Why Is This Important? Phone Triage) and Physical Exam
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Differentiate Red Eye Disorders
Introduction DIFFERENTIATE RED EYE DISORDERS • Needs immediate treatment • Needs treatment within a few days • Does not require treatment Introduction SUBJECTIVE EYE COMPLAINTS • Decreased vision • Pain • Redness Characterize the complaint through history and exam. Introduction TYPES OF RED EYE DISORDERS • Mechanical trauma • Chemical trauma • Inflammation/infection Introduction ETIOLOGIES OF RED EYE 1. Chemical injury 2. Angle-closure glaucoma 3. Ocular foreign body 4. Corneal abrasion 5. Uveitis 6. Conjunctivitis 7. Ocular surface disease 8. Subconjunctival hemorrhage Evaluation RED EYE: POSSIBLE CAUSES • Trauma • Chemicals • Infection • Allergy • Systemic conditions Evaluation RED EYE: CAUSE AND EFFECT Symptom Cause Itching Allergy Burning Lid disorders, dry eye Foreign body sensation Foreign body, corneal abrasion Localized lid tenderness Hordeolum, chalazion Evaluation RED EYE: CAUSE AND EFFECT (Continued) Symptom Cause Deep, intense pain Corneal abrasions, scleritis, iritis, acute glaucoma, sinusitis, etc. Photophobia Corneal abrasions, iritis, acute glaucoma Halo vision Corneal edema (acute glaucoma, uveitis) Evaluation Equipment needed to evaluate red eye Evaluation Refer red eye with vision loss to ophthalmologist for evaluation Evaluation RED EYE DISORDERS: AN ANATOMIC APPROACH • Face • Adnexa – Orbital area – Lids – Ocular movements • Globe – Conjunctiva, sclera – Anterior chamber (using slit lamp if possible) – Intraocular pressure Disorders of the Ocular Adnexa Disorders of the Ocular Adnexa Hordeolum Disorders of the Ocular -

CAUSES, COMPLICATIONS &TREATMENT of A“RED EYE”
CAUSES, COMPLICATIONS & TREATMENT of a “RED EYE” 8 Most cases of “red eye” seen in general practice are likely to be conjunctivitis or a superficial corneal injury, however, red eye can also indicate a serious eye condition such as acute angle glaucoma, iritis, keratitis or scleritis. Features such as significant pain, photophobia, reduced visual acuity and a unilateral presentation are “red flags” that a sight-threatening condition may be present. In the absence of specialised eye examination equipment, such as a slit lamp, General Practitioners must rely on identifying these key features to know which patients require referral to an Ophthalmologist for further assessment. Is it conjunctivitis or is it something more Iritis is also known as anterior uveitis; posterior uveitis is serious? inflammation of the choroid (choroiditis). Complications include glaucoma, cataract and macular oedema. The most likely cause of a red eye in patients who present to 4. Scleritis is inflammation of the sclera. This is a very rare general practice is conjunctivitis. However, red eye can also be presentation, usually associated with autoimmune a feature of a more serious eye condition, in which a delay in disease, e.g. rheumatoid arthritis. treatment due to a missed diagnosis can result in permanent 5. Penetrating eye injury or embedded foreign body; red visual loss. In addition, the inappropriate use of antibacterial eye is not always a feature topical eye preparations contributes to antimicrobial 6. Acid or alkali burn to the eye resistance. The patient history will usually identify a penetrating eye injury Most general practice clinics will not have access to specialised or chemical burn to the eye, but further assessment may be equipment for eye examination, e.g. -
UVEITIS Eye74 (1)
UVEITIS Eye74 (1) Uveitis Last updated: May 9, 2019 Classification .................................................................................................................................... 1 Etiologic categories .......................................................................................................................... 2 Treatment ......................................................................................................................................... 2 Complications ................................................................................................................................... 2 COMMON UVEITIC SYNDROMES ............................................................................................................. 2 Masquerade Syndromes ................................................................................................................... 3 UVEITIS - heterogenous ocular diseases - inflammation of any component of uveal tract (iris, ciliary body, choroid). CLASSIFICATION ANTERIOR UVEITIS (most common uveitis) - localized to anterior segment - iritis and iridocyclitis. IRITIS - white cells confined solely to anterior chamber. IRIDOCYCLITIS - cellular activity also involves retrolental vitreous. etiology (most do not have underlying systemic disease): 1) idiopathic postviral syndrome (most commonly 38-60%) 2) HLA-B27 syndromes, many arthritic syndromes (≈ 17%) 3) trauma (5.7%) 4) herpes simplex, herpes zoster disease (1.9-12.4%) 5) iatrogenic (postoperative). tends to -

View Returned the Following Day, Less Than OR
s s CONSEQUENTIAL CASES CASES THAT CHANGED THE WAY WE PRACTICE Three retina specialists share stories of patient encounters that left lasting impressions. LET THERE BE LIGHT By Ninel Z. Gregori, MD vision requires daily practice and hard my career in the direction of other A 52-year-old patient work. The patient had an intense innovative surgeries and clinical trials who had seen nothing rehabilitation process ahead of her at Bascom Palmer. but weak light for to help her to make sense of the And it did much more: It helped me 19 years since devel- lights. She is now able to identify light truly understand and appreciate the oping end-stage retinitis pigmentosa objects against dark backgrounds, value of careful preoperative counsel- (RP) came into my care. Then, in 2013, sort light and dark clothes, see light ing and setting realistic expectations the long-awaited promise of artificial coming in the windows, identify the for patients undergoing new treat- vision became a reality because the handle on the refrigerator, and even ments. After observing the experiences US FDA had approved the first retinal identify some letters, numbers, and of my patient receiving an Argus II prosthesis for patients with RP. I dis- simple words on a computer screen. implant, I now make sure to carefully cussed the Argus II Retinal Prosthesis She cannot, however, recognize explain the risks and limitations of System (Second Sight) with the objects and people in the environ- artificial vision options to patients who patient, and we agreed that she was a ment consistently, see faces, or read. -

Ocular Inflammation Associated with Systemic Infection
Byung Gil Moon, et al. • Ocular Inflammation Associated with Systemic Infection HMR Review Ocular Inflammation Associated with Systemic Infection Hanyang Med Rev 2016;36:192-202 http://dx.doi.org/10.7599/hmr.2016.36.3.192 pISSN 1738-429X eISSN 2234-4446 Byung Gil Moon, Joo Yong Lee Department of Ophthalmology, Asan Medical Center, University of Ulsan College of Medicine, Seoul, Korea Systemic infections that are caused by various types of pathogenic organisms can be spread Correspondence to: Joo Yong Lee Department of Ophthalmology, Asan to the eyes as well as to other solid organs. Bacteria, parasites, and viruses can invade the Medical Center, University of Ulsan eyes via the bloodstream. Despite advances in the diagnosis and treatment of systemic in- College of Medicine, 88 Olympic-ro fections, many patients still suffer from endogenous ocular infections; this is particularly 43-gil, Songpa-gu, Seoul 05505, Korea Tel: +82-2-3010-3976 due to an increase in the number of immunosuppressed patients such as those with hu- Fax: +82-2-470-6440 man immunodeficiency virus infection, those who have had organ transplantations, and E-mail: [email protected] those being administered systemic chemotherapeutic and immunomodulating agents, which may increase the chance of ocular involvement. In this review, we clinically evalu- Received 2 July 2016 Revised 21 July 2016 ated posterior segment manifestations in the eye caused by hematogenous penetration Accepted 27 July 2016 of systemic infections. We focused on the conditions that ophthalmologists encounter This is an Open Access article distributed under most often and that require cooperation with other medical specialists. -

Endophthalmitis
RETINA HEALTH SERIES | Facts from the ASRS The Foundation American Society of Retina Specialists Committed to improving the quality of life of all people with retinal disease. Endophthalmitis is an infection inside the eye SIGNS AND SYMPTOMS that can either be acute or chronic, meaning that it can develop very rapidly which is most common, or develop Endophthalmitis causes the white slowly and persist for long periods of time of the eye to be inflamed. There may be a white or yellow discharge on or inside the eyelid, and the cornea may show a white cloud- iness. There may also be a layer of white cells (hypopyon) present within the anterior chamber of the eye between the iris and the cornea. (Figure 1) Endophthalmitis is usually a very serious problem and prompt examination by an ophthalmologist is essential to make an appropriate diagnosis and initiate treatment. Other symptoms include: • Eye pain and redness • Decreased vision • Trouble looking at bright lights (photophobia), usually sudden onset Figure 1 Hypopyon is an accumulation of white blood cells in the anterior chamber of the eye and corneal WHAT IS THE RETINA? infiltrate associated with infectious endophthalmitis. Image courtesy of ©Retina Image Bank, contributed by Aleksandra V. Rachitskay, MD, Cole Eye Institute, Cleveland Clinic. 2014. Image 16250. Causes: Acute cases of endophthalmitis are caused by gram-positive (or less frequently gram-negative) bacteria and are most often seen within 6 weeks after surgery or trauma to the eye. Chronic cases that occur outside of the 6-week window are often related to a previous surgery and are commonly caused by slowly progressive infections such as Propionibacterium acnes or fungus. -
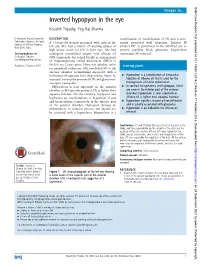
Inverted Hypopyon in the Eye Koushik Tripathy, Yog Raj Sharma
BMJ Case Reports: first published as 10.1136/bcr-2016-214638 on 17 February 2016. Downloaded from Images in… Inverted hypopyon in the eye Koushik Tripathy, Yog Raj Sharma Dr Rajendra Prasad Centre for DESCRIPTION manifestation of emulsification of SO and is com- Ophthalmic Sciences, All India A 33-year-old woman presented with pain in the monly associated with glaucoma. Inferior PI Institute of Medical Sciences, ’ 1 fi New Delhi, India left eye. She had a history of wearing glasses of (Ando s PI) is performed in the SO- lled eye to high minus power (–11D) in both eyes. She had prevent pupillary block glaucoma. Hyperoleon Correspondence to undergone vitreoretinal surgery with silicone oil necessitates SO removal. Dr Koushik Tripathy, (SO) tamponade for retinal breaks as management [email protected] of rhegmatogenous retinal detachment (RRD) in Accepted 3 February 2016 the left eye 2 years prior. There was aphakia, infer- Learning points ior peripheral iridectomy (PI), emulsified SO in the anterior chamber accumulating superiorly with a ▸ horizontal oil–aqueous level (hyperoleon, figure 1), Hyperoleon is a complication of intraocular increased intraocular pressure (IOP) and glaucomat- injection of silicone oil that is used for the ous optic neuropathy. management of retinal detachment. ▸ Hyperoleon is seen superiorly in the anterior In contrast to hyphaema and hypopyon, which chamber as SO (specific gravity 0.97) is lighter than are seen in the inferior part of the anterior aqueous humour. On the contrary, hypopyon and chamber, hyperoleon is seen superiorly as hyphaema are manifestations of deposition of pus silicone oil is lighter than aqueous humour. -

Retina II Jeanne L. Rosenthal MD MPOD FACS
Retina II by Jeanne L. Rosenthal MD MPOD FACS Surgeon Director in Ophthalmology Assoc. Director, Retina Service Attending Surgeon, Trauma Service New York Eye and Ear Infirmary Clinical Professor of Ophthalmology New York Medical College Jeanne L.Rosenthal MD OKAP 2014 Based on AAO Basic and Clinical Science Course, Section 12 Retina and Vitreous, 2006-2007 Part II Chapter 10 Retinal Degenerations Associated with Systemic Disease: I. Disorders involving other organ systems: A. Infantile-Onset to Early Childhood-Onset Syndromes 1. Retinal dysfunction and low ERG 2. Differentiate from Leber congenital amaurosis 3. Neuronal ceroid lipofuscinoses (Batten disease) 4. Peroxisome disorders: a. Refsum disease b. Zellweger (cerebrohepatorenal) syndrome c. Neonatal adrenoleukodystrophy 5. Leber's does not have seizures or deterioration in mental status B. Bardet-Biedl Complex of diseases 1. Group of diseases with similar findings: a. pigmentary retinopathy b. obesity c. polydactyly d. hypogonadism e. mental retardation f. no bone spicules C. Hearing Loss and Pigmentary Retinopathy 1. Usher Syndrome a. Association of retinitis pigmentosa and congenital sensorineural hearing loss b. 11 different genetic types c. 10% of RP patients are profoundly deaf d. Differentiate from Alport syndrome, Alström and Cockayne syndromes, dysplasia spondyloepiphysaria congenita, Hurler syndrome, and Refsum disease D. Neuromuscular Disorders 1. Spinocerebellar degenerations: Friedreich's ataxia 2. Olivopontocerebellar atrophies 3. Charcot-Marie-Tooth disease 4. Myotonic dystrophy 5. Neuronal ceroid lipofuscinosis (Batten disease) 6. Progressive external ophthalmoplegia syndromes 7. Peroxisome disorders 8. Duchenne muscular dystrophy: 3 Jeanne L.Rosenthal MD OKAP 2014 a. No visual symptoms b. Characteristic ERG abnormality: normal A wave, reduced B wave E. -

Anterior Uveitis and Hypopyon*
ANTERIOR UVEITIS AND HYPOPYON* BY Leonardo P. DAlessandro, MD (BY INVITATION), DavidJ. Forster, MD (BY INVITATION), AND Narsing A. Rao, MD INTRODUCTION ANTERIOR UVEITIS IS THE MOST COMMON FORM OF INTRAOCULAR INFLAM- mation seen by the ophthalmologist. When severe, anterior uveitis can result in the formation of hypopyon within the anterior chamber. Hypo- pyon in endogenous anterior uveitis has been related classically to Beh- get's syndrome.1-3 A few investigators have also reported the occasional observation of hypopyon in association with herpetic keratouveitis,4'5 Reiter's syndrome, and ankylosing spondylitis.6-8 We undertook a study to determine the incidence, as well as the most common causes, of hypopyon in patients with acute endogenous anterior uveitis. MATERIALS AND METHODS Medical records of all patients with endogenous anterior uveitis referred to our institution from 1984 to 1990 were reviewed. For each patient, information was obtained regarding the presence or absence ofhypopyon as determined by slit lamp examination, as well as medical history, review of systems, and results of laboratory investigations performed. Laboratory investigations had been performed using a tailored ap- proach and included any or all of the following: tests for antinuclear antibodies, angiotensin-converting enzyme, rheumatoid factor, and HLA- B27 and HLA-B5; syphilis serologic studies, tuberculin skin testing; chest radiography; and radiologic examination of the lumbosacral spine. Patients with concurrent posterior uveitis (retinitis or choroiditis), as well those who had recently undergone ocular surgery or sustained pene- trating trauma to the eye, were excluded. *From the A. Ray Irvine Jr, MD, Ophthalmic Pathology Laboratory of the Doheny Eye Institute, and the Department of Ophthalmology, University of Southern California, Los Angeles. -

Grand Rounds a String of Pearls Attendee Handout Dec 2015
9/6/16 Grand rounds: A string of pearls Case #1 Nathan Lighthizer, O.D., F.A.A.O. Assistant Professor, NSUOCO Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic [email protected] COPE #33259-AS Recurrent Corneal Erosions Recurrent Corneal Erosions (RCE’s) • Tendency for minor trauma to cause • Sx’s: significant corneal epithelial disturbances – Acute, severe pain** • Pathophysiology – Photophobia ** – Abnormally weak attachment between the basal – Redness cells of the corneal epithelium and their basement – membrane Blepharospasm – • Most common causes of the weak attachment Tearing – Mechanical trauma** – Corneal dystrophy** ***Usually sx’s present first thing in the morning upon opening the eyes.*** – Corneal surgery And often this is recurrent Recurrent Corneal Erosions Recurrent Corneal Erosions • Signs: • Signs: – Epithelial defect may be present, – If no defect is present, look for loose, irregular epithelium usually in the inferior interpalpebral area (pooling of NaFl, rapid TBUT) – Signs of corneal dystrophies (will be bilateral) 1 9/6/16 Recurrent Corneal Erosions • Tx: – Acutely: • Lubrication** • Topical Ab (Polytrim QID, erythro or bacitracin ung) • Pain control: – Cycloplegic (Homatropine BID) • Muro 128 drops or ung • Bandage lens??? – Alleviates pain, does not improve healing Recurrent Corneal Erosions Recurrent Corneal Erosions • Tx: • Surgical Tx: – After the epithelium heals (recalcitrant RCE’s): – Anterior stromal micropuncture • Fresh Kote TID (15ml bottle $25) – • Muro 128 ung qhs (3.5g tube $10) Debridement of epithelium with polishing of Bowman’s membrane with a diamond burr or • Lotemax QID X 2 weeks, BID X 6 weeks excimer laser (PTK) • Doxycycline 20-50mg BID – Azasite BID (2.5ml bottle $78) **Avoid chronic long-term AT ung** Eyelid abscess vs. -

Ocular Emergencies & Red
Ocular Emergencies & Red Eye [ Color index: Important | Notes: F1, F2 | Extra ] EDITING FILE Objectives: ➢ Not given. Done by: Monerah Alsalouli. Edited and revised by: Munerah AlOmari. Resources: Slides + Notes + Lecture Notes of Ophthalmology + 435 Team + OphthoBook, Mayoclinic + Medscape + Master the boards. Don’t freak out! This lecture is 2 lectures in one! Ocular Emergencies ﻻ ﺳﻤﺢ This lecture is so important (MCQs and future live), you may face it yourself or one of your family members .اﷲ Usually the outcome in emergency cases depend on immediate intervention (how did you manage the pt earlier), so despite the specialty you choose, you need to know these principles. General Emergencies Orbital/Ocular Trauma Corneal abrasion Corneal ulcer Corneal & conjunctival foreign bodies Uveitis Hyphema Acute angle glaucoma Ruptured globe Orbital cellulitis Orbital wall fracture Endophthalmitis Lid Laceration Retinal detachment Chemical injury ● Corneal abrasion: Corneal abrasions result from a disruption or loss of cells in the top layer of the cornea, called the corneal Epithelium. History of scratching the eye (fingernails or lenses). the epithelium has the ability to replicate. Symptoms: - Foreign body sensation. - Severe Pain. - Redness. - Tearing. - Photophobia experience of discomfort or pain to the eyes due to light exposure “Corneal Abrasion can lead to Corneal Ulcer if untreated“ Treatment: it heals within 24 hrs. Mostly will heal by itself but we fear of infections - Topical antibiotic “prophylactic to prevent infections” اﺣﯿﺎﻧﺎ ﻣﺎ ﯾﺤﺘﺎج ﻧﻐﻄﯿﻬﺎ .Pressure patch over the eye - - Refer to ophthalmologist. See them everyday until it's gone - Cycloplegia to dilate pupil to decrease pain. - Important to treat to avoid infection. -

Toxic Anterior Segment Syndrome After an Uncomplicated Vitrectomy with Epiretinal Membrane Peeling
Open Access Case Report DOI: 10.7759/cureus.14464 Toxic Anterior Segment Syndrome After an Uncomplicated Vitrectomy With Epiretinal Membrane Peeling Piotr Kanclerz 1 1. Ophthalmology, Hygeia Clinic, Gdansk, POL Corresponding author: Piotr Kanclerz, [email protected] Abstract Infectious endophthalmitis is the most devastating complication of eye surgery and is associated with severe inflammation of ocular tissues. This study aimed to present a similar condition, a case of toxic anterior segment syndrome (TASS) after an uncomplicated vitrectomy. A 69-year-old woman presented with epiretinal membrane and underwent 25-gauge pars plana vitrectomy with membrane peeling in her left eye. Thirty hours after the procedure, the patient complained of increasing loss of visual acuity and a red left eye. The ophthalmic examination revealed moderate hyperemia, hypopyon and snowbanks in the anterior vitreous. Subconjunctival and topical steroids were administered, and the inflammatory symptoms resolved within 30 days. The visual acuity improved to 20/32, however, cystoid changes were noted in the macula by optical coherence tomography. TASS should be considered a potential complication after vitrectomy. This report presents a case of TASS and discusses the differential diagnosis between TASS, infectious and non-infectious endophthalmitis. Categories: Ophthalmology Keywords: endophthalmitis, epiretinal membrane, toxic anterior segment syndrome, pars planitis, vitrectomy Introduction Postoperative endophthalmitis (POE) is the most devastating complication of intraocular surgery, and is associated with severe inflammation of ocular issues. POE following vitrectomy is relatively uncommon; in large studies the incidence rates range between 0.02% and 0.15% [1]. Toxic anterior segment syndrome (TASS) is defined as a sterile postoperative inflammation of the anterior segment after intraocular surgery [2].