Parinaud's Oculoglandular Syndrome
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

(Scrub Typhus). Incubation Period 1 to 3
TYPHUS Causative Agents TYPHUS Rickettsia typhi (murine typhus) and Orientia tsutsugamushi (scrub typhus). Causative Agents IncubationRickettsia typhi Period (murine typhus) and Orientia tsutsugamushi (scrub typhus). 1 to 3 weeks Incubation Period Infectious1 to 3 weeks Period Zoonoses with no human-to-human transmission. Infectious Period TransmissionZoonoses with no human-to-human transmission. Scrub typhus: Bite of grass mites (larval trombiculid mites) MurineTransmission typhus: Bite of rat fleas (also cat and mice fleas) RodentsScrub typhus: are the Bite preferred of grass and mites normal (larval hosts. trombiculid mites) Murine typhus: Bite of rat fleas (also cat and mice fleas) EpidemiologyRodents are the preferred and normal hosts. Distributed throughout the Asia-Pacific rim and is a common cause of pyrexia of unknownEpidemiology origin throughout SE Asia. Occupational contact with rats (e.g. construDistributedction throughout workers inthe makeAsia-Pshiftacific container rim and isfacilities, a common shop cause owners, of pyrexia granary of workers,unknown andorigin garbage throughout collectors) SE orAsia. exposure Occupational to mite habitat contacts in lonwithg grassrats (e.g. hikersconstru andction so ldiers)workers are inrisk make factors.-shift container facilities, shop owners, granary workers, and garbage collectors) or exposure to mite habitats in long grass (e.g. Inhikers Singapore, and soldiers) a total are ofrisk 13 factors. laboratory confirmed cases of murine typhus were r eported in 2008. The majority of cases were foreign workers. In Singapore, a total of 13 laboratory confirmed cases of murine typhus were Clinicalreported Featuresin 2008. The majority of cases were foreign workers. Fever Clinical Headache Features (prominent) MyalgiaFever ConjunctiHeadache val(prominent) suffusion MaculopapularMyalgia rash Conjunctival suffusion Scrub Maculopapular typhus may alsorash have: relative bradycardia, eschar (80%), painful regional adenopathy, hepatosplenomegaly, meningoencephalitis and renal failure. -

Reportable Diseases and Conditions
KINGS COUNTY DEPARTMENT of PUBLIC HEALTH 330 CAMPUS DRIVE, HANFORD, CA 93230 REPORTABLE DISEASES AND CONDITIONS Title 17, California Code of Regulations, §2500, requires that known or suspected cases of any of the diseases or conditions listed below are to be reported to the local health jurisdiction within the specified time frame: REPORT IMMEDIATELY BY PHONE During Business Hours: (559) 852-2579 After Hours: (559) 852-2720 for Immediate Reportable Disease and Conditions Anthrax Escherichia coli: Shiga Toxin producing (STEC), Rabies (Specify Human or Animal) Botulism (Specify Infant, Foodborne, Wound, Other) including E. coli O157:H7 Scrombroid Fish Poisoning Brucellosis, Human Flavivirus Infection of Undetermined Species Shiga Toxin (Detected in Feces) Cholera Foodborne Disease (2 or More Cases) Smallpox (Variola) Ciguatera Fish Poisoning Hemolytic Uremic Syndrome Tularemia, human Dengue Virus Infection Influenza, Novel Strains, Human Viral Hemorrhagic Fever (Crimean-Congo, Ebola, Diphtheria Measles (Rubeola) Lassa, and Marburg Viruses) Domonic Acid Poisoning (Amnesic Shellfish Meningococcal Infections Yellow Fever Poisoning) Novel Virus Infection with Pandemic Potential Zika Virus Infection Paralytic Shellfish Poisoning Plague (Specify Human or Animal) Immediately report the occurrence of any unusual disease OR outbreaks of any disease. REPORT BY PHONE, FAX, MAIL WITHIN ONE (1) WORKING DAY Phone: (559) 852-2579 Fax: (559) 589-0482 Mail: 330 Campus Drive, Hanford 93230 Conditions may also be reported electronically via the California -

2012 Case Definitions Infectious Disease
Arizona Department of Health Services Case Definitions for Reportable Communicable Morbidities 2012 TABLE OF CONTENTS Definition of Terms Used in Case Classification .......................................................................................................... 6 Definition of Bi-national Case ............................................................................................................................................. 7 ------------------------------------------------------------------------------------------------------- ............................................... 7 AMEBIASIS ............................................................................................................................................................................. 8 ANTHRAX (β) ......................................................................................................................................................................... 9 ASEPTIC MENINGITIS (viral) ......................................................................................................................................... 11 BASIDIOBOLOMYCOSIS ................................................................................................................................................. 12 BOTULISM, FOODBORNE (β) ....................................................................................................................................... 13 BOTULISM, INFANT (β) ................................................................................................................................................... -

Ehrlichiosis and Anaplasmosis Are Tick-Borne Diseases Caused by Obligate Anaplasmosis: Intracellular Bacteria in the Genera Ehrlichia and Anaplasma
Ehrlichiosis and Importance Ehrlichiosis and anaplasmosis are tick-borne diseases caused by obligate Anaplasmosis: intracellular bacteria in the genera Ehrlichia and Anaplasma. These organisms are widespread in nature; the reservoir hosts include numerous wild animals, as well as Zoonotic Species some domesticated species. For many years, Ehrlichia and Anaplasma species have been known to cause illness in pets and livestock. The consequences of exposure vary Canine Monocytic Ehrlichiosis, from asymptomatic infections to severe, potentially fatal illness. Some organisms Canine Hemorrhagic Fever, have also been recognized as human pathogens since the 1980s and 1990s. Tropical Canine Pancytopenia, Etiology Tracker Dog Disease, Ehrlichiosis and anaplasmosis are caused by members of the genera Ehrlichia Canine Tick Typhus, and Anaplasma, respectively. Both genera contain small, pleomorphic, Gram negative, Nairobi Bleeding Disorder, obligate intracellular organisms, and belong to the family Anaplasmataceae, order Canine Granulocytic Ehrlichiosis, Rickettsiales. They are classified as α-proteobacteria. A number of Ehrlichia and Canine Granulocytic Anaplasmosis, Anaplasma species affect animals. A limited number of these organisms have also Equine Granulocytic Ehrlichiosis, been identified in people. Equine Granulocytic Anaplasmosis, Recent changes in taxonomy can make the nomenclature of the Anaplasmataceae Tick-borne Fever, and their diseases somewhat confusing. At one time, ehrlichiosis was a group of Pasture Fever, diseases caused by organisms that mostly replicated in membrane-bound cytoplasmic Human Monocytic Ehrlichiosis, vacuoles of leukocytes, and belonged to the genus Ehrlichia, tribe Ehrlichieae and Human Granulocytic Anaplasmosis, family Rickettsiaceae. The names of the diseases were often based on the host Human Granulocytic Ehrlichiosis, species, together with type of leukocyte most often infected. -

Sexually Transmitted Diseases/Infections Chancroid
Sexually Transmitted Diseases/Infections Chancroid Chancroid is a bacterial infection caused by Haemophilus ducreyi. It is spread by sexual contact and results in genital ulcers. Chancroid is a reportable genital ulcer condition that is rarely seen in North Carolina. When infection does occur, it is usually associated with sporadic outbreaks. Chancroid, as well as genital herpes and syphilis, is a risk factor in the transmission of HIV infection. Chancroid lesions may be difficult to distinguish from ulcers caused by genital herpes or syphilis. A physician must therefore diagnose the infection by excluding other diseases with similar symptoms. The combination of a painful genital ulcer and tender suppurative inguinal adenopathy suggests the diagnosis of chancroid. A probable diagnosis of chancroid, for both clinical and surveillance purposes, can be made if all of the following criteria are met: 1) the patient has one or more painful genital ulcers; 2) the patient has no evidence of T. pallidum infection by darkfield examination of ulcer exudate or by a serologic test for syphilis performed at least 7 days after onset of ulcers; 3) the clinical presentation, appearance of genital ulcers and, if present, regional lymphadenopathy are typical for chancroid; and 4) a test for HSV performed on the ulcer exudate is negative. A definitive diagnosis of chancroid requires the identification of H. ducreyi on special culture media that is not widely available from commercial sources; even when these media are used, sensitivity is less than 80 percent. No FDA- cleared PCR test for H. ducreyi is available in the United States, but such testing can be performed by clinical laboratories that have developed their own PCR test and have conducted a CLIA verification study. -

CD Alert Monthly Newsletter of National Centre for Disease Control, Directorate General of Health Services, Government of India
CD Alert Monthly Newsletter of National Centre for Disease Control, Directorate General of Health Services, Government of India May - July 2009 Vol. 13 : No. 1 SCRUB TYPHUS & OTHER RICKETTSIOSES it lacks lipopolysaccharide and peptidoglycan RICKETTSIAL DISEASES and does not have an outer slime layer. It is These are the diseases caused by rickettsiae endowed with a major surface protein (56kDa) which are small, gram negative bacilli adapted and some minor surface protein (110, 80, 46, to obligate intracellular parasitism, and 43, 39, 35, 25 and 25kDa). There are transmitted by arthropod vectors. These considerable differences in virulence and organisms are primarily parasites of arthropods antigen composition among individual strains such as lice, fleas, ticks and mites, in which of O.tsutsugamushi. O.tsutsugamushi has they are found in the alimentary canal. In many serotypes (Karp, Gillian, Kato and vertebrates, including humans, they infect the Kawazaki). vascular endothelium and reticuloendothelial GLOBAL SCENARIO cells. Commonly known rickettsial disease is Scrub Typhus. Geographic distribution of the disease occurs within an area of about 13 million km2 including- The family Rickettsiaeceae currently comprises Afghanistan and Pakistan to the west; Russia of three genera – Rickettsia, Orientia and to the north; Korea and Japan to the northeast; Ehrlichia which appear to have descended Indonesia, Papua New Guinea, and northern from a common ancestor. Former members Australia to the south; and some smaller of the family, Coxiella burnetii, which causes islands in the western Pacific. It was Q fever and Rochalimaea quintana causing first observed in Japan where it was found to trench fever have been excluded because the be transmitted by mites. -
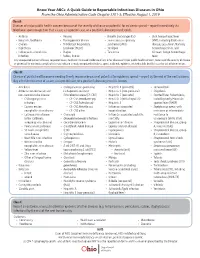
Know Your Abcs: a Quick Guide to Reportable Infectious Diseases in Ohio
Know Your ABCs: A Quick Guide to Reportable Infectious Diseases in Ohio From the Ohio Administrative Code Chapter 3701-3; Effective August 1, 2019 Class A: Diseases of major public health concern because of the severity of disease or potential for epidemic spread – report immediately via telephone upon recognition that a case, a suspected case, or a positive laboratory result exists. • Anthrax • Measles • Rubella (not congenital) • Viral hemorrhagic fever • Botulism, foodborne • Meningococcal disease • Severe acute respiratory (VHF), including Ebola virus • Cholera • Middle East Respiratory syndrome (SARS) disease, Lassa fever, Marburg • Diphtheria Syndrome (MERS) • Smallpox hemorrhagic fever, and • Influenza A – novel virus • Plague • Tularemia Crimean-Congo hemorrhagic infection • Rabies, human fever Any unexpected pattern of cases, suspected cases, deaths or increased incidence of any other disease of major public health concern, because of the severity of disease or potential for epidemic spread, which may indicate a newly recognized infectious agent, outbreak, epidemic, related public health hazard or act of bioterrorism. Class B: Disease of public health concern needing timely response because of potential for epidemic spread – report by the end of the next business day after the existence of a case, a suspected case, or a positive laboratory result is known. • Amebiasis • Carbapenemase-producing • Hepatitis B (perinatal) • Salmonellosis • Arboviral neuroinvasive and carbapenem-resistant • Hepatitis C (non-perinatal) • Shigellosis -

CASE REPORT the PATIENT 33-Year-Old Woman
CASE REPORT THE PATIENT 33-year-old woman SIGNS & SYMPTOMS – 6-day history of fever Katherine Lazet, DO; – Groin pain and swelling Stephanie Rutterbush, MD – Recent hiking trip in St. Vincent Ascension Colorado Health, Evansville, Ind (Dr. Lazet); Munson Healthcare Ostego Memorial Hospital, Lewiston, Mich (Dr. Rutterbush) [email protected] The authors reported no potential conflict of interest THE CASE relevant to this article. A 33-year-old Caucasian woman presented to the emergency department with a 6-day his- tory of fever (103°-104°F) and right groin pain and swelling. Associated symptoms included headache, diarrhea, malaise, weakness, nausea, cough, and anorexia. Upon presentation, she admitted to a recent hike on a bubonic plague–endemic trail in Colorado. Her vital signs were unremarkable, and the physical examination demonstrated normal findings except for tender, erythematous, nonfluctuant right inguinal lymphadenopathy. The patient was admitted for intractable pain and fever and started on intravenous cefoxitin 2 g IV every 8 hours and oral doxycycline 100 mg every 12 hours for pelvic inflammatory disease vs tick- or flea-borne illness. Due to the patient’s recent trip to a plague-infested area, our suspicion for Yersinia pestis infection was high. The patient’s work-up included a nega- tive pregnancy test and urinalysis. A com- FIGURE 1 plete blood count demonstrated a white CT scan from admission blood cell count of 8.6 (4.3-10.5) × 103/UL was revealing with a 3+ left shift and a platelet count of 112 (180-500) × 103/UL. A complete metabolic panel showed hypokalemia and hyponatremia (potassium 2.8 [3.5-5.1] mmol/L and sodium 134 [137-145] mmol/L). -

Melioidosis in Northern Tanzania: an Important Cause of Febrile Illness?
Melioidosis and serological evidence of exposure to Burkholderia pseudomallei among patients with fever, northern Tanzania Michael Maze Department of Medicine University of Otago, Christchurch Melioidosis Melioidosis caused by Burkholderia pseudomallei • Challenging to identify when cultured Soil reservoir, with human infection from contact with contaminated water Most infected people are asymptomatic: 1 clinical illness for 4,500 antibody producing exposures Febrile illness with a variety of presentations and bacteraemia is present in 40-60% of people with acute illness Estimated 89,000 deaths globally Gavin Koh CC BY-SA 4.0, https://commons.wikimedia.org/w/index.php?curid=4975784 Laboratory diagnosis of febrile inpatients, northern Tanzania, 2007-8 (n=870) Malaria (1.6%) Bacteremia (9.8%) Mycobacteremia (1.6%) Fungemia (2.9%) Brucellosis (3.5%) Leptospirosis (8.8%) Q fever (5.0%) No diagnosis (50.1%) Spotted fever group rickettsiosis (8.0%) Typhus group rickettsiosis (0.4%) Chikungunya (7.9%) Crump PLoS Neglect Trop Dis 2013; 7: e2324 Predicted environmental suitability for B. pseudomallei in East Africa Large areas of Africa are predicted to be highly suitable for Burkholderia pseudomallei East Africa is less suitable but pockets of higher suitability including northern Tanzania Northern Tanzania Increasing suitability for B. pseudomallei Limmathurotsakul Nat Microbiol. 2016;1(1). Melioidosis epidemiology in Africa Paucity of empiric data • Scattered case reports • Report from Kilifi, Kenya identified 4 bacteraemic cases from 66,000 patients who had blood cultured1 • 5.9% seroprevalence among healthy adults in Uganda2 • No reports from Tanzania 1. Limmathurotsakul Nat Microbiol. 2016;1(1). 2. Frazer J R Army Med Corps. 1982;128(3):123-30. -

Protecting Yourself from Zoonotic Infection
PROTECTING YOURSELF FROM ZOONOTIC INFECTION What is a Zoonoses? A zoonotic disease is an infection that is naturally transmitted from vertebrate animals to human beings. Many of these infections are transmitted directly but others are passed via vectors such as mosquitoes or fleas. Not all animal diseases are zoonotic and far more human illnesses result from contact with other humans than from animals. However, it is important for anyone working with animals to be aware of the potential for infection and takes steps to prevent exposure. The following lists some of the more common or severe zoonoses and ways to help protect yourself and others from exposure. IMPORTANT RULES TO HELP YOU AVOID DEVELOPING A SERIOUS ZOONOTIC ILLNESS: Stay current on appropriate vaccinations, such as tetanus and rabies. Wash your hands frequently with antibacterial soap, especially after handling any animal and prior to eating or smoking. Wear long pants and sturdy shoes or boots. Use gloves when handling animals and when cleaning up feces, urine, or vomit. Immediately disinfect scratches and bite wounds thoroughly. Keep scratches or other abrasions covered, especially when cleaning up after animals. Learn safe and humane animal-handling techniques and use proper equipment. Seek assistance when handling animals whose dispositions are questionable. If exposed to tick-infested areas, check your body and clothing frequently. Use tweezers and wear gloves to remove ticks, taking care not to squeeze or puncture the body of the tick. Report any bites or injuries to a supervisor and seek medical treatment as appropriate. Tell your physician that you work closely with animals, and visit him or her regularly. -

Zoonotic Diseases Associated with Free-Roaming Cats R
Zoonoses and Public Health REVIEW ARTICLE Zoonotic Diseases Associated with Free-Roaming Cats R. W. Gerhold1 and D. A. Jessup2 1 Center for Wildlife Health, Department of Forestry, Wildlife, and Fisheries, The University of Tennessee, Knoxville, TN, USA 2 California Department of Fish and Game (retired), Santa Cruz, CA, USA Impacts • Free-roaming cats are an important source of zoonotic diseases including rabies, Toxoplasma gondii, cutaneous larval migrans, tularemia and plague. • Free-roaming cats account for the most cases of human rabies exposure among domestic animals and account for approximately 1/3 of rabies post- exposure prophylaxis treatments in humans in the United States. • Trap–neuter–release (TNR) programmes may lead to increased naı¨ve populations of cats that can serve as a source of zoonotic diseases. Keywords: Summary Cutaneous larval migrans; free-roaming cats; rabies; toxoplasmosis; zoonoses Free-roaming cat populations have been identified as a significant public health threat and are a source for several zoonotic diseases including rabies, Correspondence: toxoplasmosis, cutaneous larval migrans because of various nematode parasites, R. Gerhold. Center for Wildlife Health, plague, tularemia and murine typhus. Several of these diseases are reported to Department of Forestry, Wildlife, and cause mortality in humans and can cause other important health issues includ- Fisheries, The University of Tennessee, ing abortion, blindness, pruritic skin rashes and other various symptoms. A Knoxville, TN 37996-4563, USA. Tel.: 865 974 0465; Fax: 865-974-0465; E-mail: recent case of rabies in a young girl from California that likely was transmitted [email protected] by a free-roaming cat underscores that free-roaming cats can be a source of zoonotic diseases. -

Typhus Fever, Organism Inapparently
Rickettsia Importance Rickettsia prowazekii is a prokaryotic organism that is primarily maintained in prowazekii human populations, and spreads between people via human body lice. Infected people develop an acute, mild to severe illness that is sometimes complicated by neurological Infections signs, shock, gangrene of the fingers and toes, and other serious signs. Approximately 10-30% of untreated clinical cases are fatal, with even higher mortality rates in Epidemic typhus, debilitated populations and the elderly. People who recover can continue to harbor the Typhus fever, organism inapparently. It may re-emerge years later and cause a similar, though Louse–borne typhus fever, generally milder, illness called Brill-Zinsser disease. At one time, R. prowazekii Typhus exanthematicus, regularly caused extensive outbreaks, killing thousands or even millions of people. This gave rise to the most common name for the disease, epidemic typhus. Epidemic typhus Classical typhus fever, no longer occurs in developed countries, except as a sporadic illness in people who Sylvatic typhus, have acquired it while traveling, or who have carried the organism for years without European typhus, clinical signs. In North America, R. prowazekii is also maintained in southern flying Brill–Zinsser disease, Jail fever squirrels (Glaucomys volans), resulting in sporadic zoonotic cases. However, serious outbreaks still occur in some resource-poor countries, especially where people are in close contact under conditions of poor hygiene. Epidemics have the potential to emerge anywhere social conditions disintegrate and human body lice spread unchecked. Last Updated: February 2017 Etiology Rickettsia prowazekii is a pleomorphic, obligate intracellular, Gram negative coccobacillus in the family Rickettsiaceae and order Rickettsiales of the α- Proteobacteria.