Basic Trauma Overview - ABC
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

ABCDE Approach
The ABCDE and SAMPLE History Approach Basic Emergency Care Course Objectives • List the hazards that must be considered when approaching an ill or injured person • List the elements to approaching an ill or injured person safely • List the components of the systematic ABCDE approach to emergency patients • Assess an airway • Explain when to use airway devices • Explain when advanced airway management is needed • Assess breathing • Explain when to assist breathing • Assess fluid status (circulation) • Provide appropriate fluid resuscitation • Describe the critical ABCDE actions • List the elements of a SAMPLE history • Perform a relevant SAMPLE history. Essential skills • Assessing ABCDE • Needle-decompression for tension • Cervical spine immobilization pneumothorax • • Full spine immobilization Three-sided dressing for chest wound • • Head-tilt and chin-life/jaw thrust Intravenous (IV) line placement • • Airway suctioning IV fluid resuscitation • • Management of choking Direct pressure/ deep wound packing for haemorrhage control • Recovery position • Tourniquet for haemorrhage control • Nasopharyngeal (NPA) and oropharyngeal • airway (OPA) placement Pelvic binding • • Bag-valve-mask ventilation Wound management • • Skin pinch test Fracture immobilization • • AVPU (alert, voice, pain, unresponsive) Snake bite management assessment • Glucose administration Why the ABCDE approach? • Approach every patient in a systematic way • Recognize life-threatening conditions early • DO most critical interventions first - fix problems before moving on -

Title: ED Trauma: Trauma Nurse Clinical Resuscitation
Title: ED Trauma: Trauma Nurse Clinical Resuscitation Document Category: Clinical Document Type: Policy Department/Committee Owner: Practice Council Original Date: Approved By (last review): Director of Emergency Services, Approval Date: 07/28/2014 Trauma Medical Director, Medical Director Emergency (Complete history at end of document.) Services POLICY: To provide immediate, effective and efficient patient care to the trauma patient, designated nursing staff will respond to the trauma room when a trauma page is received. TRAUMA CONTROL NURSE: 1) Role: a) The trauma control nurse (TCN) is a registered nurse (RN) with specialized training in the care of the traumatized patient, and who will function as the trauma team’s lead nurse. b) The TCN shall have successfully completed the Trauma Nurse Core Course (TNCC), Advanced Cardiac Life Support (ACLS), Emergency Nurse Pediatric Course (ENPC) or Pediatric Advanced Life Support (PALS), and role orientation with trauma services. c) Full-time employee or regularly scheduled part-time Emergency Department (ED) nurse. d) RN must have 6 months of LMH ED experience. 2) Trauma Control Duties: a) Inspects and stocks trauma room at beginning of each shift and after each trauma patient is discharged from the ED. b) Attempts to maintain trauma room temperature at 80-82 degrees Fahrenheit. c) Communicates with pre-hospital personnel to obtain patient information and prior field treatment and response. d) Makes determination that a patient meets Type I or Type II criteria and immediately notifies LMH’s Call System to initiate the Trauma Activation System. e) Assists physician with orders as directed. f) Acts as liaison with patient’s family/law enforcement/emergency medical services (EMS)/flight crews. -

Chapter 42 – Facial Trauma
CrackCast Show Notes – Facial Trauma– September 2016 www.canadiem.org/crackcast Chapter 42 – Facial Trauma Episode Overview: 1) Describe the anatomy of the bones, glands, and ducts of the face. At what ages do the sinuses appear? 2) List 5 types of facial fractures. 3) Describe the clinical presentation and associated radiographic findings of an orbital blowout fracture. 4) Describe an orbital tripod fracture and its management. 5) List the indications for antibiotics in a patient with facial trauma? 6) What is the importance of perioral electrical burns? 7) What are the indications for specialist repair of an eyelid laceration? 8) Describe the classification and management of dental fractures. a. What is the management of an avulsed tooth? b. What is a luxed tooth? How is it managed? c. What is an alveolar ridge fracture? 9) Describe the method for reducing a jaw dislocation? What is the usual direction of the dislocation? Rosen’s in Perspective mechanism of facial trauma varies significantly age highly associated with alcohol use o 49% of maxillofacial trauma was ETOH related in one study . Of these, 78% were related to violence and assaults, and 13% to motor vehicle collisions. other common mechanisms include falls, animal bites, sports, and flying debris. much more common in unprotected vehicle users such as ATVs and motorcycles o 32% of injured ATV riders will have facial injuries. facial injury in these patients correlates with injury severity score children < 17 years old, sports injuries are the largest source of facial injuries (20%) children < 6 years old most commonly suffer facial injuries from family pets such as dogs in young children the face is the most common location of trauma associated with abuse. -

Airway – Oropharyngeal: Insertion; Maintenance; Suction; Removal
Policies & Procedures Title: AIRWAY – OROPHARYNGEAL: INSERTION; MAINTENANCE; SUCTION; REMOVAL I.D. Number: 1159 Authorization Source: Nursing Date Revised: September 2014 [X] SHR Nursing Practice Committee Date Effective: October 2002 Date Reaffirmed: January 2016 Scope: SHR Acute, Parkridge Centre Any PRINTED version of this document is only accurate up to the date of printing 30-May-16. Saskatoon Health Region (SHR) cannot guarantee the currency or accuracy of any printed policy. Always refer to the Policies and Procedures site for the most current versions of documents in effect. SHR accepts no responsibility for use of this material by any person or organization not associated with SHR. No part of this document may be reproduced in any form for publication without permission of SHR. 1. PURPOSE 1.1 To safely and effectively use Oropharyngeal Airway (OPA). 2. POLICY 2.1 The Registered Nurse (RN), Registered Psychiatric Nurse (RPN), Licensed Practical Nurse (LPN), Graduate Nurse (GN), Graduate Psychiatric Nurse (GPN), Graduate Licensed Practical Nurse (GLPN) will insert, maintain, suction and remove an oropharyngeal airway (OPA). 2.2 The OPA may be inserted to establish and assist in maintaining a patent airway. 2.3 An OPA should only be used in patients with decreased level of consciousness or decreased gag reflex. 2.4 Patients with OPAs that have been inserted for airway protection should not be left unattended due to risk of aspiration if gag reflex returns unexpectedly. Page 1 of 4 Policies and Procedures: Airway – Oropharyngeal: Insertion; Maintenance; I.D. # 1159 Suction; Removal 3. PROCEDURE 3.1 Equipment: • Oropharyngeal airway of appropriate size • Tongue blade (optional) • Clean gloves • Optional: suction equipment, bag-valve-mask device 3.2 Estimate the appropriate size of airway by aligning the tube on the side of the patient’s face parallel to the teeth and choosing an airway that extends from the ear lobe to the corner of the mouth. -

Strategies to Support the COVID-19 Response in Lmics a Virtual Seminar Series Screening, Triage and Patient Flow
Strategies to support the COVID-19 response in LMICs A virtual seminar series Screening, Triage and Patient Flow Bhakti Hansoti, MBChB, MPH, PhD - Associate Professor in Emergency Medicine, Johns Hopkins University OBJECTIVES 1. Clinical Features 2. Preparing the Department 3. Initial Management 4. Other Management Considerations 5. Summary Clinical Features Severity • Most people with COVID-19 develop mild or uncomplicated illness • Approximately 14% develop severe disease requiring hospitalization and oxygen support • 5% require admission to an intensive care unit • In severe cases, COVID-19 can be complicated by • Acute respiratory disease syndrome (ARDS) • Sepsis and septic shock • Multiorgan failure, including acute kidney injury and cardiac injury. Preparing the Department Elements to be assessed have been divided into the following areas: • Establishment of a core team and key internal and external contact points • Human, material and facility capacity • Communication and data protection • Hand hygiene, personal protective equipment (PPE), and waste management • Triage, first contact and prioritization • Patient placement, moving of the patients in the facility, and visitor access • Environmental cleaning https://www.ecdc.europa.eu/en/publications-data/checklist- hospitals-preparing-reception-and-care-coronavirus-2019-covid-19 Split flow Protecting Yourself These videos can help with PPE donning and doffing technique: • Donning and doffing PPE https://www.youtube.com/watch?v=I94l IH8xXg8 • Recommended PPE during care https://www.youtube.com/watch?v=oPL -

Emergency Medical Services Program Policies – Procedures – Protocols
Emergency Medical Services Program Policies – Procedures – Protocols Protocols Table of Contents GENERAL PROVISIONS ................................................................................................ 3 DESTINATION DECISION SUMMARY-METRO BAKERSFIELD AREA ........................ 5 DETERMINATION OF DEATH ..................................................................................... 12 101 AIRWAY OBSTRUCTION ...................................................................................... 16 102 ALTERED LEVEL OF CONSCIOUSNESS ............................................................ 18 103 ALLERGIC REACTION/ANAPHYLAXIS ................................................................ 20 104 ASYSTOLE/ PULSELESS ELECTRICAL ACTIVITY ............................................. 22 105 BITES STINGS ENVENOMATION ......................................................................... 24 106 BRADYCARDIA ..................................................................................................... 26 107 BRIEF RESOLVED UNEXPLAINED EVENT ......................................................... 29 108 BURNS ................................................................................................................... 32 109 CHEMPACK ........................................................................................................... 35 110 CHEST PAIN OR ACUTE CORONARY SYNDROME ........................................... 37 111 CHEST TRAUMA .................................................................................................. -

High Performance CPR Update
High Performance CPR Update Page | 1 Final Revision 8/8/2012 As part of our ongoing Quality Assurance in Cardiac Arrest incidents, Skagit County EMS under the direction of Dr. Don Slack, MPD is making changes to the way that ALS and BLS providers perform CPR. Overview: CPR quality has a dramatic impact on pt survival when done according to these guidelines. Minimal breaks in compressions, full chest recoil, adequate compression depth and adequate compression rate are all components of CPR that an increase survival from sudden cardiac arrest. Together these components go together to create High Performance CPR (HP CPR). Roles: As a rule for the unconscious, unresponsive, pulseless patient the FIRST person to the patient starts compressions. SECOND person does defibrillation (If there are only 2 responders to begin with, ventilations should begin after the rhythm analysis and shock if indicated). THIRD person should start ventilating the patient, placing a King Airway as soon as is practical. A timekeeper needs to be assigned to ensure high quality CPR, minimal interruption and help track the ALS interventions. Principles of HP CPR 1. EMT’s own CPR!! 2. Minimize interruption in CPR at all times, use a timekeeper 3. Ensure proper depth of compressions (>2 inches) 4. Ensure full chest recoil/decompression 5. Ensure proper chest compression rate (100-120/min) 6. Rotate compressors at least every 2 minutes 7. Do not interrupt compressions to ventilate patient, even if an advanced airway is not placed 8. Hands off the chest only during analysis and shock delivery, hover hands over chest during shock delivery and be ready to resume compressions 9. -

Small Adult CPR-2 Bag with Litesaver Manometer Brochure
ORDERING INFORMATION Your Need ... Our Innovation® O Manometer 2 Detector 2 AerosolTubing Reservoir Infant Cushion Mask Expandable Large Bore Color-Coded Mask PEEP w/Filter StatCO Manometer LiteSaverTiming Light with CPR (Synthetic Rubber) CPR-2 (PVC) Light Blue Oxygen Bag Reservoir (22mm) Adult Cushion Mask SmallAdult Cushion Mask with Flange #3 Pediatric Cushion Mask Child Cushion Mask PEEP Valve Pop-Off Dark Blue Oxygen Reservoir 0-60 cm H PART # OTHER #10-56402 X X X X X X #10-56403 X X X X #10-56404 X X X X X #10-56411 X X X X #10-56412 X X X X X #10-56423 X X X X X X #10-56424 X X X X X X CPR-2 Small Adult Bag with Manometer #10-56432 X X X X X #10-56435 X X X X X X X #10-56437 X X X X #10-56438 X X X X X #10-56440 X X X X #10-58500 X X X X #10-58501 X X X X X #10-58502 X X X X X #10-58503 X X X X X X #10-58506 X X X X X X #10-58507 X X X X X #10-58509 X X X X X #10-58512 X X X X X X X #10-55901 X X X #10-55904 X X X #10-55907 X X X #10-55909 X X X X #10-55910 X X X X #10-55912 X X X #10-55913 X X X X X X No lock clip #10-55915 X X X X X #10-55916 X X X #10-55917 X X X X X #10-55918 X X X X X X #10-55922 X X X X X X X #10-55923 X X X X #10-55924 X X X X X #10-55928 X X X #10-58400 X X X X #10-55365 LiteSaver Manometer Assy 20/Box 0-60 cm H2O, Adult Frequency 10 BPM #10-55366 LiteSaver Manometer Assy 20/Box Assembly 0-60 cm H2O In-Line Tee Right Orientation, Adult Frequency 10 BPM #10-55367 LiteSaver Manometer Assy 20/Box Assembly 0-60 cm H2O In-Line Tee Left Orientation, Adult Frequency 10 BPM = CPR-2 Small Adult Bags *References Can EMS Providers Provide Appropriate Tidal Volumes in a Simulated Adult-sized Patient with a Pediatric-sized Bag-Valve-Mask? Journal Pre-hospital Emergency Care, Volume 21, 2017, Issue 1, Jeffery Siegler, MD, EMT-P, Melissa Kroll, MD, Susan Wojcik, PhD, ATC & Hawnwan Philip May, MD Avoid Airway Catastrophes on the Extremes of Minute Ventilation, Acepnow.com, January 20, 2015, Richard M. -
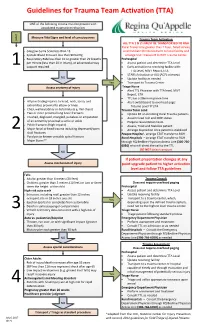
Guidelines for Trauma Team Activation (TTA)
Guidelines for Trauma Team Activation (TTA) ONE of the following criteria must be present with associated traumatic mechanism L e v e Measure Vital Signs and level of consciousness l Trauma Team Activation ALL TTA 1 & 2's MUST BE TRANSPORTED TO RGH Rural Travel time greater than 1 hour, failed airway · Glasgow Coma Scale less than 13 or immediate life threat divert to local facility and · Systolic Blood Pressure less than 90mmHg arrange STAT transport to RGH Trauma Center · Respiratory Rate less than 10 or greater then 29 breaths Prehospital per minute (less than 20 in infant), or advanced airway · Assess patient and determine TTA Level 1 support required · Early activation to receiving facility with: TTA Level, MIVT Report, ETA · STARS Activation or ALS (ACP) intercept NO · Update facility as needed Yes · Transport to Trauma Center Assess anatomy of injury Triage Nurse · Alert TTL Physician with TTA level, MIVT Report, ETA · TTL has a 20min response time · All penetrating injuries to head, neck, torso, and · Alert switchboard to overhead page: extremities proximal to elbow or knee Trauma Level ‘#’ ETA · Chest wall instability or deformity (e.g. flail chest) Trauma Team Lead · Two or more proximal long-bone fractures · Update ER on incoming Rural Trauma patients · Crushed, degloved, mangled, pulseless or amputation · Assume lead role and MRP status of an extremity proximal to wrist or ankle · Prepare resuscitation team · Pelvic fractures (high impact) · Assess, Treat and Stabilize patient 2 · Major facial or head trauma including depressed/open -

Capnography (ILS/ALS)
Capnography (ILS/ALS) Clinical Indications: 1. Capnography shall be used as soon as possible in conjunction with any airway management adjunct, including endotracheal, Blind Insertion Airway Devices (BIAD) or Bag Valve Mask (BVM). 2. Capnography should also be used on all patients treated with CPAP or epinephrine for respiratory distress. 3. Acute respiratory distress. 4. Assisted ventilations. 5. Sustained altered mental status. Procedure: 1. Attach capnography sensor to the BIAD, endotracheal tube, or oxygen delivery device. 2. Note CO2 level and waveform changes. These will be documented on each respiratory failure, cardiac arrest, or respiratory distress patient. 3. The capnometer shall remain in place with the airway and be monitored throughout the prehospital care and transport. 4. Any loss of CO2 detection or waveform indicates an airway problem and should be documented. 5. The capnogram should be monitored as procedures are performed to verify or correct the airway problem. 6. Document the procedure and results on/with the Patient Care Report (PCR) and the Airway Evaluation Form. 7. In all patients with a pulse, an ETCO2 >20 is anticipated. In the post-resuscitation patient, no effort should be made to lower ETCO2 by modification of the ventilatory rate. Further, in post- resuscitation patients without evidence of ongoing, severe bronchospasm, ventilatory rate should never be < 6 breaths per minute. 8. In the pulseless patient, and ETCO2 waveform with an ETCO2 value >10 may be utilized to confirm the adequacy of an airway to include BVM and advanced devices when Sp02 will not register. Critical Comment: • When CO2 is NOT detected, three factors must be quickly assessed : 1. -

ABBREVIATION LIST ALOC Altered Level of Consciousness ABC's Airway, Breathing, Circulation ACLS Advanced Cardiac Life Suppo
ABBREVIATION LIST ALOC Altered Level of Consciousness ABC’s Airway, Breathing, Circulation ACLS Advanced Cardiac Life Support AED Automatic External Defibrillator AICD Automatic Implantable Cardiac Defibrillator ALS Advanced Life Support AMI Acute Myocardial Infarction AMS Altered Mental Status AMR American Medical Response ASA Aspirin AV Atrial Ventricular BHPC Base Hospital Physician Contact BLS Basic Life Support BP Blood Pressure bpm Beats Per Minute BSI Body Substance Isolation BVM Bag Valve Mask CaCl Calcium Chloride CC Chief Complaint C-spine Cervical Spine CHF Congestive Heart Failure COPD Chronic Obstructive Pulmonary Edema CPR Cardiopulmonary Resuscitation CVA Cerebral Vascular Accident D12.5%W Dextrose 12.5% in water D50%W Dextrose 50% in water DKA Diabetic Ketoacidosis DM Diabetes Mellitus DNR Do Not Resuscitate ED Emergency Department EKG Electrocardiogram EMS Emergency Medical Services Epi Epinephrine ET Endotracheal Tube ETT Endotracheal Tube gm Gram GCS Glasgow Coma Scale HazMat Hazardous Materials HEENT Head, Eyes, Ears, Nose, Throat HTN Hypertension IO Interosseous IM Intramuscular ITLS International Trauma Life Support IV Intravenous IVP Intravenous Push (IV push prefed) kg Kilogram San Mateo County EMS Agency Introduction Abbreviation List 2008 Page 1 of 3 J Joule LOC Loss of Consciousness Max Maximum mcg Microgram meds Medication mEq Milliequivalent min Minute mg Milligram MI Myocardial Infarction mL Milliliter MVC Motor Vehicle Collision NPA Nasopharyngeal Airway NPO Nothing Per Mouth NS Normal Saline NT Nasal Tube NTG Nitroglycerine NS Normal Saline O2 Oxygen OB Obstetrical OD Overdose OPA Oropharyngeal Airway OPQRST Onset, Provoked, Quality, Region and Radiation, Severity, Time OTC Over the Counter PAC Premature Atrial Contraction PALS Pediatric Advanced Life Support PEA Pulseless Electrical Activity PHTLS Prehospital Trauma Life Support PID Pelvic Inflammatory Disease PO By Mouth Pt. -

Approach to the Trauma Patient Will Help Reduce Errors
The Approach To Trauma Author Credentials Written by: Nicholas E. Kman, MD, The Ohio State University Updated by: Creagh Boulger, MD, and Benjamin M. Ostro, MD, The Ohio State University Last Update: March 2019 Case Study “We have a motor vehicle accident 5 minutes out per EMS report.” 47-year-old male unrestrained driver ejected 15 feet from car arrives via EMS. Vital Signs: BP: 100/40, RR: 28, HR: 110. He was initially combative at the scene but now difficult to arouse. He does not open his eyes, withdrawals only to pain, and makes gurgling sounds. EMS placed a c-collar and backboard, but could not start an IV. What do you do? Objectives Upon completion of this self-study module, you should be able to: ● Describe a focused rapid assessment of the trauma patient using an organized primary and secondary survey. ● Discuss the components of the primary survey. ● Discuss possible pathology that can occur in each domain of the primary survey and recommend treatment/stabilization measures. ● Describe how to stabilize a trauma patient and prioritize resuscitative measures. ● Discuss the secondary survey with particular attention to head/central nervous system (CNS), cervical spine, chest, abdominal, and musculoskeletal trauma. ● Discuss appropriate labs and diagnostic testing in caring for a trauma patient. ● Describe appropriate disposition of a trauma patient. Introduction Nearly 10% of all deaths in the world are caused by injury. Trauma is the number one cause of death in persons 1-50 years of age and results in significant life years lost. According to the National Trauma Data Bank, falls were the leading cause of trauma followed by motor vehicle collisions (MVCs) and firearm related injuries with an overall mortality rate of 4.39% in 2016.