FLNC and MYLK2 Gene Mutations in a Chinese Family with Different Phenotypes
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Supplemental Information to Mammadova-Bach Et Al., “Laminin Α1 Orchestrates VEGFA Functions in the Ecosystem of Colorectal Carcinogenesis”
Supplemental information to Mammadova-Bach et al., “Laminin α1 orchestrates VEGFA functions in the ecosystem of colorectal carcinogenesis” Supplemental material and methods Cloning of the villin-LMα1 vector The plasmid pBS-villin-promoter containing the 3.5 Kb of the murine villin promoter, the first non coding exon, 5.5 kb of the first intron and 15 nucleotides of the second villin exon, was generated by S. Robine (Institut Curie, Paris, France). The EcoRI site in the multi cloning site was destroyed by fill in ligation with T4 polymerase according to the manufacturer`s instructions (New England Biolabs, Ozyme, Saint Quentin en Yvelines, France). Site directed mutagenesis (GeneEditor in vitro Site-Directed Mutagenesis system, Promega, Charbonnières-les-Bains, France) was then used to introduce a BsiWI site before the start codon of the villin coding sequence using the 5’ phosphorylated primer: 5’CCTTCTCCTCTAGGCTCGCGTACGATGACGTCGGACTTGCGG3’. A double strand annealed oligonucleotide, 5’GGCCGGACGCGTGAATTCGTCGACGC3’ and 5’GGCCGCGTCGACGAATTCACGC GTCC3’ containing restriction site for MluI, EcoRI and SalI were inserted in the NotI site (present in the multi cloning site), generating the plasmid pBS-villin-promoter-MES. The SV40 polyA region of the pEGFP plasmid (Clontech, Ozyme, Saint Quentin Yvelines, France) was amplified by PCR using primers 5’GGCGCCTCTAGATCATAATCAGCCATA3’ and 5’GGCGCCCTTAAGATACATTGATGAGTT3’ before subcloning into the pGEMTeasy vector (Promega, Charbonnières-les-Bains, France). After EcoRI digestion, the SV40 polyA fragment was purified with the NucleoSpin Extract II kit (Machery-Nagel, Hoerdt, France) and then subcloned into the EcoRI site of the plasmid pBS-villin-promoter-MES. Site directed mutagenesis was used to introduce a BsiWI site (5’ phosphorylated AGCGCAGGGAGCGGCGGCCGTACGATGCGCGGCAGCGGCACG3’) before the initiation codon and a MluI site (5’ phosphorylated 1 CCCGGGCCTGAGCCCTAAACGCGTGCCAGCCTCTGCCCTTGG3’) after the stop codon in the full length cDNA coding for the mouse LMα1 in the pCIS vector (kindly provided by P. -

FLNC Pathogenic Variants in Patients with Cardiomyopathies
FLNC pathogenic variants in patients with cardiomyopathies: Prevalence and genotype-phenotype correlations Flavie Ader, Pascal de Groote, Patricia Réant, Caroline Rooryck-Thambo, Delphine Dupin-Deguine, Caroline Rambaud, Diala Khraiche, Claire Perret, Jean-François Pruny, Michèle Mathieu-dramard, et al. To cite this version: Flavie Ader, Pascal de Groote, Patricia Réant, Caroline Rooryck-Thambo, Delphine Dupin-Deguine, et al.. FLNC pathogenic variants in patients with cardiomyopathies: Prevalence and genotype-phenotype correlations. Clinical Genetics, Wiley, 2019, 96 (4), pp.317-329. 10.1111/cge.13594. hal-02268422 HAL Id: hal-02268422 https://hal-normandie-univ.archives-ouvertes.fr/hal-02268422 Submitted on 29 Jun 2020 HAL is a multi-disciplinary open access L’archive ouverte pluridisciplinaire HAL, est archive for the deposit and dissemination of sci- destinée au dépôt et à la diffusion de documents entific research documents, whether they are pub- scientifiques de niveau recherche, publiés ou non, lished or not. The documents may come from émanant des établissements d’enseignement et de teaching and research institutions in France or recherche français ou étrangers, des laboratoires abroad, or from public or private research centers. publics ou privés. FLNC pathogenic variants in patients with cardiomyopathies Prevalence and genotype-phenotype correlations Running Title : FLNC variants genotype-phenotype correlation Flavie Ader1,2,3, Pascal De Groote4, Patricia Réant5, Caroline Rooryck-Thambo6, Delphine Dupin-Deguine7, Caroline Rambaud8, Diala Khraiche9, Claire Perret2, Jean Francois Pruny10, Michèle Mathieu Dramard11, Marion Gérard12, Yann Troadec12, Laurent Gouya13, Xavier Jeunemaitre14, Lionel Van Maldergem15, Albert Hagège16, Eric Villard2, Philippe Charron2, 10, Pascale Richard1, 2, 10. Conflict of interest statement: none declared for each author 1. -

Genetic Mutations and Mechanisms in Dilated Cardiomyopathy
Genetic mutations and mechanisms in dilated cardiomyopathy Elizabeth M. McNally, … , Jessica R. Golbus, Megan J. Puckelwartz J Clin Invest. 2013;123(1):19-26. https://doi.org/10.1172/JCI62862. Review Series Genetic mutations account for a significant percentage of cardiomyopathies, which are a leading cause of congestive heart failure. In hypertrophic cardiomyopathy (HCM), cardiac output is limited by the thickened myocardium through impaired filling and outflow. Mutations in the genes encoding the thick filament components myosin heavy chain and myosin binding protein C (MYH7 and MYBPC3) together explain 75% of inherited HCMs, leading to the observation that HCM is a disease of the sarcomere. Many mutations are “private” or rare variants, often unique to families. In contrast, dilated cardiomyopathy (DCM) is far more genetically heterogeneous, with mutations in genes encoding cytoskeletal, nucleoskeletal, mitochondrial, and calcium-handling proteins. DCM is characterized by enlarged ventricular dimensions and impaired systolic and diastolic function. Private mutations account for most DCMs, with few hotspots or recurring mutations. More than 50 single genes are linked to inherited DCM, including many genes that also link to HCM. Relatively few clinical clues guide the diagnosis of inherited DCM, but emerging evidence supports the use of genetic testing to identify those patients at risk for faster disease progression, congestive heart failure, and arrhythmia. Find the latest version: https://jci.me/62862/pdf Review series Genetic mutations and mechanisms in dilated cardiomyopathy Elizabeth M. McNally, Jessica R. Golbus, and Megan J. Puckelwartz Department of Human Genetics, University of Chicago, Chicago, Illinois, USA. Genetic mutations account for a significant percentage of cardiomyopathies, which are a leading cause of conges- tive heart failure. -

A Mutation Update for the FLNC Gene in Myopathies and Cardiomyopathies
Received: 20 December 2019 | Revised: 12 February 2020 | Accepted: 25 February 2020 DOI: 10.1002/humu.24004 MUTATION UPDATE A mutation update for the FLNC gene in myopathies and cardiomyopathies Job A. J. Verdonschot1,2 | Els K. Vanhoutte1 | Godelieve R. F. Claes1 | Apollonia T. J. M. Helderman‐van den Enden1 | Janneke G. J. Hoeijmakers3 | Debby M. E. I. Hellebrekers1 | Amber de Haan1 | Imke Christiaans4,5 | Ronald H. Lekanne Deprez4 | Hanne M. Boen6 | Emeline M. van Craenenbroeck6 | Bart L. Loeys7 | Yvonne M. Hoedemaekers5,8 | Carlo Marcelis8 | Marlies Kempers8 | Esther Brusse9 | Jaap I. van Waning10,11 | Annette F. Baas12 | Dennis Dooijes12 | Folkert W. Asselbergs13 | Daniela Q. C. M. Barge‐Schaapveld14 | Pieter Koopman15 | Arthur van den Wijngaard1 | Stephane R. B. Heymans2,16,17 | Ingrid P. C. Krapels1 | Han G. Brunner1,8,18 1Department of Clinical Genetics, Maastricht University Medical Center, Maastricht, The Netherlands 2Department of Cardiology, Cardiovascular Research Institute (CARIM), Maastricht University Medical Center, Maastricht, The Netherlands 3Department of Neurology, Maastricht University Medical Center, Maastricht, The Netherlands 4Department of Clinical Genetics, Amsterdam University Medical Center, Amsterdam, The Netherlands 5Department of Clinical Genetics, University Medical Centre Groningen, Groningen, The Netherlands 6Department of Cardiology, Antwerp University Hospital, University of Antwerp, Antwerp, Belgium 7Department of Medical Genetics, Antwerp University Hospital, University of Antwerp, Antwerp, Belgium -

Proteins That Mediate Protein Aggregation and Cytotoxicity Distinguish Alzheimer'S Hippocampus from Normal Controls
Aging Cell (2016) pp1–16 Doi: 10.1111/acel.12501 Proteins that mediate protein aggregation and cytotoxicity distinguish Alzheimer’s hippocampus from normal controls Srinivas Ayyadevara,1,2 Meenakshisundaram types of aggregation, and/or aggregate-mediated cross-talk Balasubramaniam,2,3 Paul A. Parcon,2 Steven W. Barger,1,2 between tau and Ab. Knowledge of protein components that W. Sue T. Griffin,1,2 Ramani Alla,1,2 Alan J. Tackett,4 promote protein accrual in diverse aggregate types implicates Samuel G. Mackintosh,4 Emanuel Petricoin,5 Weidong Zhou5 common mechanisms and identifies novel targets for drug and Robert J. Shmookler Reis1,2,4 intervention. Key words: Abeta(1-42); acetylation (protein); aggregation 1McClellan Veterans Medical Center, Central Arkansas Veterans Healthcare Service, Little Rock, AR 72205, USA (protein); Alzheimer (Disease); beta amyloid; C. elegans; 2Department of Geriatrics, University of Arkansas for Medical Sciences, Little microtubule-associated protein tau; neurodegeneration; Rock, AR 72205, USA neurotoxicity; oxidation (protein); phosphorylation (protein); 3BioInformatics Program, University of Arkansas for Medical Sciences and University of Arkansas at Little Rock, Little Rock, AR 72205, USA proteomics. 4Department of Biochemistry & Molecular Biology, University of Arkansas for Medical Sciences, Little Rock, AR 72205, USA 5 Center for Applied Proteomics and Molecular Medicine, George Mason Introduction University, Manassas, VA 20110, USA Summary Protein aggregation has long been recognized as a common feature of most or all age-dependent neurodegenerative diseases, and yet very little Neurodegenerative diseases are distinguished by characteristic is known about which features of aggregating proteins contribute to protein aggregates initiated by disease-specific ‘seed’ proteins; their accrual or their neurotoxicity. -
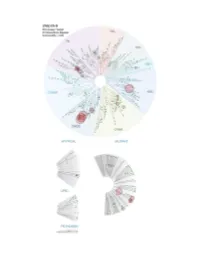
Profiling Data
Compound Name DiscoveRx Gene Symbol Entrez Gene Percent Compound Symbol Control Concentration (nM) JNK-IN-8 AAK1 AAK1 69 1000 JNK-IN-8 ABL1(E255K)-phosphorylated ABL1 100 1000 JNK-IN-8 ABL1(F317I)-nonphosphorylated ABL1 87 1000 JNK-IN-8 ABL1(F317I)-phosphorylated ABL1 100 1000 JNK-IN-8 ABL1(F317L)-nonphosphorylated ABL1 65 1000 JNK-IN-8 ABL1(F317L)-phosphorylated ABL1 61 1000 JNK-IN-8 ABL1(H396P)-nonphosphorylated ABL1 42 1000 JNK-IN-8 ABL1(H396P)-phosphorylated ABL1 60 1000 JNK-IN-8 ABL1(M351T)-phosphorylated ABL1 81 1000 JNK-IN-8 ABL1(Q252H)-nonphosphorylated ABL1 100 1000 JNK-IN-8 ABL1(Q252H)-phosphorylated ABL1 56 1000 JNK-IN-8 ABL1(T315I)-nonphosphorylated ABL1 100 1000 JNK-IN-8 ABL1(T315I)-phosphorylated ABL1 92 1000 JNK-IN-8 ABL1(Y253F)-phosphorylated ABL1 71 1000 JNK-IN-8 ABL1-nonphosphorylated ABL1 97 1000 JNK-IN-8 ABL1-phosphorylated ABL1 100 1000 JNK-IN-8 ABL2 ABL2 97 1000 JNK-IN-8 ACVR1 ACVR1 100 1000 JNK-IN-8 ACVR1B ACVR1B 88 1000 JNK-IN-8 ACVR2A ACVR2A 100 1000 JNK-IN-8 ACVR2B ACVR2B 100 1000 JNK-IN-8 ACVRL1 ACVRL1 96 1000 JNK-IN-8 ADCK3 CABC1 100 1000 JNK-IN-8 ADCK4 ADCK4 93 1000 JNK-IN-8 AKT1 AKT1 100 1000 JNK-IN-8 AKT2 AKT2 100 1000 JNK-IN-8 AKT3 AKT3 100 1000 JNK-IN-8 ALK ALK 85 1000 JNK-IN-8 AMPK-alpha1 PRKAA1 100 1000 JNK-IN-8 AMPK-alpha2 PRKAA2 84 1000 JNK-IN-8 ANKK1 ANKK1 75 1000 JNK-IN-8 ARK5 NUAK1 100 1000 JNK-IN-8 ASK1 MAP3K5 100 1000 JNK-IN-8 ASK2 MAP3K6 93 1000 JNK-IN-8 AURKA AURKA 100 1000 JNK-IN-8 AURKA AURKA 84 1000 JNK-IN-8 AURKB AURKB 83 1000 JNK-IN-8 AURKB AURKB 96 1000 JNK-IN-8 AURKC AURKC 95 1000 JNK-IN-8 -

Metformin Rescues Muscle Function in BAG3 Myofibrillar Myopathy Models
bioRxiv preprint doi: https://doi.org/10.1101/574806; this version posted March 12, 2019. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY-NC-ND 4.0 International license. Metformin rescues muscle function in BAG3 myofibrillar myopathy models Avnika A. Ruparelia1, Emily A. McKaige1, Caitlin Williams1, Keith E. Schulze2, Margit Fuchs3,4, Viola Oorschot5, Emmanuelle Lacene6, Meregalli Mirella7, Emily C. Baxter1, Yvan Torrente7, Georg Ramm5,8, Tanya Stojkovic9, Josée N. Lavoie3,4,10, and Robert J. Bryson-Richardson1* 1 School of Biological Sciences, Monash University, Melbourne 3800, Australia 2 Monash Micro Imaging, Monash University, Melbourne 3800, Australia 3 Centre de Recherche sur le Cancer de l'Université Laval, Ville de Québec, Quebec, Canada. 4 Oncologie, Centre de Recherche du Centre Hospitalier Universitaire (CHU) de Québec-Université Laval, Ville de Québec, Quebec, Canada. 5 Monash Ramaciotti Centre for Structural Cryo-Electron Microscopy, Monash University, Melbourne 3800, Australia 6 APHP, Centre de Référence de Pathologie Neuromusculaire Nord/Est/Ile-de-France, Institut de Myologie, Laboratoire de Pathologie Risler, GH Pitié-Salpêtrière, Paris, France. 7 Stem Cell Laboratory, Department of Pathophysiology and Transplantation, Università degli Studi di Milano, Fondazione IRCCS Ca’ Granda Ospedale Maggiore Policlinico di Milano, Centro Dino Ferrari, via F Sforza, 35, 20122 Milan, Italy 8 Biochemistry and Molecular Biology, Monash Biomedicine Discovery Institute, Monash University, Melbourne, Victoria, Australia. 9 Centre de référence des maladies neuromusculaires, Hôpital Pitié-Salpétrière, Assistance-Publique Hôpitaux de Paris, Paris, France. -

Novel Pathogenic Variants in Filamin C Identified in Pediatric Restrictive Cardiomyopathy
Novel pathogenic variants in filamin C identified in pediatric restrictive cardiomyopathy Jeffrey Schubert1, 2, Muhammad Tariq3, Gabrielle Geddes4, Steven Kindel4, Erin M. Miller5, and Stephanie M. Ware2. 1 Department of Molecular Genetics, Microbiology, and Biochemistry, University of Cincinnati College of Medicine, Cincinnati, OH; 2 Departments of Pediatrics and Medical and Molecular Genetics, Indiana University School of Medicine, Indianapolis, IN; 3 Faculty of Applied Medical Science, University of Tabuk, Tabuk, Kingdom of Saudi Arabia; 4Department of Pediatrics, Medical College of Wisconsin, Milwaukee, WI; 5Cincinnati Children’s Hospital Medical Center, Cincinnati, OH. Correspondence: Stephanie M. Ware, MD, PhD Department of Pediatrics Indiana University School of Medicine 1044 W. Walnut Street Indianapolis, IN 46202 Telephone: 317 274-8939 Email: [email protected] Grant Sponsor: The project was supported by the Children’s Cardiomyopathy Foundation (S.M.W.), an American Heart Association Established Investigator Award 13EIA13460001 (S.M.W.) and an AHA Postdoctoral Fellowship Award 12POST10370002 (M.T.). ___________________________________________________________________ This is the author's manuscript of the article published in final edited form as: Schubert, J., Tariq, M., Geddes, G., Kindel, S., Miller, E. M., & Ware, S. M. (2018). Novel pathogenic variants in filamin C identified in pediatric restrictive cardiomyopathy. Human Mutation, 0(ja). https://doi.org/10.1002/humu.23661 Abstract Restrictive cardiomyopathy (RCM) is a rare and distinct form of cardiomyopathy characterized by normal ventricular chamber dimensions, normal myocardial wall thickness, and preserved systolic function. The abnormal myocardium, however, demonstrates impaired relaxation. To date, dominant variants causing RCM have been reported in a small number of sarcomeric or cytoskeletal genes, but the genetic causes in a majority of cases remain unexplained especially in early childhood. -

Supplementary Table 1
SI Table S1. Broad protein kinase selectivity for PF-2771. Kinase, PF-2771 % Inhibition at 10 μM Service Kinase, PF-2771 % Inhibition at 1 μM Service rat RPS6KA1 (RSK1) 39 Dundee AURKA (AURA) 24 Invitrogen IKBKB (IKKb) 26 Dundee CDK2 /CyclinA 21 Invitrogen mouse LCK 25 Dundee rabbit MAP2K1 (MEK1) 19 Dundee AKT1 (AKT) 21 Dundee IKBKB (IKKb) 16 Dundee CAMK1 (CaMK1a) 19 Dundee PKN2 (PRK2) 14 Dundee RPS6KA5 (MSK1) 18 Dundee MAPKAPK5 14 Dundee PRKD1 (PKD1) 13 Dundee PIM3 12 Dundee MKNK2 (MNK2) 12 Dundee PRKD1 (PKD1) 12 Dundee MARK3 10 Dundee NTRK1 (TRKA) 12 Invitrogen SRPK1 9 Dundee MAPK12 (p38g) 11 Dundee MAPKAPK5 9 Dundee MAPK8 (JNK1a) 11 Dundee MAPK13 (p38d) 8 Dundee rat PRKAA2 (AMPKa2) 11 Dundee AURKB (AURB) 5 Dundee NEK2 11 Invitrogen CSK 5 Dundee CHEK2 (CHK2) 11 Invitrogen EEF2K (EEF-2 kinase) 4 Dundee MAPK9 (JNK2) 9 Dundee PRKCA (PKCa) 4 Dundee rat RPS6KA1 (RSK1) 8 Dundee rat PRKAA2 (AMPKa2) 4 Dundee DYRK2 7 Dundee rat CSNK1D (CKId) 3 Dundee AKT1 (AKT) 7 Dundee LYN 3 BioPrint PIM2 7 Invitrogen CSNK2A1 (CKIIa) 3 Dundee MAPK15 (ERK7) 6 Dundee CAMKK2 (CAMKKB) 1 Dundee mouse LCK 5 Dundee PIM3 1 Dundee PDPK1 (PDK1) (directed 5 Invitrogen rat DYRK1A (MNB) 1 Dundee RPS6KB1 (p70S6K) 5 Dundee PBK 0 Dundee CSNK2A1 (CKIIa) 4 Dundee PIM1 -1 Dundee CAMKK2 (CAMKKB) 4 Dundee DYRK2 -2 Dundee SRC 4 Invitrogen MAPK12 (p38g) -2 Dundee MYLK2 (MLCK_sk) 3 Invitrogen NEK6 -3 Dundee MKNK2 (MNK2) 2 Dundee RPS6KB1 (p70S6K) -3 Dundee SRPK1 2 Dundee AKT2 -3 Dundee MKNK1 (MNK1) 2 Dundee RPS6KA3 (RSK2) -3 Dundee CHEK1 (CHK1) 2 Invitrogen rabbit MAP2K1 (MEK1) -4 Dundee -

Dilated Cardiomyopathy Caused by Truncating Titin Variants
BMJ Publishing Group Limited (BMJ) disclaims all liability and responsibility arising from any reliance Supplemental material placed on this supplemental material which has been supplied by the author(s) J Med Genet Dilated cardiomyopathy caused by truncating titin variants – Long-term outcomes, arrhythmias, response to treatment and sex differences SUPPLEMENTARY MATERIAL Christoffer Rasmus Vissing1*, MD; Torsten Bloch Rasmussen2, MD, PhD; Anne Mette Dybro2, MD; Morten Salling Olesen3,4, MSc, PhD; Lisbeth Nørum Pedersen5; MSc, PhD; Morten Jensen, MD, PhD2; Henning Bundgaard1, MD, DMSc; Alex Hørby Christensen1,6 MD, PhD 1The Capital Region’s Unit for Inherited Cardiac Diseases, Department of Cardiology, Rigshospitalet, Copenhagen University Hospital, Copenhagen, Denmark 2Department of Cardiology, Aarhus University Hospital, Aarhus, Denmark 3Laboratory for Molecular Cardiology, University of Copenhagen, Copenhagen, Denmark 4Department of Biomedical Sciences, University of Copenhagen, Copenhagen, 2200 N, Denmark 5Department of Molecular Medicine, Aarhus University Hospital, Denmark. 6Department of Cardiology, Herlev-Gentofte Hospital, Copenhagen University Hospital, Copenhagen, Denmark *Corresponding author: Christoffer Rasmus Vissing, MD The Capital Region’s Unit for Inherited Cardiac Diseases, Department of Cardiology, The Heart Center, Rigshospitalet, Copenhagen University Hospital, Blegdamsvej 9, DK-2100 Copenhagen, Denmark, E-mail: [email protected]; Phone +45 3545 5045 1 Vissing CR, et al. J Med Genet 2020;0:1–10. -

Illuminating the Divergent Role of Filamin C Mutations in Human Cardiomyopathy
Journal of Clinical Medicine Review Cardiac Filaminopathies: Illuminating the Divergent Role of Filamin C Mutations in Human Cardiomyopathy Matthias Eden 1,2 and Norbert Frey 1,2,* 1 Department of Internal Medicine III, University of Heidelberg, 69120 Heidelberg, Germany; [email protected] 2 German Centre for Cardiovascular Research, Partner Site Heidelberg, 69120 Heidelberg, Germany * Correspondence: [email protected] Abstract: Over the past decades, there has been tremendous progress in understanding genetic alterations that can result in different phenotypes of human cardiomyopathies. More than a thousand mutations in various genes have been identified, indicating that distinct genetic alterations, or combi- nations of genetic alterations, can cause either hypertrophic (HCM), dilated (DCM), restrictive (RCM), or arrhythmogenic cardiomyopathies (ARVC). Translation of these results from “bench to bedside” can potentially group affected patients according to their molecular etiology and identify subclinical individuals at high risk for developing cardiomyopathy or patients with overt phenotypes at high risk for cardiac deterioration or sudden cardiac death. These advances provide not only mechanistic insights into the earliest manifestations of cardiomyopathy, but such efforts also hold the promise that mutation-specific pathophysiology might result in novel “personalized” therapeutic possibilities. Recently, the FLNC gene encoding the sarcomeric protein filamin C has gained special interest since FLNC mutations were found in several distinct and possibly overlapping cardiomyopathy phenotypes. Specifically, mutations in FLNC were initially only linked to myofibrillar myopathy (MFM), but are now increasingly found in various forms of human cardiomyopathy. FLNC thereby Citation: Eden, M.; Frey, N. Cardiac represents another example for the complex genetic and phenotypic continuum of these diseases. -

A Master Autoantigen-Ome Links Alternative Splicing, Female Predilection, and COVID-19 to Autoimmune Diseases
bioRxiv preprint doi: https://doi.org/10.1101/2021.07.30.454526; this version posted August 4, 2021. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY 4.0 International license. A Master Autoantigen-ome Links Alternative Splicing, Female Predilection, and COVID-19 to Autoimmune Diseases Julia Y. Wang1*, Michael W. Roehrl1, Victor B. Roehrl1, and Michael H. Roehrl2* 1 Curandis, New York, USA 2 Department of Pathology, Memorial Sloan Kettering Cancer Center, New York, USA * Correspondence: [email protected] or [email protected] 1 bioRxiv preprint doi: https://doi.org/10.1101/2021.07.30.454526; this version posted August 4, 2021. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY 4.0 International license. Abstract Chronic and debilitating autoimmune sequelae pose a grave concern for the post-COVID-19 pandemic era. Based on our discovery that the glycosaminoglycan dermatan sulfate (DS) displays peculiar affinity to apoptotic cells and autoantigens (autoAgs) and that DS-autoAg complexes cooperatively stimulate autoreactive B1 cell responses, we compiled a database of 751 candidate autoAgs from six human cell types. At least 657 of these have been found to be affected by SARS-CoV-2 infection based on currently available multi-omic COVID data, and at least 400 are confirmed targets of autoantibodies in a wide array of autoimmune diseases and cancer.