Candida Onychomycosis: Indian Scenario
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Fungal Infections from Human and Animal Contact
Journal of Patient-Centered Research and Reviews Volume 4 Issue 2 Article 4 4-25-2017 Fungal Infections From Human and Animal Contact Dennis J. Baumgardner Follow this and additional works at: https://aurora.org/jpcrr Part of the Bacterial Infections and Mycoses Commons, Infectious Disease Commons, and the Skin and Connective Tissue Diseases Commons Recommended Citation Baumgardner DJ. Fungal infections from human and animal contact. J Patient Cent Res Rev. 2017;4:78-89. doi: 10.17294/2330-0698.1418 Published quarterly by Midwest-based health system Advocate Aurora Health and indexed in PubMed Central, the Journal of Patient-Centered Research and Reviews (JPCRR) is an open access, peer-reviewed medical journal focused on disseminating scholarly works devoted to improving patient-centered care practices, health outcomes, and the patient experience. REVIEW Fungal Infections From Human and Animal Contact Dennis J. Baumgardner, MD Aurora University of Wisconsin Medical Group, Aurora Health Care, Milwaukee, WI; Department of Family Medicine and Community Health, University of Wisconsin School of Medicine and Public Health, Madison, WI; Center for Urban Population Health, Milwaukee, WI Abstract Fungal infections in humans resulting from human or animal contact are relatively uncommon, but they include a significant proportion of dermatophyte infections. Some of the most commonly encountered diseases of the integument are dermatomycoses. Human or animal contact may be the source of all types of tinea infections, occasional candidal infections, and some other types of superficial or deep fungal infections. This narrative review focuses on the epidemiology, clinical features, diagnosis and treatment of anthropophilic dermatophyte infections primarily found in North America. -

Onychomycosis/ (Suspected) Fungal Nail and Skin Protocol
Onychomycosis/ (suspected) Fungal Nail and Skin Protocol Please check the boxes of the evaluation questions, actions and dispensing items you wish to include in your customized protocol. If additional or alternative products or services are provided, please include when making your selections. If you wish to include the condition description please also check the box. Description of Condition: Onychomycosis is a common nail condition. It is a fungal infection of the nail that differs from bacterial infections (often referred to as paronychia infections). It is very common for a patient to present with onychomycosis without a true paronychia infection. It is also very common for a patient with a paronychia infection to have secondary onychomycosis. Factors that can cause onychomycosis include: (1) environment: dark, closed, and damp like the conventional shoe, (2) trauma: blunt or repetitive, (3) heredity, (4) compromised immune system, (5) carbohydrate-rich diet, (6) vitamin deficiency or thyroid issues, (7) poor circulation or PVD, (8) poor-fitting shoe gear, (9) pedicures received in places with unsanitary conditions. Nails that are acute or in the early stages of infection may simply have some white spots or a white linear line. Chronic nail conditions may appear thickened, discolored, brittle or hardened (to the point that the patient is unable to trim the nails on their own). The nails may be painful to touch or with closed shoe gear or the nail condition may be purely cosmetic and not painful at all. *Ask patient to remove nail -

Managing Athlete's Foot
South African Family Practice 2018; 60(5):37-41 S Afr Fam Pract Open Access article distributed under the terms of the ISSN 2078-6190 EISSN 2078-6204 Creative Commons License [CC BY-NC-ND 4.0] © 2018 The Author(s) http://creativecommons.org/licenses/by-nc-nd/4.0 REVIEW Managing athlete’s foot Nkatoko Freddy Makola,1 Nicholus Malesela Magongwa,1 Boikgantsho Matsaung,1 Gustav Schellack,2 Natalie Schellack3 1 Academic interns, School of Pharmacy, Sefako Makgatho Health Sciences University 2 Clinical research professional, pharmaceutical industry 3 Professor, School of Pharmacy, Sefako Makgatho Health Sciences University *Corresponding author, email: [email protected] Abstract This article is aimed at providing a succinct overview of the condition tinea pedis, commonly referred to as athlete’s foot. Tinea pedis is a very common fungal infection that affects a significantly large number of people globally. The presentation of tinea pedis can vary based on the different clinical forms of the condition. The symptoms of tinea pedis may range from asymptomatic, to mild- to-severe forms of pain, itchiness, difficulty walking and other debilitating symptoms. There is a range of precautionary measures available to prevent infection, and both oral and topical drugs can be used for treating tinea pedis. This article briefly highlights what athlete’s foot is, the different causes and how they present, the prevalence of the condition, the variety of diagnostic methods available, and the pharmacological and non-pharmacological management of the -

Candida Parapsilosis: a Review of Its Epidemiology, Pathogenesis, Clinical Aspects, Typing and Antimicrobial Susceptibility
Critical Reviews in Microbiology Critical Reviews in Microbiology, 2009; 35(4): 283–309 2009 REVIEW ARTICLE Candida parapsilosis: a review of its epidemiology, pathogenesis, clinical aspects, typing and antimicrobial susceptibility Eveline C. van Asbeck1,2, Karl V. Clemons1, David A. Stevens1 1Division of Infectious Diseases, Santa Clara Valley Medical Center, and California Institute for Medical Research, San Jose, CA 95128 USA and Division of Infectious Diseases and Geographic Medicine, Stanford University, Stanford, CA 94305, and 2Eijkman-Winkler Institute for Medical and Clinical Microbiology, University Medical Center Utrecht, Utrecht, The Netherlands Abstract The Candida parapsilosis family has emerged as a major opportunistic and nosocomial pathogen. It causes multifaceted pathology in immuno-compromised and normal hosts, notably low birth weight neonates. Its emergence may relate to an ability to colonize the skin, proliferate in glucose-containing solutions, and adhere to plastic. When clusters appear, determination of genetic relatedness among strains and identifica- tion of a common source are important. Its virulence appears associated with a capacity to produce biofilm and production of phospholipase and aspartyl protease. Further investigations of the host-pathogen inter- actions are needed. This review summarizes basic science, clinical and experimental information about C. parapsilosis. Keywords: Candida parapsilosis, epidermiology, strain differentiation, clinical aspects, pathogenesis, For personal use only. antifungal susceptibility Introduction The organism was first described in 1928 (Ashford 1928), and early reports of C. parapsilosis described the organ- Candida bloodstream infections (BSI) remain an ism as a relatively non-pathogenic yeast in the normal exceedingly common life-threatening fungal disease flora of healthy individuals that was of minor clinical and are now recognized as a major cause of hospital- significance (Weems 1992). -
Red-Brown Patches in the Groin
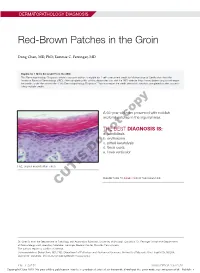
DERMATOPATHOLOGY DIAGNOSIS Red-Brown Patches in the Groin Dong Chen, MD, PhD; Tammie C. Ferringer, MD Eligible for 1 MOC SA Credit From the ABD This Dermatopathology Diagnosis article in our print edition is eligible for 1 self-assessment credit for Maintenance of Certification from the American Board of Dermatology (ABD). After completing this activity, diplomates can visit the ABD website (http://www.abderm.org) to self-report the credits under the activity title “Cutis Dermatopathology Diagnosis.” You may report the credit after each activity is completed or after accumu- lating multiple credits. A 66-year-old man presented with reddish arciform patchescopy in the inguinal area. THE BEST DIAGNOSIS IS: a. candidiasis b. noterythrasma c. pitted keratolysis d. tinea cruris Doe. tinea versicolor H&E, original magnification ×600. PLEASE TURN TO PAGE 419 FOR THE DIAGNOSIS CUTIS Dr. Chen is from the Department of Pathology and Anatomical Sciences, University of Missouri, Columbia. Dr. Ferringer is from the Departments of Dermatology and Laboratory Medicine, Geisinger Medical Center, Danville, Pennsylvania. The authors report no conflict of interest. Correspondence: Dong Chen, MD, PhD, Department of Pathology and Anatomical Sciences, University of Missouri, One Hospital Dr, MA204, DC018.00, Columbia, MO 65212 ([email protected]). 416 I CUTIS® WWW.MDEDGE.COM/CUTIS Copyright Cutis 2018. No part of this publication may be reproduced, stored, or transmitted without the prior written permission of the Publisher. DERMATOPATHOLOGY DIAGNOSIS DISCUSSION THE DIAGNOSIS: Erythrasma rythrasma usually involves intertriginous areas surface (Figure 1) compared to dermatophyte hyphae that (eg, axillae, groin, inframammary area). Patients tend to be parallel to the surface.2 E present with well-demarcated, minimally scaly, red- Pitted keratolysis is a superficial bacterial infection brown patches. -

Tinea Capitis 2014 L.C
BJD GUIDELINES British Journal of Dermatology British Association of Dermatologists’ guidelines for the management of tinea capitis 2014 L.C. Fuller,1 R.C. Barton,2 M.F. Mohd Mustapa,3 L.E. Proudfoot,4 S.P. Punjabi5 and E.M. Higgins6 1Department of Dermatology, Chelsea & Westminster Hospital, Fulham Road, London SW10 9NH, U.K. 2Department of Microbiology, Leeds General Infirmary, Leeds LS1 3EX, U.K. 3British Association of Dermatologists, Willan House, 4 Fitzroy Square, London W1T 5HQ, U.K. 4St John’s Institute of Dermatology, Guy’s and St Thomas’ NHS Foundation Trust, St Thomas’ Hospital, Westminster Bridge Road, London SE1 7EH, U.K. 5Department of Dermatology, Hammersmith Hospital, 150 Du Cane Road, London W12 0HS, U.K. 6Department of Dermatology, King’s College Hospital, Denmark Hill, London SE5 9RS, U.K. 1.0 Purpose and scope Correspondence Claire Fuller. The overall objective of this guideline is to provide up-to- E-mail: [email protected] date, evidence-based recommendations for the management of tinea capitis. This document aims to update and expand Accepted for publication on the previous guidelines by (i) offering an appraisal of 8 June 2014 all relevant literature since January 1999, focusing on any key developments; (ii) addressing important, practical clini- Funding sources cal questions relating to the primary guideline objective, i.e. None. accurate diagnosis and identification of cases; suitable treat- ment to minimize duration of disease, discomfort and scar- Conflicts of interest ring; and limiting spread among other members of the L.C.F. has received sponsorship to attend conferences from Almirall, Janssen and LEO Pharma (nonspecific); has acted as a consultant for Alliance Pharma (nonspe- community; (iii) providing guideline recommendations and, cific); and has legal representation for L’Oreal U.K. -

Detection of Histoplasma DNA from Tissue Blocks by a Specific
Journal of Fungi Article Detection of Histoplasma DNA from Tissue Blocks by a Specific and a Broad-Range Real-Time PCR: Tools to Elucidate the Epidemiology of Histoplasmosis Dunja Wilmes 1,*, Ilka McCormick-Smith 1, Charlotte Lempp 2 , Ursula Mayer 2 , Arik Bernard Schulze 3 , Dirk Theegarten 4, Sylvia Hartmann 5 and Volker Rickerts 1 1 Reference Laboratory for Cryptococcosis and Uncommon Invasive Fungal Infections, Division for Mycotic and Parasitic Agents and Mycobacteria, Robert Koch Institute, 13353 Berlin, Germany; [email protected] (I.M.-S.); [email protected] (V.R.) 2 Vet Med Labor GmbH, Division of IDEXX Laboratories, 71636 Ludwigsburg, Germany; [email protected] (C.L.); [email protected] (U.M.) 3 Department of Medicine A, Hematology, Oncology and Pulmonary Medicine, University Hospital Muenster, 48149 Muenster, Germany; [email protected] 4 Institute of Pathology, University Hospital Essen, University Duisburg-Essen, 45147 Essen, Germany; [email protected] 5 Senckenberg Institute for Pathology, Johann Wolfgang Goethe University Frankfurt, 60323 Frankfurt am Main, Germany; [email protected] * Correspondence: [email protected]; Tel.: +49-30-187-542-862 Received: 10 November 2020; Accepted: 25 November 2020; Published: 27 November 2020 Abstract: Lack of sensitive diagnostic tests impairs the understanding of the epidemiology of histoplasmosis, a disease whose burden is estimated to be largely underrated. Broad-range PCRs have been applied to identify fungal agents from pathology blocks, but sensitivity is variable. In this study, we compared the results of a specific Histoplasma qPCR (H. qPCR) with the results of a broad-range qPCR (28S qPCR) on formalin-fixed, paraffin-embedded (FFPE) tissue specimens from patients with proven fungal infections (n = 67), histologically suggestive of histoplasmosis (n = 36) and other mycoses (n = 31). -

Dermatologic Nuances in Children with Skin of Color
5/21/2019 Dermatologic Nuances in Children with Skin of Color Candrice R. Heath, MD, FAAP, FAAD Director, Pediatric Dermatology LKSOM Temple University @DrCandriceHeath Advisory Board – Pfizer, Regeneron-Sanofi Consultant –Marketing – Unilever, Proctor & Gamble Speaker’s Bureau - Pfizer I do not intend to discuss on-FDA approved or investigational use of products in my presentation. • Recognize common hair, scalp and skin disorders that may present differently in children with skin of color • Select appropriate treatment options based upon common cultural preferences to increase adherence • Establish treatment algorithm for challenging cases 1 5/21/2019 • 2050 : Over half of the United States population will be people of color • 2050 : 1 in 3 US residents will be Hispanic • 2023 : Over half of the children in the US will be people of color • Focuses on ethnic and racial groups who have – similar skin characteristics – similar skin diseases – similar reaction patterns to those skin diseases Taylor SC et al. (2016) Defining Skin of Color. In Taylor & Kelly’s Dermatology for Skin of Color. 2016 Type I always burns, never tans (palest) Type II usually burns, tans minimally Type III sometimes mild burn, tans uniformly Type IV burns minimally, always tans well (moderate brown) Type V very rarely burns, tans very easily (dark brown) Type VI Never burns (deeply pigmented dark brown to darkest brown) 2 5/21/2019 • Black • Asian • Hispanic • Other Not so fast… • Darker skin hues • The term “race” is faulty – Race may not equal biological or genetic inheritance – There is not one gene or characteristic that separates every person of one race from another Taylor SC et al. -

Candida Parapsilosis Complex Francesco Barchiesi1* , Elena Orsetti1, Patrizia Osimani3, Carlo Catassi2, Fabio Santelli4 and Esther Manso5
Barchiesi et al. BMC Infectious Diseases (2016) 16:387 DOI 10.1186/s12879-016-1704-y RESEARCH ARTICLE Open Access Factors related to outcome of bloodstream infections due to Candida parapsilosis complex Francesco Barchiesi1* , Elena Orsetti1, Patrizia Osimani3, Carlo Catassi2, Fabio Santelli4 and Esther Manso5 Abstract Background: Although Candida albicans is the most common cause of fungal blood stream infections (BSIs), infections due to Candida species other than C. albicans are rising. Candida parapsilosis complex has emerged as an important fungal pathogen and became one of the main causes of fungemia in specific geographical areas. We analyzed the factors related to outcome of candidemia due to C. parapsilosis in a single tertiary referral hospital over a five-year period. Methods: A retrospective observational study of all cases of candidemia was carried out at a 980-bedded University Hospital in Italy. Data regarding demographic characteristics and clinical risk factors were collected from the patient’s medical records. Antifungal susceptibility testing was performed and MIC results were interpreted according to CLSI species-specific clinical breakpoints. Results: Of 270 patients diagnosed with Candida BSIs during the study period, 63 (23 %) were infected with isolates of C. parapsilosis complex which represented the second most frequently isolated yeast after C. albicans. The overall incidence rate was 0.4 episodes/1000 hospital admissions. All the strains were in vitro susceptible to all antifungal agents. The overall crude mortality at 30 days was 27 % (17/63), which was significantly lower than that reported for C. albicans BSIs (42 % [61/146], p = 0.042). Being hospitalized in ICU resulted independently associated with a significant higher risk of mortality (HR 4.625 [CI95% 1.015–21.080], p = 0.048). -

Therapies for Common Cutaneous Fungal Infections
MedicineToday 2014; 15(6): 35-47 PEER REVIEWED FEATURE 2 CPD POINTS Therapies for common cutaneous fungal infections KENG-EE THAI MB BS(Hons), BMedSci(Hons), FACD Key points A practical approach to the diagnosis and treatment of common fungal • Fungal infection should infections of the skin and hair is provided. Topical antifungal therapies always be in the differential are effective and usually used as first-line therapy, with oral antifungals diagnosis of any scaly rash. being saved for recalcitrant infections. Treatment should be for several • Topical antifungal agents are typically adequate treatment weeks at least. for simple tinea. • Oral antifungal therapy may inea and yeast infections are among the dermatophytoses (tinea) and yeast infections be required for extensive most common diagnoses found in general and their differential diagnoses and treatments disease, fungal folliculitis and practice and dermatology. Although are then discussed (Table). tinea involving the face, hair- antifungal therapies are effective in these bearing areas, palms and T infections, an accurate diagnosis is required to ANTIFUNGAL THERAPIES soles. avoid misuse of these or other topical agents. Topical antifungal preparations are the most • Tinea should be suspected if Furthermore, subsequent active prevention is commonly prescribed agents for dermatomy- there is unilateral hand just as important as the initial treatment of the coses, with systemic agents being used for dermatitis and rash on both fungal infection. complex, widespread tinea or when topical agents feet – ‘one hand and two feet’ This article provides a practical approach fail for tinea or yeast infections. The pharmacol- involvement. to antifungal therapy for common fungal infec- ogy of the systemic agents is discussed first here. -

Hair and Nail Disorders
Hair and Nail Disorders E.J. Mayeaux, Jr., M.D., FAAFP Professor of Family Medicine Professor of Obstetrics/Gynecology Louisiana State University Health Sciences Center Shreveport, LA Hair Classification • Terminal (large) hairs – Found on the head and beard – Larger diameters and roots that extend into sub q fat LSUCourtesy Health of SciencesDr. E.J. Mayeaux, Center Jr., – M.D.USA Hair Classification • Vellus hairs are smaller in length and diameter and have less pigment • Intermediate hairs have mixed characteristics CourtesyLSU Health of E.J. Sciences Mayeaux, Jr.,Center M.D. – USA Life cycle of a hair • Hair grows at 0.35 mm/day • Cycle is typically as follows: – Anagen phase (active growth) - 3 years – Catagen (transitional) - 2-3 weeks – Telogen (preshedding or rest) about 3 Mon. • > 85% of hairs of the scalp are in Anagen – Lose 75 – 100 hairs a day • Each hair follicle’s cycle is usually asynchronous with others around it LSU Health Sciences Center – USA Alopecia Definition • Defined as partial or complete loss of hair from where it would normally grow • Can be total, diffuse, patchy, or localized Courtesy of E.J. Mayeaux, Jr., M.D. CourtesyLSU of Healththe Color Sciences Atlas of Family Center Medicine – USA Classification of Alopecia Scarring Nonscarring Neoplastic Medications Nevoid Congenital Injury such as burns Infectious Systemic illnesses Genetic (male pattern) (LE) Toxic (arsenic) Congenital Nutritional Traumatic Endocrine Immunologic PhysiologicLSU Health Sciences Center – USA General Evaluation of Hair Loss • Hx is -

Nails: Tales, Fails and What Prevails in Treating Onychomycosis
J. Hibler, D.O. OhioHealth - O’Bleness Memorial Hospital, Athens, Ohio AOCD Annual Conference Orlando, Florida 10.18.15 A) Onychodystrophy B) Onychogryphosis C)“Question Onychomycosis dogma” – Michael Conroy, MD D) All the above E) None of the above Nail development begins at 8-10 weeks EGA Complete by 5th month Keratinization ~11 weeks No granular layer Nail plate growth: Fingernails 3 mm/month, toenails 1 mm/month Faster in summer or winter? Summer! Index finger or 5th digit nail grows faster? Index finger! Faster growth to middle or lateral edge of each nail? Lateral! Elkonyxis Mee’s lines Aka leukonychia striata Arsenic poisoning Trauma Medications Illness Psoriasis flare Muerhrcke’s bands Hypoalbuminemia Chemotherapy Half & half nails Aka Lindsay’s nails Chronic renal disease Terry’s nails Liver failure, Cirrhosis Malnutrition Diabetes Cardiovascular disease True or False: Onychomycosis = Tinea Unguium? FALSE. Onychomycosis: A fungal disease of the nails (all causes) Dermatophytes, yeasts, molds Tinea unguium: A fungal disease of nail caused by dermatophyte fungi Onychodystrophy ≠ onychomycosis Accounts for up to 50% of all nail disorders Prevalence; 14-28% of > 60 year-olds Variety of subtypes; know them! Sequelae What is the most common cause of onychomycosis? A) Epidermophyton floccosum B) Microsporum spp C) Trichophyton mentagrophytes D) Trichophyton rubrum -Account for ~90% of infections Dermatophytes Trichophyton rubrum Trichophyton mentagrophytes Trichophyton tonsurans, Microsporum canis, Epidermophyton floccosum Nondermatophyte molds Acremonium spp, Fusarium spp Scopulariopsis spp, Sytalidium spp, Aspergillus spp Yeast Candida parapsilosis Candida albicans Candida spp Distal/lateral subungal Proximal subungual onychomycosis onychomycosis (DLSO) (PSO) Most common; T. rubrum Often in immunosuppressed patients T.