EMLA CREAM (Lidocaine 2.5% and Prilocaine 2.5%)
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

4% Citanest® Plain Dental (Prilocaine Hydrochloride Injection, USP) for Local Anesthesia in Dentistry
4% Citanest® Plain Dental (Prilocaine Hydrochloride Injection, USP) For Local Anesthesia in Dentistry Rx only DESCRIPTION 4% Citanest Plain Dental (prilocaine HCI Injection, USP), is a sterile, non-pyrogenic isotonic solution that contains a local anesthetic agent and is administered parenterally by injection. See INDICATIONS AND USAGE for specific uses. The quantitative composition is shown in Table 1. 4% Citanest Plain Dental contains prilocaine HCl, which is chemically designated as propanamide, N-(2- methyl-phenyl) -2- (propylamino)-, monohydrochloride and has the following structural formula: Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration. The specific quantitative composition is shown in Table 1. TABLE 1. COMPOSITION Product Identification Formula (mg/mL) Prilocaine HCl pH 4% Citanest® Plain Dental 40.0 6.0 to 7.0 Note: Sodium hydroxide or hydrochloric acid may be used to adjust the pH of 4% Citanest Plain Dental Injection. CLINICAL PHARMACOLOGY Mechanism of Action: Prilocaine stabilizes the neuronal membrane by inhibiting the ionic fluxes required for the initiation and conduction of impulses, thereby effecting local anesthetic action. Onset and Duration of Action: When used for infiltration injection in dental patients, the time of onset of anesthesia averages less than 2 minutes with an average duration of soft tissue anesthesia of approximately 2 hours. Based on electrical stimulation studies, 4% Citanest Plain Dental Injection provides a duration of pulpal anesthesia of approximately 10 minutes in maxillary infiltration injections. In clinical studies, this has been found to provide complete anesthesia for procedures lasting an average of 20 minutes. When used for inferior alveolar nerve block, the time of onset of 4% Citanest Plain Dental Injection averages less than three minutes with an average duration of soft tissue anesthesia of approximately 2 ½hours. -

Blockage of Neddylation Modification Stimulates Tumor Sphere Formation
Blockage of neddylation modification stimulates tumor PNAS PLUS sphere formation in vitro and stem cell differentiation and wound healing in vivo Xiaochen Zhoua,b,1, Mingjia Tanb,1, Mukesh K. Nyatib, Yongchao Zhaoc,d, Gongxian Wanga,2, and Yi Sunb,c,e,2 aDepartment of Urology, The First Affiliated Hospital of Nanchang University, Nanchang, Jiangxi 330006, China; bDivision of Radiation and Cancer Biology, Department of Radiation Oncology, University of Michigan, Ann Arbor, MI 48109; cInstitute of Translational Medicine, Zhejiang University School of Medicine, Hangzhou, Zhejiang 310029, China; dKey Laboratory of Combined Multi-Organ Transplantation, Ministry of Public Health, First Affiliated Hospital, Zhejiang University School of Medicine, Hangzhou 310058, China; and eCollaborative Innovation Center for Diagnosis and Treatment of Infectious Diseases, Zhejiang University, Hangzhou 310058, China Edited by Vishva M. Dixit, Genentech, San Francisco, CA, and approved March 10, 2016 (received for review November 13, 2015) MLN4924, also known as pevonedistat, is the first-in-class inhibitor acting alone or in combination with current chemotherapy of NEDD8-activating enzyme, which blocks the entire neddylation and/or radiation (6, 11). One of the seven clinical trials of MLN4924 modification of proteins. Previous preclinical studies and current (NCT00911066) was published recently, concluding a modest effect clinical trials have been exclusively focused on its anticancer property. of MLN4924 against acute myeloid leukemia (AML) (12). Unexpectedly, we show here, to our knowledge for the first time, To further elucidate the role of blocking neddylation in cancer that MLN4924, when applied at nanomolar concentrations, signif- treatment, we thought to study the effect of MLN4924 on cancer icantly stimulates in vitro tumor sphere formation and in vivo stem cells (CSCs) or tumor-initiating cells (TICs), a small group tumorigenesis and differentiation of human cancer cells and mouse of tumor cells with stem cell properties that have been claimed to embryonic stem cells. -

Medicare 2019 Part C & D Star Ratings Cut Point Trends
Trends in Part C & D Star Rating Measure Cut Points Updated – 12/19/2018 (Last Updated 12/19/2018) Page 1 Document Change Log Previous Revision Version Description of Change Date - Final release of the 2019 Star Ratings Cut Point Trend document 12/19/2018 (Last Updated 12/19/2018) Page i Table of Contents DOCUMENT CHANGE LOG .............................................................................................................................. I TABLE OF CONTENTS .................................................................................................................................... II INTRODUCTION ............................................................................................................................................... 1 PART C MEASURES ........................................................................................................................................ 2 Measure: C01 - Breast Cancer Screening ........................................................................................................................ 2 Measure: C02 - Colorectal Cancer Screening .................................................................................................................. 3 Measure: C03 - Annual Flu Vaccine .................................................................................................................................. 4 Measure: C04 - Improving or Maintaining Physical Health ........................................................................................... -

Evaluation of Liposomal Delivery System for Topical Anesthesia
THERAPEUTICS FOR THE CLINICIAN Evaluation of Liposomal Delivery System for Topical Anesthesia Mohamed L. Elsaie, MD, MBA; Leslie S. Baumann, MD Local anesthesia is an integral aspect of cutane- infiltrative anesthetics, now can be accomplished ous surgery. Its effects provide a reversible loss safely and comfortably with the use of topi- of sensation in a limited area of skin, allowing cal anesthetics.1 Topical anesthetics originated in dermatologists to perform diagnostic and thera- South America; native Peruvians noted perioral peutic procedures safely, with minimal discomfort numbness when chewing the leaf of the cocoa plant and risk to the patient. Moreover, the skin acts (Erythroxylon coca). The active alkaloid, cocaine, was as a major target as well as principle barrier for isolated by Niemann in 1860 and applied to con- topical/transdermal (TT) drug delivery. The stra- junctival mucosa for topical anesthesia by Koller in tum corneum (SC) plays a crucial role in barrier 1884. The development of similar benzoic acid esters function for TT drug delivery. Despite the major continued until 1943 when Loefgren synthesized lido- research and development efforts in TT systems caine hydrochloride, the first amide anesthetic.2 and their implementation for use of topical anes- We review the administration of local anes- thetics, low SC permeability limits the useful- thetics, specifically the liposomal delivery system ness of topical delivery, which has led to other for topical anesthesia, based on a review of the delivery system developments, including vesicu- literature and clinical experience. lar systems such as liposomes, niosomes, and proniosomes, with effectiveness relying on their Anatomy physiochemical properties. -

Topical Therapy As a Treatmentfor Brachioradial
Journal of Case Reports: Open Access Case report Open Access Topical Therapy as a Treatmentfor Brachioradial Pruritis: a Case Report Brianna De Souza M.D, Amy McMichael M.D* Department of Dermatology, Wake Forest University School of Medicine, Winston-Salem, North Carolina *Corresponding author: Amy McMichael, MD Department of Dermatology, Wake Forest Baptist Medical Center,1 Medical Center Blvd, Winston-Salem, NC 27157, Phone: 336-716-7882, Email: [email protected] Received Date: April 12, 2019 Accepted Date: May 06, 2019 Published Date: May 08, 2019 Citation: Brianna De Souza (2019) Topical Therapy as a Treatmentfor Brachioradial Pruritis: a Case Report. Case Reports: Open Access 4: 1-5. Abstract Management of brachioradial pruritus (BRP) presents a formidable challenge to dermatologists and neurologists. BRP is a rare, neurocutaneous condition characterized by sharply localized, chronic pain with associated itching, burning, stinging, and or tingling sensation. Effective care of this patient population is confounded by limitations within the litera- ture, comprised of case series and case reports. We present a case of one middle-aged female with a chronic history of BRP recalcitrant to the following oral therapies: pregabalin, gabapentin, mirtazapine, prednisone, and amitriptyline, as well as topical triamcinolone. After being evaluated in the clinic, the patient was started on combination therapy withKetamine 10%, Amitriptyline 5%, and Lidocaine 5% topical cream to which she responded. Keywords: Brachioradial pruritus, Brachioradial, Pruritus, Neurocutaneous ©2019 The Authors. Published by the JScholar under the terms of the Crea- tive Commons Attribution License http://creativecommons.org/licenses/ by/3.0/, which permits unrestricted use, provided the original author and source are credited. -

Prolonged Duration Topical Corneal Anesthesia with the Cationic Lidocaine Derivative QX-314
https://doi.org/10.1167/tvst.8.5.28 Article Prolonged Duration Topical Corneal Anesthesia With the Cationic Lidocaine Derivative QX-314 Alan G. Woodruff1,2, Claudia M. Santamaria1, Manisha Mehta1,2, Grant L. Pemberton1, Kathleen Cullion1,2,4, and Daniel S. Kohane1,2,3 1 Kohane Lab for Biomaterials and Drug Delivery, Department of Anesthesia, Perioperative and Pain Medicine, Division of Critical Care, Boston Children’s Hospital, Boston, MA, USA 2 Harvard Medical School, Boston, MA, USA 3 David H. Koch Institute, Massachusetts Institute of Technology, Cambridge, MA, USA 4 Department of Medicine, Division of Medicine Critical Care, Boston Children’s Hospital, Harvard Medical School, Boston, MA, USA Correspondence: Daniel S. Kohane, Purpose: Topical corneal local anesthetics are short acting and may impair corneal Laboratory for Biomaterials and healing. In this study we compared corneal anesthesia and toxicity of topically applied Drug Delivery, Department of Anes- N-ethyl lidocaine (QX-314) versus the conventional local anesthetic, proparacaine thesia, Division of Critical Care (PPC). Medicine, Boston Children’s Hospi- tal, Harvard Medical School, 61 Methods: Various concentrations of QX-314 and 15 mM (0.5%) PPC were topically Binney Street, Room 361, Boston, applied to rat corneas. Corneal anesthesia was assessed with a Cochet-Bonnet MA 02115, USA. e-mail: Daniel. esthesiometer at predetermined time points. PC12 cells were exposed to the same [email protected] solutions to assess cytotoxicity. Repeated topical corneal administration in rats was then used to assess for histologic evidence of toxicity. Finally, we created uniform Received: 6 May 2019 corneal epithelial defects in rats and assessed the effect of repeated administration of Accepted: 15 August 2019 these compounds on the defect healing rate. -

Local Anesthetics
Local Anesthetics Introduction and History Cocaine is a naturally occurring compound indigenous to the Andes Mountains, West Indies, and Java. It was the first anesthetic to be discovered and is the only naturally occurring local anesthetic; all others are synthetically derived. Cocaine was introduced into Europe in the 1800s following its isolation from coca beans. Sigmund Freud, the noted Austrian psychoanalyst, used cocaine on his patients and became addicted through self-experimentation. In the latter half of the 1800s, interest in the drug became widespread, and many of cocaine's pharmacologic actions and adverse effects were elucidated during this time. In the 1880s, Koller introduced cocaine to the field of ophthalmology, and Hall introduced it to dentistry Overwiev Local anesthetics (LAs) are drugs that block the sensation of pain in the region where they are administered. LAs act by reversibly blocking the sodium channels of nerve fibers, thereby inhibiting the conduction of nerve impulses. Nerve fibers which carry pain sensation have the smallest diameter and are the first to be blocked by LAs. Loss of motor function and sensation of touch and pressure follow, depending on the duration of action and dose of the LA used. LAs can be infiltrated into skin/subcutaneous tissues to achieve local anesthesia or into the epidural/subarachnoid space to achieve regional anesthesia (e.g., spinal anesthesia, epidural anesthesia, etc.). Some LAs (lidocaine, prilocaine, tetracaine) are effective on topical application and are used before minor invasive procedures (venipuncture, bladder catheterization, endoscopy/laryngoscopy). LAs are divided into two groups based on their chemical structure. The amide group (lidocaine, prilocaine, mepivacaine, etc.) is safer and, hence, more commonly used in clinical practice. -

Antagonism of Lidocaine Inhibition by Open-Channel Blockers That Generate Resurgent Na Current
4976 • The Journal of Neuroscience, March 13, 2013 • 33(11):4976–4987 Cellular/Molecular Antagonism of Lidocaine Inhibition by Open-Channel Blockers That Generate Resurgent Na Current Jason S. Bant,1,3 Teresa K. Aman,2,3 and Indira M. Raman1,2,3 1Interdepartmental Biological Sciences Program, 2Northwestern University Interdepartmental Neuroscience Program, and 3Department of Neurobiology, Northwestern University, Evanston, Illinois 60208 Na channels that generate resurgent current express an intracellular endogenous open-channel blocking protein, whose rapid binding upon depolarization and unbinding upon repolarization minimizes fast and slow inactivation. Na channels also bind exogenous com- pounds, such as lidocaine, which functionally stabilize inactivation. Like the endogenous blocking protein, these use-dependent inhibi- tors bind most effectively at depolarized potentials, raising the question of how lidocaine-like compounds affect neurons with resurgent Na current. We therefore recorded lidocaine inhibition of voltage-clamped, tetrodotoxin-sensitive Na currents in mouse Purkinje neu- rons, which express a native blocking protein, and in mouse hippocampal CA3 pyramidal neurons with and without a peptide from the   cytoplasmic tail of NaV 4 (the 4 peptide), which mimics endogenous open-channel block. To control channel states during drug exposure, lidocaine was applied with rapid-solution exchange techniques during steps to specific voltages. Inhibition of Na currents by lidocaine was diminished by either the 4 peptide or the native blocking protein. In peptide-free CA3 cells, prolonging channel opening with a site-3 toxin, anemone toxin II, reduced lidocaine inhibition; this effect was largely occluded by open-channel blockers, suggesting that lidocaine binding is favored by inactivation but prevented by open-channel block. -
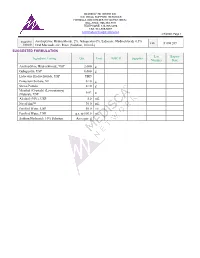
Amitriptyline Hydrochloride 2%, Gabapentin 6%, Lidocaine Hydrochloride 0.5% FIN F 008 269 Formula Oral Mucoadhesive Rinse (Solution, 100 Ml)
MEDISCA® NETWORK INC. TECHNICAL SUPPORT SERVICES FORMULATION CHEMISTRY DEPARTMENT TOLL-FREE: 866-333-7811 TELEPHONE: 514-905-5096 FAX: 514-905-5097 [email protected] 4/7/2020; Page 1 Suggested Amitriptyline Hydrochloride 2%, Gabapentin 6%, Lidocaine Hydrochloride 0.5% FIN F 008 269 Formula Oral Mucoadhesive Rinse (Solution, 100 mL) SUGGESTED FORMULATION Lot Expiry Ingredient Listing Qty. Unit NDC # Supplier Number Date Amitriptyline Hydrochloride, USP 2.000 g Gabapentin, USP 6.000 g Lidocaine Hydrochloride, USP TBD Potassium Sorbate, NF 0.10 g Stevia Powder 0.10 g Menthol (Crystals) (Levorotatory) 0.02 g (Natural), USP Alcohol (95%), USP 5.0 mL NovaFilm™ 30.0 mL Purified Water, USP 50.0 mL Purified Water, USP q.s. to 100.0 mL Sodium Hydroxide 10% Solution As required MEDISCA® NETWORK INC. TECHNICAL SUPPORT SERVICES FORMULATION CHEMISTRY DEPARTMENT TOLL-FREE: 866-333-7811 TELEPHONE: 514-905-5096 FAX: 514-905-5097 [email protected] 4/7/2020; Page 2 Suggested Amitriptyline Hydrochloride 2%, Gabapentin 6%, Lidocaine Hydrochloride 0.5% FIN F 008 269 Formula Oral Mucoadhesive Rinse (Solution, 100 mL) SPECIAL PREPARATORY CONSIDERATIONS Ingredient-Specific Information Light Sensitive (protect from light whenever possible): Amitriptyline Hydrochloride, Gabapentin Hygroscopic (protect from moisture whenever possible): Stevia Powder Narrow Therapeutic Index Lidocaine Hydrochloride Suggested Preparatory Guidelines ■ Non-Sterile Preparation □ Sterile Preparation Processing Error / To account for processing error and pH testing considerations during preparation, it is Testing Considerations: suggested to measure an additional 3 to 5% of the required quantities of ingredients. Special Instruction: This formula may contain one or more Active Pharmaceutical Ingredients (APIs) that may be classified as hazardous, please refer & verify the current NIOSH list of Antineoplastic and Other Hazardous Drugs in Healthcare Settings, 2016. -

Thermo-Responsive Poly(N-Isopropylacrylamide)- Cellulose Nanocrystals Hybrid Hydrogels for Wound Dressing
Article Thermo-Responsive Poly(N-Isopropylacrylamide)- Cellulose Nanocrystals Hybrid Hydrogels for Wound Dressing Katarzyna Zubik 1, Pratyawadee Singhsa 1,2, Yinan Wang 1, Hathaikarn Manuspiya 2 and Ravin Narain 1,* 1 Department of Chemical and Materials Engineering, Donadeo Innovation Centre in Engineering, 116 Street and 85 Avenue, Edmonton, AB T6G 2G6, Canada; [email protected] (K.Z.); [email protected] (P.S.); [email protected] (Y.W.) 2 The Petroleum and Petrochemical College, Center of Excellence on Petrochemical and Materials Technology, Chulalongkorn University, Soi Chulalongkorn 12, Pathumwan, Bangkok 10330, Thailand; [email protected] * Correspondence: [email protected]; Tel.: +1-780-492-1736 Academic Editor: Shiyong Liu Received: 29 January 2017; Accepted: 21 March 2017; Published: 24 March 2017 Abstract: Thermo-responsive hydrogels containing poly(N-isopropylacrylamide) (PNIPAAm), reinforced both with covalent and non-covalent interactions with cellulose nanocrystals (CNC), were synthesized via free-radical polymerization in the absence of any additional cross-linkers. The properties of PNIPAAm-CNC hybrid hydrogels were dependent on the amounts of incorporated CNC. The thermal stability of the hydrogels decreased with increasing CNC content. The rheological measurement indicated that the elastic and viscous moduli of hydrogels increased with the higher amounts of CNC addition, representing stronger mechanical properties of the hydrogels. Moreover, the hydrogel injection also supported the hypothesis that CNC reinforced the hydrogels; the increased CNC content exhibited higher structural integrity upon injection. The PNIPAAm- CNC hybrid hydrogels exhibited clear thermo-responsive behavior; the volume phase transition temperature (VPTT) was in the range of 36 to 39 °C, which is close to normal human body temperature. -

The Effects of Lidocaine and Mefenamic Acid on Post-Episiotomy
Shiraz E-Med J. 2016 March; 17(3):e36286. doi: 10.17795/semj36286. Published online 2016 March 27. Research Article The Effects of Lidocaine and Mefenamic Acid on Post-Episiotomy Pain: A Comparative Study Masoumeh Delaram,1,* Lobat Jafar Zadeh,2 and Sahand Shams3 1Faculty of Nursing and Midwifery, Shahrekord University of Medical Sciences, Shahrekord, IR Iran 2Faculty of Medicine, Shahrekord University of Medical Sciences, Shahrekord, IR Iran 3Faculty of Veterinary Medicine, Shahrekord University, Shahrekord, IR Iran *Corresponding author: Masoumeh Delaram, Faculty of Nursing and Midwifery, Shahrekord University of Medical Sciences, Shahrekord, IR Iran. Tel: +98-3813335648, Fax: +98-3813346714, E-mail: [email protected] Received 2016 January 13; Revised 2016 February 29; Accepted 2016 March 04. Abstract Background: Most women suffer pain following an episiotomy and oral non-steroidal anti-inflammatory drugs are commonly used for pain relief. Due to the gastrointestinal side effects of oral drugs, it seems that women are more accepting of topical medications for pain relief. Objectives: Therefore, the aim of this study was to compare the effects of lidocaine and mefenamic acid on post-episiotomy pain. Patients and Methods: This clinical trial was carried out in 2011. It involved sixty women with singleton pregnancy who were given an episiotomy at 38 to 42 weeks of gestation. The participants were randomly divided into two groups. One group received 2% lido- caine cream (n = 30), while the other group received 250 mg of mefenamic acid (n = 30). The data were collected via a questionnaire and a visual analog scale. Pain intensity was compared from the first complaint by the mother and at 6, 12, and 24 hours after the delivery in both groups. -
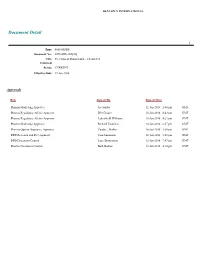

Document Detail
DENTSPLY INTERNATIONAL Document Detail 1 Type: 0090-MSDS Document No.: 0090-SDS-008[00] Title: 4% Citanest Plain Dental - US and CA Comment Status: CURRENT Effective Date: 12-Jan-2018 Approvals Role Sign-off By Sign-off Date Pharma Marketing Approver Joe Santos 12-Jan-2018 2:40 pm GMT Pharma Regulatory Affairs Approver Deb Crouse 10-Jan-2018 6:43 pm GMT Pharma Regulatory Affairs Approver Lakeisha R Williams 10-Jan-2018 4:21 pm GMT Pharma Marketing Approver Richard Tootchen 10-Jan-2018 6:57 pm GMT Pharma Quality Assurance Approver Candace Walker 10-Jan-2018 4:05 pm GMT DPD Research and Development Tom Simonton 10-Jan-2018 8:48 pm GMT DPD Document Control Lucy Brenneman 12-Jan-2018 7:47 pm GMT Pharma Document Control Beth Bodnar 12-Jan-2018 4:18 pm GMT SOP DOC.022-F01 Rev.1 Safety Data Sheet Safety Data Sheet conforms to Regulation (EC) 1907/2006, Regulation (EC) 1272/2008 and Regulation (EC) 2015/830, Date Issued: 01November 2017 US 29CFR1910.1200, Canada Hazardous Products Document Number: SDS-008 Regulation. Date Revised: New SDS Revision Number: 00 1. IDENTIFICATION OF THE SUBSTANCE/MIXTURE AND OF THE COMPANY/UNDERTAKING 1.1 Product Identifier: Trade Name (as labeled): 4% Citanest® Plain DENTAL (prilocaine HCl Injection, USP) Part/Item Numbers: 46616 71115 1.2 Relevant Identified Uses of the Substance or Mixture and Uses Advised Against: Recommended Use: Local anesthetic solution for use in peripheral nerve blocks Restrictions on Use: For Professional Use Only 1.3 Details of the Supplier of the Safety Data Sheet: Manufacturer/Supplier Name: DENTSPLY Pharmaceutical Manufacturer/Supplier Address: 1301 Smile Way York, PA 17404 Manufacturer/Supplier Telephone Number: 800-989-8826 or 717-767-8502 (Product Information) Email address: [email protected] 1.4 Emergency Telephone Number: Transportation Emergency Contact Number: 800-424-9300 Chemtrec 2.