Trench Fever in Texas
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Parinaud's Oculoglandular Syndrome
Tropical Medicine and Infectious Disease Case Report Parinaud’s Oculoglandular Syndrome: A Case in an Adult with Flea-Borne Typhus and a Review M. Kevin Dixon 1, Christopher L. Dayton 2 and Gregory M. Anstead 3,4,* 1 Baylor Scott & White Clinic, 800 Scott & White Drive, College Station, TX 77845, USA; [email protected] 2 Division of Critical Care, Department of Medicine, University of Texas Health, San Antonio, 7703 Floyd Curl Drive, San Antonio, TX 78229, USA; [email protected] 3 Medical Service, South Texas Veterans Health Care System, San Antonio, TX 78229, USA 4 Division of Infectious Diseases, Department of Medicine, University of Texas Health, San Antonio, 7703 Floyd Curl Drive, San Antonio, TX 78229, USA * Correspondence: [email protected]; Tel.: +1-210-567-4666; Fax: +1-210-567-4670 Received: 7 June 2020; Accepted: 24 July 2020; Published: 29 July 2020 Abstract: Parinaud’s oculoglandular syndrome (POGS) is defined as unilateral granulomatous conjunctivitis and facial lymphadenopathy. The aims of the current study are to describe a case of POGS with uveitis due to flea-borne typhus (FBT) and to present a diagnostic and therapeutic approach to POGS. The patient, a 38-year old man, presented with persistent unilateral eye pain, fever, rash, preauricular and submandibular lymphadenopathy, and laboratory findings of FBT: hyponatremia, elevated transaminase and lactate dehydrogenase levels, thrombocytopenia, and hypoalbuminemia. His condition rapidly improved after starting doxycycline. Soon after hospitalization, he was diagnosed with uveitis, which responded to topical prednisolone. To derive a diagnostic and empiric therapeutic approach to POGS, we reviewed the cases of POGS from its various causes since 1976 to discern epidemiologic clues and determine successful diagnostic techniques and therapies; we found multiple cases due to cat scratch disease (CSD; due to Bartonella henselae) (twelve), tularemia (ten), sporotrichosis (three), Rickettsia conorii (three), R. -
If Needed You Can Use Two Lines
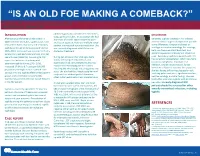
“IS AN OLD FOE MAKING A COMEBACK?” •Eyob Tadesse MD1; Samie Meskele MD1; Ankoor Biswas MD1 •Aurora Health Care, Milwaukee WI. NTRODUCTION abdomen gradually spread to her extremities, DISCUSSION I scalp, palms and soles. In association she had After being on the verge of elimination in shortness of breath, vague abdominal pain Generally, syphilis presents in HIV infected 2000 in the United States, syphilis cases have and loss of appetite, history of multiple sexual patients similar to general population yet with rebounded. Rates of primary and secondary partner, unprotected sex and prostitution. She some differences. Diagnosis is based on syphilis continued to increase overall during was recently diagnosed with HIV but not serologic test and microbiology. For serology, 2005–2013. Increases have occurred primarily started on treatment. both non treponemal antibody test, and among men, and particularly among men has specific treponemal antibody test should be used. Secondary syphilis in patients with HIV sex with men (MSM)(1). According to CDC During her admission her vital signs were has varied skin presentation, which can mimic report the incidence of primary and stable, she had pale conjunctivae, skin cutaneous lymphoma, mycobacterial secondary syphilis during 2015–2016, examination had demonstrated widespread macular and maculopapular skin lesions infection, bacillary angiomatosis, fungal increased 17.6% to 8.7 cases per 100,000 infections or Kaposi’s sarcoma. In our patient, population, the highest rate reported since involving the whole body including palms and soles. She also had thin, fragile scalp hair and she was having diffuse maculopapular rash, 1993(2). HIV and syphilis affect similar patient scalp hair loss without genital ulceration; involving palms and soles, significant hair loss, groups and co-infection is common(3). -

HIV and the SKIN • Sudden Acute Exacerbations • Treatment Failure DR
2018/08/13 KEY FEATURES • Atypical presentation of common disorders • Severe or exaggerated presentations HIV AND THE SKIN • Sudden acute exacerbations • Treatment failure DR. FREDAH MALEKA DERMATOLOGY UNIVERSITY OF PRETORIA:KALAFONG VIRAL INFECTIONS EXANTHEM OF PRIMARY HIV INFECTION • Exanthem of primary HIV infection • Acute retroviral syndrome • Herpes simplex virus (HSV) • Morbilliform rash (exanthem) : 2-4 weeks after HIV exposure • Varicella Zoster virus (VZV) • Typically generalised • Molluscum contagiosum (Poxvirus) • Pronounced on face and trunk, sparing distal extremities • Human papillomavirus (HPV) • Associated : fever, lymphadenopathy, pharyngitis • Epstein Barr virus (EBV) • DDX: drug reaction • Cytomegalovirus (CMV) • other viral infections – EBV, Enteroviruses, Hepatitis B virus 1 2018/08/13 HERPES SIMPLEX VIRUS(HSV) • Vesicular eruption due to HSV 1&2 • Primary lesion: painful, grouped vesicles on an erythematous base • HIV: attacks are more frequent and severe • : chronic, non-healing, deep ulcers, with scarring and tissue destruction • CLUE: severe pain and recurrences • DDX: syphilis, chancroid, lymphogranuloma venereum • Tzanck smear, Histology, Viral culture HSV • Treatment: Acyclovir 400mg tds 7-10 days • Alternatives: Valacyclovir and Famciclovir • In setting of treatment failure, viral isolates tested for resistance against acyclovir • Alternative drugs: Foscarnet, Cidofovir • Chronic suppressive therapy ( >8 attacks per year) 2 2018/08/13 VARICELLA • Chickenpox • Presents with erythematous papules and umbilicated -

WO 2014/134709 Al 12 September 2014 (12.09.2014) P O P C T
(12) INTERNATIONAL APPLICATION PUBLISHED UNDER THE PATENT COOPERATION TREATY (PCT) (19) World Intellectual Property Organization International Bureau (10) International Publication Number (43) International Publication Date WO 2014/134709 Al 12 September 2014 (12.09.2014) P O P C T (51) International Patent Classification: (81) Designated States (unless otherwise indicated, for every A61K 31/05 (2006.01) A61P 31/02 (2006.01) kind of national protection available): AE, AG, AL, AM, AO, AT, AU, AZ, BA, BB, BG, BH, BN, BR, BW, BY, (21) International Application Number: BZ, CA, CH, CL, CN, CO, CR, CU, CZ, DE, DK, DM, PCT/CA20 14/000 174 DO, DZ, EC, EE, EG, ES, FI, GB, GD, GE, GH, GM, GT, (22) International Filing Date: HN, HR, HU, ID, IL, IN, IR, IS, JP, KE, KG, KN, KP, KR, 4 March 2014 (04.03.2014) KZ, LA, LC, LK, LR, LS, LT, LU, LY, MA, MD, ME, MG, MK, MN, MW, MX, MY, MZ, NA, NG, NI, NO, NZ, (25) Filing Language: English OM, PA, PE, PG, PH, PL, PT, QA, RO, RS, RU, RW, SA, (26) Publication Language: English SC, SD, SE, SG, SK, SL, SM, ST, SV, SY, TH, TJ, TM, TN, TR, TT, TZ, UA, UG, US, UZ, VC, VN, ZA, ZM, (30) Priority Data: ZW. 13/790,91 1 8 March 2013 (08.03.2013) US (84) Designated States (unless otherwise indicated, for every (71) Applicant: LABORATOIRE M2 [CA/CA]; 4005-A, rue kind of regional protection available): ARIPO (BW, GH, de la Garlock, Sherbrooke, Quebec J1L 1W9 (CA). GM, KE, LR, LS, MW, MZ, NA, RW, SD, SL, SZ, TZ, UG, ZM, ZW), Eurasian (AM, AZ, BY, KG, KZ, RU, TJ, (72) Inventors: LEMIRE, Gaetan; 6505, rue de la fougere, TM), European (AL, AT, BE, BG, CH, CY, CZ, DE, DK, Sherbrooke, Quebec JIN 3W3 (CA). -

Rheumatic Manifestations of Bartonella Infection in 2 Children MOHAMMAD J
Case Report Rheumatic Manifestations of Bartonella Infection in 2 Children MOHAMMAD J. AL-MATAR, ROSS E. PETTY, DAVID A. CABRAL, LORI B. TUCKER, BANAFSHI PEYVANDI, JULIE PRENDIVILLE, JACK FORBES, ROBYN CAIRNS, and RALPH ROTHSTEIN ABSTRACT. We describe 2 patients with very unusual rheumatological presentations presumably caused by Bartonella infection: one had myositis of proximal thigh muscles bilaterally, and the other had arthritis and skin nodules. Both patients had very high levels of antibody to Bartonella that decreased in asso- ciation with clinical improvement. Bartonella infection should be considered in the differential diag- nosis of unusual myositis or arthritis in children. (J Rheumatol 2002;29:184–6) Key Indexing Terms: MYOSITIS ARTHRITIS BARTONELLA Infection with Bartonella species has a wide range of mani- was slightly increased at 9.86 IU/l (normal 4.51–9.16), and IgA was 2.1 IU/l festations in children including cat scratch disease (regional (normal 0.2–1.0). C3 was 0.11 g/l (normal 0.77–1.43) and C4 was 0.28 (nor- mal 0.07–0.40). Antinuclear antibodies were present at a titer of 1:40, the anti- granulomatous lymphadenitis), bacillary angiomatosis, streptolysin O titer was 35 (normal < 200), and the anti-DNAase B titer was encephalitis, Parinaud’s oculoglandular syndrome, Trench 1:85 (normal). Urinalysis showed 50–100 erythrocytes and 5–10 leukocytes fever (Vincent’s angina), osteomyelitis, granulomatous per high power field. Routine cultures of urine, blood, and throat were nega- hepatitis, splenitis, pneumonitis, endocarditis, and fever of tive. Liver enzymes, electrolytes, HIV serology, cerebrospinal fluid analysis, unknown origin1-3. -

CD Alert Monthly Newsletter of National Centre for Disease Control, Directorate General of Health Services, Government of India
CD Alert Monthly Newsletter of National Centre for Disease Control, Directorate General of Health Services, Government of India May - July 2009 Vol. 13 : No. 1 SCRUB TYPHUS & OTHER RICKETTSIOSES it lacks lipopolysaccharide and peptidoglycan RICKETTSIAL DISEASES and does not have an outer slime layer. It is These are the diseases caused by rickettsiae endowed with a major surface protein (56kDa) which are small, gram negative bacilli adapted and some minor surface protein (110, 80, 46, to obligate intracellular parasitism, and 43, 39, 35, 25 and 25kDa). There are transmitted by arthropod vectors. These considerable differences in virulence and organisms are primarily parasites of arthropods antigen composition among individual strains such as lice, fleas, ticks and mites, in which of O.tsutsugamushi. O.tsutsugamushi has they are found in the alimentary canal. In many serotypes (Karp, Gillian, Kato and vertebrates, including humans, they infect the Kawazaki). vascular endothelium and reticuloendothelial GLOBAL SCENARIO cells. Commonly known rickettsial disease is Scrub Typhus. Geographic distribution of the disease occurs within an area of about 13 million km2 including- The family Rickettsiaeceae currently comprises Afghanistan and Pakistan to the west; Russia of three genera – Rickettsia, Orientia and to the north; Korea and Japan to the northeast; Ehrlichia which appear to have descended Indonesia, Papua New Guinea, and northern from a common ancestor. Former members Australia to the south; and some smaller of the family, Coxiella burnetii, which causes islands in the western Pacific. It was Q fever and Rochalimaea quintana causing first observed in Japan where it was found to trench fever have been excluded because the be transmitted by mites. -

An Important One Health Opportunity
veterinary sciences Review Ehrlichioses: An Important One Health Opportunity Tais B. Saito * and David H. Walker Department of Pathology, University of Texas Medical Branch at Galveston, Galveston, TX 77555, USA; [email protected] * Correspondence: [email protected]; Tel.: +1-1409-772-4813 Academic Editor: Ulrike Munderloh Received: 15 July 2016; Accepted: 25 August 2016; Published: 31 August 2016 Abstract: Ehrlichioses are caused by obligately intracellular bacteria that are maintained subclinically in a persistently infected vertebrate host and a tick vector. The most severe life-threatening illnesses, such as human monocytotropic ehrlichiosis and heartwater, occur in incidental hosts. Ehrlichia have a developmental cycle involving an infectious, nonreplicating, dense core cell and a noninfectious, replicating reticulate cell. Ehrlichiae secrete proteins that bind to host cytoplasmic proteins and nuclear chromatin, manipulating the host cell environment to their advantage. Severe disease in immunocompetent hosts is mediated in large part by immunologic and inflammatory mechanisms, including overproduction of tumor necrosis factor α (TNF-α), which is produced by CD8 T lymphocytes, and interleukin-10 (IL-10). Immune components that contribute to control of ehrlichial infection include CD4 and CD8 T cells, natural killer (NK) cells, interferon-γ (IFN-γ), IL-12, and antibodies. Some immune components, such as TNF-α, perforin, and CD8 T cells, play both pathogenic and protective roles. In contrast with the immunocompetent host, which may die with few detectable organisms owing to the overly strong immune response, immunodeficient hosts die with overwhelming infection and large quantities of organisms in the tissues. Vaccine development is challenging because of antigenic diversity of E. -

CASE REPORT the PATIENT 33-Year-Old Woman
CASE REPORT THE PATIENT 33-year-old woman SIGNS & SYMPTOMS – 6-day history of fever Katherine Lazet, DO; – Groin pain and swelling Stephanie Rutterbush, MD – Recent hiking trip in St. Vincent Ascension Colorado Health, Evansville, Ind (Dr. Lazet); Munson Healthcare Ostego Memorial Hospital, Lewiston, Mich (Dr. Rutterbush) [email protected] The authors reported no potential conflict of interest THE CASE relevant to this article. A 33-year-old Caucasian woman presented to the emergency department with a 6-day his- tory of fever (103°-104°F) and right groin pain and swelling. Associated symptoms included headache, diarrhea, malaise, weakness, nausea, cough, and anorexia. Upon presentation, she admitted to a recent hike on a bubonic plague–endemic trail in Colorado. Her vital signs were unremarkable, and the physical examination demonstrated normal findings except for tender, erythematous, nonfluctuant right inguinal lymphadenopathy. The patient was admitted for intractable pain and fever and started on intravenous cefoxitin 2 g IV every 8 hours and oral doxycycline 100 mg every 12 hours for pelvic inflammatory disease vs tick- or flea-borne illness. Due to the patient’s recent trip to a plague-infested area, our suspicion for Yersinia pestis infection was high. The patient’s work-up included a nega- tive pregnancy test and urinalysis. A com- FIGURE 1 plete blood count demonstrated a white CT scan from admission blood cell count of 8.6 (4.3-10.5) × 103/UL was revealing with a 3+ left shift and a platelet count of 112 (180-500) × 103/UL. A complete metabolic panel showed hypokalemia and hyponatremia (potassium 2.8 [3.5-5.1] mmol/L and sodium 134 [137-145] mmol/L). -

Protecting Yourself from Zoonotic Infection
PROTECTING YOURSELF FROM ZOONOTIC INFECTION What is a Zoonoses? A zoonotic disease is an infection that is naturally transmitted from vertebrate animals to human beings. Many of these infections are transmitted directly but others are passed via vectors such as mosquitoes or fleas. Not all animal diseases are zoonotic and far more human illnesses result from contact with other humans than from animals. However, it is important for anyone working with animals to be aware of the potential for infection and takes steps to prevent exposure. The following lists some of the more common or severe zoonoses and ways to help protect yourself and others from exposure. IMPORTANT RULES TO HELP YOU AVOID DEVELOPING A SERIOUS ZOONOTIC ILLNESS: Stay current on appropriate vaccinations, such as tetanus and rabies. Wash your hands frequently with antibacterial soap, especially after handling any animal and prior to eating or smoking. Wear long pants and sturdy shoes or boots. Use gloves when handling animals and when cleaning up feces, urine, or vomit. Immediately disinfect scratches and bite wounds thoroughly. Keep scratches or other abrasions covered, especially when cleaning up after animals. Learn safe and humane animal-handling techniques and use proper equipment. Seek assistance when handling animals whose dispositions are questionable. If exposed to tick-infested areas, check your body and clothing frequently. Use tweezers and wear gloves to remove ticks, taking care not to squeeze or puncture the body of the tick. Report any bites or injuries to a supervisor and seek medical treatment as appropriate. Tell your physician that you work closely with animals, and visit him or her regularly. -

WO 2013/042140 A4 28 March 2013 (28.03.2013) P O P C T
(12) INTERNATIONAL APPLICATION PUBLISHED UNDER THE PATENT COOPERATION TREATY (PCT) (19) World Intellectual Property Organization International Bureau (10) International Publication Number (43) International Publication Date WO 2013/042140 A4 28 March 2013 (28.03.2013) P O P C T (51) International Patent Classification: NO, NZ, OM, PA, PE, PG, PH, PL, PT, QA, RO, RS, RU, A61K 31/197 (2006.01) A61K 45/06 (2006.01) RW, SC, SD, SE, SG, SK, SL, SM, ST, SV, SY, TH, TJ, A61K 31/60 (2006.01) A61P 31/00 (2006.01) TM, TN, TR, TT, TZ, UA, UG, US, UZ, VC, VN, ZA, A61K 33/22 (2006.01) ZM, ZW. (21) International Application Number: (84) Designated States (unless otherwise indicated, for every PCT/IN20 12/000634 kind of regional protection available): ARIPO (BW, GH, GM, KE, LR, LS, MW, MZ, NA, RW, SD, SL, SZ, TZ, (22) International Filing Date UG, ZM, ZW), Eurasian (AM, AZ, BY, KG, KZ, RU, TJ, 24 September 2012 (24.09.2012) TM), European (AL, AT, BE, BG, CH, CY, CZ, DE, DK, (25) Filing Language: English EE, ES, FI, FR, GB, GR, HR, HU, IE, IS, IT, LT, LU, LV, MC, MK, MT, NL, NO, PL, PT, RO, RS, SE, SI, SK, SM, (26) Publication Language: English TR), OAPI (BF, BJ, CF, CG, CI, CM, GA, GN, GQ, GW, (30) Priority Data: ML, MR, NE, SN, TD, TG). 2792/DEL/201 1 23 September 201 1 (23.09.201 1) IN Declarations under Rule 4.17 : (72) Inventor; and — of inventorship (Rule 4.17(iv)) (71) Applicant : CHAUDHARY, Manu [IN/IN]; 51-52, In dustrial Area Phase- 1, Panchkula 1341 13 (IN). -

What Do We Know About Q Fever in Mexico?
ARTÍCULO ORIGINAL What do we know about Q fever in Mexico? Javier Araujo-Meléndez,* José Sifuentes-Osornio,* J. Miriam Bobadilla-del-Valle,* Antonio Aguilar-Cruz,** Orestes Torres-Ángeles,** José L. Ramírez-González,*** Alfredo Ponce-de-León,* Guillermo M. Ruiz-Palacios,* M. Lourdes Guerrero-Almeida* * Instituto Nacional de Ciencias Médicas y Nutrición Salvador Zubirán. ** Jurisdicción Sanitaria No. 4, Huichapan, Hidalgo. *** Hospital General, Huichapan, Hidalgo. ABSTRACT ¿Qué sabemos acerca de la fiebre Q en México? In Mexico, Q fever is considered a rare disease among hu- RESUMEN mans and animals. From March to May of 2008, three pa- tients were referred, from the state of Hidalgo to a En México la fiebre Q se considera una enfermedad rara en- tertiary-care center in Mexico City, with an acute febrile ill- tre los humanos y los animales. Sin embargo, entre marzo y ness that was diagnosed as Q fever. We decided to undertake a mayo 2008 tres pacientes del estado de Hidalgo fueron refe- cross sectional pilot study to identify cases of acute disease in ridos a un hospital de tercer nivel en la Ciudad de México this particular region and to determine the seroprevalence of por una enfermedad febril aguda y fueron diagnosticados Coxiella burnetii among healthy individuals with known risk con fiebre Q. Se decidió llevar a cabo un estudio piloto para factors for infection with this bacteria. Q fever was defined identificar casos de enfermedad aguda en esa región y deter- according to the Centers for Disease Control and Prevention minar la prevalencia serológica de Coxiella burnetii en indi- criteria. -
Vectra® for Cats & Kittens and Vectra® for Cats
This is love. Wrapped in fur. Protect the love. FLEA CONTROL Facts About Fleas Can jump up to Can lay eggs 13” 24 hours after biting Females can lay 50 eggs per day Transmit and cause diseases like: Flea Allergy Dermatitis Tapeworm disease Bartonella Life cycle can be completed in Anemia (severe infestations) Feline Infectious Anemia 3 weeks Bubonic Plague Why are flea infestations so hard to get rid of? ONLY 5% OF THE FLEAS IN YOUR CAT’S ENVIRONMENT ARE ADULTS THAT BITE YOUR CAT. The remaining 95% are in the development stage ready to become adults within 3 weeks. 5% Adults 35% Larvae 50% Eggs 10% Pupae Vectra® for Cats & Kittens and Vectra® for Cats Vectra® for Cats & Kittens AND Vectra® for Cats protect your favorite feline from all stages of fleas. Applying Vectra® every month helps prevent flea infestation, re-infestation, and protects your cat or kitten from flea-borne diseases. Fast-Acting • Kills through contact so fleas do not have to bite in order to die • Protects cats and kittens against flea-borne diseases, including tularemia, rickettsiosis, Life cycle can be completed in bartonellosis, and tapeworm Flea Protection • Kills fleas at all life stages for 1 month • Adults • Eggs • Larvae • Pupae • Remains effective after exposure to sunlight Convenient • Patented applicator makes application easy, clean, and accurate • Can be used on kittens as young as 8 weeks of age How to apply Vectra® for Cats & Kittens and Vectra® for Cats Before administering Vectra® for the first time, you should ask your veterinarian to demonstrate the proper application technique.