The Endocrine System
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

WO 2013/096741 A2 27 June 2013 (27.06.2013) P CT
(12) INTERNATIONAL APPLICATION PUBLISHED UNDER THE PATENT COOPERATION TREATY (PCT) (19) World Intellectual Property Organization International Bureau (10) International Publication Number (43) International Publication Date WO 2013/096741 A2 27 June 2013 (27.06.2013) P CT (51) International Patent Classification: (74) Agents: GEORGE, Nikolaos C. et al; Jones Day, 222 A61K 35/12 (2006.01) East 41st Street, New York, NY 10017-6702 (US). (21) International Application Number: (81) Designated States (unless otherwise indicated, for every PCT/US20 12/07 1192 kind of national protection available): AE, AG, AL, AM, AO, AT, AU, AZ, BA, BB, BG, BH, BN, BR, BW, BY, (22) Date: International Filing BZ, CA, CH, CL, CN, CO, CR, CU, CZ, DE, DK, DM, 2 1 December 2012 (21 .12.2012) DO, DZ, EC, EE, EG, ES, FI, GB, GD, GE, GH, GM, GT, (25) Filing Language: English HN, HR, HU, ID, IL, IN, IS, JP, KE, KG, KM, KN, KP, KR, KZ, LA, LC, LK, LR, LS, LT, LU, LY, MA, MD, (26) Publication Language: English ME, MG, MK, MN, MW, MX, MY, MZ, NA, NG, NI, (30) Priority Data: NO, NZ, OM, PA, PE, PG, PH, PL, PT, QA, RO, RS, RU, 61/579,942 23 December 201 1 (23. 12.201 1) US RW, SC, SD, SE, SG, SK, SL, SM, ST, SV, SY, TH, TJ, 61/592,350 30 January 2012 (30.01.2012) US TM, TN, TR, TT, TZ, UA, UG, US, UZ, VC, VN, ZA, 61/696,527 4 September 2012 (04.09.2012) us ZM, ZW. (71) Applicant: ANTHROGENESIS CORPORATION (84) Designated States (unless otherwise indicated, for every [US/US]; 33 Technology Drive, Warren, NJ 07059 (US). -

Human General Histology
135 اووم څپرکي انډوکراين سيستم (Endocrine system) (hormones) (target cells) (receptors) autonomic (sinusoids) ductless glands thyroid gland Pineal gland Hypophysis cerebri(pituitary glands) supra renal( adrenal glands) parathyroid glands 136 اووم څپرکي انډوکراين سيسټم islets cell corpora lutea interstitial tissue (placenta) GIT amines neurotransmitters amines neuromodulator 137 اووم څپرکي انډوکراين سيسټم APUD cells neuroendocrine system system adrenaline, (amino acid derivatives) thyroxin noradrenalin thyroid vasopressin encephalin (small peptides) releasing hormone(TRH) TSH(thyroid stimulating parathormone hormone) cortisol Testosterone estrogen (steroids) 5,12,3 (Hypophysis Cerebri) (brain) pituitary gland (stalk) Ventricle infundibulum stalk pituitary fossa sphenoid pineal hypothalamus body 138 اووم څپرکي انډوکراين سيسټم Hypophysis cerebri Pars pars anterior pars nervosa pars posterior intermediate hypothalamus infundibulum infundibulum stalk )Pars posterior neurohypophysis median eminence (tuber cinereum) infundibulum pars neurohypophysis median eminence pars intermediate pars distalis anterior Adenohypophysis infundibulum pars anterior pars tuberalis adenohypophysis 139 اووم څپرکي انډوکراين سيسټم Adenohypophysis pars intermediate pars anterior adenohypophyisis Pars anterior fenestrated sinusoids (cords) chromophil chromophobic acidophil chromophil basophils orange G eosin PAS-positive hematoxylline Beta cells basophil Alpha cells Acidophil basophils acidophil (dese cored vesicles) alpha Beta Histochemical 140 اووم څپرکي انډوکراين -

The Physiology of Growth by S
Postgrad Med J: first published as 10.1136/pgmj.26.298.417 on 1 August 1950. Downloaded from 417 THE PHYSIOLOGY OF GROWTH BY S. LEONARD SIMPSON, M.A., M.D., F.R.C.P. Consultant Endocrinologist, St. Mary's Hospital, etc.; Formerly Research Wor7Aer, Lister Institute Although clinical and experimental evidence postulated an antagonism between growth and had previously indicated that skeletal growth sex-stimulating hormones. Further observations depended upon the pituitary gland, it was not suggested that corpora lutea were formed before until I92I that Evans and Long, at the University ovulation occurred, and that his emulsions con- of California, demonstrated that a saline emulsion tained gonadotrophic luteinizing hormone. Al- made from the anterior pituitary lobe of fresh though Evans' original giant rats were apparently glands of cattle contained a growth hormone. The adipose, later work (Lee and Schaffer, 1934), hypophyses were thrown into 40 per cent. ethyl showed that there was a retention of nitrogen and alcohol, agitated with a glass rod, transferred to a relative excess of body protein. This was also two changes of sterile normal saline, and triturated true of the excess of tissue deposited in and with force and speed with ocean sand, diluted with around the abdomen. Evans stated in a recent saline, and decanted. The layers of sand, cell discussion in London that rats treated with pure fragments and opaque pink fluid permitted the growth hormone, unlike those in the initial latter to be decanted. This emulsion, when experiments with crude extracts, were not injected daily in doses of I to i ml. -

The Fine Structure of the Parathyroid Gland*
The Fine Structure of the Parathyroid Gland* BY JERRY STEVEN TRIER, M.D. (From the Department of Anatomy, University of Washington School of Medicine, Seattle) PLATES 3 TO 10 (Received for publication, July 29, 1957) ABSTRACT The fine structure of the parathyroid of the macaque is described, and is cor- related with classical parathyroid cytology as seen in the light microscope. The two parenchymal cell types, the chief cells and the oxyphil cells, have been recognized in electron mierographs. The chief cells contain within their cyto- plasm mitochondria, endoplasmic reticulum, and Golgi bodies similar to those found in other endocrine tissues as well as frequent PAS-positive granules. The juxtanuclear body of the light microscopists is identified with stacks of parallel lamellar elements of the endoplasmic rcticulum of the ergastoplasmic or granular type. Oxyphll cells are characterized by juxtanuclear bodies and by numerous mito- chondria found throughout their cytoplasm. Puzzling lamellar whorls are described in the cytoplasm of some oxyphil cells. The endothelium of parathyroid capillaries is extremely thin in some areas and contains numerous fenestrations as well as an extensive system of vesicles. The possible significance of these structures is discussed. The connective tissue elements found in the perivascular spaces of macaque parathyroid are described. INTRODUCTION Other contributions to the present concepts con cerning the human parathyroid can be found in the It is the purpose of the present paper to report some observations on the fine structure of the reports of Bergstrand (7), Morgan (34), Pappen- parathyroid gland employing the electron micro- heimer and Wilens (45), Castleman and Mallory (10), and Gilmour (20). -

WO 2015/168656 A2 5 November 2015 (05.11.2015) P O P C T
(12) INTERNATIONAL APPLICATION PUBLISHED UNDER THE PATENT COOPERATION TREATY (PCT) (19) World Intellectual Property Organization International Bureau (10) International Publication Number (43) International Publication Date WO 2015/168656 A2 5 November 2015 (05.11.2015) P O P C T (51) International Patent Classification: (72) Inventors: HSIAO, Sonny; 1985 Pleasant Valley Avenue, A61K 48/00 (2006.01) Apartment 7, Oakland, CA 9461 1 (US). LIU, Cheng; 24 N Hill Court, Oakland, CA 94618 (US). LIU, Hong; 5573 (21) International Application Number: Woodview Drive, El Sobrante, CA 94803 (US). PCT/US20 15/02895 1 (74) Agents: GIERING, Jeffery, C. et al; Wilson Sonsini (22) International Filing Date: Goodrich & Rosati, 650 Page Mill Road, Palo Alto, CA 1 May 2015 (01 .05.2015) 94304-1050 (US). (25) Filing Language: English (81) Designated States (unless otherwise indicated, for every (26) Publication Language: English kind of national protection available): AE, AG, AL, AM, AO, AT, AU, AZ, BA, BB, BG, BH, BN, BR, BW, BY, (30) Priority Data: BZ, CA, CH, CL, CN, CO, CR, CU, CZ, DE, DK, DM, 61/988,070 2 May 2014 (02.05.2014) US DO, DZ, EC, EE, EG, ES, FI, GB, GD, GE, GH, GM, GT, (71) Applicant: ADHEREN INCORPORATED [US/US]; HN, HR, HU, ID, IL, IN, IR, IS, JP, KE, KG, KN, KP, KR, 1026 Rispin Drive, Berkeley, CA 94705 (US). KZ, LA, LC, LK, LR, LS, LU, LY, MA, MD, ME, MG, MK, MN, MW, MX, MY, MZ, NA, NG, NI, NO, NZ, OM, (72) Inventors; and PA, PE, PG, PH, PL, PT, QA, RO, RS, RU, RW, SA, SC, (71) Applicants : TWITE, Amy, A. -

Quantitation of Corticotrophs in the Pars Distalis of Stress-Prone Swine Beverly Ann Bedford Iowa State University
Iowa State University Capstones, Theses and Retrospective Theses and Dissertations Dissertations 1-1-1976 Quantitation of corticotrophs in the pars distalis of stress-prone swine Beverly Ann Bedford Iowa State University Follow this and additional works at: https://lib.dr.iastate.edu/rtd Part of the Veterinary Anatomy Commons Recommended Citation Bedford, Beverly Ann, "Quantitation of corticotrophs in the pars distalis of stress-prone swine" (1976). Retrospective Theses and Dissertations. 17953. https://lib.dr.iastate.edu/rtd/17953 This Thesis is brought to you for free and open access by the Iowa State University Capstones, Theses and Dissertations at Iowa State University Digital Repository. It has been accepted for inclusion in Retrospective Theses and Dissertations by an authorized administrator of Iowa State University Digital Repository. For more information, please contact [email protected]. Quantitation of corticotrophs in the pars distalis of stress-prone swine by Beverly Ann Bedford A Thesis Submitted to the Graduate Faculty in Partial Fulfillment of The Requirements for the Degr~e of MASTER OF SCIENCE Department: Veterinary Anatomy, Pharmacology and Physiology Major: Veterinary Anatomy ., Signatures have been redacted for privacy ' I Iowa State University Ames, Iowa 1976 ii :E5 ll I q7(p ,g3r TABLE OF CONTENTS c,J. Page INTRODUCTION 1 LITERATURE REVIEW 4 Pituitary Gland 4 General morphology 4 Development 5 Blood supply 7 Staining techniques 7 Pars distalis 13 . Pars tuberalis 25 ·pars intermedia 28 Process of secretion 36 Neurohypophysis 41 Porcine Stress Syndrome 45 MATERIALS AND MET!iODS' 52 RESULTS 56 DISCUSSION 64 SUMMARY AND CONCLUSIONS 72 BIBLIOGRAPHY 73 ACKNOWLEDGMENTS 85 APPENDIX 86 1111408 1 INTRODUCTION As early as 1953, there came reports (Ludvigsen, 1953; Briskey et al., 1959) of pale soft exudative (PSE) post-mortem porcine muscu- lature which later stimulated research into the mechanisms responsible for this condition. -

Nomenclatore Per L'anatomia Patologica Italiana Arrigo Bondi
NAP Nomenclatore per l’Anatomia Patologica Italiana Versione 1.9 Arrigo Bondi Bologna, 2016 NAP v. 1.9, pag 2 Arrigo Bondi * NAP - Nomenclatore per l’Anatomia Patologica Italiana Versione 1.9 * Componente Direttivo Nazionale SIAPEC-IAP Società Italiana di Anatomia Patologica e Citodiagnostica International Academy of Pathology, Italian Division NAP – Depositato presso S.I.A.E. Registrazione n. 2012001925 Distribuito da Palermo, 1 Marzo 2016 NAP v. 1.9, pag 3 Sommario Le novità della versione 1.9 ............................................................................................................... 4 Cosa è cambiato rispetto alla versione 1.8 ........................................................................................... 4 I Nomenclatori della Medicina. ........................................................................................................ 5 ICD, SNOMED ed altri sistemi per la codifica delle diagnosi. ........................................................... 5 Codifica medica ........................................................................................................................... 5 Storia della codifica in medicina .................................................................................................. 5 Lo SNOMED ............................................................................................................................... 6 Un Nomenclatore per l’Anatomia Patologica Italiana ................................................................. 6 Il NAP ................................................................................................................................................. -
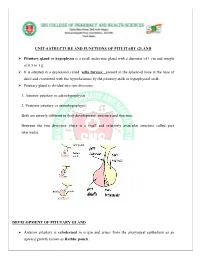
Unit-4 Structure and Functions of Pituitary Gland
UNIT-4 STRUCTURE AND FUNCTIONS OF PITUITARY GLAND Pituitary gland or hypophysis is a small endocrine gland with a diameter of 1 cm and weight of 0.5 to 1 g. It is situated in a depression called ‘sella turcica’, present in the sphenoid bone at the base of skull and connected with the hypothalamus by the pituitary stalk or hypophyseal stalk. Pituitary gland is divided into two divisions: 1. Anterior pituitary or adenohypophysis 2. Posterior pituitary or neurohypophysis. Both are entirely different in their development, structure and function. Between the two divisions, there is a small and relatively avascular structure called pars intermedia. DEVELOPMENT OF PITUTARY GLAND Anterior pituitary is ectodermal in origin and arises from the pharyngeal epithelium as an upward growth known as Rathke pouch. Posterior pituitary is neuroectodermal in origin and arises from hypothalamus as a downward diverticulum. Rathke pouch and the downward diverticulum from hypothalamus grow towards each other and meet in the midway between the roof of the buccal cavity and base of brain. There, the two structures lie close together. ANTERIOR PITUITARY OR ADENOHYPOPHYSIS Anterior pituitary is also known as the master gland because it regulates many other endocrine glands through its hormones. Anterior pituitary consists of three parts 1. Pars distalis 2. Pars tuberalis 3. Pars intermedia. Anterior pituitary has two types of cells 1. Chromophobe cells 2. Chromophil cells. Chromophobe Cells Chromophobe cells are not secretory in nature, but are the precursors of chromophil cells. Chromophil Cells On the basis of secretory nature chromophil cells are classified into five types: i. -

Histogenesis of Medullary Carcinoma of the Thyroid
J. clin. Path., (1966), 19, 114 Histogenesis of medullary carcinoma of the thyroid E. D. WILLIAMS1 From the Institute ofPathology, The London Hospital SYNOPSIS Thirty-one dog thyroid tumours and 28 spontaneous rat thyroid tumours were studied histologically and the findings compared with those of a study of 67 cases of medullary carcinoma of the human thyroid. Five of the dog tumours and 24 of the rat tumours were considered to belong to the same group of tumours as medullary carcinoma, a group characterized by solid sheets or lobules of uniform cells with granular cytoplasm and without papillary or follicular differentiation. In the rat tumours it was shown that the cell of origin was the parafollicular cell and not the thyroid follicle epithelial cell. It is suggested that medullary carcinoma is also derived from a parafollicular cell and that this origin would resolve the discrepancy between the relatively good prognosis and the apparently undifferentiated structure of this tumour. It is also concluded that the whole spectrum of clinical and pathological features of medullary carcinoma makes more sense if it is considered as a parafollicular cell tumour. Medullary carcinoma of the thyroid is a distinct the other 19 tumours, two were classified as papillary and clearly defined entity, and the histological carcinomas, nine as follicular carcinomas, two as features of 67 examples are discussed in the previous anaplastic carcinomas, while one tumour showed a paper (Williams, Brown, and Doniach, 1966). The mixture of follicular carcinoma with osteochondro- survival of patients with this tumour is often pro- sarcoma. The remaining five tumours were similar longed although paradoxically the vast majority of and were made up of nests ofuniform cells, separated cases show no evidence of differentiation towards a into groups by a connective tissue stroma which was thyroid epithelial pattern. -

Wednesday Slide Conference 2008-2009
PROCEEDINGS DEPARTMENT OF VETERINARY PATHOLOGY WEDNESDAY SLIDE CONFERENCE 2008-2009 ARMED FORCES INSTITUTE OF PATHOLOGY WASHINGTON, D.C. 20306-6000 2009 ML2009 Armed Forces Institute of Pathology Department of Veterinary Pathology WEDNESDAY SLIDE CONFERENCE 2008-2009 100 Cases 100 Histopathology Slides 249 Images PROCEEDINGS PREPARED BY: Todd Bell, DVM Chief Editor: Todd O. Johnson, DVM, Diplomate ACVP Copy Editor: Sean Hahn Layout and Copy Editor: Fran Card WSC Online Management and Design Scott Shaffer ARMED FORCES INSTITUTE OF PATHOLOGY Washington, D.C. 20306-6000 2009 ML2009 i PREFACE The Armed Forces Institute of Pathology, Department of Veterinary Pathology has conducted a weekly slide conference during the resident training year since 12 November 1953. This ever- changing educational endeavor has evolved into the annual Wednesday Slide Conference program in which cases are presented on 25 Wednesdays throughout the academic year and distributed to 135 contributing military and civilian institutions from around the world. Many of these institutions provide structured veterinary pathology resident training programs. During the course of the training year, histopathology slides, digital images, and histories from selected cases are distributed to the participating institutions and to the Department of Veterinary Pathology at the AFIP. Following the conferences, the case diagnoses, comments, and reference listings are posted online to all participants. This study set has been assembled in an effort to make Wednesday Slide Conference materials available to a wider circle of interested pathologists and scientists, and to further the education of veterinary pathologists and residents-in-training. The number of histopathology slides that can be reproduced from smaller lesions requires us to limit the number of participating institutions. -

Endocrine System Hormonal Regulation Endocrine Glands
Endocrine system Hormonal regulation Endocrine glands • Glands w/o ducts • Secretory cells release their products, hormones, into the extracellular space and blood stream • Alternatively, the hormones may affect neighbor cells (paracrine) • Structure: • c.t. – capsule + septs • irregular clumps or cords of the cells • network of capillaries • fenestrated capillaries • sinusoids Hypophysis – pituitary gland Pituitary gland – anterior pituitary Pituitary gland – anterior pituitary Chromophil cells - Acidophilic cells (produce proteins) somatotrophs mammotrophs (or lactotrophs) - Basophilic cells (produce glycoproteins) thyrotrophs produce thyroid stimulating hormone (TSH or thyrotropin). gonadotrophs produce follicle stimulating hormone (FSH) and luteinizing hormone (LH) corticotrophs (or adrenocorticolipotrophs) Chromophobe cells Adenohypophysis Adenohypophysis oranž G + PAS Neurohypophysis x Adenohypophysis Neurohypophysis - structure Structure unmyelinated nerve fibres derived from neurosecretory cells of the supraoptic and paraventricular hypothalamic nuclei pituicytes /neuroglia/ Function Two hormones are oxytocin, which stimulates the contraction of smooth muscle cell in the uterus and participates in the milk ejection reflex, and antidiuretic hormone (ADH or vasopressin), which facilitates the concentration of urine in the kidneys and, thereby, the retention of water. Usually only the oval or round nuclei of the pituicytes are visible. Hypothalamic nerve fibres typically terminate close to capillaries. Scattered, large -

Endocrine Glands
Endocrine glands David Kachlík Endocrine system • one out if two regulator systems • phylogenetically older than the nervous system • regulates activity of other systems so that they could react to changing requirements of outer and inner environment (maintains homeostasis) • does not originate from anatomically similar structures • secretion into blood – possesses no ducts • nearly all organs and tissues of the human body produce a hormone Hormone • horman in Greek = to arise • chemical messanger produced by endocrine gland and transported into blood to target organs • proteins (polypeptides) – insuline • amines – adrenaline • steroids – estrogenes Clinical consequence • hormonal excess – primary gland overproduction – secondary to excess production of trophic (releasing, stimulating) substance (hormone) • hormonal deficiency – primary gland failure – secondary to lack of stimulation by trophic (releasing, stimulating) substance (hormone) – target organ resistance Endocrine glands History Thomas Wharton • 1614-1673 • Adenographia • first detailed description of glands Ernest Henry Starling • 1866-1927 • general schemes of „endocrine secretion“ • used the already exsiting word „hormones“ Endocrine system arrangement • glands • disseminated cells • neuroendocrine cells Endocrine glands – list • hypothalamus (hypothalamus) • pituitary gland (hypophysis; gl. pituitaria) • thyroid gland (glandula thyroidea) • parathyroid bodies (gll. parathyroideae) • suprarenal glands, adrenals (gll. suprarenales) • pancreatic (Langerhans‘) island (insulae