DNA Damage in Neurodegenerative Diseases
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

BER and Folate Deficiency: a Comprehensive Overview of DNA Base Excision Repair and the Effect of Dietary Folate Lydia Lanni [email protected]
Wayne State University Honors College Theses Irvin D. Reid Honors College Winter 5-7-2012 BER and Folate Deficiency: A comprehensive overview of DNA base excision repair and the effect of dietary folate Lydia Lanni [email protected] Follow this and additional works at: https://digitalcommons.wayne.edu/honorstheses Part of the Human and Clinical Nutrition Commons Recommended Citation Lanni, Lydia, "BER and Folate Deficiency: A comprehensive overview of DNA base excision repair and the effect of dietary folate" (2012). Honors College Theses. 2. https://digitalcommons.wayne.edu/honorstheses/2 This Honors Thesis is brought to you for free and open access by the Irvin D. Reid Honors College at DigitalCommons@WayneState. It has been accepted for inclusion in Honors College Theses by an authorized administrator of DigitalCommons@WayneState. Running head: BER AND FOLATE DEFICIENCY 1 BER and Folate Deficiency: A comprehensive overview of DNA base excision repair and the effect of dietary folate Lydia Lanni Wayne State University Honors Thesis Winter 2012 Author Note A special thank you to Dr. Diane Cabelof and all those in her lab for their instruction and support. BER AND FOLATE DEFICIENCY 2 Abstract Folate is the naturally occurring form of water-soluble B vitamin that is found in foods such as leafy vegetables, fruits, legumes, etc. Dietary supplementation of folate has shown to be protective against neural tube defects and other congenital disorders, and of recent, its role in carcinogenesis has been of special interest. Though mechanistically unclear, a positive correlation has been observed between folate deficiency in the diet and decrease function of DNA base excision repair pathways. -

Oxidative Stress in Sperm Affects the Epigenetic Reprogramming in Early
Wyck et al. Epigenetics & Chromatin (2018) 11:60 https://doi.org/10.1186/s13072-018-0224-y Epigenetics & Chromatin RESEARCH Open Access Oxidative stress in sperm afects the epigenetic reprogramming in early embryonic development Sarah Wyck1,2,3, Carolina Herrera1, Cristina E. Requena4,5, Lilli Bittner1, Petra Hajkova4,5, Heinrich Bollwein1* and Rafaella Santoro2* Abstract Background: Reactive oxygen species (ROS)-induced oxidative stress is well known to play a major role in male infer- tility. Sperm are sensitive to ROS damaging efects because as male germ cells form mature sperm they progressively lose the ability to repair DNA damage. However, how oxidative DNA lesions in sperm afect early embryonic develop- ment remains elusive. Results: Using cattle as model, we show that fertilization using sperm exposed to oxidative stress caused a major developmental arrest at the time of embryonic genome activation. The levels of DNA damage response did not directly correlate with the degree of developmental defects. The early cellular response for DNA damage, γH2AX, is already present at high levels in zygotes that progress normally in development and did not signifcantly increase at the paternal genome containing oxidative DNA lesions. Moreover, XRCC1, a factor implicated in the last step of base excision repair (BER) pathway, was recruited to the damaged paternal genome, indicating that the maternal BER machinery can repair these DNA lesions induced in sperm. Remarkably, the paternal genome with oxidative DNA lesions showed an impairment of zygotic active DNA demethylation, a process that previous studies linked to BER. Quantitative immunofuorescence analysis and ultrasensitive LC–MS-based measurements revealed that oxidative DNA lesions in sperm impair active DNA demethylation at paternal pronuclei, without afecting 5-hydroxymethyl- cytosine (5hmC), a 5-methylcytosine modifcation that has been implicated in paternal active DNA demethylation in mouse zygotes. -

Uracil DNA Glycosylase (UDG) Sugar, Leaving an Abasic Site in Uracil-Containing Single Or Double-Stranded DNA
Product Specifications G5010L Rev F Product Description: Uracil-DNA Glycosylase catalyzes the Product Information hydrolysis of the N-glycosylic bond between the uracil and sugar, leaving an abasic site in uracil-containing single or Uracil DNA Glycosylase (UDG) double-stranded DNA. The enzyme shows no measurable Part Number G5010L activity on short oligonucleotides (<6 bases), or RNA substrates. Concentration 2,000 U/mL Unit Size 10,000 U Storage Temperature -25⁰C to -15⁰C Product Specifications G5010 Specific SS DS E. coli DNA Assay SDS Purity DS Exonuclease Activity Exonuclease Endonuclease Contamination Units Tested n/a n/a 100 100 100 100 >99% 77,000 U/mg <5.0% <1.0% No Conversion <10 copies Specification Released Released Source of Protein: A recombinant E. coli strain carrying the Uracil DNA Glycosylase gene from E. coli K-12. Unit Definition: 1 unit is defined as the amount of enzyme that catalyzes the release of 1.8 nmol of Uracil in 30 minutes from double-stranded, tritiated, Uracil containing-DNA at 37°C in 1X UDG Reaction Buffer. Molecular weight: 25,693 Daltons Quality Control Analysis: Unit Activity is measured using a 2-fold serial dilution method. Dilutions of enzyme were made in 1X reaction buffer and added to 50 µL reactions containing a 3H-dUTP PCR product and 1X UDG Reaction Buffer. Reactions were incubated for 10 minutes at 37°C, plunged on ice, and analyzed using a TCA-precipitation methods. Protein Concentration (OD 280 ) is determined by OD 280 absorbance. Physical Purity is evaluated by SDS-PAGE of concentrated and diluted enzyme solutions followed by silver stain detection. -

3-Methyladenine DNA Glycosylases: Structure, Function, and Biological Importance Michael D
Review articles 3-Methyladenine DNA glycosylases: structure, function, and biological importance Michael D. Wyatt,1 James M. Allan,1 Albert Y. Lau,2 Tom E. Ellenberger,2 and Leona D. Samson1* Summary The genome continuously suffers damage due to its reactivity with chemical and physical agents. Finding such damage in genomes (that can be several million to several billion nucleotide base pairs in size) is a seemingly daunting task. 3-Methyladenine DNA glycosylases can initiate the base excision repair (BER) of an extraordinarily wide range of substrate bases. The advantage of such broad substrate recognition is that these enzymes provide resistance to a wide variety of DNA damaging agents; however, under certain circumstances, the eclectic nature of these enzymes can confer some biological disadvantages. Solving the X-ray crystal struc- tures of two 3-methyladenine DNA glycosylases, and creating cells and animals altered for this activity, contributes to our understanding of their enzyme mechanism and how such enzymes influence the biological response of organisms to several different types of DNA damage. BioEssays 21:668–676, 1999. 1999 John Wiley & Sons, Inc. Introduction ately interpreted by DNA-processing enzymes. Unfortunately, DNA carries life’s genetic information encoded in the arrange- these bases are also chemically reactive, and the inevitable ment of bases along the length of the DNA molecule. Each base modifications produce a variety of biological outcomes, DNA base has a distinct chemical structure that is appropri- depending on how a cell recognizes and responds to the modification. Cellular DNA repair mechanisms target these inappropriate DNA structures, and play a vital role in maintain- 1Department of Cancer Cell Biology, Harvard School of Public Health, ing genomic integrity. -

(12) United States Patent (10) Patent No.: US 9,689,046 B2 Mayall Et Al
USOO9689046B2 (12) United States Patent (10) Patent No.: US 9,689,046 B2 Mayall et al. (45) Date of Patent: Jun. 27, 2017 (54) SYSTEM AND METHODS FOR THE FOREIGN PATENT DOCUMENTS DETECTION OF MULTIPLE CHEMICAL WO O125472 A1 4/2001 COMPOUNDS WO O169245 A2 9, 2001 (71) Applicants: Robert Matthew Mayall, Calgary (CA); Emily Candice Hicks, Calgary OTHER PUBLICATIONS (CA); Margaret Mary-Flora Bebeselea, A. et al., “Electrochemical Degradation and Determina Renaud-Young, Calgary (CA); David tion of 4-Nitrophenol Using Multiple Pulsed Amperometry at Christopher Lloyd, Calgary (CA); Lisa Graphite Based Electrodes', Chem. Bull. “Politehnica” Univ. Kara Oberding, Calgary (CA); Iain (Timisoara), vol. 53(67), 1-2, 2008. Fraser Scotney George, Calgary (CA) Ben-Yoav. H. et al., “A whole cell electrochemical biosensor for water genotoxicity bio-detection”. Electrochimica Acta, 2009, 54(25), 6113-6118. (72) Inventors: Robert Matthew Mayall, Calgary Biran, I. et al., “On-line monitoring of gene expression'. Microbi (CA); Emily Candice Hicks, Calgary ology (Reading, England), 1999, 145 (Pt 8), 2129-2133. (CA); Margaret Mary-Flora Da Silva, P.S. et al., “Electrochemical Behavior of Hydroquinone Renaud-Young, Calgary (CA); David and Catechol at a Silsesquioxane-Modified Carbon Paste Elec trode'. J. Braz. Chem. Soc., vol. 24, No. 4, 695-699, 2013. Christopher Lloyd, Calgary (CA); Lisa Enache, T. A. & Oliveira-Brett, A. M., "Phenol and Para-Substituted Kara Oberding, Calgary (CA); Iain Phenols Electrochemical Oxidation Pathways”, Journal of Fraser Scotney George, Calgary (CA) Electroanalytical Chemistry, 2011, 1-35. Etesami, M. et al., “Electrooxidation of hydroquinone on simply prepared Au-Pt bimetallic nanoparticles'. Science China, Chem (73) Assignee: FREDSENSE TECHNOLOGIES istry, vol. -
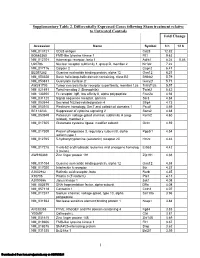
Supplementary Table 2
Supplementary Table 2. Differentially Expressed Genes following Sham treatment relative to Untreated Controls Fold Change Accession Name Symbol 3 h 12 h NM_013121 CD28 antigen Cd28 12.82 BG665360 FMS-like tyrosine kinase 1 Flt1 9.63 NM_012701 Adrenergic receptor, beta 1 Adrb1 8.24 0.46 U20796 Nuclear receptor subfamily 1, group D, member 2 Nr1d2 7.22 NM_017116 Calpain 2 Capn2 6.41 BE097282 Guanine nucleotide binding protein, alpha 12 Gna12 6.21 NM_053328 Basic helix-loop-helix domain containing, class B2 Bhlhb2 5.79 NM_053831 Guanylate cyclase 2f Gucy2f 5.71 AW251703 Tumor necrosis factor receptor superfamily, member 12a Tnfrsf12a 5.57 NM_021691 Twist homolog 2 (Drosophila) Twist2 5.42 NM_133550 Fc receptor, IgE, low affinity II, alpha polypeptide Fcer2a 4.93 NM_031120 Signal sequence receptor, gamma Ssr3 4.84 NM_053544 Secreted frizzled-related protein 4 Sfrp4 4.73 NM_053910 Pleckstrin homology, Sec7 and coiled/coil domains 1 Pscd1 4.69 BE113233 Suppressor of cytokine signaling 2 Socs2 4.68 NM_053949 Potassium voltage-gated channel, subfamily H (eag- Kcnh2 4.60 related), member 2 NM_017305 Glutamate cysteine ligase, modifier subunit Gclm 4.59 NM_017309 Protein phospatase 3, regulatory subunit B, alpha Ppp3r1 4.54 isoform,type 1 NM_012765 5-hydroxytryptamine (serotonin) receptor 2C Htr2c 4.46 NM_017218 V-erb-b2 erythroblastic leukemia viral oncogene homolog Erbb3 4.42 3 (avian) AW918369 Zinc finger protein 191 Zfp191 4.38 NM_031034 Guanine nucleotide binding protein, alpha 12 Gna12 4.38 NM_017020 Interleukin 6 receptor Il6r 4.37 AJ002942 -

Biochemical Characterization and Mutational Studies of a Novel 3
Biochemical characterization and mutational studies of a novel 3-methlyadenine DNA glycosylase II from the hyperthermophilic Thermococcus gammatolerans Donghao Jiang, Likui Zhang, Kunming Dong, Yong Gong, Philippe Oger To cite this version: Donghao Jiang, Likui Zhang, Kunming Dong, Yong Gong, Philippe Oger. Biochemical characteriza- tion and mutational studies of a novel 3-methlyadenine DNA glycosylase II from the hyperthermophilic Thermococcus gammatolerans. DNA Repair, Elsevier, 2021. hal-03035060 HAL Id: hal-03035060 https://hal.archives-ouvertes.fr/hal-03035060 Submitted on 2 Dec 2020 HAL is a multi-disciplinary open access L’archive ouverte pluridisciplinaire HAL, est archive for the deposit and dissemination of sci- destinée au dépôt et à la diffusion de documents entific research documents, whether they are pub- scientifiques de niveau recherche, publiés ou non, lished or not. The documents may come from émanant des établissements d’enseignement et de teaching and research institutions in France or recherche français ou étrangers, des laboratoires abroad, or from public or private research centers. publics ou privés. REVISED Manuscript (text UNmarked) Biochemical characterization and mutational studies of a novel 3-methlyadenine DNA glycosylase II from the hyperthermophilic Thermococcus gammatolerans Donghao Jianga, Likui Zhanga,b#, Kunming Donga, Yong Gongc# and Philippe Ogerd# aMarine Science & Technology Institute, College of Environmental Science and Engineering, Yangzhou University, China bGuangling College, Yangzhou University, China cBeijing Synchrotron Radiation Facility, Institute of High Energy Physics, Chinese Academy of Sciences, China dUniv Lyon, INSA de Lyon, CNRS UMR 5240, Lyon, France The first corresponding author: Dr. Likui Zhang E-mail address: [email protected] Tel: +86-514-89795882 Fax: +86-514-87357891 Corresponding author: Dr. -
51 Norway Carcinomas, 3 Fibroadenomas and 4 Normal Breast Samples Clustered Using the "Intrinsic" Gene Set
51 Norway Carcinomas, 3 Fibroadenomas and 4 Normal Breast Samples clustered using the "Intrinsic" Gene Set >8 >6 >4 >2 1:1 >2 >4 >6 >8 st1 st3 st2 st1 Y 55-BE Y 112-BE Y 65-BE Y 61-BE Y 104-BE Y 12-BE Y 10-BE Y 39-BE Y 17-BE Y 100-BE Y 14-BE Y 53-BE Y 101-BE Y 57-BE Y 47-BE Y 102-BE Y 26-BE Y 11-BE Y 7-BE Y 95-BE Y 22-BE Y 15-BE Y 19-BE Y 48-BE Y 51-BE Y 41-BE Y 21-BE Y 37-AF Y 81-AF Y 63-BE Y 109-BE Y 80-BE Y 85-BE Y 24-BE Y 43-AF Y 32-BE Y 111-BE Y 4-BE Y 16-BE Y 56-BE Y 8-BE Y 74-BE Y 6-BE Y 27-BE Y 18-BE Y 64-BE Y 96-AF Y 98-BE Y 29-BE Y 90-BE Y 83-BE A A A A A A A A A A A A A A A A A A A A A A A A A A A A A A A A A A A A A A A A A A A A A A A A A A A W W W W W W W W W W W W W W W W W W W W W W W W W W W W W W W W W W W W W W W W W W W W W W W W W W W NOR NOR NorwNormBr NormBr NormBr NormBr NOR NOR Benign STF 11 Benign STF 20 Benign STF 37 NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR NOR GDNF family receptor alpha 1 AA512935 amylo-1,6-glucosidase, 4-alpha-glucanotransferase glycogen debranching enzyme, glycogen storage disease type III AA668425 karyopherin alpha 6 importin alpha 7 AA009595 matrix Gla protein R76277 cadherin 1, type 1, E-cadherin epithelial W86859 cadherin 1, type 1, E-cadherin epithelial H97778 glutamic-oxaloacetic transaminase 2, mitochondrial aspartate aminotransferase 2 AA487521 KIAA0182 protein AI023801 Homo sapiens cDNA: FLJ21918 fis, clone HEP04006 T72068 serine protease inhibitor, Kunitz type, 2 AA031287 epididymis-specific, whey-acidic protein type, four-disulfide core; putative ovarian carcinoma marker AA451904 dermatan sulphate proteoglycan 3 AA131238 paternally expressed 3 AA459941 hypothetical protein FLJ20510 N53214 laminin, alpha 5 AA459289 Ser-Thr protein kinase related to the myotonic dystrophy protein kinase N35241 Putative prostate cancer tumor suppressor H13424 HBV pX associated protein-8 N69398 C3H-type zinc finger protein; similar to D. -

Reduced Hydrophobicity of the Minor Groove Intercalation Loop Is Critical
dynam mo ic er s h & T Moe et al., J Thermodyn Catal 2015, 6:3 f C o a t l DOI: 10.4172/2157-7544.1000155 a a l Journal of y n r s i u s o J ISSN: 2157-7544 Thermodynamics & Catalysis Research Article Open Access Reduced Hydrophobicity of the Minor Groove Intercalation Loop is Critical for Efficient Catalysis by Cold Adapted Uracil-DNA N-Glycosylase from Atlantic Cod Elin Moe1*, Netsanet Gizaw Assefa1, Ingar Leiros1, Kathrin Torseth2, Arne O Smalås1 and Nils Peder Willassen1 1The Norwegian Structural Biology Centre, University of Tromsø, N-9037 Tromsø, Norway 2Department of Laboratory Medicine, Children’s and Women’s Health, Norwegian University of Science and Technology, N-7489 Trondheim, Norway Abstract The minor groove intercalation loop (leucine-loop) in Uracil-DNA N-glycosylases (UNGs) undergoes significant conformational changes upon substrate interaction. Previous studies have shown that the cold adapted Atlantic cod UNG (cUNG) possesses a tenfold higher catalytic efficiency than human UNG (hUNG). A sequence alignment of the two enzymes revealed amino acid substitutions in and near the leucine-loop of cUNG which may increase the elasticity of the loop and thus explain the observed higher catalytic efficiency of cUNG compared to hUNG. In order to investigate this hypothesis we constructed five single and four multiple mutants of cUNG with cod to human UNG substitutions and characterised them by kinetic experiments at three different temperatures (15, 22 and 37°C) and Differential Scanning Calorimetry (DSC). The results showed that the mutations affected the kcat more than the KM, and mutants with apparent reduced hydrophobic properties (A266T, V267A, A266T/V267A and A266T/ V267A/A274V) showed increased or equivalent kcat to cUNG, while mutants with predicted increased hydrophobicity (A274V, H275Y, L279F, A266T/V267A/A274V/H275Y and A266T/V267A/A274V/H275Y/H250Q) showed reduced kcat compared to cUNG. -

Genomic Reconstruction of Fossil and Living Microorganisms in Ancient Siberian Permafrost Renxing Liang1* , Zhou Li2, Maggie C
Liang et al. Microbiome (2021) 9:110 https://doi.org/10.1186/s40168-021-01057-2 RESEARCH Open Access Genomic reconstruction of fossil and living microorganisms in ancient Siberian permafrost Renxing Liang1* , Zhou Li2, Maggie C. Y. Lau Vetter1,3, Tatiana A. Vishnivetskaya4,5, Oksana G. Zanina5, Karen G. Lloyd4, Susan M. Pfiffner4, Elizaveta M. Rivkina5, Wei Wang6, Jessica Wiggins6, Jennifer Miller6, Robert L. Hettich2 and Tullis C. Onstott1 Abstract Background: Total DNA (intracellular, iDNA and extracellular, eDNA) from ancient permafrost records the mixed genetic repository of the past and present microbial populations through geological time. Given the exceptional preservation of eDNA under perennial frozen conditions, typical metagenomic sequencing of total DNA precludes the discrimination between fossil and living microorganisms in ancient cryogenic environments. DNA repair protocols were combined with high throughput sequencing (HTS) of separate iDNA and eDNA fraction to reconstruct metagenome-assembled genomes (MAGs) from ancient microbial DNA entrapped in Siberian coastal permafrost. Results: Despite the severe DNA damage in ancient permafrost, the coupling of DNA repair and HTS resulted in a total of 52 MAGs from sediments across a chronosequence (26–120 kyr). These MAGs were compared with those derived from the same samples but without utilizing DNA repair protocols. The MAGs from the youngest stratum showed minimal DNA damage and thus likely originated from viable, active microbial species. Many MAGs from the older and deeper sediment appear related to past aerobic microbial populations that had died upon freezing. MAGs from anaerobic lineages, including Asgard archaea, however exhibited minimal DNA damage and likely represent extant living microorganisms that have become adapted to the cryogenic and anoxic environments. -

Characterization of the Regulation of the Er Stress Response by the Dna Repair Enzyme Aag
DECIPHERING THE CROSSTALK: CHARACTERIZATION OF THE REGULATION OF THE ER STRESS RESPONSE BY THE DNA REPAIR ENZYME AAG Clara Forrer Charlier Faculty of Health and Medical Sciences Department of Biochemistry and Physiology This thesis is submitted for the degree of Doctor of Philosophy June 2018 DECIPHERING THE CROSSTALK: CHARACTERIZATION OF THE REGULATION OF THE ER STRESS RESPONSE BY THE DNA REPAIR ENZYME AAG- Clara Forrer Charlier – June 2018 SUMMARY The genome is a very dynamic store of genetic information and constantly threatened by endogenous and exogenous damaging agents. To maintain fidelity of the information stored, several robust and overlapping repair pathways, such as the Base Excision Repair (BER) pathway, have evolved. The main BER glycosylase responsible for repairing alkylation DNA damage is the alkyladenine DNA glycosylase (AAG). Repair initiated by AAG can lead to accumulation of cytotoxic intermediates. Here, we report the involvement of AAG in the elicitation of the unfolded protein response (UPR), a mechanism triggered to restore proteostasis in the cell whose dysfunction is implicated in diseases like diabetes, Alzheimer’s disease and cancer. Firstly, we determined that not only human ARPE-19 cells were capable of eliciting the UPR, but that an alkylating agent, methyl methanesulfonate (MMS), also triggers the response, and that in the absence of AAG the response is greatly diminished. Our luciferase reporter assay indicates that the response is activated on multiple branches (IRE1 and ATF6) on both AAG-proficient and deficient cells. Although no transcriptional induction of UPR markers was detected by RT-qPCR at 6 hours post MMS treatment, preliminary western-blot data at 6 and 24h, show activation of key UPR markers (p-eIF2α, BiP and XBP-1) upon MMS treatment in wild-type cells and little or no activation on AAG -/-. -

Introduction the Terms in the Subject Index for Volume 81, January
Introduction The terms in the Subject Index for Volume 81, January-December 1984, of the PROCEEDINGS OF THE NATIONAL ACADEMY OF SCIENCES USA (Biological Sci- ences) were chosen from titles, key terms, and abstracts of articles. The index terms are alphabetized by computer; numbers, conformational prefixes, and hy- phenated Greek letters are disregarded in alphabetization. 8041 8042 Biological Sciences Subject Index Proc. Natl. Acad. Sci. USA 81 (1984) A* protein Different channel properties of Torpedo acetylcholine receptor monomers Cleavage of single-stranded DNA by the <X174 A* protein: The A*- and dimers reconstituted in planar membranes, 6222 single-stranded DNA covalent linkage, 4285 Phosphorylation of the nicotinic acetylcholine receptor by an endogenous Abelson murine leukemia virus tyrosine-specific protein kinase, 6968 Transformation-associated proteins in murine B-cell lymphomas that are Purification of the muscarinic acetylcholine receptor from porcine atria distinct from Abelson virus gene products, 4434 (Correction), 7258 Abortive infection Acetylcholine receptor-specific suppressive T-cell factor from a Virus-plasmid interactions: Mutants of bacteriophage T3 that abortively retrovirally transformed T-cell line, 7569 infect plasmid F-containing (F+) strains of Escherichia coli, 1465 Isolation and characterization of a cDNA clone for the complete protein Cytomegalovirus infects human lymphocytes and monocytes: Virus coding region of the 8 subunit of the mouse acetylcholine expression is restricted to immediate-early gene products,