Filters
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Title: ED Trauma: Trauma Nurse Clinical Resuscitation
Title: ED Trauma: Trauma Nurse Clinical Resuscitation Document Category: Clinical Document Type: Policy Department/Committee Owner: Practice Council Original Date: Approved By (last review): Director of Emergency Services, Approval Date: 07/28/2014 Trauma Medical Director, Medical Director Emergency (Complete history at end of document.) Services POLICY: To provide immediate, effective and efficient patient care to the trauma patient, designated nursing staff will respond to the trauma room when a trauma page is received. TRAUMA CONTROL NURSE: 1) Role: a) The trauma control nurse (TCN) is a registered nurse (RN) with specialized training in the care of the traumatized patient, and who will function as the trauma team’s lead nurse. b) The TCN shall have successfully completed the Trauma Nurse Core Course (TNCC), Advanced Cardiac Life Support (ACLS), Emergency Nurse Pediatric Course (ENPC) or Pediatric Advanced Life Support (PALS), and role orientation with trauma services. c) Full-time employee or regularly scheduled part-time Emergency Department (ED) nurse. d) RN must have 6 months of LMH ED experience. 2) Trauma Control Duties: a) Inspects and stocks trauma room at beginning of each shift and after each trauma patient is discharged from the ED. b) Attempts to maintain trauma room temperature at 80-82 degrees Fahrenheit. c) Communicates with pre-hospital personnel to obtain patient information and prior field treatment and response. d) Makes determination that a patient meets Type I or Type II criteria and immediately notifies LMH’s Call System to initiate the Trauma Activation System. e) Assists physician with orders as directed. f) Acts as liaison with patient’s family/law enforcement/emergency medical services (EMS)/flight crews. -

Early Management of Retained Hemothorax in Blunt Head and Chest Trauma
World J Surg https://doi.org/10.1007/s00268-017-4420-x ORIGINAL SCIENTIFIC REPORT Early Management of Retained Hemothorax in Blunt Head and Chest Trauma 1,2 1,8 1,7 1 Fong-Dee Huang • Wen-Bin Yeh • Sheng-Shih Chen • Yuan-Yuarn Liu • 1 1,3,6 4,5 I-Yin Lu • Yi-Pin Chou • Tzu-Chin Wu Ó The Author(s) 2018. This article is an open access publication Abstract Background Major blunt chest injury usually leads to the development of retained hemothorax and pneumothorax, and needs further intervention. However, since blunt chest injury may be combined with blunt head injury that typically requires patient observation for 3–4 days, other critical surgical interventions may be delayed. The purpose of this study is to analyze the outcomes of head injury patients who received early, versus delayed thoracic surgeries. Materials and methods From May 2005 to February 2012, 61 patients with major blunt injuries to the chest and head were prospectively enrolled. These patients had an intracranial hemorrhage without indications of craniotomy. All the patients received video-assisted thoracoscopic surgery (VATS) due to retained hemothorax or pneumothorax. Patients were divided into two groups according to the time from trauma to operation, this being within 4 days for Group 1 and more than 4 days for Group 2. The clinical outcomes included hospital length of stay (LOS), intensive care unit (ICU) LOS, infection rates, and the time period of ventilator use and chest tube intubation. Result All demographics, including age, gender, and trauma severity between the two groups showed no statistical differences. -

NIH Public Access Author Manuscript J Neuropathol Exp Neurol
NIH Public Access Author Manuscript J Neuropathol Exp Neurol. Author manuscript; available in PMC 2010 September 24. NIH-PA Author ManuscriptPublished NIH-PA Author Manuscript in final edited NIH-PA Author Manuscript form as: J Neuropathol Exp Neurol. 2009 July ; 68(7): 709±735. doi:10.1097/NEN.0b013e3181a9d503. Chronic Traumatic Encephalopathy in Athletes: Progressive Tauopathy following Repetitive Head Injury Ann C. McKee, MD1,2,3,4, Robert C. Cantu, MD3,5,6,7, Christopher J. Nowinski, AB3,5, E. Tessa Hedley-Whyte, MD8, Brandon E. Gavett, PhD1, Andrew E. Budson, MD1,4, Veronica E. Santini, MD1, Hyo-Soon Lee, MD1, Caroline A. Kubilus1,3, and Robert A. Stern, PhD1,3 1 Department of Neurology, Boston University School of Medicine, Boston, Massachusetts 2 Department of Pathology, Boston University School of Medicine, Boston, Massachusetts 3 Center for the Study of Traumatic Encephalopathy, Boston University School of Medicine, Boston, Massachusetts 4 Geriatric Research Education Clinical Center, Bedford Veterans Administration Medical Center, Bedford, Massachusetts 5 Sports Legacy Institute, Waltham, MA 6 Department of Neurosurgery, Boston University School of Medicine, Boston, Massachusetts 7 Department of Neurosurgery, Emerson Hospital, Concord, MA 8 CS Kubik Laboratory for Neuropathology, Department of Pathology, Massachusetts General Hospital, Harvard Medical School, Boston, Massachusetts Abstract Since the 1920s, it has been known that the repetitive brain trauma associated with boxing may produce a progressive neurological deterioration, originally termed “dementia pugilistica” and more recently, chronic traumatic encephalopathy (CTE). We review the 47 cases of neuropathologically verified CTE recorded in the literature and document the detailed findings of CTE in 3 professional athletes: one football player and 2 boxers. -
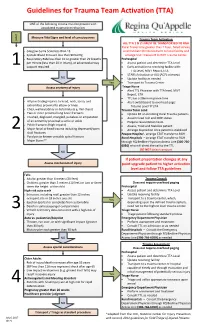
Guidelines for Trauma Team Activation (TTA)
Guidelines for Trauma Team Activation (TTA) ONE of the following criteria must be present with associated traumatic mechanism L e v e Measure Vital Signs and level of consciousness l Trauma Team Activation ALL TTA 1 & 2's MUST BE TRANSPORTED TO RGH Rural Travel time greater than 1 hour, failed airway · Glasgow Coma Scale less than 13 or immediate life threat divert to local facility and · Systolic Blood Pressure less than 90mmHg arrange STAT transport to RGH Trauma Center · Respiratory Rate less than 10 or greater then 29 breaths Prehospital per minute (less than 20 in infant), or advanced airway · Assess patient and determine TTA Level 1 support required · Early activation to receiving facility with: TTA Level, MIVT Report, ETA · STARS Activation or ALS (ACP) intercept NO · Update facility as needed Yes · Transport to Trauma Center Assess anatomy of injury Triage Nurse · Alert TTL Physician with TTA level, MIVT Report, ETA · TTL has a 20min response time · All penetrating injuries to head, neck, torso, and · Alert switchboard to overhead page: extremities proximal to elbow or knee Trauma Level ‘#’ ETA · Chest wall instability or deformity (e.g. flail chest) Trauma Team Lead · Two or more proximal long-bone fractures · Update ER on incoming Rural Trauma patients · Crushed, degloved, mangled, pulseless or amputation · Assume lead role and MRP status of an extremity proximal to wrist or ankle · Prepare resuscitation team · Pelvic fractures (high impact) · Assess, Treat and Stabilize patient 2 · Major facial or head trauma including depressed/open -

Guidelines for BLS/ALS Medical Providers Current As of March 2019
Tactical Emergency Casualty Care (TECC) Guidelines for BLS/ALS Medical Providers Current as of March 2019 DIRECT THREAT CARE (DTC) / HOT ZONE Guidelines: 1. Mitigate any immediate threat and move to a safer position (e.g. initiate fire attack, coordinated ventilation, move to safe haven, evacuate from an impending structural collapse, etc). Recognize that threats are dynamic and may be ongoing, requiring continuous threat assessments. 2. Direct the injured first responder to stay engaged in the operation if able and appropriate. 3. Move patient to a safer position: a. Instruct the alert, capable patient to move to a safer position and apply self-aid. b. If the patient is responsive but is injured to the point that he/she cannot move, a rescue plan should be devised. c. If a patient is unresponsive, weigh the risks and benefits of an immediate rescue attempt in terms of manpower and likelihood of success. Remote medical assessment techniques should be considered to identify patients who are dead or have non-survivable wounds. 4. Stop life threatening external hemorrhage if present and reasonable depending on the immediate threat, severity of the bleeding and the evacuation distance to safety. Consider moving to safety prior to application of the tourniquet if the situation warrants. a. Apply direct pressure to wound, or direct capable patient to apply direct pressure to own wound and/or own effective tourniquet. b. Tourniquet application: i. Apply the tourniquet as high on the limb as possible, including over the clothing if present. ii. Tighten until cessation of bleeding and move to safety. -

Early Post-Traumatic Pulmonary-Embolism in Patients Requiring ICU Admission: More Complicated Than We Think!
3854 Editorial Early post-traumatic pulmonary-embolism in patients requiring ICU admission: more complicated than we think! Mabrouk Bahloul1, Mariem Dlela1, Nadia Khlaf Bouaziz2, Olfa Turki1, Hedi Chelly1, Mounir Bouaziz1 1Department of Intensive Care, Habib Bourguiba University Hospital, Sfax, Tunisia; 2Centre Intermédiaire, Rte El MATAR Km 4, Sfax, Tunisia Correspondence to: Professor Mabrouk Bahloul. Department of Intensive Care, Habib Bourguiba University Hospital, 3029 Sfax, Tunisia. Email: [email protected]. Submitted Jun 10, 2018. Accepted for publication Sep 12, 2018. doi: 10.21037/jtd.2018.09.49 View this article at: http://dx.doi.org/10.21037/jtd.2018.09.49 We read with interest the article entitled “Prevalence and traumatic thromboembolism in patients who are requiring main determinants of early post-traumatic thromboembolism an ICU admission. Nevertheless, this study as mentioned in patients requiring ICU admission” (1). In this retrospective by the authors suffers from many limitations. In fact, the study, Kazemi Darabadi et al. (1) had included to their small sample size, and also the retrospective design of database, the records of 240 trauma-patients requiring the study lead to an increased probability of some bias ICU admission, with a confirmed diagnosis of pulmonary when collecting data. In fact, in this study (1), PE was embolism (PE). The patients were categorized as subjects not screened on a daily basis. As a consequence, the late with an early PE (≤3 days) and those with a late PE (>3 days). stage PE may only be a delayed diagnosis. For instance, According to their analysis, 48.5% of the patients suffering a patient who develops with PE on day 2 but without any from PE had developed this complication within 72 h symptom(s); then he is accidentally diagnosed with PE on following a trauma event and/or after ICU admission. -

The Fund at a Glance
CytoSorbentsTM Trauma and Crush Injury TRAUMA AND CRUSH INJURIES ARE CURRENTLY LEADING CAUSES OF DEATH. Trauma and crush injuries occur frequently and from multiple sources. For example, automobile or motorcycle accidents, natural disasters, and acts of criminal violence or terrorism can all yield mild to severe trauma and crush injuries. The breadth of life-threatening conditions from trauma-induced injuries, such as lung and bowel rupture, closed head injury, crush injury and rhabdomyolysis, traumatic fractures, penetrating wound injury, and limb loss, creates a very challenging environment for clinicians to employ effective treatment strategies. Better therapies are needed to reduce the mortality in patients with severe trauma injury, reduce the risk of organ failure, reduce complications (e.g. rhabdomyolysis and infection), and decrease hospital stay length. CYTOKINE STORM AND RHABDOMYOLYSIS IN TRAUMA CAN CAUSE ORGAN FAILURE AND DEATH Trauma is a well-known trigger of the immune response, and can result in the massive, uncontrolled production of cytokines, or “cytokine storm.” Cytokines are small proteins that normally help stimulate and regulate the immune system to fight infection or injury. However, in trauma, cytokine storm can be toxic, leading to a massive systemic inflammatory response syndrome (SIRS) and a cascade of events that can kill cells and damage organs, leading to organ failure and often death. Cytokine storm exacerbates physical trauma in many ways. For example, trauma can cause: Hemorrhagic shock due to blood loss while cytokine storm causes capillary leak and intravascular volume loss, and the induction of nitric oxide that can lead to myocardial depression and peripheral vasodilation, all of which exacerbate shock Severe limb injuries that often require a tourniquet. -

Traumatic Brain Injury (TBI)
Traumatic Brain Injury (TBI) Carol A. Waldmann, MD raumatic brain injury (TBI), caused either by blunt force or acceleration/ deceleration forces, is common in the general population. Homeless persons Tare at particularly high risk of head trauma and adverse outcomes to TBI. Even mild traumatic brain injury can lead to persistent symptoms including cognitive, physical, and behavioral problems. It is important to understand brain injury in the homeless population so that appropriate referrals to specialists and supportive services can be made. Understanding the symptoms and syndromes caused by brain injury sheds light on some of the difficult behavior observed in some homeless persons. This understanding can help clinicians facilitate and guide the care of these individuals. Prevalence and Distribution recover fully, but up to 15% of patients diagnosed TBI and Mood Every year in the USA, approximately 1.5 with MTBI by a physician experience persistent Swings. million people sustain traumatic brain injury disabling problems. Up to 75% of brain injuries This man suffered (TBI), 230,000 people are hospitalized due to TBI are classified as MTBI. These injuries cost the US a gunshot wound and survive, over 50,000 people die from TBI, and almost $17 billion per year. The groups most at risk to the head and many subsequent more than 1 million people are treated in emergency for TBI are those aged 15-24 years and those aged traumatic brain rooms for TBI. In persons under the age of 45 years, 65 years and older. Men are twice as likely to sustain injuries while TBI is the leading cause of death. -

Anytown Trauma Center Trauma Protocols
ANYTOWN TRAUMA CENTER TRAUMA PROTOCOLS TITLE: TRAUMA TEAM ACTIVATION PROTOCOL PURPOSE: The purpose of the protocol is to establish guidelines for trauma team activation and define the members of the responding trauma team to facilitate the resuscitation and management of critical or seriously injured patients who require rapid, organized resuscitation, evaluation and stabilization to promote optimal outcomes. It also serves to provide triage guidelines for adult and pediatric patients. PROCESS: 1. TRAUMA TEAM ACTIVATION PROTCOL A. The criteria for activation of the trauma team is clearly defined and posted at the Emergency Department triage desk, by the EMS communication station and in the resuscitation rooms. B. The trauma team may be activated prior to arrival based on the EMS communication and their assessment. C. The trauma surgeon, emergency medicine physician, emergency department charge nurse/ house supervisor, emergency department nurses and the Trauma Program Manager may activate the trauma team. D. The person calling the trauma activation will initiate the trauma page to group page the trauma team and will specify the MOI, BP, HR, ETA and level of activation required and age if available. E. If the trauma team members are present in the emergency department and alert is still communicated to ensure everyone is notified. F. Trauma team member notification and arrival times will be documented on the trauma flow sheet (paper or electronic). G. Trauma team members will sign-in when they arrive. H. Trauma team members will be activated for all patients who meet the following criteria: 1. Level 1 trauma activation (major): life threatening injuries and/or unstable vital signs, limb-threating or disability threatening injury 2. -

Traumatic Brain Injury in the UNITED STATES Emergency Department Visits, Hospitalizations and Deaths 2002–2006
Traumatic Brain Injury IN THE UNITED STATES Emergency Department Visits, Hospitalizations and Deaths 2002–2006 U.S. Department of Health and Human Services Centers for Disease Control and Prevention www.cdc.gov/TraumaticBrainInjury Traumatic Brain Injury IN THE UNITED STATES Emergency Department Visits, Hospitalizations and Deaths 2002–2006 U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Disease Control and Prevention National Center for Injury Prevention and Control www.cdc.gov/TraumaticBrainInjury MARCH ZXYX AuthoRs Traumatic Brain Injury in the United States: Emergency Department Visits, Hospitalizations and Deaths 2002–2006 is a publication of the National Center for Injury Prevention and Mark Faul, PhD, MS Control, Centers for Disease Control and Prevention. National Center for Injury Prevention and Control Division of Injury Response Centers for Disease Control and Prevention Thomas R. Frieden, MD, MPH, Director Likang Xu, MD, MS National Center for Injury Prevention and Control National Center for Injury Prevention and Control Robin Ikeda, MD, MPA, Acting Director Division of Injury Response Division of Injury Response Marlena M. Wald, MPH, MLS Richard C. Hunt, MD, FACEP, Director National Center for Injury Prevention and Control The findings and conclusions in this report are those of the Division of Injury Response authors and do not necessarily represent the official position of the Centers for Disease Control and Prevention (CDC). Victor G. Coronado, MD, MPH National Center for Injury Prevention and Control Division of Injury Response suggesteD CItAtIoN: Faul M, Xu L, Wald MM, Coronado VG. Traumatic Brain Injury in the United States: Emergency Department Visits, Hospitalizations and Deaths 2002–2006. -

Chapter 1 - Trauma Team from Prehospital Through the Emergency Department Test Questions
Chapter 1 - Trauma Team from Prehospital through the Emergency Department Test Questions 1. As the prehospital provider approaches the scene of a trauma call, they perform a. a radio transmission to the hospital b. a scene size up c. an estimate of neck size for c-collar d. an estimate of victim’s height and weight 2. Field intubation has been proven to improve outcome in a. patients with BP less than 90 mm Hg b. patients with GCS less than 9 c. patients with acute respiratory distress d. none of the above 3. A proven technique of hemorrhage control is a. Direct pressure b. Elevate above the heart c. Pressure points d. Cold application 4. Prehospital care for apparent pelvic fractures includes a. DO NOT ROCK or palpate the pelvis in the prehospital arena b. Avoid log rolling as much as possible c. Apply splint if in your area protocols d. All of the above 5. Most preventable deaths in trauma care are due to a. Delay in CPR b. Cardiac tamponade c. Airway obstruction d. Tension pneumothorax STN 2012 Electronic Library: Chapter 1 - Trauma Team from Prehospital Through the Emergency Department Test Questions 2 6. For resuscitation to occur, there must be a. Cellular perfusion and tissue oxygenation b. Restoration of a blood pressure greater than 90mm Hg c. A hemoglobin greater than 9g/dL d. A PaO2 greater than 80 mm Hg 7. The Trauma Triad of Death is a. Hypotension, tachycardia and decreased urine output b. Infection, inadequate nutrition, DVT’s c. Hypothermia, acidosis and coagulopathy d. -

Guidelines for the Management of Severe Traumatic Brain Injury 4Th Edition
Guidelines for the Management of Severe Traumatic Brain Injury 4th Edition Nancy Carney, PhD Oregon Health & Science University, Portland, OR Annette M. Totten, PhD Oregon Health & Science University, Portland, OR Cindy O'Reilly, BS Oregon Health & Science University, Portland, OR Jamie S. Ullman, MD Hofstra North Shore-LIJ School of Medicine, Hempstead, NY Gregory W. J. Hawryluk, MD, PhD University of Utah, Salt Lake City, UT Michael J. Bell, MD University of Pittsburgh, Pittsburgh, PA Susan L. Bratton, MD University of Utah, Salt Lake City, UT Randall Chesnut, MD University of Washington, Seattle, WA Odette A. Harris, MD, MPH Stanford University, Stanford, CA Niranjan Kissoon, MD University of British Columbia, Vancouver, BC Andres M. Rubiano, MD El Bosque University, Bogota, Colombia; MEDITECH Foundation, Neiva, Colombia Lori Shutter, MD University of Pittsburgh, Pittsburgh, PA Robert C. Tasker, MBBS, MD Harvard Medical School & Boston Children’s Hospital, Boston, MA Monica S. Vavilala, MD University of Washington, Seattle, WA Jack Wilberger, MD Drexel University, Pittsburgh, PA David W. Wright, MD Emory University, Atlanta, GA Jamshid Ghajar, MD, PhD Stanford University, Stanford, CA Reviewed for evidence-based integrity and endorsed by the American Association of Neurological Surgeons and the Congress of Neurological Surgeons. September 2016 TABLE OF CONTENTS PREFACE ...................................................................................................................................... 5 ACKNOWLEDGEMENTS .............................................................................................................................................