Computer Acquisition of Nuclear Medicine Images
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

US Army Photography Course Laboratory Procedures SS0509
SUBCOURSE EDITION SS0509 8 LABORATORY PROCEDURES US ARMY STILL PHOTOGRAPHIC SPECIALIST MOS 84B SKILL LEVEL 1 AUTHORSHIP RESPONSIBILITY: SSG Dennis L. Foster 560th Signal Battalion Visual Information/Calibration Training Development Division Lowry AFB, Colorado LABORATORY PROCEDURES SUBCOURSE NO. SS0509-8 (Developmental Date: 30 June 1988) US Army Signal Center and Fort Gordon Fort Gordon, Georgia Five Credit Hours GENERAL The laboratory procedures subcourse is designed to teach tasks related to work in a photographic laboratory. Information is provided on the types and uses of chemistry, procedures for processing negatives and prints, and for mixing and storing chemicals, procedures for producing contact and projection prints, and photographic quality control. This subcourse is divided into three lessons with each lesson corresponding to a terminal learning objective as indicated below. Lesson 1: PREPARATION OF PHOTOGRAPHIC CHEMISTRY TASK: Determine the types and uses of chemistry, for both black and white and color, the procedures for processing negatives and prints, the procedures for mixing and storing chemicals. CONDITIONS: Given information and diagrams on the types of chemistry and procedures for mixing and storage. STANDARDS: Demonstrate competency of the task skills and knowledge by correctly responding to at least 75% of the multiple-choice test covering preparation of photographic chemistry. (This objective supports SM tasks 113-578-3022, Mix Photographic Chemistry; 113-578-3023, Process Black and White Film Manually; 113-578-3024, Dry Negatives in Photographic Film Drier; 113-578-3026, Process Black and White Photographic Paper). i Lesson 2: PRODUCE A PHOTOGRAPHIC PRINT TASK: Perform the procedures for producing an acceptable contact and projection print. -

SPR 2013 Postgraduate Course May 14-15, 2013 SAM Questionnaire Tuesday, May 14, 2013 CHEST Digital Radiography Robert Macdougal
SPR 2013 Postgraduate Course May 14-15, 2013 SAM Questionnaire Tuesday, May 14, 2013 CHEST Digital Radiography Robert MacDougall, MSc 1. Which of the following is unaffected by the selection of Value of Interest Look Up Table (VOI-LUT): A. Diagnostic information in the processed image B. Target Exposure (ET) C. Exposure Index (EI) D. Deviation Index (DI) E. Brightness and contrast of the displayed image Correct Answer: B 2. Exposure Index (EI) represents: A. The exposure at the entrance to the patient B. The exposure at the detector plane measured with an ion chamber C. The brightness of the displayed image D. The exposure at the detector calculated from the mean signal response of the detector within the Values of Interest E. The deviation from a target exposure Correct Answer: D References 1. An Exposure Indicator for Digital Radiography: Report of AAPM Task Group 116. American Association of Physicists in Medicine. Accessed April 10, 2013. https://www.aapm.org/pubs/reports/RPT_116.pdf 2. Internation Electrotechnical Commission. Medical Electrical Equipment. Exposure Index of Digital X-ray Imaging Systems - Part 1: Definitions and Requirements for General Radiography. IEC Publication No. 62494-1. Geneva, Switzerland: International Electrotechnical Commission, 2002. Functional Chest MR Imaging Hyun Woo Goo, MD, PhD 3. Which one of the followings is the LEAST likely limitation of thoracic MR imaging? A. Low signal-to-noise ratio due to the low proton density of the lung B. Potential hazards from ionizing radiation C. Motion artifacts from respiratory motion and cardiac pulsation D. Relatively long examination time E. Susceptibility artifacts from multiple air-tissue interfaces Correct Answer: B References 1. -
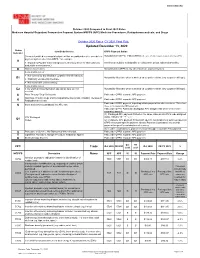
Updated December 13, 2020
WWW.SNMMI.ORG October 2020 Compared to Final 2021 Rates Medicare Hospital Outpatient Prospective Payment System HOPPS (APC) Medicine Procedures, Radiopharmaceuticals, and Drugs October 2020 Rates CY 2021 Final Rule Updated December 13, 2020 Status Item/Code/Service OPPS Payment Status Indicator Services furnished to a hospital outpatient that are paid under a fee schedule or Not paid under OPPS. Paid by MACs under a fee schedule or payment system other than OPPS. payment system other than OPPS,* for example: A ● Separately Payable Clinical Diagnostic Laboratory Services (Not subject to Services are subject to deductible or coinsurance unless indicated otherwise. deductible or coinsurance.) D Discontinued Codes Not paid under OPPS or any other Medicare payment system. Items and Services: ● Not covered by any Medicare outpatient benefit category Not paid by Medicare when submitted on outpatient claims (any outpatient bill type). E1 ● Statutorily excluded by Medicare ● Not reasonable and necessary Items and Services: E2 ● for which pricing information and claims data are not Not paid by Medicare when submitted on outpatient claims (any outpatient bill type). available G Pass-Through Drug/ Biologicals Paid under OPPS; separate APC payment NonPass-Through Drugs and nonimplantable Biologicals, including Therapeutic Paid under OPPS; separate APC payment K Radiopharmaceuticals Paid under OPPS; payment is packaged into payment for other services. Therefore, Items and Services packaged into APC rate N there is no separate APC payment. Paid under OPPS; Addendum B displays APC assignments when services are separately payable. (1) Packaged APC payment if billed on the same claim as a HCPCS code assigned STV-Packaged status indicator “S,” “T,” or “V.” Q1 Codes (2) Composite APC payment if billed with specific combinations of services based on OPPS composite-specific payment criteria. -

Fresnel Zone Plate Imaging in Nuclear Medicine
FRESNEL ZONE PLATE IMAGING IN NUCLEAR MEDICINE Harrison H. Barrett Raytheon Research Division, Waltham, Massachusetts Considerable progress has been made in recent so that there is essentially no collimation. The zone years in detecting the scintillation pattern produced plate has a series of equi-area annular zones, alter by a gamma-ray image. Systems such as the Anger nately transparent and opaque to the gamma rays, camera (7) and Autoflouroscope (2) give efficient with the edges of the zones located at radii given by counting while an image intensifier camera (3,4) rn = n = 1,2, N. gives better spatial resolution at some sacrifice in (D efficiency. However, the common means of image To understand the operation of this aperture, con formation, the pinhole aperture and parallel-hole sider first a point source of gamma rays. Then collimator, are very inefficient. Only a tiny fraction the scintillation pattern on the crystal is a projected (~0.1-0.01%) of the gamma-ray photons emitted shadow of the zone plate, with the position of the by the source are transmitted to the detector plane shadow depending linearly on the position of the (scintillator crystal), and this fraction can be in source. The shadow thus contains the desired infor creased only by unacceptably degrading the spatial mation about the source location. It may be regarded resolution. It would be desirable, of course, to have as a coded image similar to a hologram. Indeed, a a large-aperture, gamma-ray lens so that good col Fresnel zone plate is simply the hologram of a point lection efficiency and good resolution could be ob source (9). -

Criteria for Acceptability of Medical Radiological Equipment Used in Diagnostic Radiology, Nuclear Medicine and Radiotherapy
EUROPEAN COMMISSION RADIATION PROTECTION N° 162 Criteria for Acceptability of Medical Radiological Equipment used in Diagnostic Radiology, Nuclear Medicine and Radiotherapy Directorate-General for Energy Directorate D — Nuclear Safety & Fuel Cycle Unit D4 — Radiation Protection 2012 This report was prepared by Quality Assurance Reference Centre for the European Commission under contract N°. ENER/10/NUCL/SI2.581655 and represents those organisations’ views on the subject matter. The views and opinions expressed herein do not necessarily state or reflect those of the European Commission and should not be relied upon as a statement of the Commission’s views. The European Commission does not guarantee the accuracy of the data included in this report, nor does it accept responsibility for any use made thereof. Europe Direct is a service to help you find answers to your questions about the European Union Freephone number (*): 00 800 6 7 8 9 10 11 (*) Certain mobile telephone operators do not allow access to 00 800 numbers or these calls may be billed. More information on the European Union is available on the Internet (http://europa.eu). Luxembourg: Publications Office of the European Union, 2012 ISBN 978-92-79-27747-4 doi: 10.2768/22561 © European Union, 2012 Reproduction is authorised provided the source is acknowledged. Printed in Luxembourg 2 FOREWORD Luxembourg, October 2012 The work of the European Commission in the field of radiation protection is governed by the Euratom Treaty and the secondary legislation adopted under it. Council Directive 97/43/Euratom (the Medical Exposure Directive, MED) is the legal act defining the Euratom requirements on radiation protection of patients and of other individuals submitted to medical exposure. -

Diagnostic Radiology Physics Diagnostic This Publication Provides a Comprehensive Review of Topics Relevant to Diagnostic Radiology Physics
A Handbook for Teachers and Students A Handbook for Teachers Diagnostic Diagnostic This publication provides a comprehensive review of topics relevant to diagnostic radiology physics. It is intended to provide the basis for the education of medical physicists in the field of diagnostic radiology. Bringing together the work of 41 authors and reviewers from 12 countries, the handbook covers a broad range of topics including radiation physics, dosimetry and Radiology instrumentation, image quality and image perception, imaging modality specific topics, recent advances in digital techniques, and radiation biology and protection. It is not designed to replace the large number of textbooks available on many aspects of diagnostic radiology physics, but is expected Radiology Physics Physics to fill a gap in the teaching material for medical radiation physics in imaging, providing in a single manageable volume the broadest coverage of topics currently available. The handbook has been endorsed by several international professional bodies and will be of value to those preparing for their certification A Handbook for as medical physicists, radiologists and diagnostic radiographers. Teachers and Students D.R. Dance S. Christofides A.D.A. Maidment I.D. McLean K.H. Ng Technical Editors International Atomic Energy Agency Vienna ISBN 978–92–0–131010–1 1 @ DIAGNOSTIC RADIOLOGY PHYSICS: A HANDBOOK FOR TEACHERS AND STUDENTS The following States are Members of the International Atomic Energy Agency: AFGHANISTAN GHANA OMAN ALBANIA GREECE PAKISTAN ALGERIA GUATEMALA -

Quantitative Schlieren Measurement of Explosively‐Driven Shock Wave
Full Paper DOI: 10.1002/prep.201600097 Quantitative Schlieren Measurement of Explosively-Driven Shock Wave Density, Temperature, and Pressure Profiles Jesse D. Tobin[a] and Michael J. Hargather*[a] Abstract: Shock waves produced from the detonation of the shock wave temperature decay profile. Alternatively, laboratory-scale explosive charges are characterized using the shock wave pressure decay profile can be estimated by high-speed, quantitative schlieren imaging. This imaging assuming the shape of the temperature decay. Results are allows the refractive index gradient field to be measured presented for two explosive sources. The results demon- and converted to a density field using an Abel deconvolu- strate the ability to measure both temperature and pres- tion. The density field is used in conjunction with simulta- sure decay profiles optically for spherical shock waves that neous piezoelectric pressure measurements to determine have detached from the driving explosion product gases. Keywords: Schlieren · Explosive temperature · Quantitative optical techniques 1 Introduction Characterization of explosive effects has traditionally been charge. This work used the quantitative density measure- performed using pressure gages and various measures of ment to estimate the pressure field and impulse produced damage, such as plate dents, to determine a “TNT Equiva- by the explosion as a function of distance. The pressure lence” of a blast [1,2]. Most of the traditional methods, measurement, however, relied on an assumed temperature. however, result in numerous equivalencies for the same The measurement of temperature in explosive events material due to large uncertainties and dependencies of can be considered a “holy grail”, which many researchers the equivalence on the distance from the explosion [3,4]. -

Diffraction-Enhanced X-Ray Imaging of in Vitro Breast Tumours
UNIVERSITY OF HELSINKI REPORT SERIES IN PHYSICS HU-P-D113 DIFFRACTION-ENHANCED X-RAY IMAGING OF IN VITRO BREAST TUMOURS Jani Keyriläinen Division of X-ray Physics Department of Physical Sciences Faculty of Science University of Helsinki Helsinki, Finland Department of Oncology Helsinki University Central Hospital Helsinki, Finland ACADEMIC DISSERTATION To be presented, with the permission of the Faculty of Science of the University of Helsinki, for public criticism in Auditorium D101 of the Department of Physical Sciences (Physicum), Gustaf Hällströmin katu 2, on October 29th, 2004, at 12 o’clock noon. Helsinki 2004 ISSN 0356-0961 ISBN 952-10-1655-8 ISBN 952-10-1656-6 (pdf-version) http://ethesis.helsinki.fi/ Helsinki 2004 Yliopistopaino PREFACE This thesis is based on research done at the Division of X-ray Physics, Department of Physical Sciences, University of Helsinki (HU, Finland), at the Medical Beamline ID17, European Synchrotron Radiation Facility (ESRF, Grenoble, France), and at the departments of Oncology, Pathology and Radiology, Helsinki University Central Hospital (HUCH, Finland), all of which are acknowledged. I wish to express my gratitude to Professor Juhani Keinonen, Ph.D., Head of the Department of Physical Sciences, and to Professor Seppo Manninen, Ph.D., former Head of the Division of X-ray Physics, for the opportunity to work at the Department. I also wish to thank Professor Heikki Joensuu, M.D., Ph.D., Head of the Department of Oncology, and William Thomlinson, Ph.D., former Beamline Responsible, ID17, for allowing me to use the outstanding working facilities of their institutions. I am most grateful to my supervisors, Professor Pekka Suortti, Ph.D., Department of Physical Sciences, and Docent Mikko Tenhunen, Ph.D., Chief Physicist of the Department of Oncology, for proposing to me the topic of this study and guiding me throughout this research work. -

Whole Body MR
Whole Body MR: Techniques and Staging in Oncology ‐ How To • Extent of disease and staging • Response to treatment – Early assessment of response to treatment may allow more individualized therapy • Surveillance • Complications – Osteonecrosis – Infection • Cancer predisposition syndromes screening Condition Associated neoplasms Surveillance NF type I Optic nerve glioma, neurofibromas, leukemia (especially juvenile Annual physical examination; annual ophthalmologic examination in early childhood (to age 5 y); regular myelomonocytic leukemia developmental assessment and blood pressure monitoring; appropriate monitoring by a specialist and myelodysplastic syndromes, MPNST (lifetime risk of 8%–13%), GIST according to CNS, skeletal, or cardiovascular abnormalities (lifetime risk of 6%), pheochromocytoma (1%), rhabdomyosarcoma, neuroblastoma Beckwith- Wilms tu (40%–43%), hepatoblastoma (12-20%), adrenocortical ca, Abdominal US every 3 mo to age 7 y; measurement of serum AFP level every 3 mo to age 4 y; daily Wiedemann neuroblastoma, rhabdomyosarcoma abdominal examination by the caretaker at the discretion of the caretaker or parent; abdominal syndrome examination by a physician every 6 mo MEN 1 Parathyroid gland adenomas (65%–90%), pancreatic neuroendocrine tumors Screening starting at age 5–10 y, including measurement of fasting glucose, calcium, PTH, insulin, (50%–70%), and anterior pituitary gland adenomas (25%–65%) prolactin, and IGF1 levels; annual pancreatic US; pancreatic and pituitary MR imaging every 3–5 y; yearly abdominal CT or MR -

The Integrity of the Image
world press photo Report THE INTEGRITY OF THE IMAGE Current practices and accepted standards relating to the manipulation of still images in photojournalism and documentary photography A World Press Photo Research Project By Dr David Campbell November 2014 Published by the World Press Photo Academy Contents Executive Summary 2 8 Detecting Manipulation 14 1 Introduction 3 9 Verification 16 2 Methodology 4 10 Conclusion 18 3 Meaning of Manipulation 5 Appendix I: Research Questions 19 4 History of Manipulation 6 Appendix II: Resources: Formal Statements on Photographic Manipulation 19 5 Impact of Digital Revolution 7 About the Author 20 6 Accepted Standards and Current Practices 10 About World Press Photo 20 7 Grey Area of Processing 12 world press photo 1 | The Integrity of the Image – David Campbell/World Press Photo Executive Summary 1 The World Press Photo research project on “The Integrity of the 6 What constitutes a “minor” versus an “excessive” change is necessarily Image” was commissioned in June 2014 in order to assess what current interpretative. Respondents say that judgment is on a case-by-case basis, practice and accepted standards relating to the manipulation of still and suggest that there will never be a clear line demarcating these concepts. images in photojournalism and documentary photography are world- wide. 7 We are now in an era of computational photography, where most cameras capture data rather than images. This means that there is no 2 The research is based on a survey of 45 industry professionals from original image, and that all images require processing to exist. 15 countries, conducted using both semi-structured personal interviews and email correspondence, and supplemented with secondary research of online and library resources. -

Whole Body Low Dose Computed Tomography (WBLDCT) Can Be Comparable to Whole-Body Magnetic Resonance Imaging (WBMRI) in the Assessment of Multiple Myeloma
diagnostics Article Whole Body Low Dose Computed Tomography (WBLDCT) Can Be Comparable to Whole-Body Magnetic Resonance Imaging (WBMRI) in the Assessment of Multiple Myeloma Davide Ippolito 1,2,* , Teresa Giandola 1,2, Cesare Maino 1,2 , Davide Gandola 1,2 , Maria Ragusi 1,2, Pietro Andrea Bonaffini 2,3 and Sandro Sironi 2,3 1 Department of Diagnostic Radiology, “San Gerardo” Hospital, via Pergolesi 33, 20900 Monza, MB, Italy; [email protected] (T.G.); [email protected] (C.M.); [email protected] (D.G.); [email protected] (M.R.) 2 School of Medicine, University of Milano-Bicocca, via Cadore 48, 20900 Monza, MB, Italy; pa.bonaffi[email protected] (P.A.B.); [email protected] (S.S.) 3 Department of Diagnostic Radiology, H Papa Giovanni XXIII, Piazza OMS 1, 24127 Bergamo, BG, Italy * Correspondence: [email protected] Abstract: Aim of the study is to compare the agreement between whole-body low-dose computed tomography (WBLDCT) and magnetic resonance imaging (WBMRI) in the evaluation of bone marrow involvement in patients with multiple myeloma (MM). Patients with biopsy-proven MM, who underwent both WBLDCT and WBMRI were retrospectively enrolled. After identifying the presence of focal bone involvement (focal infiltration pattern), the whole skeleton was divided into five Citation: Ippolito, D.; Giandola, T.; anatomic districts (skull, spine, sternum and ribs, pelvis, and limbs). Patients were grouped according Maino, C.; Gandola, D.; Ragusi, M.; to the number and location of the lytic lesions (<5, 5–20, and >20) and Durie and Salmon staging Bonaffini, P.A.; Sironi, S. Whole Body system. The agreement between CT and MRI regarding focal pattern, staging, lesion number, and Low Dose Computed Tomography distribution was assessed using the Cohen Kappa statistics. -

Paleoradiology Imaging Mummies and Fossils
R. K. Chhem · D. R. Brothwell Paleoradiology R. K. Chhem · D. R. Brothwell Paleoradiology Imaging Mummies and Fossils With 390 Figures and 58 Tables 123 Don R. Brothwell, PhD Department of Archaeology The University of York The King’s Manor York Y01 7EP UK Rethy K. Chhem, MD, PhD, FRCPC Department of Diagnostic Radiology and Nuclear Medicine Schulich School of Medicine and Dentistry University of Western Ontario London Health Sciences Centre 339 Windermere Road London, Ontario N6A 5A5 Canada Library of Congress Control Number: 2007936308 ISBN 978-3-540-48832-3 Springer Berlin Heidelberg New York This work is subject to copyright. All rights are reserved, whether the whole or part of the material is concerned, specifically the rights of translation, reprinting, reuse of illustrations, recitation, broadcasting, reproduction on microfilm or in any other way, and storage in data banks. Duplication of this publication or parts thereof is permitted only under the provisions of the German Copyright Law of September 9, 1965, in its current version, and permission for use must always be obtained from Springer-Verlag. Violations are liable for prosecution under the German Copyright Law. Springer is a part of Springer Science+Business Media springer.com © Springer-Verlag Berlin Heidelberg 2008 The use of general descriptive names, registered names, trademarks, etc. in this publication does not imply, even in the absence of a specific statement, that such names are exempt from the relevant protective laws and regulations and therefore free for general use. Product liability: The publishers cannot guarantee the accuracy of any information about dosage and application contained in this book.