Digestive Glands
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Te2, Part Iii
TERMINOLOGIA EMBRYOLOGICA Second Edition International Embryological Terminology FIPAT The Federative International Programme for Anatomical Terminology A programme of the International Federation of Associations of Anatomists (IFAA) TE2, PART III Contents Caput V: Organogenesis Chapter 5: Organogenesis (continued) Systema respiratorium Respiratory system Systema urinarium Urinary system Systemata genitalia Genital systems Coeloma Coelom Glandulae endocrinae Endocrine glands Systema cardiovasculare Cardiovascular system Systema lymphoideum Lymphoid system Bibliographic Reference Citation: FIPAT. Terminologia Embryologica. 2nd ed. FIPAT.library.dal.ca. Federative International Programme for Anatomical Terminology, February 2017 Published pending approval by the General Assembly at the next Congress of IFAA (2019) Creative Commons License: The publication of Terminologia Embryologica is under a Creative Commons Attribution-NoDerivatives 4.0 International (CC BY-ND 4.0) license The individual terms in this terminology are within the public domain. Statements about terms being part of this international standard terminology should use the above bibliographic reference to cite this terminology. The unaltered PDF files of this terminology may be freely copied and distributed by users. IFAA member societies are authorized to publish translations of this terminology. Authors of other works that might be considered derivative should write to the Chair of FIPAT for permission to publish a derivative work. Caput V: ORGANOGENESIS Chapter 5: ORGANOGENESIS -

Classical Liver (Hepatic) Lobules It Is Formed of a Polygonal Mass of A- Capsule: Glisson’S Capsule
LIVER & SPLEEN Color index: Slides.. Important ..Notes ..Extra.. Objectives: By the end of this lecture, the student should be able to describe: 1. The histological structure of liver with special emphasis on: . Classical hepatic (liver) lobule. Hepatocytes. Portal tract (portal area). Hepatic (liver) blood sinusoids. Space of Disse (perisinusoidal space of Disse) . Bile canalculi. 2. The histological structure of spleen with special emphasis on: . White pulp. Red Pulp. LIVER 1-Stroma; 2-Parenchyma; mainly C.T, but not in humans. Classical liver (hepatic) lobules It is formed of a polygonal mass of a- Capsule: Glisson’s Capsule. liver tissue, bounded by b- Septa (absent in human) interlobular septa with portal areas & Portal areas (Portal tracts) at the periphery & central Portal area: surrounded by (centrolobular) vein in the center. other structures. Central vein: surrounded by c- Network of reticular fibers. hepatocytes LIVER Contents of the Classic Liver Lobule: Borders of the Classical Liver Lobule the rows of hepatocytes should be next to each other; 1- Septa: C.T. septa (e.g. in pigs). remember canaliculi 2- Portal areas (Portal tracts): 1- Anastomosing plates of hepatocytes. Are located in the corners of the classical hepatic 2- Liver blood sinusoids (hepatic blood lobule (usually 3 in No.). sinusoids): between the plates. Contents of portal area: 3- Spaces of Disse (perisinusoidal spaces of a- C.T. b- Bile ducts (interlobular bile ducts). Disse) between the hepatocytes and sinusoids c- Venule (Branch of portal vein). 4- Central vein. d- Arteriole (Branch of hepatic artery). 5- Bile canaliculi. Hepatic artery: surrounded by smooth muscles while the bile duct is not. -

Vocabulario De Morfoloxía, Anatomía E Citoloxía Veterinaria
Vocabulario de Morfoloxía, anatomía e citoloxía veterinaria (galego-español-inglés) Servizo de Normalización Lingüística Universidade de Santiago de Compostela COLECCIÓN VOCABULARIOS TEMÁTICOS N.º 4 SERVIZO DE NORMALIZACIÓN LINGÜÍSTICA Vocabulario de Morfoloxía, anatomía e citoloxía veterinaria (galego-español-inglés) 2008 UNIVERSIDADE DE SANTIAGO DE COMPOSTELA VOCABULARIO de morfoloxía, anatomía e citoloxía veterinaria : (galego-español- inglés) / coordinador Xusto A. Rodríguez Río, Servizo de Normalización Lingüística ; autores Matilde Lombardero Fernández ... [et al.]. – Santiago de Compostela : Universidade de Santiago de Compostela, Servizo de Publicacións e Intercambio Científico, 2008. – 369 p. ; 21 cm. – (Vocabularios temáticos ; 4). - D.L. C 2458-2008. – ISBN 978-84-9887-018-3 1.Medicina �������������������������������������������������������������������������veterinaria-Diccionarios�������������������������������������������������. 2.Galego (Lingua)-Glosarios, vocabularios, etc. políglotas. I.Lombardero Fernández, Matilde. II.Rodríguez Rio, Xusto A. coord. III. Universidade de Santiago de Compostela. Servizo de Normalización Lingüística, coord. IV.Universidade de Santiago de Compostela. Servizo de Publicacións e Intercambio Científico, ed. V.Serie. 591.4(038)=699=60=20 Coordinador Xusto A. Rodríguez Río (Área de Terminoloxía. Servizo de Normalización Lingüística. Universidade de Santiago de Compostela) Autoras/res Matilde Lombardero Fernández (doutora en Veterinaria e profesora do Departamento de Anatomía e Produción Animal. -

Study Guide Medical Terminology by Thea Liza Batan About the Author
Study Guide Medical Terminology By Thea Liza Batan About the Author Thea Liza Batan earned a Master of Science in Nursing Administration in 2007 from Xavier University in Cincinnati, Ohio. She has worked as a staff nurse, nurse instructor, and level department head. She currently works as a simulation coordinator and a free- lance writer specializing in nursing and healthcare. All terms mentioned in this text that are known to be trademarks or service marks have been appropriately capitalized. Use of a term in this text shouldn’t be regarded as affecting the validity of any trademark or service mark. Copyright © 2017 by Penn Foster, Inc. All rights reserved. No part of the material protected by this copyright may be reproduced or utilized in any form or by any means, electronic or mechanical, including photocopying, recording, or by any information storage and retrieval system, without permission in writing from the copyright owner. Requests for permission to make copies of any part of the work should be mailed to Copyright Permissions, Penn Foster, 925 Oak Street, Scranton, Pennsylvania 18515. Printed in the United States of America CONTENTS INSTRUCTIONS 1 READING ASSIGNMENTS 3 LESSON 1: THE FUNDAMENTALS OF MEDICAL TERMINOLOGY 5 LESSON 2: DIAGNOSIS, INTERVENTION, AND HUMAN BODY TERMS 28 LESSON 3: MUSCULOSKELETAL, CIRCULATORY, AND RESPIRATORY SYSTEM TERMS 44 LESSON 4: DIGESTIVE, URINARY, AND REPRODUCTIVE SYSTEM TERMS 69 LESSON 5: INTEGUMENTARY, NERVOUS, AND ENDOCRINE S YSTEM TERMS 96 SELF-CHECK ANSWERS 134 © PENN FOSTER, INC. 2017 MEDICAL TERMINOLOGY PAGE III Contents INSTRUCTIONS INTRODUCTION Welcome to your course on medical terminology. You’re taking this course because you’re most likely interested in pursuing a health and science career, which entails proficiencyincommunicatingwithhealthcareprofessionalssuchasphysicians,nurses, or dentists. -

Basic Histology (23 Questions): Oral Histology (16 Questions
Board Question Breakdown (Anatomic Sciences section) The Anatomic Sciences portion of part I of the Dental Board exams consists of 100 test items. They are broken up into the following distribution: Gross Anatomy (50 questions): Head - 28 questions broken down in this fashion: - Oral cavity - 6 questions - Extraoral structures - 12 questions - Osteology - 6 questions - TMJ and muscles of mastication - 4 questions Neck - 5 questions Upper Limb - 3 questions Thoracic cavity - 5 questions Abdominopelvic cavity - 2 questions Neuroanatomy (CNS, ANS +) - 7 questions Basic Histology (23 questions): Ultrastructure (cell organelles) - 4 questions Basic tissues - 4 questions Bone, cartilage & joints - 3 questions Lymphatic & circulatory systems - 3 questions Endocrine system - 2 questions Respiratory system - 1 question Gastrointestinal system - 3 questions Genitouirinary systems - (reproductive & urinary) 2 questions Integument - 1 question Oral Histology (16 questions): Tooth & supporting structures - 9 questions Soft oral tissues (including dentin) - 5 questions Temporomandibular joint - 2 questions Developmental Biology (11 questions): Osteogenesis (bone formation) - 2 questions Tooth development, eruption & movement - 4 questions General embryology - 2 questions 2 National Board Part 1: Review questions for histology/oral histology (Answers follow at the end) 1. Normally most of the circulating white blood cells are a. basophilic leukocytes b. monocytes c. lymphocytes d. eosinophilic leukocytes e. neutrophilic leukocytes 2. Blood platelets are products of a. osteoclasts b. basophils c. red blood cells d. plasma cells e. megakaryocytes 3. Bacteria are frequently ingested by a. neutrophilic leukocytes b. basophilic leukocytes c. mast cells d. small lymphocytes e. fibrocytes 4. It is believed that worn out red cells are normally destroyed in the spleen by a. neutrophils b. -

Epithelium 2 : Glandular Epithelium Histology Laboratory -‐ Year 1, Fall Term Dr
Epithelium 2 : Glandular Epithelium Histology Laboratory -‐ Year 1, Fall Term Dr. Heather Yule ([email protected]) October 21, 2014 Slides for study: 75 (Salivary Gland), 355 (Pancreas Tail), 48 (Atrophic Mammary Gland), 49 (Active Mammary Gland) and 50 (Resting Mammary Gland) Electron micrographs for : study EM: Serous acinus in parotid gland EM: Mucous acinus in mixed salivary gland EM: Pancreatic acinar cell Main Objective: Understand key histological features of glandular epithelium and relate structure to function. Specific Objectives: 1. Describe key histological differences between endocrine and exocrine glands including their development. 2. Compare three modes of secretion in glands; holocrine, apocrine and merocrine. 3. Explain the functional significance of polarization of glandular epithelial cells. 4. Define the terms parenchyma, stroma, mucous acinus, serous acinus and serous a demilune and be able to them identify in glandular tissue. 5. Distinguish exocrine and endocrine pancreas. 6. Compare the histology of resting, lactating and postmenopausal mammary glands. Keywords: endocrine gland, exocrine gland, holocrine, apocrine, merocrine, polarity, parenchyma, stroma, acinus, myoepithelial cell, mucous gland, serous gland, mixed or seromucous gland, serous demilune, exocrine pancreas, endocrine pancreas (pancreatic islets), resting mammary gland, lactating mammary gland, postmenopausal mammary gland “This copy is made solely for your personal use for research, private study, education, parody, satire, criticism, or review -

Liver • Gallbladder
NORMAL BODY Microscopic Anatomy! Accessory Glands of the GI Tract,! lecture 2! ! • Liver • Gallbladder John Klingensmith [email protected] Objectives! By the end of this lecture, students will be able to: ! • trace the flow of blood and bile within the liver • describe the structure of the liver in regard to its functions • indicate the major cell types of the liver and their functions • distinguish the microanatomy of exocrine and endocrine function by the hepatocytes • explain the functional organization of the gallbladder at the cellular level (Lecture plan: overview of structure and function, then increasing resolution of microanatomy and cellular function) Liver and Gallbladder Liver October is “Liver Awareness Month” -- http://www.liverfoundation.org Liver • Encapsulated by CT sheath and mesothelium • Lobes largely composed of hepatocytes in parenchyma • Receives blood from small intestine and general circulation Major functions of the liver • Production and secretion of digestive fluids to small intestine (exocrine) • Production of plasma proteins and lipoproteins (endocrine) • Storage and control of blood glucose • Detoxification of absorbed compounds • Source of embyronic hematopoiesis The liver lobule • Functional unit of the parenchyma • Delimited by CT septa, invisible in humans (pig is shown) • Surrounds the central vein • Bordered by portal tracts Central vein, muralia and sinusoids Parenchyma: Muralia and sinusoids • Hepatocyte basolateral membrane faces sinusoidal lumen • Bile canaliculi occur between adjacent hepatocytes • Cords anastomose Vascularization of the liver • Receives veinous blood from small intestine via portal vein • Receives freshly oxygenated blood from hepatic artery • Discharges blood into vena cava via hepatic vein Blood flow in the liver lobes • flows in via the portal vein and hepatic artery • oozes through the liver lobules to central veins • flows out via the hepatic vein Portal Tract! (aka portal triad) • Portal venule • Hepatic arteriole • Bile duct • Lymph vessel • Nerves • Connective tissue Central vein! (a.k.a. -

An Analysis of Benign Human Prostate Offers Insights Into the Mechanism
www.nature.com/scientificreports OPEN An analysis of benign human prostate ofers insights into the mechanism of apocrine secretion Received: 12 March 2018 Accepted: 22 February 2019 and the origin of prostasomes Published: xx xx xxxx Nigel J. Fullwood 1, Alan J. Lawlor2, Pierre L. Martin-Hirsch3, Shyam S. Matanhelia3 & Francis L. Martin 4 The structure and function of normal human prostate is still not fully understood. Herein, we concentrate on the diferent cell types present in normal prostate, describing some previously unreported types and provide evidence that prostasomes are primarily produced by apocrine secretion. Patients (n = 10) undergoing TURP were prospectively consented based on their having a low risk of harbouring CaP. Scanning electron microscopy and transmission electron microscopy was used to characterise cell types and modes of secretion. Zinc levels were determined using Inductively Coupled Plasma Mass Spectrometry. Although merocrine secretory cells were noted, the majority of secretory cells appear to be apocrine; for the frst time, we clearly show high-resolution images of the stages of aposome secretion in human prostate. We also report a previously undescribed type of epithelial cell and the frst ultrastructural image of wrapping cells in human prostate stroma. The zinc levels in the tissues examined were uniformly high and X-ray microanalysis detected zinc in merocrine cells but not in prostasomes. We conclude that a signifcant proportion of prostasomes, possibly the majority, are generated via apocrine secretion. This fnding provides an explanation as to why so many large proteins, without a signal peptide sequence, are present in the prostatic fuid. Tere are many complications associated with the prostate from middle age onwards, including benign prostatic hyperplasia (BPH) and prostate cancer (PCa). -

Epithelium and Glands
EPITHELIUM AND GLANDS OBJECTIVES: After completing this exercise, students should be able to do the following: 1. Identify glands. 2. Classify glands based on secretory type. ASSIGNMENT FOR TODAY'S LABORATORY GLASS SLIDES SL 111 (Trachea) cilia and unicellular glands (goblet cells) SL 019 (Jejunum, PAS) unicellular glands SL 092 (Submandibular gland) serous, mucous and demilune secretory units SL 093 (Sublingual gland) mucous secretory units POSTED ELECTRON MICROGRAPHS # 7 Organelles # 11 Desmosomes # 12 Epithelium # 13 Freeze-fracture Lab 5 Posted EMs; Lab 5 Posted EMs with some yellow labels SUPPLEMENTAL MATERIAL: SUPPLEMENTARY ELECTRON MICROGRAPHS Rhodin, J. A.G., An Atlas of Histology. Glands pp. 46 - 52 Copies of this text are on reserve in the HSL. Glandular epithelium is specialized for the production and secretion of products. The cells that form glands are usually cuboidal or columnar in shape. In this exercise we are emphasizing morphological differences in glands with respect to secretory products. A. UNICELLULAR GLANDS: SL 111 (low, high), (Trachea, H&E); SL 019 (oil), (Jejunum, PAS), for review. Goblet cells may be few or numerous and are found in epithelia of the respiratory and alimentary systems. The secretory product is emptied into the lumen of the organ rather than into ducts (J. Fig. 4-18, 15-24; R. 5.38, Plate 60) B. MULTICELLULAR GLANDS: In general these glands are formed by invagination, proliferation, and differentiation of the epithelium from which they are derived. Glands that maintain a connection with the surface epithelium through ducts are termed exocrine glands, whereas glands that have lost this connection, and secrete instead to blood vessels, are called endocrine glands (see J. -
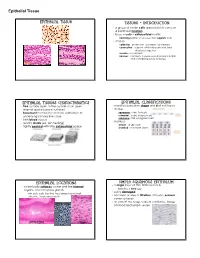
Epithelial Tissue
Epithelial Tissue Epithelial Tissue Tissues - Introduction · a group of similar cells specialized to carry on a particular function · tissue = cells + extracellular matrix nonliving portion of a tissue that supports cells · 4 types epithelial - protection, secretion, absorption connective - support soft body parts and bind structures together muscle - movement nervous - conducts impulses used to help control and coordinate body activities Epithelial Tissues Characteristics Epithelial Classifications · free surface open to the outside or an open · classified based on shape and # of cell layers internal space (apical surface) · shape · basement membrane anchors epithelium to squamous - thin, flat cells underlying connective tissue cuboidal - cube-shaped cells columnar - tall, elongated cells · lack blood vessels · number · readily divide (ex. skin healing) simple - single layer · tightly packed with little extracellular space stratified - 2 or more layers Epithelial Locations Simple Squamous Epithelium · a single layer of thin, flattened cells · cover body surfaces, cover and line internal organs, and compose glands looks like a fried egg · easily damaged skin cells, cells that line the stomach and small intestine, inside your mouth · common at sites of filtration, diffusion, osmosis; cover surfaces · air sacs of the lungs, walls of capillaries, linings cheek cells of blood and lymph vessels intestines skin Epithelial Tissue Simple Cuboidal Epithelium Simple Columnar Epithelium · single layer of cube-shaped cells · single layer of cells -

Nomina Histologica Veterinaria, First Edition
NOMINA HISTOLOGICA VETERINARIA Submitted by the International Committee on Veterinary Histological Nomenclature (ICVHN) to the World Association of Veterinary Anatomists Published on the website of the World Association of Veterinary Anatomists www.wava-amav.org 2017 CONTENTS Introduction i Principles of term construction in N.H.V. iii Cytologia – Cytology 1 Textus epithelialis – Epithelial tissue 10 Textus connectivus – Connective tissue 13 Sanguis et Lympha – Blood and Lymph 17 Textus muscularis – Muscle tissue 19 Textus nervosus – Nerve tissue 20 Splanchnologia – Viscera 23 Systema digestorium – Digestive system 24 Systema respiratorium – Respiratory system 32 Systema urinarium – Urinary system 35 Organa genitalia masculina – Male genital system 38 Organa genitalia feminina – Female genital system 42 Systema endocrinum – Endocrine system 45 Systema cardiovasculare et lymphaticum [Angiologia] – Cardiovascular and lymphatic system 47 Systema nervosum – Nervous system 52 Receptores sensorii et Organa sensuum – Sensory receptors and Sense organs 58 Integumentum – Integument 64 INTRODUCTION The preparations leading to the publication of the present first edition of the Nomina Histologica Veterinaria has a long history spanning more than 50 years. Under the auspices of the World Association of Veterinary Anatomists (W.A.V.A.), the International Committee on Veterinary Anatomical Nomenclature (I.C.V.A.N.) appointed in Giessen, 1965, a Subcommittee on Histology and Embryology which started a working relation with the Subcommittee on Histology of the former International Anatomical Nomenclature Committee. In Mexico City, 1971, this Subcommittee presented a document entitled Nomina Histologica Veterinaria: A Working Draft as a basis for the continued work of the newly-appointed Subcommittee on Histological Nomenclature. This resulted in the editing of the Nomina Histologica Veterinaria: A Working Draft II (Toulouse, 1974), followed by preparations for publication of a Nomina Histologica Veterinaria. -

Anatomy of the Gallbladder and Bile Ducts
BASIC SCIENCE the portal vein lies posterior to these structures; Anatomy of the gallbladder the inferior vena cava, separated by the epiploic foramen (the foramen of Winslow) lies still more posteriorly, and bile ducts behind the portal vein. Note that haemorrhage during gallbladder surgery may be Harold Ellis controlled by compression of the hepatic artery, which gives off the cystic branch, by passing a finger through the epiploic foramen (foramen of Winslow), and compressing the artery Abstract between the finger and the thumb placed on the anterior aspect A detailed knowledge of the gallbladder and bile ducts (together with of the foramen (Pringle’s manoeuvre). their anatomical variations) and related blood supply are essential in At fibreoptic endoscopy, the opening of the duct of Wirsung the safe performance of both open and laparoscopic cholecystectomy can usually be identified quite easily. It is seen as a distinct as well as the interpretation of radiological and ultrasound images of papilla rather low down in the second part of the duodenum, these structures. These topics are described and illustrated. lying under a characteristic crescentic mucosal fold (Figure 2). Unless the duct is obstructed or occluded, bile can be seen to Keywords Anatomical variations; bile ducts; blood supply; gallbladder discharge from it intermittently. The gallbladder (Figures 1 and 3) The biliary ducts (Figure 1) The normal gallbladder has a capacity of about 50 ml of bile. It concentrates the hepatic bile by a factor of about 10 and also The right and left hepatic ducts emerge from their respective sides secretes mucus into it from the copious goblet cells scattered of the liver and fuse at the porta hepatis (‘the doorway to the throughout its mucosa.