Managing Athlete's Foot
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Molecular Analysis of Dermatophytes Suggests Spread of Infection Among Household Members
Molecular Analysis of Dermatophytes Suggests Spread of Infection Among Household Members Mahmoud A. Ghannoum, PhD; Pranab K. Mukherjee, PhD; Erin M. Warshaw, MD; Scott Evans, PhD; Neil J. Korman, MD, PhD; Amir Tavakkol, PhD, DipBact Practice Points When a patient presents with tinea pedis or onychomycosis, inquire if other household members also have the infection, investigate if they have a history of concomitant tinea pedis and onychomycosis, and examine for plantar scaling and/or nail discoloration. If the variables above areCUTIS observed, think about spread of infection and treatment options. Dermatophyte infection from the same strains may Drs. Ghannoum, Mukherjee, and Korman are from University be an important route for transmission of derma- Hospitals Case Medical Center, Cleveland, Ohio. Dr. Warshaw is from the University of Minnesota, Minneapolis, and Minneapolis Veterans tophytoses within a household. In this study, we AffairsDo Medical Center. Dr. Evans is from Notthe Harvard School of Public used molecularCopy methods to identify dermatophytes Health, Boston, Massachusetts. Dr. Tavakkol was from Novartis in members of dermatophyte-infected households Pharmaceuticals Corporation, East Hanover, New Jersey, and and evaluated variables associated with the currently is from Topica Pharmaceuticals, Inc, Los Altos, California. spread of infection. Fungal species were identi- This article was supported by a grant from Novartis Pharmaceuticals Corporation. Dr. Ghannoum has served as a consultant and/or fied by polymerase chain reaction (PCR) using speaker for and has received grants and contracts from Merck & Co, primers targeting the internal transcribed spacer Inc; Novartis Pharmaceuticals Corporation; Pfizer Inc; and Stiefel, (ITS) regions (ITS1 and ITS4). For strain differen- a GSK company. -

Dermatophyte and Non-Dermatophyte Onychomycosis in Singapore
Australas J. Dermatol 1992; 33: 159-163 DERMATOPHYTE AND NON-DERMATOPHYTE ONYCHOMYCOSIS IN SINGAPORE JOYCE TENG-EE LIM, HOCK CHENG CHUA AND CHEE LEOK GOH Singapore SUMMARY Onychomycosis is caused by dermatophytes, moulds and yeasts. It is important to identify the non-dermatophyte moulds as they are resistant to the usual anti-fungals. A prospective study was undertaken in the National Skin Centre, Singapore to study the pattern of dermatophyte and non-dermatophyte onychomycosis. 53 male and 47 female patients seen between June 1990 and June 1991 were entered into the study. Direct microscopy was done and the nail clippings were cultured. Toe and finger nails were equally infected. Dermatophytes were isolated from 21 patients namely, T. rubrum (12/21), T. interdigitale (5/21), T. mentagrophytes (3/21) and T. violaceum (1/21). Candida onychomycosis occurred in 39 patients and was caused by C. albicans (38/39) and C. parapsilosis (1/39). 37/39 patients had associated paronychia. 5 types of moulds were isolated from 12 patients, namely Fusarium species (6/12), Aspergillus species (3/12), S. brevicaulis (1/12), Aureobasilium species (1/12) and Penicillium species (1/12). Although the clinical pattern and microscopy may predict the type of organisms, in practice this is difficult. Only cultures were confirmatory. 28% (28/100) had negative cultures despite a positive microscopy, and moulds (12/100) grown might be contaminants rather than pathogens. Key words: Moulds, yeasts, fungi, tinea, onychomycosis, dermatophyte, non-dermatophyte INTRODUCTION METHODS AND MATERIALS Onychomycosis, a common nail disorder, is 100 consecutive patients, seen in our centre caused by dermatophytes, non-dermatophyte between June 1990 and June 1991, with a new moulds, or yeasts. -

P2399 Lateral Flow Immunoassay for Rapid Detection of Dermatophytes in Clinical Specimens
P2399 Lateral flow immunoassay for rapid detection of dermatophytes in clinical specimens Amanda Burnham-Marusich*1, Caitlyn Orne1 2, Alexander Kvam3, Heather Green2, Alexandra Myers4, Aline Rodrigues Hoffmann4, Amy Crum5, Mahmoud Ghannoun6, Thomas Kozel1 3 1DxDiscovery, Reno, United States, 2University of Nevada, Reno, Reno, United States, 3University of Nevada, Reno School of Medicine, Reno, United States, 4Texas A&M University, College Station, United States, 5Houston SPCA, Houston, United States, 6Case Western Reserve University, Cleveland, United States Background: Fungal skin infections affect approximately 1 billion people each year. Most infections are treated with topical antifungal agents. Other infections, e.g., tinea capitis and onychomycosis, require use of oral antifungal agents that may produce significant side effects in some patients. Laboratory confirmation of fungal infection prior to use of antifungal agents is recommended but often not done due, in part, to the time and cost of laboratory testing. The goal of this study was to develop a lateral flow immunoassay (LFIA) for rapid diagnosis of dermatophytosis. Materials/methods: Monoclonal antibody (mAb) 2DA6 was produced from splenocytes of mice immunized with fungal cell wall fragments. Hybridomas were generated using standard methods. Results: A LFIA was constructed from mAb 2DA6 for detection of mannans of dermatophyte fungi in clinical samples. The antibody is reactive with the alpha-1,6 mannose backbone in mannans of fungi of the Zygomycota and the Ascomycota. However, mAb 2DA6 has an exquisite sensitivity for mannans of dermatophytes and the Zygomycota due to an apparent low level of side chain substitution found on these mannans vs. high levels of side chain substitution that occludes the backbone in mannans of other fungi. -
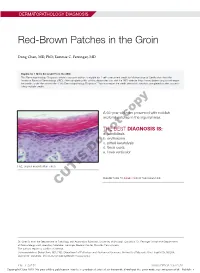
Red-Brown Patches in the Groin
DERMATOPATHOLOGY DIAGNOSIS Red-Brown Patches in the Groin Dong Chen, MD, PhD; Tammie C. Ferringer, MD Eligible for 1 MOC SA Credit From the ABD This Dermatopathology Diagnosis article in our print edition is eligible for 1 self-assessment credit for Maintenance of Certification from the American Board of Dermatology (ABD). After completing this activity, diplomates can visit the ABD website (http://www.abderm.org) to self-report the credits under the activity title “Cutis Dermatopathology Diagnosis.” You may report the credit after each activity is completed or after accumu- lating multiple credits. A 66-year-old man presented with reddish arciform patchescopy in the inguinal area. THE BEST DIAGNOSIS IS: a. candidiasis b. noterythrasma c. pitted keratolysis d. tinea cruris Doe. tinea versicolor H&E, original magnification ×600. PLEASE TURN TO PAGE 419 FOR THE DIAGNOSIS CUTIS Dr. Chen is from the Department of Pathology and Anatomical Sciences, University of Missouri, Columbia. Dr. Ferringer is from the Departments of Dermatology and Laboratory Medicine, Geisinger Medical Center, Danville, Pennsylvania. The authors report no conflict of interest. Correspondence: Dong Chen, MD, PhD, Department of Pathology and Anatomical Sciences, University of Missouri, One Hospital Dr, MA204, DC018.00, Columbia, MO 65212 ([email protected]). 416 I CUTIS® WWW.MDEDGE.COM/CUTIS Copyright Cutis 2018. No part of this publication may be reproduced, stored, or transmitted without the prior written permission of the Publisher. DERMATOPATHOLOGY DIAGNOSIS DISCUSSION THE DIAGNOSIS: Erythrasma rythrasma usually involves intertriginous areas surface (Figure 1) compared to dermatophyte hyphae that (eg, axillae, groin, inframammary area). Patients tend to be parallel to the surface.2 E present with well-demarcated, minimally scaly, red- Pitted keratolysis is a superficial bacterial infection brown patches. -

Tinea Capitis 2014 L.C
BJD GUIDELINES British Journal of Dermatology British Association of Dermatologists’ guidelines for the management of tinea capitis 2014 L.C. Fuller,1 R.C. Barton,2 M.F. Mohd Mustapa,3 L.E. Proudfoot,4 S.P. Punjabi5 and E.M. Higgins6 1Department of Dermatology, Chelsea & Westminster Hospital, Fulham Road, London SW10 9NH, U.K. 2Department of Microbiology, Leeds General Infirmary, Leeds LS1 3EX, U.K. 3British Association of Dermatologists, Willan House, 4 Fitzroy Square, London W1T 5HQ, U.K. 4St John’s Institute of Dermatology, Guy’s and St Thomas’ NHS Foundation Trust, St Thomas’ Hospital, Westminster Bridge Road, London SE1 7EH, U.K. 5Department of Dermatology, Hammersmith Hospital, 150 Du Cane Road, London W12 0HS, U.K. 6Department of Dermatology, King’s College Hospital, Denmark Hill, London SE5 9RS, U.K. 1.0 Purpose and scope Correspondence Claire Fuller. The overall objective of this guideline is to provide up-to- E-mail: [email protected] date, evidence-based recommendations for the management of tinea capitis. This document aims to update and expand Accepted for publication on the previous guidelines by (i) offering an appraisal of 8 June 2014 all relevant literature since January 1999, focusing on any key developments; (ii) addressing important, practical clini- Funding sources cal questions relating to the primary guideline objective, i.e. None. accurate diagnosis and identification of cases; suitable treat- ment to minimize duration of disease, discomfort and scar- Conflicts of interest ring; and limiting spread among other members of the L.C.F. has received sponsorship to attend conferences from Almirall, Janssen and LEO Pharma (nonspecific); has acted as a consultant for Alliance Pharma (nonspe- community; (iii) providing guideline recommendations and, cific); and has legal representation for L’Oreal U.K. -

25 Chrysosporium
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Universidade do Minho: RepositoriUM 25 Chrysosporium Dongyou Liu and R.R.M. Paterson contents 25.1 Introduction ..................................................................................................................................................................... 197 25.1.1 Classification and Morphology ............................................................................................................................ 197 25.1.2 Clinical Features .................................................................................................................................................. 198 25.1.3 Diagnosis ............................................................................................................................................................. 199 25.2 Methods ........................................................................................................................................................................... 199 25.2.1 Sample Preparation .............................................................................................................................................. 199 25.2.2 Detection Procedures ........................................................................................................................................... 199 25.3 Conclusion .......................................................................................................................................................................200 -

Detection of Histoplasma DNA from Tissue Blocks by a Specific
Journal of Fungi Article Detection of Histoplasma DNA from Tissue Blocks by a Specific and a Broad-Range Real-Time PCR: Tools to Elucidate the Epidemiology of Histoplasmosis Dunja Wilmes 1,*, Ilka McCormick-Smith 1, Charlotte Lempp 2 , Ursula Mayer 2 , Arik Bernard Schulze 3 , Dirk Theegarten 4, Sylvia Hartmann 5 and Volker Rickerts 1 1 Reference Laboratory for Cryptococcosis and Uncommon Invasive Fungal Infections, Division for Mycotic and Parasitic Agents and Mycobacteria, Robert Koch Institute, 13353 Berlin, Germany; [email protected] (I.M.-S.); [email protected] (V.R.) 2 Vet Med Labor GmbH, Division of IDEXX Laboratories, 71636 Ludwigsburg, Germany; [email protected] (C.L.); [email protected] (U.M.) 3 Department of Medicine A, Hematology, Oncology and Pulmonary Medicine, University Hospital Muenster, 48149 Muenster, Germany; [email protected] 4 Institute of Pathology, University Hospital Essen, University Duisburg-Essen, 45147 Essen, Germany; [email protected] 5 Senckenberg Institute for Pathology, Johann Wolfgang Goethe University Frankfurt, 60323 Frankfurt am Main, Germany; [email protected] * Correspondence: [email protected]; Tel.: +49-30-187-542-862 Received: 10 November 2020; Accepted: 25 November 2020; Published: 27 November 2020 Abstract: Lack of sensitive diagnostic tests impairs the understanding of the epidemiology of histoplasmosis, a disease whose burden is estimated to be largely underrated. Broad-range PCRs have been applied to identify fungal agents from pathology blocks, but sensitivity is variable. In this study, we compared the results of a specific Histoplasma qPCR (H. qPCR) with the results of a broad-range qPCR (28S qPCR) on formalin-fixed, paraffin-embedded (FFPE) tissue specimens from patients with proven fungal infections (n = 67), histologically suggestive of histoplasmosis (n = 36) and other mycoses (n = 31). -

Common Tinea Infections in Children Mark D
Common Tinea Infections in Children MARK D. ANDREWS, MD, and MARIANTHE BURNS, MD Wake Forest University School of Medicine, Winston-Salem, North Carolina The common dermatophyte genera Trichophyton, Microsporum, and Epidermophyton are major causes of superficial fungal infections in children. These infections (e.g., tinea corporis, pedis, cruris, and unguium) are typically acquired directly from contact with infected humans or animals or indirectly from exposure to contaminated soil or fomi- tes. A diagnosis usually can be made with a focused history, physical examination, and potassium hydroxide micros- copy. Occasionally, Wood’s lamp examination, fungal culture, or histologic tissue examination is required. Most tinea infections can be managed with topical therapies; oral treatment is reserved for tinea capitis, severe tinea pedis, and tinea unguium. Topical therapy with fungicidal allylamines may have slightly higher cure rates and shorter treatment courses than with fungistatic azoles. Although oral griseofulvin has been the standard treatment for tinea capitis, newer oral antifungal agents such as terbinafine, itraconazole, and fluconazole are effective, safe, and have shorter treatment courses. (Am Fam Physician. 2008;77(10):1415-1420. Copyright © 2008 American Academy of Family Physicians.) inea refers to dermatophyte infec- tinea infections.1,2,4,5 This technique directly tions, which are generally classified shows hyphae and confirms infection. The by anatomic location: tinea capitis specimen is examined under the microscope is located on the scalp, tinea pedis after a drop of 10 to 20 percent KOH solu- T on the feet, tinea corporis on the body, tinea tion is added to the scraping from the active cruris on the groin, and tinea unguium on border of the lesion. -

Therapies for Common Cutaneous Fungal Infections
MedicineToday 2014; 15(6): 35-47 PEER REVIEWED FEATURE 2 CPD POINTS Therapies for common cutaneous fungal infections KENG-EE THAI MB BS(Hons), BMedSci(Hons), FACD Key points A practical approach to the diagnosis and treatment of common fungal • Fungal infection should infections of the skin and hair is provided. Topical antifungal therapies always be in the differential are effective and usually used as first-line therapy, with oral antifungals diagnosis of any scaly rash. being saved for recalcitrant infections. Treatment should be for several • Topical antifungal agents are typically adequate treatment weeks at least. for simple tinea. • Oral antifungal therapy may inea and yeast infections are among the dermatophytoses (tinea) and yeast infections be required for extensive most common diagnoses found in general and their differential diagnoses and treatments disease, fungal folliculitis and practice and dermatology. Although are then discussed (Table). tinea involving the face, hair- antifungal therapies are effective in these bearing areas, palms and T infections, an accurate diagnosis is required to ANTIFUNGAL THERAPIES soles. avoid misuse of these or other topical agents. Topical antifungal preparations are the most • Tinea should be suspected if Furthermore, subsequent active prevention is commonly prescribed agents for dermatomy- there is unilateral hand just as important as the initial treatment of the coses, with systemic agents being used for dermatitis and rash on both fungal infection. complex, widespread tinea or when topical agents feet – ‘one hand and two feet’ This article provides a practical approach fail for tinea or yeast infections. The pharmacol- involvement. to antifungal therapy for common fungal infec- ogy of the systemic agents is discussed first here. -

Application to Add Itraconazole and Voriconazole to the Essential List of Medicines for Treatment of Fungal Diseases – Support Document
Application to add itraconazole and voriconazole to the essential list of medicines for treatment of fungal diseases – Support document 1 | Page Contents Page number Summary 3 Centre details supporting the application 3 Information supporting the public health relevance and review of 4 benefits References 7 2 | Page 1. Summary statement of the proposal for inclusion, change or deletion As a growing trend of invasive fungal infections has been noticed worldwide, available few antifungal drugs requires to be used optimally. Invasive aspergillosis, systemic candidiasis, chronic pulmonary aspergillosis, fungal rhinosinusitis, allergic bronchopulmonary aspergillosis, phaeohyphomycosis, histoplasmosis, sporotrichosis, chromoblastomycosis, and relapsed cases of dermatophytosis are few important concern of southeast Asian regional area. Considering the high burden of fungal diseases in Asian countries and its associated high morbidity and mortality (often exceeding 50%), we support the application of including major antifungal drugs against filamentous fungi, itraconazole and voriconazole in the list of WHO Essential Medicines (both available in oral formulation). The inclusion of these oral effective antifungal drugs in the essential list of medicines (EML) would help in increased availability of these agents in this part of the world and better prompt management of patients thereby reducing mortality. The widespread availability of these drugs would also stimulate more research to facilitate the development of better combination therapies. -

Failure of Treatment in Chronic Dermatophyte Infections R
Postgraduate Medical Journal (September 1979) 55, 608-610 Failure of treatment in chronic dermatophyte infections R. J. HAY M.R.C.P. Department ofMicrobiology, London School of Hygiene and Tropical Medicine, London WC1E 7HT Summary (Roth, Sallman and Blank, 1959). It seems, there- A proportion of dermatophyte infections fail to fore, that the effectiveness of griseofulvin is depen- respond to normally adequate courses of griseofulvin dent on host factors such as the immune response and tropical antifungal therapy. The organism Tricho- and a normal turnover of epidermis which tends to phyton rubrum was isolated from 96°o of 50 patients shed the organism into the environment. studied, but no instances of in vitro resistance were Griseofulvin remains a useful drug, surprisingly seen. Of these patients, 57%o had an underlying free of side effects in the doses normally used condition, commonly hay fever/asthma, atopic eczema, (Livingood et al., 1960). Gastric intolerance, head- collagen disease or ichthyosis. Defective delayed type aches, urticaria and rashes, and leucopenia have hypersensitivity responses and leucocyte migration been described. inhibition to the specific antigen, trichophytin, were The patients described here had chronic dermato- demonstrated. Immediate type hypersensitivity was phyte infections, often of many years' standing. The seen in 58% and this was partially suppressible with clinical presentation was remarkably constant and chlorpheniramine and cimetidine. The relationship the very rare variants, dermatophyte mycetoma -

Yeast Infection Division of Disease Control What Do I Need to Know?
Division of Disease Control What Do I Need To Know? Yeast Infection (Thrush, Diaper Rash, Vaginitis) What is a yeast infection? Yeast infections are caused by a fungus called Candida albicans. These infections can present in a variety of forms. Yeast infections in women can infect the vagina, called vaginitis. Thrush causes mouth infections in young infants and can also be a presenting sign of HIV infection in adults. Candida also may be the cause of many types of diaper rash in young children. Who is at risk for a yeast infection? Anyone can get a yeast infection. What are the symptoms of a yeast infection? Candidia diaper rash: The diaper area is red. The redness is worse in the creases. Redness is often bordered by red pimples. Rash may have a shiny appearance. Sores or cracking or oozing is present in severe cases. Thrush White patches appear on the inside of cheeks and gums and tongue. Thrush usually causes no other signs or symptoms. Vaginitis Vaginal irritation, intense itchiness and vaginal discharge. How soon do symptoms appear? Incubation period is unknown. How is a yeast infection spread? The fungus is present in the intestinal tract and mucous membranes of healthy people. A warm environment allows for growth and spread. Page 1 of 2 Last Updated: 01/2016 Person-to-person transmission may occur from a woman to her infant when the mother has a yeast infection in her vagina and in breastfeeding mothers whose babies with thrush infect the mothers’ nipples. When and for how long is a person able to spread the disease? A person can spread disease as long as the infection is present.