Pediatric Orbital Tumors and Lacrimal Drainage System
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Ciliary Zonule Sclera (Suspensory Choroid Ligament)
ACTIVITIES Complete Diagrams PNS 18 and 19 Complete PNS 23 Worksheet 3 #1 only Complete PNS 24 Practice Quiz THE SPECIAL SENSES Introduction Vision RECEPTORS Structures designed to respond to stimuli Variable complexity GENERAL PROPERTIES OF RECEPTORS Transducers Receptor potential Generator potential GENERAL PROPERTIES OF RECEPTORS Stimulus causing receptor potentials Generator potential in afferent neuron Nerve impulse SENSATION AND PERCEPTION Stimulatory input Conscious level = perception Awareness = sensation GENERAL PROPERTIES OF RECEPTORS Information conveyed by receptors . Modality . Location . Intensity . Duration ADAPTATION Reduction in rate of impulse transmission when stimulus is prolonged CLASSIFICATION OF RECEPTORS Stimulus Modality . Chemoreceptors . Thermoreceptors . Nociceptors . Mechanoreceptors . Photoreceptors CLASSIFICATION OF RECEPTORS Origin of stimuli . Exteroceptors . Interoceptors . Proprioceptors SPECIAL SENSES Vision Hearing Olfaction Gustation VISION INTRODUCTION 70% of all sensory receptors are in the eye Nearly half of the cerebral cortex is involved in processing visual information Optic nerve is one of body’s largest nerve tracts VISION INTRODUCTION The eye is a photoreceptor organ Refraction Conversion (transduction) of light into AP’s Information is interpreted in cerebral cortex Eyebrow Eyelid Eyelashes Site where conjunctiva merges with cornea Palpebral fissure Lateral commissure Eyelid Medial commissure (a) Surface anatomy of the right eye Figure 15.1a Orbicularis oculi muscle -
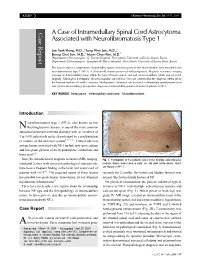
A Case of Intramedullary Spinal Cord Astrocytoma Associated with Neurofibromatosis Type 1
KISEP J Korean Neurosurg Soc 36 : 69-71, 2004 Case Report A Case of Intramedullary Spinal Cord Astrocytoma Associated with Neurofibromatosis Type 1 Jae Taek Hong, M.D.,1 Sang Won Lee, M.D.,1 Byung Chul Son, M.D.,1 Moon Chan Kim, M.D.2 Department of Neurosurgery,1 St. Vincent Hospital, The Catholic University of Korea, Suwon, Korea Department of Neurosurgery,2 Kangnam St. Mary's Hospital, The Catholic University of Korea, Seoul, Korea The authors report a symptomatic intramedullary spinal cord astrocytoma in the thoracolumbar area associated with neurofibromatosis type 1 (NF-1). A 38-year-old woman presented with paraparesis. Magnetic resonance imaging revealed an intramedullary lesion within the lower thoracic spinal cord and conus medullaris, which was removed surgically. Pathological investigation showed anaplastic astrocytoma. This case confirms that the diagnosis criteria set by the National Institute of Health Consensus Development Conference can be useful to differentiate ependymoma from astrocytoma when making a preoperative diagnosis of intramedullary spinal cord tumor in patients of NF-1. KEY WORDS : Astrocytoma·Intramedullary cord tumor·Neurofibromatosis. Introduction eurofibromatosis type 1 (NF-1), also known as von N Recklinghausen's disease, is one of the most common autosomal dominant inherited disorders with an incidence of 1 in 3,000 individuals and is characterized by a predisposition to tumors of the nervous system5,6,12,16). Central nervous system lesions associated with NF-1 include optic nerve glioma and low-grade gliomas of the hypothalamus, cerebellum and brain stem6,10). Since the introduction of magnetic resonance(MR) imaging, Fig. 1. Photograph of the patient's back shows multiple subcutaneous incidental lesions with uncertain pathological characteristic nodules (black arrow) and a cafe-au-lait spot (white arrow), which have been a frequent finding in the brain and spinal cord of are typical of NF-1. -

Adrenaline Dacryolith: Detection by Ultrasound Examination of the Nasolacrimal Duct
Br J Ophthalmol: first published as 10.1136/bjo.72.12.935 on 1 December 1988. Downloaded from British Journal ofOphthalmology, 1988, 72, 935-937 Adrenaline dacryolith: detection by ultrasound examination of the nasolacrimal duct JOHN A BRADBURY,' IAN G RENNIE,' AND M ANDREW PARSONS2 From the Departments of'Ophthalmology and 2Pathology, University ofSheffield SUMMARY A 73-year-old woman on topical pilocarpine and adrenaline for chronic simple glaucoma for three years presented with a mass in the medial canthus of the right eye. Although dacryocystography showed a dilated and partially obstructed nasolacrimal system, ultrasound examination was able to demonstrate a mass in the nasolacrimal duct. At operation a black dacryolith was found, of the diameter predicted by ultrasound. Histological examination of the dacryolith suggested its derivation from breakdown products of adrenaline. Ultrasound examination of the nasolacrimal drain- her right conjunctival sac. In between these acute age system has been shown to be of value when the episodes the epiphora and a slight swelling at the copyright. system is dilated in cases such as a mucocoele or acute medial canthus persisted but were less troublesome. dacryocystitis. It is of limited value in functional Her right nasolacrimal duct had been irrigated during disorders, where the passage of fluid through the one of these acute episodes, which had caused some nasolacrimal system is slowed, producing a minimally resolution of her symptoms. dilated system.' No reports so far have illustrated the On examination a firm mass was palpable over the ability of ultrasound to demonstrate a mass in the right lacrimal fossa extending slightly above the nasolacrimal duct. -

Neuro-Oncology 1 XX(XX), 1–12, 2016 | Doi:10.1093/Neuonc/Now267
Neuro-Oncology 1 XX(XX), 1–12, 2016 | doi:10.1093/neuonc/now267 Defining the temporal course of murine neurofibromatosis-1 optic gliomagenesis reveals a therapeutic window to attenuate retinal dysfunction Joseph A. Toonen, Yu Ma, and David H. Gutmann Department of Neurology, Washington University School of Medicine (WUSM), St Louis, Missouri (J.A.T., Y.M., D.H.G.) Corresponding Author: David H. Gutmann, MD, PhD, Department of Neurology, Washington University, Box 8111, 660 S. Euclid Avenue, St. Louis MO 63110 ([email protected]). Abstract Background. Optic gliomas arising in the neurofibromatosis type 1 (NF1) cancer predisposition syndrome cause reduced visual acuity in 30%–50% of affected children. Since human specimens are rare, genetically engineered mouse (GEM) models have been successfully employed for preclinical therapeutic discovery and validation. However, the sequence of cellular and molecular events that culminate in retinal dysfunction and vision loss has not been fully defined relevant to potential neuroprotective treatment strategies. Methods. Nf1flox/mut GFAP-Cre (FMC) mice and age-matched Nf1flox/flox (FF) controls were euthanized at defined intervals from 2 weeks to 24 weeks of age. Optic nerve volumes were measured, and optic nerves/retinae analyzed by immunohistochemistry. Optical coherence tomography (OCT) was performed on anesthetized mice. FMC mice were treated with lovastatin from 12 to 16 weeks of age. Results. The earliest event in tumorigenesis was a persistent elevation in proliferation (4 wk), which preceded sustained microglia numbers and incremental increases in S100+ glial cells. Microglia activation, as evidenced by increased interleukin (IL)-1β expression and morphologic changes, coincided with axonal injury and retinal ganglion cell (RGC) apoptosis (6 wk). -

Stage Surgery on Inverted Papilloma Which Invaded Lacrimal Sac, Periorbita, Ethmoid and Frontal Sinus
臨床耳鼻:第 27 卷 第 1 號 2016 ••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••••• J Clinical Otolaryngol 2016;27:143-147 증 례 Stage Surgery on Inverted Papilloma which Invaded Lacrimal Sac, Periorbita, Ethmoid and Frontal Sinus Jae-hwan Jung, MD, Minsic Kim, MD, Sue Jean Mun, MD and Hwan-Jung Roh, MD, PhD Department of Otorhinolaryngology-Head & Neck Surgery, Pusan National University Yangsan Hospital, Yangsan, Korea - ABSTRACT - Inverted papilloma of the nasal cavity and the paranasal sinuses is a benign epithelial tumor with a high rate of recurrence, local aggressiveness, and malignant transformation. For these reasons, inverted papilloma has been treated like malignant tumors with extensive surgical resection. With the help of endoscopic sinus surgery tech- nique, it is now available to treat inverted papilloma with stage surgery without severe complications which usu- ally resulted from extensive one stage resection. We report a case of stage surgery on inverted papilloma which invaded lacrimal sac, periorbita, ethmoid and frontal sinus. (J Clinical Otolaryngol 2016;27:143-147) KEY WORDS:Inverted papillomaㆍLacrimal sacㆍPeriorbitaㆍSurgery. Authors present a successful endoscopic stage sur- Introduction gery on IP which invaded lacrimal sac, periorbita, ethmoid and frontal sinus with the literature review. Inverted papilloma (IP) of the nasal cavity and the paranasal sinuses is a benign epithelial tumor with a Case Report high rate of recurrence, local aggressiveness, and ma- lignant transformation.1,2) For these reasons, IP has A 41-year-old female presented in outpatient clinic been treated like malignant tumors with extensive sur- with a complaint of tender swelling mass on the in- gical resection. ner side of her right eye for 5 years which suddenly IP of lacrimal sac and periorbita is rarely reported aggravated 2 months ago. -

Nasolacrimal Duct Flushes in Rabbits
Practice Tip Nasolacrimal Duct Flushes in Rabbits Anthony A. Pilny, DVM, DABVP (Avian) The Center for Avian and Exotic Medicine New York, New York he nasolacrimal system of rabbits consists of a single punctum located in the ventral eyelid near the medial canthus (FIGURE 1). TThe lacrimal sac is rostral to the punctum and caudal to the nasolacrimal duct aperture. The duct extends from the orbit to the nasal fossa, exiting on the ventromedial aspect of the alar fold just caudal to the mucocutaneous junction of the nares. • The most common indication for nasolacrimal duct flushing is unilateral or bilateral epiphora secondary to an obstructed nasolacrimal duct (FIGURE 2). Most of these rabbits present without other clinical signs and are healthy other than the ocular discharge. In other cases, the epiphora is secondary to infection (e.g., Pasteurella multocida), elon- gation of maxillary incisor or first premolar roots, or dental abscessation. Figure 2. Epiphora in a pet rabbit. Note the hair loss from chronic tearing. The A condition resolved completely after appropriate nasolacrimal duct flushes. • Treatment of epiphora in rabbits involves irrigation of the B nasolacrimal duct to restore patency. After a topical anes- thetic (e.g., proparacaine HCI 0.5%) has been instilled and proper restraint instituted, the lower eyelid can be abducted and the punctum identified. Although a lacrimal cannula can be used, a 22- or 24-gauge standard intravenous catheter works well and is most commonly used (FIGURE 3). In most cases, lubrication is not needed to insert the catheter. Magnification may help in identifying the punctum in smaller rabbits or those with conjunctivitis. -

Clinical Manifestations of Hypothalamic Tumors*
ANNALS OF CLINICAL AND LABORATORY SCIENCE, Vol. 10, No. 6 Copyright © 1980, Institute for Clinical Science, Inc. Clinical Manifestations of Hypothalamic Tumors* ADOLFO D. GARNICA, M.D., MICHAEL L. NETZLOFF, M.D.,f and A. L. ROSENBLOOM, M.D. Department of Pediatrics, University of Florida College of Medicine, Gainesville, FL 32610 and f Department of Human Development, Michigan State University East Lansing, MI 88823 ABSTRACT The regulatory function of the central nervous system encompasses di verse endocrine, metabolic, and behavioral processes. Many of these origi nate, are integrated, or are coordinated through hypothalamic pathways or nuclei. Thus, tumors affecting areas projecting to the hypothalamus, tumors of the hypothalamus, and tumors invading or compressing the hypothalamus can produce abnormalities of hypothalamic function. Introduction tary.4,7,31 A secretory function for certain hypothalamic neurons was postulated in Until recently, no endocrine disorder 1928 and subsequently confirmed by the directly attributable to hypothalamic dys demonstration of hormone synthesis in function had been recognized, and the the supraoptic and paraventricular nu majority of endocrine-metabolic homeo clei.28,53 Moreover, observations on the static processes were acknowledged to be effects of environment on the menstrual under the control of the anterior pitui cycles of women and the study of repro tary.48,49 However, in 1901 Frohlich re ductive cycles in animals have shown a ported a patient with a suprasellar tumor, functional connection -

Eye External Anatomy of Eye Accessory Structures
4/22/16 Eye Bio 40B Dr. Kandula External Anatomy of Eye Accessory Structures l Eyebrows l Levator Palpebrae Superioris - opens eye l Eyelashes l Ciliary glands – modified sweat glands l Small sebaceous glands l Sty is inflamed ciliary glands or small sebaceous glands 1 4/22/16 Terms: Lacrimal gland and duct Surface of eye Lacrimal puncta Lacrimal sac Nasolacrimal duct Nasal cavity Tears / Lacrimal fluid l a watery physiologic saline, with a plasma-like consistency, l contains the bactericidal enzyme lysozyme; l it moistens the conjunctiva and cornea, l provides nutrients and dissolved O2 to the cornea. Extrinsic Muscles of the Eye: Lateral/medial rectus Important to know Superior/inferior rectus actions and nerve Superior/inferior oblique supply in table 2 4/22/16 Extrinsic Eye Muscles • Eye movements controlled by six extrinsic eye muscles Four recti muscles § Superior rectus – moves eyeball superiorly supplied by Cranial Nerve III § Inferior rectus - moves eyeball inferiorly supplied by Cranial Nerve III § Lateral rectus - moves eyeball laterally supplied by Cranial Nerve VI § Medial rectus - moves eyeball medially supplied by Cranial Nerve III Extrinsic Eye Muscles Two oblique muscles rotate eyeball on its axis § Superior oblique rotates eyeball inferiorly and laterally and is supplied by Cranial Nerve IV § Inferior oblique rotates superiorly and laterally and is supplied by Cranial Nerve III Convergence of the Eyes l Binocular vision in humans has both eyes looking at the same object l As you look at an object close to your face, -

Anatomy of the Periorbital Region Review Article Anatomia Da Região Periorbital
RevSurgicalV5N3Inglês_RevistaSurgical&CosmeticDermatol 21/01/14 17:54 Página 245 245 Anatomy of the periorbital region Review article Anatomia da região periorbital Authors: Eliandre Costa Palermo1 ABSTRACT A careful study of the anatomy of the orbit is very important for dermatologists, even for those who do not perform major surgical procedures. This is due to the high complexity of the structures involved in the dermatological procedures performed in this region. A 1 Dermatologist Physician, Lato sensu post- detailed knowledge of facial anatomy is what differentiates a qualified professional— graduate diploma in Dermatologic Surgery from the Faculdade de Medician whether in performing minimally invasive procedures (such as botulinum toxin and der- do ABC - Santo André (SP), Brazil mal fillings) or in conducting excisions of skin lesions—thereby avoiding complications and ensuring the best results, both aesthetically and correctively. The present review article focuses on the anatomy of the orbit and palpebral region and on the important structures related to the execution of dermatological procedures. Keywords: eyelids; anatomy; skin. RESU MO Um estudo cuidadoso da anatomia da órbita é muito importante para os dermatologistas, mesmo para os que não realizam grandes procedimentos cirúrgicos, devido à elevada complexidade de estruturas envolvidas nos procedimentos dermatológicos realizados nesta região. O conhecimento detalhado da anatomia facial é o que diferencia o profissional qualificado, seja na realização de procedimentos mini- mamente invasivos, como toxina botulínica e preenchimentos, seja nas exéreses de lesões dermatoló- Correspondence: Dr. Eliandre Costa Palermo gicas, evitando complicações e assegurando os melhores resultados, tanto estéticos quanto corretivos. Av. São Gualter, 615 Trataremos neste artigo da revisão da anatomia da região órbito-palpebral e das estruturas importan- Cep: 05455 000 Alto de Pinheiros—São tes correlacionadas à realização dos procedimentos dermatológicos. -
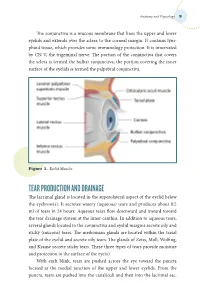
TEAR PRODUCTION and DRAINAGE the Lacrimal Gland Is Located in the Superolateral Aspect of the Eyelid Below the Eyebrow(S)
Anatomy and Physiology 9 The conjunctiva is a mucous membrane that lines the upper and lower eyelids and extends over the sclera to the corneal margin. It contains lym- phoid tissue, which provides some immunology protection. It is innervated by CN V, the trigeminal nerve. The portion of the conjunctiva that covers the sclera is termed the bulbar conjunctiva; the portion covering the inner surface of the eyelids is termed the palpebral conjunctiva. Figure 1. Eyelid Muscles TEAR PRODUCTION AND DRAINAGE The lacrimal gland is located in the superolateral aspect of the eyelid below the eyebrow(s). It secretes watery (aqueous) tears and produces about 0.2 ml of tears in 24 hours. Aqueous tears flow downward and inward toward the tear drainage system at the inner canthus. In addition to aqueous tears, several glands located in the conjunctiva and eyelid margins secrete oily and sticky (mucous) tears. The meibomian glands are located within the tarsal plate of the eyelid and secrete oily tears. The glands of Zeiss, Moll, Wolfing, and Krause secrete sticky tears. These three types of tears provide moisture and protection to the surface of the eye(s). With each blink, tears are pushed across the eye toward the puncta located at the medial junction of the upper and lower eyelids. From the puncta, tears are pushed into the canaliculi and then into the lacrimal sac. 10 Essentials of Ophthalmic Nursing They are drained from the lacrimal sac and nasolacrimal duct to the inside of the nose and down the throat (see Figure 2). Figure 2. Lacrimal System TEAR FILM The tear film has three distinct layers. -

Low-Grade Central Nervous System Tumors
Neurosurg Focus 12 (2):Article 1, 2002, Click here to return to Table of Contents Low-grade central nervous system tumors M. BEATRIZ S. LOPES, M.D., AND EDWARD R. LAWS, JR., M.D. Departments of Pathology (Neuropathology) and Neurological Surgery, University of Virginia Health Sciences Center, Charlottesville, Virginia Low-grade tumors of the central nervous system constitute 15 to 35% of primary brain tumors. Although this cate- gory of tumors encompasses a number of different well-characterized entities, low-grade tumors constitute every tumor not obviously malignant at initial diagnosis. In this brief review, the authors discuss the pathological classification, diagnostic procedures, treatment, and possible pathogenic mechanisms of these tumors. Emphasis is given in the neu- roradiological and pathological features of the several entities. KEY WORDS • glioma • astrocytoma • treatment outcome Low-grade gliomas of the brain represent a large pro- toses. The pilocytic (juvenile) astrocytoma is a character- portion of primary brain tumors, ranging from 15 to 35% istic, more circumscribed lesion occurring primarily in in most reported series.1–5 They include a remarkable di- childhood and with a predilection for being located in the versity of lesions, all of which have been lumped together cerebellum. It usually appears as a cystic tumor with a under the heading of "low-grade glioma." This category mural nodule. The tumor tissue itself may have features of includes virtually every tumor of glial origin that is not microcystic degeneration and Rosenthal fibers which are overtly malignant at the time of initial diagnosis. degenerative structures in the astrocytic processes. Other reasonably common types of low-grade gliomas include CLASSIFICATION OF GLIOMAS the low-grade oligodendroglioma and the low-grade ependymoma, which is usually anatomically related to the Table 1 provides a classification of low-grade tumors of ventricular ependymal lining. -

Nasolacrimal Probing and Intubation Chapter 4 53 Nasolacrimal Probing and Intubation 4 Lisa Pierroth, D.A
Chapter 4Nasolacrimal Probing and Intubation Chapter 4 53 Nasolacrimal Probing and Intubation 4 Lisa Pierroth, D.A. Della Rocca and R.C. Della Rocca Core Messages! 4.1 Introduction and Background of the Technique Q We perform the probing first through the upper canaliculus and then through the Congenital nasolacrimal duct obstruction is the most inferior canaliculus. common cause for epiphora in the newborn. The most common location of obstruction is at the opening of Q It is important to not rotate the punctual the nasolacrimal system due to an imperforate valve dilator horizontally before 2 mm of vertical of Hasner [1]. Other causes of obstruction may be dilation, so as to avoid damage to the vertical atypical in the nasolacrimal duct to end, within the part of the canaliculus. bony nasal lacrimal canal, in the wall of the maxillary sinus, or below the inferior turbinate. The nasolacri- Q The probe is advanced medially until a hard mal canal may end as a tube of mucosa lateral to the stop is felt. The lid is pulled laterally to ensure inferior turbinate. that the horizontal canaliculus is not kinked, Embryologically, the lacrimal system proceeds as false passageways must be avoided. from proximal to distal and 30% of full-term new- borns present with an imperforate valve of Hasner [2]. Q The probe is passed 18–20 mm in children Most infants undergo spontaneous valve opening by before entering the nose through the ob- age 6 weeks, but the remaining 10% may require prob- structed site typically at the valve of Hasner.