FMHC's Patient Newsletter
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Required Procedural Training in Family Medicine Residency: a Consensus Statement
248 April 2008 Family Medicine Residency Education Required Procedural Training in Family Medicine Residency: A Consensus Statement Melissa Nothnagle, MD; Julie M. Sicilia, MD; Stuart Forman, MD; Jeremy Fish, MD; William Ellert, MD; Roberta Gebhard, DO; Barbara F. Kelly, MD; John L. Pfenninger, MD; Michael Tuggy, MD; Wm. MacMillan Rodney, MD; STFM Group on Hospital Medicine and Procedural Training Background and Objectives: Specific procedural training standards for US family medicine residen- cies do not exist. As a result, family physicians graduate with highly variable procedural skills, and the scope of procedural practice for family physicians remains poorly defined. Our objective was to develop a standard list of required procedures for family medicine residencies. Methods: The Society of Teachers of Family Medicine Group on Hospital and Procedural Training convened a working group of 17 family physician educators. A multi-voting process was used to define categories and propose a list of required procedures for US family medicine residency programs. Results: The group defined five categories of procedures within the scope of family medicine. Consensus was reached for a core list of procedures that all family medicine residents should be able to perform by the time of graduation. Conclusions: Defining standards for procedural training in family medicine will help clarify family medicine’s scope of practice and should benefit both patients and family physicians. We propose that with input from national family medicine organizations, the procedure list presented in this report be used to develop a national standard for required procedural training. (Fam Med 2008;40(4):248-52.) Controversy exists over which procedures should be requirements for procedure skills to include “a list of taught in family medicine residency. -

AAFP Toolkit: Building and Growing a Sustainable Telehealth Program
A Toolkit for Building and Growing a Sustainable Telehealth Program in Your Practice SEPTEMBER 2020 This toolkit was developed in partnership with Manatt Health. About AAFP The American Academy of Family Physicians (AAFP) is the national association of family physicians. It is one of the largest national medical organizations, with 136,700 members in 50 states, D.C., Puerto Rico, the Virgin Islands and Guam, as well as internationally. We are a membership organization in the purest sense: an association of family physicians led by family physicians. With our colleagues throughout the country, we work to solidify family medicine as the cornerstone of a functioning health care system. We lobby government, negotiate with payers, partner with employers, educate patients, and champion family medicine on the national stage. The AAFP exists to support family physicians so they can spend more time doing what they do best: providing quality, cost-effective patient care. About Manatt Health Manatt Health combines firsthand experience in shaping public policy, sophisticated strategy insight, deep analytic capabilities, and legal excellence to provide uniquely valuable professional services to the full range of health industry stakeholders. Manatt has deep expertise in advising providers, states, payers, and health tech companies on developing, providing, and paying for innovative virtual care solutions. Our diverse team of more than 160 attorneys and consultants from Manatt, Phelps & Phillips, LLP, and its consulting subsidiary, Manatt Health Strategies, LLC, is passionate about helping our clients advance their business interests, fulfill their missions, and lead health care into the future. For more information, visit https://www.manatt.com/Health. -

Curriculum of the Faculty of Family Medicine
CURRICULUM OF THE FACULTY OF FAMILY MEDICINE WEST AFRICAN COLLEGE OF PHYSICIANS TABLE OF CONTENTS Chapter One: Introduction 1.1 Introductory statement 1.2 Needs analysis 1.3 Mission of the Faculty 1.4 Aim and Goals of the Residency Training 1.5 The philosophy. Chapter Two: Pre-Entry (Primary) Syllabus 2.1 Aim of the primary exam 2.2 The Primary syllabus 2.3 The Primary revision course 2.4 The Primary examination Chapter Three: Membership Syllabus 3.1 Goal of the membership training 3.2 Introduction/General structure 3.3 Rotations with durations 3.4 Syllabus for core knowledge 3.5 Syllabus for skills acquisition Chapter Four: Fellowship Syllabus 4.1 Goal of the fellowship training 4.2 Introduction/General structure 4.3 Rotations with durations 4.4 Syllabus for core knowledge 4.5 Syllabus for skills acquisition 4.6 Proposal writing 4.7 Dissertation writing 4.8 Casebook writing Chapter Five: Training institutions and requirements for accreditation 5.1 Accreditation procedure 5.2 Accreditation requirements Chapter Six: Assessments 6.1 Introduction 6.2 Summative Assessments 6.3 Formative Assessments 6.4 Mentorship Appendices CHAPTER ONE – INTRODUCTION 1.1 Introductory statement Family medicine is the medical discipline also known as general practice, general medical practice, family practice, or primary care. It is a discipline which integrates several medical specialties into a new whole. It is concerned with the holistic approach to patient care in which the individual is seen in his totality and in the context of his family and community. The trainees in family medicine should be appropriately equipped to meet the contemporary and future health needs of individuals and families within their practice community. -

Ophthalmology Lecture 2: Red Eye for the Family Physician
University of Massachusetts Medical School eScholarship@UMMS PEER Liberia Project UMass Medical School Collaborations in Liberia 2020-06-08 Ophthalmology Lecture 2: Red Eye for the Family Physician Louis Oteng-Gyimah Sunyani SDA Hospital Let us know how access to this document benefits ou.y Follow this and additional works at: https://escholarship.umassmed.edu/liberia_peer Part of the Eye Diseases Commons, Family Medicine Commons, Medical Education Commons, and the Ophthalmology Commons Repository Citation Oteng-Gyimah L. (2020). Ophthalmology Lecture 2: Red Eye for the Family Physician. PEER Liberia Project. https://doi.org/10.13028/z1ka-g173. Retrieved from https://escholarship.umassmed.edu/ liberia_peer/41 This material is brought to you by eScholarship@UMMS. It has been accepted for inclusion in PEER Liberia Project by an authorized administrator of eScholarship@UMMS. For more information, please contact [email protected]. RED EYE FOR THE FAMILY PHYSICIAN ELWA Family Medicine Residency Program LOUIS OTENG-GYIMAH, MBChB, MGCS OPHTHALMOLOGIST @ SUNYANI SDA HOSPITAL BONO REGION, GHANA INTRODUCTION For the primary care physician, the occurrence of a red eye is a frequent and prominent finding of a disease process in patients. A careful history and simple examination with the observation of typical clinical signs are important for the management of this common disorder. The causes can be classified as painful red eye, trauma, and other common conditions. The most frequent causes of a red eye, such as dry eye, conjunctivitis, keratitis, iritis, acute glaucoma, subconjunctival hematoma, foreign bodies, corneal abrasion, and blunt or penetrating trauma Often benign and self-limiting, some diseases associated with a red eye can nevertheless threaten eyesight or even life. -
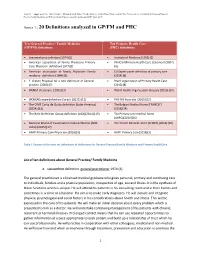
Annex 1 ; 20 Definitions Analyzed in GP/FM and PHC
Annex 1 ; supplement to ; Marc Jamoulle, Melissa Resnick, Robert Vander Stichele, Ashwin Ittoo, Elena Cardillo, Marc Vanmeerbeek. Analysis of definitions of General Practice/Family Medicine and Primary Health Care (accepted for publication BJGP Open 2017) Annex 1 ; 20 Definitions analyzed in GP/FM and PHC Ten General Practice / Family Medicine Ten Primary Health Care (GP/FM) definitions (PHC) definitions • Leeuwenhorst definition (1974)(1) • Institute of Medicine (1996) (2) • American association of Family Physicians Primary • PAHO (4)Primary Health Care statement (2007) Care Physician definition( 1977)(3) (4) • American association of Family Physicians Family • EU Expert panel definition of primary care medicine definition (1984) (5) (2014) (6) • F. Olesen Proposal for a new definition of General • Brazil organization of Primary Health Care practice (2000) (7) (2013) (8) • WONCA dictionary ( 2003) (9) • World Health Organization Glossary (2016) (10) • WONCA Europe definition Euract (2011) (11) • PHC-RIS Australia (2015)(12) • The CIMF Carta de Quito definition (Latin América) • The Belgian Medical Home (FMMCSF) (2014) (13) (2016)(14) • The Role Definition Group definition (USA)(2014) (15) • The Primary care medical home (AHRQ)(2016)(16) • National Board of Examination India definition (NBE • The French Medical Home (FFMPS) (2016) (18) India) (2015) (17) • AAFP Primary Care Physician (2016)(3) • AAFP Primary Care (2016)(3) Table 1 Sources of the two set definitions of definitions for General Practice/Family Medicine and Primary HealthCare List of ten definitions about General Practice/ Family Medicine 1. Leeuwenhorst definition general practitioner 1974 (1) The general practitioner is a licensed medical graduate who gives personal, primary and continuing care to individuals, families and a practice population, irrespective of age, sex and illness. -

Introductory Ophthalmology for Internists
Common Eye Conditions Every Primary Care Clinician Should Know Cynthia S. Chiu, MD, FACS Associate Professor UCSF Department of Ophthalmology UCSF Family Medicine Board Review March 9, 2016 http://www.timandjeni.com/images/cookiemonster.jpg Disclosure I have no financial interest in any of the products mentioned in this presentation The Eye Exam Eye Vital Sign Near Vision Card Held at 14 inches Glasses as needed http://www.drbanker.com/images/Nearvision.gif Pupils Look for afferent pupillary defect Swinging flashlight test +APD indicates optic nerve or large retinal lesion http://img.tfd.com/ElMill/thumb/F0P-24-S2958.jpg Motility Six extraocular muscles Test cardinal fields of gaze http://www.opsweb.org/OpPhoto/Extern/Motility/muscle.jpg http://www.opsweb.org/OpPhoto/Extern/Motility/9gazedwg.jpg Confrontational Visual Fields Cover eyes on same side Hold fingers midway between Normal per eye: 60-60-60-90 http://www.ncbi.nlm.nih.gov/bookshelf/br.fcgi?book=cm&part=A3460&rendertype=figure&id=A3464 Penlight Exam Lids Lashes Conjunctiva/Sclera Cornea Iris/Pupil Puncta Lens http://cache.heraldinteractive.com/blogs/sports/rap_sheet/wp-content/uploads/2009/11/bionic-eye.jpg Anterior Chamber Depth Deep chamber: illumination of nasal iris Shallow chamber: shadow on nasal iris Dilation: Phenylephrine 2.5%, Tropicamide 1% http://iei.ico.edu/images/anatomy.jpg http://www.ophthobook.com/wp-content/uploads/2007/12/video-glaucoma-shallowpenlight.jpg Fundoscopy PanOptic or Direct Ophthalmoscope Evaluate optic nerve, retinal vessels, macula -

GLOSSARY of TERMS WHO European Primary Health Care Impact, Performance and Capacity Tool (PHC-IMPACT)
GLOSSARY OF TERMS WHO European Primary Health Care Impact, Performance and Capacity Tool (PHC-IMPACT) WHO European Framework for Action on Integrated Health Services Delivery Glossary of terms WHO European Primary Health Care Impact, Performance and Capacity Tool (PHC-IMPACT) Series editors Juan Tello, WHO Regional Office for Europe Erica Barbazza, University of Amsterdam Zhamin Yelgezekova, WHO European Centre for Primary Health Care Ioana Kruse, WHO European Centre for Primary Health Care Niek Klazinga, University of Amsterdam Dionne Kringos, University of Amsterdam WHO European Framework for Action on Integrated Health Services Delivery Abstract This glossary of terms aims to provide clarifying definitions related to the WHO European Primary Health Care Impact, Performance and Capacity Tool (PHC-IMPACT). PHC-IMPACT sets out to support the monitoring and improvement of primary health care in the European Region and the measurement of progress towards the services delivery component of global universal health coverage targets. The framework underpinning PHC-IMPACT has been guided by the WHO European Framework for Integrated Health Services Delivery. This glossary of terms accompanies PHC-IMPACT’s Indicator Passports – a resource providing detailed information for the use of the full suite of indicators that make up the tool. Importantly, the definitions included here have relied as far as possible on existing international classifications including the International Classification for Health Accounts, International Standard Classification of Occupations and International Standard Classification of Education. Keywords HEALTH SERVICES PRIMARY HEALTH CARE HEALTH CARE SYSTEMS HEALTH POLICY EUROPE Address requests about publications of the WHO Regional Office for Europe to: Publications WHO Regional Office for Europe UN City, Marmorvej 51 DK-2100 Copenhagen Ø Denmark Alternatively, complete an online request form for documentation, health information, or for permission to quote or translate, on the Regional Office website (http://www.euro.who.int/pubrequest). -

First 15 Family Medicine Residency Programs
Center for the History of Family Medicine 11400 Tomahawk Creek Parkway, Leawood, KS 66211-2672 Telephone: (913) 906-6007 Fax: (913) 906-6095 Administered by the Email: [email protected] American Academy of Family Physicians Website: www.aafpfoundation.org/chfm Foundation THE FIRST FIFTEEN FAMILY MEDICINE RESIDENCY PROGRAMS A frequent question directed to the Center is: “Which Family Medicine residency was the first?” The answer should be simple, but it is not. Many of the earliest residencies were in existence before essentials for Family Medicine residencies were developed. However, some of those residencies were not listed as accredited until several years later. What can be documented are the first fifteen residencies approved by the Residency Review Committee in December 1968 under the new “Essentials for Approved Residencies in Family Practice.” They are as follows*: School Program Program Director or Person in Charge University of California-Irvine Family Medicine Robert Combs, MD College of Medicine Los Angeles, California General Hospital Ventura County Family Practice J.A. Daly, MD Ventura, California University of Miami School of Medicine Division of Family Medicine Lynn P. Carmichael, MD Miami, Florida (Jackson Memorial Hospital) Wesley Medical Center Family Practice Residency G. Gayle Stephens, MD Wichita, Kansas University of Maryland School of Medicine Division of Family Medicine William L. Stewart, MD Baltimore, Maryland (University of Maryland Hospital) Harvard Medical School Family Health Care Program Joel J. Alpert, MD Boston, Massachusetts (Peter Bent Brigham Hospital, Children’s Hospital Medical Center & Family Health Care Program at Harvard) *As printed in “Graduate Training Programs in Family Practice,” December 1968. This printout is now known as Reprint 135-B: ACGME Accredited Residency Programs in Family Practice. -

Roadmap to Choosing a Medical Specialty Questions to Consider
Roadmap to Choosing a Medical Specialty Questions to Consider Question Explanation Examples What are your areas of What organ system or group of diseases do you Pharmacology & Physiology à Anesthesia scientific/clinical interest? find most exciting? Which clinical questions do Anatomy à Surgical Specialty, Radiology you find most intriguing? Neuroscience à Neurology, Neurosurgery Do you prefer a surgical, Do you prefer a specialty that is more Surgical à Orthopedics, Plastics, Neurosurgery medical, or a mixed procedure-oriented or one that emphasizes Mixed à ENT, Ob/Gyn, EMed, Anesthesia specialty? patient relationships and clinical reasoning? Medical à Internal Medicine, Neurology, Psychiatry See more on the academic advising website. What types of activities do Choose a specialty that will allow you to pursue Your activity options will be determined by your practice you want to engage in? your non-medical interests, like research, setting & the time constraints of your specialty. Look at teaching or policy work. the activities physicians from each specialty engage in. How much patient contact Do you like talking to patients & forming Internal & Family Medicine mean long-term patient and continuity do you relationships with them? What type of physical relationships. Radiology & Pathology have basically no prefer? interaction do you want with your patients? patient contact. Anesthesiologists & EMed docs have brief and efficient patient interactions. What type of patient Look at the typical patient populations in each Oncologists have patients with life-threatening diseases. population would you like specialty you’re considering. What type of Pediatricians may deal with demanding parents as well as to work with? physician-patient relationship do you want? sick infants and children. -

Family Medicine Telehealth Clinic with Medical Students Carolyn Peterseim | Kristen Hood Watson, MD Primer
Family Medicine Telehealth Clinic With Medical Students Carolyn Peterseim | Kristen Hood Watson, MD PRiMER. 2020;4:35. Published: 12/21/2020 | DOI: 10.22454/PRiMER.2020.861306 Abstract COVID-19 has altered clinical clerkships for medical students, providing an opportunity for telehealth with medical students to take center stage in the age of technology. This research brief demonstrates why and how to incorporate medical students into telehealth. For the purposes of clinical students, telehealth is a better educational alternative to in-person patient care than online modules. We performed a successful outpatient family medicine telehealth pilot program at the Medical University of South Carolina (MUSC) that is currently being scaled up to other clerkships. This pilot was very limited in scope, but serves as a scalable model for future telehealth programs and curricula incorporating medical students. Introduction Telehealth is an enhanced clinical learning opportunity for clinical medical students and a good substitute for in-person clinical time.1-4 Clinical time is deZned by real-time interaction with real patients. Online modules do have certain utility for board review, but they are not an adequate clinical substitute. Through telehealth, students can see patients, write notes, learn from attendings, and train to operate with modern medical technology. Family medicine is ideal to facilitate telehealth clinical experiences for students, as many clinic visits are follow-up appointments with primary care providers, requiring small changes to their treatment plan. There are some advantages to telehealth over in-person clinical time. Telehealth offers increased accessibility to patients and reduces transportation barriers to care. Providers and students can easily check a patient’s chart during a clinic visit without disrupting it. -

Letter to Our Family Medicine Community May 29,2020
LETTER TO OUR FAMILY MEDICINE COMMUNITY MAY 29, 2020 RE: COVID-19 IMPACTS TO 2020-2021 RESIDENCY INTERVIEW PROCESS The global COVID-19 pandemic will provide unique challenges to both applicants and residency programs in the process of residency selection. The Coalition for Physician Accountability’s Work Group on Medical Students in the Class of 2021 Moving Across Institutions for Post Graduate Training (The Coalition) has made recommendations to assist students and programs in navigating this challenging time. We (the undersigned) have considered these recommendations for their applicability to the 2020-21 residency interview process and the 2021 match for family medicine. Primary considerations include: the health of patients, communities, learners, and the healthcare workforce; a deliberately equitable approach to providing opportunities for students and consideration of candidates; minimizing uncertainty and confusion; maximizing transparency; and the value of a shared response from the “family” of Family Medicine. We concur with The Coalition that “this guidance is intended to add to, but not supersede, the independent judgement of a medical school, sponsoring institution, or residency program.” We agree with The Coalition’s recommendations with additions applicable to family medicine: 1. Away rotations should be discouraged for the 2020-2021 academic year, except under the following circumstances: a. Learners who have an interest in family medicine and do not have access to a clinical experience with a residency program in family medicine in their school’s system. b. Learners for whom an away rotation is required for graduation or accreditation requirements. c. In addition, family medicine residency programs should consider their away rotation policy to accommodate students from institutions or hometowns geographically close to their programs whose medical schools do not offer adequate family medicine clinical experiences to meet student demand. -

The European Definition of General Practice / Family Medicine
THE EUROPEAN DEFINITION OF GENERAL PRACTICE / FAMILY MEDICINE WONCA EUROPE 2011 Edition 1 THE EUROPEAN DEFINITIONS of The Key Features of the Discipline of General Practice The Role of the General Practitioner and A description of the Core Competencies of the General Practitioner / Family Physician. Prepared for WONCA EUROPE (The European Society of General Practice/ Family Medicine), 2002. Dr Justin Allen Director of Postgraduate General Practice Education Centre for Postgraduate Medical Education, University of Leicester, United Kingdom President of EURACT Professor Bernard Gay President, CNGE, Paris, France University of Bordeaux, France Professor Harry Crebolder Maastricht University The Netherlands Professor Jan Heyrman Catholic University of Leuven, Belgium Professor Igor Svab, University of Ljubljana, Slovenia Dr Paul Ram Maastricht University The Netherlands Edited by: Dr Philip Evans President WONCA Europe This statement was published with the support and co-operation of the WHO Europe Office ,Barcelona ,Spain. Revised in 2005 by a working party of EURACT Council led by Dr Justin Allen, on behalf of WONCA European Council. Revised in 2011 by a Commission of the WONCA European Council led by Dr. Ernesto Mola and Dr. Tina Eriksson 2 THE WONCA TREE – AS PRODUCED BY THE SWISS COLLEGE OF PRIMARY CARE (Revised 2011) 3 CONTENTS 1. Introductions Page 3 2. The New Definitions and Competencies Statements Page 5 3. Explanatory notes – rationale and academic review new definitions Page 7 4. Explanatory notes , rationale and academic review - core competencies Page 20 5. Appendices Page 25 Appendix 1 – Leeuwenhorst, WONCA and Olesen definitions Appendix 2 – Acknowledgements Appendix 3 -- English Language definitions Using this document This document contains statements of the characteristics of the discipline and the core competences, and then sections with short explanatory notes.