Chapter 1 - Trauma Team from Prehospital Through the Emergency Department Test Questions
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Emergency Medicine – Trauma: What You Need to Know Whiteboard Animation Transcript with Kaushal Shah, MD
Emergency Medicine – Trauma: What You Need to Know Whiteboard Animation Transcript with Kaushal Shah, MD Trauma comes in two basic varieties: blunt trauma and penetrating trauma. Nonetheless, major trauma patients should always be approached the same way: primary survey followed by a secondary survey. Don’t let the blood and gore distract you. The primary survey entails a systematic assessment using ABCDE in order to identify the true life-threatening injuries and initiate resuscitation. Then a detailed head-to-toe exam should occur, which we call the secondary survey. A. Airway assessment. If blood, vomit or the patient’s own saliva is blocking the airway (which often occurs in unconscious patients), they will need suctioning and possibly intubation. B. Breathing. Examine the chest through inspection, auscultation, and palpation. You are looking for life-threatening injuries. Decreased breath sounds, subcutaneous emphysema, broken ribs, and tracheal deviation, are concerning for a tension pneumothorax, hemothorax, pulmonary contusions, flail chest, and cardiac tamponade. C. Circulation. If the patient has a fast heart rate or low blood pressure, suspect ongoing hemorrhage or blood loss, the number one cause of preventable death in trauma. Bleeding is likely in one of four locations: chest, abdomen, pelvis, or fractured long bones. Start IV fluids or blood transfusion through two big intravenous lines. D. Disability. A basic neurologic assessment will help you calculate a GCS or Glasgow Coma Scale. It evaluates Eye Opening, Verbal Response, and Motor Response that is universally understood on a 15-point scale. E. Exposure. The patient should be completely undressed to look for all injuries. -

Title: ED Trauma: Trauma Nurse Clinical Resuscitation
Title: ED Trauma: Trauma Nurse Clinical Resuscitation Document Category: Clinical Document Type: Policy Department/Committee Owner: Practice Council Original Date: Approved By (last review): Director of Emergency Services, Approval Date: 07/28/2014 Trauma Medical Director, Medical Director Emergency (Complete history at end of document.) Services POLICY: To provide immediate, effective and efficient patient care to the trauma patient, designated nursing staff will respond to the trauma room when a trauma page is received. TRAUMA CONTROL NURSE: 1) Role: a) The trauma control nurse (TCN) is a registered nurse (RN) with specialized training in the care of the traumatized patient, and who will function as the trauma team’s lead nurse. b) The TCN shall have successfully completed the Trauma Nurse Core Course (TNCC), Advanced Cardiac Life Support (ACLS), Emergency Nurse Pediatric Course (ENPC) or Pediatric Advanced Life Support (PALS), and role orientation with trauma services. c) Full-time employee or regularly scheduled part-time Emergency Department (ED) nurse. d) RN must have 6 months of LMH ED experience. 2) Trauma Control Duties: a) Inspects and stocks trauma room at beginning of each shift and after each trauma patient is discharged from the ED. b) Attempts to maintain trauma room temperature at 80-82 degrees Fahrenheit. c) Communicates with pre-hospital personnel to obtain patient information and prior field treatment and response. d) Makes determination that a patient meets Type I or Type II criteria and immediately notifies LMH’s Call System to initiate the Trauma Activation System. e) Assists physician with orders as directed. f) Acts as liaison with patient’s family/law enforcement/emergency medical services (EMS)/flight crews. -
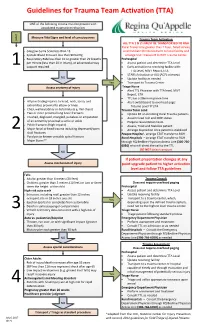
Guidelines for Trauma Team Activation (TTA)
Guidelines for Trauma Team Activation (TTA) ONE of the following criteria must be present with associated traumatic mechanism L e v e Measure Vital Signs and level of consciousness l Trauma Team Activation ALL TTA 1 & 2's MUST BE TRANSPORTED TO RGH Rural Travel time greater than 1 hour, failed airway · Glasgow Coma Scale less than 13 or immediate life threat divert to local facility and · Systolic Blood Pressure less than 90mmHg arrange STAT transport to RGH Trauma Center · Respiratory Rate less than 10 or greater then 29 breaths Prehospital per minute (less than 20 in infant), or advanced airway · Assess patient and determine TTA Level 1 support required · Early activation to receiving facility with: TTA Level, MIVT Report, ETA · STARS Activation or ALS (ACP) intercept NO · Update facility as needed Yes · Transport to Trauma Center Assess anatomy of injury Triage Nurse · Alert TTL Physician with TTA level, MIVT Report, ETA · TTL has a 20min response time · All penetrating injuries to head, neck, torso, and · Alert switchboard to overhead page: extremities proximal to elbow or knee Trauma Level ‘#’ ETA · Chest wall instability or deformity (e.g. flail chest) Trauma Team Lead · Two or more proximal long-bone fractures · Update ER on incoming Rural Trauma patients · Crushed, degloved, mangled, pulseless or amputation · Assume lead role and MRP status of an extremity proximal to wrist or ankle · Prepare resuscitation team · Pelvic fractures (high impact) · Assess, Treat and Stabilize patient 2 · Major facial or head trauma including depressed/open -

Effect of Hypothermia on Haemostasis and Bleeding Risk: a Narrative Review
Review Journal of International Medical Research 2019, Vol. 47(8) 3559–3568 Effect of hypothermia on ! The Author(s) 2019 Article reuse guidelines: haemostasis and bleeding sagepub.com/journals-permissions DOI: 10.1177/0300060519861469 risk: a narrative review journals.sagepub.com/home/imr Thomas Kander and Ulf Schott€ Abstract It must be remembered that clinically important haemostasis occurs in vivo and not in a tube, and that variables such as the number of bleeding events and bleeding volume are more robust measures of bleeding risk than the results of analyses. In this narrative review, we highlight trauma, surgery, and mild induced hypothermia as three clinically important situations in which the effects of hypothermia on haemostasis are important. In observational studies of trauma, hypothermia (body temperature <35C) has demonstrated an association with mortality and morbidity, perhaps owing to its effect on haemostatic functions. Randomised trials have shown that hypothermia causes increased bleeding during surgery. Although causality between hypothermia and bleeding risk has not been well established, there is a clear association between hypothermia and negative outcomes in connection with trauma, surgery, and accidental hypothermia; thus, it is crucial to rewarm patients in these clinical sit- uations without delay. Mild induced hypothermia to 33C for 24 hours does not seem to be associated with either decreased total haemostasis or increased bleeding risk. Keywords Hypothermia, coagulopathy, haemostasis, bleeding, trauma, surgery, injury Date received: 20 March 2019; accepted: 13 June 2019 Introduction Many studies have been conducted to inves- Lund University, Ska˚ne University Hospital, Department tigate the effects of hypothermia on haemo- of Clinical Sciences Lund, Intensive and Perioperative stasis, and these have yielded contradictory Care, Lund, Sweden results. -

Anytown Trauma Center Trauma Protocols
ANYTOWN TRAUMA CENTER TRAUMA PROTOCOLS TITLE: TRAUMA TEAM ACTIVATION PROTOCOL PURPOSE: The purpose of the protocol is to establish guidelines for trauma team activation and define the members of the responding trauma team to facilitate the resuscitation and management of critical or seriously injured patients who require rapid, organized resuscitation, evaluation and stabilization to promote optimal outcomes. It also serves to provide triage guidelines for adult and pediatric patients. PROCESS: 1. TRAUMA TEAM ACTIVATION PROTCOL A. The criteria for activation of the trauma team is clearly defined and posted at the Emergency Department triage desk, by the EMS communication station and in the resuscitation rooms. B. The trauma team may be activated prior to arrival based on the EMS communication and their assessment. C. The trauma surgeon, emergency medicine physician, emergency department charge nurse/ house supervisor, emergency department nurses and the Trauma Program Manager may activate the trauma team. D. The person calling the trauma activation will initiate the trauma page to group page the trauma team and will specify the MOI, BP, HR, ETA and level of activation required and age if available. E. If the trauma team members are present in the emergency department and alert is still communicated to ensure everyone is notified. F. Trauma team member notification and arrival times will be documented on the trauma flow sheet (paper or electronic). G. Trauma team members will sign-in when they arrive. H. Trauma team members will be activated for all patients who meet the following criteria: 1. Level 1 trauma activation (major): life threatening injuries and/or unstable vital signs, limb-threating or disability threatening injury 2. -

EDUCATION STANDARDS Tabe of Contents
2020 NATIONAL EMERGENCY MEDICAL SERVICES EDUCATION STANDARDS Tabe of Contents Executive Summary 4 Pathophysiology X Introduction X Life Span Development X Historical Development of EMS in the United States X The National EMS Education Standards X Public Health X Description, Explanation, and Rationale Related to the Update X Pharmacology X 2019 National EMS Scope of Practice Model Relationship X Principles of Pharmacology X NREMT Practice Analysis X Medication Administration X Domains of EMS: Learning, Competency, Authorization, and X Emergency Medications X Operational/Local Qualification X Education Standards vs. Instructional Guidelines vs. Curriculum X Airway Management, Respirations and Artificial Ventilation X What Are the Instructional Guidelines: X Airway Management X Beyond the Scope of the Project X Respiration X Degree Requirements X Artificial Ventilation X AEMT Accreditation X Portable Technologies X Assessment X Instructional Practices: X Scene Size-Up X Interprofessional Education, Simulation, Shadowing X Primary Assessment X Team Composition X History Taking X Sequence of Instruction X Secondary Assessment X Locally Identified Topics X Monitoring Devices X Implicit Expectations X Reassessment X Resource Documents/Appendix X Evidence Based Guidelines – NASEMSO Clinical Guidelines X Medicine X Education Standards with Noteworthy Adjustment X Medical Overview X Neurology X National EMS Education Standards X Abdominal and Gastrointestinal Disorders X Preparatory X Immunology X EMS Systems X Infectious Diseases X Research X -

Staged Abdominal Re-Operation for Abdominal Trauma
TJTES Ulus Travma Derg. 2003 Jul;9(3):149-153 TURKISH JOURNAL OF TRAUMA & EMERGENCY SURGERY STAGED ABDOMINAL RE-OPERATION FOR ABDOMINAL TRAUMA Korhan TAVILOGLU, MD, FACS ABSTRACT Background: To review the current developments in staged abdominal re-operation for abdominal trauma. Methods: To overview the steps of damage control laparotomy. Results: The ever increasing importance of the resuscitation phase with current intensive care unit (ICU) support techniques should be emphasized. Conclusions: General surgeons should be familiar to staged abdominal re-operation for abdominal trauma and collaborate with ICU teams, interventional radiologists and several other specialties to overcome this entity. Key words: abdominal trauma, staged laparotomy, abdominal compartment syndrome, damage control surgery INTRODUCTION Feliciano et al.12 reported the survival in nine of ten During the past decade, a new surgical patients who underwent temporary laparotomy approach to patients with devastating trauma has with pad tamponade for hepatic injuries. In the emerged. Based on a modified operative beginning of the 1980’s, two studies reported sequence using rapid lifesaving techniques, abdominal packing followed by rapid abdominal definitive resection and reconstruction are closure that was used for treatment of delayed until the patient can be adequately coagulopathy of nonhepatic abdominal injuries. resuscitated and stabilized in the surgical intensive care unit.1-5 WHAT IS STAR? Damage control is currently the most common STAR is a technique of serial -
General Approach to Traumatic Injuries
Cambridge University Press 978-1-108-45028-7 — The Emergency Medicine Trauma Handbook Edited by Alex Koyfman , Brit Long Excerpt More Information Chapter General Approach to 1 Traumatic Injuries Ryan O’Halloran and Kaushal Shah Introduction Trauma is the fourth leading cause of death overall in the United States and the number one cause of death for ages 1 to 44 – second only to heart disease and cancer in those older than 45 (CDC).1 As the disease burden from infectious diseases declines and secondary preven- tion of chronic conditions improves, the relative importance of the practice of trauma care becomes even more apparent. Though safety engineering has improved across many indus- tries (one need only consider examples such as crosswalk and bike lane planning, football helmet technology, and motor vehicle computerized improvements), trauma remains a significant threat to life and limb in emergency medicine. The Trauma Team The American College of Surgeons, the governing body for credentialing trauma centers, has provided guidelines for optimal resources necessary for a coordinated response to a critically injured trauma patient. Box 1.1 demonstrates the players suggested for an optimal response. While response teams may vary, several principles are key to the functioning of a good, interdisciplinary team. These include clearly establishing roles for members of the team, following policy and protocols established in advance, briefing prior to the arrival of the patient, and debriefing after the event, whether immediately after the event -

Basic Trauma Overview - ABC
Basic Trauma Overview - ABC Dale Dangleben, MD, FACS 1 2 Team 3 Extended Team 4 Team Leader Decrease chaos / optimize care. – Remains calm – Maintains control and provides direction – Stays decisive – Sees the big picture (situational awareness) – Is open to other team members input – Directs resuscitation – Makes early decision to transfer the patients that exceed the local capabilities 5 Team Members − Know your roles in the trauma team − Remain calm − Be responsive to team leader −Voice suggestions or concerns 6 Responsibilities – Perform the Primary and secondary survey – Verbalize patient care – Report completed tasks 7 Responsibilities – Monitors the patient – Manual BP – Obtains IV access – Administers medications – Dresses wounds – Performs or assists in resuscitative procedures 8 Responsibilities Records data Ensures documentation accompanies patient upon transfer Assists team members as needed 9 Responsibilities – Obtains needed supplies – Coordinates communication with local and external resources – Assists team members as needed 10 Responsibilities • Place Oxygen on patient • Manage airway • Hold C spine • Manage ventilator if • Manage rapid infuser line patient intubated where indicated • Assists team members as needed 11 Organization of trauma resuscitation area – Basic adult and pediatric equipment for: • Airway management (cart) • IV access with warm fluids • Chest tube insertion • Hemorrhage control (tourniquets, pelvic binders) • Immobilization • Medications • Pediatric length/weight based tape (Broselow Tape) – Warming -

Early Acute Management in Adults with Spinal Cord Injury: a Clinical Practice Guideline for Health-Care Professionals
SPINAL CORD MEDICINE EARLY ACUTE EARLY MANAGEMENT Early Acute Management in Adults with Spinal Cord Injury: A Clinical Practice Guideline for Health-Care Professionals Administrative and financial support provided by Paralyzed Veterans of America CLINICAL PRACTICE GUIDELINE: Consortium for Spinal Cord Medicine Member Organizations American Academy of Orthopaedic Surgeons American Academy of Physical Medicine and Rehabilitation American Association of Neurological Surgeons American Association of Spinal Cord Injury Nurses American Association of Spinal Cord Injury Psychologists and Social Workers American College of Emergency Physicians American Congress of Rehabilitation Medicine American Occupational Therapy Association American Paraplegia Society American Physical Therapy Association American Psychological Association American Spinal Injury Association Association of Academic Physiatrists Association of Rehabilitation Nurses Christopher and Dana Reeve Foundation Congress of Neurological Surgeons Insurance Rehabilitation Study Group International Spinal Cord Society Paralyzed Veterans of America Society of Critical Care Medicine U. S. Department of Veterans Affairs United Spinal Association CLINICAL PRACTICE GUIDELINE Spinal Cord Medicine Early Acute Management in Adults with Spinal Cord Injury: A Clinical Practice Guideline for Health-Care Providers Consortium for Spinal Cord Medicine Administrative and financial support provided by Paralyzed Veterans of America © Copyright 2008, Paralyzed Veterans of America No copyright ownership -

Zone 1 Vascular Abdominal Trauma. Damage Control and Staged Management
Review Article Clinics in Surgery Published: 12 Feb, 2018 Zone 1 Vascular Abdominal Trauma. Damage Control and Staged Management Ioannis Stamatatos1*, Marigo Theodorou2, Efstathios Metaxas3, Dimitrios Klapsakis4, Konstantinos Bouboulis2,3, Nikolaos Tzatzadakis3 and Athanasios Rogdakis2 1Department of Vascular and Endovascular Surgery, General Hospital Nikaia, Greece 2Department of General Surgery, General Hospital Nikaia, Greece 3Department of Cardiothoracic Surgery, General Hospital Nikaia, Greece 4Department of Orthopaedics and Trauma, General Hospital Nikaia, Greece Abstract Vascular abdominal injuries of major vessels in zone 1 abdominal cavity are the most common cause of death after penetrating abdominal trauma. Abdominal arterial and vein injuries occur with the same incidence. Patients with retroperitoneal vascular injury and intact retroperitoneum may present hemodynamically stable due to tamponade. The main goal of staged approach is to control any major haemorrhage into the abdomen until the patient is hemodynamically stabilized in the ICU and reconstruction can be done in final reoperation. Multidisciplinary management is imperative to prevent the “lethal triad” and assures the best optimal outcome for these critically wounded patients. Introduction Abdominal vascular injuries are the most common cause of death after penetrating abdominal trauma. Blunt injuries to major abdominal vessels are rare. Major injuries to large vessels in the abdominal zone 1 usually cause significant hemoperitoneum and shock. The type of clinical presentation varies widely and depends on the presence of retroperitoneal tamponade. Patients with an intact retroperitoneum may be hemodynamically stable on presentation but when the OPEN ACCESS retroperitoneum tamponade is lost, signs of shock and acute hypovolemia are present. Many patients with major abdominal vascular injuries require massive blood transfusions, are hypotensive, *Correspondence: and become severely hypothermic, acidotic, and coagulopathic intra operatively. -

Autologous Transfusion of Shed Pleural Blood in Trauma - a Register Study to Determine Applicability
Sahlgrenska academy Autologous transfusion of shed pleural blood in trauma - a register study to determine applicability Degree Project in Medicine Henrik Örtenwall Programme in Medicine, The Sahlgrenska Academy Gothenburg, Sweden, 2021 Supervisors: Dr. Ragnar Ang, trauma surgeon, SU Doc. Jenny Skytte-Larsson, anesthesiologist, FömedC Table of contents Abbreviations ............................................................................................................................. 3 Abstract ...................................................................................................................................... 4 Introduction ................................................................................................................................ 5 Aim ............................................................................................................................................. 6 Background ................................................................................................................................ 6 History ................................................................................................................................................. 6 Transfusion guidelines ........................................................................................................................ 9 Pros and cons of allogenic blood component transfusion ................................................................. 10 Pros and cons of autologous whole blood transfusion .....................................................................