Bicuspid Aortic Valve
Total Page:16
File Type:pdf, Size:1020Kb

Load more
Recommended publications
-

Having an Echocardiogram to Screen for a Bicuspid Aortic Valve
Having an echocardiogram to screen for a bicuspid aortic valve UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm What is a bicuspid aortic valve? The aortic valve sits between the main chamber of the heart (the left ventricle) and the aorta. Its function is to ensure that blood flows correctly forward from the left ventricle into the aorta. Normally it has three thin leaflets which open as the heart contracts and then close to prevent back-flow of blood towards the ventricle. Aortic valve Tricuspid aortic valve (normal) Bicuspid aortic valve (abnormal) Some people may be born with an aortic valve made up of only 2 leaflets. The valve is then called bicuspid. This may cause problems with the functioning of the valve in that it may be more prone to gradually becoming narrowed or leaky. Sometimes a bicuspid valve may be associated with widening of the portion of the aorta that is connected to it. Widening of the aorta may occur in some relatives even if they have an aortic valve with 3 leaflets. If this widening is significant it is known as an aortic aneurysm. Is a bicuspid valve a common problem? Studies have suggested that this is not an uncommon valve problem and may occur in up to 1 in 200 people. 2 | PI18_1443_03 Having an echocardiogram to screen for a bicuspid aortic valve Recently there has been evidence that this condition may be genetic and thus have a tendency to run in a family. -

Echo in Asymptomatic Mitral and Aortic Regurgitation
2017 ASE Florida | Orlando, FL October 9, 2017 | 10:40 – 11:00 PM | 20 min | Grand Harbor Ballroom South Echo in Asymptomatic Mitral and Aortic Regurgitation Muhamed Sarić MD, PhD, MPA Director of Noninvasive Cardiology | Echo Lab Associate Professor of Medicine Disclosures Speakers Bureau (Philips, Medtronic) Advisory Board (Siemens) Regurgitation Axioms ▪Typically, regurgitation is NOT symptomatic unless severe ▪The opposite is not true: Severe regurgitation may be asymptomatic ▪ Chronic regurgitation leads to chamber dilatation on either side of the regurgitant valve Regurgitation Discovery ▪ Regurgitation as a anatomic entity was recognized in the 17th century ▪ Regurgitation was first clinically diagnosed by auscultation in the 19th century, well before the advent of echocardiography First Use of Regurgitation Term in English 1683 W. Charleton Three Anat. Lect. i. 18 Those [valves] that are placed in the inlet and outlet of the left Ventricle, to obviate the regurgitation of the bloud into the arteria venosa, and out of the aorta into the left Ventricle. Walter Charleton (1619 – 1707) English Physician Heart Murmur OXFORD ENGLISH DICTIONARY DEFINITION ▪ Any of various auscultatory sounds ▪ Adventitious sounds of cardiac or vascular origin [that is, separate from standard heart sounds: S1, S2, S3, S4] ▪ Sometimes of no significance ▪ But sometimes caused by valvular lesions of the heart or other diseases of the Στῆθος : Stēthos = chest circulatory system René Laënnec Stethoscope (1781 – 1826) (‘Chest examiner’) French Physician Hollow wooden cylinder Inventor of stethoscope in 1816 Laënnec Performing Auscultation Painted by Robert Alan Thom (1915 – 1979), American illustrator Commissioned by Parke, Davis & Co. 1816 1832 René Laënnec, James Hope French physician British physician Invents MONAURAL stethoscope separates MS from MR murmur 1852 1862 George Cammann Austin Flint Sr. -

Congenital Mitral Incompetence and Coarctation Ofaorta
Thorax: first published as 10.1136/thx.27.6.729 on 1 November 1972. Downloaded from Thorax (1972), 27, 729. Congenital mitral incompetence and coarctation of aorta Report of two cases treated surgically' ABDEL K. TERZAKI2, ROBERT D. LEACHMAN3, M. KHALIL ALI, GRADY L. HALLMAN, and DENTON A. COOLEY Department of Medicine and the Cora and Webb Mading Department of Surgery, Baylor University College of Medicine, and the Cardiology and Surgical Sections of the Texas Heart Institute of St. Luke's Episcopal and Texas Children's Hospitals, Houston, Texas, U.S.A. Two patients with congenital mitral incompetence and coarctation of the aorta are presented. One patient had associated patent ductus arteriosus, bicuspid aortic valve, and endocardial fibro- elastosis. The diagnosis in the two patients presented is well established by clinical, laboratory, and surgical findings and also by necropsy examination in one case. It is proposed that the rarity of reported cases in the literature may have resulted from the frequent diagnosis of left ventricular failure in infancy secondary to coarctation, leading to the assumption that a mitral insufficiency murmur, when present, is due to functional regurgitation. Likewise, the murmur may be mistakenly thought to originate from a ventricular septal defect. The diagnosis of coarctation of the aorta presented no problem in either patient, while detection of the mitral incompetence was difficult. Coarctation of the aorta complicated by copyright. pulmonary hypertension in the absence of intracardiac shunt should draw attention to the possi- bility of associated mitral incompetence. Congestive heart failure, especially after correction of coarctation, was also an indication of possible associated mitral insufficiency. -

Prevalence of Migraine Headaches in Patients with Congenital Heart Disease
Prevalence of Migraine Headaches in Patients With Congenital Heart Disease Tam Truong, MD, Leo Slavin, MD, Ramin Kashani, BA, James Higgins, MD, Aarti Puri, BS, Malika Chowdhry, BS, Philip Cheung, BS, Adam Tanious, BA, John S. Child, MD, FAHA, Joseph K. Perloff, MD, and Jonathan M. Tobis, MD* The prevalence of migraine headaches (MH) is 12% in the general population and increases to 40% in patients with patent foramen ovale. This study evaluated the prevalence of MH in patients with congenital heart disease (CHD). Of 466 patients contacted from the UCLA Adult Congenital Heart Disease Center, 395 (85%) completed a questionnaire to determine the prevalence of MH. Patients were stratified by diagnosis of right-to-left, left-to-right, or no shunt. A group of 252 sex-matched patients with acquired cardiovascular disease served as controls. The prevalence of MH was 45% in adults with CHD compared to 11% in the controls (p <0.001). Of the 179 patients with MH, 143 (80%) had migraines with aura and 36 (20%) had migraines without aura versus 36% and 64% observed in the controls (p <0.001). The frequency of MH was 52% in the right-to-left shunt group, 44% in the left-to-right, and 38% in the no ,NS). In patients with a right-to-left shunt who underwent surgical repair ؍ shunt group (p 47% had complete resolution of MH, whereas 76% experienced >50% reduction in headache days per month. In conclusion, the prevalence of MH in all groups of adults with CHD is 3 to 4 times more than a sex-matched control population, with increasing prevalence of MH in patients with no shunt, left-to-right, and right-to-left shunt. -
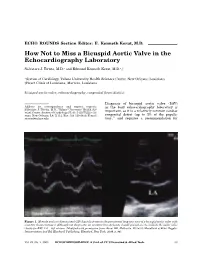
How Not to Miss a Bicuspid Aortic Valve in the Echocardiography Laboratory
ECHO ROUNDS Section Editor: E. Kenneth Kerut, M.D. How Not to Miss a Bicuspid Aortic Valve in the Echocardiography Laboratory Salvatore J. Tirrito, M.D.∗ and Edmund Kenneth Kerut, M.D.∗,† ∗Section of Cardiology, Tulane University Health Sciences Center, New Orleans, Louisiana †Heart Clinic of Louisiana, Marrero, Louisiana bicuspid aortic valve, echocardiography, congenital heart disease Diagnosis of bicuspid aortic valve (BAV) Address for correspondence and reprint requests: in the busy echocardiography laboratory is Salvatore J. Tirrito, M.D., Tulane University Health Sci- important, as it is a relatively common cardiac ences Center, Section of Cardiology SL-48, 1430 Tulane Av- enue, New Orleans, LA 71112. Fax: 504 529-9649; E-mail: congenital defect (up to 3% of the popula- 1 [email protected] tion), and requires a recommendation for Figure 1. M-mode and two-dimensional (2D) diastolic frame in the parasternal long-axis view of a bicuspid aortic valve with eccentric closure (arrows). Although not diagnostic, an eccentric line of closure should prompt one to evaluate the aortic valve closely for BAV. LA = left atrium. (Modified with permission from: Kerut EK, McIlwain, Plotnick: Handbook of Echo-Doppler Interpretation 2nd Ed, Blackwell Publishing, Elmsford, New York, 2004, p. 84) Vol. 22, No. 1, 2005 ECHOCARDIOGRAPHY: A Jrnl. of CV Ultrasound & Allied Tech. 53 TIRRITO AND KERUT Figure 2. Diastolic (left panel) and systolic (right panel) two-dimensional (2D) short-axis image of a BAV. In diastole the raphe may appear as a commissure (arrow), appearing to be a normal tri-leaflet valve. However,the systolic frame has a typical “fish-mouth” appearance. -

Bicuspid Aortic Valve
© 2012 The Children’s Heart Clinic NOTES: Children’s Heart Clinic, P.A., 2530 Chicago Avenue S, Ste 500, Minneapolis, MN 55404 West Metro: 612-813-8800 * East Metro: 651-220-8800 * Toll Free: 1-800-938-0301 * Fax: 612-813-8825 Children’s Minnesota, 2525 Chicago Avenue S, Minneapolis, MN 55404 West Metro: 612-813-6000 * East Metro: 651-220-6000 © 2012 The Children’s Heart Clinic Reviewed March 2019 Bicuspid Aortic Valve A bicuspid aortic valve is form of congenital heart disease where the aortic valve only has two leaflets, instead of three. This typically results from fusion (joining) of two cusps of the valve along their coaptation point. A bicuspid aortic valve occurs in 1-2% of the population. It can occur alone or be associated with other left-sided heart lesions, such as mitral valve abnormalities (see mitral stenosis), or coarctation of the aorta. Symptoms and presentation can vary for patients with bicuspid aortic valve depending upon the degree of stenosis (narrowing) or regurgitation (leaking) of the valve. Physical Exam/Symptoms: Most patients with bicuspid aortic valve have no symptoms (asymptomatic), unless there is associated aortic stenosis (AS) (narrowing) or regurgitation (leaking) (AR) Most children are asymptomatic with mild to moderate AS. Fatigue, chest pain with exertion, or syncope (fainting) may occur in severe AS. In critical AS, neonates develop poor perfusion, pulmonary edema (fluid retention in the lungs) within days or weeks after birth as the ductus arteriosus (see Patent Ductus Arteriosus) closes. Clinical picture may resemble that of sepsis (severe infection). Murmur of AS: Harsh, grade II/VI systolic murmur heard best at the second left intercostal space, with transmission to the head and neck. -

Dextrocardia and Hiatal Hernia in a Patient with Turner Syndrome
IJMS Vol 30, No 2, June 2005 Case Report Dextrocardia and Hiatal Hernia in a Patient with Turner Syndrome R. Vakili, M. Horri1 Abstract Turner syndrome is a sex-chromosome disorder occurring in one out of 2500 female births and characterized by growth re- tardation, gonadal dysgenesis and cardiovascular anomalies. The 45, XO karyotype is the most frequent type of this disease. Herein, we report on a 6-year-old girl with Turner syndrome and 45, XO karyotype presenting with short stature. She had dextrocardia and hiatal hernia. To the best of our knowledge, the association of Turner syndrome, dextrocardia and hiatal hernia is quite rare. Iran J Med Sci 2005; 30(2): 97-99. Keywords ● Turner syndrome ● dextrocardia ● hiatal hernia Introduction urner syndrome (TS) is the most common chromoso- mal abnormalities resulting in the loss of all or a part of T an X chromosome. The rate of the syndrome reported variably between 1/2000 and 1/5000 live born phenotypically female births.1 This syndrome is characterized by short stature, gonadal failure, low posterior hairline, thoracic and cardiovas- cular malformations.2 The occurrence of cardiac malformations in TS has long been recognized.3 Coarctation of the aorta and bicuspid aortic valves are the most common heart defects in TS.4 Other cardiovascular malformations such as aortic steno- sis and regurgitation, hypoplastic left heart have also been re- ported with less frequency.5 Case Presentation A 6-year-old girl referred to the Pediatrics Endocrinology & Me- tabolism Clinic of Mashhad University of Medical Sciences, Mashhad, Iran, for evaluation of growth retardation. -

Valvular Heart Disease CLASS (STRENGTH) of RECOMMENDATION LEVEL (QUALITY) of EVIDENCE‡ CLASS 1 (STRONG) Benefit >>> Risk LEVEL A
Clinical Update ADAPTED FROM: 2020 ACC/AHA Guideline for the Management of Patients With Valvular Heart Disease CLASS (STRENGTH) OF RECOMMENDATION LEVEL (QUALITY) OF EVIDENCE‡ CLASS 1 (STRONG) Benefit >>> Risk LEVEL A Suggested phrases for writing recommendations: • High-quality evidence‡ from more than 1 RCT • Is recommended • Meta-analyses of high-quality RCTs • Is indicated/useful/effective/beneficial • One or more RCTs corroborated by high-quality registry studies • Should be performed/administered/other Table 1. • Comparative-Effectiveness Phrases†: LEVEL B-R (Randomized) − Treatment/strategy A is recommended/indicated in preference to • Moderate-quality evidence‡ from 1 or more RCTs treatment B ACC/AHA • Meta-analyses of moderate-quality RCTs − Treatment A should be chosen over treatment B LEVEL B-NR (Nonrandomized) Applying Class of CLASS 2a (MODERATE) Benefit >> Risk • Moderate-quality evidence‡ from 1 or more well-designed, well- Suggested phrases for writing recommendations: executed nonrandomized studies, observational studies, or registry Recommendation Is reasonable • studies • Can be useful/effective/beneficial • Meta-analyses of such studies and Level of • Comparative-Effectiveness Phrases†: − Treatment/strategy A is probably recommended/indicated in preference to LEVEL C-LD (Limited Data) treatment B Evidence to − It is reasonable to choose treatment A over treatment B • Randomized or nonrandomized observational or registry studies with limitations of design or execution Clinical Strategies, CLASS 2b (Weak) Benefit ≥ Risk • Meta-analyses of such studies • Physiological or mechanistic studies in human subjects Suggested phrases for writing recommendations: Interventions, • May/might be reasonable LEVEL C-EO (Expert Opinion) • May/might be considered Treatments, or • Usefulness/effectiveness is unknown/unclear/uncertain or not well-established • Consensus of expert opinion based on clinical experience. -

A Possible Increase in the Incidence of Congenital Heart Defects Among the Offspring of Affected Parents
CORE Metadata, citation and similar papers at core.ac.uk Provided by Elsevier - Publisher Connector 376 lACC Vol. 6, No.2 August 1985:376-82 PEDIATRIC CARDIOLOGY A Possible Increase in the Incidence of Congenital Heart Defects Among the Offspring of Affected Parents VERA ROSE, BSc, MB, BS, FRCP(C) , REYNOLD JOHN MORLEY GOLD, MB, BCHIR, PHD, FCCMG, GAIL LINDSAY, RN, MSN, BScN, MARYLIN ALLEN, RN, PHN Toronto, Ontario, Canada The incidence of congenital heart disease in the children dence than that reported in most comparable studies. of219 probands was determined. Each of these probands The difference is highly significant statistically and there• had one of four selected defects: atrial septal defect, fore is likely to be genuine. The cause of the high re• coarctation of the aorta, aortic valve stenosis or complex currence is probably environmental. dextrocardia. Of their children, 8.8% had substantial (J Am Coli CardioI1985;6:376-82) congenital cardiac defects. This is a much higher inci- The successful medical and surgical treatment of congenital first degree relatives of those affected with it therefore offers heart disease has increased the importance of its early di• evidence as to whether the disease is polygenic. agnosis and this in tum has contributed to the growing Nora et al. (4) were the first to undertake family studies interest in the risk of cardiac defects in the offspring of to determine whether the actual incidence of congenital heart affected parents. Although a few cases of congenital heart disease in first degree relatives corresponds to that predicted disease are known to be caused by environmental agents, by this model. -

Pathology of the Aortic Valve: Aortic Valve Stenosis/Aortic Regurgitation
Current Cardiology Reports (2019) 21: 81 https://doi.org/10.1007/s11886-019-1162-4 STRUCTURAL HEART DISEASE (RJ SIEGEL AND NC WUNDERLICH, SECTION EDITORS) Pathology of the Aortic Valve: Aortic Valve Stenosis/Aortic Regurgitation Gregory A. Fishbein1 & Michael C. Fishbein1 Published online: 5 July 2019 # Springer Science+Business Media, LLC, part of Springer Nature 2019 Abstract Purpose of Review This discussion is intended to review the anatomy and pathology of the aortic valve and aortic root region, and to provide a basis for the understanding of and treatment of the important life-threatening diseases that affect the aortic valve. Recent Findings The most exciting recent finding is that less invasive methods are being developed to treat diseases of the aortic valve. There are no medical cures for aortic valve diseases. Until recently, open-heart surgery was the only effective method of treatment. Now percutaneous approaches to implant bioprosthetic valves into failed native or previously implanted bioprosthetic valves are being developed and utilized. A genetic basis for many of the diseases that affect the aortic valve is being discovered that also should lead to innovative approaches to perhaps prevent these disease. Sequencing of ribosomal RNA is assisting in identifying organisms causing endocarditis, leading to more effective antimicrobial therapy. Summary There is exciting, expanding, therapeutic innovation in the treatment of aortic valve disease. Keywords Aortic stenosis . Aortic regurgitation . Calcific degeneration . Bicuspid aortic valve . Rheumatic valve disease . Endocarditis . Transcatheter aortic valve implantation (TAVI) . Aortic valve replacement . Myxomatous degeneration . Endocarditis . Non-bacterial thrombotic endocarditis (NBME) Introduction aortic valve disease; however, effective methods of valve repair and replacement exist and percutaneous approaches Hemodynamically significant aortic valve disease, in one to treat aortic valve disease are being utilized with increasing form or another, is a relatively common disorder. -

Evaluation of the Mitral and Aortic Valves with Cardiac CT Angiography
PICTORIAL ESSAY Evaluation of the Mitral and Aortic Valves With Cardiac CT Angiography Samir V. Chheda, BS, Monvadi B. Srichai, MD, Robert Donnino, MD, Danny C. Kim, MD, Ruth P. Lim, MBBS, and Jill E. Jacobs, MD annulus shares structural continuity with the aortic annulus Abstract: Cardiac computed tomographic angiography (CTA) through 3 fibrous trigones (Fig. 1). Owing to this anatomic using multidetector computed tomographic scanners has proven to connection, diseases of the mitral annulus can affect the be a reliable technique to image the coronary vessels. CTA also aortic annulus and vice versa.1 Unless the mitral annulus is provides excellent visualization of the mitral and aortic valves, and calcified, its border is difficult to identify on CTA.2 yields useful information regarding valve anatomy and function. The mitral valve is the only cardiac valve with 2 Accordingly, an assessment of the valves should be performed whenever possible during CTA interpretation. In this paper, we leaflets. The anterior leaflet is semicircular in shape, highlight the imaging features of common functional and struc- whereas the posterior leaflet is rectangular. Owing to its tural left-sided valvular disorders that can be seen on CTA position within the left ventricle, the anterior leaflet also examinations. functions as a separation between the inflow and outflow tracts of the left ventricle. Key Words: computed tomography, cardiac, valves, angiography The 2 commissures are clefts that divide the 2 leaflets (J Thorac Imaging 2010;25:76–85) from each other. In some pathologic states, however, the commissural spaces may become obliterated and the leaflets appear fused. -

CHD Associated with Syndromic Diagnoses: Peri-Operative Risk Factors and Early Outcomes
CORE Metadata, citation and similar papers at core.ac.uk Provided by IUPUIScholarWorks HHS Public Access Author manuscript Author ManuscriptAuthor Manuscript Author Cardiol Manuscript Author Young. Author manuscript; Manuscript Author available in PMC 2016 November 28. Published in final edited form as: Cardiol Young. 2016 January ; 26(1): 30–52. doi:10.1017/S1047951115001389. CHD associated with syndromic diagnoses: peri-operative risk factors and early outcomes Benjamin J. Landis, David S. Cooper, and Robert B. Hinton Heart Institute, Cincinnati Children’s Hospital Medical Center, Cincinnati, Ohio, United States of America Abstract CHD is frequently associated with a genetic syndrome. These syndromes often present specific cardiovascular and non-cardiovascular co-morbidities that confer significant peri-operative risks affecting multiple organ systems. Although surgical outcomes have improved over time, these co- morbidities continue to contribute substantially to poor peri-operative mortality and morbidity outcomes. Peri-operative morbidity may have long-standing ramifications on neurodevelopment and overall health. Recognising the cardiovascular and non-cardiovascular risks associated with specific syndromic diagnoses will facilitate expectant management, early detection of clinical problems, and improved outcomes – for example, the development of syndrome-based protocols for peri-operative evaluation and prophylactic actions may improve outcomes for the more frequently encountered syndromes such as 22q11 deletion syndrome. Keywords