative. Conclusion: We speculate that SARS‐CoV‐2 may be detected in the tears and conjunctival secretions in NCP patients with conjunctivitis. KEYWORDS coronavirus, horizontal transmission, infection 1 | INTRODUCTION outbreak as a public health emergency of international concern.4 At the close of day (on 18 February 2020 at 24:00:00), the cumulative In December 2019, 41 cases of unexplained pneumonia were clus- number of infected people worldwide was 73 332, and the cumula- tered in Wuhan, Hubei Province, China. -

Blocked Tear Duct (Nasolacrimal Duct Obstruction)
Blocked tear duct (Nasolacrimal duct obstruction) Tears are produced to lubricate the surface of the eye and drain through small openings in the inner corner of the upper and lower eyelids. The tears then flow down the tear duct and into the nose. If the tear duct is blocked the tears will not drain properly and will spill over onto the cheek. The mucus produced by the tear sac also will not drain. The result is a watery and sticky eye. What causes blocked tear ducts? Most commonly it’s caused by failure of a membrane at the end of the tear duct to open normally (at the time of birth). Blocked tear ducts most commonly open within the first 12 months of life. Other causes may be: narrow tear duct system, infection, or tight or absent (rare) canaliculus (beginning of the tear duct system). What are the signs and symptoms of a blocked tear duct? • Watery eyes • Eyelids may be red and swollen • Sticky yellowish-green discharge – caused by a failure of normal tear sac mucus to properly flush down the blocked tear duct. Generally, this does not mean infection and is not conjunctivitis • The severity of the signs above may be worse under certain conditions such as when your child has a cold, or when outdoors in a windy or cold environment (this may cause eyes to water more) • If a child has a cold they may have increased watery eyes or discharge (this may or may not be related to a blocked tear duct) How is a blocked tear duct treated? Approximately 90% of babies with a blocked tear duct will spontaneously resolve during the first 12 months of life. -

Blocked Tear Ducts)
Nasolacrimal Duct Obstruction (Blocked Tear Ducts) Nasolacrimal Duct Obstruction occurs when the tear duct is blocked by a membrane or is not fully developed from birth. This causes the tears to build up in the duct and overflow in your child’s eyes and run down their cheek. What is Nasolacrimal Duct Obstruction (NLDO) is a blocked tear duct. This problem Nasolacrimal Duct goes away on its own in about 90% of children by age 10 to 12 months. Obstruction? The eyes continually produce tears. They keep the eyes moist and clean. The tears drain into tiny holes in the upper and lower lids, called puncta. The tears then go down small tubes (canaliculi) into the tear duct (lacrimal sac). Then they flow from the tear duct into the nose. NLDO occurs when the tear duct is blocked by a membrane or its f no ully developed from birth. This causes the tears to build up in the duct and backflow into your child’s eyes and run down their cheeks. The blockage can be on one or both sides. Blocked tear duct. The blockage can occur in one or both eyes What are the signs • Large amount of tears when your child is not crying of NLDO? • Crusty or mucus discharge on eyelashes or eyelids How do you treat The options for treatment are: NLDO? • Massaging the tear ducts • Antibiotic drops or ointment if there is a secondary infection present • Surgery to open the tear duct 1 of 2 To Learn More Free Interpreter Services • Ophthalmology • In the hospital, ask your nurse.