Diagnosing and Managing Bicuspid Aortic Valve
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

4B. the Heart (Cor) 1
Henry Gray (1821–1865). Anatomy of the Human Body. 1918. 4b. The Heart (Cor) 1 The heart is a hollow muscular organ of a somewhat conical form; it lies between the lungs in the middle mediastinum and is enclosed in the pericardium (Fig. 490). It is placed obliquely in the chest behind the body of the sternum and adjoining parts of the rib cartilages, and projects farther into the left than into the right half of the thoracic cavity, so that about one-third of it is situated on the right and two-thirds on the left of the median plane. Size.—The heart, in the adult, measures about 12 cm. in length, 8 to 9 cm. in breadth at the 2 broadest part, and 6 cm. in thickness. Its weight, in the male, varies from 280 to 340 grams; in the female, from 230 to 280 grams. The heart continues to increase in weight and size up to an advanced period of life; this increase is more marked in men than in women. Component Parts.—As has already been stated (page 497), the heart is subdivided by 3 septa into right and left halves, and a constriction subdivides each half of the organ into two cavities, the upper cavity being called the atrium, the lower the ventricle. The heart therefore consists of four chambers, viz., right and left atria, and right and left ventricles. The division of the heart into four cavities is indicated on its surface by grooves. The atria 4 are separated from the ventricles by the coronary sulcus (auriculoventricular groove); this contains the trunks of the nutrient vessels of the heart, and is deficient in front, where it is crossed by the root of the pulmonary artery. -

Having an Echocardiogram to Screen for a Bicuspid Aortic Valve
Having an echocardiogram to screen for a bicuspid aortic valve UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm What is a bicuspid aortic valve? The aortic valve sits between the main chamber of the heart (the left ventricle) and the aorta. Its function is to ensure that blood flows correctly forward from the left ventricle into the aorta. Normally it has three thin leaflets which open as the heart contracts and then close to prevent back-flow of blood towards the ventricle. Aortic valve Tricuspid aortic valve (normal) Bicuspid aortic valve (abnormal) Some people may be born with an aortic valve made up of only 2 leaflets. The valve is then called bicuspid. This may cause problems with the functioning of the valve in that it may be more prone to gradually becoming narrowed or leaky. Sometimes a bicuspid valve may be associated with widening of the portion of the aorta that is connected to it. Widening of the aorta may occur in some relatives even if they have an aortic valve with 3 leaflets. If this widening is significant it is known as an aortic aneurysm. Is a bicuspid valve a common problem? Studies have suggested that this is not an uncommon valve problem and may occur in up to 1 in 200 people. 2 | PI18_1443_03 Having an echocardiogram to screen for a bicuspid aortic valve Recently there has been evidence that this condition may be genetic and thus have a tendency to run in a family. -

Anatomy of the Heart
Anatomy of the Heart DR. SAEED VOHRA DR. SANAA AL-SHAARAWI OBJECTIVES • At the end of the lecture, the student should be able to : • Describe the shape of heart regarding : apex, base, sternocostal and diaphragmatic surfaces. • Describe the interior of heart chambers : right atrium, right ventricle, left atrium and left ventricle. • List the orifices of the heart : • Right atrioventricular (Tricuspid) orifice. • Pulmonary orifice. • Left atrioventricular (Mitral) orifice. • Aortic orifice. • Describe the innervation of the heart • Briefly describe the conduction system of the Heart The Heart • It lies in the middle mediastinum. • It is surrounded by a fibroserous sac called pericardium which is differentiated into an outer fibrous layer (Fibrous pericardium) & inner serous sac (Serous pericardium). • The Heart is somewhat pyramidal in shape, having: • Apex • Sterno-costal (anterior surface) • Base (posterior surface). • Diaphragmatic (inferior surface) • It consists of 4 chambers, 2 atria (right& left) & 2 ventricles (right& left) Apex of the heart • Directed downwards, forwards and to the left. • It is formed by the left ventricle. • Lies at the level of left 5th intercostal space 3.5 inch from midline. Note that the base of the heart is called the base because the heart is pyramid shaped; the base lies opposite the apex. The heart does not rest on its base; it rests on its diaphragmatic (inferior) surface Sterno-costal (anterior)surface • Divided by coronary (atrio- This surface is formed mainly ventricular) groove into : by the right atrium and the right . Atrial part, formed mainly by ventricle right atrium. Ventricular part , the right 2/3 is formed by right ventricle, while the left l1/3 is formed by left ventricle. -

Echo in Asymptomatic Mitral and Aortic Regurgitation
2017 ASE Florida | Orlando, FL October 9, 2017 | 10:40 – 11:00 PM | 20 min | Grand Harbor Ballroom South Echo in Asymptomatic Mitral and Aortic Regurgitation Muhamed Sarić MD, PhD, MPA Director of Noninvasive Cardiology | Echo Lab Associate Professor of Medicine Disclosures Speakers Bureau (Philips, Medtronic) Advisory Board (Siemens) Regurgitation Axioms ▪Typically, regurgitation is NOT symptomatic unless severe ▪The opposite is not true: Severe regurgitation may be asymptomatic ▪ Chronic regurgitation leads to chamber dilatation on either side of the regurgitant valve Regurgitation Discovery ▪ Regurgitation as a anatomic entity was recognized in the 17th century ▪ Regurgitation was first clinically diagnosed by auscultation in the 19th century, well before the advent of echocardiography First Use of Regurgitation Term in English 1683 W. Charleton Three Anat. Lect. i. 18 Those [valves] that are placed in the inlet and outlet of the left Ventricle, to obviate the regurgitation of the bloud into the arteria venosa, and out of the aorta into the left Ventricle. Walter Charleton (1619 – 1707) English Physician Heart Murmur OXFORD ENGLISH DICTIONARY DEFINITION ▪ Any of various auscultatory sounds ▪ Adventitious sounds of cardiac or vascular origin [that is, separate from standard heart sounds: S1, S2, S3, S4] ▪ Sometimes of no significance ▪ But sometimes caused by valvular lesions of the heart or other diseases of the Στῆθος : Stēthos = chest circulatory system René Laënnec Stethoscope (1781 – 1826) (‘Chest examiner’) French Physician Hollow wooden cylinder Inventor of stethoscope in 1816 Laënnec Performing Auscultation Painted by Robert Alan Thom (1915 – 1979), American illustrator Commissioned by Parke, Davis & Co. 1816 1832 René Laënnec, James Hope French physician British physician Invents MONAURAL stethoscope separates MS from MR murmur 1852 1862 George Cammann Austin Flint Sr. -

Congenital Mitral Incompetence and Coarctation Ofaorta
Thorax: first published as 10.1136/thx.27.6.729 on 1 November 1972. Downloaded from Thorax (1972), 27, 729. Congenital mitral incompetence and coarctation of aorta Report of two cases treated surgically' ABDEL K. TERZAKI2, ROBERT D. LEACHMAN3, M. KHALIL ALI, GRADY L. HALLMAN, and DENTON A. COOLEY Department of Medicine and the Cora and Webb Mading Department of Surgery, Baylor University College of Medicine, and the Cardiology and Surgical Sections of the Texas Heart Institute of St. Luke's Episcopal and Texas Children's Hospitals, Houston, Texas, U.S.A. Two patients with congenital mitral incompetence and coarctation of the aorta are presented. One patient had associated patent ductus arteriosus, bicuspid aortic valve, and endocardial fibro- elastosis. The diagnosis in the two patients presented is well established by clinical, laboratory, and surgical findings and also by necropsy examination in one case. It is proposed that the rarity of reported cases in the literature may have resulted from the frequent diagnosis of left ventricular failure in infancy secondary to coarctation, leading to the assumption that a mitral insufficiency murmur, when present, is due to functional regurgitation. Likewise, the murmur may be mistakenly thought to originate from a ventricular septal defect. The diagnosis of coarctation of the aorta presented no problem in either patient, while detection of the mitral incompetence was difficult. Coarctation of the aorta complicated by copyright. pulmonary hypertension in the absence of intracardiac shunt should draw attention to the possi- bility of associated mitral incompetence. Congestive heart failure, especially after correction of coarctation, was also an indication of possible associated mitral insufficiency. -

The Functional Anatomy of the Heart. Development of the Heart, Anomalies
The functional anatomy of the heart. Development of the heart, anomalies Anatomy and Clinical Anatomy Department Anastasia Bendelic Plan: Cardiovascular system – general information Heart – functional anatomy Development of the heart Abnormalities of the heart Examination in a living person Cardiovascular system Cardiovascular system (also known as vascular system, or circulatory system) consists of: 1. heart; 2. blood vessels (arteries, veins, capillaries); 3. lymphatic vessels. Blood vessels Arteries are blood vessels that carry blood away from the heart. Veins carry blood back towards the heart. Capillaries are tiny blood vessels, that connect arteries to veins. Lymphatic vessels: lymphatic capillaries; lymphatic vessels (superficial and deep lymph vessels); lymphatic trunks (jugular, subclavian, bronchomediastinal, lumbar, intestinal trunks); lymphatic ducts (thoracic duct and right lymphatic duct). Lymphatic vessels Microcirculation Microcirculatory bed comprises 7 components: 1. arterioles; 2. precapillaries or precapillary arterioles; 3. capillaries; 4. postcapillaries or postcapillary venules; 5. venules; 6. lymphatic capillaries; 7. interstitial component. Microcirculation The heart Heart is shaped as a pyramid with: an apex (directed downward, forward and to the left); a base (facing upward, backward and to the right). There are four surfaces of the heart: sternocostal (anterior) surface; diaphragmatic (inferior) surface; right pulmonary surface; left pulmonary surface. External surface of the heart The heart The heart has four chambers: right and left atria; right and left ventricles. Externally, the atria are demarcated from the ventricles by coronary sulcus (L. sulcus coronarius). The right and left ventricles are demarcated from each other by anterior and posterior interventricular sulci (L. sulci interventriculares anterior et posterior). Chambers of the heart The atria The atria are thin-walled chambers, that receive blood from the veins and pump it into the ventricles. -

Prevalence of Migraine Headaches in Patients with Congenital Heart Disease
Prevalence of Migraine Headaches in Patients With Congenital Heart Disease Tam Truong, MD, Leo Slavin, MD, Ramin Kashani, BA, James Higgins, MD, Aarti Puri, BS, Malika Chowdhry, BS, Philip Cheung, BS, Adam Tanious, BA, John S. Child, MD, FAHA, Joseph K. Perloff, MD, and Jonathan M. Tobis, MD* The prevalence of migraine headaches (MH) is 12% in the general population and increases to 40% in patients with patent foramen ovale. This study evaluated the prevalence of MH in patients with congenital heart disease (CHD). Of 466 patients contacted from the UCLA Adult Congenital Heart Disease Center, 395 (85%) completed a questionnaire to determine the prevalence of MH. Patients were stratified by diagnosis of right-to-left, left-to-right, or no shunt. A group of 252 sex-matched patients with acquired cardiovascular disease served as controls. The prevalence of MH was 45% in adults with CHD compared to 11% in the controls (p <0.001). Of the 179 patients with MH, 143 (80%) had migraines with aura and 36 (20%) had migraines without aura versus 36% and 64% observed in the controls (p <0.001). The frequency of MH was 52% in the right-to-left shunt group, 44% in the left-to-right, and 38% in the no ,NS). In patients with a right-to-left shunt who underwent surgical repair ؍ shunt group (p 47% had complete resolution of MH, whereas 76% experienced >50% reduction in headache days per month. In conclusion, the prevalence of MH in all groups of adults with CHD is 3 to 4 times more than a sex-matched control population, with increasing prevalence of MH in patients with no shunt, left-to-right, and right-to-left shunt. -

Regulation of the Aortic Valve Opening
REGULATION OF THE Aortic valve orifice area was dynamically measured in anesthetized dogs AORTIC VALVE OPENING with a new measuring system involving electromagnetic induction. This system permits us real-time measurement of the valve orifice area in In vivo dynamic beating hearts in situ. The aortic valve was already open before aortic measurement of aortic pressure started to increase without detectable antegrade aortic flow. valve orifice area Maximum opening area was achieved while flow was still accelerating at a mean of 20 to 35 msec before peak blood flow. Maximum opening area was affected by not only aortic blood flow but also aortic pressure, which produced aortic root expansion. The aortic valve orifice area's decreasing curve (corresponding to valve closure) was composed of two phases: the initial decrease and late decrease. The initial decrease in aortic valve orifice area was slower (4.1 cm2/sec) than the late decrease (28.5 cm2/sec). Aortic valve orifice area was reduced from maximum to 40% of maximum (in a triangular open position) during the initial slow closing. These measure- ments showed that (1) initial slow closure of the aortic valve is evoked by leaflet tension which is produced by the aortic root expansion (the leaflet tension tended to make the shape of the aortic orifice triangular) and (2) late rapid closure is induced by backflow of blood into the sinus of Valsalva. Thus, cusp expansion owing to intraaortic pressure plays an important role in the opening and closing of the aortic valve and aortic blood flow. (J THORAC CARDIOVASC SURG 1995;110:496-503) Masafumi Higashidate, MD, a Kouichi Tamiya, MD, b Toshiyuki Beppu, MS, b and Yasuharu Imai, MD, a Tokyo, Japan n estimation of orifice area of the aortic valve is ers, 4 as well as echocardiography. -

1-Anatomy of the Heart.Pdf
Color Code Important Anatomy of the Heart Doctors Notes Notes/Extra explanation Please view our Editing File before studying this lecture to check for any changes. Objectives At the end of the lecture, the student should be able to : ✓Describe the shape of heart regarding : apex, base, sternocostal and diaphragmatic surfaces. ✓Describe the interior of heart chambers : right atrium, right ventricle, left atrium and left ventricle. ✓List the orifices of the heart : • Right atrioventricular (Tricuspid) orifice. • Pulmonary orifice. • Left atrioventricular (Mitral) orifice. • Aortic orifice. ✓Describe the innervation of the heart. ✓Briefly describe the conduction system of the Heart. The Heart o It lies in the middle mediastinum. o It consists of 4 chambers: • 2 atria (right& left) that receive blood & • 2 ventricles (right& left) that pump blood. o The Heart is somewhat pyramidal in shape, having: 1. Apex Extra 2. Sterno-costal (anterior surface) 3. Diaphragmatic (inferior surface) 4. Base (posterior surface). o It is surrounded by a fibroserous sac called pericardium which is differentiated into: an outer fibrous layer inner serous sac (Fibrous pericardium) (Serous pericardium). further divided into Parietal Visceral (Epicardium) The Heart Extra Extra The Heart 1- Apex o Directed downwards, forwards and to the left. o It is formed by the left ventricle. o Lies at the level of left 5th intercostal space (the same level of the nipple) 3.5 inch from midline. Note that the base of the heart is called the base because the heart is pyramid shaped; the base lies opposite to the apex. The heart does not rest on its base; it rests on its diaphragmatic (inferior) surface. -

Unit 1 Anatomy of the Heart
UNIT 1 ANATOMY OF THE HEART Structure 1.0 Objectives 1.1 Introduction 1.2 Chambers of Heart 1.3 Orifices of Heart 1.4 The Conducting System of the Heart 1.5 Blood Supply of the Heart 1.6 Surface Markings of the Heart 1.7 Let Us Sum Up 1.8 Answers to Check Your Progress 1.0 OBJECTIVES After reading this unit, you should be able to: • understand the proper position of a heart inside the thorax; • know the various anatomical structures of various chambers of heart and various valves of heart; • know the arterial supply, venous drainage and lymphatic drainage of heart; and • describe the surface marking of heart. 1.1 INTRODUCTION The human heart is a cone-shaped, four-chambered muscular pump located in the mediastinal cavity of the thorax between the lungs and beneath the sternum, designed to ensure the circulation through the tissues of the body. The cone-shaped heart lies on its side on the diaphragm, with its base (the widest part) upward and leaning toward the right shoulder, and its apex pointing down and to the left. Structurally and functionally it consists of two halves–right and left. The right heart circulates blood only through the lungs for the purpose of pulmonary circulation. The left heart sends blood to tissues of entire body/systemic circulation. The heart is contained in a sac called the pericardium. The four chambers are right and left atria and right and left ventricles. The heart lies obliquely across the thorax and the right side is turned to face the front. -
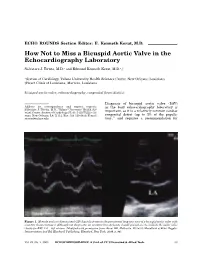
How Not to Miss a Bicuspid Aortic Valve in the Echocardiography Laboratory
ECHO ROUNDS Section Editor: E. Kenneth Kerut, M.D. How Not to Miss a Bicuspid Aortic Valve in the Echocardiography Laboratory Salvatore J. Tirrito, M.D.∗ and Edmund Kenneth Kerut, M.D.∗,† ∗Section of Cardiology, Tulane University Health Sciences Center, New Orleans, Louisiana †Heart Clinic of Louisiana, Marrero, Louisiana bicuspid aortic valve, echocardiography, congenital heart disease Diagnosis of bicuspid aortic valve (BAV) Address for correspondence and reprint requests: in the busy echocardiography laboratory is Salvatore J. Tirrito, M.D., Tulane University Health Sci- important, as it is a relatively common cardiac ences Center, Section of Cardiology SL-48, 1430 Tulane Av- enue, New Orleans, LA 71112. Fax: 504 529-9649; E-mail: congenital defect (up to 3% of the popula- 1 [email protected] tion), and requires a recommendation for Figure 1. M-mode and two-dimensional (2D) diastolic frame in the parasternal long-axis view of a bicuspid aortic valve with eccentric closure (arrows). Although not diagnostic, an eccentric line of closure should prompt one to evaluate the aortic valve closely for BAV. LA = left atrium. (Modified with permission from: Kerut EK, McIlwain, Plotnick: Handbook of Echo-Doppler Interpretation 2nd Ed, Blackwell Publishing, Elmsford, New York, 2004, p. 84) Vol. 22, No. 1, 2005 ECHOCARDIOGRAPHY: A Jrnl. of CV Ultrasound & Allied Tech. 53 TIRRITO AND KERUT Figure 2. Diastolic (left panel) and systolic (right panel) two-dimensional (2D) short-axis image of a BAV. In diastole the raphe may appear as a commissure (arrow), appearing to be a normal tri-leaflet valve. However,the systolic frame has a typical “fish-mouth” appearance. -

Bicuspid Aortic Valve
© 2012 The Children’s Heart Clinic NOTES: Children’s Heart Clinic, P.A., 2530 Chicago Avenue S, Ste 500, Minneapolis, MN 55404 West Metro: 612-813-8800 * East Metro: 651-220-8800 * Toll Free: 1-800-938-0301 * Fax: 612-813-8825 Children’s Minnesota, 2525 Chicago Avenue S, Minneapolis, MN 55404 West Metro: 612-813-6000 * East Metro: 651-220-6000 © 2012 The Children’s Heart Clinic Reviewed March 2019 Bicuspid Aortic Valve A bicuspid aortic valve is form of congenital heart disease where the aortic valve only has two leaflets, instead of three. This typically results from fusion (joining) of two cusps of the valve along their coaptation point. A bicuspid aortic valve occurs in 1-2% of the population. It can occur alone or be associated with other left-sided heart lesions, such as mitral valve abnormalities (see mitral stenosis), or coarctation of the aorta. Symptoms and presentation can vary for patients with bicuspid aortic valve depending upon the degree of stenosis (narrowing) or regurgitation (leaking) of the valve. Physical Exam/Symptoms: Most patients with bicuspid aortic valve have no symptoms (asymptomatic), unless there is associated aortic stenosis (AS) (narrowing) or regurgitation (leaking) (AR) Most children are asymptomatic with mild to moderate AS. Fatigue, chest pain with exertion, or syncope (fainting) may occur in severe AS. In critical AS, neonates develop poor perfusion, pulmonary edema (fluid retention in the lungs) within days or weeks after birth as the ductus arteriosus (see Patent Ductus Arteriosus) closes. Clinical picture may resemble that of sepsis (severe infection). Murmur of AS: Harsh, grade II/VI systolic murmur heard best at the second left intercostal space, with transmission to the head and neck.