Virtual Telepharmacist-Delivered Chronic Care Management Services
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Required Procedural Training in Family Medicine Residency: a Consensus Statement
248 April 2008 Family Medicine Residency Education Required Procedural Training in Family Medicine Residency: A Consensus Statement Melissa Nothnagle, MD; Julie M. Sicilia, MD; Stuart Forman, MD; Jeremy Fish, MD; William Ellert, MD; Roberta Gebhard, DO; Barbara F. Kelly, MD; John L. Pfenninger, MD; Michael Tuggy, MD; Wm. MacMillan Rodney, MD; STFM Group on Hospital Medicine and Procedural Training Background and Objectives: Specific procedural training standards for US family medicine residen- cies do not exist. As a result, family physicians graduate with highly variable procedural skills, and the scope of procedural practice for family physicians remains poorly defined. Our objective was to develop a standard list of required procedures for family medicine residencies. Methods: The Society of Teachers of Family Medicine Group on Hospital and Procedural Training convened a working group of 17 family physician educators. A multi-voting process was used to define categories and propose a list of required procedures for US family medicine residency programs. Results: The group defined five categories of procedures within the scope of family medicine. Consensus was reached for a core list of procedures that all family medicine residents should be able to perform by the time of graduation. Conclusions: Defining standards for procedural training in family medicine will help clarify family medicine’s scope of practice and should benefit both patients and family physicians. We propose that with input from national family medicine organizations, the procedure list presented in this report be used to develop a national standard for required procedural training. (Fam Med 2008;40(4):248-52.) Controversy exists over which procedures should be requirements for procedure skills to include “a list of taught in family medicine residency. -

AAFP Toolkit: Building and Growing a Sustainable Telehealth Program
A Toolkit for Building and Growing a Sustainable Telehealth Program in Your Practice SEPTEMBER 2020 This toolkit was developed in partnership with Manatt Health. About AAFP The American Academy of Family Physicians (AAFP) is the national association of family physicians. It is one of the largest national medical organizations, with 136,700 members in 50 states, D.C., Puerto Rico, the Virgin Islands and Guam, as well as internationally. We are a membership organization in the purest sense: an association of family physicians led by family physicians. With our colleagues throughout the country, we work to solidify family medicine as the cornerstone of a functioning health care system. We lobby government, negotiate with payers, partner with employers, educate patients, and champion family medicine on the national stage. The AAFP exists to support family physicians so they can spend more time doing what they do best: providing quality, cost-effective patient care. About Manatt Health Manatt Health combines firsthand experience in shaping public policy, sophisticated strategy insight, deep analytic capabilities, and legal excellence to provide uniquely valuable professional services to the full range of health industry stakeholders. Manatt has deep expertise in advising providers, states, payers, and health tech companies on developing, providing, and paying for innovative virtual care solutions. Our diverse team of more than 160 attorneys and consultants from Manatt, Phelps & Phillips, LLP, and its consulting subsidiary, Manatt Health Strategies, LLC, is passionate about helping our clients advance their business interests, fulfill their missions, and lead health care into the future. For more information, visit https://www.manatt.com/Health. -

Self-Management Strategies and Patient Education
Self-Management Strategies and Patient Education • Cynthia Olivas, MSN • Nurse Manager: ECHO Pain & Rheumatology TeleECHO Clinics • March 9, 2015 I have nothing to disclose. Objectives 1. Describe Self-Management Strategies 2. Define the Five A’s Model 3. Describe how functional goals can contribute to patient engagement in their plan of care 4. Discuss Performance-Function and Life Improvement Plans 5. Identify how to utilize change plans to engage patients in self-management strategies Chronic Pain Experience • Chronic pain (or any chronic condition) is best understood as a process that evolves over time • The chronic pain experience results from the entire progression of the patient’s illness, the sociocultural context in which it occurs, and the interactions between healthcare professionals and patients Osterweis, M., Kleinman, A. Mechanic, D., Pain and Disability: clinical behavioral and public policy perspectives. Washington, DC: National Academy Press, 1987 Distinction between simple and complex pain Simple: Chronic pain responds to standard treatments • Patient is generally functional • Interactions are mutually satisfying Complex: Chronic pain does not respond to standard treatments (this includes education) • Syndrome across all painful conditions • Declining function over time in spite of progressively more aggressive, expensive, and risky medical treatments • History of complicated or mysterious presentations to multiple providers • Mutually unpleasant interactions (provider to patient – patient to provider – patient to loved ones or acquaintances) Why use the Chronic Care Model for pain care? This model can provide for productive interactions between patient, their families, and the care team. There are six elements to the care model that influence the ability to deliver effective chronic illness care: 1. -

Curriculum of the Faculty of Family Medicine
CURRICULUM OF THE FACULTY OF FAMILY MEDICINE WEST AFRICAN COLLEGE OF PHYSICIANS TABLE OF CONTENTS Chapter One: Introduction 1.1 Introductory statement 1.2 Needs analysis 1.3 Mission of the Faculty 1.4 Aim and Goals of the Residency Training 1.5 The philosophy. Chapter Two: Pre-Entry (Primary) Syllabus 2.1 Aim of the primary exam 2.2 The Primary syllabus 2.3 The Primary revision course 2.4 The Primary examination Chapter Three: Membership Syllabus 3.1 Goal of the membership training 3.2 Introduction/General structure 3.3 Rotations with durations 3.4 Syllabus for core knowledge 3.5 Syllabus for skills acquisition Chapter Four: Fellowship Syllabus 4.1 Goal of the fellowship training 4.2 Introduction/General structure 4.3 Rotations with durations 4.4 Syllabus for core knowledge 4.5 Syllabus for skills acquisition 4.6 Proposal writing 4.7 Dissertation writing 4.8 Casebook writing Chapter Five: Training institutions and requirements for accreditation 5.1 Accreditation procedure 5.2 Accreditation requirements Chapter Six: Assessments 6.1 Introduction 6.2 Summative Assessments 6.3 Formative Assessments 6.4 Mentorship Appendices CHAPTER ONE – INTRODUCTION 1.1 Introductory statement Family medicine is the medical discipline also known as general practice, general medical practice, family practice, or primary care. It is a discipline which integrates several medical specialties into a new whole. It is concerned with the holistic approach to patient care in which the individual is seen in his totality and in the context of his family and community. The trainees in family medicine should be appropriately equipped to meet the contemporary and future health needs of individuals and families within their practice community. -

Supporting Self-Management in Patients with Chronic Illness MARY THOESEN COLEMAN, M.D., PH.D., and KAREN S
Supporting Self-management in Patients with Chronic Illness MARY THOESEN COLEMAN, M.D., PH.D., and KAREN S. NEWTON, M.P.H. University of Louisville School of Medicine, Louisville, Kentucky Support of patient self-management is a key component of effective chronic illness care and improved patient outcomes. Self-management support goes beyond traditional knowledge-based patient education to include processes that develop patient problem-solving skills, improve self-efficacy, and support application of knowledge in real-life situa- tions that matter to patients. This approach also encompasses system- focused changes in the primary care environment. Family physicians can support patient self-management by structuring patient-physician interactions to identify problems from the patient perspective, making office environment changes that remove self-management barriers, and providing education individually and through available com- munity self-management resources. The emerging evidence supports the implementation of practice strategies that are conducive to patient self-management and improved patient outcomes among chronically ill patients. (Am Fam Physician 2005;72:1503-10. Copyright © 2005 American Academy of Family Physicians.) See editorial on global rise in life expectancy and interventions in individual nonmanaged page 1454. an increase in cultural and envi- care practices has yet to be determined.3,5-7 A ronmental risks such as smoking, review7 of 41 studies assessing interventions unhealthy diet, lack of physical to improve diabetes outcomes in primary A activity, and air pollution are associated with care revealed that adding patient-oriented an epidemic of chronic illness. Approxi- interventions can lead to improvements mately 120 million Americans have one or in outcomes such as glycemic control. -

Exploring Indonesia's “Low Hospital Bed Utilization- Low Bed Occupancy-High Disease Burden” Paradox
www.sciedu.ca/jha Journal of Hospital Administration, 2013, Vol. 2, No.1 ORIGINAL ARTICLE Exploring Indonesia’s “low hospital bed utilization- low bed occupancy-high disease burden” paradox Niyi Awofeso1, 2, Anu Rammohan3, Ainy Asmaripa4 1. School of Population Health, University of Western Australia, Cnr Gordon & Clifton Street Nedlands Campus, Australia. 2. School of Public Health, University of New South Wales, Sydney, Australia. 3. School of Business, Discipline of Economics, University of Western Australia, Crawley campus, Australia. 4. Faculty of Public health, Sriwijaya University, Indonesia Correspondence: Niyi Awofeso. Address: School of Population Health, University of Western Australia, M431, Cnr Gordon & Clifton Street Nedlands Campus, 6009, Australia. E-mail: [email protected] Received: October 8, 2012 Accepted: October 28, 2012 Online Published: November 22, 2012 DOI: 10.5430/jha.v2n1p49 URL: http://dx.doi.org/10.5430/jha.v2n1p49 Abstract Indonesia’s current hospital bed to population ratio of 6.3/10,000 compares unfavourably with a global average of 30/10,000. Despite low hospital bed-to-population ratio and a significant “double burden” of disease, bed occupancy rates range between 55% - 60% in both government and private hospitals in Indonesia, compared with over 80% hospital bed occupancy rates for the South-East Asian region. Annual inpatient admission in Indonesia is, at 140/10,000 population, the lowest in the South East Asian region. Despite currently low utilisation rates, Indonesia’s Human Resources for Health Development Plan 2011-2025 has among its objectives the expansion of hospital bed numbers to 10/10,000 population by 2014. The authors examined the reasons for the paradox and analysed the following contributory factors; health system’s shortcomings; epidemiological transition; medical tourism; high out-of-pocket payments; patronage of traditional medical practitioners, and increasing use of outpatient care. -

Family Physicians As Team Leaders: “Time” to Share the Care
VOLUME 6: NO. 2, A59 APRIL 2009 SPECIAL TOPIC Family Physicians as Team Leaders: “Time” to Share the Care Kimberly S. H. Yarnall, MD, Truls Østbye, MD, PhD, Katrina M. Krause, MA, Kathryn I. Pollak, PhD, Margaret Gradison, MD, J. Lloyd Michener, MD Suggested citation for this article: Yarnall KSH, Østbye T, Several interventions to improve preventive service Krause KM, Pollak KI, Gradison M, Michener JL. Family delivery and chronic disease management have been physicians as team leaders: “time” to share the care. tested. For example, Put Prevention Into Practice was an Prev Chronic Dis 2009;6(2):A59. http://www.cdc.gov/pcd/ effort to reorganize the delivery of preventive services, but issues/2009/apr/08_0023.htm. Accessed [date]. evaluations of this program failed to show significant sus- tained increases in preventive service delivery (4). Efforts PEER REVIEWED to automate reminder systems and improve efficiency in both prevention and chronic disease management have yielded initial improvements in randomized trials (5), but Abstract the effectiveness of computerized prompts appears to drop rapidly in the 6 months after implementation (6). A major contributor to shortfalls in delivery of recom- mended health care services is lack of physician time. On The common denominator in the failure to deliver ser- the basis of recommendations from national clinical care vices is probably lack of physician time. Our previous anal- guidelines for preventive services and chronic disease yses have suggested that primary care physicians simply management, and including the time needed for acute do not have enough time to deliver all the preventive and concerns, sufficiently addressing the needs of a standard chronic disease services recommended in national clinical patient panel of 2,500 would require 21.7 hours per day. -

Ophthalmology Lecture 2: Red Eye for the Family Physician
University of Massachusetts Medical School eScholarship@UMMS PEER Liberia Project UMass Medical School Collaborations in Liberia 2020-06-08 Ophthalmology Lecture 2: Red Eye for the Family Physician Louis Oteng-Gyimah Sunyani SDA Hospital Let us know how access to this document benefits ou.y Follow this and additional works at: https://escholarship.umassmed.edu/liberia_peer Part of the Eye Diseases Commons, Family Medicine Commons, Medical Education Commons, and the Ophthalmology Commons Repository Citation Oteng-Gyimah L. (2020). Ophthalmology Lecture 2: Red Eye for the Family Physician. PEER Liberia Project. https://doi.org/10.13028/z1ka-g173. Retrieved from https://escholarship.umassmed.edu/ liberia_peer/41 This material is brought to you by eScholarship@UMMS. It has been accepted for inclusion in PEER Liberia Project by an authorized administrator of eScholarship@UMMS. For more information, please contact [email protected]. RED EYE FOR THE FAMILY PHYSICIAN ELWA Family Medicine Residency Program LOUIS OTENG-GYIMAH, MBChB, MGCS OPHTHALMOLOGIST @ SUNYANI SDA HOSPITAL BONO REGION, GHANA INTRODUCTION For the primary care physician, the occurrence of a red eye is a frequent and prominent finding of a disease process in patients. A careful history and simple examination with the observation of typical clinical signs are important for the management of this common disorder. The causes can be classified as painful red eye, trauma, and other common conditions. The most frequent causes of a red eye, such as dry eye, conjunctivitis, keratitis, iritis, acute glaucoma, subconjunctival hematoma, foreign bodies, corneal abrasion, and blunt or penetrating trauma Often benign and self-limiting, some diseases associated with a red eye can nevertheless threaten eyesight or even life. -

Family Caregivers Providing Complex Chronic Care
OCTOBER 2012 HOME ALONE: Family Caregivers Providing Complex Chronic Care Susan C. Reinhard, RN, PhD Senior Vice President and Director, AARP Public Policy Institute Carol Levine, MA Director, Families and Health Care Project, United Hospital Fund Sarah Samis, MPA Senior Health Policy Analyst, United Hospital Fund funded by HOME ALONE: Family Caregivers Providing Complex Chronic Care Susan C. Reinhard, RN, PhD Senior Vice President and Director, AARP Public Policy Institute Carol Levine, MA Director, Families and Health Care Project, United Hospital Fund Sarah Samis, MPA Senior Health Policy Analyst, United Hospital Fund AARP’s Public Policy Institute informs and stimulates public debate on the issues we face as we age. Through research, analysis and dialogue with the nation’s leading experts, PPI promotes development of sound, creative policies to address our common need for economic security, health care, and quality of life. The United Hospital Fund is a nonprofit health services research and philanthropic organization whose primary mission is to shape positive change in health care for the people of New York. We advance policies and support programs that promote high- quality, patient-centered health care services that are accessible to all. We undertake research and policy analysis to improve the financing and delivery of care in hospitals, health centers, nursing homes, and other care settings. We raise funds and give grants to examine emerging issues and stimulate innovative programs. And we work collaboratively with civic, professional, and volunteer leaders to identify and realize opportunities for change. The views expressed herein are for information, debate, and discussion, and do not necessarily represent official policies of AARP or the United Hospital Fund. -
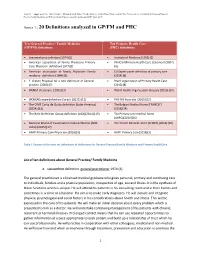
Annex 1 ; 20 Definitions Analyzed in GP/FM and PHC
Annex 1 ; supplement to ; Marc Jamoulle, Melissa Resnick, Robert Vander Stichele, Ashwin Ittoo, Elena Cardillo, Marc Vanmeerbeek. Analysis of definitions of General Practice/Family Medicine and Primary Health Care (accepted for publication BJGP Open 2017) Annex 1 ; 20 Definitions analyzed in GP/FM and PHC Ten General Practice / Family Medicine Ten Primary Health Care (GP/FM) definitions (PHC) definitions • Leeuwenhorst definition (1974)(1) • Institute of Medicine (1996) (2) • American association of Family Physicians Primary • PAHO (4)Primary Health Care statement (2007) Care Physician definition( 1977)(3) (4) • American association of Family Physicians Family • EU Expert panel definition of primary care medicine definition (1984) (5) (2014) (6) • F. Olesen Proposal for a new definition of General • Brazil organization of Primary Health Care practice (2000) (7) (2013) (8) • WONCA dictionary ( 2003) (9) • World Health Organization Glossary (2016) (10) • WONCA Europe definition Euract (2011) (11) • PHC-RIS Australia (2015)(12) • The CIMF Carta de Quito definition (Latin América) • The Belgian Medical Home (FMMCSF) (2014) (13) (2016)(14) • The Role Definition Group definition (USA)(2014) (15) • The Primary care medical home (AHRQ)(2016)(16) • National Board of Examination India definition (NBE • The French Medical Home (FFMPS) (2016) (18) India) (2015) (17) • AAFP Primary Care Physician (2016)(3) • AAFP Primary Care (2016)(3) Table 1 Sources of the two set definitions of definitions for General Practice/Family Medicine and Primary HealthCare List of ten definitions about General Practice/ Family Medicine 1. Leeuwenhorst definition general practitioner 1974 (1) The general practitioner is a licensed medical graduate who gives personal, primary and continuing care to individuals, families and a practice population, irrespective of age, sex and illness. -

Introductory Ophthalmology for Internists
Common Eye Conditions Every Primary Care Clinician Should Know Cynthia S. Chiu, MD, FACS Associate Professor UCSF Department of Ophthalmology UCSF Family Medicine Board Review March 9, 2016 http://www.timandjeni.com/images/cookiemonster.jpg Disclosure I have no financial interest in any of the products mentioned in this presentation The Eye Exam Eye Vital Sign Near Vision Card Held at 14 inches Glasses as needed http://www.drbanker.com/images/Nearvision.gif Pupils Look for afferent pupillary defect Swinging flashlight test +APD indicates optic nerve or large retinal lesion http://img.tfd.com/ElMill/thumb/F0P-24-S2958.jpg Motility Six extraocular muscles Test cardinal fields of gaze http://www.opsweb.org/OpPhoto/Extern/Motility/muscle.jpg http://www.opsweb.org/OpPhoto/Extern/Motility/9gazedwg.jpg Confrontational Visual Fields Cover eyes on same side Hold fingers midway between Normal per eye: 60-60-60-90 http://www.ncbi.nlm.nih.gov/bookshelf/br.fcgi?book=cm&part=A3460&rendertype=figure&id=A3464 Penlight Exam Lids Lashes Conjunctiva/Sclera Cornea Iris/Pupil Puncta Lens http://cache.heraldinteractive.com/blogs/sports/rap_sheet/wp-content/uploads/2009/11/bionic-eye.jpg Anterior Chamber Depth Deep chamber: illumination of nasal iris Shallow chamber: shadow on nasal iris Dilation: Phenylephrine 2.5%, Tropicamide 1% http://iei.ico.edu/images/anatomy.jpg http://www.ophthobook.com/wp-content/uploads/2007/12/video-glaucoma-shallowpenlight.jpg Fundoscopy PanOptic or Direct Ophthalmoscope Evaluate optic nerve, retinal vessels, macula -

GLOSSARY of TERMS WHO European Primary Health Care Impact, Performance and Capacity Tool (PHC-IMPACT)
GLOSSARY OF TERMS WHO European Primary Health Care Impact, Performance and Capacity Tool (PHC-IMPACT) WHO European Framework for Action on Integrated Health Services Delivery Glossary of terms WHO European Primary Health Care Impact, Performance and Capacity Tool (PHC-IMPACT) Series editors Juan Tello, WHO Regional Office for Europe Erica Barbazza, University of Amsterdam Zhamin Yelgezekova, WHO European Centre for Primary Health Care Ioana Kruse, WHO European Centre for Primary Health Care Niek Klazinga, University of Amsterdam Dionne Kringos, University of Amsterdam WHO European Framework for Action on Integrated Health Services Delivery Abstract This glossary of terms aims to provide clarifying definitions related to the WHO European Primary Health Care Impact, Performance and Capacity Tool (PHC-IMPACT). PHC-IMPACT sets out to support the monitoring and improvement of primary health care in the European Region and the measurement of progress towards the services delivery component of global universal health coverage targets. The framework underpinning PHC-IMPACT has been guided by the WHO European Framework for Integrated Health Services Delivery. This glossary of terms accompanies PHC-IMPACT’s Indicator Passports – a resource providing detailed information for the use of the full suite of indicators that make up the tool. Importantly, the definitions included here have relied as far as possible on existing international classifications including the International Classification for Health Accounts, International Standard Classification of Occupations and International Standard Classification of Education. Keywords HEALTH SERVICES PRIMARY HEALTH CARE HEALTH CARE SYSTEMS HEALTH POLICY EUROPE Address requests about publications of the WHO Regional Office for Europe to: Publications WHO Regional Office for Europe UN City, Marmorvej 51 DK-2100 Copenhagen Ø Denmark Alternatively, complete an online request form for documentation, health information, or for permission to quote or translate, on the Regional Office website (http://www.euro.who.int/pubrequest).