Blocked Tear Ducts
Total Page:16
File Type:pdf, Size:1020Kb

Load more
Recommended publications
-

Altered Hyaluronic Acid Content in Tear Fluid of Patients with Adenoviral Conjunctivitis
Anais da Academia Brasileira de Ciências (2015) 87(1): 455-462 (Annals of the Brazilian Academy of Sciences) Printed version ISSN 0001-3765 / Online version ISSN 1678-2690 http://dx.doi.org/10.1590/0001-3765201520140122 www.scielo.br/aabc Altered hyaluronic acid content in tear fluid of patients with adenoviral conjunctivitis JULIANA L. DREYFUSS1,2*, CAIO V. REGATIERI1,3,5*, BRUNO COELHO1, JOSÉ B. BARBOSA3, DENISE DE FREITAS3, HELENA B. NADER1 and JOÃO R. MARTINS1,4 1Departamento de Bioquímica, Disciplina de Biologia Molecular, Universidade Federal de São Paulo, Rua Três de Maio, 100, 4º andar, 04044-020 São Paulo, SP, Brasil 2Departamento de Informática em Saúde, Grupo Interdisciplinar de Ciências Exatas em Saúde, Universidade Federal de São Paulo, Rua Botucatu, 862, 04023-062 São Paulo, SP, Brasil 3Departamento de Oftalmologia, Universidade Federal de São Paulo, Rua Botucatu, 821, 04023-062 São Paulo, SP, Brasil 4Departamento de Medicina, Disciplina de Endocrinologia, Universidade Federal de São Paulo, Rua Borges Lagoa, 800, 04038-001 São Paulo, SP, Brasil 5Department of Ophthalmology, New England Eye Center, Tufts Medical Center, 800 Washington Street, 02111 Boston, MA, USA Manuscript received on March 13, 2014; accepted for publication on October 24, 2014 ABSTRACT The adenoviral conjunctivitis is one of the biggest causes of conjunctival infection in the world. Conjunctivitis causes relatively nonspecific symptoms, as hyperaemia and chemosis. Even after biomicroscopy, complex laboratory tests, such as viral culture, are necessary to identify the pathogen or its etiology. To contribute to the better understanding of the pathobiology of the adenoviral conjunctivitis, the tear fluids of patients with unilateral acute adenovirus conjunctivitis (UAAC), normal donors (control) and patients with allergic conjunctivitis were analyzed. -

Ciliary Zonule Sclera (Suspensory Choroid Ligament)
ACTIVITIES Complete Diagrams PNS 18 and 19 Complete PNS 23 Worksheet 3 #1 only Complete PNS 24 Practice Quiz THE SPECIAL SENSES Introduction Vision RECEPTORS Structures designed to respond to stimuli Variable complexity GENERAL PROPERTIES OF RECEPTORS Transducers Receptor potential Generator potential GENERAL PROPERTIES OF RECEPTORS Stimulus causing receptor potentials Generator potential in afferent neuron Nerve impulse SENSATION AND PERCEPTION Stimulatory input Conscious level = perception Awareness = sensation GENERAL PROPERTIES OF RECEPTORS Information conveyed by receptors . Modality . Location . Intensity . Duration ADAPTATION Reduction in rate of impulse transmission when stimulus is prolonged CLASSIFICATION OF RECEPTORS Stimulus Modality . Chemoreceptors . Thermoreceptors . Nociceptors . Mechanoreceptors . Photoreceptors CLASSIFICATION OF RECEPTORS Origin of stimuli . Exteroceptors . Interoceptors . Proprioceptors SPECIAL SENSES Vision Hearing Olfaction Gustation VISION INTRODUCTION 70% of all sensory receptors are in the eye Nearly half of the cerebral cortex is involved in processing visual information Optic nerve is one of body’s largest nerve tracts VISION INTRODUCTION The eye is a photoreceptor organ Refraction Conversion (transduction) of light into AP’s Information is interpreted in cerebral cortex Eyebrow Eyelid Eyelashes Site where conjunctiva merges with cornea Palpebral fissure Lateral commissure Eyelid Medial commissure (a) Surface anatomy of the right eye Figure 15.1a Orbicularis oculi muscle -

Ν Prefit Examination
Cosmetics and the Contact Lens Wearer - What and Why By Diane F. Drake, LDO, ABOM, FCLSA Mission Statement Better Quality of Life Through Better Vision Course Description This presentation discusses cosmetics offered for the male and female contact lens wearers. Obvious and not so obvious cosmetics such as hairsprays, aftershaves, colognes, and soaps will be discussed. Proper handling and hygiene of contact lenses and the various structures of the tear layer and ocular structure will be included. Discover how improper cosmetic use can affect tear layers and the success or lack of success of the contact lens wearer. Introduction ν Tear layers ν Cosmetic usage ν Importance of tear film ν Patient instructions ν Types of cosmetics ν Conclusion - Communication ν Prefit examination Anatomy of the Eye Cornea Eyelids ν Five distinct layers ν Important in health of eye – Epithelium – Help to keep eye moist – Bowman’s layer – Help to distribute tears, oxygen and – Stroma nutrients – Descemets membrane – Protects the eye from light and injury – Endothelium – Lids are elastic ν Lose elasticity with age Tissues of Eyelids Conjunctiva ν Conjunctiva ν Thin mucous membrane, running ν Termed palpebral aperture continuous from lid to corneal limbus – While opened – Not always same size – Palpebral - lids – Bulbar - Globe of eye ν Contain Meibomian glands ν Contain Sebaceous glands ν Muscles of eyelid – Levator Muscle ν Pumps tears away – Orbicularis Oculi Muscle Contact lenses cannot get lost behind the eye Lacrimal Apparatus - Tear Production ν The conjunctival -

Adrenaline Dacryolith: Detection by Ultrasound Examination of the Nasolacrimal Duct
Br J Ophthalmol: first published as 10.1136/bjo.72.12.935 on 1 December 1988. Downloaded from British Journal ofOphthalmology, 1988, 72, 935-937 Adrenaline dacryolith: detection by ultrasound examination of the nasolacrimal duct JOHN A BRADBURY,' IAN G RENNIE,' AND M ANDREW PARSONS2 From the Departments of'Ophthalmology and 2Pathology, University ofSheffield SUMMARY A 73-year-old woman on topical pilocarpine and adrenaline for chronic simple glaucoma for three years presented with a mass in the medial canthus of the right eye. Although dacryocystography showed a dilated and partially obstructed nasolacrimal system, ultrasound examination was able to demonstrate a mass in the nasolacrimal duct. At operation a black dacryolith was found, of the diameter predicted by ultrasound. Histological examination of the dacryolith suggested its derivation from breakdown products of adrenaline. Ultrasound examination of the nasolacrimal drain- her right conjunctival sac. In between these acute age system has been shown to be of value when the episodes the epiphora and a slight swelling at the copyright. system is dilated in cases such as a mucocoele or acute medial canthus persisted but were less troublesome. dacryocystitis. It is of limited value in functional Her right nasolacrimal duct had been irrigated during disorders, where the passage of fluid through the one of these acute episodes, which had caused some nasolacrimal system is slowed, producing a minimally resolution of her symptoms. dilated system.' No reports so far have illustrated the On examination a firm mass was palpable over the ability of ultrasound to demonstrate a mass in the right lacrimal fossa extending slightly above the nasolacrimal duct. -

Pediatric Orbital Tumors and Lacrimal Drainage System
Pediatric Orbital Tumors and Lacrimal Drainage System Peter MacIntosh, MD University of Illinois • No financial disclosures Dermoid Cyst • Congenital • Keratinized epidermis • Dermal appendage • Trapped during embryogenesis • 6% of lesions • 40-50% of orbital pediatric orbital lesion • Usually discovered in the first year of life • Painless/firm/subQ mass • Rarely presents as an acute inflammatory lesion (Rupture?) • Frontozygomatic (70%) • Maxillofrontal (20%) suture Imaging - CT • Erosion/remodeling of bone • Adjacent bony changes: “smooth fossa” (85%) • Dumbell dermoid: extraorbital and intraorbital components through bony defect Imaging - MRI • Encapsulated • Enhancement of wall but not lumen Treatment Options • Observation • Risk of anesthesia • Surgical Removal • Changes to bone • Rupture of cyst can lead to acute inflammation • Irrigation • Abx • Steroids Dermoid INFANTILE/Capillary Hemangioma • Common BENIGN orbital lesion of children • F>M • Prematurity • Appears in 1st or 2nd week of life • Soft, bluish mass deep to the eyelid • Superonasal orbit • Rapidly expands over 6-12 months • Increases with valsalva (crying) • Clinical findings • Proptosis Astigmatism • Strabismus Amblyopia INFANTILE/Capillary Hemangioma • May enlarge for 1-2 years then regress • 70-80% resolve before age 7 • HIGH flow on doppler • Kasabach-Merritt Syndrome • Multiple large visceral capillary hemangiomas • Sequestration of platelets into tumor • Consumptive thrombocytopenia • Supportive therapy and treat underlying tumor • Complications • DIC • death •Homogenous -

Epiphora (Excessive Tearing)
EPIPHORA (EXCESSIVE TEARING) INTRODUCTION Epiphora, or excessive tearing, is the overflow of tears from one or both eyes. Epiphora can occur all the time or only sometimes. It can be split into two categories. Either too many tears are produced or not enough of the tears are cleared. The following information will focus on tears not being cleared. ANATOMY The part of your body that makes tears is the lacrimal apparatus (See Figure 1). It is a system of tubes and sacs. It begins at the outer corner of your eyes in the lacrimal gland. This is the gland that produces tears. Tears then wash across the surface of the eye from the outer to inner corner, protecting, moistening and cleaning the outer layer of the eye. The upper and lower eyelids each have a single opening near the inner corner. These openings are on slightly raised mounds called puncta (See Figure 2). Each punctum drains tears into a tube called the canaliculus. There is an upper and lower canaliculus. Each of these small tubes drains tears into a larger tube called the common canaliculus. The common canaliculus delivers tears to the lacrimal sac, which is under the inner corner of the eye near the nose. The duct then drains tears from the lacrimal sac into the nose. Tears enter the nasal cavity through an opening near the bottom known as Hasner's valve. Too much tearing can result from problems that happen anywhere along this path. A common area to see obstruction is in the nasolacrimal duct. Figure 1. -

Nasolacrimal Duct Flushes in Rabbits
Practice Tip Nasolacrimal Duct Flushes in Rabbits Anthony A. Pilny, DVM, DABVP (Avian) The Center for Avian and Exotic Medicine New York, New York he nasolacrimal system of rabbits consists of a single punctum located in the ventral eyelid near the medial canthus (FIGURE 1). TThe lacrimal sac is rostral to the punctum and caudal to the nasolacrimal duct aperture. The duct extends from the orbit to the nasal fossa, exiting on the ventromedial aspect of the alar fold just caudal to the mucocutaneous junction of the nares. • The most common indication for nasolacrimal duct flushing is unilateral or bilateral epiphora secondary to an obstructed nasolacrimal duct (FIGURE 2). Most of these rabbits present without other clinical signs and are healthy other than the ocular discharge. In other cases, the epiphora is secondary to infection (e.g., Pasteurella multocida), elon- gation of maxillary incisor or first premolar roots, or dental abscessation. Figure 2. Epiphora in a pet rabbit. Note the hair loss from chronic tearing. The A condition resolved completely after appropriate nasolacrimal duct flushes. • Treatment of epiphora in rabbits involves irrigation of the B nasolacrimal duct to restore patency. After a topical anes- thetic (e.g., proparacaine HCI 0.5%) has been instilled and proper restraint instituted, the lower eyelid can be abducted and the punctum identified. Although a lacrimal cannula can be used, a 22- or 24-gauge standard intravenous catheter works well and is most commonly used (FIGURE 3). In most cases, lubrication is not needed to insert the catheter. Magnification may help in identifying the punctum in smaller rabbits or those with conjunctivitis. -

Dry Eye Syndrome: Excessive Tear Evaporation
IOWA CITY DEPARTMENT OF VETERANS AFFAIRS (VA) MEDICAL CENTER Medical Center 601 Highway 6 West, Iowa City, IA 52246-2208 Community-Based Outpatient Clinics 2979 Victoria Street, Bettendorf, IA 52722-2784 200 Mercy Drive, Suite 106, Dubuque, IA 52201-7343 387 E. Grove Street, Galesburg, IL 61401-3728 721 Broadway, Quincy, IL 62301-2708 1015 S. Hackett, Waterloo, IA 50701-3500 Coralville Clinic: 520 10th Avenue, Suite 200, Coralville, IA 52241-1923 Dry Eye Syndrome: Excessive Tear Evaporation Dry eye syndromes can be caused by excessive tear evaporation. The root cause of this condition is obstruction and poor quality of the eyelid (meibomian) oil glands. These glands are responsible for coating the tears with a layer of oil that helps prevent evaporation. Meibomian gland dysfunction, or, more simply, MGD, is the most common dry eye syndrome, accounting for approximately 85% of cases. MGD may occur as a consequence of getting older and may be become symptomatic in 10% to 15% of adults over the age of 50. It can also occur in patients with acne rosacea (where it is almost universally present), in patients with multiple allergies (especially those with strong family histories of allergy and/or eczema), and after eye surgery (especially LASIK, but also after cataract or glaucoma surgery). The MOST common symptom of MGD is fluctuation of vision. This is most noticeable during visual tasks that are associated with decreased blinking, such as reading, using the computer, watching television, and driving. It is aggravated during exposure to “evaporative conditions,” such as low environmental humidity and blowing air, especially ceiling and floor fans and heaters or air conditioners. -

Sympathy Crying: Insights from Infrared Thermal Imaging on a Female Sample
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Portsmouth University Research Portal (Pure) RESEARCH ARTICLE Sympathy Crying: Insights from Infrared Thermal Imaging on a Female Sample Stephanos Ioannou1*, Paul Morris2, Samantha Terry2, Marc Baker2, Vittorio Gallese3,4, Vasudevi Reddy2 1 Alfaisal University, Department of Physiological Sciences, College of Medicine, Riyadh, Kingdom of Saudi Arabia, 2 Department of Psychology-Centre for Situated Action and Communication, University of Portsmouth, Portsmouth, United Kingdom, 3 Parma University, Department of Neuroscience, Section of Human Physiology, Parma, Italy, 4 Institute of Philosophy, School of Advanced Study, University of London, London, United Kingdom * [email protected] a11111 Abstract Sympathy crying is an odd and complex mixture of physiological and emotional phenom- ena. Standard psychophysiological theories of emotion cannot attribute crying to a single subdivision of the autonomic nervous system (ANS) and disagreement exists regarding the emotional origin of sympathy crying. The current experiment examines sympathy crying OPEN ACCESS using functional thermal infrared imaging (FTII), a novel contactless measure of ANS activ- Citation: Ioannou S, Morris P, Terry S, Baker M, ity. To induce crying female participants were given the choice to decide which film they Gallese V, Reddy V (2016) Sympathy Crying: Insights wanted to cry to. Compared to baseline, temperature started increasing on the forehead, from Infrared Thermal Imaging on a Female Sample. PLoS ONE 11(10): e0162749.doi:10.1371/journal. the peri-orbital region, the cheeks and the chin before crying and reached even higher tem- pone.0162749 peratures during crying. The maxillary area showed the opposite pattern and a gradual tem- Editor: Alessio Avenanti, University of Bologna, perature decrease was observed compared to baseline as a result of emotional sweating. -

Eye External Anatomy of Eye Accessory Structures
4/22/16 Eye Bio 40B Dr. Kandula External Anatomy of Eye Accessory Structures l Eyebrows l Levator Palpebrae Superioris - opens eye l Eyelashes l Ciliary glands – modified sweat glands l Small sebaceous glands l Sty is inflamed ciliary glands or small sebaceous glands 1 4/22/16 Terms: Lacrimal gland and duct Surface of eye Lacrimal puncta Lacrimal sac Nasolacrimal duct Nasal cavity Tears / Lacrimal fluid l a watery physiologic saline, with a plasma-like consistency, l contains the bactericidal enzyme lysozyme; l it moistens the conjunctiva and cornea, l provides nutrients and dissolved O2 to the cornea. Extrinsic Muscles of the Eye: Lateral/medial rectus Important to know Superior/inferior rectus actions and nerve Superior/inferior oblique supply in table 2 4/22/16 Extrinsic Eye Muscles • Eye movements controlled by six extrinsic eye muscles Four recti muscles § Superior rectus – moves eyeball superiorly supplied by Cranial Nerve III § Inferior rectus - moves eyeball inferiorly supplied by Cranial Nerve III § Lateral rectus - moves eyeball laterally supplied by Cranial Nerve VI § Medial rectus - moves eyeball medially supplied by Cranial Nerve III Extrinsic Eye Muscles Two oblique muscles rotate eyeball on its axis § Superior oblique rotates eyeball inferiorly and laterally and is supplied by Cranial Nerve IV § Inferior oblique rotates superiorly and laterally and is supplied by Cranial Nerve III Convergence of the Eyes l Binocular vision in humans has both eyes looking at the same object l As you look at an object close to your face, -
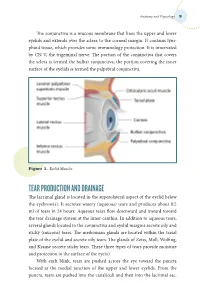
TEAR PRODUCTION and DRAINAGE the Lacrimal Gland Is Located in the Superolateral Aspect of the Eyelid Below the Eyebrow(S)
Anatomy and Physiology 9 The conjunctiva is a mucous membrane that lines the upper and lower eyelids and extends over the sclera to the corneal margin. It contains lym- phoid tissue, which provides some immunology protection. It is innervated by CN V, the trigeminal nerve. The portion of the conjunctiva that covers the sclera is termed the bulbar conjunctiva; the portion covering the inner surface of the eyelids is termed the palpebral conjunctiva. Figure 1. Eyelid Muscles TEAR PRODUCTION AND DRAINAGE The lacrimal gland is located in the superolateral aspect of the eyelid below the eyebrow(s). It secretes watery (aqueous) tears and produces about 0.2 ml of tears in 24 hours. Aqueous tears flow downward and inward toward the tear drainage system at the inner canthus. In addition to aqueous tears, several glands located in the conjunctiva and eyelid margins secrete oily and sticky (mucous) tears. The meibomian glands are located within the tarsal plate of the eyelid and secrete oily tears. The glands of Zeiss, Moll, Wolfing, and Krause secrete sticky tears. These three types of tears provide moisture and protection to the surface of the eye(s). With each blink, tears are pushed across the eye toward the puncta located at the medial junction of the upper and lower eyelids. From the puncta, tears are pushed into the canaliculi and then into the lacrimal sac. 10 Essentials of Ophthalmic Nursing They are drained from the lacrimal sac and nasolacrimal duct to the inside of the nose and down the throat (see Figure 2). Figure 2. Lacrimal System TEAR FILM The tear film has three distinct layers. -

Nasolacrimal Probing and Intubation Chapter 4 53 Nasolacrimal Probing and Intubation 4 Lisa Pierroth, D.A
Chapter 4Nasolacrimal Probing and Intubation Chapter 4 53 Nasolacrimal Probing and Intubation 4 Lisa Pierroth, D.A. Della Rocca and R.C. Della Rocca Core Messages! 4.1 Introduction and Background of the Technique Q We perform the probing first through the upper canaliculus and then through the Congenital nasolacrimal duct obstruction is the most inferior canaliculus. common cause for epiphora in the newborn. The most common location of obstruction is at the opening of Q It is important to not rotate the punctual the nasolacrimal system due to an imperforate valve dilator horizontally before 2 mm of vertical of Hasner [1]. Other causes of obstruction may be dilation, so as to avoid damage to the vertical atypical in the nasolacrimal duct to end, within the part of the canaliculus. bony nasal lacrimal canal, in the wall of the maxillary sinus, or below the inferior turbinate. The nasolacri- Q The probe is advanced medially until a hard mal canal may end as a tube of mucosa lateral to the stop is felt. The lid is pulled laterally to ensure inferior turbinate. that the horizontal canaliculus is not kinked, Embryologically, the lacrimal system proceeds as false passageways must be avoided. from proximal to distal and 30% of full-term new- borns present with an imperforate valve of Hasner [2]. Q The probe is passed 18–20 mm in children Most infants undergo spontaneous valve opening by before entering the nose through the ob- age 6 weeks, but the remaining 10% may require prob- structed site typically at the valve of Hasner.